Annual Report of the Chief Medical Officer 2012 - Population Health and Improvement Science
The Annual Report of the Chief Medical Officer 2012
CHAPTER 2
Healthy Ageing
In 2006, EuroHealthNet, a partnership of European organisations involved in promoting health and wellbeing, published a review of future trends in the health of older people in European countries. "Healthy ageing - a challenge for Europe" (available at www.healthyageing.eu) defined the challenge as "the process of optimising opportunities for physical, social and mental health to enable older people to take an active part in society without discrimination and to enjoy an independent and good quality of life."
The authors of the report suggested that the need for policies to promote healthy ageing is a challenge for all European countries. They estimated that by 2025 about one-third of Europe's population will be aged 60 years and over, and there will be a particularly rapid increase in the number of people aged 80 years and older.
The population of Scotland on Census Day in 2011 was estimated to be 5,295,000 - the highest ever. The population had increased by 233,000 (5%) since the last census in 2001. This was the fastest growth rate between 2 census years in the last century and projections indicated that there would be a substantial increase in the number of people of pensionable age in Scotland between 2010 and 2035. Figure 2 shows the potential scale of the increase.
Figure 2: The projected percentage change in Scotland's population by age group.
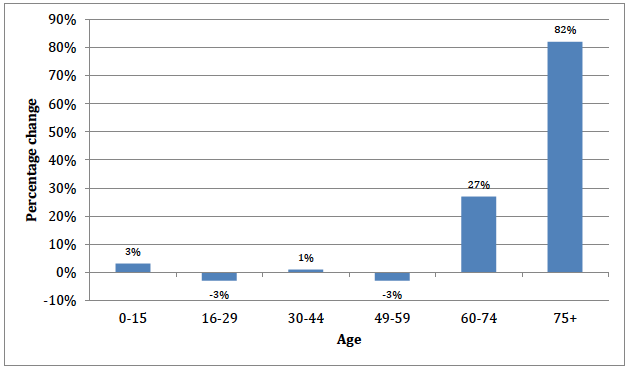
A more elderly population also means a more dependent population. The dependency ratio is defined as the ratio of people aged under 16 and over pensionable age to those of working age. This ratio is projected to rise from 60 per 100 in 2010 to 64 per 100 in 2035 and in the most elderly sections of the population that are projected to increase most dramatically. Between 2010 and 2035 the number of those aged 75 and over are projected to increase by 82%. At present, there are estimated to be around 820 people in Scotland over 100. This number is projected to increase to 7,600 by 2035.
Implications for society
There is considerable economic interest in the ageing population. The phenomenon is frequently referred to as the "demographic time bomb" by economists because of the possible impact of a relative reduction in the size of the workforce on economic growth and the increasing need for public expenditure to support an increasingly dependent group of elderly people.
However, ageing should not be seen as a burden. It does not necessarily decrease a person's ability to contribute to society. Older people can enjoy a high quality of life and make important contributions to society. If we are to maximise wellbeing and support older people to make their contribution to society, we need to see an opportunity rather than a burden. This means taking an assets approach to older people's wellbeing.
It would be a mistake to focus exclusively on older people's problems, seeing them simply as dependent individuals requiring services. We should concentrate on what people can do, rather than what they cannot. If we are to minimise the economic impact of the ageing population but, more importantly, if we are to do the right thing for older people, we should try to create a positive sense of control amongst the elderly. In doing so, we create the conditions to promote healthy behaviours amongst older people.
The health of older Scots
The Scottish Health Survey has reported on the health of older Scots. Twenty-two percent of adults aged 65 and over describe their health as 'very good', compared with 39% of adults aged 16-64 years. Predictably, there was a decline in the number of people reporting very good health as age increased and only 16% in those aged 85 years and over felt themselves to be in good health. (Figure 3)
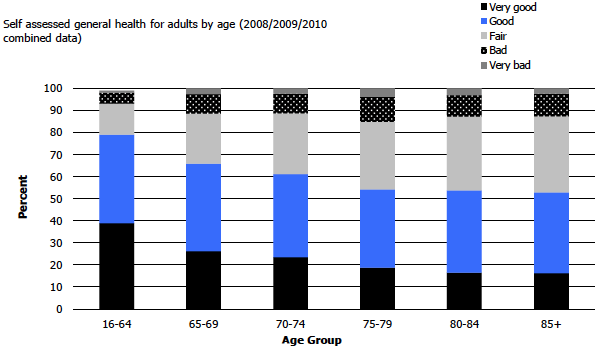
The factors independently associated with poor or very poor health in over 65s were living in an area of deprivation and being a current or an ex-smoker. Wellbeing, as measured by the Warwick-Edinburgh Mental Wellbeing Scale, was higher among adults aged 65 and over than those aged 16-64, though it decreased with age among older adults, particularly among men. Among adults aged 65 and over, the odds of having poor wellbeing were higher in people living alone. People who were married or cohabiting reported higher levels of wellbeing.
Sixty-six percent of men and 67% of women aged 65 years and over had a long-term health condition compared with 33% of men and 37% of women aged 16-64. The 3 most common categories of conditions reported by adults aged 65 and over were musculoskeletal conditions, conditions of the heart and circulatory system, and endocrine and metabolic disorders such as diabetes. Interestingly, older people had lower rates of mental disorders and skin complaints than in the 16-64 age group.
Health related behaviours remain a significant issue for the elderly. Although the proportion of the population exceeding recommended weekly limits for alcohol consumption declines after the age of 70, it remains significant. (Figure 4)
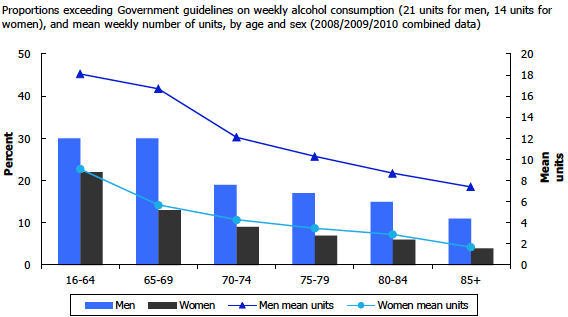
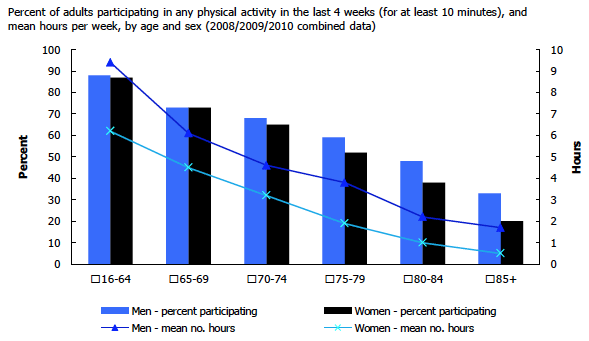
Physical activity is also a challenge after the age of 65 with a decline in the number reporting participation in any activity lasting more than 10 minutes. (Figure 5). While it is a challenge, physical activity can also be seen as an opportunity for the elderly to increase social connectedness by participating in activities in group settings.
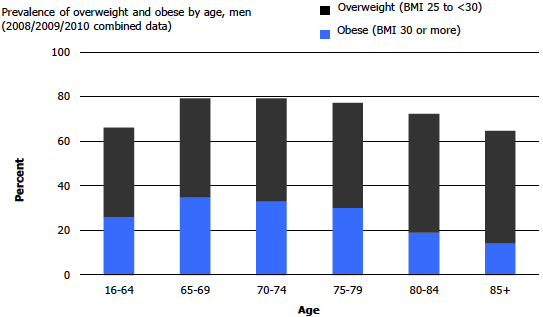
The proportion of the population who are overweight or obese increases after the age of 65 (Figure 6). The reducing levels of physical activity associated with retiral from work may contribute to this effect.
A healthy ageing collaborative?
The approach being taken to improve care of children in the Early Years Collaborative seems applicable to improving wellbeing of older people. It begins by setting aims for improvement and then identifying the drivers of change. Identifying those drivers which help maintain wellness in the older Scottish population could allow us to identify interventions likely to enhance wellness.
The World Health Organisation in Europe has identified a number of policies and interventions which it believes could produce significant gains. These include:
- prevention of falls;
- promotion of physical activity;
- vaccination of older people and prevention of infectious disease in health-care settings;
- public support for informal care giving with a focus on home care, including self-care;
- building capacity in geriatrics and gerontology among the health and social care workforce;
- prevention of social isolation and social exclusion;
- strategies to ensure the quality of care for older people, with a focus on dementia care and palliative care for long-term patients;
- prevention of elder maltreatment.
Some drivers of wellbeing in the elderly
Physical activity
Undoubtedly, the broad benefits of physical activity for older people are well documented and associated with improved length and quality of life. People tend to become progressively less active as they get older and more imaginative ways of helping them remain involved in taking regular exercise are important. The 3 leading causes of death due to injury in older people in Europe are self-inflicted injuries, falls and road traffic injuries. Exercising balance and strengthening muscles reduce falls in older people.
Health promotion programmes
Management of conventional risk factors such as tobacco and alcohol would also improve fitness in the elderly. A majority of smoking-related deaths in the EU occur in older people and smokers who stop at the age of 65-70 halve their excess risk of premature death. Smoking cessation remains the most effective method of altering such risk. Health problems caused by alcohol use are often under-detected and neglected among older people. Also, considerable gains in terms of mortality and function could be achieved if older people adopted a healthier lifestyle with healthy eating habits. (Figures 4,5 and 6)
Healthcare
Access to health care may be difficult for the elderly. Older people with low socioeconomic status may have low "health literacy"; that is, they may know significantly less than other people about disease and how to maintain good health. Health literacy is a more meaningful predictive factor than education for older people's use of preventive services, and has implications for the design of interventions.
In addition, older people are the largest per capita users of medication. The risk of adverse reactions increases with the number of individual drugs taken. Lack of overall knowledge of what medicines and treatment a patient is receiving is an important explanation of drug problems. As well under-use, over-use and unsuitable combination of medication are other common problems.
Pre-retirement planning
Ageing is a gradual process and there is much we can do to promote good mental health and well-being in later life. In the retirement and pre-retirement phase of working life, employers and employees alike need to take responsibility for the health of the older members of the workforce so that these can work to higher ages. Anticipatory social interventions concerning pre-retirement have positive effects and contribute to empowerment.
Connectedness
There is strong evidence that complex patterns of social connectedness enhance a sense of control and wellbeing. Providing opportunities for older people to do voluntary work with others improves the quality of life of the volunteers and those who receive the services. Low social capital correlates with mortality. In addition, mental health is improved with social connectedness. Participation in meaningful activities, strong personal relationships and good physical health are key factors, while age discrimination has a negative impact.
Strained family relations are risk factors for the abuse of older people or for violence. The issue of "elder abuse" is not particularly visible and it is an area which merits further research and attention. Promoting social interaction and involving older people in a wide circle of friends is likely to be a mitigating factor for domestic violence in isolated homes
Environment
A supportive environment which encourages physical activity and socialization is helpful in promoting wellness. Accessible green areas allow older people with poor mobility or disability to spend time outdoors, are an important determinant of good health and the quality of the environment in terms of safety, freedom from crime and freedom from exposure to hazards such as air pollution is important in encouraging participation.
Economic support
Poverty is an important socioeconomic health determinant, with negative effects on health, life expectancy, disease and disability. In healthy-ageing strategies, health promotion should give priority to addressing the health of the more disadvantaged older people. Poverty is also a risk factor for mental ill-health.
Gender differences
Gender has to be taken into account when planning and implementing health promotion. Women living alone often risk poverty in later life because their lifetime earnings are less than those of men, as are their pension entitlements. Women live longer than men in all European countries but report more psychological symptoms and consult health professionals more often and receive more treatment than men do. Men and women need to be motivated differently to participate in health promotion activities. The relationship between belonging to a minority group and ageing and health needs more exploration.
Sustainable policies and programmes
Most European countries seem to have policies and strategies for healthy ageing and there are many examples of good practice. However, policies are often disjointed and rarely present a holistic view of older people's needs. As a result, funding is precarious. Most policies do not refer to or apparently collect health data. Policies seldom allocate funds explicitly for health promotion, which may hinder local implementation. There is a need to involve older people in planning, and to promote positive images of ageing, avoiding any arbitrary focus on chronological age.
The EuroHealthNet Report indicate the importance of sustainability, i.e. transforming projects into programmes, and collaboration by people throughout the community. It describes a number of healthy ageing projects already working in Europe. Most of the projects are described as being suitable for implementation in other countries. Building social capital and promoting physical activity are the most common major topics in the 'good practice' projects. Often in combination, they may lead to improved physical health and the alleviation of loneliness. The key issue for Scotland is to commit to a programme to promote healthy ageing. We should set aims with timescales and start work on the drivers of change.
Contact
Email: Diane Dempster