Annual Report 2014 - Reporting on the Quality and Efficiency Support Team
QuEST’s Annual Report 2014 provides an overview of QuEST programmes’ achievements in 2014 and upcoming priorities for 2015. The report features a wealth of case studies from Boards as well as our programmes. These case studies form a comprehensive collection of innovative quality improvement work currently undertaken in NHSScotland – driven, supported and/or resourced by QuEST. The report’s foreword is provided by Shona Robison, Cabinet Secretary for Health, Wellbeing and Sport.
Part 08: Prescribing
ABOUT THE PROGRAMME
Simon Hurding
t: 0131 244 2397
e: simon.hurding@scotland.gsi.gov.uk
drivers
NHSScotland spends £1.3 billion a year on medicines. Of this expenditure, around £1 billion is spent on medicines dispensed in primary care.
There has been considerable work to improve the quality and efficiency of primary care prescribing over the last 10 years. Further improvements are possible and require partnership working between the NHS Boards and all clinicians involved in prescribing.
The Prescribing Programme is now in its third year, with the aim to take a national approach to improving the use of evidence-based and cost-effective prescribing.
aims
- Identifying the improvement opportunities in Scottish prescribing
- Developing national prescribing strategies
- Monitoring progress and sharing learning and expertise between NHS Boards
workstreams
- National Therapeutic Indicators
- Polypharmacy
- National prescribing strategies (respiratory and diabetes)
- Waste and repeat prescribing
- Development and support of the Scottish Prescribing Advisers Association
achievements 2014
- There have been three sets of National Therapeutic Indicators (NTI) from 2012-13 to 2014-15. They provide comparative prescribing data between the NHS Boards and between Scottish General Practices. They are based around agreed areas of prescribing that are suitable for the use of comparative data. The key aim is to challenge inappropriate variation whilst recognising the different case mix of patients treated. Analysis of the distribution curve of achievement allows the setting of practice-based individualised targets for practices to work to. The NTI 2013-14 demonstrated £8.1 million of improved efficiency whilst also improving the quality of prescribing.
- The first National Polypharmacy prescribing guideline was published in 2012-13. The strategy provides a framework for the review of patients with multiple conditions, who are subsequently prescribed multiple medicines. The guideline has been used by the NHS Boards to implement polypharmacy reviews. The requirement for polypharmacy has been included as part of the Scottish GP contract (2013-14 and 2014-15) and most NHS Boards have an enhanced service polypharmacy contract for General Practices to use. The guideline recognises that many patients on multiple medications are deriving benefit. The challenge is to identify those patients who are at increasing risk of an adverse drug event. The polypharmacy guideline is currently undergoing an in depth review.
- National prescribing strategies in both diabetes and respiratory were published in May 2014. These have been developed through partnership working between the relevant managed clinical networks, the NHS Boards and the QuEST National Prescribing Programme. The aim for the strategies is to help standardise care between the NHS Boards to improve the quality and efficiency of patient care.
priorities 2015
- The work of the QuEST National Prescribing Programme has been transferred to the Pharmacy and Medicines division as the nascent Therapeutics branch.
- NTIs will be refreshed for 2015 and work will be undertaken to continue to embed these in prescribing practice. Work is on-going to ascertain the success of this approach.
- Work will be undertaken to support the implementation of polypharmacy reviews and to measure the impact of the reviews on patient safety.
- The Scottish Therapeutics Utility (STU) is being developed as an IT tool to help General Practices review their use of repeat medicines with the ultimate aim of reducing medicines waste.
- Publication and follow-up for the diabetes and respiratory prescribing strategies.
- Review of the medicines management domain of the Scottish GP contract.
http://www.qihub.scot.nhs.uk/quality-and-efficiency/prescribing.aspx
Programme Case Study
Prescribing - National Therapeutic Indicators
Background and context
The annual drugs budget for primary care is approximately £1 billion per year - this equates to around 10 per cent of the total NHSScotland spend. It is important that this resource is used as effectively as possible.
National Therapeutic Indicators (NTIs) were first established in April 2012 to provide benchmarking across primary care prescribing in Scotland.
NTIs are a way of providing an evidence-based prescribing standard. They identify major areas where there is variation in prescribing quality; the intention is to reduce inappropriate variation in prescribing. The ideal indicator promotes effective, safe and efficient prescribing.
Within the last 10 years, medicine use has consistently risen between 3 and 5 per cent annually. During 2013-14 the increase rate was reduced to 1.7 per cent in Scotland - further work is required to identify the NTIs role in the reduced rate of medicines volume increase.
Problem
- Variation occurs in prescribing practice, between NHS Boards and between General Practices. This can have implications for health outcomes for patients as well as the overall efficiency and cost of the service.
- An aging population is one factor leading to an increase in morbidity rates as well as a growth in the volume of medicines use. The resulting increase in prescriptions and implications for drug expenditure is considered potentially unsustainable.
- There are a number of national medicines use priority areas, where variation between General Practices may have an effect on clinical outcomes and patient safety. One important area is around the inappropriate use of antibiotics.
Aim
The aim for NTIs is to improve the quality (effectiveness, safety, equitability and efficiency) of primary care prescribing. Specific focus is on:
- identifying the improvement opportunities in Scottish prescribing
- informing the development of local and national prescribing strategies
- monitoring programmes and sharing learning and expertise between NHS Boards
- informing NHS Board prescribing plans
- facilitating NHS Boards to challenge inappropriate variation whilst recognising the different case mix of patients treated
- achieving improved health outcomes for patients through appropriate use of medicines
Action taken
The Prescribing Information System for Scotland (PRISMS) is recognised as a source of highly robust primary care prescribing data, and provides the data used for the NTIs. PRISMS is maintained by Information Services Division (ISD) and allows access to the data collected by Practitioner Services Division (PSD) when processing each prescription dispensed. The resulting payment verification data is then accessed via PRISMS.
QuEST coordinated the compilation of data and led the analysis and interpretation - the resulting report was the first instance of a consistent national approach to benchmarking of prescribing in primary care.
The report presents the rationale as to why NTIs will improve prescribing and advocates a consistent approach to data collection. Achievement against each indicator is analysed from the normal distribution curve. 'Best in class' practices are identified from the lower quartile for indicators promoting a reduction in medicines use, and the upper quartile for indicators promoting increased medicines use.
QuEST has also worked towards the creation of wider structures to support NTIs. One NTI focuses on the prescription of antibiotics; and this is aligned to the HEAT target focusing on reducing antibiotic prescribing.
NTIs allow prescribers, general practices, Community Health Partnerships (CHPs) and NHS Boards to compare current practice against the national position. Moving towards the agreed standard can lead to change in prescribing behaviour and ultimately improve patient care. The belief is that a national approach with shared focus on key areas will deliver the improvements in quality and efficiency required to maintain the excellent standard of healthcare in Scotland.
The report is refreshed annually with the 2014-15 version being the third edition to be published. This enables general practices to have access to the most up-to-date data available on a continuous basis.
NHS Boards are empowered to use their own approaches for local adoption of NTIs to suit local needs. NHS Boards have used a combination of methods, including incentives and action through the GP contract to drive change.
The backbone of improvement through NTIs has been QuEST's collaboration with the Scottish Prescribing Advisors Association (SPAA). The Association's improvement advisors aim to visit all Scottish General Practices at least once a year. NTIs provide a national framework based on clinical evidence which enables prescribing advisors to provide better and more consistent improvement advice.
Results
The results of the National Therapeutic Indicators project can be described as:
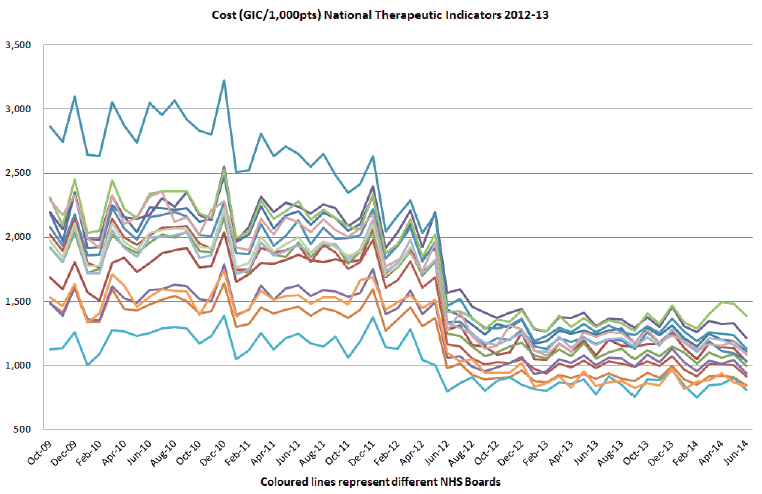
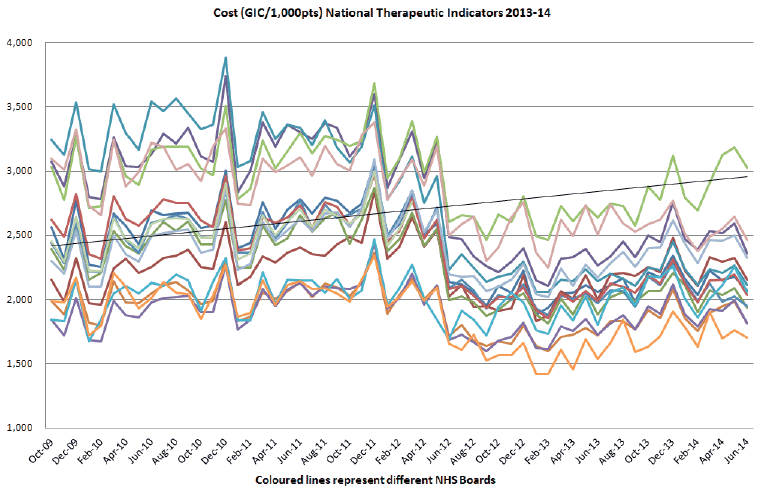
- Variation in prescribing has been reduced, as shown by the decreasing gaps between the lines representing NHS Boards on the graph below.
- Comparative cost per patient for the suite of NTI medicines reduced during 2012-13. Fewer unnecessary prescriptions are being processed; contributing to a reduced rate of prescription volume increase in Scotland.
- An increase in the number of patients moved from branded drugs, which are more expensive, to generic drugs, which are just as effective but better value for money.
- A reduction in the use of broad spectrum antibiotics has occurred. There is an associated reduction in the rate of Clostridium difficile infections.
See graph below.
Patient experience
The following patient benefits are anticipated as a result of the NTI project:
- Improved clinical outcomes
- Reduced variation between NHS Boards
- A reduction in the risk of adverse drug reactions on account of (where clinically appropriate):
- reducing dosage
- reducing the use of unsafe medicines
- discontinuing the use of inappropriate medicines
Staff experience
The following staff benefits are anticipated as a result of the NTI project:
- Staff feel more supported due to the availability of evidence-based national guidance for improving the care of patients.
- Less variation in prescribing practice enables staff to feel more confident in their day-to-day work.
- NTIs provide prescribing advisors with a consistent approach across NHSScotland.
- Prescribing advisors are not working in isolation due to improved national guidance.
Efficiency savings and productive gains
Improvements in prescribing has led to around £8 million in efficiency savings for 2013-14.
See graph below.
Sustainability
The following key activities will ensure that the benefits of the NTIs project are sustainable:
- NTIs are refreshed and reissued annually; this ensures that guidance is based on recent evidence and data at all times.
- The QuEST Prescribing Programme has now successfully transitioned to the Therapeutics Branch of Pharmacy and Medicines Division of the Scottish Government; this means that funding for the NTIs workstream is agreed until at least March 2016.
- Continued monitoring of PRISMS data - ensuring that NTIs are flexible and adjusted if required.
Lessons learned
The following lessons have been learned:
- Well-validated indicators need to be used to ensure quality is maintained; at the same time new indicators should be introduced to realise further opportunities for improvement.
- Providing NHS Boards with comparative data is a powerful tool in changing prescribing behaviour.
- Collaboration with partners and a focus on local implementation were very successful methods. Local control has facilitated ownership, which in turn led to excellent results. The NTIs project is not viewed as Scottish Government enforced but is aligned to national strategy.
- Engagement of stakeholders is key - involving prescribing advisers from all NHS Boards in the development of NTIs facilitated a feeling of ownership and helped to lend credibility to the report.
NHS Board Case Study
NHS Lothian
Polypharmacy for Patients identified at Risk using the SPARRA Tool
Background and context
In 2012 the Scottish Government released CEL 36 Appropriate Prescribing for Patients and Polypharmacy Guidance for Review of Quality, Safe and Effective Use of Long-Term Medication. NHS Lothian worked with the Scottish Government to develop a data collection spreadsheet to capture data regarding patient risk assessment scores, quantity of high-risk medication prescribed before and after medication review, numbers of medicines stopped and reduced.
In a successful pilot in Lothian (2012) medication use was reviewed in 2,616 patients living in care homes or identified as high risk by GPs and this resulted in an overall reduction in the use and dose of medicines. On average 1.0 medicines per patient were stopped.
In April 2013 NHS Lothian Efficiency and Productivity - Invest to Save funding was made available to support a further 12 month Polypharmacy project to review medication in patients identified at risk using the Scottish Patients at Risk of Readmission and Admission (SPARRA) tool.
Problem
The increase in the prevalence of chronic illnesses and an ageing population have seen a significant rise in the number of people on four or more (and often 10 or more) repeat medicines. Research has demonstrated that patients on multiple medications are more likely to suffer drug side effects which can consequently lead to hospital admission.
Aim
This project aimed to improve patient safety, provide high quality pharmaceutical care, increase awareness amongst prescribers as to the potential harm from polypharmacy prescribing and report on the financial efficiencies which had been delivered as a consequence of this quality work.
Action taken
Using the SPARRA tool 3,076 eligible patients were identified in 87 participating GP Practices across Lothian during 2013-14.
A team of clinical pharmacists undertook joint polypharmacy medication reviews with GPs who signed an SLA with NHS Lothian Primary Care Contract Organisation.
2,969 patients were reviewed between April 2013 and March 2014 and detailed analysis of a subgroup of 602 patients was completed in April 2014.
Results
A total of 6,870 medicines were reviewed in the subgroup of 602 patients from 24 GP practices and the following 1,111 interventions took place:
- 659 medicines stopped (this includes 150 high-risk medicines stopped)
- 169 medicines doses reduced
- 26 medicines doses increased
- 91 new medicines started
- 166 medicines switched e.g. to formulary choices and/or safer and more cost effective alternatives
The average number of medicines per patient before review was 11.4 and after review 10.5, a reduction of 0.9 across Lothian.
Patient experience
Patients have benefited from this approach as the average number of medicines per patient was reduced. For a number of patients the dose of medicines was reduced and a number of patients did no longer require high-risk medicines as a direct result of this work.
Staff experience
The joint review between pharmacist and prescriber raised awareness amongst prescribers as to the potential harm from polypharmacy prescribing. The feedback from GPs has been positive with many of them seeing the benefits to their patients from reducing risk of harm to reducing their "pill burden".
Efficiency savings and productive gains
The 1,111 interventions in the subgroup of 602 patients resulted in a saving of £39,049 and a cost avoidance of £16,139, representing an average saving of £64.87 and a cost avoidance of £26.81 per patient per year.
The financial efficiency and productivity gain from reduced adverse events and hospital admissions have not yet been quantified and Lothian are in discussions with the Information Services Division about further analysis which may be undertaken to evaluate impact.
The cost savings and cost avoidance achieved in this project were lower than in the pilot involving care home patients, although the number of medicines stopped were on average broadly the same.
Data analysis of the full cohort of 2,969 patients is on-going and has not been completed, however based on the initial findings of the subgroup of 602 patients it is anticipated savings of around £193,000 and a cost avoidance of around £80,000 have been achieved in 2013-2014.
Sustainability
The success of the polypharmacy medicines review and the impact on patient safety, quality of prescribing and efficiency savings has been recognised by the Efficiency and Productivity Group and GP prescribers. The CHP General Managers have agreed to a top slicing of the primary care prescribing budget for 2014-15 to continue the on-going work and a sustainable future for this work is currently being discussed.
Lessons learned
- Quality improvements and recurrent savings were achieved using the polypharmacy medicines review approach, further improvements can be achieved with continued funding for additional pharmacist hours and GP engagement.
- Strong engagement between Pharmacy nd Primary care was essential to ensure the success of this work.
- Consistent data collection and analysis was necessary to evaluate and measure the impact of the project.
- Further analysis is required to understand the variance in efficiency savings gained from reviews conducted in care home patients versus those living in the community.
Next steps
The next steps for the NTI project will be:
- Gathering more qualitative data on benefits using a QuEST template; this will draw on knowledge and expertise of SPAA.
- One challenge will be to evidence directly improved health outcomes. The project team will improve the use of available data, for example, patient-identifiable prescribing data is now available which can then be linked to clinical outcomes.
NHS Board Case Study
NHS Lothian
Promoting Quality and Cost-Effectiveness in the use of Wound Dressings
Background and context
The expenditure on wound management products has been increasing over the past years, an increase of 4.7 per cent was observed between 2011-12 and 2012-13 with silver dressings being widely used across primary and secondary care. Silver dressings are antimicrobial dressings used in the prevention of wound infection, which are more expensive than non-medicated wound dressings. The Healthcare Improvement Scotland technologies scoping report (Jan 2013) stated that there is a lack of clinical efficacy and cost-effectiveness evidence to support or refute the use of silver dressings to either prevent wound infections or completely heal wounds. The National Therapeutics Indicators (2012-13 and 2013-14) have allowed NHS Boards to benchmark their comparative use of antimicrobial dressings. Based on these findings NHS Lothian removed silver dressings from the formulary and aimed to ensure any non-formulary use of silver dressings was appropriate on the advice of a specialist in tissue viability.
Problem
Silver dressings are being used widely for many indications without adequate evidence for effectiveness. Other wound dressings that are potentially more cost-effective but provide the same quality of wound management are available.
Aim
The aim was to promote adherence with the wound dressings specified in the Lothian Joint Formulary and to reduce the use of silver dressings with the aid of a step by step guide (i.e. Ropper Lothian Ladder).
Action taken
The work taken forward in Primary Care focused on providing prescribing data to individual prescribers as well as providing education on how to effectively use the new products contained in the formulary. The aim was to promote adherence with the first and second choice dressings as specified in the Lothian Joint Formulary to ensure appropriate and cost-effective prescribing. Invest to save funding for a part-time band 6 nurse was used to support change management and maintain onward education and awareness.
The work taken forward in Secondary Care focused on engaging clinicians and service managers in a range of specialties, discussing the need for silver dressings and introducing the requirement for approval by specialist prescribers.
In addition, pharmacy staff promoted the change in the dressings on formulary. Silver dressings were withdrawn from all clinical areas as stock items and request for supplies from pharmacy should have been accompanied by a non-formulary dressing requests form.
Results
Adherence to the Lothian Joint Formulary for antimicrobial dressings has improved as a result of this work (i.e. adherence is defined as the use of formulary drugs as a percentage of all drugs in the relevant section).
The Medicines Utilisation Review Group adherence monitoring showed that between January-March 2013 adherence for antimicrobial dressings was 18 per cent in primary care; 30 per cent in secondary care; and 33 per cent in the Royal Edinburgh and associated hospitals. The reports for January-March 2013 showed an increase to 48 per cent in primary care; 72 per cent in secondary care; and 70 per cent in the Royal Edinburgh and associated hospitals.
The work in primary care and secondary care resulted in a reduction in the use of silver dressings. The exception to this was within the burns service where specialist clinicians were allowed to continue the use of silver dressings for the entire pathway journey from inpatient care to outpatient care and in the homecare setting. The decision was made after consultation with this clinical area. Preliminary discussions have been held with medical and nursing academics with a view to undertaking a study in burns around the efficacy and cost-effectiveness of silver dressings compared to alternatives.
Efficiency savings and productive gains
In primary care in 2012-13 total dressing expenditure was £3.686 million, of which £494,000 was for silver dressings. In 2013-14 around £3.72 million was spent on all dressings of which £216,000 on silver dressings. The work done in primary care has resulted in a reduction of silver dressing spend of £278,000. The overall expenditure on dressings increased.
In secondary care, the following table shows the change in expenditure on dressings between 2012-13 and 2013-14:
| 2012-13 (£k) |
2013-14 (£k) |
Change (£k) |
Change (%) |
|
|---|---|---|---|---|
| Total dressings | 1,092 | 1,078 | -14 | -1% |
| Medicated | 790 | 679 | -111 | -14% |
| Non-medicated | 302 | 393 | 91 | 30% |
| Silver | 105 | 67 | -38 | -36% |
| Honey | 14 | 21 | 7 | 50% |
| Iodine | 12 | 13 | 1 | 8% |
There was a 14 per cent decrease in the expenditure on medicated dressings and a 36 per cent decrease in the expenditure on silver dressings. However, there was a 30 per cent increase in the expenditure on non‑medicated dressings and honey dressings, and iodine dressings expenditure increased by 50 per cent and 8 per cent respectively. Therefore the work may have resulted in a shift in practice from the use of silver dressings to the use other non-medicated dressings or honey or iodine dressings. Overall the decrease in expenditure on dressings was £14,000.
In previous years an increase of around 4.7 per cent on dressings expenditure was observed, therefore the decrease of 1 per cent in 2013-14 represents a cash releasing saving of 1 per cent and a cost avoidance of around 4.7 per cent.
Sustainability
Adherence to the Lothian Joint Formulary is essential to ensure appropriate and cost-effective prescribing. Pharmacy will continue to promote adherence to the formulary. Education in relation to wound management and the use of appropriate dressings has resulted in a change in practice. There are on-going discussions to extend the band 6 nurse post to maintain education and awareness of effective prescribing in dressings.
Lessons learned
Lessons learned include:
- Engagement and clear communication with all relevant staff about upcoming changes in prescribing and the reasons for the changes is required in advance of any changes.
- The work achieved a reduction in silver dressings expenditure of £278,000 in primary care and £38,000 in secondary care. However the reduction in overall expenditure on dressings was small as expenditure on alternative dressings increased.
- Education and training with the aid of a treatment guide is an effective way of increasing the adherence to the Lothian Joint Formulary.