Annual Report 2014 - Reporting on the Quality and Efficiency Support Team
QuEST’s Annual Report 2014 provides an overview of QuEST programmes’ achievements in 2014 and upcoming priorities for 2015. The report features a wealth of case studies from Boards as well as our programmes. These case studies form a comprehensive collection of innovative quality improvement work currently undertaken in NHSScotland – driven, supported and/or resourced by QuEST. The report’s foreword is provided by Shona Robison, Cabinet Secretary for Health, Wellbeing and Sport.
Part 06: Mental Health
ABOUT THE PROGRAMME
Mental Health
Fiona McMahon
t: 0141 2420317
e: fiona.mcmahon@scotland.gsi.gov.uk
Focus on Dementia
Amanda Johnson
t: 0141 2421237
e: amanda.johnson@scotland.gsi.gov.uk
Michelle Miller
t: 0141 2425643
e: michelle.miller@scotland.gsi.gov.uk
drivers
- Timely access to healthcare is a key measure of quality and that applies equally in respect of access to mental health services. Early action is more likely to result in full recovery and in the case of children and young people will also minimise the impact on other aspects of their development such as their education, so improving their wider social development outcomes.
- Mental Health Strategy for Scotland: 2012-2015
- Scotland's National Dementia Strategy 2013-2016
aims
- Support NHS Boards to deliver a maximum waiting time of 18 weeks from referral to treatment for psychological therapies and Child and Adolescent Mental Health Services (CAMHS) by December 2014.
- Establish a National Dementia Care Improvement Programme to support services in their work to improve the care and treatment provided to individuals with dementia and their families.
workstreams
- Mental Health
- Psychological Therapies Referral to Treatment
- Child and Adolescent Mental Health Services Referral to Treatment
- Effective and Efficient Community Mental Health Services
- Dementia
- Timely Diagnosis
- Post Diagnostic Support
- 8 Pillar Post Diagnostic Support Test Sites
- 10 Key Actions in Acute Care
- Using Data to Drive Improvement (an enabling workstream supporting the two main workstreams)
achievements 2014
- The Improving Access to Psychological Therapies: Early Implementer Event was held in May 2013. The aim of this national event was to share key lessons learned from the DCAQ Early Implementer work by QuEST and NHS Lothian and to provide an opportunity for those doing similar work in NHS Boards to consider the implications for their own workstreams.
- The Improving Efficiency Without Compromising Quality Event was held in October 2013. This event, jointly hosted by NHS Education for Scotland, focused on delivering the Psychological Therapies HEAT Target.
- Finalisation of the Effective and Efficient Community Mental Health Services (CMHS) Toolkit which provides guidance on application of improvement methodologies in the CMHS setting. This reference toolkit was coproduced with NHS Boards and is available at the QI Hub website.
- Dementia Post Diagnostic Support (PDS) One Year On event was held in March 2014 and resources from that day are available on the QI Hub website.
- Delivered a series of WebExs on a variety of topics such as: planning and running activity audits, using CORE-Net and information flow mapping.
- Developed the Mental Health Data for Improvement Network running workshops on run charts and SPC charts.
- Provided ongoing support to Health Boards around Psychological Therapies, CAMHS and Dementia.
All resources are available on the QuEST Mental Health section of the QI Hub Website.
priorities 2015
- Supporting NHS Boards to deliver a maximum waiting time of 18 weeks from referral to treatment across psychological therapies and CAMHS by December 2014 through:
- enabling the use of system improvement techniques in mental health including Demand, Capacity, Activity and Queue theory
- ensuring clinical outcomes and service user experience data are routinely used to drive improvement
- developing and implementing mechanisms to monitor overall risk to delivery and highlight to the Mental Health Delivery Team Boards where risks are elevated
- developing the Mental Health Data for Improvement Network.
- Leading the development of the National Dementia Care Improvement Programme by working with a range of partners to ensure a programme of support is designed and initiated that will enable local health and social care services to:
- Ensure individuals receive a timely diagnosis
- Provide person-centred post diagnostic support to ensure future care provision is in line with the person's own wishes
- Test the 8 Pillars post diagnostic support model to Improve dementia care in acute hospitals
- Using data to effectively drive improvement - leading effective programme closure for the National Dementia Demonstrator sites, working with a range of partners including the Health Economics Research Unit (HERU), Integrated Resource Framework (IRF) Team, Information Services Division (ISD), Blake Stevenson, Joint Improvement Team (JIT) and the sites to produce both site level and national evaluation reports.
- Designing and implementing an effective spread strategy - supporting NHS Boards to release efficiency and productivity savings in mental health services whilst maintaining or improving the quality of care by developing the second edition of the Effective and Efficient Community Mental Health Services Toolkit.
- Providing performance support as required.
http://www.qihub.scot.nhs.uk/quality-and-efficiency/mental-health.aspx
Programme Case Study
Testing the "8 Pillars" Model of Community Support
Background and context
In June 2013, Scottish Government and the Convention of Scottish Local Authorities (COSLA) published Scotland's second 3-year National Dementia Strategy. A major part of implementing the strategy is supporting better community-based, integrated health and social care (including housing) support for those people whose dementia has advanced to the extent that they need intensive interventions to stay living at home for as long as possible. This will increasingly take place within the context of local partnership work to develop joint commissioning plans that seek to shift the balance of care towards community-based support, as part of service re-design to provide better integrated care and support.
Commitment 3 of the National Dementia Strategy is intended to complement this partnership activity and states that the Scottish Government will, in partnership with the Joint Improvement Team (JIT), COSLA, Scottish Social Services Council (SSSC) and Alzheimer Scotland, test and evaluate a range of approaches to providing better integrated care and support , on the basis of Alzheimer Scotland's "8 Pillars" model of community support.
This partnership approach, which forms part of the Focus on Dementia Programme, is testing this innovative, world-leading, model which focuses on improving the support and care for people with dementia and their carers.
Problem
There are currently around 80,000 people with dementia in Scotland and this number is set to double in the next 25 years. Currently around 36 per cent of people with dementia receive their care in an institutionalised setting (this can be as low as 10 per cent in other countries such as Japan).
The current model of care is not sustainable. People with moderate to severe dementia need to be supported to stay at home for as long as possible with high quality support which helps to avoid the need for hospital admission and institutionalised care.
People with dementia currently receive a minimum of one year post diagnostic support with a link worker to enable them to move to a period of self-management. However, as people with dementia deteriorate and dementia becomes more severe they are often admitted to hospital or care home due to crisis. The "8 Pillars" model provides a comprehensive, integrated, coordinated approach to support people with dementia and their families and carers. By tackling a full range of factors that influence the experience of the illness in a coordinated way, this work takes a therapeutic approach to enhancing the resilience of people with dementia and their families and carers; equipping and supporting them to cope with the symptoms of the moderate to severe stages of the illness.
Aim
The aim of the Focus on Dementia Programme is to improve experience, safety and coordination of care for people with dementia, their carers and staff by January 2016, through testing and evaluating a range of approaches to providing better integrated care and support in the community using the "8 Pillars" Model.
The Programme will:
- Test different models and approaches to delivering the key role of the Dementia Practice Coordinator within the "8 Pillars" model
- Assess the costs and benefits of implementing the "8 Pillars" model including the Dementia Practice Coordinator role.
- Better understand which groups of individuals might benefit from a Dementia Practice Co-ordinator and demonstrate those benefits in practice in test sites
- Assess the helpfulness of the other seven pillars in directing the development of integrated care and support and, where appropriate, develop a better understanding of the distribution of need/ demand across each of the pillars
- Engage wider community planning partners in testing how their services can contribute to the other seven pillars through responding better to the needs of people with dementia.
The output of the programme will be used to inform the Dementia Strategy for 2016.
Action taken
The Focus on Dementia Programme has established a series of learning sessions, WebEx calls, peer support and improvement expertise:
- An introductory event was held in January 2014, to enable test site teams to meet each other and to learn from other related dementia workstreams, including dementia demonstrator sites and post diagnostic support test sites.
- A Knowledge and Skills Needs Analysis has been carried out to identify individual requirements in order to design effective support for individuals and teams.
- To date, four out of eight planned national learning sessions have been held (each learning session focuses on one of the pillars). Learning sessions have been supported by WebEx calls to ensure continuous engagement and shared learning.
- A 'Managing Qualitative Data' session was held in September 2014 to build capacity and capability in this area.
- Test site visits, telephone support calls and tailored educational sessions have been made available to support test sites. In addition, JIT Associates also provide 'critical friend' support to the test sites and attend and contribute to local steering groups.
- Existing change package material including the Post Diagnostic Services test sites toolkit is available for test site teams to use and adapt to fit with their local context.
- Funding for improvement capacity locally has been made available to test sites.
- External evaluation is currently being commissioned to work closely with the test sites to support the evaluation of the different models.
- A measurement framework, change package and qualitative data framework has been developed and test sites are beginning to gather both quantitative and qualitative data from people with dementia, carers and staff.
Results
- Each of the five test sites have identified a Dementia Practice Coordinator who will ensure access to the other seven pillars of support on an on-going basis as appropriate to each individual, and will coordinate between all the practitioners delivering care, treatment and support.
- Each of the five test sites have submitted flash reports and driver diagrams to share learning, progress, highlights and challenges.
- Data collection to provide evidence of improvement has commenced at each of the five test sites.
- Evaluations from the learning sessions held to date demonstrate an increase in knowledge and understanding of the pillars within the "8 pillars" model, and improved knowledge and understanding of improvement methodologies. Delegates have valued the opportunity to share learning with the other test sites.
- As a result of attending Learning Session 3, on average 89% participants believe their knowledge and understanding of a variety of therapeutic interventions had improved.
- As a result of attending the Managing Qualitative Data session, 100% of participants believe their understanding of how to analyse and report on personal outcomes data had improved. Participants also reported increased confidence in their ability to do this.
- The following qualitative feedback has also been received:
- "Thanks for the opportunity to attend a really interesting day - I will use the learning in many areas of my work."
- "Good day, time well spent."
- "All really positive, energising and uplifting."
- "Good wide ranging exploration of the variety of specific interventions, encouraging open mindedness in this respect."
Person with dementia/carer experience
Whilst it is too early in the programme to have evidence of improved outcomes, improvements are anticipated in the following areas:
- Improved experience - both people with dementia and their carers should have increased satisfaction with the service received. What is important to the person with dementia is central to their personalised plan. Carers feel supported in their role.
- Improved safety - crises should be averted and/or managed leading to reduced emergency call-outs, reduced A&E attendance and reduced emergency admissions. People with dementia and their carers feel safe.
- Improved coordination - People with dementia and their carers have access to the right support at the right time. It should be easier to access multiagency interventions (with fewer steps required to access support). The experience of working across a range of professions and services should be improved, with effective partnership working arrangements, processes and shared responsibility. People with dementia and their carers feel responded to.
Staff experience
Whilst it is too early in the programme to have evidence of improved outcomes, improvements are anticipated in the following areas:
- Improved experience - staff should have the necessary skills and support in order to deliver the highest quality care.
Efficiency savings and productive gains
Whilst it is too early in the programme to have evidence improved efficiency, benefits are anticipated in the following areas:
- Through averting/managing crises there should be a reduction in emergency call-outs, A&E attendances and emergency admissions. As such time should be released that can be used to deliver care elsewhere.
- There should also be a reduction in the number of preventable GP contacts (it is noted that people with dementia may have multiple comorbidities which necessitate frequent GP attendance which is unavoidable).
- By shifting the balance of care into the community, ensuring that people with dementia can stay at home for longer, the number of care home admissions should also be reduced.
Sustainability
The programme will test the model until 2016 when a recommendation will be made about whether it should be rolled out across Scotland or modified to ensure spread and sustainability.
Lessons learned
- Partnership working has been key to the success of the Programme to date. Working with people with dementia, carers, staff and key agencies (JIT, COSLA, SSSC and Alzheimer Scotland) has enabled relationships to be built and has provided a richness to the work.
- Evaluation planning should be undertaken from the start of a programme to ensure this is embedded in the programme from an early stage.
Next steps
- Learning session five focused on the General Care Health and Treatment pillar will be held in February 2015
- Test sites will continue to gather and report data
- An interim report on the work will be published in May 2015
NHS Board Case Study
NHS Dumfries and Galloway
Outcome Measures and Qlikview Connection
Background and context
Previously very little outcome measure data was collected. It was essential to collect data on the efficiency and effectiveness of clinicians.
Problem
Engaging staff to collect data and complete "even more paperwork" was the main challenge. It was crucial to be able to produce meaningful data quickly to prove the benefit of the data. Being funded to employ an assistant psychologist dedicated to this project allowed sufficient planning, training and support during the initial set up. This assistant is reporting manually to clinicians until the Qlikview data is 'live'. He is training staff, both psychologists and other teams, i.e. occupational therapists, inpatient and community nurses. These teams are starting to collect data in a comparative fashion. This assists in the development of other DCAQ work.
Aim
To demonstrate the effectiveness of the psychological intervention to all stakeholders, as well as utilise data for reflective practice, management purposes and service planning, and professional development. To monitor the service aim that the throughput of the department is efficient as well as effective.
Action taken
Data has been collected for one year now. (Not all the data has been entered yet due to the previous assistant being accepted on a course and delay in recruiting to the vacancy).
Work has been undertaken with IT to enable the creation of the data via Qlikview which in the longer term will save on analysis time.
We are just about at the stage where we can use the data:
- for reflective practice via individual reports
- for governance purposes related to the quality of service provided
- to consider development needs of clinicians
- to highlight areas for service development
- to inform the targeting of resources to enhance quality.
Results
Staff have been impressed by the amount of data we can now easily report on.
The next stage is to develop routine individual and aggregate service reports and organise access for managers and clinicians to live data which can inform development review, individual reflective practice and highlight service quality issues requiring strategic planning.
Efficiency savings and productive gains
The next stage will be to review efficiency and productivity gains such as identifying where we are most effective and to shape working practices as well as guiding individual and service development plans. Qlikview reporting will streamline this process, allowing for live data and a growing evidence base.
Sustainability
Sustainability is an issue as in the longer term we will not have funding for an assistant psychologist.
Qlikview will help towards the sustainability of the data analysis.
We are just about to pilot electronic data entry by clinicians of one small team. If this is successful, it would remove the longer term need to have someone manually entering data.
Lessons learned
- Having an assistant psychologist dedicated to implementing the project has been a key factor in the success so far.
- Data entry has been more time consuming than anticipated.
- It was essential to have a structured programme of training for clinicians to ensure engagement of those completing the data collection.
- Having an assistant psychologist to scrutinise the data for anomalies/errors close to the time of clinician data recording on paper is crucial, since missing data can easily be retrieved from currently open files.
- Value of Qlikview for timely reports for efficiency/quality monitoring.
- Potential for usefulness of data produced to:
- Identify training needs
- Focus on areas most efficient - identify where not so efficient and work out why
- Look at outcomes with clients from particular referring agents and action feedback to them if there are referrer-specific patterns. Also value for informing wider service training needs, outcome patterns per type of problem, clinician training needs.
- In relation to the HEAT target, potential to understand pattern of resources needed to achieve certain outcomes with certain problems (e.g. look at patterns in numbers of sessions offered using different models for same problem - would any more resource be more efficienct than others?)
NHS Board Case Study
NHS Greater Glasgow and Clyde
Achieving and Sustaining CAMHS Referral To Treatment HEAT Targets
Background and context
NHS Greater Glasgow and Clyde (GG&C) Specialist Children's Services established a programme of work to deliver the 26 Week Referral To Treatment Target for access to Child and Adolescent Mental Health Services (CAMHS) by March 2013 and the future target of 18 weeks by December 2014.
The programme was designed to deliver improvement in the waiting times for CAMHS services at Tier 3 as well as improving the patient journey and service provided to ensure consistency across NHS GG&C CAMHS teams.
Problem
In order to achieve the RTT targets within current resources, and faced with excessive waiting times as part of the work to redesign and develop the NHS GG&C CAMHS Service Framework, a number of key areas have been identified for improvement:
- Gaining a better understanding of our demand and capacity within teams and the projected capacity within our new CAMHS workforce model by introducing Lean methodology.
- Improving service efficiency, by improving our referral and administrative processes within teams.
- Reducing the inequalities in access, structure and quality of service delivery and reducing the variations in workforce and practice across NHS GG&C CAMHS teams.
- Delivering quality outcomes as defined by children and families.
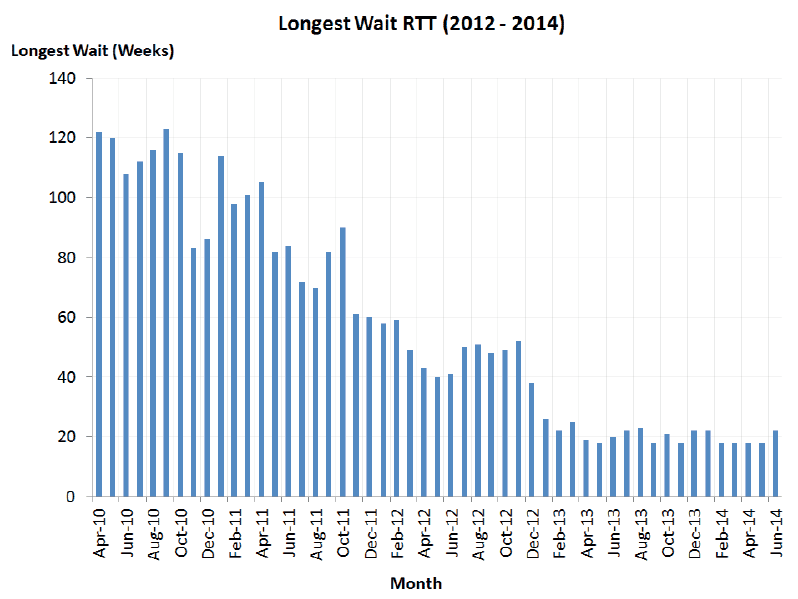
Historically NHS GG&C CAMHS had significantly long waiting times from referral to treatment. The graph below demonstrates the problems which were faced in 2010 and 2011. In April 2010, the longest wait for RTT was 123 weeks and this figure remained extremely high until nearer 2012.
Please refer to the graph below.
As shown, the data has been improving since 2010 and this will be focused on later in this case study.
Aim
To achieve sustained improvements to access CAMHS for children and young people consistently across NHS GG&C, whilst achieving Referral to Treatment Heat Targets.
Action taken
Within the programme of work and redesign of the NHS GG&C CAMHS Service Framework, key overarching workstreams have been identified as being central to the achievement of the RTT targets and the development of the areas indicated as problems:
- Implementation of CAPA (Choice and Partnership Approach) as our Lean Methodology for managing demand and capacity in all NHS GG&C CAMHS teams.
- Established robust information and data collection systems within teams and performance reporting and monitoring purposes consistent across NHS GG&C.
- Establishing CORC (CAMHS Outcomes Research Consortium) as our Clinical Outcomes Measurement Tool.
- Reviewed our business processes and administration support.
- Development of the above processes as part of a single patient management system (EMIS Web project requirements).
Results
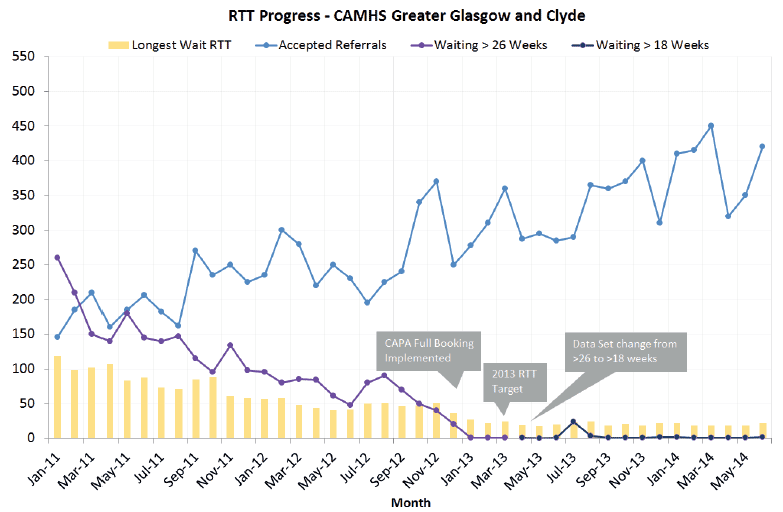
Over the past three years, we have seen dramatic improvements as a result of the above work. For instance, in January 2011, the longest RTT wait was 113 weeks. This figure has been reduced to below 26 weeks by March 2013 target and continues to decrease toward the 18 weeks target in December 2014. The graph below demonstrates this.
In the graph, there is a noticeable decrease in waiting times and numbers waiting over 26 and 18 weeks. However, the increased accepted referral trend stands out.
It is clear that the data produced from this work demonstrates excellent results, allowing CAMHS to accept a larger demand, whilst drastically improving access to service.
Efficiency savings and productive gains
Throughout the time period shown in the data, there has been no increase in resource to NHS GG&C CAMHS. Efficiencies have been realised through the use of CAPA and the informatics which accompany this model.
Looking at the accepted referral statistics, there has been a 223 per cent increase in accepted referrals since January 2011 to its peak in March 2014. Analysis shows that this increase is not necessarily due to re-referrals as our re-referral rate is currently at 21 per cent which is standard to NHS England CAMHS and CAMHS in Ireland and Australia.
It is likely that this increase is due to various reasons. For instance, it is clear from analysis that there has been an increase in referrals sources as professionals become more aware of the service. Coupled with the third party organisations decrease in activity and funding, CAMHS have seen an unprecedented increase in demand.
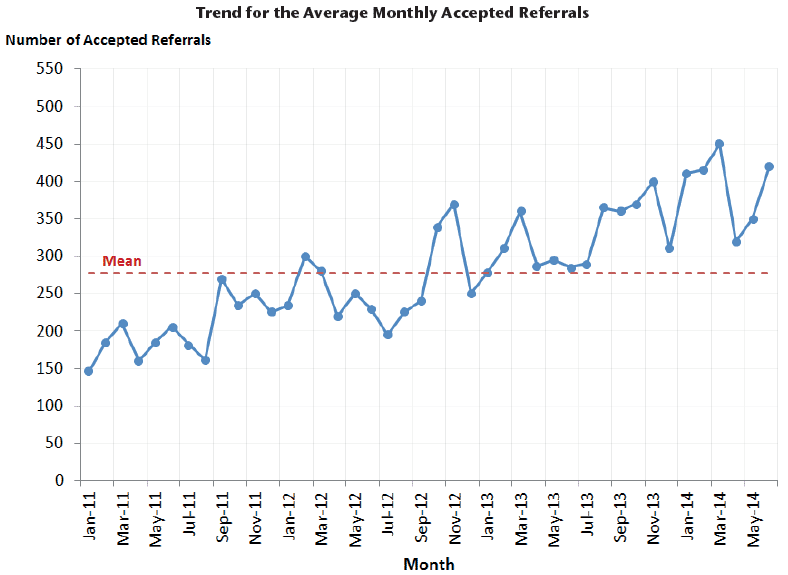
The graph below demonstrates the trend against the average monthly accepted referrals. There is a clear positive trend overall and we can see some prolonged bias in the most recent 17 months of data.
The data highlights that the workforce is now operating much more efficiently than it has done before with no extra resource. This data will continue to be monitored, and further efficiencies will be sought with assistance from the current data and future analysis.
Sustainability
The programmes of work are intrinsically linked and the benefits of achieving these will ensure the following:
- Ensure we continue to meet the 18 week CAMHS RTT target
- Support full implementation of CORC across NHS GG&C CAMHS
- Ensure the quality of data for performance and reporting for HEAT targets and internal performance and monitoring purposes
- Continuous service improvement through robust performance and monitoring, and improved access to services and quality of care for children and young people and their families
- Streamlined business process for CAMHS
- On-going implementation/training of EMIS Web Patient Management System across CAMHS
Lessons learned
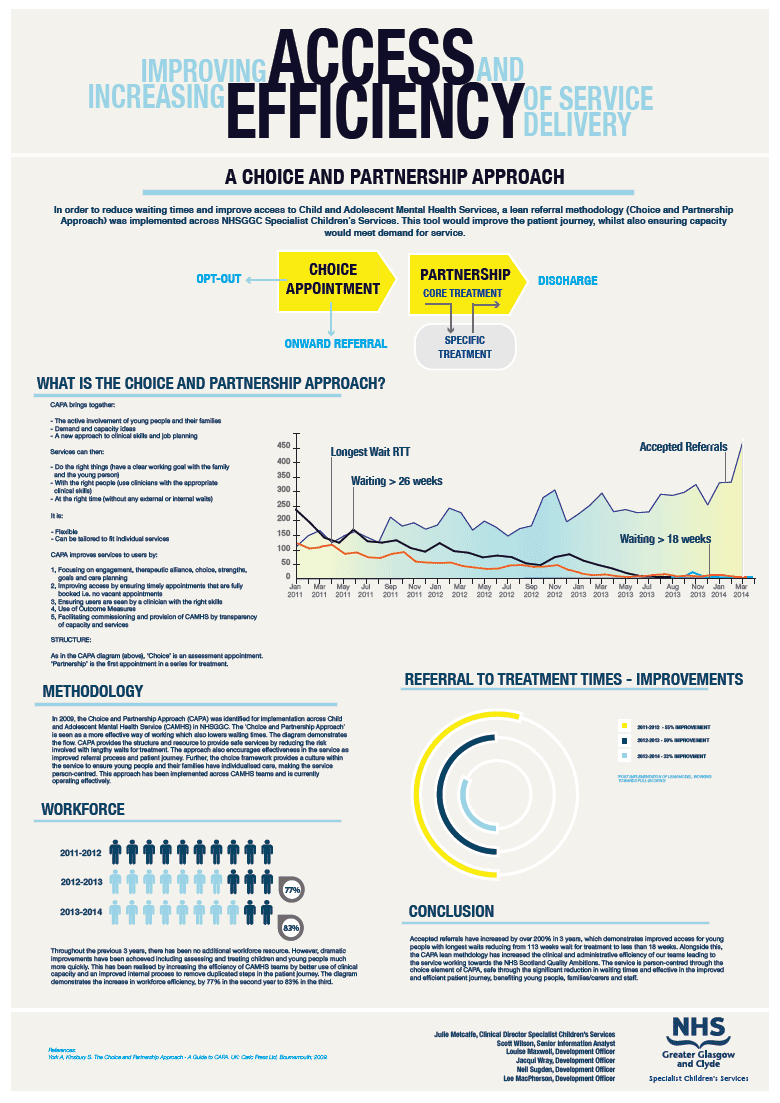
One of the main lessons learned is to increase the awareness of the success in CAMHS. In June, we submitted a poster presentation to the NHSScotland Event with details of the methodology and data analysis used to improve CAMHS waiting times. This poster won 1st place in the Effective category and an award was presented to CAMHS and SCS Management by the Cabinet Secretary for Health and Wellbeing.
A copy of the poster is shown below.
Programme Case Study
NHS Highland
Improved Access to the Community Mental Health Team in Mid-Argyll
Background and context
The Community Mental Health Team (CMHT) in Mid-Argyll had a total of 109 clients being seen within the service in 2013. There were a further 23 clients waiting for their first appointment with the service - with the average wait being 34 weeks - and the longest wait being 58 weeks.
Problem
The CMHT is a small team comprising a core of five members supported by other specialists looking after clients from the geographic area of Mid-Argyll. There was variation in referrals into the service, and variation in the methods used to process referrals once received.
Case load triage on referral was via a single point, with 1st and 2nd stage triage being a completely manual process.
Clients were allocated in accordance with need, priority, specialty and available capacity (gender preference also a consideration).
There was variation in capacity of specialist team members to accommodate Mid Argyll referrals, due to their commitments in Kintyre and Islay.
Clients placed onto the waiting list were not offered an appointment until an existing client was discharged from a team member's case load (if at capacity). There was variation in waiting time for first appointment.
Aim
To decrease the lead time from a client being referred into the service to the date of first appointment.
Action taken
We used a Lean Rapid Process Improvement Workshop (RPIW). This had a twelve week preparation phase, in which the scope of the work was agreed, and observations were conducted. Staff identified waste and completed ideas forms. A value stream map was produced and percentage load charts developed. In the RPIW week, staff from the service reviewed the service flows, and their ideas forms. They developed new ways of working including streamlining the current referral and triage process, and also undertaking 5S on equipment and rooms. Standard work was developed by the team and incorporated into an RPIW newspaper (action plan) which was supported by a series of standard process descriptions and a skills matrix (to support training and development requirements).
A visual display board was used to monitor progress of clients through the service, and the use of WebEx conferencing allowed team review sessions (weekly) to be joined by team members working from the Kintyre and Islay areas.
The referral and single stage triage process are now completely electronic.
Results
The average wait in the service was 34 weeks at the baseline measurement. Following the RPIW, the average wait slowly decreased to an average figure of 20 weeks at 90D.
However, at 365D the longest wait for first appointment is:
- Tier 1 - 2 weeks
- Tier 2 - 11 weeks
- Tier 3 / 4 - 7 weeks
Patient experience
Clients are experiencing improvements in access to the service, which is benefiting from a team approach to their well-being.
Staff experience
Some team members were apprehensive about the RPIW at the outset. The team excelled in the process, and have 'shared and spread' their work to other parts of Mid-Argyll.
Efficiency savings
and productive gains
No additional staff were required, although at the outset there was a belief that a further CPN would be needed to manage the caseload.
Waiting times have decreased from an average of 34 weeks to figures quoted in the Results section.
Sustainability
- A sweep system was introduced for 5S.
- A visual control board was developed to allow staff to see their service status quickly.
- All staff now use electronic diaries, and all referrals are made into the service via SCI gateway.
- Staff are following Standard Work and effectively 'Sharing and Spreading' their success to other areas within Mid-Argyll.
Lessons learned
The RPIW process, using Lean principles, was effective. There were implementation challenges related to staff concerns, and our main lesson was that service staff are the key agents of change, and need to be supported as much as possible. This demonstrated that understanding the boundaries of a process is important, and that changes outside the scope of the original work can take longer.