Annual Report 2014 - Reporting on the Quality and Efficiency Support Team
QuEST’s Annual Report 2014 provides an overview of QuEST programmes’ achievements in 2014 and upcoming priorities for 2015. The report features a wealth of case studies from Boards as well as our programmes. These case studies form a comprehensive collection of innovative quality improvement work currently undertaken in NHSScotland – driven, supported and/or resourced by QuEST. The report’s foreword is provided by Shona Robison, Cabinet Secretary for Health, Wellbeing and Sport.
Part 04: Whole System Patient Flow
ABOUT THE PROGRAMME
Martin Hopkins
t: 0131 244 5178
e: martin.hopkins@scotland.gsi.gov.uk
drivers
Designing care systems with effective patient flow is critical to the delivery of NHSScotland's Quality Ambitions of safe, person-centred and effective health care.
Poor patient flow means reduced quality which may result in patients:
- waiting for treatment
- possibly not receiving as effective care or perhaps waiting longer
- not receiving all the care they need
- being delayed once their treatment is completed
Good patient flow supports optimal care for patients' needs and contributes to safe, person-centred and effective care. It also eliminates or reduces inefficiencies.
aims
- Adopt a whole systems approach to patient flow, designed to ensure patients receive the right care, at the right time, in the right place, by the right team
- Promote the bringing together of both elective and unscheduled workstreams to support a whole system approach
- Test new and innovative approaches to improving patient flow
- Reduce artificial variation in health care
- Develop a culture of sharing and continuous improvement across NHSScotland
workstreams
- Proof of Concept - testing new and innovative approaches to improving patient flow
- Day and Short Stay Surgery
- Enhanced Recovery
- Fracture Clinic Redesign
- Criteria Led Discharge (established in 2014-15)
- Hospital Huddles (established in 2014-15)
As well as focusing on the above workstreams the programme aims to support NHS Boards to have effective infrastructure is in place to enable:
- Frontline administrative, clinical and managerial staff to optimise the management of pathways and queues on a day to day basis, further embedding monitoring and management tools and real time pathway management reports
- The development of an embedded approach to Demand, Capacity, Activity, Queue (DCAQ) analysis and the operational application of it
- The use of prediction tools to plan emergency capacity and real time demand and capacity management techniques
- To further build a system across acute sites to assess the balance of resources across both emergency and elective care with a view to maintaining effective flow both at strategic and operational level
achievements 2014
- Proof of concept - procurement of a technical partner to test an innovative approach to improving patient flow. Our technical partner is the Institute for Healthcare Optimisation (IHO). The work has commenced in NHS Forth Valley, NHS Borders, NHS Greater Glasgow and Clyde and NHS Tayside. The basic principles of the model are the application of queuing theory, separation of flows (unscheduled and scheduled), and the use of variability methodology.
Delivery of two national events focused on patient flow, engaging staff from across NHSScotland:
- The first event focused on exploring the relationships and interdependencies between flow, patient safety and our Quality Ambitions and showcased best practice in improving patient flow.
- The second event, held jointly with the Royal College of Physicians of Edinburgh (RCPE) reached a consensus on how to reduce unnecessary bed moves for patients and improve patient flow, so as to ensure that there is sufficient capacity in hospitals and the community for patients' needs including in times of winter pressure.
- The Fracture Redesign Model originating in NHS Greater Glasgow and Clyde has further spread across Scotland and England, and has been recognised internationally. Support for NHS Boards in implementation and spread continues.
- Development of a set of measures to enable measurement for improvement in respect of Enhanced Recovery. Regular reporting to commence in 2014-15 to aid spread and sustainability.
priorities 2015
Taking a whole system approach to patient flow will influence how healthcare is delivered in all areas. It is recognised that there is a great deal of work being progressed both locally and nationally that has a bearing on patient flow. Those within the pyramid are specifically related to the Whole System Patient Flow Improvement Programme and its priority areas.
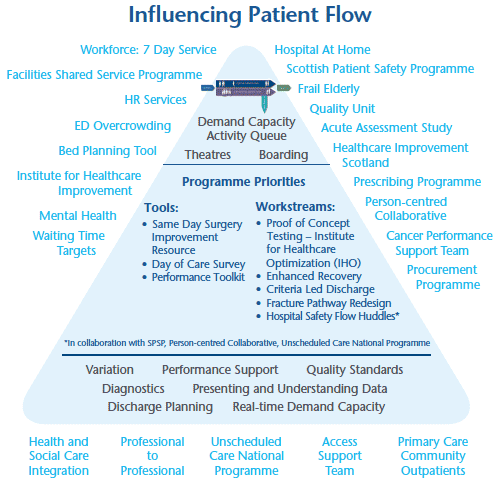
http://www.qihub.scot.nhs.uk/quality-and-efficiency/whole-systems-patient-flow.aspx
Programme Case Study
Enhanced Recovery After Surgery
Background and context
Enhanced Recovery after Surgery (ERAS) is an evidence-based approach that helps patients to recover more quickly after surgery. It focuses on ensuring that patients are active participants in their recovery process, and it is important that all staff have knowledge of the evidence supporting Enhanced Recovery so that their relationship with the patient is built on mutual trust and respect.
The underlying principle behind Enhanced Recovery is to minimise the physical and mental stresses the patient goes through, so that they can recover more quickly, have a reduced stay in hospital, and are able to return to normal activities earlier. The pathway starts in primary care, moves through pre-operative, admission, operative and post-operative stages, and ends with the follow-up stage.
Enhanced Recovery involves a number of evidence-based interventions which individually have been shown to be beneficial, however when used together in a protocol they have been shown to result in substantially improved outcomes.
Enhanced Recovery is the sum of marginal improvements - if 1 per cent improvements are made in all areas, this adds up to make a significant improvement for patients and their carers.
Problem
Enhanced Recovery has been delivered in the UK since the early 2000s. In early 2012 a baselining exercise was undertaken by QuEST (formerly Improvement Support Team) to establish the position for Scotland. It was identified that, while Enhanced Recovery was being carried out in some areas, this was not standard practice or consistent between or within NHS Boards.
Through establishing the Enhanced Recovery Programme (now part of the Whole System Patient Flow Improvement Programme), QuEST provided an overarching structure and national coordination for the implementation and spread of Enhanced Recovery.
Aim
QuEST aims to support NHS Boards to achieve a reduction in variation in the delivery of Enhanced Recovery principles across NHS Scotland, ensuring reliable implementation and spread to improve quality of care and patient and carer experience.
The Enhanced Recovery programme aims to:
- Bring together the best practice in organisation of care and clinical management, so that patients receive evidence-based care use patients and families as a resource in planning and managing the patient's recovery and care
- Focus on less invasive surgical techniques, optimised pain relief and management of fluids and diet, in order to mobilise patients more quickly post-operatively
- Make the patient's time in hospital as normal as possible
- Promote a wellness, rather than an illness, model of care.
Action taken
In order to achieve the aim of reduced variation and reliable implementation and spread of Enhanced Recovery principles QuEST has supported NHS Boards by:
- Providing one-to-one Service Improvement Manager support to Enhanced Recovery Coordinators within NHS Boards.
- Establishing an Enhanced Recovery Forum for NHS Boards Enhanced Recovery Coordinators and Analysts to come together to share best practice, successes and challenges, in addition to shaping the future requirements for support from QuEST.
- Establishing an online Enhanced Recovery Network to support individuals leading/ working on local programmes of work and to encourage the sharing of best practice across NHSScotland.
- Developing an National Enhanced Recovery Data Analysis Toolkit which provides NHS Boards with a national dataset of up- to-date information for improvement. This information allows NHS Boards to identify where the opportunities for improvement exist (through highlighting of variation) and identifies areas of best practice.
- Developing a LearnPro eLearning module (in partnership with NHS Boards) to raise awareness of Enhanced Recovery principles and ways of working across all staff groups.
- This eLearning module underwent user testing in various NHS Boards during August 2014.
Providing financial support to enable NHS Boards to:
- establish an infrastructure, across the organisation, to coordinate improvement activities in this area
- secure clinical champions to lead and support this work across the organisation and within priority specialities
- embed data collection processes to ensure the agreed bundle of improvement measures are consistently collected
- embed Enhanced Recovery into the core clinical service delivery
Results
To date there has been a lack of robust data which describes the level of Enhanced Recovery implementation across Scotland.
QuEST has developed a National Enhanced Recovery Data Analysis Toolkit which contains clinical data elements submitted by NHS Boards. This is the first time that Enhanced Recovery clinical data has been available for this number of specialties across NHS Boards in the UK. We are now moving towards being able to demonstrate evidence-based care for all elective admissions.
Collating a national dataset of information for improvement allows NHS Boards to understand where the opportunities for improvement exist. The use of real-time clinical data enables an understanding of how systems are currently delivering services and the level of variation that exists. As a result, systems will be able to continuously monitor and improve services when redesigning care pathways and thereafter measure the impact of these changes.
QuEST will engage with NHS Boards to identify variation in compliance with Enhanced Recovery principles and to support NHS Boards to develop:
- plans to tackle challenges in further roll out
- a plan for spread and reliable implementation and ensure sustainability
Patient experience
Enhanced Recovery provides a way of managing care and rehabilitation that improves patient outcomes and speeds up a patient's recovery after surgery, enabling them to return to normal activities more quickly.
There are a number of benefits to patients which align to our Quality Ambitions:
- Person-centred - patients and carers are active partners in their own care and recovery process. Patients are more informed and have more choice about the management of their care which improves their experience and clinical outcomes.
- Safe - patients on an Enhanced Recover pathway have fewer complications and readmissions. Patients have a reduced length of stay which improves patient safety from reduced risk of hospital associated infections.
- Effective - patients receive improved pre-operative care, reduction in the physical stress of the operation and increased comfort post-operatively. In addition, Enhanced Recovery can aid early detection of complications and additional care interventions can be given earlier if required (e.g. chemotherapy, radiotherapy).
Staff experience
There are a number of benefits to staff working with Enhanced Recovery pathways, including:
- improved multidisciplinary experience
- team building opportunities
- education and training opportunities
- improved focus on use of technology
- recognition for achieving improvements in quality and patient experience
Efficiency savings and productive gains
Implementation of Enhanced Recovery has the potential to deliver significant productive gains through reduced length of stay and bed days saved, including:
- potential to treat more patients within same resources
- increased bed capacity for hospitals to support optimum patient flow
Enhanced Recovery also provides the opportunity to harmonise care across the NHS to support optimum patient pathways and to assist NHS Boards in meeting operational performance standards (e.g. 18 Weeks and Treatment Time Guarantee).
Sustainability
QuEST has supported NHS Boards to develop an infrastructure to ensure that Enhanced Recovery is the default approach to managing care before and after surgery. The new ways of working are being embedded within NHS Boards and QuEST continues to support implementation and spread.
Lessons learned
Key lessons learned include:
- It is critical that NHS Boards have dedicated resource to 'pump prime' the move to Enhanced Recovery and embed the new ways of working
- The establishment of networks to support individuals delivering Enhanced Recovery in NHS Boards is important for sharing best practice and addressing challenges
- Communicating opportunities within NHS Boards is vital - for example ensuring staff are aware of training opportunities such as the LearnPro eLearning module
- Providing networking opportunities is key to support cross NHS Board working
Next steps
Good progress has been made in NHS Boards in colorectal, urology, gynaecology, orthopaedics and breast surgery and the next stage is to test and spread the approach to other specialties.
Next steps for the QuEST national team include:
- Supporting an Enhanced Recovery pilot in obstetrics for planned caesarean section procedures
- Providing on-going support for the National Enhanced Recovery Data Analysis Toolkit
- Launching the newly developed LearnPro eLearning module to raise awareness of NHS staff of Enhanced Recovery principles
- Contributing to a national Whole System Patient Flow event in October 2014 through delivery of Enhanced Recovery workshops
- Continue to engage with local teams and understand further opportunities for spread to other specialties and support as appropriate.
NHS Board Case Study
NHS Borders
Improving the Emergency Access Standard
Background and context
Since September 2013 the national Emergency Access Standard (EAS) has stipulated that 95 per cent of all patients presenting to UK Emergency Departments (EDs) should be seen, treated and admitted or discharged within four hours.
Problem
It is extremely challenging to achieve the Emergency Access Standard consistently.
Aim
This study aimed to address the on-going problem of Emergency Access Standard breaches at a district general hospital.
Action taken
Senior managers and senior clinicians met weekly for fifteen minutes in the ED. Using improvement methodology, tests of change were devised to address recurring causes for breaches in each patient flow group:
- flow 1 - minor injuries
- flow 2 - acute illness
- flow 3 - medical admissions
- flow 4 - surgical admissions
Each test of change was implemented on a plan-do-study-act (PDSA) basis and data was displayed on statistical process control charts. Data interrogation identified recurring reasons for breaches and specific PDSAs were devised to address these. The impact of each PDSA was then analysed, discussed and refined at the weekly meetings.
Results
Over an eight-month period (July 2013 - February 2014) initial testing focused on flow groups 1, 2 and 3 which in turn all demonstrated reduced variation in performance evinced as a significant reduction in patient waits. The greatest impact was on breaches in flow 1 which were reduced from 1.31 per cent (July 2012 - February 2013) to 0.5% (July 2013 - February 2014). Over the study period the Borders General Hospital averaged 98 per cent on the Emergency Access Standard whereas for the same period in 2012-2013 performance averaged 96 per cent.
Patient experience
NHS Borders is now consistently meeting the Emergency Access Standard. 98 per cent of patients are seen, treated and admitted or discharged within 4 hours, thereby improving the patient experience at the 'front door' of the hospital.
Staff experience
Staff have gained a greater understanding of why breaches occur and have the confidence to employ PDSA cycles to address any future issues. Up to date performance data is visually displayed in the department which helps engage staff and ensures a focus on quality.
Efficiency savings and productive gains
NHS Borders has consistently achieved and exceeded the Emergency Access Standard averaging 98 per cent over the study period. This was achieved within existing resources.
Sustainability
The weekly 15 minute 'Alpha Zone' meeting is now thoroughly embedded in the department ensuring on-going scrutiny of the performance data and providing a forum to introduce further PDSA cycles as necessary.
Lessons learned
This study has shown that the application of improvement methodology, using PDSA iterative cycles, and a patient safety approach, can address special cause variation in patient waits in a district general hospital. Furthermore, a joint working partnership between clinicians and managers allowed PDSAs to be implemented and spread across the wider hospital community. The authors would recommend that a similar team-based, patient safety approach be adopted in other NHS Boards.
NHS Board Case Study
NHS Dumfries and Galloway
Pilot of a Surgical Assessment Unit
Background and context
NHS Dumfries and Galloway was struggling to achieve the interim four hour waiting times target (95 per cent) within the emergency department at Dumfries and Galloway Royal Infirmary (DGRI).
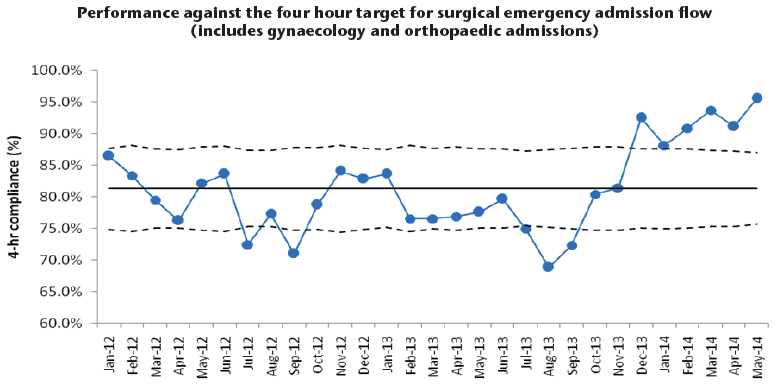
The opening of the Acute Medicine Unit with access to assessment beds had improved the medical flow of patients providing better experience for the patient and improved performance against the target for this flow. However, traditionally Flow 4 - the surgical admissions flow - was the lowest performing flow for the four hour emergency access target (appendix 1). This performance led to slow assessment and poorer care of patients. As such the Board agreed to the trial of a Surgical Assessment Unit (SAU).
Problem
Traditionally all surgical patients referred for emergency admission by GPs, or assessed as requiring emergency admission by the emergency department, were managed within the emergency department.
The assessment of the patient followed a very traditional pattern with the junior undertaking an initial clerk-in followed by a hierarchy of assessment. This assessment could be delayed because the senior medical staff were in theatre or otherwise busy within the ward.
Aim
NHS Dumfries and Galloway was keen to deliver high quality assessment, treatment and diagnosis for all acutely ill surgical patients with prompt access to decision maker followed by rapid initiation of treatment and investigations and either admission or discharge as appropriate. It was anticipated that the introduction of a Surgical Assessment Unit would support these goals and improve performance against the four hour target.
Action taken
A five bed area (one single and one four bedded room) was identified within one of the general surgical wards to support development of a Surgical Assessment Unit.
The surgical assessment area was provided with dedicated nursing staff, being sited within the ward area itself provided improved access to medical staff within the ward.
The unit was opened on 2 December 2013 although initially (until 6 January 2014), due to recruitment difficulties, was only open between 8am and 8pm. The unit is now fully functioning and is open 24 hours per day, seven days per week and receives adult surgical emergency admissions with the exception of orthopaedic and gynaecology presentations.
The surgical admissions flow was redesigned so that GP referred patients received a quick initial assessment in the emergency department before going on to be formally assessed in SAU. The self-presentations or 999 ambulance patients are assessed in the emergency department before being referred on to the unit. The unit was provided with dedicated nursing input, FY1 and middle grade cover, access to a range of diagnostic tests and a single room where treatments could be carried out.
The unit has functioned well since opening.
Results
Impact on the Emergency Department
The SAU has undoubtedly had a beneficial impact on the emergency department. Firstly, since opening there has been a step change improvement in our emergency department four hour performance (appendix 1). This has gone from achieving around 70 per cent to 90 per cent performance, including one week where we reached 98 per cent. Secondly, the length of time our patients are spending in the emergency department has reduced dramatically (appendix 2). Finally, the emergency department staff have found that the unit helps to improve their working as the surgical patients move from the unit much faster.
Impact on General Surgery
The General Surgery staff are finding the unit beneficial as the patients are easier to manage once in the SAU. In addition, the patients are being looked after by trained surgical nurses rather than emergency department staff who are working with a range of patients.
Performance of SAU
The SAU is showing strong performance against its original measures. We are currently using a manual input for data collection the information which suggests that 21 per cent of patients are being discharged directly from the SAU. Work is currently underway with information services to capture this data using existing systems.
Efficiency savings and productive gains
As already outlined the aim of this pilot was to improve the quality of patient journey for the surgical flow of patient. This also forms a key component of the of our improvement towards the four hour emergency department waiting times target and early steps towards the development of our combined assessment area in the new District General Hospital. No cash releasing savings were envisaged.
However as can be evidenced by the mean waiting times in the emergency department (appendix 2) the impact of this investment has been to improve the efficiency of flow in the emergency department.
Sustainability
The pilot is designed to inform the development of a combined assessment unit for the new District General Hospital and has been extended for another year.
Lessons learned
Key to the success of this pilot has been the high level of engagement of the wider team throughout.
In the initial planning stages a there was a weekly meeting of key staff to develop and agree the operational policy and detail of the patient flow.
During the initial weeks of the unit opening there was a daily huddle to identify and resolve issues as they developed.
This high level of engagement has continued with a weekly ward huddle and until recently a two weekly steering group meeting. The steering group meeting has dropped to monthly in the last week.
Appendix 1
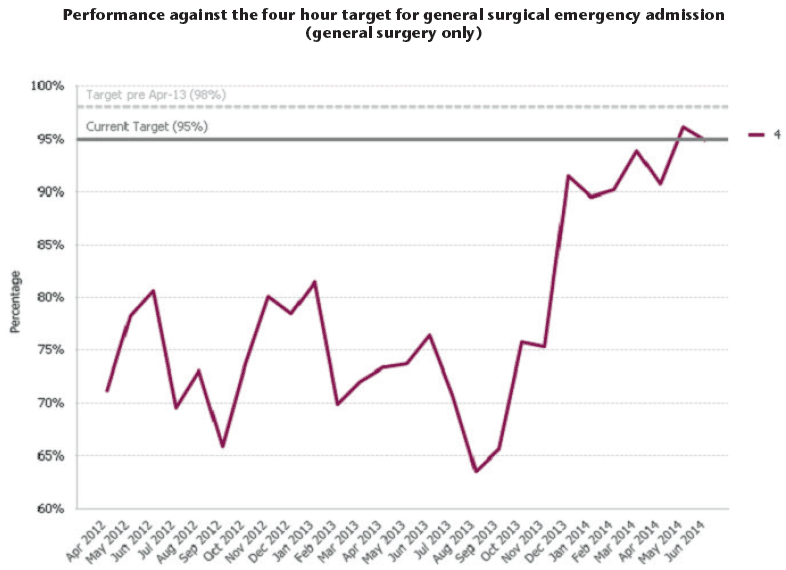
Appendix 2
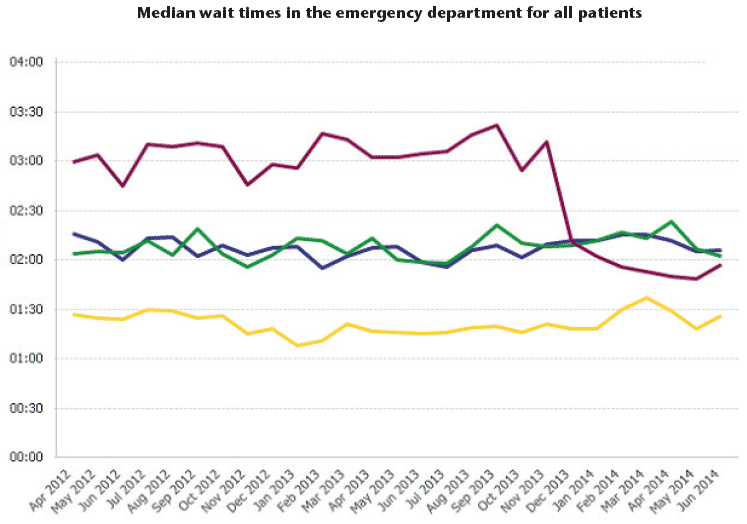
Coloured lines represent different patient groups admitted to the emergency department.
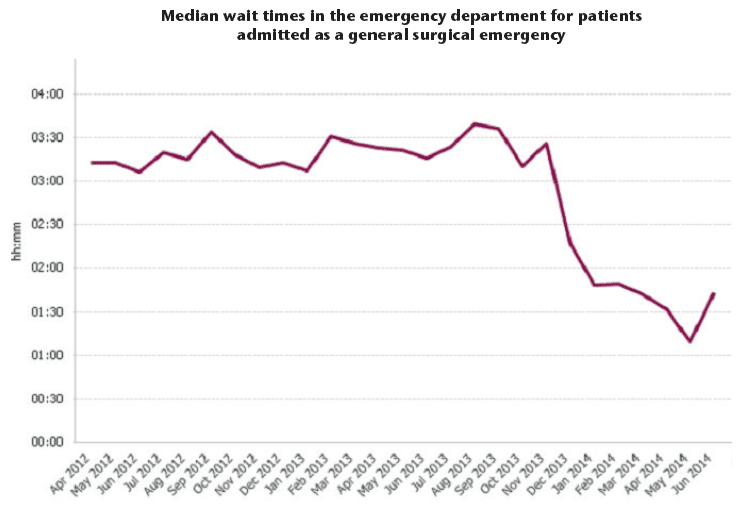
NHS Board Case Study
NHS Shetland
Orthopaedic pathway for pre-operative assessment - surgeries off-island
Background and context
The NHS Boards' corporate objectives are to provide quality, effective and safe services, delivered in the most appropriate setting for the patient. Several NHS Shetland pathways were identified as potentially having challenges and variation within them; pre-operative assessment for off-island procedures was identified as one of the priorities. It was therefore this pathway that was chosen as a project to identify the current state so the challenges could be identified from within pre-operative assesment.
Problem
The main problem was that the staff members working within this pathway were voicing confusion and finding it stressful working within the current system. Initial conversations with staff members revealed variation, duplication and ambiguity and it was decided to map the current state so the problem could be identified and future recommendations suggested.
Aim
The aim over a four month period was to identify the current pathway for patients and their clinical information for pre-assessment for planned hip and knee joint replacements off island. This would take into account both the staff and patient experience.
By the end of the four months, the current pathway would be identified and shared with the staff members (on Shetland, Elgin and Aberdeen) involved. On-island, Shetland staff members will be aware of their own and each other's roles within the current system and future recommendations will be made.
Action taken
Initially a project initiation document, contract, charter and driver diagram were drawn up. Then, interviews were held with staff members involved in the current system (10 members of staff on island) and telephone/email conversations with staff members off-island (five in Elgin, six in Woodend) and the current system was drawn up as a process map. This map was sense checked with all staff members to ensure it was accurate. Data was collected to find out how many patients went through the system. Patient stories were collected using emotional touch points.
Following collection of this information, a facilitated discussion was held on Shetland with the NHS Shetland staff members involved. During this session staff members measured their understanding of each other's roles at the beginning and end of the session on a scale 1-10 (1 being they do not understand the role at all, 10 being full understanding of the role). The beginning of the day saw scores varying from 1-10, the end showing variation of 8-10. This session also allowed future recommendations to be set.
During the project, there were several risks identified that were resolved. Procedural errors were highlighted where staff were unaware around policy sharing and this was addressed immediately. There was also ambiguity of words on documents being shared with across NHS Boards which was highlighted and changed. It was highlighted that there was variation in how patient information was being sent to the mainland (posted recorded delivery and scanned and emailed) and this was streamlined to be the same system for all hospitals.
Results
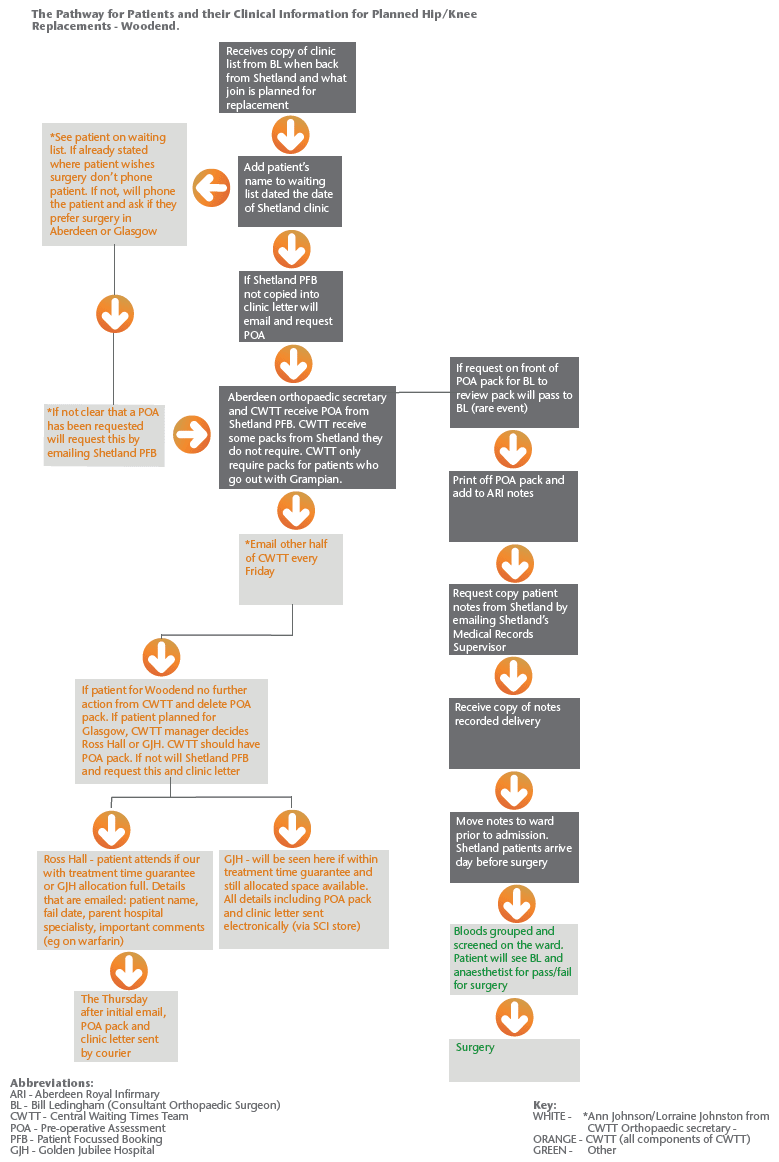
Attached at the end of the case study are three figures which show the pathways for Shetland, Elgin and Aberdeen as they currently stand.
This work benefits patients as staff are now aware of the current process they follow so can better inform them of their journey which leads to less confusion. Staff members appear happier in their work and have a clearer understanding of their role and each other's, thus enhancing working relationships. This work has raised the profile of NHS Shetland within mainland NHS Boards. Organisationally staff are compliant with policies within the pathway and variation has been reduced, thus lowering associated costs.
Efficiency savings and productive gains
Productivity has been improved because staff are now fully aware of the system they work within, they are able to provide the same service within existing budget but are able to inform the patients better around their journey. Costs have been lowered by scanning and emailing pre assessment pack to the mainland rather than sending recorded delivery which has led to a more efficient and cost effective means of producing the same results with less input.
The future recommendations this project has identified will further add to the efficiency and productive gains by further reducing variation and streamlining the system to ensure faster throughput of patients.
Sustainability
A local working orthopaedic group has been established on-island to take forward to recommendations from this project. All key stakeholders have been identified and invited. This will ensure regular and effective communication links are maintained between key staff members, which will also ensure sustainability of the current changes.
Lessons learned
The main lesson learned from this work was the time it took to extract the information from all stakeholders and the complexity of working across NHS Boards. It highlighted the importance of having a clear working pathway which everyone is aware of and understands. Challenging assumptions was another learning point, as these assumptions are often not factual and can further lead to confusion. The local orthopaedic working group will take forward the recommendations which have been identified by completing this work. Others looking to map similar pathways could use this as a means of demonstrating the benefits of this type of analysis - without mapping these pathways, it would have been impossible to find where the variation and ambiguity was and therefore identify solutions.
Figure 1 - Shetland Pathway
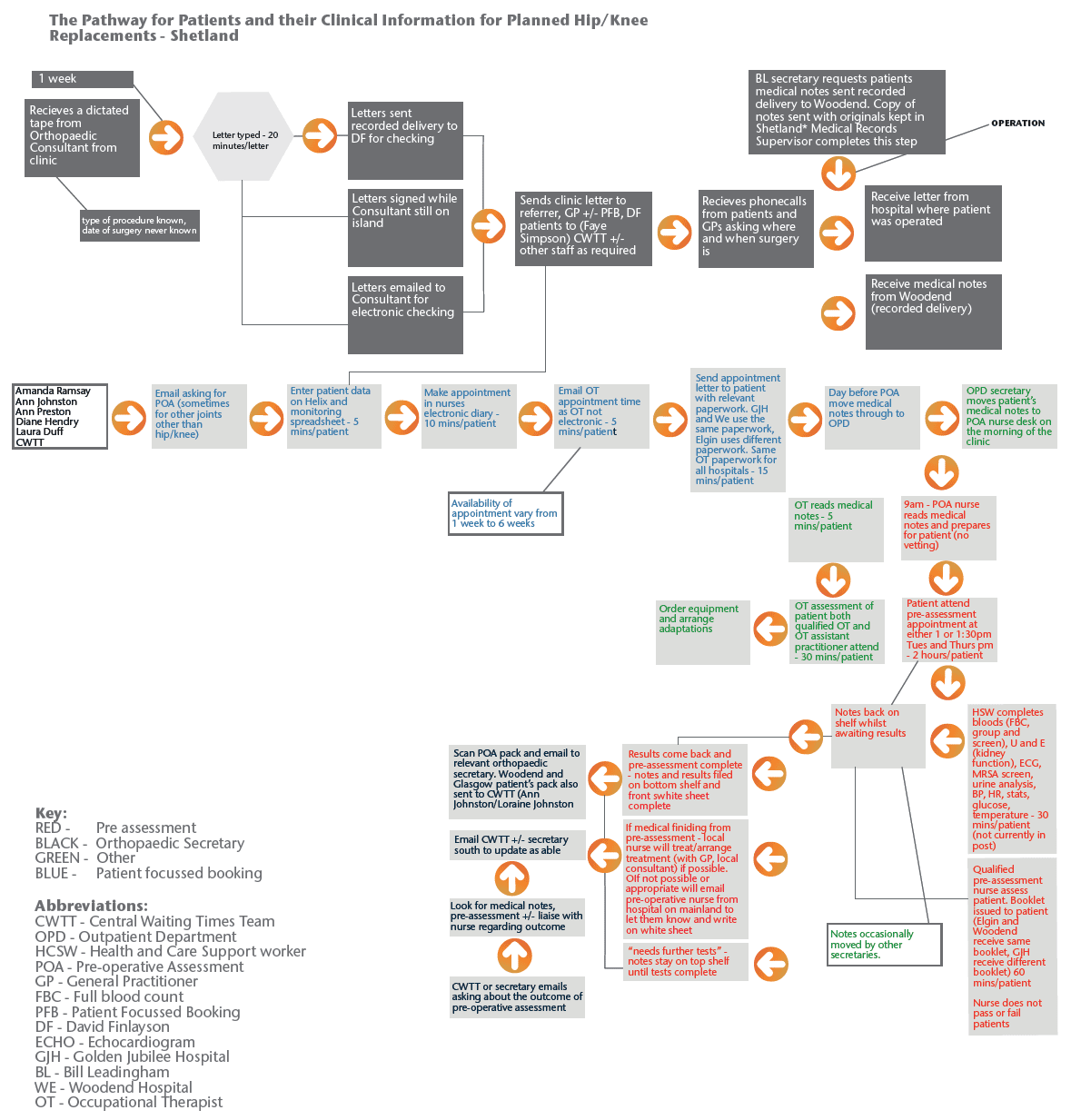
Figure 2 - Elgin Pathway
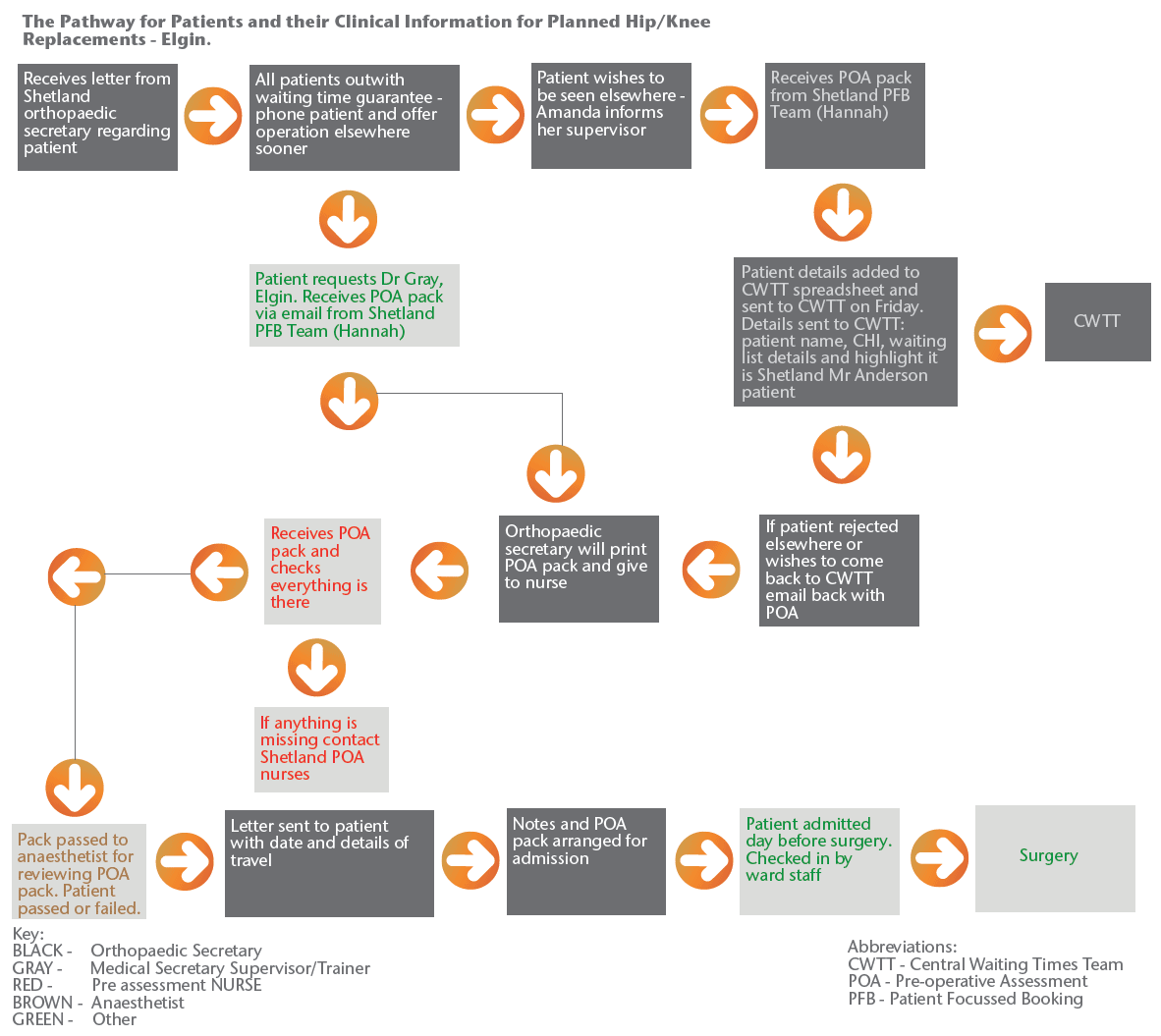
Figure 3 - Aberdeen Pathway (Woodend)
NHS Board Case Study
NHS Western Isles
Real-time DCAQ Data Dashboards
Background and context
The QuEST Efficiency and Productivity Report identified NHS Western Isles as outlier in the number of measures of mental health delivery while national benchmarking products continued to place Western Isles Hospital as an outlier for a number of efficiency measures most notably around average length of medical stay. Key to improving these metrics has been a recognition of the need to apply DCAQ information to redesigning system processes and embed its use in operational management. While collection of DCAQ data has seen developments, these were not yet fully realised while there is a real need for support to facilitate the use of such information within the operational service planning of these services. It has recently been a critical time for these services in Western Isles as we undertake a full mental health redesign and wider hospital modernisation programmes. There will be a key requirement when implementing new models that the principles and applications of improvement advice and key role for DCAQ metrics are at the centre of operationalising this model.
Problem
Past attempts to redesign processes or services have tended to rely on reactive responses to particular situations and utilised ad hoc information. This information was more often than not unclear on its links to the problem, out of date once utilised and did not form part of the on-going management and monitoring of the process/service redesign. The result often was that when addressing issues such as peaks in demand, loss of capacity, activity build-ups and waiting time pressures there was a deficit in timely information available to either anticipate or alert immediately when processes/services were out of balance. In addition the use of such information did not form part of the on-going routine operational management to ensure such balance once re-established was sustainable and maintained.
This situation was a product of both lack of manager engagement with such data and the deficiencies in the data itself.
Aim
The aim of project was to develop and introduce a suite of electronic DCAQ dashboards for use by operational managers beginning with identified key needs for referrals/activity and waiting lists by end of March 2014.
Action taken
The aim was to be delivered via a change in both the content and delivery mechanism of data to provide managers with a more self-serve approach to intelligence required. An initial gathering of information requirements and user engagement was carried out both pre and post introduction of the change in information delivery. Training in use and interpretation of the new information dashboards was arranged which included a move to more statistical process control trending and benchmarking information outputs to measure progress over time and comparatively with peers.
Results
Dashboards were developed and trained in primary care (referrals/activity), out of island referrals (SCI Gateway and ECR referral analytics), waiting lists and theatre utilisation.
Efficiency savings and productive gains
It is early days yet in evaluating the impacts on the service improvements from such new tools and DCAQ approaches. Examples of gains have been described by Theatre Administrators as improving theatre utilisation, and by GPs as an increased ability to track their referrals/admissions over time and benchmarked to their peers. Alerts for acute admission enable care planning and discharge.
Sustainability
This is now the primary method of data delivery for our operational teams. A programme of future planned developments is underway into Clinical Quality which will replicate similar analysis techniques for this area around hospital mortality, average length of stay, A&E waiting times, DC rates and selected metrics from Patient Safety programme. The regular awareness raising and training of staff in this approach to data delivery is planned alongside developments.
Lessons learned
Key lessons from learning were twofold:
1. Engagement with key staff at outset to get their requirements and sign-up to change to new way of data delivery and its utilisation.
2. Availability of right data at right time was key to success of take up. Data therefore needed to be as near to real-time as feasible and relatively straightforward to interpret (which is where use of run charts and benchmark comparisons were effective). The early developments suffered from being perhaps over complex while gradually have simplified to focus on these key data outputs that can be used relatively easily.
NHS Board Case Study
NHS National Waiting Times Centre Board
Orthopaedic Pathway Improvement
Background and context
The Orthopaedic service within the Golden Jubilee National Hospital (GJNH) has been established for ten years and has strived to be a centre of excellence for lower limb arthroplasty which incorporates two differing referral flows: 'treat'(patients who have previously been assessed for surgery by a consultant or extended scope practitioner at their host NHS Board) and 'see and treat' programme (patients who are assessed for surgery and treated as appropriate by a consultant within GJNH ). Since 2008 it has led the way in developing a designated Enhanced Recovery Programme (ERP), and the CALEDonian® Technique, which has resulted in improvements in patient outcomes whilst reducing length of stay following surgery (McDonald et al, 2012).
From 2010, a national programme to establish ERP as the normal pathway of care for all patients undergoing joint arthroplasty has been developed. This has improved patient care throughout Scotland and has led to reductions in:
- Catheterisation rates
- Blood transfusions
- The mean post-operative length of stay for patients around Scotland (MSK Audit 2013)
Problem
Although the GJNH outcomes from the ERP programme have remained consistent, they have now become the norm. To sustain the hospital's position as the centre of excellence for lower limb arthroplasty, it was necessary to review the whole patient journey from referral to follow up. This review had to:
- Take into consideration the impact that the steep rise in the number of 'see and treat' referrals was having on service delivery
- Help establish where further improvements could be made that would benefit the patient and provide the highest quality of care
- Provide increased capacity to accommodate the demand
Aim
To achieve this it was decided that a clear quality improvement methodology was necessary which would help to structure, analyse, implement and sustain the proposed improvement. The objective of the programme was to maximize capacity in order to service the increasing demand in Scotland for lower limb arthroplasty.
From this, the Orthopaedic Improvement Group decided on the following two aims:
1. To ensure all patients are pre-assessed and fit for surgery two weeks prior to their operation
2. To reduce average length of stay for primary Total Hip Replacements and Total Knee Replacements by two days
Action taken
A series of workshops was arranged with all relevant stakeholders and a decision was taken to use a natural variance model which:
- Focused on the management of variability within healthcare processes
- Provided a structured process to follow
- Used data to support findings and facilitated the development of measurable outcomes
By following this model, the groups were able to identify what would prevent the two aims being achieved. Data was collected to support these findings and then objective changes were made along the whole patient pathway to improve service delivery.
As well as following this model, the input of an external expert with experience in both quality improvement work and service delivery in orthopaedics helped to:
- Provide constructive challenges for the staff
- Bring ideas and examples of alternative ways of working
- Instil a discipline of following a quality improvement model
- Make the team focus on the key areas to be improved
- Monitor these improvements
Results
One of the main challenges identified that would prevent the achievement of the first aim was the lack of a robust waiting list management system. This has been addressed and there are now electronic referrals being received from NHS Lanarkshire, NHS Lothian, NHS Greater Glasgow and Clyde, NHS Ayrshire and Arran, NHS Dumfries and Galloway and NHS Forth Valley.
Data collected would suggest that this work has been successful with the majority of "treat" patients being received early in their nine week treatment pathway (Figure 1).
Figure 1: Wait times from referral to admission in weeks
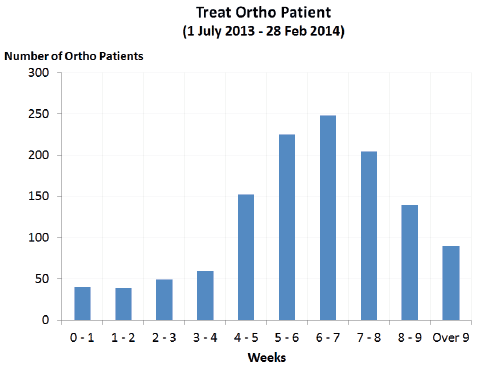
Clinic activity has also increased since the redesign released capacity with the average monthly attendance now averaging 500 patients (Figure 2).
Figure 2: Clinic activity from August 2013 - Feb 2014
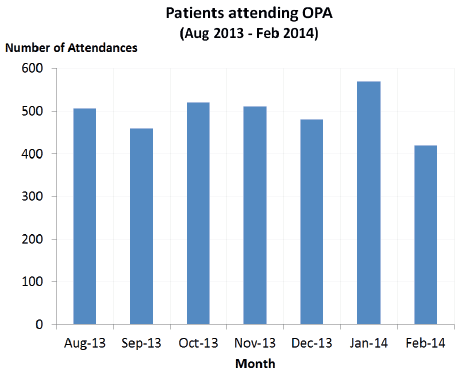
Prior to the implementation of the improvement work, there were a high number of patients attending clinic less than two weeks before their pre-booked theatre date. This would often lead to theatre slots not being filled, as there was insufficient time to contact other patients to replace anyone who was unfit for surgery. This programme has resulted in improvements in the referral management systems and new Service Level agreements with other NHS Boards which has led to:
- Reduced 'batching' and a smoothing out of booking office activity with patients being referred earlier in the pathway
- Improved and timely population of the pre-operative assessment clinics
- Better theatre utilisation because of the increased time between pre-operative assessment and procedure date (Figure 3/Table 1)
Figure 3: Wait time for patients between pre-assessment and procedure
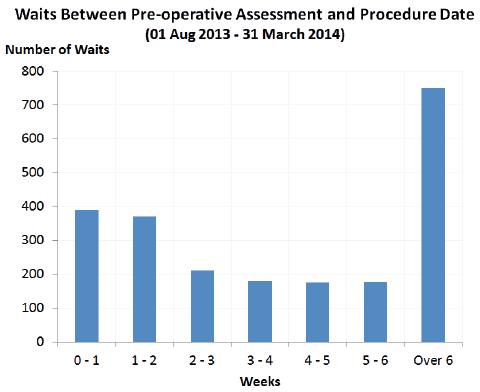
Table 1: Percentage waits between pre-operative assessment and procedure date
| Weeks | Number | % |
|---|---|---|
| 0-1 | 347 | 17 |
| 1-2 | 349 | 16 |
| 2-3 | 210 | 10 |
| 3-4 | 167 | 8 |
| 4-5 | 146 | 7 |
| 5-6 | 149 | 7 |
| Over 6 | 757 | 35 |
| TOTAL | 2,152 | 100 |
Efficiency savings and productive gains
The changes made to the patient pathway following this improvement work have clearly demonstrated that:
- The vast amount of patients are being seen within nine weeks of receipt of referral.
- Attendance at outpatient clinics continues to rise.
- Patients now attend for their pre-operative assessment in a timely fashion that allows for any challenges such as patient's being unfit for surgery to be managed appropriately.
- Nurses now pre-assess patients independently of the surgeon's consultation which has increased the capacity and greatly improved the patient flow through the clinic.
Sustainability
The monitoring of the new Service Level Agreement with other NHS Boards ensures that referrals are received in a timely fashion. Data relating to pre-operative assessment activity is now reported monthly and meetings with relevant stakeholders are held weekly to review waiting times.
Lessons learned
The Orthopaedic Improvement programme has, from the start, showed encouraging results. It has also clearly demonstrated the benefit of following a quality improvement methodology which is
- Simple
- Based on data which is continually reported
- Used to monitor, modify and sustain improvement