Non-surgical cosmetic procedures regulation: consultation analysis - final report
Independent analysis of the responses to our consultation on the regulation of non-surgical cosmetic procedures, which ran in 2020.
Chapter 2 – Findings
Introduction
2.1 This chapter takes each consultation question in turn and explores the responses to each. It sets out similarities and divergences in opinion, by respondent grouping.
Q1: Do you agree that further regulation of non-surgical cosmetic procedures is needed?
Quantitative analysis
2.2 Respondents were asked to indicate whether their response was yes/ no/ don't know to this question. A total of 434 out of 437 respondents answered this portion of the question. Al most all felt that there was a need for further regulation. All organisations agreed – across all organisational respondent categories - and almost all individuals. See Appendix Two for a detailed breakdown.
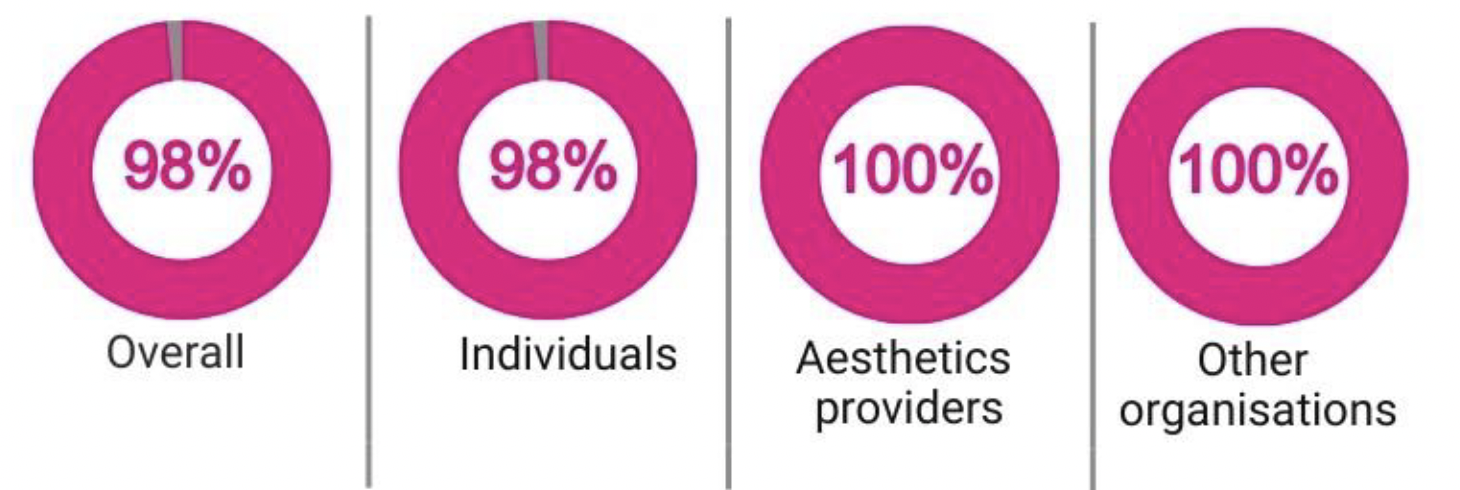
Qualitative analysis
2.3 There were 343 written responses to the open part of this question. Most highlighted their reasons for believing that further regulation was needed. Most respondents - both individuals and organisations - felt that non-surgical cosmetic procedures should be conducted by trained, qualified and regulated healthcare professionals. Many respondents commented on or referenced the Review of the Regulation of Cosmetic Interventions (2013).
2.4 Respondents highlighted the:
- risk of physical harm
- risk of psychological harm
- cost to the NHS; and
- possible regulatory solutions.
2.5 These points are taken in turn below.
Risk of physical harm
2.6 The primary concern from respondents saying that more regulation was needed was that there is a risk of serious error and injury with these procedures, such as burns, skin necrosis or blindness. Some respondents also highlighted the risk of cross-contamination and transmission of blood-borne viruses.
"It's easy to train to deliver these injections, it requires far more expertise to reverse or manage complications. Anyone who cannot manage their own complications should not be delivering these treatments." Individual
"These procedures are in fact clinical procedures and should not be carried out by lay people who are not registered and regulated health professionals… Ultimately, this is about protecting patients from physical and psychological harm." Individual
"Complications can cause blindness and death of skin tissue therefore the procedure should always be carried out in a medical environment with emergency protocols and drugs available." British Association of Cosmetic Nurses
"There is a potential for severe burns that may require skin grafts, permanent scarring, tissue loss, and psychological harm as a result of these injuries." Association of Personal Injury Lawyers
2.2 2.7 Respondents were concerned that the products used in non-surgical cosmetic procedures on the face can be dangerous, particularly because the head and face is anatomically complex. Some felt that anyone conducting non-surgical cosmetic procedures should have detailed knowledge and understanding of the anatomy and physiology. Some respondents from the aesthetics providers group reported that they had seen the complications which could arise from non-surgical cosmetic procedures, and they were concerned that these posed a serious risk to the general public.
"These potentially complicated procedures can lead to devastating side effects if given by unqualified practitioners. These side effects include skin necrosis and worst of all, permanent blindness." Suffolk Medical and Beauty Clinic Ltd.
2.8 Respondents from organisations felt that people who were not healthcare professionals did not have the expertise or access to specialist treatments to effectively diagnose and manage these complications. Some noted that currently, anyone could offer these procedures after completing a short training course that took only a few days. They felt that this level of training had no parity with the extensive training and ongoing professional development undertaken by healthcare professionals.
"These procedures should only be carried out by those with a medical background and access to and training in dealing with extremely serious complications that can arise." Simply Skin Facial Aesthetics
2.9 In particular, some respondents noted that the medication required to treat some complications is only accessible through a prescription from a medical practitioner, such as antibiotics to treat infections or hyaluronidase to reverse dermal fillers. They were concerned that practitioners without access to these medicines would not be able to rectify the complications, and that this put the public at risk.
2.10 Many respondents, both individual and organisations, said that they were aware of an increasing body of evidence indicating that the serious complications arising from these procedures were as a result of unregulated practitioners, or those in unregulated premises. Several respondents reported that they were aware, anecdotally, of poorly performed procedures in an unregulated environment.
2.11 One organisation had conducted a survey which found that 10% of people who had a negative side effect from a procedure went on to need medical treatment. And another organisation had conducted research and provided links to further research investigating the potential harm of non-surgical cosmetic procedures. These are available in Appendix One.
2.12 One individual, who self-identified as a healthcare professional said that they were aware of high-risk practices in the unregulated sector, such as the sharing of vials between different patients.
2.13 There was also some concern about follow up and traceability, leaving patients at serious risk with no accountability to the practitioner.
"As a solicitor working in clinical negligence I have seen first hand the devastation that non-surgical cosmetic procedures can do when they go wrong. Often the risks of a procedure are not explained properly or are under played. It is not clear what training the person has had and what standards they are adhering to." Individual
"There is no traceability at the moment and many people do not have the correct skills and training and emergency equipment." Soft Touches Aesthetics
"We are seeing more and more problems in our clinic from patients who have had treatments from non medics such as beauticians, who then block them on social media once there is a problem." Individual
2.14 One organisation noted that registration and indemnification is voluntary for non-healthcare practitioners, which they found contradictory to the regulations for healthcare professionals.
2.15 Respondents also said that in an unregulated environment, there was a higher risk of patients being injected with poor quality products. A few respondents were concerned that unregulated practitioners purchased low quality products (e.g. dermal fillers) online.
2.16 One organisation also noted that regulation was important to maintain professional standards, so that individuals with blood-borne viruses are not discriminated against and can still safely access non-surgical cosmetic procedures.
Risk of psychological harm
2.17 Many respondents noted that the unregulated sector posed a significant risk to the public due to unethical practices, poor clinical environments and limited or inadequate aftercare for patients. A few individual respondents and organisations felt that this posed an increased risk of psychological harm, as well as physical harm.
2.18 The main concerns were that unregulated practitioners were more likely to exploit young or vulnerable people, who felt they needed to change their image.
"In addition, full medical training is required to be able to assess medical suitability for these procedures e.g. to assess the interactions of other drugs they may be on, or to assess for signs of body dysmorphia which may mean than treatment should not be carried out. This cannot be taught on courses lasting days or weeks. It takes years of training." Individual
2.19 Several respondents noted that mental health was a key concern in the sector. They felt that providers should be aware of potential mental health issues and risks associated with medical aesthetic procedures. They felt that a regulated sector was more able to manage these risks.
2.20 Some respondents also felt that unregulated practitioners were less likely to adhere to a code of ethics, which would ensure good practice in terms of consent, confidentiality and a cooling off period prior to the procedure.
"It also concerns me that individuals may feel pressurised to have treatment and that there is no compulsory calling off period following a consultation." Individual
2.21 A few respondents from aesthetics providers felt that this risk was higher in the non-regulated sector, because it was primarily concerned with income generation, to the extent that it might put patients at risk. One respondent noted that practitioners themselves may also be at risk from the unregulated sector. Without clear regulation, practitioners may be vulnerable to people selling expensive training courses, which are insufficient and do not adequately prepare them for practice.
Cost to the NHS
2.22 A few respondents (from different categories) noted that complications arising from unregulated non-surgical cosmetic procedures are dealt with by the NHS, often when patients present to the Accident and Emergency department. They felt that it was unfair for the NHS to bear the burden of the cost associated with the risk of these procedures. And they felt that more regulation would lead to fewer sub-standard procedures, and less burden on the NHS.
Views on the current regulatory framework
2.23 Some respondents, both individuals and organisations (aesthetics providers, regulatory/standard setting bodies, membership representative bodies) commented on the current regulatory framework. In Scotland, medical and dental professionals (medical practitioner, dental practitioner, registered nurse, registered midwife or dental care professional) are regulated by HIS. They are also subject to a range of standards and ongoing professional development requirements as set out by regulatory councils, such as the General Medical Council and Nursing and Midwifery Council. However, there is no corresponding regulation for others delivering these procedures, such as beauticians or beauty therapists.
2.24 Some noted that there was a contradiction between the regulations for registered healthcare professionals and the lack of regulations for others performing similar non-surgical cosmetic procedures. Respondents noted that the regulations for non-surgical cosmetic procedures should apply to both the individual practitioners and the place in which the procedures are delivered. Some respondents felt that there was a higher risk of complications when procedures were conducted in unregulated premises, which might be unhygienic and unfit for purpose.
2.25 Some respondents, across categories, felt that regulation of practitioners should include insurance, such as public liability insurance or professional indemnity in order to protect patients. A few respondents shared examples of instances where patients had experienced harm from poorly delivered procedures, but had no recourse or compensation as the practitioner did not have appropriate insurance.
"Non regulated individuals are free to practice increasingly complex and dangerous procedures without regulation or redress – indeed there is no requirement for insurance, adequate premises, sterile procedures, safe disposal of sharps or contaminated (essentially clinical) waste nor for the testing and vaccination of non-medical "practitioners" for Hepatitis B. This anomaly puts patients at an increased risk…" British College of Aesthetic Medicine (BCAM)
2.26 A few respondents from organisations, also noted that regulated professionals must adhere to standards for their premises and professional conduct, as well as insurance, health and safety processes and policies for patient protection. Without these standards in place, they felt there was a risk to patients.
"More regulation is required to give the public assurance that the practitioners they choose are being held to an appropriate level of professional standards and are competent to carry out the procedures." Royal Pharmaceutical Society
2.27 However, some respondents felt that there should better regulation overall, both for healthcare professionals and individuals with no health qualifications. This included both individual respondents, and respondents from membership or representative bodies.
2.28 One local authority noted that the regulations needed to be comparable for healthcare professionals and those who are not healthcare professionals delivering the same treatments.
2.29 There were two main points here. Firstly, some felt that some healthcare trained practitioners were working outwith their specialty or area of expertise and were posing a risk to patient safety. For example, several respondents felt that only healthcare professionals with training and experience of injecting should be able to offer procedures requiring injecting.
"I also think only medical professionals who have extensive experience in injecting should be allowed to do these procedures, again all to do with risks from poor technique." Individual
2.30 Secondly, a few felt that specialist non-medical practitioners could bring more expertise in non-surgical cosmetic procedures than some medical practitioners.
2.31 One membership/representative body and a few individuals felt that where non-healthcare practitioners were highly trained in aesthetics procedures, they may be more skilled, and safer, than healthcare professionals without specific training.
Possible regulatory solutions
2.32 Many respondents indicated that an approach similar to the current regulation by HIS would be welcomed. Most of these respondents also felt that non-surgical cosmetic procedures should only be conducted by healthcare professionals. HIS, which currently regulates independent clinics run by certain healthcare professionals, also indicated that the practice of these procedures should be limited to healthcare professionals.
"Whilst we support further regulation, we are not indicating that we believe it desirable to extend the provision of certain non-surgical cosmetic procedures (for example injectables) beyond registered healthcare professionals, in order to ensure the public are appropriately safeguarded." Healthcare Improvement Scotland
2.33 One respondent from an organisation (local authority) noted that non-surgical cosmetic procedures could be regulated in a similar way to skin piercing and tattooing, which is subject to legislation and regulation by local authorities under the Civic Government (Scotland) Act 1982. However a few respondents noted that they felt regulation by local authorities would not be rigorous enough.
2.34 One organisation suggested that the Joint Council for Cosmetic Practitioners would be an appropriate regulatory body.
2.35 Several respondents suggested that Scotland could look to other countries in Europe or further afield, where there are stricter regulations.
2.36 A small number of individuals voluntarily indicated in their response that they were practitioners who were not regulated by HIS. Most agreed that there should be more regulation, covering areas such as training, insurance, premises and infection control.
"As a beauty therapist I think it's disgraceful that the whole beauty therapy and hairdressing industries are not regulated at all and there is no minimum level of training required…." Individual
2.37 One felt that the same standards should apply both to medically trained healthcare professionals non-medically trained professionals.
"I believe that it should come down to the training that the person has received. I also think it should not just be non medics that should require the license. I am a non medic aesthetics practitioner. I had fantastic training and passed and have all my certificates. I carry insurance and only practice safely." Individual
Reasons for not seeking further regulation
2.38 Of the eight individual respondents who felt that further regulation was not needed, five provided further comments. However, two of these felt that no further regulation was needed because individuals with no professional health qualifications should not be permitted to offer non-surgical cosmetic procedures.
2.39 The remaining three individual respondents who said that no further regulation was needed felt that individuals with no professional health qualifications could be trained to an appropriate level.
"I think it's unfair to push beauticians out of this industry or make it hard for them. There's some absolutely fantastic beauticians carrying out these procedures." Individual
Question 2: Do you agree that the carrying out of non-surgical cosmetic procedures (that pierce/penetrate the skin) by individuals who are not qualified healthcare professionals should be licensed under Part 1 of the Civic Government (Scotland) Act 1982?
Quantitative analysis
2.40 Almost two thirds of respondents (61%) agreed that individuals who are not qualified healthcare professionals should be licensed under the Civic Government (Scotland) Act 1982. Just over a third of respondents (36%) felt that they should not. A small proportion of respondents didn't know, or chose not to answer this question.
2.41 Responses varied between different groups. While just over half of aesthetics providers agreed, this increased to three quarters for other organisations.
Figure 2.2: Respondents who agreed with the proposal to license non-surgical cosmetic procedures under Part 1 of the Civic Government (Scotland) Act 1982
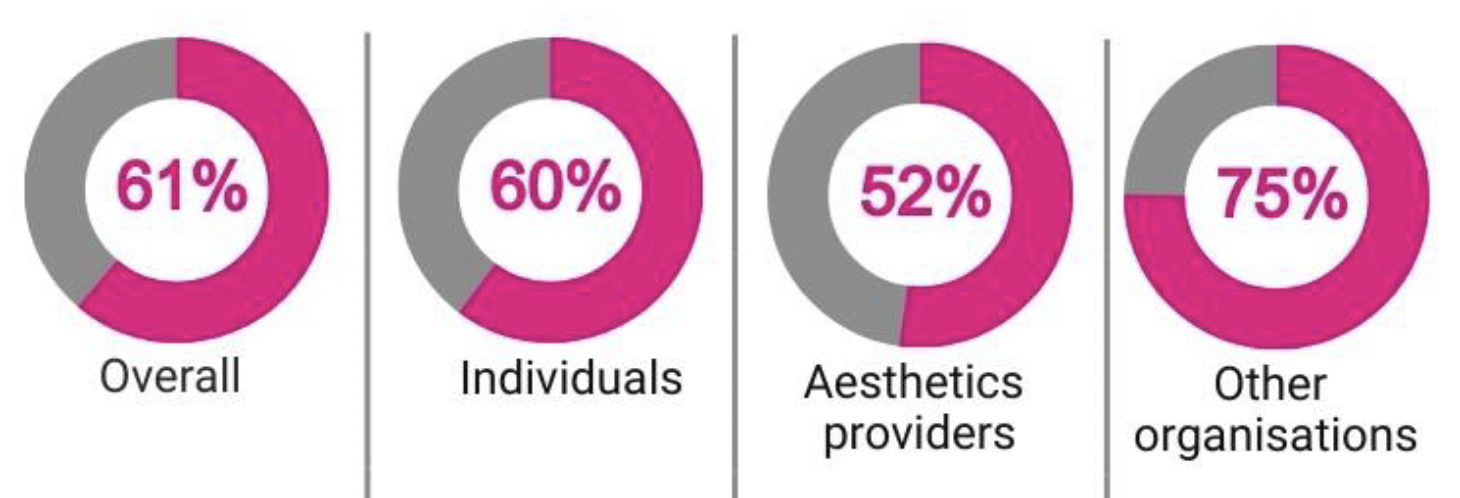
2.42 A majority of organisations across all categories agreed with the proposals for licensing. See Appendix Two for a detailed breakdown.
Qualitative analysis
2.43 There were 324 written responses to this part of the question. Respondents who both agreed and disagreed with the proposals often made similar points.
2.44 Most respondents choosing 'yes' felt that this was in line with their view that the unregulated sector needed more regulation. Some of the respondents agreeing with the proposal felt that licensing under the current framework was not enough, and that it should be accompanied with further regulation and requirements for indemnity insurance or infection control measures.
2.45 Similarly, most respondents choosing 'no' said that they disagreed with the proposal because they felt that licensing alone was not enough. These respondents either felt that there needed to be much stricter regulation of the sector, or that these procedures should only be conducted by healthcare professionals, and so no further regulation was required.
Respondents who agreed with the proposal
2.46 Most respondents – both individuals and organisations - agreed with the proposals. Respondents agreeing with the proposal largely felt that more licensing was a step in the right direction towards increased regulation of the sector. They felt that it would improve industry standards and patient safety, and ensure a record was kept of those able to undertake these procedures.
"From our experience, regulation enhances public confidence, ensures patient and public safety and furthermore give assurance that the risks to patients and the public has been measured and considered. In addition, it encourages those who are regulated to enhance their offering and further improve their standards." General Pharmaceutical Council (GPhC)
"There need to be a register and control over anybody doing these procedures." Individual
2.47 Most membership/representative bodies and local authority respondents agreed that individuals who are not healthcare professionals should be licensed under the Civic Government (Scotland) Act 1982 to perform these procedures. They felt that this would align with the current regulations for skin piercing and tattooing and would fit in well with the current framework.
2.48 HIS which currently regulates independent clinics run by certain healthcare professionals delivering these procedures agreed that licensing under the Civic Government (Scotland) Act 1982 would allow regulation of individuals who are not healthcare professionals. It noted that licensing should involve adhering to a clear set of standards for those who are not healthcare professionals.
2.49 Many individual respondents expressed their perception that licensing and regulation would improve patient safety. They felt that licensing would deter underqualified or incompetent practitioners and encourage good practice.
"This would ensure that people are properly trained and qualified and more likely to meet proper requirements and insurance needs." Individual
"This will protect the patients from non professionals and will encourage treatment providers to get some qualification before treating their clients." Individual
"I am a beauty therapist who offers Electrolysis and required to have a license for using the smallest of needles when there are therapists injecting into muscle with much larger needle, possibly causing potential damage. There are too many therapists injecting with not enough training. Having new rules would help eradicate those unscrupulous injectors." Individual
2.50 A few respondents questioned if the licensing would apply to other non-surgical cosmetic procedures, beyond those involving injecting e.g. laser treatments or microneedling.
"Peels and laser treatments are also beset with major, permanent risks and need to be regulated in the same way." Individual
2.51 However some respondents agreeing with the proposal felt that licensing under the Civic Government (Scotland) Act 1982 would not be sufficient. They felt that more thorough regulation and oversight was necessary.
"Licencing is the wrong word. They need to be regulated, both the person and the premises. This approach is nowhere near sufficient to maintain patient safety." Individual
2.52 Many respondents reiterated their view that these procedures should only be carried out by healthcare professionals, as they have the ability to manage the risks and potential complications.
"The licence should only allow doctors and dentists to do such work, no-one else. It is only doctors and dentists who have the detailed knowledge of anatomy and pharmacology, and who are competent to treat complications." Individual
2.53 Some respondents felt that for licensing to be effective, there should be clear criteria specific to the types of procedures covered. One respondent suggested that additional conditions under Part 2 of the Act might be helpful. And one local authority noted that the requirements would need to be detailed and that officers would need training to ensure that licensed practitioners worked to the same standards as healthcare professionals.
"Part 1 of the Civic Government (Scotland) Act 1982 refers to the general provisions governing licensing; it is not specific and presumably therefore additional conditions under Part II of the act – Licensing and Regulation – Particular Activities would be required." British College of Aesthetic Medicine
2.54 Some respondents suggested that licensing should include a mandatory infection control qualification, as recommended in the 2013 Review of the Regulation of Cosmetic Interventions (Keogh Review). A few respondents noted that Scotland could look to Wales, which they highlighted has a licensing and regulation scheme for practitioners offering non-surgical cosmetic procedures.
Respondents who disagreed with the proposal
2.55 Most respondents who disagreed with the proposals felt that these procedures should only be performed by medically trained healthcare professionals. As such, they did not feel there was a need for licensing. Many were in favour of increased regulation but did not feel that licensing under the Civic Government (Scotland) Act 1982 was sufficient.
2.56 Some respondents reiterated their view that only healthcare professionals should perform these procedures. Some respondents felt that people who are not qualified healthcare professionals do not have the knowledge or skills to manage potentially life threatening complications that can arise from these procedures. Some respondents reiterated that unregulated individuals do not have the authority to prescribe the medicines required to reverse procedures or treat complications, where required.
"This is not appropriate, and should not be allowed. Regulation should ensure that only qualified healthcare professionals undertake elective aesthetic clinical treatments." Individual
2.57 However, some respondents who felt that only healthcare professionals should perform these procedures noted that if individuals who are not healthcare professionals were to continue offering these procedures, they should be registered and regulated in the same way as healthcare professionals.
2.58 A few organisations noted that any licensing scheme would need to set out clear requirements and eligibility criteria. It would also need to be enforced, to ensure that the public and practitioners had a high level of trust in its implementation.
2.59 Some respondents noted any regulation should be to the same standard, or a higher standard, than healthcare professionals, who are already regulated by their own professional bodies and HIS. Some respondents felt it would be unfair to have different regulatory systems, with different costs for healthcare professionals and individuals who are not healthcare professionals delivering the same procedures.
"Any regulation must apply the same standards to all in order to be fit for purpose." Save Face
"It has to be a slightly higher standard which is that of a healthcare professional because there are potentially huge medical implications such as infection or nerve damage or death." Individual
2.60 A few respondents specifically noted that non-surgical cosmetic procedures involving injectables differ significantly from skin piercing and tattooing procedures.
"There should be a new act. Piercing or body piercing does not carry the same risk as injecting under the dermis, down through tissue layers to the bone. It is NOT remotely close to the legislation required." Individual
"Current legislations should be changed to prohibit any such aesthetic procedures from being carried out by anyone who is not a medically qualified individual. I do not believe that piercing or tattooing should be considered under the same remit as this." Temple Medical
2.61 And one organisation felt strongly that only medically trained healthcare professionals should be allowed to undertake these procedures. It suggested that dermal fillers should be reclassified as medicines (as opposed to devices) and called for greater public awareness of the risks associated with these procedures.
2.62 A few respondents voiced concern that licensing under the Civic Government (Scotland) Act 1982 might give the public a false sense of security regarding the risks associated with the procedures and the competency of the practitioner delivering them.
"Licencing would validate the role of non-medical individuals carrying out non-surgical medical aesthetic procedures and reduce the public perception of these medical procedures to that of beauty treatments, which would put the public at risk." Association of Aesthetic Patient Protection Scotland
2.63 One individual felt that individuals who are not healthcare professionals could be permitted to offer these procedures, within the currently regulated sector i.e. a clinic regulated by HIS. This type of clinic is managed by healthcare professionals who would have specialist knowledge and access to the medications that might be necessary in the event of a complication.
"I would have no objection to fully qualified beauty therapists providing these services in a HIS registered setting under the supervision of a medical professional." Individual
2.64 One organisation felt that licensing for individual practitioners was not suitable. It suggested a single, national register for practices, rather than individual practitioners. It also suggested that registration should be free and managed by the government. It felt that this would encourage uptake and ensure that the register did not become a commercial enterprise.
2.65 One individual respondent who disagreed with the proposals felt that people working in the beauty industry were more experienced in some procedures than medical professionals. They felt that additional licensing was unfair to those working in the beauty industry.
"Beauty therapists are trained at a high level carrying out procedures on the skin such as semi permanent makeup, aesthetic procedures such as electrolysis and may have had years training in this area. Medics have not. I believe this is a discriminatory approach to one sector." Individual
2.66 Responses from aesthetics providers were split, with around half agreeing and half disagreeing with the proposal. However, those who commented were in agreement that only medical professionals or practitioners working under the supervision of medical professionals should be able to perform these procedures.
Respondents who neither agreed nor disagreed with the proposal
2.67 A small number of respondents providing comments selected 'don't know' or chose not to provide an answer to the closed question.
2.68 One organisational respondent from a regulatory/standard setting body provided a detailed response indicating that while some regulation is preferable to no regulation, it would be important to clarify certain details. These included the definitions and standards for people to meet the licensing requirements. It also noted that licensing of these procedures would add to the existing workload of local authority officers. This response also queried the remit of the licensing, particularly whether it would extend to prescribed treatments, as well as non-prescribed treatments.
2.69 A small number of individuals answered 'don't know'. Most felt that these procedures should only be offered by healthcare professionals, or that all practitioners should be subject to the same level of regulation under HIS.
2.70 They cited similar reasons as those mentioned in question one. Namely, that non-surgical cosmetic procedures have a high level of risk, and that unregulated practitioners have little to no accountability when procedures go wrong.
"At present, there is no necessity for a beauty therapist to carry insurance legally and no controlling body which can stop them from practicing regardless of location. These are mandatory basic requirements of a healthcare professional." Individual
Question 3: Do you agree that services provided by pharmacists who undertake independent healthcare practices (including non-surgical cosmetic procedures), outwith the terms of an NHS contract should be regulated by Healthcare Improvement Scotland?
Quantitative analysis
2.71 Most respondents agreed that services provided by pharmacists who undertake independent healthcare practices outwith the terms of an NHS contract should be regulated by HIS.
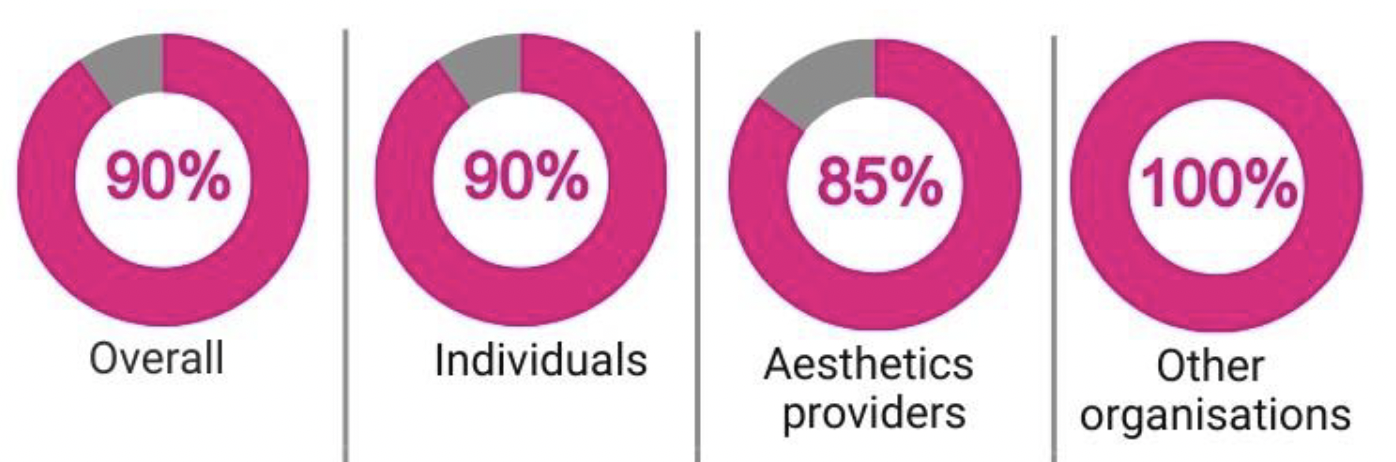
2.72 All organisational respondent groups except some aesthetics providers agreed with these proposals. For a detailed breakdown see Appendix Two.
Qualitative analysis
2.73 There were 267 written responses to this question. Most felt that pharmacists should be regulated by HIS, in the same way as other healthcare professionals. They were keen that the industry should be better regulated overall, and felt that it was necessary to regulate pharmacists, along with any other practitioners in the sector.
2.74 Around half of the respondents (including those both agreeing and disagreeing with the proposal) felt that pharmacists should not be able to offer these procedures. These respondents felt strongly that only healthcare professionals with practical clinical knowledge and experience of injecting (predominantly doctors, dentists and nurses) should be able to perform these procedures.
Respondents who agreed with the proposal
2.75 Most individual and organisational respondents agreed that pharmacists should be regulated, in line with other healthcare professionals.
"Yes this would align pharmacists with other health professionals providing similar services." Royal Pharmaceutical Society
"All practitioners should be regulated and be accountable, to maintain safety and standards." Individual
2.76 Most reiterated their earlier feelings that everyone performing these procedures should be regulated to the same level by HIS. They felt that there should be a clear, consistent set of standards that applied to all practitioners, healthcare professionals or otherwise, who wish to offer these procedures. Some respondents felt that it was an oversight not to have included pharmacists in the original legislation.
"Anyone providing elective medical aesthetics should be regulated by their regulatory body and by HIS. No exceptions." Individual
"Anyone carrying out these treatments should be regulated by the same body. It shouldn't be regulation for one and nothing for another." Elanic
2.77 One respondent reiterated their call for all practitioners in the sector, including pharmacists, to self-regulate through the Joint Council for Cosmetic Practitioners (JCCP). Two individual respondents who self-identified as pharmacists said that they would welcome more regulation and inspection.
2.78 Some respondents specified that pharmacists should not be performing non-surgical cosmetic procedures, as they did not have the requisite training or skills to inject into the head and neck. However they noted that if pharmacists were permitted to perform them, they should also be regulated by HIS, as other healthcare professionals are.
"Although pharmacists are well trained and highly knowledgeable about prescription medication, I do not believe that they should be carrying out cosmetic procedures, as this requires broad experience and knowledge of all disciplines of medicine." Individual
2.79 Some of these respondents indicated that they agreed with the proposals because they felt that if pharmacists, or any other non-medical practitioners were regulated by HIS, they would not fulfil the requirements, and would in effect be prevented from performing these procedures.
Respondents who disagreed with the proposal
2.80 Respondents who did not agree with the proposal were individuals or respondents from aesthetics providers. Many felt that pharmacists did not have the appropriate knowledge or skills to perform non-surgical cosmetic procedures. Whilst some respondents acknowledged that pharmacists would have a high level of knowledge relating to the medicines and products used for the procedures, they did not feel that pharmacists had the practical skills or training. As such, they did not feel pharmacists should offer these procedures, and so, did not need to be regulated.
"Pharmacists should not be carrying out non-surgical cosmetic procedures. This is out with the scope of their training and area of expertise." Individual
2.81 Most of these respondents reiterated their views that only doctors, dentists and nurses should perform these procedures. They noted that these healthcare professionals have the requisite skillset and access to specialist support, if required.
"Pharmacists are degree level trained clinicians who do not usually have any training in surgical procedures and are less likely to be practiced in the use of sharps and aseptic and clean techniques." Individual
2.82 Some respondents noted that pharmacists are already regulated by the General Pharmaceutical Council, and these regulations would be sufficient. And one respondent felt that pharmacists should only perform these procedures in a HIS regulated clinic, and so did not need any further regulation.
"I think that pharmacists have their own governing body that can manage their activities." Individual
2.83 One respondent suggested that the medical councils for each group of professionals (i.e. General Medical Council, Nursing and Midwifery Council, General Pharmaceutical Council) should be responsible for regulating cosmetic procedures conducted by their members. However another individual noted that the pharmacy regulator should not be responsible for this, as it did not have the experience or power to regulate these activities.
Wider concerns
2.84 A few individual respondents expressed concern over the commercialisation of regulation. They felt that regulatory bodies were focused on profit making, rather than patient safety. And they felt that the current system "over regulates the regulated", specifically in reference to healthcare professionals who are regulated by their own regulatory bodies and by HIS.
2.85 A few respondents also expressed concern that pharmacists could prescribe products for non-surgical cosmetic procedures to unregulated practitioners, who would then administer them. They felt that regulating pharmacists would prevent this practice. However, a few respondents also noted that guidance for pharmacists, through the General Pharmaceutical Council (GPhC), should ensure that they only offer prescribed products to healthcare professionals who are competent to administer safely. A few respondents felt that this potential loophole could be rectified with more regulation of pharmacists in the sector.
"Whilst pharmacists and pharmacy premises are regulated by the GPhC, on line prescribing services, or any independent clinic provided by a pharmacist, is not regulated by the GPhC. There is therefore currently a regulatory gap for independent healthcare services that use pharmacists to deliver the clinical care."
Healthcare Improvement Scotland
2.86 A few respondents felt there was a loophole in the regulation, which allowed healthcare professionals with NHS contracts to avoid regulation by HIS. Similarly, a few respondents noted that the current regulations also allow non-medical professionals to access prescribed products from prescribers who do not have to register with HIS. They felt that these issues should be addressed to ensure that all professionals performing these procedures were regulated equally.
Question 4: Do you have any other comments?
2.87 There were 244 written responses to this question. A total of 204 individuals and 40 organisations provided further comment.
2.88 Most respondents referenced or reiterated previous views that non-surgical cosmetic procedures should only be conducted by regulated healthcare professionals. Some reinforced their view that these procedures are medical interventions with the potential for serious complications. A few respondents noted that whilst pharmacists were explicitly included in this consultation, the regulation should apply to all healthcare professionals, and indeed, anyone wishing to offer these procedures.
2.89 The issues raised were similar to responses to the previous questions. The main concerns were around:
- patient safety;
- lack of accountability;
- comparisons with regulations in other countries; and
- the cost to the NHS.
2.90 Respondents also discussed:
- licensing;
- regulation of products used in non-surgical cosmetic procedures;
- the need to raise awareness; and
- support for the consultation.
2.91 A very small number of individuals reiterated their view that additional regulation was not required, and would place an unnecessary burden on practitioners.
Patient safety – physical and mental health
2.92 As mentioned throughout the consultation, respondents were primarily concerned with the safety of customers and patients. They felt that the procedures carried a high level of potential risk, and so should only be performed by qualified, regulated professionals.
2.93 Some respondents felt that a minimum age limit should be enforced to ensure that people under 18 could not access these procedures. One respondent noted that any future accreditation scheme should include a module on mental health and the protection of vulnerable adults who may seek to access non-surgical cosmetic procedures.
Accountability
2.94 Some respondents repeated their concerns that without regulation, practitioners of these procedures were not accountable for their actions. They felt that this left patients/customers in an unsafe position, particularly if complications arose.
Commercial aspects of the sector
2.95 Some respondents expanded on their views relating to the commercial nature of elective non-surgical cosmetic procedures.
2.96 Some respondents noted that there was a risk of exploitation of vulnerable people or people with mental health issues. They felt that regulation was important to ensure that people offering these procedures worked to a high standard with appropriate ethical guidelines and codes of conduct.
"Reform is long overdue to protect uninformed, vulnerable members of the public who will often opt for the cheaper treatments provided by untrained and unskilled non-professionals." Individual
2.97 Some respondents, individuals and some from aesthetic clinics, felt that regulation of healthcare professionals came at a substantial cost, which increases the cost for the consumer. The unregulated sector does not have these costs and can offer customers these procedures at a significantly lower cost. They felt that this discrepancy in price encouraged customers to opt for cheaper procedures from unregulated practitioners and put them at risk.
"Rather than care for the patient's health needs they are putting commercialism first." Association of Aesthetic Patient Protection Scotland
"My concern is that many of the public are unaware and will go to an injector without any research. Some looking for the cheaper treatment... The market for injectables is becoming saturated with too many non medics with not enough training. That is of huge concern for the British public, Beauty industry and medics." Individual
Regulations in other countries
2.98 Many respondents reiterated comments comparing the Scottish and UK regulations to other countries. They felt that the UK was unique in allowing the unregulated practice of non-surgical cosmetic procedures and felt that this should be rectified as soon as possible.
2.99 Many respondents expressed their hope that Scotland would "lead the way" with this regulation. And one organisation noted that if regulations were to change in Scotland, it would be important to introduce similar regulation in other parts of the UK to avoid cross-border tourism.
Licensing
2.100 Several respondents reiterated that they felt licensing should be part of wider training, regulations and enforcement of the regulation to maintain standards and protect patients/customers.
"Unless the licence is policed and training with a recognised body is required...a license will not improve standards." Individual
2.101 A few local authority respondents commented on the impact of licensing, noting that it would increase the demand on local authority teams. And two local authorities noted that it was important to set clear competency levels and criteria, so that practices could be adequately and consistently assessed.
Cost to the NHS
2.102 Some respondents emphasised the effect that the unregulated sector has on the NHS. They felt that there was an additional burden on the NHS from treating complications that arose from poor practice by unregulated practitioners.
Regulation of products as well as practice
2.103 A few respondents felt that the products used in non-surgical cosmetic procedures (i.e. the injectable products) should be regulated, as well as the practice itself. They expressed concerns over how and where products were sourced, and the fact that lack of regulation posed a risk to the public. A few respondents commented that remote prescribing practices posed a risk and were not appropriate for cosmetic procedures. And a few respondents also noted that all products used for non-surgical cosmetic procedures should be categorised as prescription only medicines, and so would be subject to more rigorous regulation. They felt that in order to ensure high standards and safety for the public, the products used, as well as the practice of the procedures should be regulated.
Raising awareness
2.104 Some respondents felt that it was important to raise awareness amongst the general public about these procedures. They felt that the current unregulated sector was difficult for potential customers to navigate, and that many people assumed that if a practitioner had access to needles and medical products, they were qualified to conduct the procedure. These respondents felt that a more regulated sector would raise awareness of the risks, limit the practice of these procedures to qualified and regulated healthcare professionals, and so would reduce the risk to the general public.
"We consider that it would be essential that any further regulation of non-surgical cosmetic procedures in Scotland as is being proposed needs to be accompanied by a high-profile public awareness campaign. We suggest that such a campaign is aimed both at ensuring those currently providing non-surgical cosmetic procedures are aware of the requirements to obtain a licence, and that the public are empowered to seek proof of such licence when engaging their services and to report non-compliance via appropriate and accessible channels." Law Society of Scotland
Support for the consultation
2.105 Some organisations and individuals noted their approval that a consultation into this issue was conducted. A few felt that this was a positive first step and welcomed more regulation of unregulated practices in the hair and beauty sector.
"This is a huge step in the right direction to making Aesthetics regulated on a level playing field. I'm pleased!" Individual
"With something as important as someone's face which forms part of their identity, it is good to see the government is taking action..." Individual
2.106 Several individual and organisational respondents felt that there were a range of other cosmetic procedures that do not involve injection but do pose a potential risk to the public, such as chemical peels and laser treatments.
2.107 Membership and representative organisations that represented non-medical professionals said that they were keen to work with Scottish Government to reach a solution that was proportionate and did not automatically exclude non-medical professionals from offering non-surgical cosmetic procedures, whist safeguarding the general public.
2.108 One organisation noted that it plans to launch an independent inspectorate which would voluntarily inspect member's premises. This organisation is a charity that represents the views of non-medical professionals in the aesthetics industry. It also has a professional code of conduct for its members. The organisation extended an offer to discuss the issues arising from this consultation further with Scottish Government through its Scottish members.