Non-surgical cosmetic procedures regulation: consultation analysis - final report
Independent analysis of the responses to our consultation on the regulation of non-surgical cosmetic procedures, which ran in 2020.
Executive summary
About this report
This report provides an analysis of responses to the Scottish Government consultation on the licensing and regulation of non-surgical cosmetic procedures.
As part of the Scottish Government's commitment to a safer Scotland it wants to ensure that anyone providing non-surgical cosmetic procedures does so safely and is competent and trained to do so. Non-surgical cosmetic procedures can include work such as dermal fillers, lip fillers and wrinkle smoothers. At this time there is no regulation to prevent or restrict individuals who are not healthcare professionals from carrying out such procedures.
Since the 2013 Keogh Review, which highlighted the lack of regulation and the potential risk of harm from non-surgical cosmetic procedures, the Scottish Government has taken steps to improve safety and regulation. In 2015 an expert interventions group was set up and from 2016, independent clinics run by certain healthcare professionals were brought within the regulation of Healthcare Improvement Scotland (HIS).
The consultation set out three questions around:
- The need for further regulation of non-surgical cosmetic procedures.
- The proposal that those who are not qualified healthcare professionals and who provide higher risk non-surgical cosmetic procedures that pierce or penetrate the skin are regulated by licence under Part 1 of the Civic Government (Scotland) Act 1982.
- The proposal to regulate independent health care services provided by registered pharmacy professionals, including cosmetic procedures, within an independent healthcare setting where these professionals are not providing pharmaceutical services under an NHS contract.
It also offered respondents the chance to share any further comments through an additional open question.
Overview of responses
The consultation received 459 responses. Most responses were received through Citizen Space, the online platform for consultations. After the removal or reconciliation of multiple responses, there were a total of 437 responses – 382 from individuals and 55 from organisations. There were 27 responses from independent aesthetics providers that conduct non-surgical cosmetic procedures, most of whom were registered with HIS, and 28 responses from other organisations including local authorities, membership/representative bodies, public or patient representative/advisory groups and regulatory bodies.
Findings
Further regulation of non-surgical cosmetic procedures
Respondents were asked to indicate through a yes/no/don't know question whether they agreed that further regulation was needed. A total of 434 out of 437 respondents answered the closed portion of the question. Almost all felt that there was a need for further regulation.
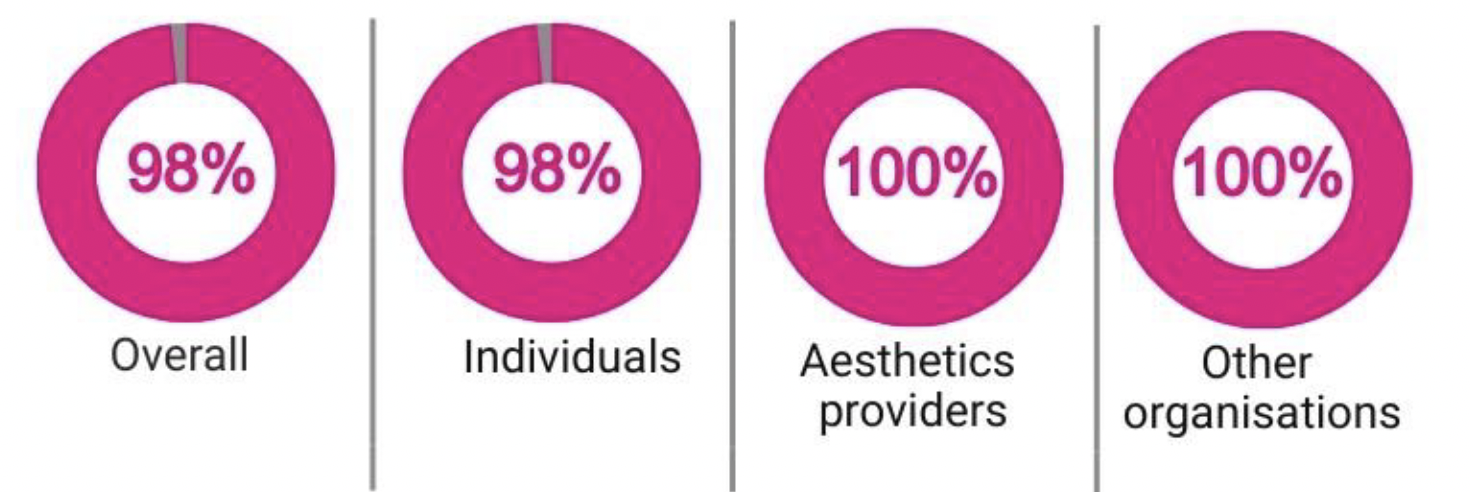
There were 343 written responses to the open part of this question. Almost all respondents across all categories felt that further regulation of non-surgical cosmetic procedures was needed.
Most respondents felt that non-surgical cosmetic procedures should be conducted by trained, qualified and regulated healthcare professionals.
Organisations which were regulatory bodies largely felt that more oversight was required, either through increased regulation or licensing. HIS which currently regulates independent clinics run by certain healthcare professionals, indicated that it would not be in favour of further regulation which would allow individuals other than healthcare professionals to perform non-surgical cosmetic procedures.
The main reason respondents called for increased regulation was to reduce the risk of physical and psychological harm to the public. In terms of physical harm, respondents were particularly concerned about the risk of errors that could cause burns, skin necrosis, blindness or cross-contamination of blood-borne viruses. They felt that unqualified and unregulated people did not have the knowledge or skills to rectify the complications. And a few believed that the NHS was currently, unfairly, bearing the burden of cost for treating these injuries. One respondent signposted towards evidence relating to the potential harm from cosmetic procedures, including non-surgical cosmetic procedures[1].
Some respondents observed that the medicines used to treat injuries or infections require a prescription, and so the procedures should only be delivered by those who are able to prescribe these products. Some respondents also felt that the products used in non-surgical cosmetic procedures, such as dermal fillers, should be prescription-only medicines.
Some respondents had concerns around the psychological impact of the procedures, and the need for a high standard of ethical practice. There were concerns that in an unregulated sector, the public was at risk of exploitation or negligence due to a lack of professional standards, oversight and accountability.
Respondents also commented on the inconsistency of the current system in which healthcare professionals require additional regulation to provide non-surgical cosmetic procedures, while individuals with no professional health qualifications do not. Many respondents felt that the current system overregulated healthcare professionals, who are already subject to regulation and oversight from their professional bodies. Some were frustrated at what they felt was a contradiction between high levels of regulation for healthcare professionals, and the lack of regulation for individuals with no professional health qualifications. Broadly, respondents felt that the level of regulation should be comparable between healthcare professionals and those who are not healthcare professionals, and that those who were unable to meet the professional standards should be prohibited from offering the procedures.
Broadly, the few respondents who did not believe that more regulation was necessary were of the view that individuals who were not healthcare professionals should not be allowed to offer non-surgical cosmetic procedures. As such, they felt there was no need for further regulation.
Throughout the consultation, some respondents compared the lack of regulation in Scotland and in the UK with the perceived clearer and stricter regulation in other developed countries.
A small number of respondents felt that individuals who were not healthcare professionals could be trained to an appropriate level. They felt that limiting the delivery of these procedures to healthcare professionals was unfair for beauticians; beauty therapists and the beauty industry.
Regulating practice by licence under Part 1 of the Civic Government (Scotland) Act 1982.
Respondents were asked if they agreed or disagreed with the proposal to regulate individuals with no professional health qualifications under the Civic Government (Scotland) Act 1982.
Almost two thirds of respondents (61%) agreed that individuals who are not qualified healthcare professionals should be licensed. Just over a third of respondents (36%) felt that they should not. A small proportion of respondents didn't know, or chose not to answer this question.
Responses varied between different groups. While just over half of aesthetics providers agreed, this increased to three quarters for other organisations.
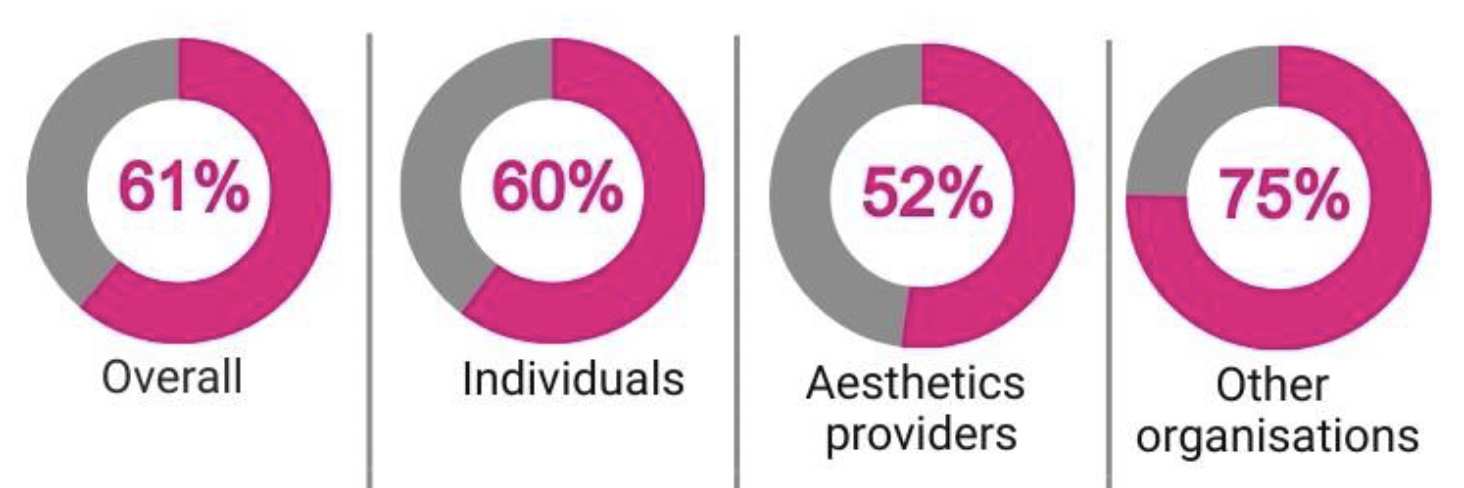
A total of 324 respondents provided further comment on their response. Respondents had mixed views. Most respondents who agreed with the proposal to license the practice of non-surgical cosmetic procedures felt that this was in line with their view that the unregulated parts of the sector needed more regulation.
Some of the respondents agreeing with the statement felt that licensing under the current framework was not enough, and that it should be accompanied with further regulation and requirements for training, indemnity insurance or infection control measures. And some highlighted the need for greater public awareness of the potential risks from these procedures.
Similarly, most respondents who disagreed with the proposal, did so because they felt that licensing alone was not enough. These respondents either felt that there needed to be much stricter regulation of the sector, or that these procedures should only be conducted by healthcare professionals, and so no further regulation was required.
One respondent who disagreed with the proposal felt that practitioners in the beauty industry did not feel that licensing was appropriate or necessary because they felt that beauticians had a good understanding of skincare.
Regulating independent health care services provided by registered pharmacy professionals
Respondents were asked if they agreed that services provided by pharmacists who undertake independent healthcare practices, including non-surgical cosmetic procedures, outwith the terms of an NHS contract should be regulated by HIS. All organisational respondent groups except aesthetics providers, agreed with these proposals.
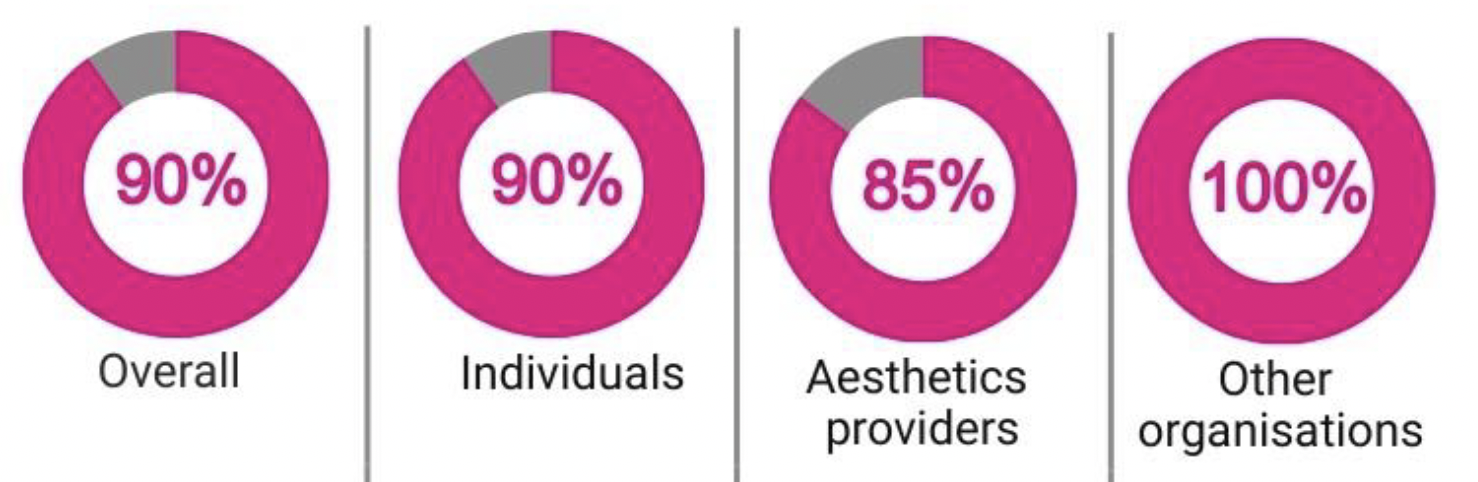
There were 267 written responses to this question. Broadly, respondents felt that pharmacists should be regulated by HIS, in the same way as other healthcare professionals. They were keen that the industry should be better regulated overall, and felt that it was necessary to regulate pharmacists, along with all other practitioners in the sector.
Around half of the respondents (of those agreeing and disagreeing with the statement) felt that pharmacists should not be able to offer these procedures. Their view was that pharmacists did not have the requisite knowledge or clinical skills to perform these procedures, or to manage any potential complications.