Time, Space, Compassion Three simple words, one big difference: Recommendations for improvements in suicidal crisis response
Recommendations for improvements in suicidal crisis response.
Background
In 2020, 805 lives in Scotland were lost to suicide and it is estimated that over the course of a lifetime 1 in 15 people will have attempted suicide[2], that's an estimated 368,500 people in Scotland.
For many of the real people behind these numbers there may well have been opportunities missed to reach out for help or to intervene to offer it. In healthcare settings, for example, data is collected on an individual's contacts with the service in the year prior to a death by suicide. Between 2011 & 2019[3], 77.3% of those who had died by suicide in Scotland had contact with at least one of nine healthcare services in the 12 months prior to their death. Nearly a third (31%) had been discharged from a general hospital setting in the 12 months before death and 30% had attended Accident and Emergency in the three months prior to their death (36% for females and 27% for males). A recent study[4] of middle-aged men who died by suicide in 2017 identified that 82% had been in contact with their GP at some time and 43% had been in recent contact with primary care services. Compared to the general population, people who died by suicide had more contact with the healthcare services where information was available.
This is a partial picture of opportunities for intervention or help-seeking; information is not available which would allow similar information to be provided for contact with non-statutory services, or for contact with social care, criminal justice, housing service and so on.
Figure 1 details a range of potential touchpoints for people in suicidal crisis to seek help or for an intervention to be made. These go far beyond the healthcare settings where data is available and demonstrate the range of potential opportunities where an effective approach to crisis response could be provided and be of benefit to those in need.
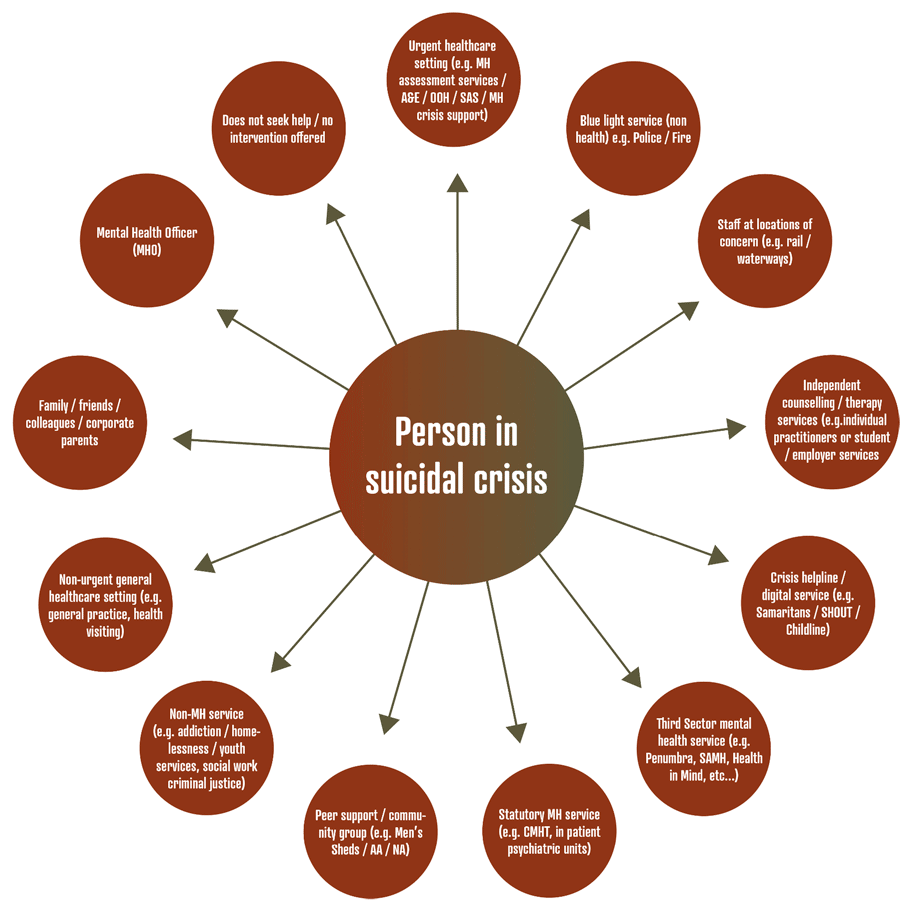
This report attempts to provide a unifying approach to improvement in suicidal crisis response which could apply across settings and services and support anyone who seeks help, and anyone who sees the opportunity to offer help.