Supporting children and young people experiencing a mental health crisis: framework
This Framework provides the principles of what cohesive and effective support for children and young people experiencing a mental health crisis should look like across Scotland.
The Role of the Workforce in Supporting Children and Young People Experiencing a Mental Health Crisis
Who is this document for?
This document is for practitioners and service leads involved in providing crisis support to children and young people, from initial compassionate responses, through to specialist services
What will this document support you to do?
This document will provide an overview of who has a role in providing support when a child or young person is experiencing a mental health crisis, and outlines the skills, national policies and guidance that are available to support in your practice.
When might this document be most helpful?
This document will be most helpful when designing new services, or when supporting current practitioners to feel more confident when providing support to children and young people experiencing a mental health crisis.
Who has a Role to Play in Assessing and Supporting Children and Young People in Crisis?
A key component of this Framework is that it is applicable to everyone who may find themselves engaging with a child or young person in crisis – no matter what the setting or context.
This means that, wherever children and young people present in crisis, they should encounter services which are able to respond to their needs and support them to access the right support, at the right time, underpinned by the GIRFEC approach.
It is also essential that these crisis responses are centred around the UNCRC (in particular Article 12[16]) to help us listen and respond to the needs of children, young people and the adults that support them regardless of where they present. This means an initial response which begins where the initial presentation was made, and is supported by strong multiagency communication and swift escalation to specialist services if required.
There are a variety of existing settings and services which are more specifically orientated towards supporting children and young people in crisis. These span:
- NHS and Health & Social Care support, such as CAMHS.
- Statutory services outside of health, such as social work and educational psychology.
- Third sector providers, including specialist crisis support and youth work services. These can be delivered in person, online, or by phone.
What Good Support Looks Like for Children and Young People in Crisis
There are a variety of key contact points during crisis. These range from initial support, to setting the conditions for longer-term follow up support. Practitioners should consider the following questions in relation to their practice (noting that sometimes these do not always play out in discrete separate stages).
Initial crisis presentation
- Which partners should be contacted/involved?
- What is the context of the crisis presentation?
- Child, family and carer involvement in decision making and planning (here and throughout)
- What immediate and longer term risks are present?
Supported handover
- How do partners work together to provide stabilisation support for children, young people and their families?
- How can effective, proportionate communication and clear lines for escalation of concerns be put in place?
Active crisis support
- What does an effective pathway/handover look like after the crisis has been stabilised?
- How can I manage this in a rights respecting manner (embedding Time Space Compassion)
Longer term follow up
- What does longer term support look like for children, young people and their wider family?
- What is the role of partners?
Some illustrative examples of what good support looks like can be found in the Case Studies Document.
Workforce Knowledge and Skills
There are three key national Knowledge and Skills Frameworks which relate closely to the skills and awareness required to put in place appropriate responses to children and young people experiencing a mental health crisis. Across the three frameworks they cover trauma informed responses, self-harm, suicide and children and young people’s mental health.
It is likely that practitioners supporting children and young people in crisis will be familiar with at least one of the three Knowledge and Skills Frameworks, and will undertake their role in line with the key elements described in each. This is applicable to all practitioners from schools to community settings to social work to CAMHS.
These frameworks are:
- Children and young people's mental health and wellbeing : a knowledge and skills framework for the Scottish workforce | Turas | Learn
- Mental Health Improvement & Suicide Prevention Framework: Scotland’s Knowledge and Skills Framework for Mental Health Improvement, Self-Harm and Suicide Prevention and,
- Transforming psychological trauma: a knowledge and skills framework for the Scottish workforce
Within each framework, the knowledge and skills required are set out into four different practice types: Informed, Skilled, Enhanced, Specialist.
Informed – Refers to the majority of universal provision. These are settings that may come into contact with children and young people experiencing a mental health crisis.
Skilled – Applies to settings or individuals who encounter crisis presentations more frequently or who aim to be crisis-informed.
Enhanced – Relevant for services that deal more directly with crisis management.
Specialist – Relevant to services managing complex or repeat crisis presentations.
The following diagram outlines what this looks like from the context of the different practice types laid out in these national Knowledge and Skills Frameworks:
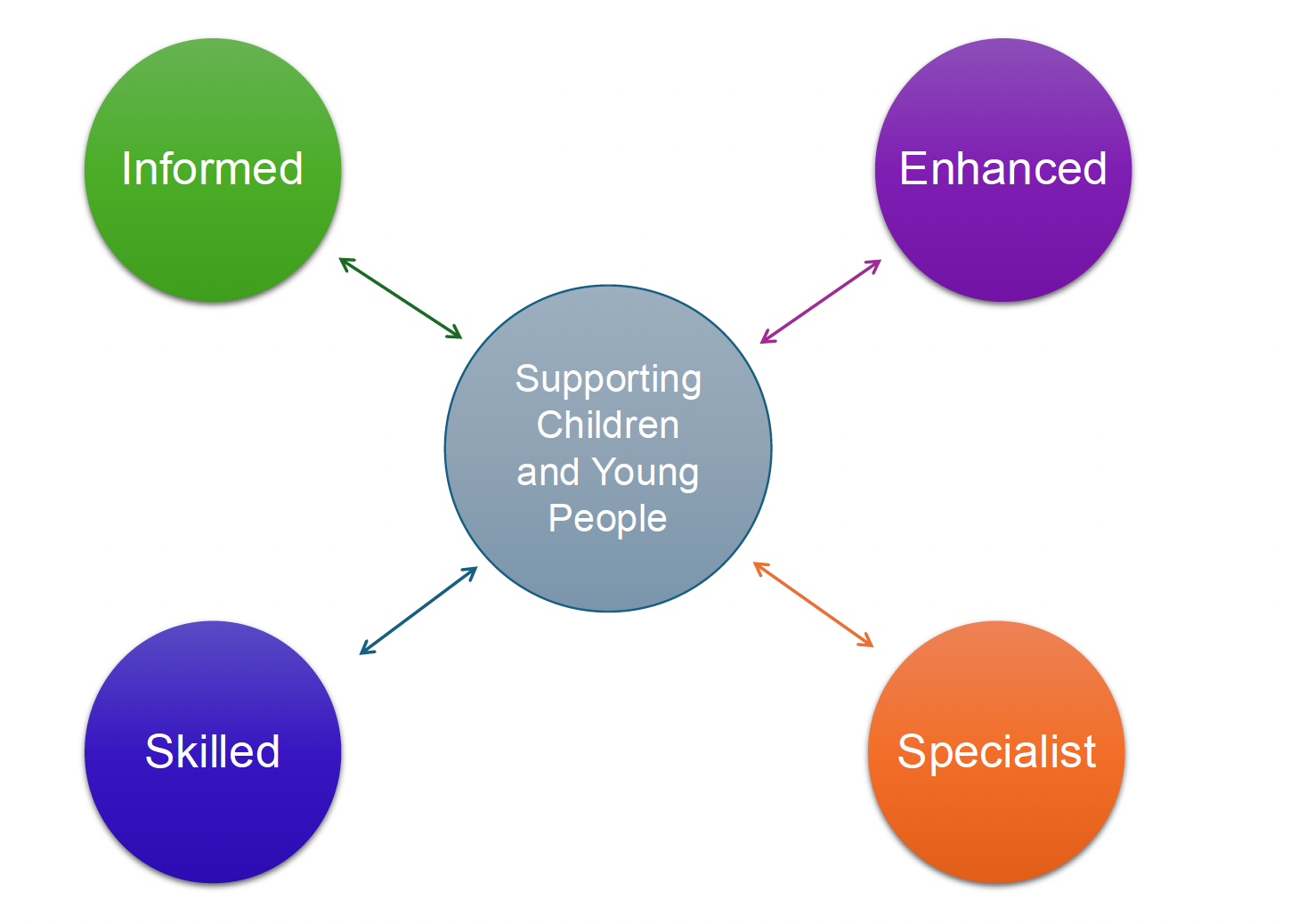
Informed
Type of response: Compassionate response. First point of crisis management. Additional support can be sought if needed.
Provided by:
- Parents, carers, friends, community
- Wider services e.g. schools and youth work
Skilled
Type of response: Initial crisis management and compassionate support. Follow up support if required.
Provided by:
- Wider services
Enhanced
Type of response: focused crisis support
Provided by:
- Dedicated crisis supports (statutory and third sector)
Specialist
Type of support: Crisis focussed support for children/young people with elevated need.
Provided by:
- Specialist services such as CAMHS
Appropriate supervision, support and risk management should be incorporated as required as part of this practice for both specialist and universal services. Services should consider the impact of their reach across different equalities groups and through an intersectional lens, with an active focus on rights based practice.
We recognise that the different practice types are not service dependent (across both specialist and universal services). Some practitioners may move between the different types depending on their experience, training and expertise. More information about the different practice types is outlined in the following table.
Informed
Core skills required across professionals and communities to support responses which are trauma informed and contribute to mental health improvement and the prevention/management of self-harm and suicide. This includes wider workforce whose roles may not centre around mental health or wellbeing.
This will also apply in a population wide setting, having relevance across all communities where there is the potential to provide initial support to a child or young person presenting in crisis. Additionally, support to wider family should be considered, recognising the emotional distress which is likely to occur.
Skilled
This practice type moves on to including staff who are in non-specialist roles but may be more likely to encounter a child or young person presenting in crisis. This includes roles where there is direct and/or substantial contact with people who may be at risk of mental ill health, self-harm or suicide.
Enhanced
The skills and knowledge at this level practice type around staff who are increasingly more likely to provide enhanced support around crisis responses, de-escalation and whose role involves facilitated handover to specialist crisis support if needed.
Specialist
This practice type is focussed around staff who have a specialist role in mental health, prevention/management of self-harm or suicide, or crisis management. The knowledge and skills at this level will be driven by the context of the organisation and practice recognising that crisis responses span across multiple specialist inputs.
Further resources to support learning and practice can be found in the Further Resources Document.
Delivery Landscape and Embedding National Policies and Resources
This Framework sits in the context of crisis across multiple systems and services, from non-specialist support to CAMHS. Although there are specifically crisis-orientated services and supports, we also know that management of crisis responses for children and young people can be part of a number of services. These services may not be focused around crisis, or even mental health, but are simply the first point of contact for children and young people seeking support.
GIRFEC is both an approach and framework used by services across Scotland to improve and uphold the wellbeing of children and their families. It underpins the delivery of high-quality universal and targeted support through a single, shared approach to planning across education, social work, and health and social care; and between public services, the third sector and community partners.
The National Practice Model within the GIRFEC approach brings together the My World Triangle, Resilience Matrix, eight wellbeing indicators and the four contexts for learning within Curriculum for Excellence, to support overall assessment. It provides practitioners, together with children, young people and the adults that support them, with a framework to structure and analyse information in a consistent way, holistically take account of a child or young person’s needs, identify their strengths and any challenges they face, and consider the most appropriate offer of timely support for the child or young person and the adults that support them.
The GIRFEC approach enables those supporting children and young people to fully participate in decisions which affect them across a continuum of need, from early help and support through to more intensive support. This provides a consistent approach during crisis.
Time Space Compassion is an approach and practical resource for anyone who wants to explore what part their team, organisation or community can play in preventing suicide and supporting people affected by suicide and self-harm.
Time Space Compassion provides an opportunity to apply a relational lens to the support and resources offered to children, young people and the adults that support them when experiencing a mental health crisis. Young People from the Suicide Prevention Youth Advisory Group have told us that “even when in crisis, they do not always want answers, they sometimes just want people to listen to them”. By using Time Space Compassion support can be provided in a way that children and young people feel they need.
Time
Time is focused around ensuring people feel heard and listened to. Focusing on helping people feel validated and understood as well as providing continuity across a person's journey.
Space
Space focuses on the accessibility of safe spaces, both in creating safe space where people are and in supporting people to reach other safe spaces. This might be in service settings, in communities or at home. And can be a virtual safe space as well as a physical one. It is also about offering emotional and psychological space to support people to make sense of crisis.
Compassion
Compassion is rooted in kindness, respect, and sensitivity, understanding how trauma and crisis can affect people’s behaviour. It involves identifying opportunities to offer direct support, or connect them to others who can provide support that reduces the drivers of distress in the person’s life. It recognises both the impact that people's previous experiences of stigma and discrimination can have on how they engage with services now. It also includes being clear on boundaries. And that compassion extends to an individual’s support network as well.
Time Space Compassion in Practice
Time
This might include: working to start a conversation well when someone may be experiencing suicidal crisis; actively developing and practising listening skills; and understanding the factors that might lead to suicidal thoughts and behaviours. And making sure that follow up is clear for the person you are supporting, so they understand what they can expect going forward without needing to retell their story unnecessarily.
Space
Being clear on what support is available, drawing on national guidance. It also means reaching into communities as well as opening your space up to them. Being alongside someone as they develop their safety plan and creating space to ask about and take action to help people feel safe both physically and emotionally whilst being clear on confidentiality processes and governance.
Compassion
Putting time into building connections, focussing on trauma informed support, and understanding that people might need different ways to express what they need. Setting clear expectations of what a person can expect and how their personal information will be managed also helps embed a compassionate response into the practicalities of support.
You can find more examples of Time Space Compassion in practice on Suicide Prevention Scotland’s website. Including examples from statutory providers and the third sector.
In the context of this Framework, these principles should be applied from two perspectives:
- To highlight how increasing awareness of the importance of applying the values in each of the dimensions of Time Space Compassion can improve service responses in relation to self-harm and suicidality in children and young people.
- To consider how the broader principles can support the Framework in all areas of crisis and distress, supporting empathic and respectful spaces for children and young people.
Together, these will support further discussion about how suicidality and self-harm do not only appear at times we traditionally describe as crisis, but can appear at different times, and with different presentations, across children and young peoples’ journeys.
Applying the principles of Time Space Compassion in relation to crisis for children and young people can support all professionals to:
- Increase awareness of what matters to children and young people
- Better understand crisis as a dynamic, complex interplay across multiple factors
- Formulate responses which are deeply rooted in compassion and care
Below are further national polices and resources that should be considered in relation to this Framework.
The One Good Adult Job Description resource provides a high-level description of the skills required by adults to help them develop safe, nurturing and encouraging relationships with children and young people. These relationships could help foster positive mental health and wellbeing in children and young people and provide support when they are experiencing a mental health crisis. There is a strong body of evidence and guidance, embedded in public health policy to support this approach.
Children’s Services Planning sets out what services, support and improvement activities will be delivered in each local area. Children’s services planning plays a crucial role in supporting a collaborative and whole systems approach to planning and delivery of supports and services for children, young people and their families. This includes supporting the mental wellbeing and health of children and young people, including when they are experiencing a mental health crisis.
The Child and Adolescent Mental Health Service (CAMHS) Specification outlines the provisions young people and their families can expect from the NHS. This includes providing or contributing to an all hours mental health crisis response service which covers advice/support to frontline services, assessment/intervention/treatment, and access to inpatient care. CAMHS crisis supports play a key role in ensuring safety and facilitating access to follow up care.
The National Neurodevelopmental Specification for Children and Young People: Principles and Standards of Care aims to ensure that children, young people, and the adults that support them, receive the supports and access to services that meet their needs at the earliest opportunity, based on the GIRFEC approach. For many children and young people, such support is likely to be community based but should also include appropriate involvement of health services, and should be quickly and easily accessible.
The Children and Young People’s Community Mental Health and Wellbeing Services and Supports Framework sets out the broad approach that should be taken in the provision of community-based mental health and wellbeing supports and services for children, young people and their families. Currently community-based services promote positive mental wellbeing and provide support for those children and young people experiencing emotional distress, however, we know that individuals in crisis may also present to these types of supports and services. It is therefore important that all types of children and young people’s services are aware of what they can do to care for a child or young person experiencing a mental health crisis, and have clear routes in place to escalate concerns where appropriate.
Through the Mental Health Unscheduled Care Network, Scottish Government has completed a national review of Psychiatric Emergency Plans (PEPs). PEPs are local protocols that guide the immediate response of services when a person is at risk of detention, ensuring timely, coordinated, and effective care. The review identified measures that support an improved and consistent response across Scotland and that strengthen how local services and emergency responders work together. The Scottish Government and its national partners are developing national guidance to support local services and emergency responders with implementing these measures.
The Multi-Agency Partnership Approach to Distress – Framework for Collaboration[17] sets out the principles for multi-agency collaboration when supporting people who are experiencing distress. This includes setting out the key components of an effective approach which includes local multi-agency forums, agreeing processes and pathways, and building strong relationships across key partners and stakeholders. This Framework mirrors and works in parallel with these aims.
The National Guidance for Child Protection in Scotland (updated in 2023) describes the responsibilities and expectations for all involved in protecting children and will support the care and protection of children.
School nurses play a vital role in supporting the health and emotional wellbeing of school aged children in Scotland. The role of a school nurse centres around 10 priority areas which can influence poor health in later life. These 10 priority areas include, but are not limited to, “emotional health and wellbeing”, “child protection”, “substance misuse” and “care experience”. The school nursing approach is holistic, with a strong focus on prevention, early intervention and support for the most vulnerable children and young people aged between five and nineteen years of age. They work within multi-disciplinary and multi-agency teams to support young people’s needs. Where more specialised care is required, school nurses can make referrals into other services, ensuring young people receive the correct care and support at the right time.
Educational Psychologists bring extensive experience in the practical application of psychology, the effective use of implementation approaches, and the facilitation of collaborative problem solving to address some of the most complex challenges faced by Education and Children’s Services. They are well placed to support improvement at the level of individual children, schools and early learning and childcare settings, local authorities, and the national system. Educational Psychologists work across the continuum of prevention, early intervention and crisis response, with a continual focus on prioritising prevention and early intervention. They aim to achieve this by supporting improvements in systems, processes, and staff knowledge and skills to meet the needs of learners, particularly those with additional support needs.
Allied Health Professionals (AHPs) play a huge role in the health and emotional wellbeing of children in Scotland. AHPs are generically trained to support children with both physical and emotional concerns. AHPs work in universal and specialist services including paediatric health services and CAMHS. They work as part of multi-agency teams to support children and young people to participate in and focus on living a life that they value, and can participate in.
The Framework should be considered alongside relevant legislation, policies, national health and well-being standards and health, and social care standards including:
- Core Mental Health Standards (2023)
- National Health and Wellbeing Outcomes Framework (2015)
- Health and Social Care Standards: My support, my life (2018)
- Secure care: pathway and standards (2020)
- National Specification for the Delivery of Psychological Therapies and Interventions in Scotland (2023)
Reducing Barriers, Upholding Rights and Supporting Equality Led Approaches
Crisis support should be accessible to a wide range of children and young people. We know that parity of provision does not equal parity of outcomes. With this in mind, it is important that supports and services take into account the following when considering how to support a child or young person in crisis:
- Ensuring a trauma informed approach is taken at multiple levels (with sensitivity to how trauma may be experienced and expressed differently by different groups.
- Embedding cultural sensitivity across all practice and materials (including awareness of how disability intersects with other aspects of identity such as race, gender, and socioeconomic status).
- Ensuring services are available and accessible to meet a wide variety of needs, for example, interpretation, or accessible formats such as Easy Read, British Sign Language (BSL), or Augmentative or Alternative Communication (AAC)[18].
In order to do this, services should:
- Be clear about confidentiality and governance, explaining what might have to be shared in ways that are understandable and accessible to the individual child or young person;
- Consider crisis management within their impact assessment activity;
- Have a clear understanding of the strengths and limitations of any services they support a child or young person to access especially in relation to accessibility, communication, and sensory needs, and;
- Ensure awareness and understanding across all staff around concepts such as minority stress[19], intersectionality, and ableism, acknowledging that this will be different across all children and young people.
Four UNCRC articles which are particularly relevant to upholding children’s rights in relation to management of mental health and wellbeing crisis points are:
- Non-discrimination (Article 2)
- Best interest of the child (Article 3)
- Right to life, survival and development (Article 6)
- Right to be heard (Article 12)
In relation to Article 12, the Lundy Model of Participation demonstrates how to give space for children and young people to share their views, support them to share their voice, ensure the audience is able to take on what is being communicated and through influence ensure that what has been shared is responded to.
Stigma continues to be a core issue to tackle across mental health awareness and in removing barriers to accessing support. Minority stress shows that individuals with protected characteristics can experience a compounding effect in relation to stigma, discrimination, inequality and wider social determinants.
When developing and delivering crisis supports and services in different areas (urban/rural/island areas), and across different populations, it will be crucial to do so with local demographics in mind, using local data and feedback, and aligning development with culturally competent and sensitive approaches and the Social Model of Disability.
This model shifts the focus away from individual impairments and instead emphasises the societal and environmental barriers that disable people. Applying this model means recognising, for example, that disabled children and young people are not inherently limited by their conditions, but by inaccessible systems, attitudes, and environments. Services must therefore be designed to remove these barriers - whether physical, communicative, attitudinal, or procedural - and promote full participation and dignity.
This includes ensuring that the needs of all children and young people are actively considered in service design, with attention to accessibility, communication needs, and inclusive engagement. An asset-based, rather than a deficit-based, approach to individual needs is encouraged. Areas will also need to consider how to form a locally appropriate balance between in-person and digital support, recognising that for some children and young people, digital options may enhance access, while for others, they may present additional barriers.
Considerations for Service Leads and Commissioners
Whilst we know that there are some places children and young people may present in crisis more often, there is a growing recognition that a key component of this centres around the person that the child or young people knows and trusts most. The resource One Good Adult[20] sets out the personal qualities an adult should embody, through a job description co-produced with children and young people.
Children’s Services Planning leadership[21] and arrangements are a core aspect of crisis prevention and management of crisis escalation for children, young people and the adults that support them. Specifically, whilst a preventative approach should always be sought where possible, there is the need to ensure that children and young people in crisis receive intensive support (aligned with Criteria 11 (Family Support)[22]) when necessary.
Service design, delivery and appraisal should work cohesively at both operational and strategic levels in order to ensure that the needs of children, young people and the adults that support them are being met in a way which is manageable, and is supported by current and future service infrastructure. In practice, this means ensuring that the principles of GIRFEC are central to any crisis response, and being responsive to the voices of children, young people, families and practitioners.
Understanding local population need is crucial to ensuring that crisis supports and services are fit for purpose locally. Ensuring that services are gathering and analysing data on crisis presentations and service user experience will support service leads and commissioners to understand the types of support required for their local populations.
To support the development of services, it will also be important to think about how support is delivered regionally, if populations or workforce are small. Scottish Government has emphasised the need for collaborative planning arrangements[23]. While Health Boards remain legally responsible for their statutory roles, the complexity of health services means that collaboration on a sub-national basis may be helpful to achieve better outcomes for children and young people experiencing a mental health crisis.
Rural and Island Areas
Access to mental health support varies across Scotland, with those living in our urban areas generally having greater access to a wider range of service options in comparison to those living in our more rural and island communities.
Although there are many aspects of rural and island life that can positively contribute to mental health and wellbeing, there are also unique stressors facing our rural and island communities. The Young Islanders Network have told us that these stressors can also be magnified when we look between island communities, with Scotland’s smaller islands sometimes facing further difficulties compared with larger islands.
A literature review by Heaton (2022) on mental health within island communities within Scotland showed a number of recurring themes[24],which included people in rural Scotland facing isolation, worsened by remoteness and experience stigma and fear as a result. These can be heightened by poor digital connectivity, inadequate transport links, and a lack of anonymity. There is also a higher likelihood of limited or delayed intervention and limited or unobtainable options due to workforce shortages.
As above, however, there are also benefits to living in Scotland’s rural and islands communities. We know that there are stronger community relationships and reduced exposure to noise and pollution. This coupled with direct access to green spaces and nature can result in lower rates of anxiety and depression. Recent data does show that mental wellbeing remains higher in rural areas in comparison to a general downward trend across Scotland[25]
As outlined previously, services may need to be delivered regionally rather than locally due to workforce and population need. Rural and island communities are already experienced in sharing knowledge, good practice, and skills across statutory and third sector services through the use of mechanisms such as Community Planning Partnerships.
Contact
Email: Sophie.Avery@gov.scot