Stroke Improvement Plan
The Stroke Improvement Plan sets out the priorities and actions to deliver improved prevention, treatment and care for all people in Scotland affected by stroke.
2. Stroke Care in Scotland
Background
19. Cerebrovascular Disease (CVD) is a condition that develops as a result of problems with the blood vessels supplying the brain. This can cause a stroke, a transient ischaemic attack (TIA) or a subarachnoid haemorrhage. Although CVD is largely a preventable disease, stroke remains the third biggest killer in Scotland and the leading cause of disability. Reducing the number of deaths from stroke has been a clinical priority for NHSScotland since the mid-1990s.
History and Progress
20. The stroke priorities in our Better Heart Disease and Stroke Care Action Plan (2009) have been the focus of improvement work that has been undertaken by the stroke community in Scotland since it was published.
21. The priorities for stroke have been continually updated informed by the progress that has been made. As priorities have been achieved, others have been added - either developing from existing priorities or identified through research.
22. One of the key priorities set out in the 2009 action plan was to establish stroke units in all hospitals in Scotland. Once the stroke units were in place the Admission HEAT target was developed and introduced from 1 April 2011:
'To improve stroke care, 90% of all patients admitted with a diagnosis of stroke will be admitted to a stroke unit on the day of admission, or the day following presentation by March 2013.'
23. The Scottish Stroke Care Audit (www.strokeaudit.scot.nhs.uk) shows that progress against this previous HEAT target continued to improve by 4% in 2013.
24. In order to continue to progress the work of the HEAT target Boards are now required to report against progress on the 'Stroke Care Bundle' in their Local Delivery Plans (LDPs). The development of the bundle was informed by the data collected on the updated Stroke Care Standards (2013) (Annex 2), which highlighted that although patients were getting access to a stroke unit, they were not necessarily receiving other key elements of stroke care. It includes the most important drivers for improving outcomes for people admitted to hospital with a stroke: stroke unit admission, CT brain scan, swallow screen test and aspirin delivered within the recommended time. This year's audit shows that NHSScotland has achieved a 10% improvement in 2013 in delivering the key elements of the Stroke Care Bundle.
25. The Stroke Care Bundle is reflected in the updated priorities 2 and 3 in this Plan and as stated above is the focus for performance improvement through its inclusion in NHS Boards LDPs for 2014/15.
26. Over the last 10 years the number of new cases of CVD in Scotland has decreased by 21% and mortality rates for CVD have fallen steadily - there are approximately 4,500 deaths in Scotland each year (4,479 people in 2012) where CVD is the underlying cause. The decrease for men (45.4%) has been greater than for women (39.2%), with a narrowing of the difference between the rates for men and women to almost zero. The percentage of people surviving 30 days or more following their first emergency admission to hospital with a stroke has improved slightly over the last 10 years from 80.2% in 2003/04 to 84.0% in 2012/13.
Path to New Priorities
27. To improve services effectively this Improvement Plan recognises the need to set clear aims that have been established through a number of sources - the Scottish Stroke Care Standards (2013), emerging priorities from the Better Heart Disease and Stroke Care Action Plan (2009), data collected through the Scottish Stroke Care Audit (SSCA), evidence of best practice and patient experience feedback.
28. The stroke community will continue to work together to ensure that quality improvement approaches are utilised locally to deliver priorities, and improvements in stroke care throughout Scotland.
29. This Plan sets out areas where improvement is most needed and identifies 8 priorities for stroke care, with aims and actions aligned with the Route Map to the 2020 Vision (Annex 1). These priorities have been developed to ensure improvement across the whole patient journey as detailed in the stroke care pathway (chapter 3).
30. Most importantly, implementation of the priorities will deliver better outcomes for people who have had a stroke using health and social care services through a quality improvement approach already widely used by the stroke community.
Engagement
31. In developing this Plan, we worked closely with the National Advisory Committee for Stroke (NACS), and its members who represent a range of stakeholders, both NHS and Third Sector. Patient experience is essential in developing services that are truly person-centred. Involving Patients is an important part of the stroke community at the local level through the Managed Clinical Network patient groups. All Stroke MCNs have active involvement from people who have had a stroke and their families.
32. Engagement is not a one-off process. We are committed to actively engaging with people during the period of life after stroke to ensure that the priorities identified within this aspect of care reflect their needs and experiences.
Mechanisms
33. By giving recognition to the importance of this Plan, Boards will ensure that every patient admitted with a stroke is given speedy access to specialist care. Boards are responsible for delivering stroke care services in Scotland via their stroke MCNs. This means in practice that they are responsible for continuous improvement against the priorities set out in this Plan; the Scottish Stroke Care Standards and the Stroke Care Bundle indicator as outlined in Local Delivery Plans - and so improving the quality of stroke care delivered across Scotland.
34. Implementing the priorities for stroke care has been and continues to be led by the Stroke MCNs, which exist in each of the territorial NHS Boards, with the National Advisory Committee for Stroke (NACS) overseeing and providing direction at a national level. The Scottish Stroke Improvement Team provides support and guidance to MCNs and NACS through the monitoring and interrogation of the data submitted to the Scottish Stoke Care Audit (SSCA). Where appropriate local small scale improvement data may also need to be collected to monitor any local projects that are being tried out and tested.
35. The Stroke Improvement Team will continue to work closely with, and support NACS and the stroke MCNs to ensure that the key priorities from this Plan, and the wider stroke work are implemented and monitored. Figure 1 below sets out the structure.
Figure 1
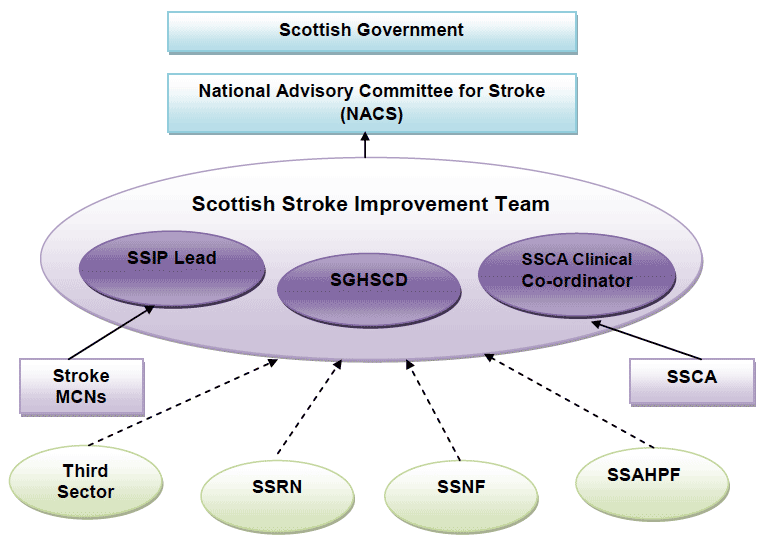
Key:
SSCA (Scottish Stroke Care Audit)
MCN (Managed Clinical Network)
SSRN (Scottish Stroke Research Network)
SSNF (Scottish Stroke Nurse Forum)
SSAHPF (Scottish Stroke Allied Health Professional Forum)
SSIP (Scottish Stroke Improvement Programme)
SGHSCD (Scottish Government Health and Social Care Directorate)
36. Stroke MCNs are encouraged to develop local improvement plans and good practice and share this nationally. To support continuous improvement, stroke MCNs can access real time SSCA data along with the exception reporting methodology introduced in 2012/13. By examining emerging trends and deviations in stroke care small tests of change can be identified to influence change leading to improvement in patient care.
37. The Scottish Stroke Improvement Team, along with the National Advisory Committee for Stroke, will continue to support Boards and the stroke community in delivering improvement aims, and to help share best practice.
38. MCNs should also continue to share best practice at the National Stroke MCN Managers Forum, chaired by the Stroke Improvement Lead. Local MCN patient and carer groups and the Stroke Voices Programme, both of which empower stroke patients to share their views and expectations both nationally and as part of local forums will also be able to contribute to this improvement work.
Contact
Email: Margaret Syme