Shaping the Future Together: Remote and Rural General Practice Working Group report
Report of the first year of work of the Remote and Rural General Practice Working Group.
PART ONE
Context: Challenges and Opportunities
The New GP Contract
The 2018 General Medical Services Contract was launched on 1 April 2018. It is the first GP Contract to be negotiated entirely within Scotland and was agreed jointly by the Scottish Government and the Scottish General Practitioners’ Committee (SGPC) of the British Medical Association (BMA), with Health Boards and Health and Social Care Partnerships supporting its implementation. This agreement is made up of a number of components: the existing GMS (17J) Regulations and PMS (17C) Agreement were refreshed and updated; a new formula, the Scottish Workload Formula (SWF), for determining national funding for each General Practice was introduced, and the Scottish Government began a three year period of transforming primary care which aims to improve access for patients, address health inequalities and improve population health including mental health, provide financial stability for GPs, and reduce GP workload through the expansion of the primary care multidisciplinary team.
For the Scottish Government, the new Contract is intended to support and enhance General Practice by improving the GP role, and reducing existing financial instability, risks, and inappropriate workload.
For GPs, the new Contract seeks to provide greater support in their daily clinical practice and to enhance the potential to attract and retain new recruits and existing experienced GPs. It recognises the expert medical generalist role of the GP, exercising leadership and support of colleagues working in MDTs and through GP Clusters.
To realise this, the Scottish Government and BMA agreed to six priority services to be commissioned by Health and Social Care Partnerships (HSCPs) and delivered by territorial Health Boards, to be implemented across a transformation period running from 1 April 2018 to 31 March 2021:
- Vaccination Transformation Programme – services to be Board run by 2021
- Pharmacotherapy - a pharmacotherapy service for the patients of every practice by 2021
- Community Treatment and Care Services – a service in every area, by 2021, starting with phlebotomy
- Urgent Care – a sustainable advanced practitioner service for urgent unscheduled care as part of a practice or cluster-based team by 2021
- Additional Professional Roles - the addition of members of MDT such as physiotherapists and mental health workers.
- Community Links Workers – non-clinical staff, totalling initially 250 nationally, providing support to patients who need it, starting in deprived areas.
This transformation programme is supported by increased investment to HSCPs to deliver this change, guided by a Memorandum of Understanding, agreed by the Scottish Government, BMA, Health Boards and HSCPs. The Memorandum of Understanding (MoU) sets out the seven key principles, in line with the guiding principles published in the national review of Out of Hours (OOH) services published in 2015: Pulling Together - Transforming Urgent Care Services for the People of Scotland, that should guide primary care redesign, namely that future services should be:
- safe for patients and staff
- person-centred
- equitable
- outcome focussed
- effective
- sustainable
- affordable
The BMA and Scottish Government agreed that a transitional period of three years would allow for these services to be safely and sustainably transferred in line with the MoU principles. The Scottish Government asked all 31 Health and Social Partnerships to work locally with Boards and their GP-Subcommittees to develop Primary Care Improvement Plans (PCIPs).
The Remote and Rural General Practice Group
The Scottish Government and BMA agreed to establish a Remote and Rural General Practice Working Group, to provide advice and give recommendations to the Scottish Government and the BMA on ways to ensure that the views of rural clinicians and communities are better recognised in primary care policy development. The Group was formed in June 2018, initially on a short life basis (The membership of the Group is listed in Annex A).
The original remit of the Group was to carry out the following activities:
- To engage with and seek the views of stakeholders involved in developing and implementing Primary Care Improvement Plans in rural areas, to gather learning of best practice, and emerging opportunities and challenges.
- Provide advice and support to HSCPs on the implementation of policies to deliver the 2018 GMS Contract and Memorandum of Understanding in remote and rural areas.
- Consider and provide advice and recommendations to the Scottish Government on any issues which are thought to affect / have been stated to affect the implementation of primary care redesign and Phase 1 in rural areas, in line with the development of HSCP’s Primary Care Improvement Plans and NHS Boards.
- Provide advice to the Scottish Government and Scottish General Practitioners Committee of the BMA on ways to ensure that remote and rural practices can fully benefit from the changes in the new 2018 GMS Contract.
The agreed output for the Group was to provide advice to the Scottish Government. Advice from the Group was also to inform negotiations taken forward by the Scottish Government and the BMA. The Group was also to provide a report to the Scottish Government to include a description of the Group’s activities, including stakeholder engagement, evidence gathering, and lessons learned, and a summary of its recommendations. Details of how the Group has provided advice under its terms of reference are set out in this report.
Rural Fund
The Scottish Government requested that the Group inform the investment of additional funding intended to provide support for remote and rural general practice and primary care. This funding should be deployed to fund projects that support implementation in remote and rural areas, including recruitment and retention initiatives. We have referred to elements of this fund throughout this report. A full breakdown of the allocated funds in 2018/19 and 2019/20 is included as Annex C to this report. The Rural Fund presently stands at an annual allocation of £2 million.
Rural Group Engagement
Group membership comprises a range of representatives including GPs and colleagues from remote and rural locations, representatives of Health Boards, HSCPs with rural populations, the Rural GP Association for Scotland (RGPAS), and the Patient Representative P3 Group of RCGP. A list of the Group’s members and observers is included as Annex A to this report.
As at December 2019, the Group has met on six occasions. We have sought to carry out an inclusive programme of engagement to hear directly from colleagues living and working in Scotland’s rural communities about how best to deliver on our remit. This programme includes interviews carried out with Group members and others, and a programme of visits to remote and rural communities across Scotland to meet and listen to GPs, Health Boards, HSCP teams and public representatives. We have also been working closely with the Scottish Government Primary Care team as they monitor the implementation of Primary Care Improvement Plans.
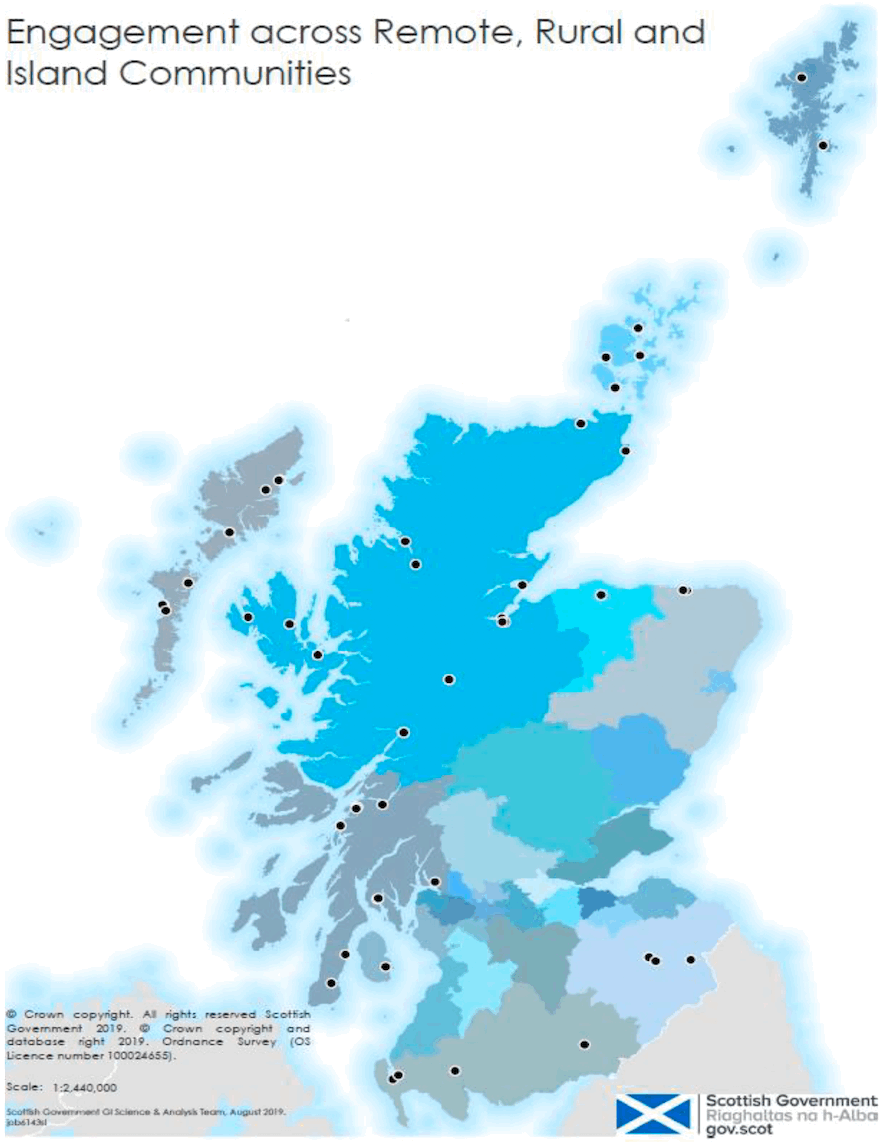
Figure 1 – Group Engagement Map – Each Point indicates an area where visits were made with primary care clinicians, other care providers and service planner
Defining Remote and Rural General Practice
The Group agreed that we would not seek to develop a new definition of ‘Remote and Rural’ for General Practice in Scotland and by extension create arbitrary lines that exclude the experience of some GPs and general practices from consideration under the Group’s remit. Instead, we have sought to understand how existing definitions are applied now, and how well those definitions are supporting rural communities. This operating principle reflects what is set out in the MoU, which emphasises that implementing the Contract is about delivering services that fit the needs of communities, as well as available workforce capacity and resources.
A range of definitions and criteria are available for different purposes. At national level definitions of rurality are used to inform the National Resource Allocation Committee (NRAC) Formula. Figure 2 shows the Scottish Urban / Rural Classification (SURC) 8-fold categories used to delineate ‘rural Scotland’ as covering the green and blue areas on the map. Together, this covers 70% of the land mass of Scotland[1]. 17% of Scottish General Practices are located in Rural Areas[2], serving 9% of Scottish patients. There are marked differences between rural communities in Scotland, but in general they have an older population. They have a smaller proportion of people living in the most deprived areas as defined by the Scottish Index of Multiple Deprivation but still have significant smaller pockets of deprivation.
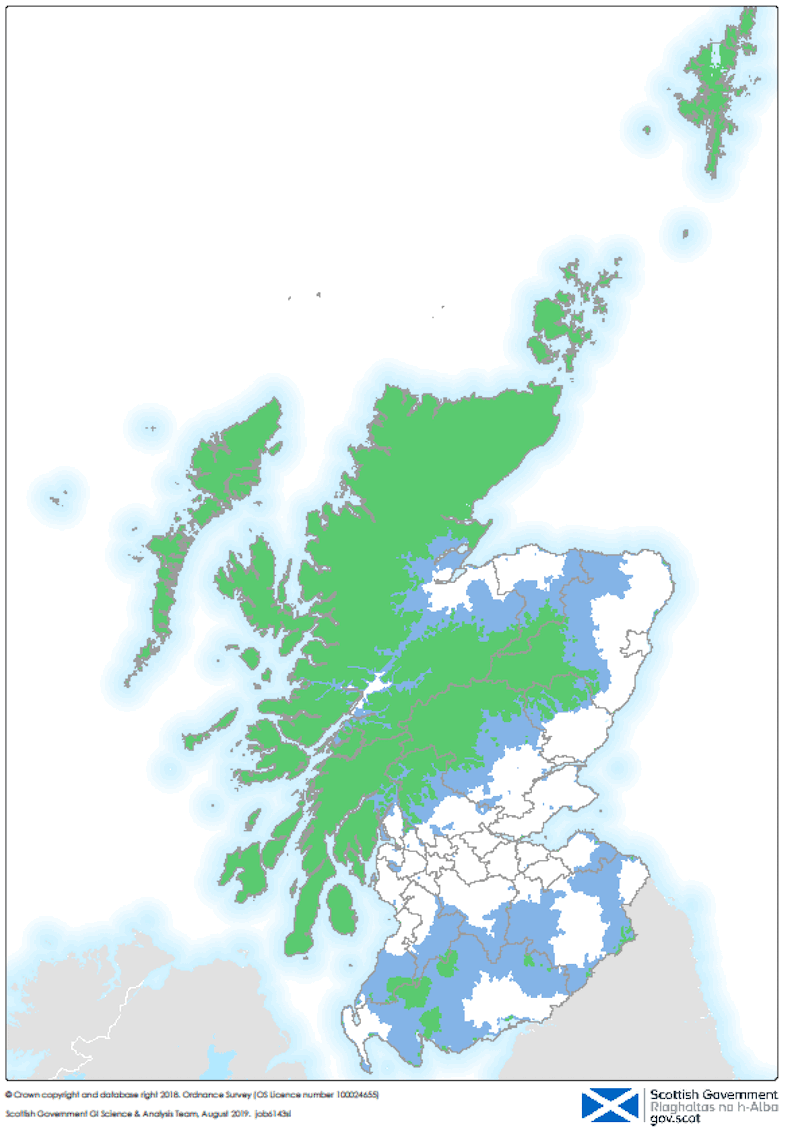
Figure 2 - Map of Rural Scotland using Scottish Urban / Rural Classification 8-fold categories. The Blue areas are ‘Remote’ and the Green areas ‘Very Remote’ using the 8-fold categories.
Practices in remote (blue) areas of the map are a 30 to 60 minute drive from a settlement of at least 10,000 people. Practices in remote small towns may often be as large as those in urban areas, but those in more rural areas are usually smaller.
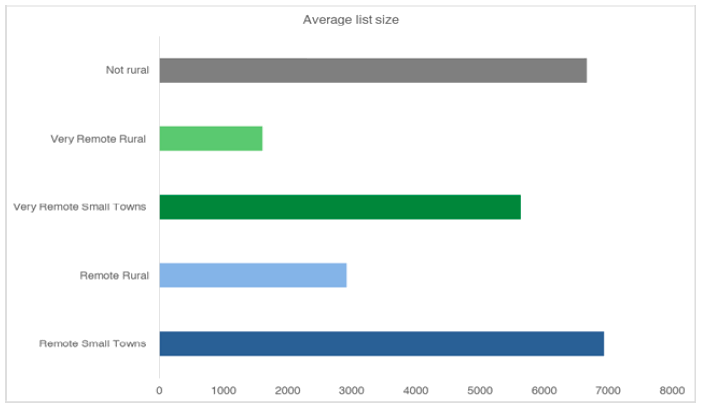
Figure 3 – Average List Size
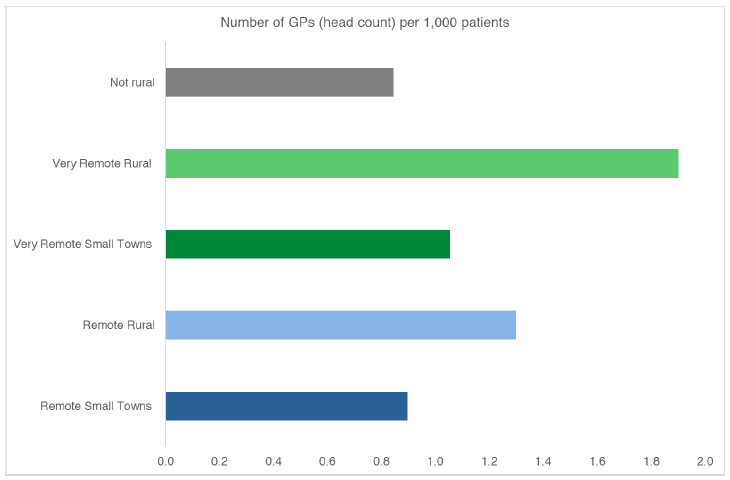
Figure 4 – Number of GPs (head count) per 1000 patients
As described in Figure 3 and Figure 4, practices in very remote (green) areas of the map are more than a 60 minute drive from a settlement of at least 10,000 people. They tend to have smaller list sizes and also have the highest number of GPs per 1,000 patients. They are much more likely to be dispensing practices. A greater proportion of these practices are managed by local health boards.
Although existing data helps us to describe broad characteristics of remote and rural GP practices, they cannot tell us about the experience of GPs and other clinicians delivering health care in those areas. They do not inform us about the effectiveness of the clinical teams working in and around rural practices, or their resilience to short and long-term workforce challenges. Through our engagement programme, and by considering the progress of Primary Care Improvement Plans, it also appears that there are GPs working in practices across Scotland outwith Figure 2 green or blue areas, who face similar challenges.
The Group engaged the Scottish School of Primary Care to provide a Briefing Paper examining the specific nature of descriptors and challenges of remote and rural general practice to allow us to better understand its distinct contributions and challenges. Professor John Gillies presented a draft version of this work (Rural General Practice in Scotland: Descriptors and Challenges) at the September 2019 meeting of the Group.
The SSPC report is based on extracts from GPs and NES rural fellows’ experience of rural general practice in Scotland. The evidence gathered indicated that defining aspects of rural general practice involve a greater need to provide emergency care of patients, addressing the health needs of geographically dispersed patient populations, 24 hour on-call responsibility and the importance of continuity of care. The SSPC Briefing Paper has since been published to support our work.
It has informed our programme of engagement, as well as the advice we have provided to the Scottish Government and BMA throughout our meetings. We have encouraged them to support HSCPs to work with their local partners and the public to determine population needs in Primary Care Improvement Plans.
Over the course of our engagement programme, we consistently heard that the delivery of healthcare to rural communities posed unique challenges and demanded tailored solutions. The lower density of population and the distances needed to travel within rural areas to receive and deliver care, and the distance of travel to secondary care facilities, require rural practitioners to acquire and maintain a broad range of skills and knowledge.
We have repeatedly heard that one size does not fit all, when considering future models of healthcare provision. Individual rural general practices have evolved to meet the specific needs of their communities, their geography and the impact on care delivery of adverse weather and transport issues. They normally provide a wider range of services to their patients, including intermediate care, that in an urban environment would be delivered by other clinical colleagues. They tend to live within the communities they serve and will often take on additional roles outside their immediate professional remit to address unmet need. The smallest of these teams in very rural or island areas are composed of a GP, nurse and receptionist. Small teams can be fragile whether a practice is urban or rural, and they depend on individuals and are vulnerable to illness or resignation. Attracting new GPs and clinicians to fill vacant posts can be particularly challenging in rural communities.
The distinctiveness of the rural GP role needs to be better understood within the profession, by associated clinical and administrative professionals and by Boards and HSCPs working to deliver healthcare services in rural areas. Over the course of our work we have listened to rural GPs describe their day-to-day role and how each can differ significantly from their peers in urban areas. We have also listened to their views about how the new Contract impacts on that role.
This remote and rural GP role is eloquently described by Dr Kirsty Brightwell GP, Western Isles, in her personal reflection: ‘Remote and Rural General Practice and the New GP Contract: a Crisis of Identity’. Dr Brightwell shared her reflection with the Group, which is reproduced in full in this report, with her kind permission, as Annex D.
The Remote and Rural GP Role
We heard from a range of individuals and groups that the expert medical generalist role described by the new GP Contract is already in place for GPs working in rural practices. This is largely due to smaller team limitations and access to clinical services dispersed across wider geographies. The strengths of these broad generalist teams are informed by research we commissioned from HIS, SSPC and Rossall Research & Consultancy and based on:
- An intimate knowledge of patients, their circumstances and needs in small and close knit remote and rural communities
- Working together closely with all team members
- Networking with geographically distant colleagues providing expert advice and support, when needed.
- Supporting each other in times of difficulty or crisis. This function is important in providing resilience to geographically isolated teams that work within the same communities that they and their families live in.
- Understanding factors which are unique to each setting, such as how service delivery can be affected by travel times, geography, weather and the limitations of available infrastructure.
This approach to care is not exclusive to rural practice. The Govan SHIP, a project involving four Deep End Practices in Glasgow, was built around a number of these principles and has produced evidence indicating the success of its approach. It represents a structure of care delivery and philosophy, rather than an urban/rural divide. It is important that the new Contract is flexible enough to incorporate these core values and philosophies.
The extended role of rural practice is predicated by the need to provide urgent care and the desire to reduce patient travel, especially in the elderly. It can perhaps be broadly categorised as follows:
- Emergency Care - The provision of lifesaving care to critically ill and injured patients in the community. In some very remote locations this care may need to be delivered continuously for several hours whilst waiting for patient evacuation to distant acute hospital services.
- Urgent Care - Care for conditions that are not life-threatening but require a response before the next routine care service is available, including: minor injuries, fractures, wounds requiring closure, acute illness and mental health crisis. Rural practitioners often deal with greater uncertainty and manage increased risk in the absence of more locally accessible diagnostic facilities, Accident and Emergency/Emergency Departments and acute (secondary) hospital care services.
- Intermediate Care - Provision of a wider range of care within the community (including community hospital care, where available), managing acute illness in the home and delivering ongoing complex out of hospital care (ideally with remote consultant support). Effective palliative and end of life care is of paramount importance. In remote and rural areas, delivery of palliative and end of life care is often constrained by distance (more lengthy home visit travel requirements) and may be compounded by adverse weather conditions.
- Additional Roles - The rural team may often take on additional or extended roles due to the absence of other professionals such as social workers, community psychiatric nurses, physiotherapists, occupational therapists, or carers.
Many GPs we spoke to, emphasised that remote and rural general practice offers enhanced opportunities for continuity of care and more intimate knowledge of patients, their families and life circumstances.
We heard significant concerns that the 2018 GP Contract did not fully appreciate the nature of the rural GP role and the differences to delivering general practice in rural communities. These concerns were amplified by members of the public through a petition to the Scottish Parliament’s Petitions Committee. The Committee considered the petition and have referred the matter on to the Health and Sport Committee for further discussion. There were concerns expressed that the requirements of the new Contract would be difficult, inefficient and expensive to implement, with the risk of providing inferior patient outcomes by disrupting continuity of care and fragmenting the service.
In late 2017, the Rural GP Association of Scotland (RGPAS) published Looking at the Right Map), a detailed response to the proposed new GP Contract. In that document RGPAS set out their agreement with the positive, aspirational aims of the Contract and broadly welcomed the multidisciplinary team approach. However, they also set out their concerns about the lack of detail to achieve those proposals, as well as how additional investment would address lack of training opportunities, recruitment and funding to realise transferred services. A key concern was their criticisms of the Scottish Workload Formula (SWF), which was used to determine revised payments to general practitioners in Scotland. The implications and limitations of the SWF were discussed in detail at the Petitions Committee of the Scottish Parliament on 9 May 2019.
Across our interviews and visits, there was clear recognition that the diversity and richness of general practice needs to be better recognised and rewarded. This is amplified in the briefing paper commissioned from the Scottish School of Primary Care and the report from Rossall Research & Consultancy.
An Income-Expenses Guarantee was introduced alongside the SWF formula to ensure no practice actually lost funding. However, it created the impression among some rural GPs that the distinctiveness of their role had not been appropriately recognised, and so was undervalued. RGPAS concluded from their analysis of the SWF that: ”The new formula simply fails to reflect the workload and services provided by rural GPs and their teams.” They felt undervalued because their impression of the SWF is that it failed to recognise the complexity and breadth of remote and rural general practice.
The Group also heard concerns that the Income and Expenses Guarantee was not seen as permanent, and that it could be changed or removed at some point in the future resulting in planning blight and a significant disruption to rural general practice stability. The Scottish Government and BMA have made clear that the Guarantee will remain in place until a new funding model is in place that either maintains or improves the current funding offer.
The joint Scottish Government-BMA negotiation team is working towards this as part of their plans for Phase 2 of the Contract. This will involve using income and expenses data gathered nationally to develop funding models that better reflects the true costs of delivering general practice services across Scotland. This is set out in the 2018 General Medical Service Contract in Scotland document:
“The guarantee to protect GP practice income and expenses in Phase 1 will continue until there is a proposal acceptable to the profession for the introduction of Phase 2. Future funding uplifts will apply to all GP practices’ share of the total, derived by the new formula during Phase 1, including the new income guarantee. Population increases will apply to the formula sum only.” (p21)
This assurance has been reiterated in communications by both the Scottish Government and BMA. However, while engaging with rural GPs, the Group has continued to hear of uncertainty around the nature and duration of that commitment.
The first recommendation of this report fully acknowledges these ongoing concerns and addresses them foursquare.
We note that RGPAS also recognised (in their report) that Deep End Practices working in urban areas of high deprivation expressed similar concerns about facing distinct challenges. While Deep End practices are outwith the scope of this report, we recognise that there is a shared issue here. Rural practices and those in the areas of highest deprivation face not only national challenges, but also ones that are distinct to the realities of delivering general practice in a unique setting.
Retention and Recruitment
Difficulties with recruitment and retention remain a significant challenge across Scotland and the whole of the UK - but can be worse in remote and rural communities. In some areas there is an over-reliance on expensive locums, placing an increased administrative burden on incumbent GPs. Locum availability, along with cost and the logistics of travel and accommodation, especially during tourist seasons, result in additional pressures. The extended role of rural practice, particularly the provision of pre-hospital emergency care, can be a significant barrier to both recruitment and obtaining locums. Accessible, affordable and relevant education, appropriate to the broader scope of care provided by rural practitioners, can be difficult to find and this can also be affected by the availability and cost of locum cover.
Throughout our engagement work, we heard a shared view of the importance of developing a clear vision of training, recruitment and retention of GPs and indeed of the wider MDT. This requires clear routes for training and continued professional development in the extended skills and knowledge required for rural practice throughout the “recruitment pipeline”, and strategies to support GPs and the MDT in their posts are essential. We commend and support the recent report, Undergraduate Medical Education in Scotland, led by Professor John Gillies, promoting greater use of general practice for undergraduate medical education, and in this context within remote and rural settings. We have extended this to include the training of other multidisciplinary team members, reflected in our tenth recommendation.
Service Redesign Challenges
Across the Primary Care Improvement Plans – and regardless of urban or rural composition - digital connectivity and suitable premises are regarded as key enablers to support service redesign:
- In rural areas, the availability of reliable digital connectivity enables high quality day to day delivery of care. Video conferencing allows rural GPs and other clinicians to develop mutually supportive networks with colleagues, and speak to patients, without incurring travel time to do so. It also supports innovative ways of delivering MDT input to rural practices, such as the work being done through NHS Near Me in NHS Highland. In our visits and engagement across rural communities we heard of how delivery challenges are intensified by poorly resourced IT provision and access to IT support.
- We frequently heard concerns that available premises cannot easily support an expanded MDT or make best use of opportunities to improve recruitment by offering spaces to train and mentor prospective GPs and other multidisciplinary clinicians. We saw examples of excellent facilities able to support these aspirations, but we also heard first hand of the barriers to realising them where GP premises are not able to achieve this. These concerns are reflected in our sixth, seventh and tenth recommendations.
Vaccination Transformation Programme (VTP) and Community Treatment and Care Services (CTAC)
Of the six key priorities set out in the Memorandum of Understanding, the greatest concerns raised across our engagement were around the Vaccination Transformation Programme, Community Treatment and Care (CTAC) Services, and Urgent Care Services.
Rural practices take pride in their high vaccination rates and see the delivery of readily accessible vaccinations as an opportunity for the team to hear, observe and gain a sense of family and continuity. They fear that this may be jeopardised by a visiting service, as is the chance of opportune vaccination during other interactions. Widespread concerns were expressed that moving to a non-practice employed/based team, could diminish accessibility and sustainability of service, ultimately adversely impacting on vaccination rates. The phrase: “If it’s not broken, why fix it?” was heard most often, with regard to this service, which is of paramount importance for primary prevention from infectious diseases. Despite this concern, we have seen some notable success in this area. NHS Western Isles has developed a successful model that uses Health Board employed teams (described in more detail later in this report). However, this is a pressing matter - we understand that a review of the governance and delivery of the Vaccination Transformation Programme is presently underway within Scottish Government.
In smaller populations the demand for individual elements of service is smaller and less predictable, creating challenges around service planning, sustainable resourcing, and resilience of the clinical team. The provision of CTAC services within rural practices helps support the employment of generalist nurses within the team. This nursing resource, well supported, can be utilised flexibly to deliver many aspects of care as required. An important element of general practice is the ability to respond to clinical need within an appropriate timeframe. This requires a team of sufficient capacity and capability. In rural practice, experienced staff with a broad skill set are required to meet the wide diversity of demand.
We often heard concerns raised that removing CTAC and urgent care services from practices could risk reducing the rationale for employing a suitably broad generalist team. As reflected in the RGPAS report: Looking at the Right Map, it is important to understand where rural economies of scale favour these service provision models.
Views were expressed that providing these services through HSCP/Board employed staff may reduce the ability of practices to respond to variable demand, would be more expensive than the existing model and would lead to services being less resilient where staff travelling further distances to work would be more vulnerable to travel disruption. There seemed to be an initial perception that the required model was of a centralised team, travelling out to rural areas, or requiring patients travelling to designated treatment rooms. We have seen from Primary Care Improvement Plans submitted by HSCPs that the ‘no one-size-fits-all’ approach encouraged by the Scottish Government and BMA has been largely embraced, although it is still early days. We are encouraged by the variety of flexible, innovative models deployed across the six service redesign work streams. As reflected in the recommendations of this report, the Group believes it is vital that those innovative models are supported and appropriately evaluated. Where successfully evaluated (see our twelfth recommendation), these should be promoted as examples for rural areas but potentially across the whole of Scottish general practice and primary care.
However there remains a widely held concern that these models are more vulnerable to impact from logistical issues, such as poor weather, absence within the team or from visiting colleagues. When this happens, the workload could revert to local practices that may lack team capacity and resources to deal with unscheduled increased demand on their time and resources. In addition, as we aim to reduce our impact on the environment and carbon footprint, serious consideration needs to be given to prevent increasing distances travelled by patients and staff.
Additional pharmacotherapy, physiotherapy, psychiatric nursing and community link worker services
The provision of additional professional roles; pharmacotherapy, physiotherapy, mental health workers and community link workers were in general welcomed by rural practices. Concerns were expressed regarding the ability to recruit them to rural areas and how services could be configured to maximally utilise the small allocation of time to individual practices.
Some GPs have expressed a strong desire to directly employ members of the MDT, which does not align with the GP Contract aim to improve stability in general practice by reducing the risks to partnerships related to staff employment. The motivation for wanting to employ staff is about seeking flexibility and the ability to coordinate staff working within the team to deliver care to the practice community. There is a fear that employment by the local HSCP or Health Board will result in staff being deployed over wider areas, threatening loss of close working relationships and continuity of care. This is an issue of trust and collaborative working. We have heard that in areas where GPs have well developed working relationships with HSCPs and Boards there are fewer problems in teams composed of individuals with different employers. Where relationships are historically less developed there is a sense of greater risk attached to service redesign. As we move forward, nurturing professional relationships and trust will be key, as will meaningful, co-production and engagement with local communities. This is reflected in the eighth and ninth recommendations in this report, and also the fourth recommendation to support dispensing practices.
Key Messages
- There is no single definition of a rural GP. It is a continuum of experience, influenced by many factors such as the needs of communities, the demands of geographies and infrastructure, and the surrounding network of clinical support. These factors are ever-evolving and yet determine the realities of the day-to-day job. To support implementation, national policy makers and regional and service planners should seek to listen, understand and respond to the experiences of the clinicians in these roles.
- The expert medical generalist role set out in the new GP Contract describes an approach that has been in place in rural communities since the Highlands and Islands Medical Service was established following the 1912 Dewar Report. This model contributed to the development of the UK National Health Service.
- In our early engagement there was a strong sense that the new Contract did not do enough to support GPs faced with the specific challenges characteristic of rural primary care. There was a clear sense that the exceptional opportunities for learning, innovation and progressive working in remote and rural areas had been overlooked.
- We believe that this perception is gradually changing over time as Primary Care Improvement Plans bring GPs together with HSCPs, Boards, as well as with patients and communities. This is happening alongside other developments such as the maturation of GP Clusters that also support co-produced, intelligence driven service planning. The intense collaboration and momentum required to deliver PCIPs must continue unabated. This needs to carry on after the threeyear transition period ends (end March 2021) and requires not only pragmatism but boldness and innovation. This holds true not just for remote and rural areas but for all of Scotland.

Meeting of Remote and Rural General Practice Workshop – September 2019
Contact
Email: joseph.mckeown@live.co.uk