Scottish Out-of-Hospital Cardiac Arrest data linkage project: 2015/16 – 2016/17 results
This report reviews the data from Scotland’s Strategy for Out-of-Hospital Cardiac Arrest from the years 2015-16 to the years 2016-17.
Out-of-Hospital Cardiac Arrest Analysis
1. Number of worked arrests: 'Worked arrests' are those OHCA non-traumatic OHCA in patients where resuscitation was attempted by the Scottish Ambulance Service. This number forms the denominator for all subsequent outcome calculations. There are a number of reasons why SAS may not attempt resuscitation including obvious death ( i.e. the patient shows obvious signs of having been dead for some time) and or the confirmation that this was not the patient's wish ( i.e. by the presence of a valid 'do not attempt CPR' order as part of an anticipatory care plan). Thresholds for attempting resuscitation have been demonstrated to vary between ambulance services [iii] which may make an important difference to survival figures quoted by different services. Figure 1 shows that the number of worked arrests per year in Scotland has gradually increased from 2692 cases in 2011/12 to 3455 in 2016/17. It is unclear why this should be the case. If the explanation for this increase is a significant lowering of the threshold for resuscitation we would expect this to manifest as a greater number of unsuccessful attempts and a reduction in return of spontaneous circulation ( ROSC) rates and survival to 30 days. This is not what the data shows (see below).
Figure 1: Number of worked arrests by year
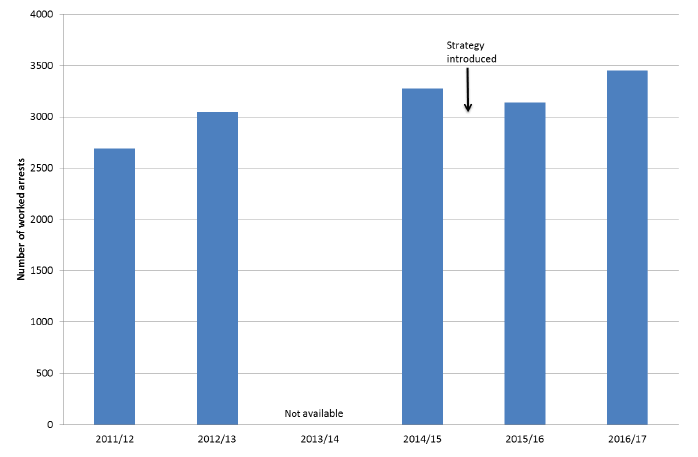
Figure 1: Chart shows the number of worked arrests reported by the Scottish Ambulance Service between 2011/12 and 2016/17. Data for 2013/14 is not currently available.
2. Data linkage rate: The set of worked arrests supplied by SAS were linked to patient records by determining the CHI for each OHCA where available. This was done by querying the Unscheduled Care Datamart followed by an additional bespoke probabilistic matching process. Further detail can be found in the report: Initial Results of the Scottish Out-of-Hospital Cardiac Arrest Data Linkage Project [iv] .
Figure 2 shows the proportion of 'worked arrest' incidents in the SAS dataset which were successfully linked, enabling patient survival to be determined. The linkage rate has steadily increased between 2011/12 and 2016/17 which is likely to represent an increase in the completeness of OHCA incident data recorded by SAS.
It is of note that in our analysis the worked arrest incidents which could not be linked have been treated as deaths. The basis for assuming that almost all of this group were pronounced dead at the scene of the OHCA incident is that arrival at an Emergency Department ( ED) would usually result in enough information added to the SAS record to allow linkage. We recognise that there will be a very small group which will remain unidentified in the ED, or who do not have a CHI number. This is a crucially important assumption, as our overall 'worked arrest' denominator for ROSC and survival calculations is not artificially reduced by ignoring this group of patients with incomplete data. It is not always clear that this approach is taken in other centres and can make international comparisons of survival difficult. In addition, the gradual change in linkage rate of our dataset with time makes year on year comparisons less straightforward but would not be expected to distort reported survival figures if our assumptions about the nature of these incidents holds.
Figure 2: Percentage of worked arrests linked
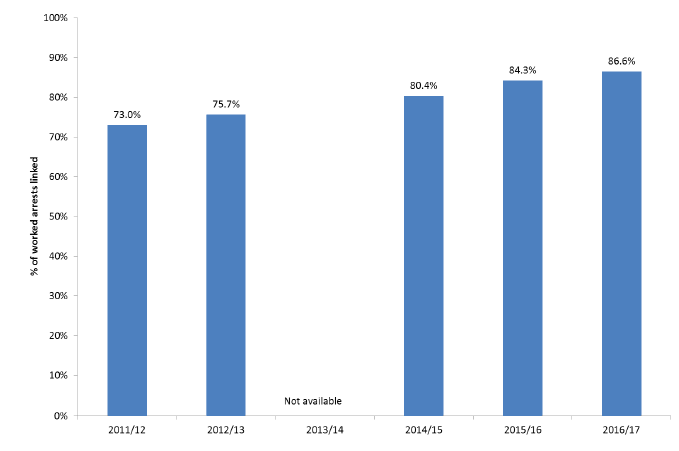
Figure 2: Chart showing the proportion of SAS OHCA incidents which were successfully linked to a CHI number between 2011/12 and 2016/17. Data for 2013/14 is not currently available.
3. Demographics - age, sex, SIMD and location.
There has been little change in the age of patients suffering OHCA over the whole period from 2011-2016/17. The mean age of patients in 2011-2014/15 was 67.7 years, and 66.8 years in 2015/16-2016/17. Figure 3 suggests that this small overall decrease in average age has been a result of a small reduction in the mean age of OHCA patients in the SIMD 1 and SIMD 2 quintiles. Similarly, the sex ratio of patients remains static at 62.2% males in 2011-2014/15, and 62.7% males in 2015/16-2016/17.
Figure 3: Average age of OHCA patients by quintile
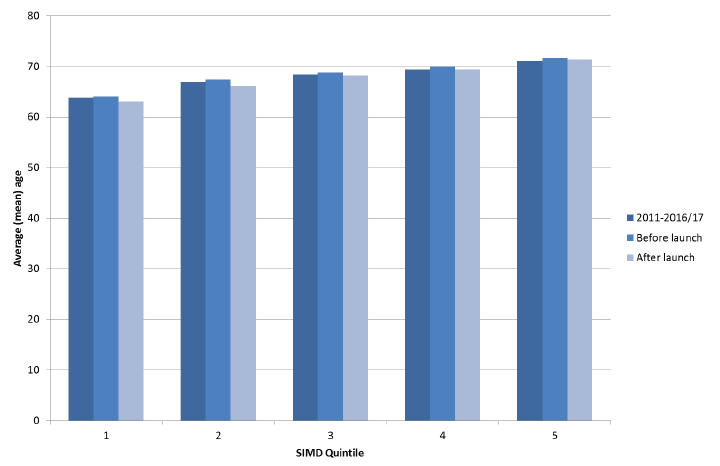
Figure 3 shows the (mean) average age of OHCA patients in each SIMD quintile for the whole dataset 2011-2016/17, before the strategy launch 2011/15 and after the launch 2015/17. Data for 2013/14 is not included. The Scottish Index of Multiple Deprivation ( SIMD) is a measure designed to identify area concentrations of multiple markers of deprivation. Scotland is divided into areas called 'datazones', each with a population of around 500 to 1,000 residents. The SIMD ranks the 6,505 datazones that cover Scotland from most deprived (ranked 1) to least deprived (ranked 6,505). These SIMD-ranked datazones can then be split into quintiles reflecting the most deprived 20% of the population ( SIMD1) up to the least deprived 20% ( SIMD5).
The proportion of OHCA in each of the SIMD quintiles appears to have shifted slightly (Figure 4), but the most deprived sectors of the community continue to be over-represented with SIMD 1 and 2 accounting for over half (50.7%) of all worked OHCA in 2016/17.
Figure 4: Proportion of OHCA patients in each SIMD quintile by year
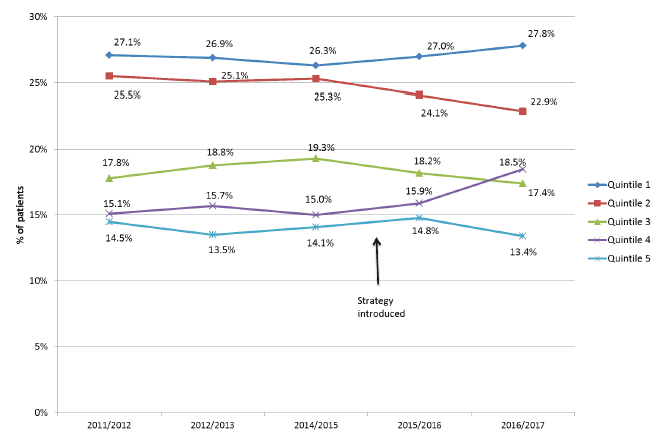
Figure 4 shows the percentage of patients suffering OCHA in each of the SIMD quintiles over time. Data for 2013/14 is not included. SIMD1 contains the most deprived 20% of the population up to SIMD5 which contains the least deprived 20% of the population.
With respect to type of location of OHCA the proportion of incidents occurring in an urban setting was 84% in 2015/16-2016/17, essentially unchanged from 85.2% in 2011-2014/15.
4. Bystander CPR
The rate of bystander CPR is a crucial metric for the impact of the strategy because its profound effect on likelihood of survival and its position early in the Chain of Survival. Data for 2011/12 to 2016/17 show a gradual increase in CPR rates, climbing more steeply after the launch of the Strategy (see Figure 5). Overall the rate has increased from an average of 41.3% in 2011-2014/15 to an average rate of 49.3% in 2015/16-2016/17.
This increase may be attributable to a range of interventions designed to increase public awareness of, and readiness to perform, CPR by the Save a Life for Scotland partners and others. There have also been changes in the method of bystander CPR data collection with new digital tablets rolled out to SAS in 2017. These changes to the method of data capture may also have affected the reported bystander CPR rate.
5. Survival
Survival to 30 days is perhaps the final arbiter of success of the Strategy. There is a trend towards increasing 30 day survival, but this is very much a 'lag' measure. Better survival is prefigured by a number of 'lead' measures which involve system optimisation across the Chain of Survival. All of the partners involved in implementing the Strategy have worked to improve the elements within their sphere of influence, some of which is captured in the Strategy first year review [v] .
Figure 5 shows the relationship between bystander CPR rates, initial resuscitation success indicated by return of spontaneous circulation ( ROSC = pulse on arrival in hospital) and survival at 30 days after OHCA. There is a trend towards an increase in ROSC and a parallel increase in 30 day survival. The mean survival in the five years before the launch of the strategy was 6.2%, in the two years after the launch of the Strategy it is 7.7%.
Figure 5: Bystander CPR, ROSC and 30 day survival, by year
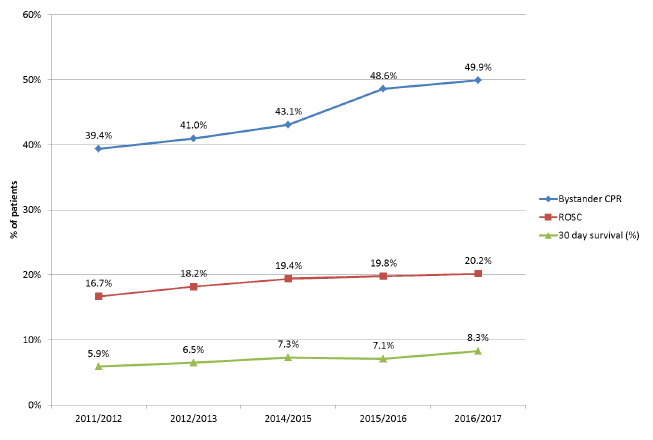
Figure 5 This chart shows the proportion of worked arrests receiving bystander CPR, rate of Return of Spontaneous Circulation ( ROSC = pulse on arrival in hospital) and survival at 30 days after OHCA. Data for 2013/14 is not shown.
Figure 6 is another visualistaion of the same 30 day survival data. The chart shows a comparison of the calculated 30 day survival after OHCA including all worked arrests and assuming that all unlinked incidents are deaths, compared to the survival rate recalculated after excluding unlinked worked arrests from the dataset. Including all worked arrests in the denominator gives a lower overall survival rate as expected (more deaths), but the two lines remain roughly parallel over time. The gradual narrowing of the gap between them represents the improvement in data linkage, reducing the numerical difference between the denominators in the two datasets. The actual 30-day survival percentage will lie between the two figures, but is probably closer to that reported based on all worked arrests (shown in the lighter line on the following chart).
Figure 6: 30 day survival after OHCA, linked versus all worked arrests as denominator
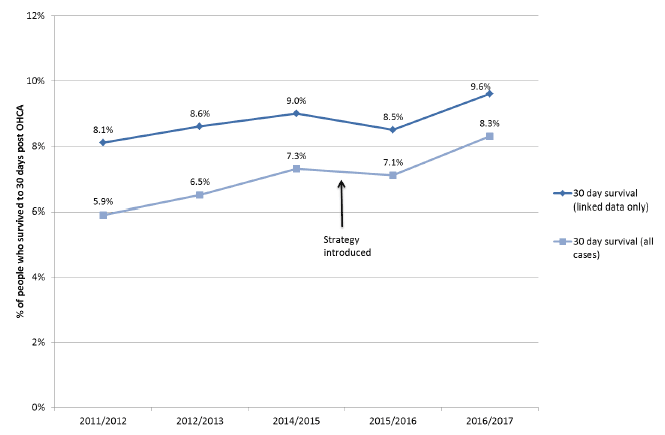
Figure 6 Shows 30 day survival after OHCA illustrating the impact of assuming that all unlinked worked arrests resulted in death (30 day survival (%) all), or disregarding all unlinked worked arrests (30 day survival (%) linked). Data for 2013/14 is not included.
6. Concluding remarks
This work updates our previous report on the initial results of the Scottish OHCA data linkage project. This analysis monitors progress against the OHCA Strategy. Further updates from the data linkage project will be published during the course of the strategy.