Scottish Mental Health Nursing Review
The Mental Health Nursing Review report aims to enhance the conditions for mental health nursing to flourish in Scotland, now and in the future. The report was co-developed by mental health nurses, students, academics, with support from carers and people accessing mental health nursing care.
5. Review Process
Human centred design principles underpinned the Review process. Drawing upon advice and experience offered through the Leadership Advisory Group, we adopted the Design Council’s double diamond model to shape the approach to the Review.
This involved four broad and dynamic phases for the Review – discover, define, design, and deliver. These phases were not linear. For example, discovery was a constant element throughout the work of the Review.
Discover: We explored and gathered insights from mental health nurses, students, people with lived experience and carers, through our National Mental Health Nursing Conversation and through engagement events and meetings. A literature review was undertaken to further explore the evidence base.
Define: We analysed the feedback we received and heard, both from the National Mental Health Nursing Conversation and the evidence base.
Develop: Working with our Advisory Groups and stakeholders, we explored the themes arising from our discovery and defining work and considered the emerging challenges, possible solutions and proposed actions in detail with a range of stakeholders.
Deliver: We co-developed our final report with our Advisory Groups and agreed co-delivery of our Review actions, through the Review Implementation Group.
5.1.1 Discovery
To ensure mental health nurses, people receiving mental health nursing support and carers were at the centre of the Review process, we established three Advisory Groups, who informed the direction and provided advice and contribution for the contents of the Review. The membership of each group is available at Annex A.
The Mental Health Nursing Review Steering Group, Chaired by Professor Alex McMahon CBE, consisted of a diverse range of stakeholders from a variety of sectors, including social care, education, as well as stakeholders holding professional leadership roles, and representatives from the lived experience and carer communities who have a particular focus on mental health recovery. The Group provided oversight and strategic advice throughout the Review process.
The Mental Health Nursing Review Leadership Advisory Group was chaired by Keith Russell, Nurse Director Mental Health and Learning Disabilities, NHS Tayside.
Membership of this group consisted of mental health nurse leaders from NHS, social care, and education settings. The group regularly advised on key questions, priorities, recommendations, and actions for the Review, and facilitated a range of engagement events with mental health nurses across Scotland, through the National Mental Health Conversation, as set out in Section 5.1.3.
The Mental Health Nursing Review Practitioner Reference Group, chaired by Dr Hamish Fulford, Consultant Nurse with the Forensic Network and State Hospital, consisted of practitioners from various levels of practice across a variety of sectors and settings, academics, and student mental health nurses. This group was established to further maximise the contribution and voice of mental health nursing in Scotland. The Practitioner Reference Group were key in compiling the evidence base for the review and to help increase understanding of the existing challenges and, consequently, ensure the proposition of informed, evidence-based solutions. The report can be found at The Mental Health Nurse; Exploring the Job, its Roles and Responsibilities: A National and International Scoping Literature Review.
In December 2024, the Leadership Advisory Group and Practitioner Reference Group combined to draw on the collective expertise of the groups in supporting the articulation and development of the key themes.
A dedicated webpage was established at the outset of the Review to enable effective cross sector stakeholder engagement and communication with the wider mental health nursing workforce and population. The webpage provided a concise overview of the Review, contact information and monthly updates were published on progress. The website also helped promote opportunities for mental health nurses and students to participate in the Review directly. It provided links for individuals to contribute to the National Mental Health Nursing Conversations and a platform to submit examples of positive and innovative practice.
Monthly Review updates were shared with the Scottish Government’s Mental Health
Directorate’s networks, via external newsletters. Colleagues across the Scottish Government and external partners were also encouraged to share with their own networks.
5.1.2 Perspectives on Mental Health Nursing
The Discovery phase of the Review was designed to gain different perspectives on mental health nursing. Hearing the views of people who have prior and current experience of care and support from mental health nurses was important, as were the views of carers.
Working with Voices of Experience (VOX) Scotland and Carers Trust Scotland, discussions were held with their respective stakeholder communities to seek views and feedback on the role and impacts of mental health nurses.
Voices of Experience (VOX) Scotland is a national membership-led charity run by people with lived experience, for people with lived experience of mental ill health.
VOX Scotland members were invited to reflect on their experiences of mental health nursing care and to identify what it was about that care that was most helpful for them. Members reported that the most helpful aspects included:
- Empathetic, compassionate, caring attitude and behaviour
- Trusting relationships built up and maintained through regular consistent contact
- Persistence in relating to and finding out what works for the person - flexibility
- An equal relationship based on humanity
- Taking the time to really talk and genuinely listen to the person
- Person-centred care, which enables personal agency.
“Need to recognise how important good nurses can be – inpatient and outpatient – you interact much more with nurses than you do with doctors, and it can make a vital impact on someone’s life – such an important profession that needs the right people doing the right things at the right time for those in their care.”
VOX Scotland Member
VOX members reported feeling uncertain about the role and scope of a mental health nurse in helping them and highlighted that this information was not communicated clearly or consistently. They felt that the role and duties were also unclear and inconsistent for the nurses themselves in some cases. Members reflected that it was important to take time to ensure understanding and awareness of what therapies or treatments mental health nurses offer in hospital and community settings.
Well managed and supported transitions in care were also highlighted as being important, particularly between hospital and the community, with some members reporting being discharged without safe or supported transitions back home. Mental health nurses can plan and support those transitions well, but there were concerns about how separated the roles of in-patient mental health nurses and community mental health nurses seem to be. The importance of continuity of care was also emphasised and some members described service pressures led to individuals being discharged, when they felt they needed ongoing support.
VOX Scotland members also emphasised that mental health nurses need to be neurodevelopmentally aware and informed in their practice, and that they should have access to the resources to help them achieve this. This is important as neurodevelopmental conditions are known to affect between 10 and 15% of the Scottish population, and that up to 70% of this group may seek mental health support (National Autism Implementation Team Adult Neurodevelopmental Pathways Report, 2023).
Members also spoke about less helpful and sometimes negative aspects of nursing care they had experienced. They explained how unhelpful attitudes and behaviours had affected them. This included issues such as a lack of empathy, respect, choice, flexibility, as well as wider systems issues relating to waiting times, staff shortages, increasing demand and stigma. Members emphasised the importance of truly trauma-informed care, with training being given consistently to mental health nurses to support this.
“There are those mental health nurses who care, those who just do the job, and those who wish you didn’t exist.”
VOX Scotland Member
VOX Scotland members also fed back on what would help ensure ’good’ mental health nursing in Scotland. This included:
1. A sustainable workforce strategy for mental health nurses where training, recruitment, and retention are considered carefully for all areas of Scotland, mindful of unique needs and wider issues such as housing and transport, cultural contexts, and representation.
2. Mental health nurses have good conditions, consistency, support for their own mental health and wellbeing, and access to professional development.
3. Recruitment makes the role of the nurse clear and has a focus on empathy and communication – how to talk to patients as equals.
4. Training for mental health nurses that includes input in some way from those with lived experience (both initial and ongoing). The training should include topics such as neurodivergence, suicide prevention, trauma-informed care, anti-racism, and unconscious bias training.
Participants in the work led by Carers Trust Scotland were asked to reflect on their roles as a carer for someone receiving, or who had previously received mental health nursing care. More specifically, they were asked: ‘When the person(s) you care for has experienced mental health nursing, what was it about that care which was most helpful for you?’
Respondents expressed the importance of mental health nurses being ‘carer aware.’ Having awareness of their role was seen as important for a few reasons:
- By having increased confidence, carers felt more comfortable to engage with staff, and in some cases, noted that their confidence in the service helped the person they care for have more confidence and willingness to accept treatment.
- Participants felt more included. When caring for someone with a mental health condition, many expressed how often they can feel ignored by services. This can be particularly frustrating when the carer feels as though they have vital information which can help inform professionals when diagnosing, or when there have been significant changes in the patient's behaviour.
- Having regular, consistent interaction with mental health nurses was agreed amongst most participants as being significantly helpful.
Other key aspects that unpaid carers mentioned as being most helpful included: clear communication of care plans shared with the patient and carer, having a kind, empathic attitude towards the patient and carer, and communicating any changes to care plans or treatment with advance notice, and trauma-informed practice.
Participants were also asked: ‘when the person(s) you care for has experienced mental health nursing, what was it about that care that was less helpful for you?’ Responses included:
- Some participants shared experiences of feeling dismissed and excluded when trying to share information regarding the ‘patient’ or when asking questions such as medication side-effects. In some examples, participants felt that they were labelled as “trouble” or “interfering,” rather than as someone helpful.
- Inconsistency in approach – care planning and staffing.
- Being unaware of changes in treatment/discharge and thus being less able to help as a carer.
- The importance of a patient’s right to confidentiality and having this right upheld was seen as significantly important by participants. However, many shared how confidentiality rules are often a barrier to access and can leave unpaid carers in the dark about diagnosis, changes in treatment and discharge information.
Carers Trust Scotland offered three recommendations from their engagement work:
1. All mental health nursing staff should receive ‘unpaid carer’ awareness training. Training should be co-designed and co-delivered by people with lived experience of receiving mental health care and unpaid carers. This should focus on how staff can engage and work in partnership with unpaid carers to truly see them as experts in experience. This will help meet the duties set out in the Carers (Scotland) Act 2016.
2. Adopt Triangle of Care practice across Scotland, where unpaid carers, those receiving care, services and mental health professionals work in equal partnership to promote safety, support recovery, and sustain wellbeing.
3. Financial investment into mental health services and support services, including local carer organisations, third sector organisations and advocacy services.
“The difference a good mental health nurse makes, who cares and asks you what you need, and wants to offer their skills is massive. It can change your life. That’s the power it can have – but they need to care, and they need to have the time, training and skills to let them do that.”
Carers Trust Member
5.1.3 Our National Mental Health Nursing Conversation
Hearing views and feedback from mental health nurses working at all levels and in all sectors in Scotland was an important principle of the Review and was the largest area of focus in the Discovery phase. Our National Mental Health Nursing Conversations asked:
1. How does it feel to be a mental health nurse working in Scotland right now?
2. What are your top three priority areas for the future of mental health nursing that you think are important for the Review to consider?
3. Mental health nurses have been described as ‘relational experts.’ In your role as a mental health nurse, who are you relating to and with, and what is the impact of those connections?
4. How might we work together as a mental health nursing community in Scotland to deliver the Review?
Over 1000 mental health nurses engaged with the national conversation from a broad range of practice areas. Both individual and group responses from engagement events were reviewed by Scottish Government data analysts and the findings are summarised below.
Mental health nurses reported a mix of positive and negative emotions regarding their roles. Factors such as challenging working conditions, high levels of clinical demand and high levels of administrative burden were identified as contributing to stress and pressure.
Concerns were raised about pay levels, pay parity and limited career progression opportunities. A loss of professional identity was also reported, with this being a common theme throughout the work of the Review. Despite this, mental health nurses expressed immense pride in their work and a strong drive and ambition to provide the best quality care possible.
“We are tired, but the job is rewarding, and you get a sense of satisfaction having made a difference to someone.”
“A professional vulnerability where I feel we have reached a point of such diversity in our role that we are really at risk of losing ourselves in terms of our professional identity. Because we now do so much, it feels like we’re losing our ability to articulate what it is that we actually do.”
“Overwhelming. Lots of demand and not enough supports available to help people in the way that they actually need.”
Priorities for the Review were thematically analysed and grouped into themes:
- Improved access to training/education/supervision
- Improve practice/patient care
- Improved conditions and pay
- Provide clarity on the role of mental health nurses
- Reduce administrative burden and improve systems
- Improve access to/contact with other services
Feedback highlighted that relational aspects of care were significant. While building therapeutic relationships with individuals is one of the central duties of a mental health nurse, they also reported a depth and breadth of multifaceted connections and relationships beyond the individual, that were an essential part of meeting the person’s needs.
Relational expertise emerged as a recurring theme throughout the Review, as a critical, impactful, and highly regarded part of the role, underpinned by highly developed communication skills.
Participants also expressed a commitment to work together to implement the findings of the Review, emphasising the importance of co-production, co-delivery, with collaboration and clear communication being essential in achieving this.
5.1.4 Reviewing the Evidence
In response to evidence and feedback obtained during the development of the
Workforce Action Plan and as part of the Discovery phase of the Review, the
Scottish Government funded See Me Scotland to undertake an Anti-Stigma and Discrimination Research Project. This project considered the extent to which stigma impacts mental health nurses and students experience, including in relation to recruitment and retention challenges. A summary of the research findings can be found at Section 6.3 and the full research paper is available at http://seemescotland.org/mentalhealthnursing.
To inform our evidence-base for the Review, an evidence search was undertaken by NES, based on themes offered by Scotland’s Mental Health Nurse Leads Group. This focused on the mental health nursing role and contribution to trauma informed practice, rights-based practice, and least restrictive practice.
The job, purpose and identity of mental health nursing was a recurring theme in the Discovery phase of the Review. To explore this, a wider literature scoping thematic review was undertaken by the Practitioner Reference Group, supported by colleagues from NHS 24, The State Hospital and NES. The aim of this literature review was to explore and synthesise existing research and literature to:
- Identify and describe the various roles of mental health nurses
- Understand the responsibilities and duties associated with mental health nursing
- Explore the job and work environment of mental health nurses • Identify gaps in the literature and suggest areas for future research.
The literature review presents a comprehensive scoping of the literature focused on the roles, responsibilities, and job experiences of mental health nurses, from a national and international perspective. The review synthesises findings across various themes, including competencies, education, training, professional identity, and challenges within mental health nursing and offers recommendations and implications for policy and practice. The literature review report will be published shortly.
The findings from the evidence base were key to finalising our priority themes and actions for the Review report.
5.1.5 Sharing Best Practice and Innovation
A request for submissions was issued, inviting mental health nurses to highlight best practice and innovative approaches that could be shared nationally and help inform the work of the Review. Numerous submissions were received, highlighting best practices and innovation driven and led by mental health nurses in Scotland, across various levels of practice within the health, social care, and education sectors.
The submissions highlighted in this report and at Annex C, provided examples of the crucial work mental health nurses do each day in practice. As part of this work, a series of podcasts have been developed to learn more about the nurse behind the submission, their leadership, and their drive to support best practice and change in mental health services in Scotland.
5.2 Definition and Development
After analysing the findings from the National Mental Health Nursing conversations, our Advisory Groups evaluated which findings fell within the scope of the Review and the synergies with other areas of work and policy. For example, as agreed in the terms of reference, the scope of the Review did not include pay, and matters such as administration burden which were being considered through the Nursing and Midwifery Taskforce. Therefore, these priorities from the National Conversations were not considered as part of this Review process.
Our Advisory Groups carefully considered the engagement findings, including examples of what is going well and where there is scope for improvement and advice from those with direct, frontline experience, people with lived and living experience of receiving mental health nursing support and carers. This helped us develop a clear understanding of where the challenges are and what changes are needed, within the remit of the Review. It was through this open and collaborative approach that led to the key themes and actions being identified and agreed, and which are set out in the sections below. These actions will help build on many of the positive examples reported and will help deliver the longer-term improvement that is needed to ensure our services, and our mental health nursing workforce are sustainable for the future.
The Getting it Right for Everyone model places the person at the centre of all the decision making that affects them, with a joined-up consistent approach, regardless of the support needed at any stage of life.
Based on this model, our Advisory Groups developed the illustration below to summarise key themes and priorities for achieving excellence in mental health nursing practice and to enhance support for the person receiving care. Our Advisory Groups agreed that the work of the Review, and work of mental health nurses should be guided by the Mental Health and Wellbeing Strategy and Workforce Action Plan visions and outcomes.
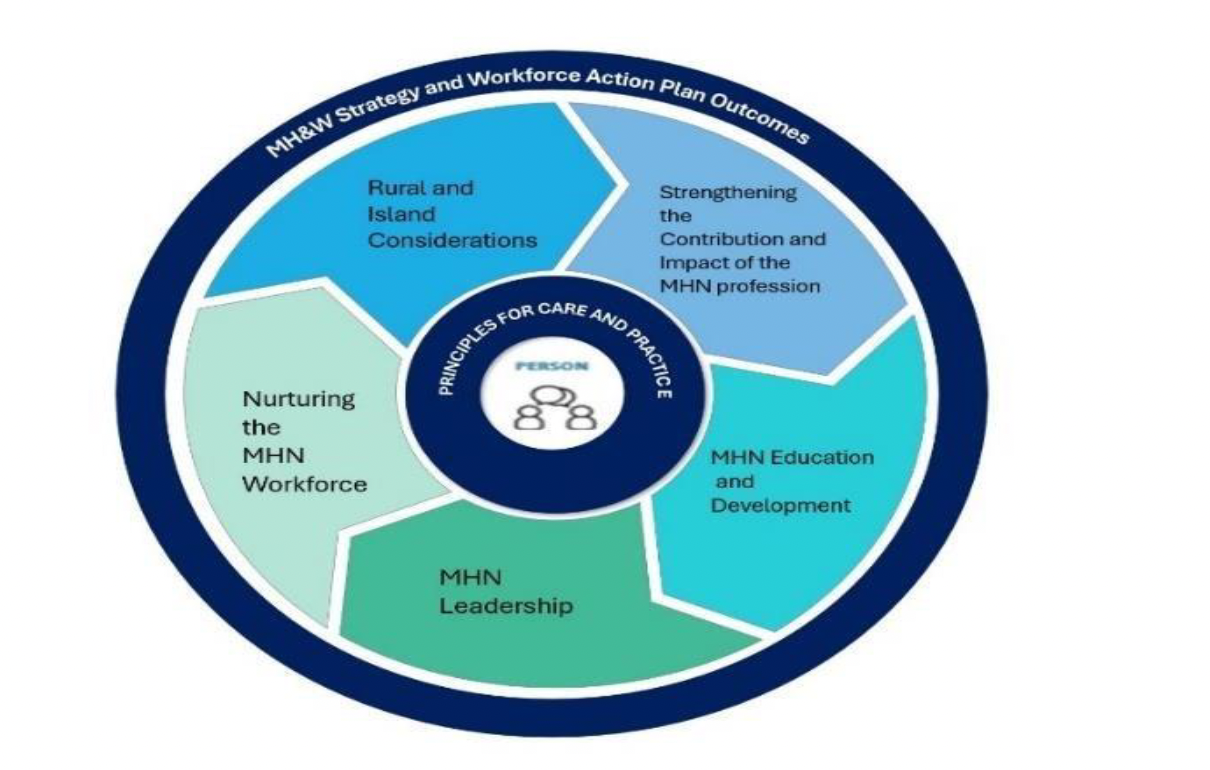
Alternative text: The person accessing care and support is at the centre of all decision making that affects them. Wrapped around the person, are core Principles for Care and Practice which help to ensure clarity of mental health nursing identity, purpose, and values.
To achieve sustainable change, we must be innovative and identify new ways of working collaboratively. Therefore, we will continue our human centred design approach and our commitment to co-design and co-delivery, as we move towards delivering the actions identified in the Review.
1. ACTION: We will establish an inclusive Mental Health Nursing Review Implementation Group to enable regular monitoring and evaluation of actions within the Review report and sharing of best practice with mental health nurses across a variety of roles and sectors and seeking advice from those with lived and living experience and carers.
To ensure constructive collaboration and sharing of best practice across sectors, the Mental Health Nursing Review Implementation Group will provide updates to both the Nursing and Midwifery Taskforce Ministerial Oversight Group, as well as the Mental Health and Wellbeing Leadership Board, as set out in Section 11.
Contact
Email: mhnursingreview@gov.scot