Scottish Inpatient Patient Experience Survey 2014 Volume 1: National Results
Results from the fourth Scottish Inpatient Patient Experience Survey.
6. Results - Patient Safety
Summary
- A range of new questions were introduced into this year's survey relating to issues around patient safety.
- The survey found that around one in five patients felt that they had experienced problems relating to their care such as infections, bed sores, reactions to medications, or falls.
- Seven per cent of patients felt that they had experienced clinical errors during their stay in hospital, the most common being 'delayed or incorrect test results'. The survey results further suggested that where clinical errors occurred, they were not always dealt with to patients' satisfaction. In over a third of instances (36%) patients reported that staff did not discuss the error with them and in 40% of cases patients were not happy with how the errors were dealt with.
- There was also a specific question relating to drips and needles in patients' veins. This found that one in four patients felt that either: their drip was not checked regularly enough; their drip was not changed when required; or their drip was not removed quickly enough.
Introduction
6.1. In line with the healthcare quality strategy outcome for NHS Scotland that "Healthcare is safe for every person, every time", new questions were included in order to provide an insight into the incidence and nature of events which impact upon patient safety.
6.2. Evidence from other sources shows that all health care workers make errors and that levels of harm are comparable in all settings[10]. The Scottish Patient Safety Programme[11] was launched in 2008 to improve the safety and reliability of healthcare and reduce harm, whenever care is delivered whether in acute or community settings. Within adult acute care, the programme is now organised into nine priority areas for improvement[12] which includes reducing: mortality and harm from sepsis, falls, pressure ulcers, medicine errors, catheter associated infections among other things.
6.3. A range of new questions were added to this year's survey to gather patients' perspectives on a number of issues relating to patient safety whilst in hospital:
- Situations where a patient's condition worsens
- Peripheral catheters
- Harm or injuries to patients such as infections, falls, and beds sores
- Clinical errors
Response to worsening of patients' condition.
6.4. Whilst in hospital it is not unknown for a patient's condition to deteriorate for various reasons. It is important that patients are appropriately monitored and that they get an effective, timely response. The recent SIGN recommendations on Care of deteriorating patients[13] set out the essential elements for prompt and reliable recognition of and appropriate response to deteriorating patients in Scotland's acute health care settings.
6.5. Almost a quarter of patients responding to the survey (24%) reported that they had experienced a worsening of their condition whilst in hospital.
6.6. In situations where patients felt that their condition had worsened, over one in ten (12%) of patients felt that the staff did not respond quickly. Whilst this does mean that in the vast majority of instances (88%) staff did respond quickly, a figure of over one in ten suggests that there is scope for improvement from the patient's perspective.
6.7. Some caution would be advised in interpreting these results. These figures relate to patients' own assessment of their condition and the survey does not provide information on to how serious the deterioration was, nor whether the situation experienced by the patient would constitute a deterioration in condition as judged by a health professional.
Peripheral catheters
6.8. New questions were added to this survey to investigate patients' views on how well drips or needles in the vein giving medicines or fluids (peripheral venous cannulas [PVCs]) were being maintained by medical staff. PVCs are widely used in a hospital setting: it has been estimated that as many as one in three hospital patients has one at any given time[14]. PVCs are associated with potential medical complications, such as bloodstream infections, which can have serious consequences.[15]
6.9. Observation and monitoring are crucial to identifying complications at an early stage. Both the Royal College of Nursing and Health Protection Scotland recommend that PVC sites are checked at least on a daily basis[16] . It is further recommended that the site is checked during injection of drugs, when IV fluid bags are changed and when drip flow rates are checked. PVCs should be removed as soon as they become clinically unnecessary.
6.10. In order to assess how well patients felt that their PVCs were maintained, survey respondents who had a PVC were asked whether it was checked regularly enough, whether it was changed when required, and whether it was removed quickly enough (Table 6).
6.11. The results showed that one in four patients felt that their PVCs were not being maintained appropriately. A quarter of patients (25%) felt that at least one of the listed actions were not happening. The most common report was that patients felt that their drip was not checked regularly enough.
Table 6 peripheral venous cannulas [PVCs]
| Statement | % |
|---|---|
| Not checked regularly enough | 12 |
| Not changed when required | 8 |
| Not removed quickly enough | 10 |
| At least one of the above | 25 |
Harm or injuries to patients
6.12. New questions were also added to the survey this year regarding problems that may have arisen during, or as a result of, the patient's hospital stay. Patients were asked to indicate whether they had experienced any of the following:
- Infection (e.g. urinary tract infection, surgical wound infection, MRSA, CDiff etc.)
- Blood poisoning/sepsis
- Blood clot (e.g. Deep Vein Thrombosis [DVT], Embolism)
- Bed sore (pressure sore)
- Injury from falling over
- Bad reaction to medication
- Complication from surgery
- Any other problems
6.13. One in five survey respondents (19%) had experienced at least one of the problems listed. By far the most common was an infection, with 8% of all survey respondents experiencing an infection during their inpatient stay (Table 7).
6.14. Four per cent of respondents selected the option 'any other problems' . As a result it is not clear what problem they will have been considering when responding to this question.
| Harm or injuries | % |
|---|---|
| Infection | 8 |
| Blood poisoning/sepsis | 1 |
| Blood clot | 1 |
| Bed sore (pressure sore) | 2 |
| Injury from falling over | 1 |
| Bad reaction to medication | 4 |
| Complication from surgery | 3 |
| Any other problems | 4 |
| At least one of the above | 19 |
6.15. The Patient Rights Act 2011 includes the principle that "no avoidable harm or injury is to be caused to the patient by the healthcare provided"[17]. The question of whether any harm was avoidable is complex and needs to be considered in local review on an individual basis. The above information does not distinguish harms that might have been avoidable.
Clinical errors
6.16. For the first time survey respondents were also asked whether they had experienced any of five listed clinical errors.
- Incorrect diagnosis
- Wrong treatment
- Incorrect medicines
- Incorrect doses of medicines
- Delayed or incorrect test results
6.17. Seven per cent of patients responding to the survey felt that they had experienced at least one of the events listed. The most common of these was 'delayed or incorrect test results', which was experienced by 3% of patients.
| Clinical error | % |
|---|---|
| Incorrect diagnosis | 2 |
| Wrong treatment | 1 |
| Incorrect medicines | 2 |
| Incorrect doses of medicines | 2 |
| Delayed or incorrect test results | 3 |
| At least one of the above | 7 |
Responding to clinical errors
6.18. An important aspect of reducing and managing risk is to ensure that when mistakes do occur they are acknowledged and dealt with. The Learning from adverse events through reporting and review: A national framework for NHSScotland approach[18] stressed that the needs of the patient and their family should be addressed as a priority when something has gone wrong. This includes being open and honest about what has happened and communicating about any reviews or improvement plans.
6.19. Where survey respondents felt that any of the five errors above occurred during their care, they were asked whether staff had discussed the error with them.
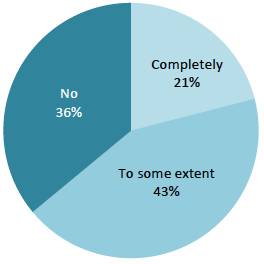
6.20. In over a third of instances (36%) patients reported that staff did not discuss the error with them. A further 43% of patients had the event discussed with them 'to some extent' and 21% had the issue discussed with the 'completely'. These results suggest that, when mistakes do errors do occur, more could be done to discuss the situation with the patient.
Chart 7 Did a member of staff discuss the error with you?
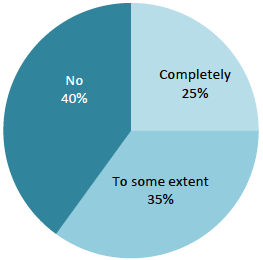
6.21. Patients were also asked whether they were satisfied with how the events had been dealt with. Fully 40% of patients indicated that they were not satisfied, a further 35% indicated that they were satisfied 'to some extent', and a quarter were 'completely' satisfied.
Chart 8 Were you happy with how the error was dealt with?
Contact
Email: Sophie David