Health and Social Care: medium term financial framework
This Framework supports the Health and Social Care Delivery Plan and sets out in more detail the potential approach and type of initiatives required to ensure continued delivery of a financially balanced and sustainable Health and Social Care system.
Reforming Health and Social Care
Introduction
The actions required to address the challenges facing the health and social care system in Scotland are set out in the Health and Social Care Delivery Plan. The Delivery Plan brings together earlier reform programmes – such as the National Clinical Strategy, and other reform initiatives – into a framework that is designed to provide focus and acceleration for reform. Its actions are designed to set us on the right course to address the financial pressures facing the health and social care sector by reforming the way care is delivered, as well as reshaping the future balance of expenditure across care settings.
This framework has been developed to support plans at a local, regional and national level in identifying the financial impact of various policy initiatives and how they will contribute to system sustainability. The analysis provides a high level indication of the scale and type of factors that will help reform the health and social care system. Further work will be carried out at a local and regional level to develop these into more detailed delivery plans.
Reform Activities
Five specific areas of activity have been modelled as contributing to the reform of health and social care delivery across Scotland and these are summarised below:
Shifting the Balance of Care
This is one of the key policy commitments of the Health and Social Care Delivery plan and underpins our longer-standing commitment to integrating health and social care. Many activities currently undertaken in hospital could be delivered in primary, community and social care settings so a patient is seen closer to home. There is also evidence which highlights the variance in care levels across Scotland, for example, with hospital admission rates and A&E attendance rates varying widely across geographical areas.
The Financial Framework assumes potential productive opportunities through reduced variation across A&E attendance rates, outpatient follow up rates and hospital inpatient lengths of stay. These estimates are based on the health and social care system improving performance to the national average and provide a high level view of the potential scale of savings that this can deliver. Local systems will then use these high level assumptions to reflect local circumstances building on evidence about variation.
While it will be challenging given existing pressures in the system, shifting care out of a hospital setting requires investment in primary, community and social care service provision, and it is assumed that approximately 50% of savings released from the hospital sector would be redirected accordingly under the direction of Integration Authorities through their strategic commissioning plans.
Regional Working
This activity relates to better collaboration to improve services, including greater regional approaches to the planning and delivery of services. This will help drive change in how clinical networks are formed and help to reduce duplication in services and functions. The National Clinical Strategy[14] also envisages a range of reforms so that healthcare across the country can become more coherent, comprehensive and sustainable. It sets out, for example, a framework for how certain specialist acute services should be provided on a wider regional footprint.
Based on evidence from other healthcare systems it is assumed that productivity savings of just over 1% could be delivered through effective regional working.
Public Health and Prevention
Scotland, in common with many developed societies face challenges associated with lifestyle behaviours, and wider cultural factors that can prevent positive health choices being made. Addressing these requires a concerted, sustained and comprehensive approach and a number of health improvement actions have been set out in relation to smoking, exercise, diet and alcohol. These initiatives, alongside the promotion of self-care, and helping to stop people entering the health system through prevention and shared decision making (i.e. Realistic Medicine) are important themes within the Health and Social Care Delivery Plan. For example, in the East of Scotland, work is being undertaken to deliver a prevention programme to reduce the incidence or reversal of type-2 diabetes in the region dramatically. The region is taking forward a comprehensive approach to health-based interventions such as weight-loss support and advising on self-management of the condition, and more widely, the promotion of active travel and targeted interventions for children and young people. The work links into the Scottish Government’s Diet and Healthy Weight Strategy.
It is not yet possible to fully quantify how these policies will ultimately impact upon the health and social care sector but it is important to capture the potential. As a result, a 1% reduction in demand is included in the financial framework from the implementation of these initiatives, starting towards the end of the five year period.
Once for Scotland
The Health and Social Care Delivery Plan also sets out how taking a ‘Once for Scotland’ approach can continue to deliver more effective and consistent delivery of services, building on the principles of the National Clinical Strategy. For the purposes of the financial framework a 0.25% reduction in cost is assumed, to reflect potential savings in this area. These savings estimates could increase further in the future through advances in technology.
Annual Savings Plans
These relate to the operational delivery of productivity and efficiency savings that all health and social care organisations manage on an annual basis. They typically consist of a number of improvement initiatives, from reducing the reliance on bank and agency staff, to making savings on medical or surgical consumable purchases, right through to changing how services are delivered.
The financial framework has included a target of 1% year on year against these plans, although there is potential for further savings to be delivered in this way. For example, a study by NHS England estimated that historical savings in the NHS were around 0.8% year on year, but that it was considered feasible for providers to deliver efficiency savings as high as 1.5-3% year on year.[15]
Bridging the Financial Challenge
The Financial Framework provides an indication of the potential approach and type of initiatives that would create a financially balanced and sustainable health and social care system. This presents a macro level view across Scotland and within this framework, local systems will put in place local level delivery plans and developments. These plans and developments will vary in each part of the country, depending on the requirements and arrangements put in place.
Figure 8 illustrates how all of the assumptions on these reform initiatives and ongoing efficiency savings would combine to address the financial challenge over the coming years. Taking account of assumed Barnett resource consequentials through to 2023/24, total funding will be £4.1 billion higher than in 2016/17 and this is presented in figure 8. This is split between an inflationary growth in funding, and additional investment for reform. Based on this modeling there would remain a residual balance of £159 million across the health and social care system in 2023/24.[16] We would anticipate further updates to the assumptions on the reform activities mentioned above in order to address the residual balance over the period.
Figure 8. System Reform Bridging Analysis
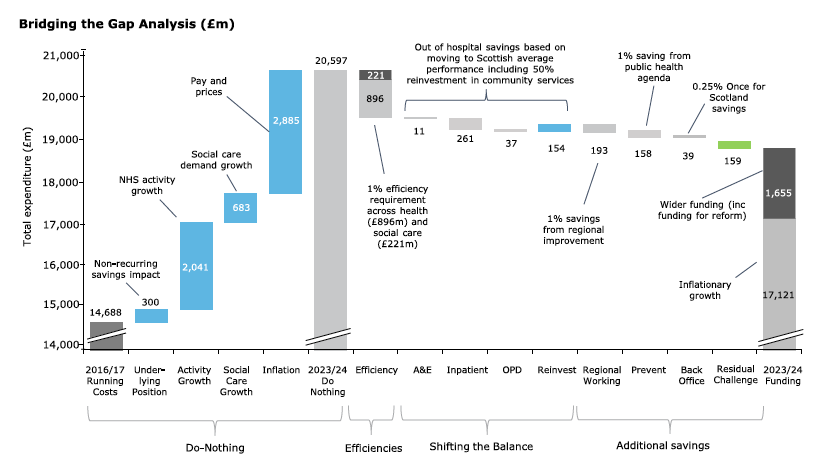
Figure 8 illustrates that from a starting point in 2016/17, with running costs of £14.7 billion, the health and social care system would require expenditure of £20.6 billion in 2023/24 if the system did nothing to change. Reform programmes have however already begun, particularly the integration of health and social care, which will help to address this ‘do nothing’ challenge. More progress is nonetheless needed to drive forward reform and address the residual savings balance. This will require further work across the health and care system to identify new ways to provide services to the population of Scotland.
Future iterations of the Financial Framework will include assessments of local and regional delivery plans in achieving these ambitions.
Summary
The Health and Social Care Delivery Plan brings together a number of policy initiatives that have been designed to reform how care is delivered to the people of Scotland. These will not only support the delivery of high quality care, but will help the system to manage the predicted growth in demand for health and social care over the next five years. There are challenges associated with this, for example, savings assumed through preventative plans may not deliver as anticipated, while the challenges are different across localities due to varying pressures.
In addition, although initial plans are in place, delivering on this agenda will require further change beyond the scope of this framework. Building on progress already underway through integration, there will need to be proportionately less care delivered in hospitals and there is an expectation that new digital technology will change care delivery models.
The System Bridging Reform Analysis does however provide a clear framework from which, regions, NHS Boards and Integration Authorities can build plans. It draws out the significant additional investment through to 2023/24, but highlights that this investment must be used to support the reform that is required across the health and social care system to ensure ongoing sustainability.
Contact
Health Finance Team:
Health_Finance_Divisional_Support@gov.scot