Scottish COVID-19 Mental Health Tracker Study Wave 5 Report
This is the final report of the Scottish COVID-19 (SCOVID) Mental Health Tracker Study, covering findings for a range of mental health outcomes across all the five waves of the Study.
3. Subgroup mental health outcomes
This section presents the mental health findings for intersectional subgroups across the waves of the SCOVID Mental Health Tracker Study. Additional findings from these subgroups are included in Annex 5.
The main subgroups reported are: young women, young men, young adults, and women. These subgroups consistently reported the poorest mental health in previous waves of the study compared with their subgroup counterparts. Within these subgroup sections, the mental health and wellbeing of young adults and women who also have a pre-existing mental health condition, a pre-existing physical health condition, caring responsibilities, young dependents (under 5 years), or vaccine hesitancy is also reported. Unfortunately, sample sizes were too small to report the mental health and wellbeing of these groups for young women and young men.
As in the previous section, this section reports findings relating to depressive symptoms, anxiety symptoms, suicidal thoughts, and mental wellbeing.
3.1 Mental health of young women
The SCOVID study appears to be consistent with wider research that shows that young women may be at a particularly high risk of mental health problems during the COVID-19 pandemic (Sadler et al., 2018). For example, the Adult Psychiatric Morbidity Survey (APMS, 2014) in England found that mental health symptoms were more common in young women (16-24 years; 26.0%) than young men (9.1%). Further, evidence from the Office of National Statistics (ONS) suggests that during the COVID-19 pandemic, 43% of women aged 16-29 years experienced depressive symptoms, compared with 26% of men of the same age (Williams et., 2021).
Background and health of young women at Wave 5:
- 42.6% of young women (18-29 years) were in the lower SEG,
- 35.7% stated that their working status had changed during the COVID-19 pandemic (i.e., furloughed, lost job),
- 27.2% were key workers,
- 18.0% of young women had a pre-existing mental health disorder,
- 12.9% reported that they had unpaid caring responsibilities,
- 10.7% had dependents under 5 years old,
- 6.6% had a pre-existing physical health disorder.
Compared with young men, young women were more likely to be in the lower SEG and have a pre-existing mental health condition, factors that may make them more at risk for poor mental health.
Wave 5 Findings:
- 14.8% reported suicidal thoughts,
- 34.9% reported depressive symptoms, and
- 36.8% reported anxiety symptoms.
- The average mental wellbeing score for young women was 19.80 (out of a possible score of 35), lower than the average of 22.08
Trends across the SCOVID study
Age and sex counterpart comparison
Findings from Wave 1 to Wave 5 of the SCOVID study suggest that young women (18-29 years) appear to be at risk for worse mental health outcomes than their age (30-59 year old women, 60+ year old women) and sex (young men) counterparts. Young women consistently reported the worst mental health over the pandemic; across most waves they reported the highest rates of suicidal thoughts, depressive symptoms, and anxiety symptoms, and the lowest mental wellbeing compared with young men. Wave 2 is the notable exception, whereby young men appeared to have worse mental health overall, although this finding should be treated with caution as there may be some inflation due to the young men subgroup being under-represented in the data at Wave 2.
Mental health and pandemic restrictions
The SCOVID data suggest that young women appeared to be at highest risk of poor mental health when COVID-19 mitigation restrictions on movement and socialising were in place.
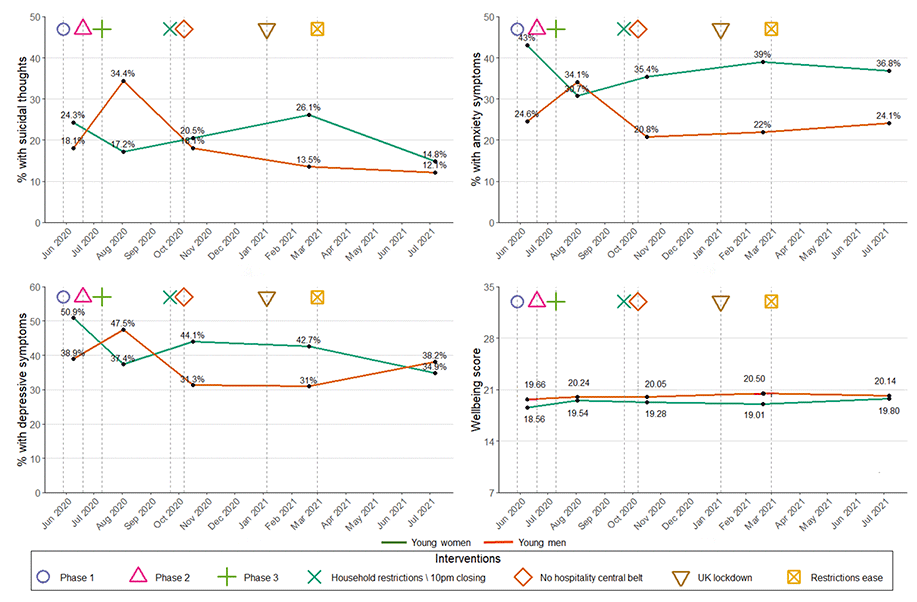
Figure 3.1 illustrates mental health outcome trends (suicidal thoughts, depressive symptoms, anxiety symptoms, and the SWEMWBS wellbeing scores) for young women across the SCOVID study in context of changes in pandemic restrictions. This figure shows that poor mental health was most clear at Wave 1 (Spring 2020), Wave 3 (Autumn 2020), and Wave 4 (Winter 2021). It is reassuring to note that mental health outcomes appeared to improve when restrictions were reduced at Wave 2 (Summer 2020) and Wave 5 (Summer 2021). Indeed, at Wave 5, young women reported the lowest rates of suicidal thoughts, depressive symptoms, and highest mental wellbeing than at any other stage of the pandemic.
Similar trends were found within a comparable period for the UK COVID-19 Mental Health & Wellbeing study (Wetherall et al., under review). Data from Wave 4 to Wave 7 (reflecting SCOVID Wave 1 to Wave 4) suggests that overall young women reported higher rates of depressive and anxiety symptoms than young men across the waves, although they reported similar rates of suicidal thoughts. For young women, rates of depressive symptoms and anxiety symptoms were at their lowest at Wave 5, during a time of loosened restrictions, and by Wave 7, when a lockdown was in place, rates of suicidal thoughts and depressive symptoms were at their highest. Therefore, consistent with the SCOVID study, the mental health of young women appeared be negatively impacted by COVID-19 restrictions.
3.2 Mental health of young men
Wider research on the mental health of young men shows that although women consistently report higher rates of common mental health disorders than men (APMS, 2016), there is some evidence that men's mental health has been worsening in recent years. For example, the Scottish Health Survey (SHeS) (2019) found that the proportion of men reporting symptoms of depression and anxiety has increased in the 2018/2019 survey compared with the levels reported at 2010/2011 survey, and prevalence decreased with age, with the highest rate recorded among younger people aged 16-24 years.
Background and health of the young men subgroup at Wave 5,
- 38.3% were key workers,
- 35.8% were in the lower SEG,
- 36.1% stated that their working status had changed during the COVID-19 pandemic (i.e., furloughed, lost job),
- 15.7% of young men had a pre-existing mental health disorder,
- 15.7% of young men reported that they had caring responsibilities,
- 8.0% had a dependent aged 5 years or younger.
Compared with young women, young men in the SCOVID sample were more likely to be a key worker, a factor that may place them at higher risk of poor mental health.
Wave 5 Findings:
- 12.1% reported suicidal thoughts,
- 38.2% reported depressive symptoms, and
- 24.1% reported anxiety symptoms.
- The average mental wellbeing score was 20.14 (out of a possible score of 35), lower than the sample average of 22.08.
Trends across the SCOVID study
Age and sex counterpart comparison
Findings from Wave 1 to Wave 5 of the SCOVID study suggest that young men (18-29 years) consistently reported higher rates of suicidal thoughts, depressive symptoms, and anxiety symptoms, and lower mental wellbeing, than men aged 30-59 year olds and 60+ year olds. Only at Wave 5 did 30-59 year old men report a higher rate of suicidal thoughts (16.1%) than young men (12.1%). Overall, young men reported better mental health outcomes across the waves than young women. The main exception was at Wave 2, where young men reported higher rates of suicidal thoughts (34.4%), depressive symptoms (47.5%), and anxiety symptoms (34.1%) than young women, although this finding should be treated with caution as there may be some inflation due to the young men subgroup being under-represented in the data.
Mental health and pandemic restrictions
The SCOVID data suggests that young men appeared to be at highest risk of poor mental health when COVID-19 mitigation restrictions on movement and socialising were reduced, specifically at Wave 2 (Summer 2020) and Wave 5 (Summer 2021). This is a pattern in contrast to that for young women.
Figure 3.1 illustrates mental health outcome trends (suicidal thoughts, depressive symptoms, anxiety symptoms, and the SWEMWBS wellbeing scores) for young men across the SCOVID study in context of changes in pandemic restrictions. This figure shows that, for example, when restrictions were relaxed between Wave 1 (Spring 2020) and Wave 2 (Summer 2020), young men's mental health appeared to worsen rather than improve, with higher proportions of young men reporting suicidal thoughts, anxiety symptoms, and depressive symptoms at Wave 2, compared with Wave 1. Furthermore, from Wave 2 to Wave 3 (Autumn 2020) and Wave 4 (Winter 2021), periods which coincided with the increasing of restrictions (Wave 3) and a national lockdown (Wave 4), mental health for young men appeared to improve, or return to rates more similar to Wave 1. We cannot state why young men appeared to experience the opposite pattern to young women regarding restrictions and mental health outcomes, although there are some notable caveats due to loss to follow-up for this group. One interpretation could be that for young men there may be a lag between restrictions being in place and their negative impact upon mental health, so that it is taking longer for young men to feel the consequences of the restrictions upon their mental health, and also the benefits of restrictions being lifted.
Looking at trends within a comparable period for the UK COVID-19 Mental Health & Wellbeing study (Wetherall et al., under review), data from Wave 4 to Wave 7 (reflecting SCOVID Wave 1 to Wave 4) suggests that although young men reported overall better mental health than young women, they consistently reported worse mental health than men aged 30-59 years and men aged 60+ years. For young men in the UK study, rates of suicidal thoughts, depressive symptoms, and anxiety symptoms were relatively stable from Wave 4 to Wave 5. At Wave 6 suicidal thoughts and anxiety symptoms were at their lowest, which coincided with a time when restrictions were beginning to increase, similar to the trends found in the SCOVID data. In contrast to the SCOVID findings, young men's suicidal thoughts, depressive symptoms and anxiety symptoms were highest at Wave 7 (e.g., 20.2% of young men reported suicidal thoughts at Wave 7), when there was a national lockdown in place. Therefore, although there is some consistency with the SCOVID study, in the UK study the mental health of young men appeared be negatively impacted by the COVID-19 lockdown, while in the SCOVID study young men appeared to have better mental health during periods of restrictions.
3.3 Mental health of young adults
Wider research suggests that young adults may be at higher risk of poor mental health and wellbeing, before and during the pandemic, which corroborates the findings of the SCOVID study. Before the pandemic, the mental health of the UK's children and young adults was already deteriorating, with an increase in anxiety, depression, and self-harm from 2000 to 2014 (Pitchforth et al., 2016). Data published from the UK COVID-MH survey (O'Connor et al., 2021), found that young adults (18-29 years) reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms, and lower wellbeing, across each wave, compared with the older age groups (30-59 years and 60 years). Additionally, a study looking at all the recent research investigating suicidal thoughts during the pandemic found that younger age was a risk factor for suicidal thinking (Dube et al., 2021).
Background and health of young adults at Wave 5,
- 39.2% were in the lower SEG,
- 35.9% reported that their working status had changed (e.g., furloughed, lost job),
- 32.8% were key workers,
- 16.8% had a pre-existing mental health condition,
- 14.3% reported having unpaid caring responsibilities,
- 9.3% had dependents under 5 years,
- 6.0% had a physical health condition.
Compared with the older age groups (30-59 years and 60 years), young adults were more likely to be a key worker, and more likely to have a mental health condition compared with 60+ year olds; these factors may place them at higher risk of poor mental health.
Wave 5 Findings:
- 13.4% reported suicidal thoughts,
- 36.6% reported depressive symptoms,
- 30.4% reported anxiety symptoms, and
- The average mental wellbeing score for young adults was 19.97 (out of a possible score of 35), lower than the average of 22.08.
Trends across the SCOVID study
Age and sex counterpart comparison
At the majority of waves, young adults reported higher suicidal thoughts, depressive symptoms, anxiety symptoms, and lower mental wellbeing than 30-59 year olds and 60+ year olds.
In addition, a clear relationship between age and poor mental health emerged across the waves; reporting poor mental health was less likely as the age group bracket increased. For example, the youngest age group (18-29) reported the poorest mental health and wellbeing outcomes, followed by those aged between 30 and 59, with people aged 60+ reporting the best outcomes (see Table F in Annex 4).
Mental health and pandemic restrictions
The SCOVID data suggests that young adults reported overall better mental health and wellbeing when restrictions were eased.
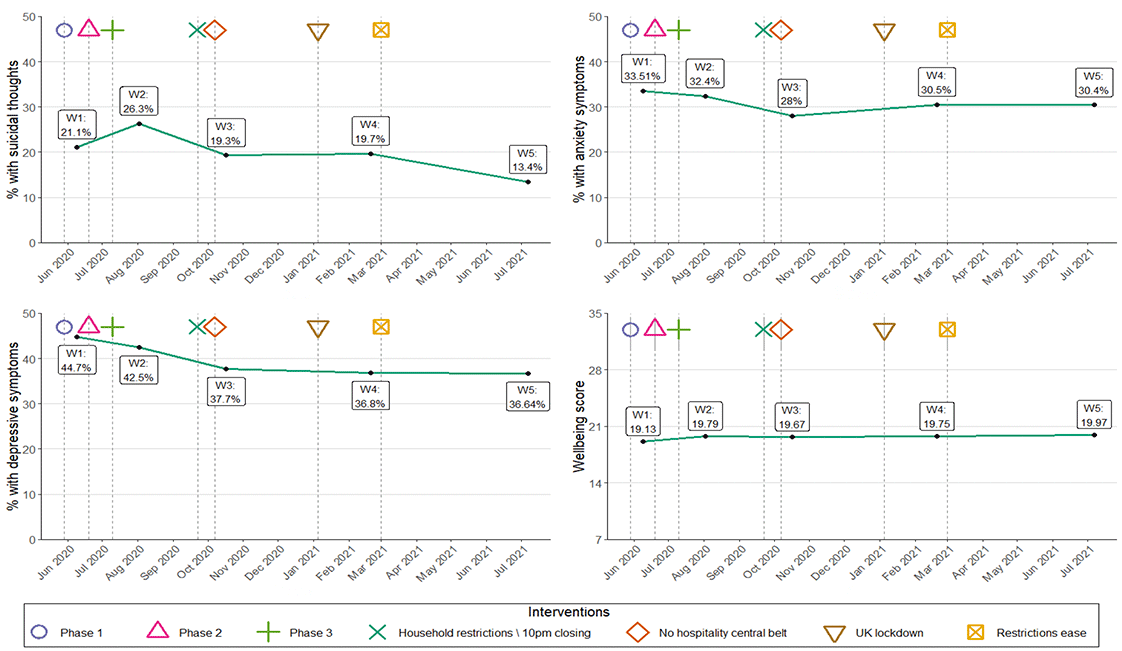
Figure 3.2 illustrates mental health outcome trends (suicidal thoughts, depressive symptoms, anxiety symptoms, and the SWEMWBS wellbeing scores) for young adults across the SCOVID study in context of changes in pandemic restrictions. Looking at these trends across the waves, young adults reported the highest rates of depressive symptoms and anxiety symptoms, and the lowest mental wellbeing at Wave 1 (Spring 2020), a time when restrictions were still in place, although Phase 1 of the easing of lockdown had begun in Scotland. The highest rates of suicidal thoughts were reported at Wave 2 (Summer 2020), which coincided with Phase 3 of easing out of lockdown. The lowest rates of suicidal thoughts, depressive symptoms, and highest wellbeing scores were reported at Wave 5 (Summer 2021), which coincided with a period of easing of restrictions.
Intersectional findings
Trends across the waves of the SCOVID study suggest that young adults (18-29 years) with particular background and health factors are at increased risk for worse mental health and wellbeing, including:
- a pre-existing mental health condition,
- a pre-existing physical health condition,
- unpaid caring responsibilities, or
- vaccine hesitancy[8].
Additional findings from these subgroups are included in in Annex 4 and 5.
Young adults with a pre-existing mental health condition
- Findings from Wave 1 to Wave 5 of the SCOVID study suggest that young adults (18-29 years) with a pre-existing mental health condition are at higher risk of poorer mental health than young adults with no pre-existing mental health condition. For example, at Wave 5, 28.8% of young adults with no pre-existing mental health condition reported depressive symptoms, compared with 74.7% of young adults with a mental health condition (see Annex 4 Table F).
- At most waves, young adults with a pre-existing mental health condition reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms and lower mental wellbeing than the other age groups (30-59 years and aged 60+ years) who also had a pre-existing mental health condition.
- Looking at trends over the waves in context of changes in pandemic restrictions, findings suggest that although young adults with a pre-existing mental health condition reported overall better mental health and wellbeing when restrictions were eased, symptoms of anxiety appeared to remain high.
- Although we do not know whether rates of poor mental health for young adults represent an increase from pre-pandemic levels, a recent Young Minds survey conducted with young people with mental health needs in the UK found that 80% of respondents felt that the COVID-19 pandemic had made their mental health worse (Young Minds, 2020).
Young adults with a pre-existing physical health condition
- Findings from Wave 1 to Wave 5 of the SCOVID study suggest that young adults with a pre-existing physical health condition are at higher risk of mental health problems than young adults with no pre-existing physical health condition. For example, at Wave 5 33.2% of young adults with no pre-existing physical health condition reported depressive symptoms, compared with 85.3% of young adults with a health condition (see Annex 4 Table F).
- At all waves, young adults with a physical health condition reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms, and lower mental wellbeing, than their age group counterparts (30-59 years, 60+ years) who also had a pre-existing physical health condition.
- Looking at trends over the waves in context of changes in pandemic restrictions, findings suggest that young adults with a pre-existing physical health condition reported poorer mental health when restrictions were eased in Scotland.
Young adults with unpaid caring responsibilities
- Findings from Wave 1 to Wave 5 of the SCOVID study suggest that young adults with caring responsibilities (young carers) are at higher risk for mental health problems than young adults with no caring responsibilities. For example, at Wave 5 32.3% of young carers reported depressive symptoms, compared with 61.5% of young adults with unpaid caring responsibilities (see Annex 4 Table F).
- At all waves, young carers reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms, and lower mental wellbeing, than their age group counterparts (30-59 years, 60+ years) who also had unpaid caring responsibilities.
- Looking at trends over the waves in context of changes in pandemic restrictions, findings suggest the mental health of young carers was worst during periods of lockdown and higher restrictions, and better during periods of eased restrictions.
Young adults who reported vaccine hesitancy
- Vaccine hesitancy (i.e., a delay in choosing to get vaccinated or refusing to get vaccinated) was measured at Wave 4 and Wave 5 of the SCOVID study. At Wave 5 of the SCOVID study, 12.3% of young adults reported vaccine hesitancy, compared with 8.8% of 30-59 year olds, and 1.7% of 60+ year olds.
- Findings from Wave 4 and Wave 5 of the SCOVID study suggest that young adults with vaccine hesitancy tended to be at higher risk of mental health problems than young adults with no vaccine hesitancy. For example, at Wave 5 11.8% of young adults with no vaccine hesitancy reported suicidal thoughts, compared with 25.4% of young adults with vaccine hesitancy (see Annex 4, Table F).
- Additionally, young adults with vaccine hesitancy tended to report higher rates of depressive symptoms and anxiety symptoms, than their age group counterparts (30-59 years, 60+ years) who also had vaccine hesitancy.
3.4 Mental health of women
Findings show that, pre-pandemic, women are more likely than men to report and be diagnosed with a mental health condition. For example, the Adult Psychiatric Morbidity Survey (APMS, 2016) reported that one in five women (20.7%) had a common mental disorder (e.g., depression, anxiety) compared with one in eight men (13.2%). Similarly, in the Scottish Health Survey (SHeS, 2019), 19% of women reported having psychiatric symptoms, compared with 15% of men. Therefore, women were potentially more vulnerable to poor mental health and wellbeing during the pandemic.
Findings published from the UK COVID-MH survey (O'Connor et al., 2021) found that women reported higher rates of depressive symptoms and anxiety symptoms, and lower wellbeing, across each wave compared with men. These findings related to the mental health of women are corroborated by the SCOVID study.
Background and health of women at Wave 5:
- 61.7% reported that their working status had changed (i.e., furloughed, lost job)
- 38.8% were in the lower SEG
- 22.8% were key workers
- 22.3% had a physical health condition 19.2% reported having unpaid caring responsibilities
- 14.3% had a pre-existing mental health condition
- 8.3% had dependents under 5 years
Compared with men, women were more likely to be in the lower SEG, have had a change to working status, have caring responsibilities, and have a physical health condition; these factors may place them at higher risk of poor mental health.
Wave 5 Findings:
- 9.3% of women reported suicidal thoughts,
- 22.5% reported depressive symptoms,
- 19.6% reported anxiety symptoms, and
- The average mental wellbeing score for women was 21.85 (out of a possible score of 35), lower than the average of 22.08.
Trends across the SCOVID study
Age and sex counterpart comparison
Across Waves 1 to 5 of the SCOVID study, overall women reported worse mental health outcomes compared with men. At most waves, women reported higher depressive symptoms, anxiety symptoms, and lower mental wellbeing than men. The main exception was rates of suicidal thoughts, with men reporting higher suicidal thoughts overall, for example, at Wave 2, 16.3% of men reported suicidal thoughts compared with 10.5% of women.
Mental health and pandemic restrictions
The SCOVID data suggest that women reported the highest rates of depressive symptoms, anxiety symptoms, and lowest levels of mental wellbeing, at Wave 1 (Spring 2020), a time when restrictions were still in place, although Phase 1 of the easing of lockdown had begun in Scotland.
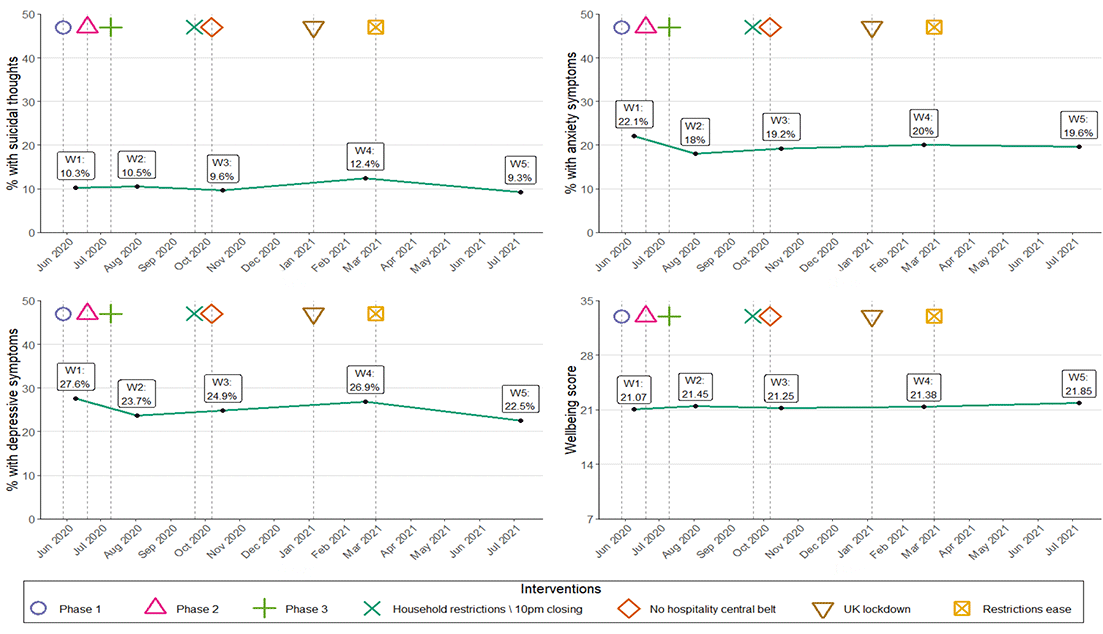
Figure 3.3 illustrates mental health outcome trends (suicidal thoughts, depressive symptoms, anxiety symptoms, and the SWEMWBS wellbeing scores) for women across the SCOVID study in context of changes in pandemic restrictions, This figure shows that the highest rates of suicidal thoughts, and high rates of depressive symptoms, were reported at Wave 4 (Winter 2021), during a national lockdown. By Wave 5 (Summer 2021), suicidal thoughts and depressive symptoms were at their lowest, and mental wellbeing was at its highest, which coincided with a period of easing of restrictions. This suggests that women reported overall worse mental health and wellbeing when restrictions were in place.
Intersectional findings for women
Trends across the waves of the SCOVID study suggest that women with particular background and health factors are at increased risk for worse mental health and wellbeing, including:
- a pre-existing mental health condition,
- a pre-existing physical health condition,
- unpaid caring responsibilities,
- young dependents, or
- vaccine hesitancy[9].
Women with a pre-existing mental health condition
- Wave 1 to Wave 5 of the SCOVID study suggests that the mental health of women with a pre-existing mental health condition was consistently much worse than for women without a pre-existing mental health condition. For example, at Wave 5, 15.6% of women with no pre-existing mental health condition reported depressive symptoms, compared with 63.8% of women with a mental health condition, and this trend is seen for each outcome across the waves (see Annex 4 Table F).
- Compared with men with a pre-existing mental health condition, women in this group consistently reported higher rates of depressive symptoms and anxiety symptoms across the waves, although rates of suicidal thoughts and levels of mental wellbeing appeared to fluctuate more.
- Looking at trends over the waves in context of changes in pandemic restrictions, women with a pre-existing mental health condition appeared to report lower rates of suicidal thoughts, depressive symptoms and anxiety symptoms at Wave 5 (June - July 2021), when restrictions had been eased, compared with when restrictions were in place (e.g., Wave 4).
Women with a pre-existing physical health condition
- Looking across the study waves, mental health outcomes for women with a pre-existing physical health condition were consistently worse than for women without a pre-existing physical health condition. For example, at Wave 5, 18.8% of women with no pre-existing health condition reported depressive symptoms, compared with 35.4% of women with a pre-existing health condition, and this trend is seen for each outcome across the waves (see Annex 4 Table F).
- Compared with men with a pre-existing physical health condition, women in with a heath condition tended to report higher rates of depressive symptoms and anxiety symptoms across the waves, although overall men reported higher rates of suicidal thoughts and lower levels of mental wellbeing.
- Looking at trends over the waves in context of changes in pandemic restrictions, findings suggest that mental health and wellbeing for women with a pre-existing physical health condition was generally worse at times when restrictions were easing. Although we cannot state why the pattern for those with a physical health problem is different from most other groups, it has been suggested that the moves made to make life more accessible from home, for example increased use of video-conferencing technology, may have increased flexibility for those who have chronic illness or are disabled (Barnardo's, 2021).
Women with unpaid caring responsibilities
- In the UK, women were more likely to take on caring roles than men before the pandemic (Carers UK), and emerging research worldwide suggests that the crisis and its subsequent shutdown response have resulted in an increase in this burden (Power, 2020).
- Findings from Wave 1 to Wave 5 of the SCOVID study suggest that women with unpaid caring responsibilities are at higher risk of mental health problems than women with no unpaid caring responsibilities. For example, at Wave 5, 19.9% of women with no caring responsibilities reported depressive symptoms, compared with 33.3% of women with caring responsibilities (see Annex 4 Table F).
- At most waves women with caring responsibilities reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms, and lower mental wellbeing, than men who also had caring responsibilities. The main exception was at Wave 5, when men with caring responsibilities reported higher suicidal thoughts, depressive symptoms, and anxiety symptoms.
- Looking at trends across the waves in context of changes in pandemic restrictions, it appears the mental health of women carers was worst during periods of lockdown and higher restrictions, and better during a period of eased restrictions.
Women with young dependents (under 5 years)
- Findings from Wave 1 to Wave 5 of the SCOVID study suggest that women with young dependents tended to be at higher risk of mental health problems than women with no young dependents. For example, at Wave 5, 21.9% of women with no young dependents reported depressive symptoms, compared with 28.3% of women with young dependents (see Annex 4, Table F).
- At most waves, women with young dependents reported higher rates of suicidal thoughts, depressive symptoms, anxiety symptoms, and lower mental wellbeing, than men who also had young dependents.
- Looking at trends across the waves in context of changes in pandemic restrictions, it appears the mental health of women with young dependents was worst during periods of lockdown and higher restrictions, and better during a period of eased restrictions.
Women who reported vaccine hesitancy
- Vaccine hesitancy (i.e., a delay in choosing to get vaccinated or refusing to get vaccinated) was measured at Wave 4 and Wave 5 of the SCOVID study. At Wave 5 of the SCOVID study, 7.1% of women reported vaccine hesitancy, compared with 7.6% of men.
- Findings from Wave 4 and Wave 5 of the SCOVID study suggest that women with vaccine hesitancy tended to be at higher risk of mental health problems than women with no vaccine hesitancy. For example, at Wave 5, 18.3% of women with no vaccine hesitancy reported anxiety symptoms, compared with 37.0% of women with vaccine hesitancy (see Annex 4, Table F).
- Additionally, women with vaccine hesitancy tended to report higher rates of anxiety symptoms and lower mental wellbeing than men who also had vaccine hesitancy.
- Looking at trends at Wave 4 and Wave 5 in context of changes in pandemic restrictions, it appears the mental health of women who were vaccine hesitant overall was poorer when restrictions were in place.
Contact
Email: socialresearch@gov.scot