Scottish Cancer Patient Experience Survey 2015/16: Analysis of Free-text Comments
Analysis of free-text comments provided by patients as part of Scotland’s first Cancer Patient Experience Survey.
Results
The breakdown of numbers of comments by top level category are given in Appendix C. Overall, there were more positive (2,528) than negative (1,969) comments. 671 participants made both positive and negative remarks within the same Comments Box. Participants also made 1,208 factual/neutral comments, and 585 miscellaneous comments. There were more positive than negative comments (a ratio of 1:0.78) for every comment box except Comment Boxes 1 (lead up to diagnosis) and 7 (experience of cancer care).
Proportionally, more negatively oriented comments appeared in Comment Box 1 than in any other text box, indicating that respondents were least happy with the lead up to diagnosis. Comments Box 3 had the highest proportion of positive to negative comments, indicating participants were proportionately more happy with the support they received (including from a clinical nurse specialist).
Due to the large volume of data, creating top level categories sorted responses into positive and negative comments, imposing a false dichotomy between positive and negative experiences. In reality, participants had variable experiences, not overwhelmingly negative. However, separating the positive and negative experiences allowed the analysis to focus on common issues when things either went right or wrong for patients.
Positive Comments
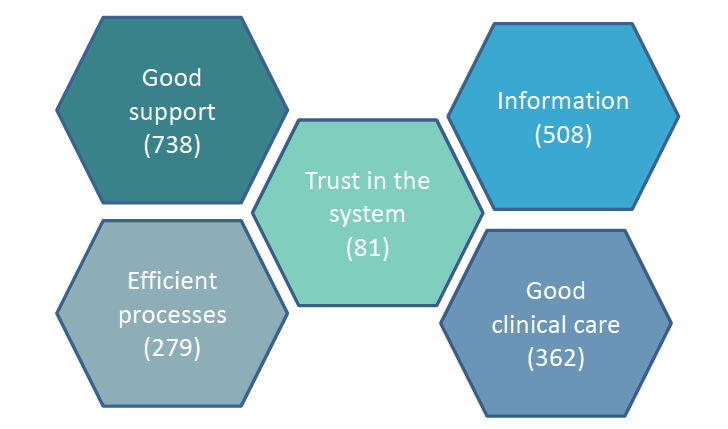
Overall, participants in the survey made more positive (2,528) than negative (1,969) comments about their cancer patient experience. Positive comments tended to be shorter and less descriptive and detailed than negative comments. The average number of words in positive comments was 24 words, compared to an average of 43 words in negative comments. Other cancer patient experience surveys have found a similar trend, with positive comments being less descriptive and of a much more general nature than negative comments (Wagland, Bracher, Esqueda, Schofield, Richardson, 2015). If people commented on a positive experience it was generally characterised by having good support, the system working quickly and efficiently, being given clear information, receiving good clinical care and having trust in the system ( Figure 1).
Participants described a generally positive experience in terms of receiving good, great or excellent care, having no complaints, and being pleased and happy with their experience. This was a common positive, with 1,995 comments describing a generally good experience across all seven comment boxes.
"Could not have been better."
Male, Age 66-75, Colorectal Cancer
"First class."
Male, Age 76 and over, Lung Cancer
Figure 1: Positive aspects of care (number of comments)
Information
Comments suggest that respondents particularly valued being given clear information, and thorough explanations of their cancer and treatment, including treatment options. Patients appreciated staff being sensitive in the way they gave information, and taking the time to provide details about procedures. Positive comments were frequently made about being given detailed enough information to enable people to have clear expectations of their cancer experience. Overall, there were 508 positive comments about clear information.
"The cancer diagnosis and treatment plan was explained very clearly in detail on the first appointment. Subsequently this was very helpful in my expectations of all the treatments."
Female, Age 51-65, Gynaecological Cancer
"All decisions were fully discussed and explained in a manner which was both sympathetic and sensitive, as well as in terms that I could understand."
Male, Age 51-65, Upper Gastrointestinal Cancer
Efficient Processes
199 participants commented in a positive way about the speed of treatment. Comments related to the swift and efficient organisation of tests in the run up to diagnosis, not having to wait long on the day for outpatient or radiotherapy treatment, or being well informed about delays when in the waiting room.
A further 43 positive comments related to smooth and efficient processes around screening, and to being prompted by adverts or media articles to get tested for cancer. Many participants whose cancer had been identified through screening commented positively on the efficiency, information and support provided by the screening process, along with their relief that the cancer had been detected early before they had symptoms.
"From my doctor finding that I was anaemic and asking [hospital name removed] to look at my bowel it was all done within two weeks. Excellent by everyone."
Male, Age 66-75, Colorectal Cancer
"My cancer diagnosis came about as a result of the bowel screening programme. I was not ill and had no symptoms and if not for the screening my outcome may well have been different."
Male, Age 66-75, Colorectal Cancer
A small number of comments related to receiving treatment in a comfortable environment (21) and receiving local outpatient, chemotherapy or radiotherapy treatment, which participants felt made life considerably easier than having to travel for treatment (16).
Participants commented more fully on the specific importance of having good support during their cancer journey, having trust in the system, and receiving good clinical care.
Good Support
Good support was described as being looked after by staff who were caring, supportive, kind, approachable and informative, and who treated the patient as an individual (738 comments). Patients also appreciated staff being cheerful, friendly and professional. There were many positive comments specifically describing support from clinical nurse specialists and other nurses, particularly emphasising and valuing their role as a point of contact, information and reassurance.
Participants also described receiving support from a range of charities ( e.g. Macmillan, Maggie's, Urological CANcers Aberdeen, CLAN Cancer Support, Citizens Advice Scotland etc) and commented on how valuable this was as an additional source of support, information and contact. However, many participants remarked that they had only heard about the support available from charities through word of mouth from other patients. Good support was described in comments about inpatient and outpatient care, but not in those made about the lead up to diagnosis or the way decisions were made about treatment.
"I have found that most doctors/nurses etc. (bar one!) have been so nice to me and understand how nervous and scared I can be. Having cancer is terrifying and at times a very lonely place, we need to be cared for in a kind and gentle way, we get very scared."
Female, Age 36-50, Breast Cancer
"It was great having support from the nurse specialist. Before my surgery she took me through what may happen, colonoscopy etc. and what support would be available. Following discharge I contacted her at least twice for advice prior to carrying out some activities."
Male, Age 51-65, Colorectal Cancer
"I did use Maggie's as someone recommended it, otherwise I wouldn't have known it was there. The help I got was from Maggie's and a short course delivered at Maggie's. That was very helpful. A consultant came to speak at it and I found having time to ask questions there was very helpful."
Female, Age 51-65, Breast Cancer
Good Clinical Care
Good clinical care was portrayed (362 comments) as the treatment or operation going well and the patient receiving specific help with side effects or self-care. Many participants outlined the confidence they felt in their clinical care team, describing how they felt safe when they were treated by the same team both before and after surgery or treatment. A strong clinical team was epitomised as having a respected clinical team leader (oncologist or surgeon) who had met with the patient, and who, along with other team members, had provided clear explanations about treatment and procedures, with no conflicting messages. Good clinical care was reported in comment boxes relating to inpatient and outpatient care, chemotherapy and radiotherapy treatment, and overall experience of cancer care.
"I feel privileged, to be looked after by such professional medical teams of surgeons and nurses. Any worries I had before operation were easily cast aside by their answers. Having [condition removed] always adds additional care required after an anaesthetic, but again, I always receive it. My grateful thanks to you all."
Female, Age 66-75, Breast Cancer
"I had very good pre-op and any post-op care while in for major surgery with specialist nursing for pain control. Clinical nursing specialist and excellent ward nursing care towards self care and enhanced recovery."
Female, Age 66-75, Colorectal Cancer
Trust In the System
A number of respondents (81 comments) specifically expressed their trust in the system. Patients particularly conveyed trust in relation to clinical staff 'knowing best', and to all necessary experts being involved in their care. Trust arose as a particularly important issue around the way decisions were made about treatment, with participants valuing joint decision making – being spoken to with respect, and being involved in the decision making process.
"With [name removed] and [name removed] I felt very much that we were a team dealing with this together and they then discussed my case with the other specialists."
Female, Age 51-65, Breast Cancer
"The most important consultation about possible treatment options at [hospital name removed] involved both the consultant urologist and a clinician from the [hospital name removed]. This was a most helpful arrangement which allowed me to understand the options very well."
Male, Age 66-75, Prostate Cancer
Negative Comments
The 1,969 negative comments tended to be longer and more detailed than those describing positive aspects of experience.
Analysis of the main themes emerging from the data across all stages of the cancer journey ( i.e. all comments boxes in the questionnaire) suggested two core issues at the heart of patients' negative experiences of care. These were (i) not feeling confident within the system and (ii) not feeling that individual needs were met. Within these core themes, a range of sub-themes characterised more negative experiences of care ( Figure 2).
Figure 2: Negative Aspects of Care
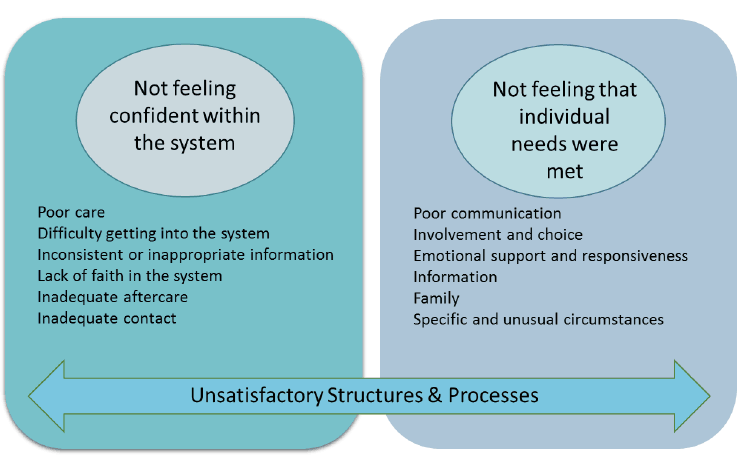
Participants also discussed underlying issues with the system and the organisation of services which contributed to poorer experiences in both of these areas. These were characterised as problems with (i) structures – the way services and environments are set up; and (ii) processes – the organisation of care and treatment (Figure 2). An overview of the analysis is presented in Table 3; brief definition of the sub-themes is presented in Appendix D.
Table 3: Summary of the themes and sub themes
| Themes | Sub Themes | Number of comments |
|---|---|---|
| Not feeling confident within the system | Poor care | 372 |
| Inadequate aftercare | 262 | |
| Difficulty getting into the system | 200 | |
| Inconsistent or inappropriate information | 158 | |
| Lack of faith in the system | 158 | |
| Inadequate contact | 50 | |
| Total number of comments about Not feeling confident within the system | 1,200 | |
| Not feeling that individual needs were met | Information | 407 |
| Poor communication | 345 | |
| Emotional Support and Responsiveness | 270 | |
| Involvement and choice | 97 | |
| Specific and unusual circumstances | 34 | |
| Family | 21 | |
| Total number of comments about Not feeling that individual needs were met | 1,174 | |
| Structures | Unsuitable or uncomfortable environment | 145 |
| Staffing Levels | 143 | |
| Privacy | 67 | |
| Transport | 49 | |
| Total number of comments about Structures | 404 | |
| Processes | Waits and delays | 454 |
| Ineffective and unreliable processes (organisational systems) | 289 | |
| Fragmented care | 276 | |
| Total number of comments about Processes | 1,019 |
Not feeling confident within the system
Thematic analysis revealed a number of negative experiences that appeared to relate to not feeling confident about their care or the way in which the system worked for them. These included receiving poor care, having difficulty getting into the system, receiving inconsistent or inappropriate information, having no faith in the system, receiving inadequate aftercare, and having inadequate contact with health professionals.
Poor care
Participants described a range of issues related to poor care including problems with treatment, being left alone and isolated, acquiring hospital infections, receiving inadequate pain relief and not feeling that side effects were managed adequately (372 comments). Many participants felt that hospital staff did not listen to, believe or understand their concerns – this was particularly the case for poor pain management and bowel problems. Respondents noted particular issues when receiving care from staff who had not been specifically trained in cancer care, commenting on differences in the quality of care they received on cancer wards or high dependency units compared to general wards. Patients reported feeling isolated on general wards, and appeared to feel that ward staff were unaware of and uncomfortable dealing with the needs of cancer patients.
Isolation was a particular issue for patients in single rooms, who could be left for hours without being visited by a nurse. Some participants felt that care at night and weekends was of poorer quality than during the day, with long delays due to staff shortages. Participants felt that the poor care they received resulted in clinical problems taking longer to be resolved and hospital stays being prolonged. In some cases poor care led to the patient having to be readmitted to hospital after discharge. Often patients described feeling ignored, isolated, alone and vulnerable, with staff rigidly following internal routines and regimens rather than responding to patients' needs.
"I was in severe pain following the operation, when I said so the nurses were talking among themselves that I couldn't be in that much pain, only to discover that I wasn't getting the correct strength of pain relief. I didn't find that the bedside manner of nurses are there any more. My daughter had to shower me. I had a bedsore and hair had to be cut due to it being matted."
Female, Age 36-50, Colorectal Cancer
"During the day the ward was well staffed with qualified cancer nurses, although they were under severe pressure at times. At night, staffing was inadequate to cope with the demands of very ill patients and at times treatment and medication were badly delayed due to emergencies."
Female, Age 66-75, Haematological Cancer
"Being admitted was the worst experience I could possibly have had. To say the staff were inexperienced in caring for cancer patients was an understatement. I couldn't talk because my mouth was so sore and swollen, my partner was telling them what was wrong and the two nurses on duty stood at the end of the bed and discussed between themselves as though we weren't there on how they had never heard of my condition before.
None of the staff knew how to take blood or administer drugs through a Hickman Line so they had to get one of the nurses down from the ward to show them. I was eventually put into a room by myself where a nurse from another department was helping out… They tried to send me for a CT scan, I refused, but it turned out that I wasn't the patient they were looking for.
All in all I spent seven hours without any real treatment for my condition. Treatment only started once I had been transferred up to the ward. Staff need much, much more training so they can competently deal and treat cancer patients."
Female, Age 36-50, Haematological Cancer
Difficulty getting into the system
Another source of concern for participants was the difficulty they experienced in receiving a cancer diagnosis (200 comments). Many respondents described having multiple visits to their GP practice, sometimes over months and years, before undergoing the diagnostic tests for cancer. During this time they were either told that nothing was wrong, or they were treated for a range of other wrongly diagnosed ailments, while continuing to struggle with their cancer symptoms. These participants felt their GPs had: insufficient awareness and knowledge of cancer and the common symptoms; paid insufficient attention to the patient's concerns; and were sometimes unwilling to refer the patient for diagnostic testing. Some patients described bypassing their GP by going to A&E or using private healthcare in order to be diagnosed, others described collapsing and being admitted to hospital as an emergency due to lack of earlier diagnosis and appropriate treatment.
"My GPs weren't very good. I had to eventually press them for an urgent referral. I knew there was something wrong. I had a tumour in my larynx, whilst my GP kept on treating me for asthma when previously I had been a fit individual so it was obvious I had/have a good set of lungs on me, not asthma. It took over 6 months to get to see a consultant. There was even another symptom - tingling fingers that could have pointed the GP in the right direction. If blood tests had been carried out they may have showed up reduced blood calcium levels, a symptom of which can be tingling fingers, which I had told the GP about at my first visit but was misdiagnosed."
Male, Age 36-50, Lung Cancer
Inconsistent or inappropriate information
Being given wrong or conflicting information was a cause of confusion, worry and anxiety to participants (158 comments). This was a particular problem during diagnosis if the patient was told their tumour was benign, only to discover after further tests that it was cancerous, or when the patient's expectations were set that they would receive 'simple' treatment, to then find out later that their treatment would be much more complex and invasive.
"I feel that the way I received the diagnosis information was not thorough enough or consistent. I do understand that a full diagnosis cannot be done until all the screening tests are completed, but that does not mean that I should receive contradictory information. In fact, I was so confused that I had to chase up a full explanation from the consultant, who was not available the first time my results were in. The breast nurse did this, but wasn't very supportive or informative, i.e. said the diagnosis confirmed that the cancer was invasive when I was previously told that it wasn't. She was on the computer looking for the details of the next patient when I was still there trying to find some answers of why information was omitted from me. This created a lot of anxiety as I was trying to research information on the web to try to understand."
Female, Age 36-50, Breast Cancer
Participants also described being given unclear and conflicting information by different health professionals and specialists involved in their treatment. This lack of consistent information made it difficult for some patients to feel confident in the decisions that were made about their treatment.
"Too many doctors were telling me different things, I got a bit confused by all the different stories the doctors were telling me. I didn't know who to listen to."
Female, Age 66-75, Upper Gastrointestinal Cancer
Lack of faith in the system
Several participants described having lost faith in the system (158 comments), not trusting that a deterioration in their health would be picked up. Participants described instances when tests were not carried out at all, not carried out at the correct time, tests did not pick up the cancer, results were wrongly interpreted, or they were not given timely or clear feedback on the results of tests. As a result, participants required a lot more reassurance that their cancer treatment had been successful and that their health was being monitored effectively.
"It's well over a year since I had my tumour removed but the bone has not been scanned again. I am also concerned about this cancer has spread throughout my body as it was there for several years before it was removed."
Male, Age 51-65, Head and Neck Cancer
Inadequate support after treatment
In addition to concerns about monitoring, many participants made comments about inadequate support after treatment (262 comments). Participants described confusion over who was responsible for care after treatment, with patients not receiving clear communication, or having a clear understanding of (i) who they should contact for ongoing support, and (ii) what should happen next in their cancer care. This was described by participants as being frightening, and led to patients feeling anxious and isolated. Patients were often left with debilitating side effects as a result of treatment, and many struggled to manage physically and emotionally when back at home. Many participants received no help or advice about self-care or how to self-manage side effects, and were discharged from hospital with no care plan, inadequate support at home, and no access to specialist services for additional support.
Several respondents commented in particular about the lack of support they received from their GP practice after treatment, describing an absence of contact from their GP practice, difficulties with attending the practice after major surgery, and their GP having little awareness of cancer treatment, side effects, or palliative care.
"Very disappointed felt like the cancer I had wasn't important enough.
I have had nothing but struggles since having cancer and feel completely disappointed I wasn't giving a MacMillan support nurse. Nothing! Dealt with most of it on my own and left wondering had my cancer been cleared or not since no one informed me."
Female, Age 16-25, Head and Neck Cancer
"Post-op I was discharged with no advice on how to best mobilise and no walking aids, no physiotherapy or advice on footwear. I waited weeks to see orthopaedic consultant to have an insole made. In those weeks I still needed to walk about. Very painful and difficult."
Female, Age 66-75, Skin Cancer
"I was sent home from Hospital with no care plan - I live on my own and had a difficult time to do things, nurse had told me everything was as planned and people would come to my home to help for a few weeks, but no one came. I was left on my own."
Female, Age 51-65, Lung Cancer
Inadequate contact
A small number of participants commented (50 comments) that they did not feel they had received adequate contact with cancer specialists. In some cases, participants reported either seeing a specialist clinical nurse, or a more junior doctor, however, this was not felt to be as reassuring as seeing an oncologist.
"I am checked up at dermatology and plastic surgery clinics. I rarely see a cancer specialist apart from the specialist clinical nurse. If this is a common experience arrangements should be made for the patient to be seen by an oncologist from time to time."
Female, Age 51-65, Skin Cancer
Not feeling that individual needs were met
Alongside not feeling confident within the system, the other major theme which negatively affected patients' experience of cancer care was not feeling that individual needs were met or respected. A range of issues fell within this theme, and contributed to patients feeling that their individual needs were not met. These included poor communication, lack of involvement and choice, poor emotional support and responsiveness, lack of information, lack of support for families, and difficulties with specific and unusual circumstances.
Poor communication
Many participants described experiencing communication problems at some point during their treatment (345 comments). These were particularly notable in the lead up to diagnosis, but were reported at all points of the cancer journey. Participants described feeling that staff did not listen to them or treat them with respect. Although they acknowledged that most staff were pleasant to them, many participants described isolated interactions where communication was rude, insensitive, impersonal, blunt, dismissive, condescending, cold and uncaring. At the time of diagnosis, respondents did not appreciate dramatic and fatalistic, or unclear communication, nor did they appreciate receiving an overload of information. A number of participants were never actually told in so many words that they had cancer, and others were told in a vague way using euphemisms – both approaches left patients feeling confused about their health.
"To be honest, I don't completely remember being told I had cancer, perhaps it would have been better if they made it clearer rather than using medical terminology."
Male, Age 36-50, Urological Cancer
"On admission for my sentinel node biopsy I was asked would I prefer to die at home, in hospital or in a hospice! I found this quite shocking and upsetting to be asked this when I was only just diagnosed, very frightened, and not terminal!"
Female, Age 36-50, Breast Cancer
"I was made to wait 2 hours. The specialist, who I believe is [detail removed], was more interested in their paperwork than explaining my problem and was very insensitive."
Male, Age 66-75, Prostate Cancer
Lack of involvement and choice
This was another aspect of care which appeared to contribute to participants feeling their individual needs were not met (97 comments). Some felt they were not involved in making decisions about their treatment, or felt pushed into making a decision. A small number of patients with breast cancer wondered later whether they should have had preventive mastectomies, but were not offered this as an option at the time. Some participants felt they had been given no choice as to their treatment, that their options weren't made clear to them, or that the options they were interested in were not available to them. Other participants commented that while they had been given options to choose from, they would have valued a recommendation or steer from the experts.
"It is helpful to hear about treatment options, but sometimes it would be good for an expert to tell you what to do. A difficult balance I know, but my GP stepped in when I became paralysed by indecision."
Female, Age 36-50, Skin Cancer
"We only saw the consultant once and that was when we asked to speak to someone about transport and staying at [location removed]. My wife ventured to ask [gender removed] about alternatives to radiotherapy but was abruptly told that this was the treatment decided for me. Very upsetting! Never saw them again!"
Male, Age 66-75, Prostate Cancer
Poor emotional support and responsiveness
Many participants felt that they did not get the level of emotional support which they needed (270 comments). Types of support sought by participants included sympathy, reassurance, counselling, contact, help with emotions, detailed explanations, someone to talk to, company, practical advice, and being warned or prepared for next steps. Comments suggested that patients felt unsupported if they did not have contact during and after treatment with the people they perceived as being providers of support, for example if they were not assigned a clinical nurse specialist, or had only briefly or never met a specialist nurse; or were not able to access a Macmillan nurse. Continuity of support was an issue for some participants if their assigned nurse was part-time, went on holiday or changed role and they were not made aware of a replacement contact. Lack of support during and after treatment left patients feeling alienated, isolated and alone.
Several participants commented that they had not brought family or friends with them to an appointment, including at the time of diagnosis, because they had not been expecting to receive a diagnosis. This was usually because they were attending for a biopsy and didn't expect to receive the results so quickly, or because they had previously been led to believe that their tumour was probably benign. Participants felt that some prior warning that they might receive a cancer diagnosis would have helped them to prepare for the news.
"When I was having chemo I did get a little depressed and felt very isolated. I did go to my GP and asked for help just to talk to someone, they said there was nothing. So I just had to get on with it. It was a lonely time for me, but I just got on with it. There was the Macmillan at [hospital name removed] but when you are so ill, it was hard for me to go there."
Female, Age 51-65, Colorectal Cancer
"I met my clinical nurse specialist for the first time at a three monthly follow-up clinic, eighteen months after my surgery. It would have helped me a great deal to have met her at the time."
Female, Age 51-65, Tumour group not known
"I had a biopsy taken and I was told twice by the nurse/doctor performing this that "it was certainly nothing to worry about". I had no idea I was going to be told the news I did and if I had an inkling, I would have taken my husband or a family member with me."
Female, Age 36-50, Head and Neck Cancer
Lack of information
Many participants did not receive the amount or type of information they required to meet their individual needs (407 comments). For a small number of participants, this meant being given too much information at once, leading to participants feeling rushed, struggling to process the information, and in some cases making patients feel anxious and frightened. However, more frequently, participants felt they did not receive enough information, in particular information about side effects of treatment. Many participants felt that prior to making decisions about treatment, they would have liked to receive a much more detailed explanation of treatment, what to expect, and likely or potential side effects and consequences of treatment. After treatment, participants would have appreciated more detailed advice and information on how to recognise and manage side effects, and how to self-care after surgery, including receiving realistic information about recovery times.
The other area where participants felt they received inadequate information was around being signposted to additional services. Many participants had individual needs for welfare advice, emotional support, physiotherapy, and nutritional advice, which could have been met by other NHS services or charities, yet the participants were not told about these services.
"Macmillan support, Maggie Centre, financial advice etc. Nothing was ever mentioned or offered at any time, by anyone."
Female, Age 66-75, Colorectal Cancer
"Information about side effects too vague e.g. you might get this, you might get that, not how bad it could be or what to do about it. The nurse who gave me the drugs to take home went through everything very quickly with no written information. The information on the [word unreadable] were inadequate and in one case completely wrong and led to dreadful side effects."
Female, Age 51-65, Haematological Cancer
Lack of support for families
A small number of participants commented on the lack of consideration for their family while they were being treated for cancer (21 comments). Some participants described the difficulties their family members had encountered when trying to find out information from specialists about their care. Another source of concern was the difficulty patients experienced in having family members visit them in hospital or clinics. This was particularly problematic when patients were forced to wait alone for procedures, when they would have felt much more relaxed waiting with a family member.
"My chemotherapy treatment began as an outpatient. I took ill and was admitted to ward [number removed] in [hospital name removed]. I felt that I was not treated there as a person there but a thing on a" to-do list". Although I spent many hours there with nothing happening my wife was excluded after the first 10 minutes. She was even handed a piece of paper saying that this is the ward policy. This was the only time in hospital where I feel the staff had forgotten that patients are human beings. At that point it looked like death was not very far away and emotional support from my wife was very important for me."
Male, Age 51-65, Colorectal Cancer
Specific individual needs
A small number of participants had specific individual circumstances which affected their treatment or care needs (34 comments). Participants felt that these specific circumstances were not sufficiently taken into account for aspects of their diagnosis or care. Particular problems arose for patients (i) with disabilities, or comorbidities; (ii) with a family history of cancer; (iii) whose location meant they were unable to access services; (iv) whose fertility was affected by their cancer treatment. Participants felt that the support provided around their diagnosis or treatment was insufficiently sensitive to their specific needs.
"The cancer treatment affected my fertility but no options were discussed prior to treatment starting and I didn't know there were options available to me until it was too late. This was a really difficult thing to find out as I may have chosen to freeze eggs or embryos and now I can't."
Female, Age 36-50, Breast Cancer
"The service was very slow to give the diagnosis and the attitude of "wait and see" was unacceptable given that the family history indicated a very high risk of that particular type of cancer. A complaint had to be made to bring the appointment forward and on the whole the appointments system was in my view a shambles. Once the diagnosis was made the process was satisfactory and the support outstanding."
Male, Age 51-65, Prostate Cancer
Structures
Participants described a number of problems with the way the healthcare system or environment of care was structured, and these negatively impacted on their experience as a cancer patient. These structural problems included aspects of the care environment, difficulties with transport, inadequate staffing levels and lack of privacy.
Care environment
Comments about the care environment (145 comments) were most often related to staying overnight in hospital, and included: concerns about the food not being suitable for specific cancer patient needs or not meeting clinical recommendations following certain types of treatment; hygiene issues, especially in relation to shared ward toilets; high noise levels on wards, particularly ward staff chatting loudly at night when patients were trying to sleep; and uncomfortable beds and chairs. Participants also commented negatively about problems with bed or chair availability and how these impacted on their experience, both as inpatients and during outpatient chemotherapy treatment. Bed availability was a particular problem at admission, and again at discharge, with some patients being left in pain for hours without a bed. Several participants commented on insufficient or broken facilities impacting on their comfort or their care, for example broken buzzers, lights, televisions, or lack of blankets, dressings, colostomy bags.
"I had operation in [hospital name removed], my week in unit [name removed] was very good, nursing staff to patient ratio excellent. But then in general ward not enough staff to deal with amount of patients who needed some form of assistance and at weekends ran out of dressings/towels and bedding because stores closed. Staff were excellent but understaffed and overworked."
Male, Age 51-65, Upper Gastrointestinal Cancer
"Noisy ward at night. Nursing talking/giggling. No concern for patients trying to sleep."
Male, Age 51-65, Colorectal Cancer
Transport
Problems with transport contributed to a very negative cancer experience for the relatively small number of patients who commented on this (49 comments). Difficulties included: problems with parking; ineligibility for, or lack of availability of patient transport, meaning some patients had to travel home after chemotherapy or surgery on public transport; and the high cost of transport. Cancer treatment and diagnostic tests being carried out in multiple locations meant that patients often had several long journeys in one week, even though they were feeling poorly; this was particularly problematic if appointments were made for first thing in the morning. Although only affecting a very small number of patients, cancer care for people from the Islands was notably difficult, both due to the lack of support for cancer patients on the Islands, and the difficulties of travelling by ferry when there are no facilities for patients on the boat.
"Found it very tiring travelling [number removed] days per week for 4 weeks to [hospital name removed] for radiotherapy by public transport. I enquired about patient transport, but they could not accommodate my appointment times."
Female, Age 66-75, Breast Cancer
Inadequate staffing levels
Staffing levels were mentioned at all points of the cancer journey (143 comments), but particularly in relation to overnight stays in hospital. Participants felt that wards and clinics were understaffed, and the staff who were working were very busy and had too many patients to deal with. Patients did not want to bother staff because they were so busy, and this meant that patients were unwilling to ask for help or support. Outpatient appointments were rushed due to the volume of patients, resulting in patients not having an opportunity to fully discuss their cancer, not having time to ask questions, and not feeling listened to.
"I'm just out of [hospital name removed] and there were definitely not enough nurses. I would ask for something, the answer would be "back in a minute", but then they would disappear off the planet."
Male, Age 66-75, Lung Cancer
"Felt nurses were busy and I felt I did not and was not able to be spoken to as a person. Breast care nurse allocated I saw about four times. I felt if I managed to get her she would say "need to go" all the time. So I gave up and I still struggling with this very badly."
Female, Age 51-65, Breast Cancer
Lack of privacy
Lack of privacy was a serious issue for a number of respondents (67 comments), particularly at the time of diagnosis and when staying overnight in hospital. At the time of diagnosis, patients felt uncomfortable receiving a cancer diagnosis when there were lots of people in the room, or receiving their diagnosis over the telephone when they were in a public place. When staying overnight in hospital, patients felt intensely embarrassed, vulnerable and exposed to have personal details about their treatment and cancer prognosis discussed on the ward with only a curtain separating them from other patients. Several colorectal cancer patients also mentioned how undignified they felt during procedures, and while learning how to manage drains and stoma on a ward.
"Ward with several patients sharing meant there was no privacy to discuss my condition or treatment. Everyone could hear everything. I had an unplanned stoma and had to learn to manage it on a shared ward with one toilet. I didn't want anyone to know I had a stoma, but it felt like everyone did. I found the lack of privacy very distressing. There wasn't even anywhere I could cry in private."
Female, Age 51-65, Colorectal Cancer
"My abiding memory about being told what was wrong with me was lying in a ward with the curtains drawn around the bed. I was fairly bluntly told that there was nothing that could be done to help me. It was pretty shocking and when the curtains were opened I knew that everyone else on the ward had heard too. My [family member removed] was with me but I still felt very exposed, vulnerable and helpless."
Female, Age 66-75, Tumour group not known
Processes
Participants also described numerous problems with the organisation of treatment and care. Processes which negatively affected their experience included ineffective and unreliable administrative systems, waits and delays and fragmented care.
Administrative systems
Participants described struggling with a number of the processes used by the NHS to manage patients including administration of letters and appointments, administration of patient notes, and call handling (289 comments). Problems with the administration of letters and appointments included: delays for letters to be sent to GPs and patients; no appointments being sent out for scans, surgery, the start of radiotherapy and chemotherapy, and follow-up clinics; and appointments being cancelled or postponed without adequate communication. Participants described the administration system as being 'not fit for purpose' and chaotic, and viewed this as putting their healthcare at risk. A frequent concern of respondents was that they had been told by clinical staff that they should have regular follow-ups after cancer treatment, however, the administration system either reduced the frequency of appointments, or regularly sent the appointments out months late, so that the patient never received the level of follow-up care apparently recommended by clinicians.
Many respondents commented on the inefficient administration of tests and scan appointments in relation to follow-up clinic appointments with specialists – with tests frequently occurring after follow-up appointments, meaning that test results weren't discussed until the next appointment which was often months later. Administration of patient notes and test results was an issue for several participants, who reported notes and results going missing or being mislaid. Problems with call handling included difficulty with getting hold of named contacts, calls not being returned, delays in response times to calls, and patients not being given correct phone numbers to call for assistance.
"Follow up appointments not adhering to the six monthly timescale I was told about. I also feel that as a patient I should be informed of results of tests undertaken as soon as possible. Recently I had an ultra scan and x-ray carried out and my next appointment with my consultant is not until four months later. It would be re-assuring to know that everything is fine."
Male, Age 51-65, Urological Cancer
"Firstly I was given an incorrect number. When I did eventually make contact my nurse was on leave and the person who answered my call was unable to advise me. A follow-up call went unanswered for so long that the reason had become irrelevant. I did not call again."
Male, Age 51-65, Prostate Cancer
Waits and delays
The greatest number of negative comments in this theme concerned waits and delays (454 comments). These were frequently made alongside comments about ineffective administration. Participants experienced waits and delays waiting for appointments, waiting for surgery, and sitting waiting on the day for outpatient and chemotherapy appointments. Participants described experiencing a high level of stress and anxiety due to waits and delays, and in some cases reported that their cancer had progressed or spread during the time they were waiting to be treated.
Three circumstances were frequently described as being associated with difficult periods of waiting (i) being on the waiting list for surgery for much longer if the patient had chosen breast reconstruction instead of mastectomy only; (ii) waiting for hours in the hospital for an operation with no food or water after being asked to come in for a morning appointment; (iii) waiting for hours to receive chemotherapy because the drugs had not been sent down from the pharmacy.
"Felt pressurised into just having mastectomy. They said everything I wanted involved two surgeons and was a very hard operation. Told mastectomy could be done within 6 days, yet had to wait 9 weeks approx. for my reconstruction and mastectomy op. Too long."
Female, Age 51-65, Breast Cancer
"Had to be at hospital on morning of operation for 7:30. However, was left sitting in the waiting room till after lunch before being given a bed, then left till 5pm until called for surgery. As never had surgery before, found just being left all day very stressful."
Female, Age 66-75, Breast Cancer
Fragmented care
Many participants described receiving treatment and care which seemed fragmented because numerous people were involved from different departments and hospitals (276 comments). Participants expressed the negative effect this fragmentation had on their anxiety levels and confidence in their treatment. Particular issues outlined by patients included that: different teams didn't have access to notes and there was poor communication between departments; different people involved didn't know what tests or procedures the patient had already received, and made conflicting decisions about treatment plans; the patient had no point of contact regarding their treatment and felt that no health professional had ownership or control of their case as a whole; overall, patients described a lack of continuity of care, feeling passed around and receiving a varying quality of treatment which was not joined up.
"Other than my consultant [name removed], the other doctors at both the [hospital names removed] do not seem to know any details at all about me or my treatment, even asking me what medication and dosage I am on."
Male, Age 51-65, Head and Neck Cancer
"I did not like that there was no apparent overall control. I was sent to different specialists who only spoke about their own expertise."
Male, Age 51-65, Urological Cancer
Analysis of Individual Comment Boxes
Each of the seven free-text comment boxes were analysed at the sub-theme level to identify the major issues for patients at that point in their cancer experience. All subthemes which represent at least 5% of the comments for that comment box are included in the following charts. All subthemes which represent less than 5% of the comments for that comment box are amalgamated into the 'Other' section for each chart. Although there is no double-counting of respondents' comments within any sub-theme, an individual respondent could contribute to more than one sub-theme in any given comment box if their free-text comment covered several issues.
The lead up to diagnosis and finding out what was wrong with you (Comment Box 1)
Positive
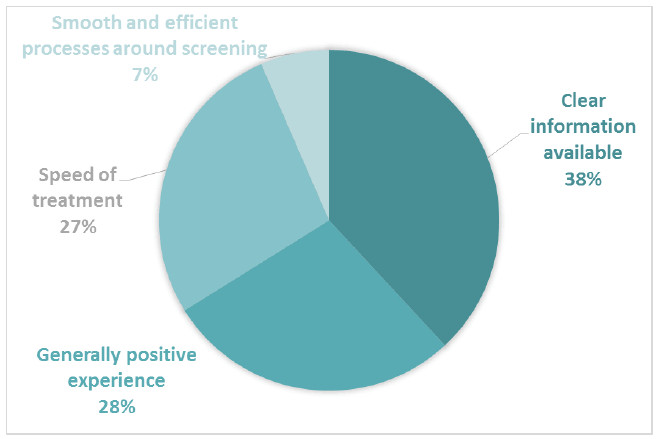
Analysis of the positive subthemes for Comment Box 1 indicate that respondents valued being given clear information, having a generally positive experience, and speed of treatment (Figure 3). 567 positive comments were coded into subthemes in Comment Box 1.
Figure 3 Positive subthemes for Comment Box 1 – Lead up to diagnosis
Negative
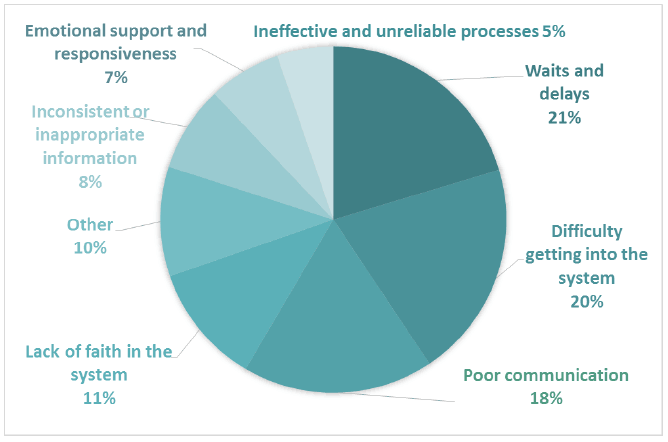
Breakdown of the negative subthemes for Comment Box 1 indicates that patients had particular issues with waits and delays, difficulty getting into the system, and poor communication in the lead up to diagnosis (Figure 4). 987 negative comments were coded into subthemes in Comment Box 1.
Figure 4 Negative subthemes for Comment Box 1 - Lead up to diagnosis
Decisions about treatment (Comment Box 2)
Positive
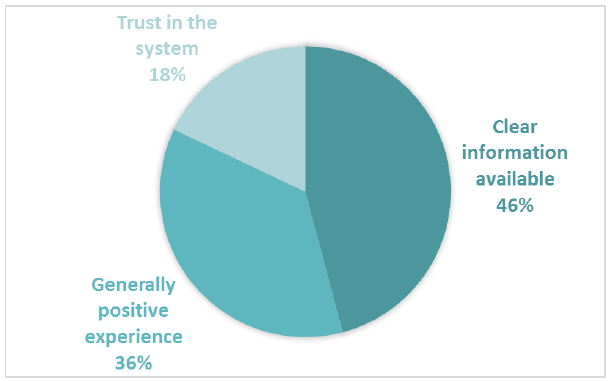
The most common positive subtheme for Comment Box 2 was having clear information available (Figure 5). Participants liked receiving explanations about treatment and procedures, having their options clearly explained and having their expectations set about outcomes, at the time of decision making about treatment. 423 positive comments were coded into subthemes in Comment Box 2.
Figure 5 Positive subthemes for Comment Box 2 – The way decisions were made about treatment
Negative
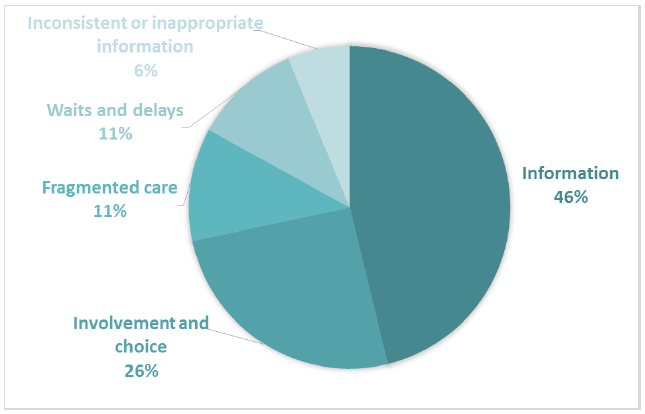
Breakdown of the negative subthemes for Comment Box 2 indicates that patients' negative experiences of the way decisions were made about treatment centred around unmet information needs and lack of involvement and choice in decision making (Figure 6). Participants described unmet information needs at the time of decision making in terms of being given inadequate explanations of treatment, outcomes or side effects. Several participants commented that a clearer knowledge of likely side effects might have changed their treatment decisions; others felt that being prepared for side effects would have helped with self-management after treatment, and reduced needless worry about whether symptoms were side-effects or new cancer symptoms. 353 negative comments were coded into subthemes in Comment Box 2.
Figure 6 Negative subthemes for Comment Box 2 - The way decisions were made about treatment
Support (Comment Box 3)
Positive
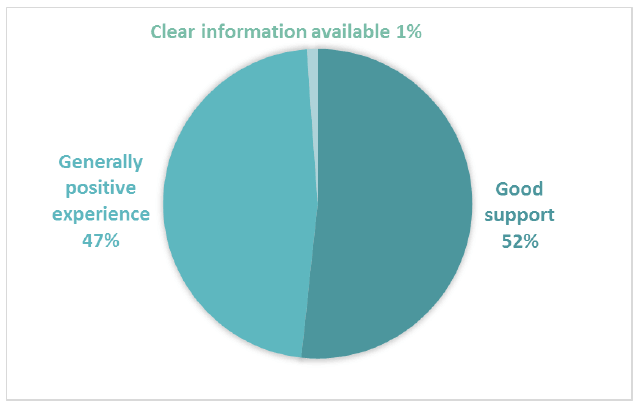
Over half the positive comments in Comment Box 3 related to receiving good support (Figure 7). Participants were often positive about the support they received from a clinical nurse specialist or other cancer specific nurse, describing staff as supportive and approachable, and available to offer support. Participants also described receiving support from a range of charities. 621 positive comments were coded into subthemes in Comment Box 3.
Figure 7 Positive subthemes for Comment Box 3 – The support you received
Negative
Breakdown of the negative subthemes in Comment Box 3 shows that common issues related to negative perceptions of support included lack of emotional support and responsiveness and lack of information (Figure 8). The concept of 'support' meant different things to different participants, with frequent interpretations of the word support being sympathy, contact, counselling, detailed information and signposting to services. Respondents to this comment box described that lack of emotional support left them feeling alienated and alone. Many described having had expectations that they would receive emotional support and care from their clinical nurse specialist ( CNS), but feeling that in reality their CNS was busy and did not have time to maintain contact with them. This comment box came directly after explicit questions about the CNS, which may explain why CNSs were specifically mentioned in the comments. Many patients also commented on receiving fragmented care, and on ineffective and unreliable processes. 446 negative comments were coded into subthemes in Comment Box 3.
Figure 8 Negative subthemes for Comment Box 3 - The support you received
Operation or overnight stay in hospital (Comment Box 4)
Positive
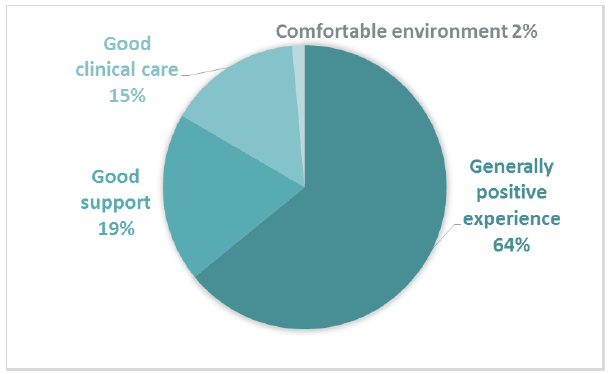
The majority of positive comments about having an operation or overnight stay in hospital related to having a generally good experience (Figure 9). Participants also commented positively about receiving good support and good clinical care. 705 positive comments were coded into subthemes in Comment Box 4.
Figure 9 Positive subthemes for Comment Box 4 – The care you received when you had an operation or stayed overnight in hospital
Negative
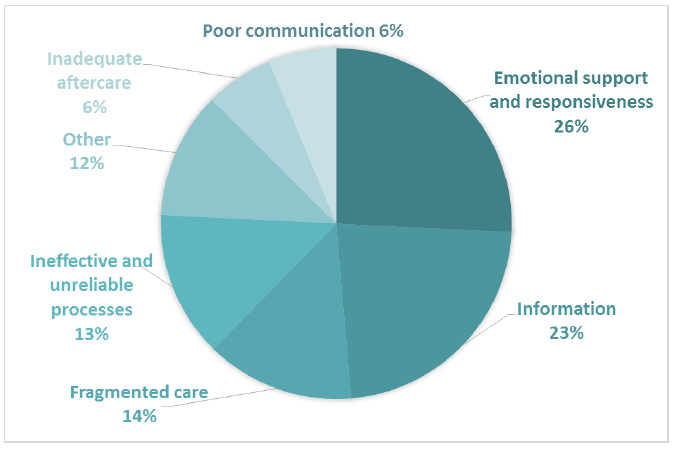
Several issues emerged in response to Comment Box 4 (Figure 10). The most frequent negative comment related to receiving poor care – patients feeling that their individual needs were not being addressed, particularly in relation to side effects, pain and bowel issues; feeling that general ward staff did not understand the specific needs of cancer patients; and feeling ignored and isolated when staying overnight in hospital. Other common issues related to the environment being uncomfortable or unsuitable, and inadequate aftercare, for example being discharged too quickly, or not receiving help with how to self-manage. 662 negative comments were coded into subthemes in Comment Box 4.
Figure 10 Negative subthemes for Comment Box 4 - The care you received when you had an operation or stayed overnight in hospital
Day patient/outpatient care (Comment Box 5)
Positive
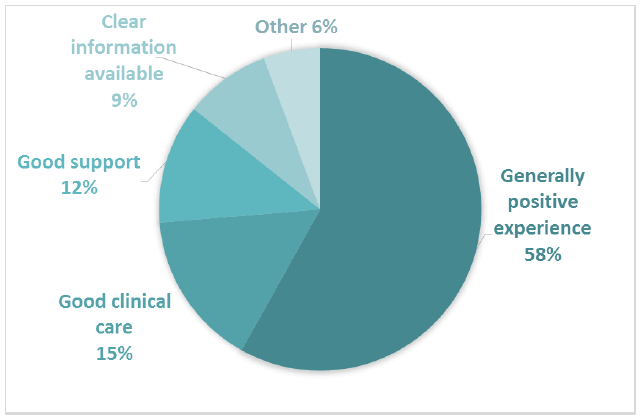
Breakdown of the subthemes for Comment Box 5 indicated that most positive comments described having a generally good experience (Figure 11). Participants also commented positively about receiving good clinical care and good support. 475 positive comments were coded into sub-themes in Comment Box 5.
Figure 11 Positive subthemes for Comment Box 5 – The day patient/outpatient care you received
Negative
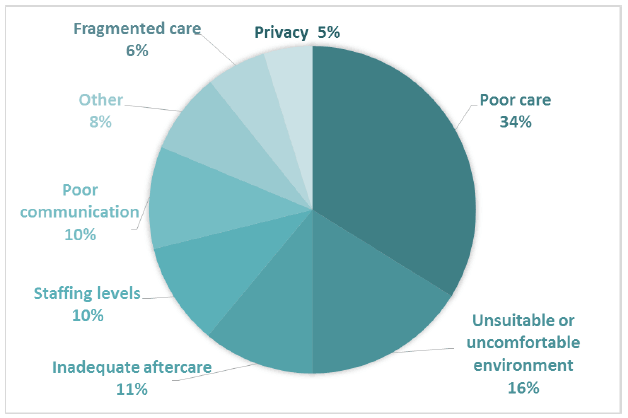
Of the negative sub-themes raised by participants about day patient and outpatient care they received (Comment Box 5), the most common related to fragmented care, waits and delays, and ineffective and unreliable processes (Figure 12). Fragmented care was described by participants as a lack of continuity of care, with poor communication and access to notes between departments, hospitals and the GP. 289 negative comments were coded into sub-themes in Comment Box 5.
Figure 12 Negative subthemes for Comment Box 5 - The day patient/outpatient care you received
Chemotherapy/radiotherapy treatment (Comment Box 6)
Positive
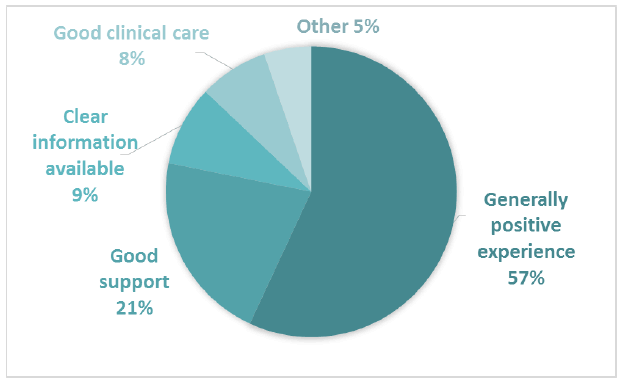
The majority of positive comments for Comment Box 6 related to having a generally good experience, and receiving good support (Figure 13). 325 positive comments were coded into subthemes in Comment Box 6.
Figure 13 Positive subthemes for Comment Box 6 – Chemotherapy/Radiotherapy treatment
Negative
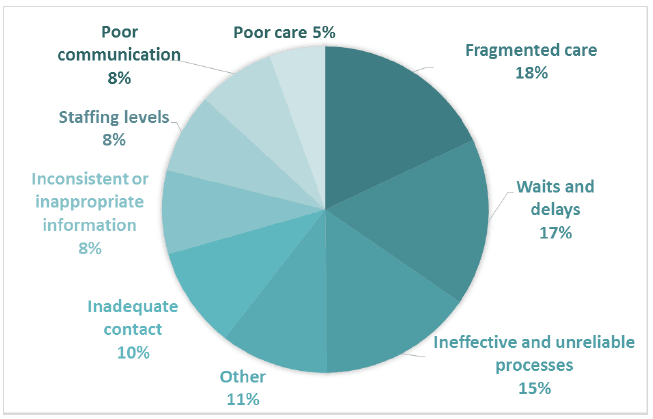
The breakdown of negative subthemes in Comment Box 6, showed that respondents had no single major issue with chemotherapy/radiotherapy treatment (Figure 14). The most common issues raised were with a lack of information, and lack of emotional support and responsiveness. Lack of information in the context of chemotherapy/radiotherapy was attributed to participants feeling that they had not been given sufficient information or explanation about potential problems with treatment or side effects, or about the long term effects of treatment. Lack of emotional support and responsiveness referred to staff solely focusing on the clinical aspects of care during chemotherapy/radiotherapy sessions, and not providing patients with any emotional support. 194 negative comments were coded into sub-themes in Comment Box 6.
Figure 14 Negative subthemes for Comment Box 6 - Chemotherapy/ Radiotherapy treatment
Experience of cancer care (Comment Box 7)
Positive
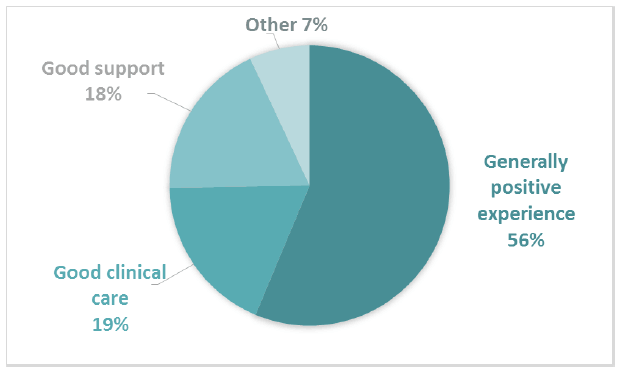
847 positive comments were coded into subthemes in Comment Box 7, which asked patients to comment on anything else about their experiences of cancer care. The most common subthemes were having a generally positive experience, receiving good clinical care, and having good support (Figure 15).
Figure 15 Positive subthemes for Comment Box 7 – Experience of cancer care
Negative
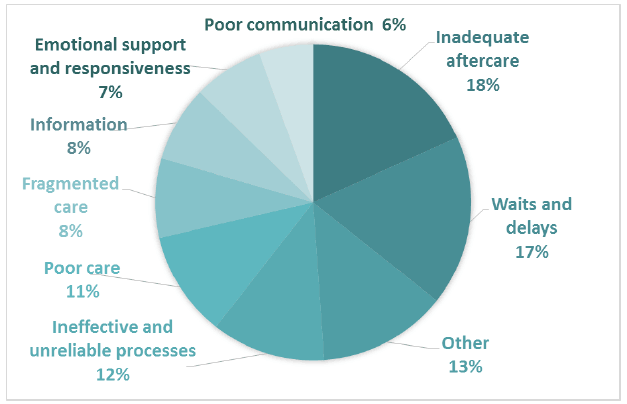
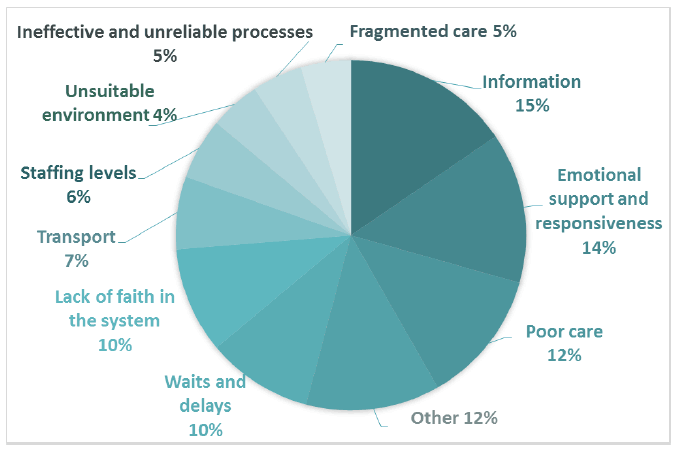
849 negative comments were coded into subthemes in Comment Box 7. The most common subthemes were receiving inadequate aftercare, and waits and delays (Figure 16). Patients described inadequate aftercare as receiving no care or follow-up after treatment, feeling alone and not receiving support from GPs and district nurses once hospital based treatment had ended.
Figure 16 Negative subthemes for Comment Box 7 - Experience of cancer care