Scottish allied health professions public health strategic framework implementation plan: 2022 to 2027
In 2019, the first UK wide Allied Health Professions (AHPs) Public Health Strategic Framework 2019-2024 was published by all four nations, intended to help AHPs and partners to further develop their role in public health. Thereafter, each nation agreed to develop their own implementation plan.
Appendix 1: AHPs in Action – Examples of Good Practice
AHPs represent a diverse range of professions that work across a broad range of settings, which can make it more challenging to understand the myriad ways in which their work can improve upon public health. This section provides case studies that demonstrate just how innovative and important AHP interventions with a clear public health focus can be for the people who receive their services.
All case studies have been reproduced with permission from the author.
Case study 1: Speech & Language Therapy – a transformational approach for children and young people, NHS Forth Valley
Beginning in 2019, NHS Forth Valley Speech and Language Therapy (SLT) has worked in partnership with three local authorities to undertake a transformational approach to improving outcomes for children and young people (C&YP). Amongst the key drivers for change was the need to address health inequalities, with recognition that many families living in poverty were not accessing AHP expertise in the traditional 'refer, assess, treat model'. We aimed to answer the fundamental question; 'What do children with communication needs require in order to be safe, healthy, achieving, nurtured, active, respected, responsible and included?'
Our shared vision is that C&YP in Forth Valley will demonstrate improved outcomes through access to a SLT service that is based on relationships, is accessible, person centred, outcome focused, integrated and delivers quality universal, targeted and individualised support.
Outcomes
- Speech and Language Therapists are now closer to the communities we serve, working with individual education settings to offer a balanced system (Gascogne, 2018) with quality universal, targeted and individualised approaches to the many children with an 'unseen need.'
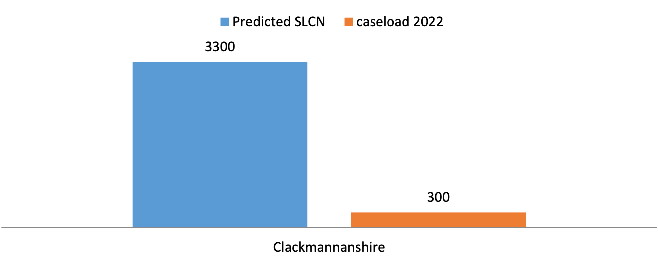
- In Clackmannanshire for example, 3300 C&YP have a predicted Speech, Language and Communication Need (SLCN). As the current caseload is 300 C&YP, this indicates that individualised supports alone would only meet the needs of 10% of C&YP with SLCN.
- This academic year, C&YP in Clackmannanshire have accessed targeted and universal SLT support through
- Environment– 15 education placements trained in excellent communication environment
- Workforce - An increasingly skilled and knowledgeable workforce – 46 training events delivered within placements to 530 staff in total
- Identification – 252 targeted, pre-request support conversations with education staff
- The request rate from education has dropped from 55% to 34% between 2018/19 and 2021/22
- Intervention - SLTs delivering interventions in whole classes 50 times, and in targeted groups 44 times.
C&YP are now accessing expertise without the need for a request for assistance and as we increase our early intervention and prevention offers fewer C&YP are requiring to be stepped into individualised level.
In partnership with education we have transformed our service. A greater number of C&YP living in poverty are accessing quality services closer to their community and there is evidence to demonstrate that we are closing the spoken language gap, improving attainment, participation and the wellbeing of the people we serve.
Case Study 2: Art Therapists at the Start, Dundee
'Art at the Start' offers a range of arts-based interventions to promote the mental health and wellbeing of parents and their infants (aged 0-3 years). It is a collaboration between University of Dundee and Dundee Contemporary Arts, running from 2018-2022, led by an art therapist. The project aims to support infant mental health by building strong attachment relationships through art making. By embedding an art therapy service within a gallery, a public building with visible creativity and a social community space, and by providing a spectrum of art-based activities, the art therapist is able to meet the needs of a diverse range of families:
- Parent-infant art therapy groups support poor attachments and parents struggling with their mental health through targeted referrals. They help parents and infants to experience positive interactions by engaging in playful art making together, whilst giving therapeutic support to parental wellbeing, encouraging attuned responsive parenting, and increasing behaviours which build secure attachments.
- Messy play sessions, open to all parents and infants aged 0-3 years, encourage engagement with the gallery and more shared art making, giving parents ideas and infants new experiences and potential for connection through art making. Outreach through additional activity within the community, targeting marginalised groups, helps to broaden participation in these sessions.
- Home Art Boxes supported vulnerable families during COVID-19 lockdown by providing materials and encouragement for parents to try art making with their infants at home.

Feedback and outcomes
Feedback shows families involved in the project have appreciated the opportunity to get involved in the arts and the support offered. Results from the Art Boxes showed that they encouraged positive interactions between young children and their parents (Armstrong & Ross, 2021) with increased parental involvement in the play and positive signs of infant engagement. In pilot results from our parent-infant art therapy, parental wellbeing increased, as did positive, attachment-focused, behaviours (Armstrong et al, 2019), offering an early intervention which could have a long-term impact on children's mental health and parental recovery from perinatal mental health conditions.
Case Study 3 – Physiotherapy Programme at Robert Gordon University – NHS Orkney
As part of the newly developed undergraduate Masters of Physiotherapy programme in Robert Gordon University (RGU) which incorporates public health learning, a split physiotherapy student placement was established in NHS Orkney between the Paediatric Physiotherapy Service and the Public Health Department. This placement was an opportunity to consolidate and embed the principles of Public Health learnt through the undergraduate physiotherapy programme in RGU into practice.
To achieve the learning outcomes required within the Public Health aspect of the placement, the student was given opportunities to visit partner organisations with a focus on child health and wellbeing such as Home Start Orkney and Bookbug sessions. A child health and wellbeing focus was chosen as much as possible to support the connection between the two split areas of work.
Within the department, the student shadowed smoking cessation staff and the WELL programme staff who deliver face to face public health-based interventions to individuals. The student was challenged to use their developing people skills and note taking skills to practice how they would approach these interventions. They observed 'Living Life to the Full' group sessions lead by Public Health and then were supported to develop and deliver desk-based exercise workshops for delivery to staff at Orkney Islands Council.
Within this placement, the student was required to present to the Public Health team on the topic of 'How to Achieve a More Active Scotland'. This activity challenged the student to consider the national and local context of physical activity in Orkney and make evidence-based recommendations for future Public Health work.
The student managed well with the split placement and achieved the outcomes required in both areas of work. The main benefits from the Public health aspect of the placement which the student identified were increased knowledge of the Public Health system, being aware of services to sign post people to and learning how to communicate with people in relation to sensitive issues.
RGU has a commitment to offering authentic and contemporary placements to its physiotherapy students. This partnership with NHS Orkney allowed the student to explore at first hand the importance of Public Health and role of physiotherapy within Public Health. This placement also offered development of broader professional skills including communication, collaboration, networking, and partnership working all of which are essential for the evolving healthcare environment.
Case Study 4 - Get Nourished: preventing, identifying and treating malnutrition in older people in Dundee – NHS Tayside
It is estimated that one in ten people over the age of 65 are malnourished or at risk of malnutrition. It is both a cause and consequence of ill-health but is often overlooked1. It was predicted that the COVID-19 pandemic would exacerbate nutritional risk due to limited access to shopping and a reduction in essential care and support2. Restrictions on face-to-face activities required innovative ways of working and partnership with a number of organisations. Five initiatives were used to prevent and improve the detection and management of malnutrition in older people in Dundee.
1. Staff and volunteers were trained to use the Patients Association Nutrition Checklist to identify people at risk of malnutrition, give basic advice and signpost to services for further support. Feedback indicated that it was easy to use.
2. A telephone advice line was established for people concerned about malnutrition risk either in themselves or someone they care for. Individuals were screened for malnutrition risk, provided with first line nutritional advice and signposted to other services where appropriate. Seventy people called the advice line over a one year period, 51% of whom were able to fully implement the advice provided and 25% implemented it partially.
3. People identified as being at risk of malnutrition were offered Boost Boxes. These contained 14 nutritious snacks to provide extra nourishment when appetite was reduced. Trained volunteers delivered the Boost Boxes, reviewed their use weekly and refilled the boxes where appropriate for three weeks. Ideas for suitable snacks were discussed if appetite remained reduced after the three-week period, enabling self-management of long term conditions to prevent avoidable admissions to hospital or care homes. Over a one-year period, 150 Boost Boxes were delivered. Some of those referred had complex and chaotic lives and food insecurity was the main issue rather than poor appetite. Availability of Boost Boxes needs to be continuously advertised to promote their use.
4. An existing supper club was adapted to provide a weekly meal delivery service and social check-in. Meals were cooked by staff in a local school that had been furloughed and delivered by healthcare support workers. Additionally they received weekly telephone calls to reduce social isolation. Between March and October 2020, over 3000 meals were delivered and over 1600 phone calls were made. Evaluation indicated a number of benefits including being better nourished, feeling physically healthier and feeling valued and supported by the community. One recipient commented "It has helped me a great deal especially as I have no family nearby. Getting a phone call and knowing where to turn for support is brilliant. I really appreciate everything. I would like to come to the supper club when it starts up again."
5. Short training videos were developed and made available on YouTube, which enabled training to be delivered quickly, efficiently and consistently. A professionally produced training video on recognising the signs of symptoms of malnutrition is being developed. This will be endorsed by the Care Inspectorate and Healthcare Improvement Scotland, with the aim that care providers will include it within their mandatory training.
References
1Malnutrition Task Force (2021) State of the Nation 2021: Older People and malnutrition in the UK today. Available from https://www.malnutritiontaskforce.org.uk/ (Accessed: 28th February 2022).
Contact
Email: abigail.parkin@gov.scot