Rights, respect and recovery: alcohol and drug treatment strategy
Scotland’s strategy to improve health by preventing and reducing alcohol and drug use, harm and related deaths.
Chapter 3: Context and Challenges
| High-risk alcohol and problematic drug use remains high |
Drug related deaths and hospital admissions are increasing and remain too high for alcohol |
Problematic alcohol and drug use disproportionately impacts deprived communities |
| Complex needs of an ageing population |
More needs to be done to protect those most at risk of harm and death |
Dynamic and changing drugs market and challenges |
| Stigma remains a significant barrier |
Services need to be person-centred, trauma-informed and better integrated |
The whole family needs support |
| Respect, diversity and ensure equity |
Fewer people (including young people) are using drugs and drinking alcohol |
Recovery communities are flourishing |
| Information and evidence is vital |
The Justice System has a role to play |
Need to build on Partnership working |
1. There are a number of key challenges which we face today, many are interconnected or underpinned by the same socio-economic and demographic challenges.
Harmful alcohol and drug use remains high compared with similar countries
2. It is a challenge to reliably estimate the size and scale of problematic alcohol and drug use. However, the most recent prevalence study estimated 61,500 individuals, aged between 15-64, were engaged in problematic use of opiates and/or benzodiazepines in Scotland[6] and it is estimated that around 4% of the adult population have possible alcohol dependency[7]. This means that it is likely that we all have someone in our life who has experienced these challenges.
Drug related deaths and hospital admissions are increasing, and remain too high for alcohol
3. Nine hundred and thirty four people lost their life to a drug related death in Scotland in 2017 - the highest number ever recorded and more than double the number recorded in 2007. There has also been a corresponding rise in drug related hospital admissions and repeat stays.
4. Alcohol-specific deaths and hospital admissions have reduced in recent years but remain far higher than they were in the early 1980s[8].
Deaths 2017:
1,120 Alcohol-specific
934 Drug-related
Drug-related deaths by age, Scotland, 1996-2016
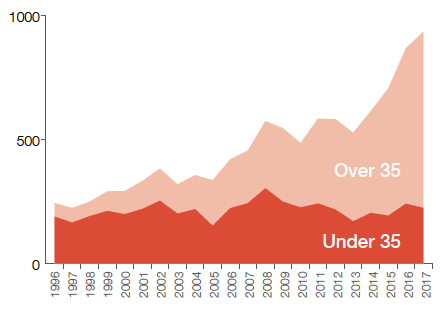
Stays in Hospital 2016/17:
8,546 Drugs
36,235 Alcohol
(93%+ Emergency Admissions)
Alcohol-specific deaths in Scotland, 1981 to 2017
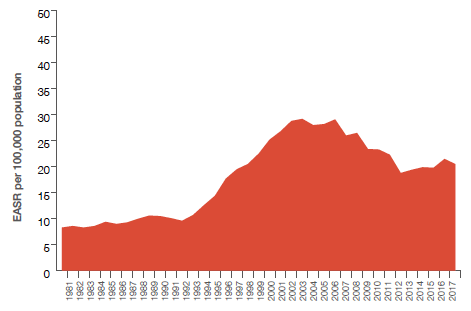
Source; Health Scotland: NRS data[9], [10]
Problematic alcohol and drug use disproportionately impacts deprived communities
5. Our ambition, as set out in the Fairer Scotland Action Plan, is ‘to build a better country - one with low levels of poverty and inequality, genuine equality of opportunity, stronger life chances and support for all those who need it.’
6. The NHS Health Scotland Burden of Disease study highlights that alcohol and drug dependence are major contributors to absolute inequalities and recommends that alongside other measures we must tackle conditions that are more prevalent within higher levels of deprivation[11]. This Strategy reaffirms our commitment to this aim.
| The disease burden of drug use disorders is 17 times higher and alcohol dependence 8.4 times higher in the most deprived areas compared with the least deprived areas[12]. |
Hospital Admissions 54% 41% were patients living in the 20% most deprived areas[13]. |
29% of those living in the 10% most deprived neighbourhoods felt that drug misuse was a ‘very’ or ‘fairly’ common local problem compared with 12% overall[14]. |
An ageing population of higher risk alcohol and problematic drug users bring with it complex additional health challenges
7. There is a clear trend of an ageing population of users for whom drug use has become more harmful over time[15]. As evidenced by the steep rise in drug related deaths in recent years. In addition, while harmful use of alcohol is increasing among older adults[16].
8. Older service users are more likely to present with complex multi-morbidities, often having used drugs and alcohol for many years.

Source: NRS, 2018.
Dynamic and changing drugs market and challenges
9. The drugs market is increasingly dynamic with a rapid growth in new psychoactive substances as well as new routes to market through the internet, dark web and social media. Concerning new drug trends include an increase in the prevalence and potency of many drugs in the market including cannabis, cocaine and benzodiazepine-type drugs alongside an increase in poly-substance use, which is a particular concern for the most vulnerable population of people who use drugs.
More needs to be done to protect those most at risk of harm and death
10. The pioneering National Drug Related Deaths Database[18] and recently commissioned Dying for a Drink[19] study give us a valuable insight into the life circumstances of those most at risk of harm and death.
11. While we know that being in treatment is a protective factor we must also endeavour to reduce the harms experienced by those who feel unready for treatment. Incidences like the recent HIV outbreak in Glasgow among people who use drugs highlight the importance of harm reduction measures and a co-ordinated response.
| 281 Injecting Equipment Provision outlets distributing over 4.4 million needles and syringes per year[20]. |
A total of 46,037 take-home Naloxone kits were supplied in Scotland between 2011/12 and 2017/18[21]. |
Initiatives such as Housing First provide |
Stigma remains a significant barrier
12. People who experience alcohol or drug problems, either through use or by association, often experience the most stigma in our society. Negative attitudes and stigma from society, from professionals within services, and self-stigmatisation, can be one of the biggest barriers to accessing treatment, community services and other activities. Stigma needs to be challenged across the sector and society.
13. The language used in this strategy conforms wherever possible to the Global Commission on Drugs Policy guidelines[22] to help combat stigma.
Services need to be person-centred, trauma-informed and better integrated
14. Many people attending alcohol and drug services are thought to have a history of trauma (as well as being particularly vulnerable to experiencing further trauma)[23]. Studies have consistently shown a high prevalence of comorbidity of mental disorders in people who have problems with alcohol and drugs and clear connections with homelessness and interactions with the criminal justice system.
15. People need support from professionals across a wide range of services and more integrated approaches are needed to address homelessness, mental health problems, unemployment and general healthcare needs. It is this integration which is fundamental to the success of this strategy.
| A high of rough sleepers and 1 in 5 of all people who experienced homelessness had health interactions for drug or alcohol use.[24] |
The most frequent psychiatric comorbidities among people who use drugs are depression, anxiety and personality disorders.[25] |
The whole family needs support
16. Alcohol and drug use by a loved one can cause trauma and distress for their families[1], often leading to relationship breakdown and increased caring responsibilities. Family members can play an important role in supporting the recovery of a loved one but also need support in their own right.
| Multiple ACEs: |
16% of people in treatment for drug use are living with their friends/families, 16% are living with a spouse/partner[27]. |
38% of all child protection case conferences cited parental drug and/or alcohol use as |
15: average age of starting drug use by people seeking treatment. (Source: SDMD) |
Respect diversity and ensure equity
17. Services need to be accessible and responsive to all who need them. The last decade has seen new trends in drug use among particular groups including chemsex, practiced mainly by men who have sex with men[29], and a reported increase in the use of Image and Performance Enhancing Drugs such as anabolic steroids[30].
18. While the majority of service users are male, the recent disproportionate rise in drug related deaths among women[31] has made us consider further the challenges of supporting this group. Services are also faced with meeting the often complex needs of a growing group of older people with alcohol and drug problems alongside meeting the needs of young people.
19. We have undertaken an Equalities Impact Assessment in the development of this strategy and a full report of this process will be published in due course.
Fewer people (including young people) are using drugs and drinking alcohol
20. The latest household survey data shows that self-reported levels of both drug use and alcohol consumption levels have decreased (although alcohol sales data suggests a long term increase in overall consumption). Furthermore, drinking and drug taking amongst young people have generally been declining since 2002[32].
| 6% of adults had Source: Scottish Crime and
|
Source: Scottish Health Survey, 2017. |
Source: SALSUS, 2015. |
Recovery communities are flourishing
21. We have seen the rapid growth of recovery communities in Scotland which have grown up alongside existing peer-led mutual aid groups. This has added a new dimension to Scotland’s response to alcohol and drug problems. It has enabled those involved to socialise, reduce isolation and support each other. It has also improved the overall understanding of addiction, and recovery, and the impact of stigma and discrimination.
Information and evidence is vital
22. In Scotland we invest in a wide range of public health surveillance data and intelligence and benefiting from a wealth of excellence and expertise – which includes the voice of lived and living experience. We need to ensure that we maximise the potential of these resources.
The Justice System has a role to play
| 36% of prisoners stated their drug use was a problem for them on the outside; 32% stated alcohol affected their relationships with family[33]. |
Recorded drug crime has fallen by 20% in a decade[34]; Recorded offences for drunkenness in Scotland halved between 2008/09 and 2016/17[35]. |
76% of prisoners tests on reception were positive for illegal drugs[36]. |
23. People with alcohol and drug problems often interact with the criminal justice system, each stage presents an opportunity to engage and support this vulnerable group but we must also look at alternatives and diversions.
24. In 2017 the Scottish Government established the Health and Justice Collaboration Improvement Board[37], to improving collaborative working, reducing health inequalities and reducing the risk of offending.
25. Diverting those with problematic alcohol and drug use away from the justice system and into treatment support, and other interventions that reduce harm and preserve life, is essential. This approach needs to run through how the police lead the work to control the supply of drugs, sentencing, the provision of treatment and support in prison setting, as well as supporting continuity of care on release.
Contact
Email: William Doyle