Family Nurse Partnership in Scotland: revaluation report
Findings from family nurses, the families they work with and wider stakeholders on how the Family Nurse Partnership programme works in practice in Scotland.
4 Findings
4.1 FNP Value
A main aim of the revaluation study was to understand the perceived value of FNP from the perspectives of those operating within the system, through stories generated by clients, their families, Family Nurses and other professionals and wider stakeholders.
In this section, themes that emerged from the collected stories around the value of FNP are presented and discussed with illustrative quotes. The themes are grouped under the following overarching topics – The FNP approach, Value for FNP clients, Value for FNP babies and finally, Value for other professionals and services.
Specifically, these themes highlight that FNP is perceived to add value through:
- the nature of the Family Nurse and client relationship,
- a holistic approach to breaking inter-generational cycles of poor parenting,
- maternal mental health,
- maternal confidence and self-efficacy,
- maternal education and employment,
- minimisation of risk of abuse,
- positive parenting,
- mitigating risks to children - supporting child development,
- interagency working,
- helping to ease the workloads of other services
- helping clients and professionals to engage with each other effectively.
4.2 The FNP Approach
4.2.1 The Nature of the Family Nurse-Client Relationship
FNP aims to help young mothers to make wide-ranging changes to improve the trajectory of their lives, and to give their children the best possible start in life.
FNP is designed in such a way that Family Nurses are able to build strong, trusting relationships with their clients which allow them greater access to their clients’ thoughts, feelings, circumstances and environments than other professionals would traditionally have been able to gain.
From the first engagement with the client enrollment onwards, the Family Nurse works gradually to build up a relationship in which clients feel comfortable and safe opening up to her about their lives. This is a gradual process, in which Family Nurses see themselves as "breaking down barriers [with the client] a little bit at a time" (Family Nurse). They take a non-prescriptive, non-judgmental approach, whereby they do not tell clients what they think that they should do. Rather, they help each client and her partner to reflect (if the partner also chooses to engage with FNP) on their own lives and the environment in which they live, and to begin to see how they can make changes to their lives and environment for the better. As one FNP Lead describes it:
"The Nurse never tells the client what to do. The client is the expert in her own life." (FNP Lead)
The notion that "the client is the expert in her own life" is central to the approach of FNP. Once a trusting relationship has been established and the client begins to reflect on how she could make decisions to improve her life course and the environment in which she will raise her child, Family Nurses seek to instil clients with the confidence and self-efficacy to make positive decisions and take action for themselves. Family Nurses achieve this by taking a strengths-based approach, in which they focus on providing affirmation of clients’ own qualities and inner-strength in order to give them the confidence to take control of deciding what is best for them and their babies.
One client summed up the importance of the trusting, non-judgemental relationship for developing her self-confidence:
"I have more confidence because I got to know you and trust you… it’s better [than other services] ’cos it’s just one person you [clients] see and you don’t judge me" (Client).
Building up this relationship is supported by a range of materials such as FNP’s specially designed resources including "facilitators", along with Partnership in Parenting Education (PIPE) and unique to FNP, the Dyadic and Naturalistic Caregiver Experiences (DANCE) resources.
Facilitators are sets of exercises and discussion topics covering all aspects of the programme which Family Nurses use to facilitate discussions on specific topics in a structured way.
PIPE is an evidence-based interactive educational tool which helps parents to understand their child’s emotional needs, to support attachment and relationship-building, and to encourage play as a way for children to develop and learn.
And DANCE is a validated observation tool that allows the Family Nurse to code and analyse the interaction between the child and his or her caregiver. From this the Family Nurse is able to draw out and build on the strengths demonstrated in the parent-child interactions, and recognise areas for development.
These resources are "agenda matched" to each individual client, based on the Family Nurse’s knowledge of what the client’s needs are, and what a client is able to manage. The importance of adapting to what each individual client is able to manage was summed up by the father of one client, who explained that:
"You [the Family Nurse] understand [my daughter] and show her care. Other services ask too much of her. It stresses her out. I think it’s really valuable as having a baby at a young age is very hard and trying to manage money and dealing with agencies is hard. Having FNP helps with that." (Client’s Father).
4.2.2 A Holistic Approach to Breaking Intergenerational Cycles of Poor Parenting
"Most other services take a topic-based approach to intervention. E.g. they’re for obesity, or smoking, or sexual health. But it doesn’t work like that. None of these single-issue interventions works. Our holistic approach changes the mother and the child…and then the single outcomes appear. The biggest change is to the trajectory of the mother and child’s lives" (FNP Lead)
As this FNP Lead summarises, FNP takes a holistic approach to improving the life course of both clients and babies and breaking intergenerational cycles of poor parenting. Although Family Nurses will focus on single-issues such as healthy diet, reducing smoking, intimate partner violence, sexual health or breastfeeding, each Family Nurse seeks to encourage a far broader change in the life trajectories of each client and her baby. By and large, these changes are seen by Family Nurses as being immeasurable, as they amount to unquantifiable shifts in the way that clients see themselves and their place in their world, and their behaviours across a wide range of domains. As another FNP lead explains:
"We’re not as interested in smoking or breastfeeding as we are in transforming lives. [When trying to quantify FNP] we end up measuring what’s easy to measure, not what’s most important." (FNP Lead)
This is not to say that FNP is not interested in reducing smoking or increasing breastfeeding among their clients per se. Rather, what this FNP Lead seeks to highlight is the idea that much larger changes are needed to make it possible for her to care for all aspects of her child’s development. For Family Nurses, then, it is more important to focus on providing a role model for forging a positive relationship, which clients can seek to replicate in their relationship with their own child, with the intention that this will help drive behaviour changes.
For many Family Nurses, the greatest value of FNP lies in their perceived ability to use this holistic approach, along with the deep, trusting relationships that they build with clients, to break intergenerational cycles of poor parenting and other poor outcomes. Family Nurses report that a some clients appear to have been poorly parented themselves, often with their own parents having not developed strong attachments with them, or having failed to protect them from physical, emotional and sexual violence or neglect. One Family Nurse, for example, saw the value of FNP for one client in the fact that the client was able to keep her child out of care despite several generations of her family having been in the care system as children:
"In one case every child in generations of the family had been taken into care and the FNP client’s child was the first not to have been." (Family Nurse)
This view is supported by a social worker, who suggested that the structure of the FNP visits to a client who herself had been subject to poor parenting as a child was central to helping this client to recognise the difference between poor and positive parenting:
"The early intervention of the FNP Programme has been very valuable and [the client] trusts her Family Nurse. It is evident that [the client] is confident communicating with her Family Nurse and the consistency, and the frequency of visits has played a part in this. [The client] is now able to recognise what is right and what is not right and this is fundamental in breaking cycles [of poor parenting]." (Social Worker)
Family Nurses felt that this was made possible by the emphasis of FNP on helping clients to reflect on their own environments and childhoods, and thinking about the positives and negatives of how their own parents had raised them. As one Family Nurse explained:
"A number of my clients had faced significant vulnerabilities, adversities and trauma in their lives. Most of my clients wanted their child to have a different childhood than what they had experienced themselves. I found my clients to be extremely reflective and understood the actions and/or situations their parents had found themselves in had an impact on their ability as parents. Most of my clients wanted their child to do well in their lives and were able to identify why school did not work out for them and what they could do to change this for their children." (Family Nurse)
Clients, too, spoke of the value of FNP for breaking cycles of poor parenting. One client explained, for example, how her mother failed to care for her adequately when she was using alcohol and drugs. However, she felt that as a result of working with her Family Nurse, she has learned to ensure that if she is struggling, she does not let her mood affect her child:
"When my mum was having a good day she was good but she was often out of her face with drink and drugs… I am very different to that. If I am having a bad day I really try to not let it affect my child." (FNP Client)
Clients, Family Nurses, and other professionals, then, see the specially-designed approach that FNP takes to working with young mothers as extremely valuable. The close, trusting relationships that form between Family Nurses and the clients allow clients to open up in a comfortable, respecting, and non-judgmental environment. It gives Family Nurses the kind of access to clients’ lives which is rarely possible for other professionals due to the limited opportunities that other professionals have to develop deep, trusting relationships. Coupled with the holistic, agenda-matched approach of FNP – focusing on wide-ranging interventions aimed at changing the entire life course of young mothers and their children – this is seen as allowing Family Nurses to foster meaningful, long-lasting improvements to these young women’s lives.
The following sections of this report focus on drawing out the perceived value of this FNP approach – from the point of view of clients, clients’ family members, other professionals, and Family Nurses – in four different areas. First, it will examine the perceived value of FNP for the mothers and children who are the focus of FNP’s work, then it will go on to examine the perceived value of FNP in terms of supporting other services and professionals, and the value of FNP to Family Nurses themselves in both their personal and professional lives.
4.3 Value for FNP Clients
"I am 21 with a 4-year-old son. I came from being 17 and pregnant to a confident, goal driven mum and woman. I am currently finishing studying my degree […] with a future goal of working for FNP and giving back the support and reassurance I desperately needed." (Client)
A central aim of FNP is to improve the life course of FNP clients, in order that they are both set on a path towards a better future for themselves, and that they are able to understand what it takes to provide the best possible care for their children. Family Nurses report that a significant proportion of clients enrol onto FNP with multiple vulnerabilities, many of which can make the prospect of motherhood feel daunting and overwhelming. Family Nurses seek to strengthen their trusting relationships with their clients to help clients to recognise any aspects of their lives which might reduce their ability to set and achieve personal goals. Family Nurses are also able to harness clients’ desires to be good mothers to encourage them to better manage certain aspects of their lives, such as their mental and physical health, by helping them to think through how challenges in these areas might impact on their child.
While Family Nurses support clients to achieve a wide range of outcomes, this section focuses on four specific outcomes: maternal mental health; self-efficacy; education and employment; and minimisation of the risk of abuse.
4.3.1 Maternal Mental Health
FNP is seen by many clients, as well as Family Nurses and other professionals, as having a positive impact on clients’ mental health. Family Nurses report high levels of mental health issues among FNP clients, especially anxiety and depression. They therefore work to identify any mental health issues and to help clients better understand and manage their mental health.
Family Nurses see themselves as particularly well-placed to help clients whose mental health issues would be unlikely to come to the attention of other service providers. Many FNP clients face difficulties engaging with other services – indeed, some clients struggle to even leave the house – and because of the stigma associated with mental health, they are often unlikely to be willing to speak about their mental health or seek mental health support from a GP. However, given the gradual building of a close, trusting relationship between Family Nurses and their clients, Family Nurses report clients reaching a point where they feel that they can open up about their mental health without feeling judged or stigmatised. Once Family Nurses are able to open up conversations about mental health with their clients, they will then work with the client to help provide them with coping strategies and, if necessary, support them to access professional or specialist help.
Many clients felt that working with their Family Nurses had helped them to come to realise for the first time that they were struggling with their mental health. One client noted that she had been living with depression without realising, and claimed that it was only through working with her Family Nurse that she came to learn that "depression isn’t normal like I thought it was". Similarly, another client explained that her Family Nurse "helped me to see that I needed to go to the doctors" about her mental health, and felt that she would have continued to struggle with her mental health without the input of her Family Nurse.
Expressing a similar sentiment, another client explained that:
"When I was really down a few weeks after [my child’s] birth – I felt utter despair and had thoughts of self-harm – my nurse had a visit. I still don’t know what happened but I was in tears. I got a hug and I talked about my feelings. After she left I decided not to self-harm. [I] went to the GPs and haven’t looked back since. [Without FNP] I think I would have had poorer mental health for longer." (Client)
In this example, the client demonstrates that it was through talking with her Family Nurse, being listened to and empathised with, that she was eventually able to find the strength to seek help from her GP to improve her mental health.
Supporting these testimonies, one staff member suggested that a particular client’s mental health would have deteriorated without the influence of the Family Nurse, and that this would have affected the client’s child as well:
"[Without FNP involvement] I think [the client’s] mental health would have started to deteriorate and this would have impacted on [her baby]. [Her baby] would definitely not be such a content and settled baby. [The client] would not have gained the confidence to provide [her baby] with social interaction, including weekly book bug groups, swimming classes and baby groups in the community." (Staff Member)
4.3.2 Maternal confidence and self-efficacy
As the mention of self-confidence above alludes to, regarding clients’ psychological resources, FNP is not only seen as valuable for more than just the influence that Family Nurses can have on mental illness. More broadly, Family Nurses aim to instil young mothers with a sense of self-efficacy which enables them to have the confidence to make their own positive life choices, and gives them the belief that they can set and achieve their goals and aspirations. Family Nurses report that the majority of clients enrol onto FNP feeling that they have no or very little control over their own lives. They describe that they have had little opportunity to make decisions that would affect their lives, and have little experience of being asked their opinions, being given choices, or feeling listened to.
Family Nurses focus on actively listening to their clients, to find out what the client would like to achieve, and what strengths they have that the Family Nurse can help them to build on. Rather than telling clients what to do, they help clients to think through their options and make their own decisions.
They also focus on providing clients with affirmation. This means actively pointing out to clients not only their achievements, however small or large, but, importantly, the strengths that the client brought to a situation. As one FNP Supervisor put it, they seek to point out "what is the strength within the client that has helped them to achieve what they achieved". This kind of affirmation is something which Family Nurses perceive that many of their clients have lacked throughout their lives. As a result, they find that clients often appear frightened of making decisions or setting goals, as they have rarely received affirmation that they have the necessary strengths and qualities to do so.
The mother of one client summed up how the affirmative approach of FNP has worked for her daughter:
"I think it [FNP] is a good scheme. [My daughter] has really benefited from it. I think the approach is good. [The Family Nurse] doesn’t dictate to [the client] what she should do and always asks her what she thinks and feels about everything. She doesn’t treat her like she is a daft wee lassie. It is empowering and has helped build both [my daughter] and [my daughter’s partner’s] confidence. It made [my daughter] feel she could do it and do it well." (Client’s mother)
As this client’s mother highlights, by listening carefully and encouraging clients without telling them what to do, Family Nurses are seen as an empowering presence in clients’ lives, giving them the confidence to feel that they are capable of achieving things that they had previously seen as beyond their abilities. This confidence is something that many clients also allude to when speaking about the value of FNP. As one client explained, she felt that FNP gave her the confidence to be a good mother:
"I was 15 years old, in my 4th year at secondary school, pregnant with no self-confidence. I was shy, kept myself to myself, rarely went out when I was pregnant. Now I am a mum. I have got a college interview this week. I am going to groups with [my child]. I can take [my child] swimming by myself. I am more confident. I am going to keep being a good mum." (Client)
4.3.3 Maternal Education and Employment
Education and employment is another area in which Family Nurses’ efforts to instil their clients with confidence are seen as valuable. Family Nurses report that often when clients enrol on FNP, their lack of self-esteem is such that they see things such as educational achievement as beyond their abilities, and not for "people like them". Family Nurses will therefore often work with clients to improve their self-esteem in this area, in order to help them onto the path towards sustainable and rewarding employment.
One client explained how she went from being "muddled" and "in a mess" at the beginning of her time on FNP to having gained more qualifications, stayed in college, and having greater aspirations for her future career:
"At time of recruitment to FNP I was muddled, in a mess, coming to terms with pregnancy, unsure where to go, also in the middle of a college course. Now […] I now have my own tenancy, my own car, I have more qualifications, and I am still attending college. For the future I hope to get a bigger house, better car, and get on the property ladder with a good career. [My child] will continue to be my beautiful, intelligent ray of sunshine." (Client)
Family Nurses can also engender the confidence to pursue educational opportunities in their clients by endorsing their clients in concrete, practical ways such as providing references. As another client explained:
"I went for my interview at college. I had no one else who could give a reference, but they called you [the Family Nurse] for a reference I was so happy but a little bit scared when they emailed to give me a place." (Client)
Finally, as one FNP Lead pointed out, setting clients on the path towards employment can also potentially have a beneficial longer-term effect for local health and social care services. Family Nurses report that some clients become inspired to move into the health and social care profession themselves. And, with FNP now having been operating in Scotland for ten years, some staff have begun to see this motivation bear fruit as former clients enter the sector:
"We help clients build pathways to employment. And it’s notable how many ex-clients become employees in the Health and Social Care system." (FNP Lead)
4.3.4 Minimisation of the Risk of Abuse
Family Nurses report that a significant number of their clients are in, or have been in, abusive relationships at the time of their enrolment. This poses a significant challenge to a client’s ability to keep herself and her baby safe, and to keep her baby off the Child Protection Register or from going into care.
Numerous Family Nurses, clients, family members and other professionals spoke of the central role that Family Nurses often play in helping clients to recognise when they are in an abusive relationship, and to support them in any action they may choose to remove themselves from such a situation. Through the trust built up gradually over time in the relationship between Family Nurse and client, and the non-judgemental way in which they approach clients’ lives, Family Nurses are often able to begin conversations about abuse which clients would not be willing to have with any other professional.
With regard to violent or abusive relationships, Family Nurses support the client to open up about, and reflect on, their intimate relationships. This, alongside discussions and exercises which explore what constitutes a healthy relationship, allows them to help clients to see for themselves whether the relationship that they are in is unhealthy, or even potentially dangerous. Some Family Nurses reported that, having grown up in a context in which violence or abuse are normalised, some clients have been in abusive relationships without realising that this is the case.
As with self-efficacy, Family Nurses therefore work to help build a sense of self-worth in their clients, helping them to understand their own self-worth, which in turn helps them to recognise when they are not being treated as worthy by their partners. And, as in other areas of clients’ lives, Family Nurses take a non-judgemental, non-prescriptive approach to their clients’ relationships, avoiding blaming the client for being in a problematic relationship or telling them they must leave a relationship. Instead, they focus on helping them to come to see their situation for themselves, giving them the confidence to make their own decisions, and assisting them in making safety plans and knowing where to seek help when it is needed.
"Speaking to my family nurse and then hearing it back led me to making my own decision about my partner and I never felt judged. I wouldn’t have been able to follow through with ending my relationship without my FN – I would have gone back to him [her ex-partner]." (Client)
Speaking about her experience of FNP, one client summed up the effect of the Family Nurse’s non-judgemental, non-prescriptive, and supportive approach on her ability to remove herself from an unhealthy relationship:
In this example, the Family Nurse was able to open up conversations with the client about unhealthy relationships, and help the client to examine for herself the situation that she was in, without feeling judged, and explore the options for changing her circumstances.
In another example, a client pointed out how important it was that her Family Nurse gave her the confidence to question why she was being treated badly, and helped her to reflect on her situation:
"[Without the Family Nurse] I wouldn’t have felt so certain about things. Getting a chance to reflect on decision making helps when you need to make a decision. I have attended for a short-term psychology intervention [and] gained confidence to question why I was allowing myself to be treated in a bad way." (Client)
Explaining where she felt that the value of FNP lies, the mother of another client credited this approach not only with helping her daughter move away from a violent relationship, but with keeping her daughter alive:
"I believe if you [the Family Nurse] had not reached out to [my daughter] the way you did, not judging her, just listening and supporting her and giving her invaluable advice, then [my daughter] would have been killed by her ex-partner. But you reached out and I reached in and between the two of us we caught her and she didn’t fall through the net. Because of your help and support, [my daughter and her baby] are thriving and very happy to be safe. I could not have done it alone as you are part of the system and caught her from the other side I cannot reach. You are an example why the service is invaluable to young girls and women like [my daughter]. Without you and people like you there would be more domestic violence related deaths. But luckily [my daughter] is safe because she had the privilege of meeting you and having the support when she needed it the most. [My daughter] felt totally judged by social work and not listened to or supported in any way." (Client’s mother)
Again, like the other client quoted above, this mother highlights the importance of the Family Nurse’s non-judgemental approach, and her ability to listen and support this client. This is contrasted with professionals from other services, by whom the client felt judged and therefore unable to open up in order to receive the support that she needed.
As the evidence presented in this section suggests, clients, clients’ family members and Family Nurses see the value of FNP as lying in Family Nurse’s ability to help clients reflect on aspects of their lives that might be negatively affecting them, and supporting them to take action to improve their situations. This is important not only for improving the quality of clients’ lives, but also for helping clients to care for their children to the best of their abilities. The next section will look in more detail at how people involved in FNP see the programme as beneficial to these children.
4.4 Value for FNP Babies
4.4.1 Positive Parenting
"We [client and her partner] want [our child] to feel loved and the centre of attention. We don’t want her to ever feel that we are getting bored of her. We don’t want her to feel that she is having to bring herself up. We both want to feel a strong bond and connection with her that we didn’t experience from our own parents." (FNP Client).
A central aim of the Family Nurse Partnership is to attempt to break intergenerational cycles of poor parenting, child abuse and neglect, setting clients on a path towards more positive parenting. Family Nurses tend to report some clients have suffered from some form of neglect, abuse, or other poor parenting in their own childhoods.
In each individual case, Family Nurses take a gradual, multi-layered approach to understanding what challenges a client might face in caring for her baby, and helping her to understand any potential risks to the child and how to mitigate these. This begins early in pregnancy, when Family Nurses will gradually try to encourage clients and their partners to think about their own norms, values, and cultures, and the environments in which they live. They are also asked to reflect on how they were brought up themselves, and to think about any positive and negative experiences from their own upbringings. Reflecting on all these aspects of their own environments, they are encouraged to consider how the circumstances in which they live might impact on their child. This enables clients to think about whether changes might need to be made and what other resources they could draw on to make their environment more suitable for raising a child. Clients are then supported by Family Nurses to set achievable goals, develop plans and make changes in their lives in line with their aspirations.
This work is seen by Family Nurses, clients and other stakeholders as playing an important role in both ensuring that babies are not subject to potentially harmful situations, and promoting positive child development among babies on the FNP caseload.
4.4.2 Mitigating Risks to Children
When asked where they saw the value in FNP, a number of Family Nurses, clients, clients’ family members and other professionals highlighted the important role that Family Nurses play in helping parents to recognise when their children might be at risk of harm, and when they need to act to remove their children from potentially harmful circumstances.
With many FNP clients having experienced physical, sexual or emotional violence, Family Nurses place great value on the potential for clients and Family Nurses to intervene and protect children from witnessing or being a victim of violence themselves. This view is supported by clients and other professionals. For example, one client felt that as a result of FNP:
"I have left an abusive relationship. I have removed my daughter from witnessing domestic abuse." (Client)
Similarly, a social worker highlighted the role that the Family Nurse played in protecting one particular baby:
"As a Social Worker, I can feel confident that the child’s development is being looked at rigorously [by the Family Nurse]. The Nurse plays a nurturing role for the mum, helping her to become a confident mum. The Nurse has a clearer focus on the mum, the dad, and the child’s needs. The educational material is good. The Family Nurse reduced risk and got the child off the CPR [Child Protection Register] faster." (Social Worker)
The story of one particular client demonstrates how Family Nurses see themselves as able to influence the reduction of risks posed to babies on FNP:
"This client had been sexually abused by a relative as a child. She was subsequently placed into foster care, and had self-harmed and attempted suicide on a number of occasions. Her unborn baby was placed on the Child Protection Register and her Family Nurse noticed that she expressed resentment and frustration about her own childhood and the way that her parents had treated her.
One of the biggest challenges to this client’s ability to raise her child was that some controlling behaviour was demonstrated in the relationship between her and her partner. The Family Nurse therefore worked with the couple to help them think about the importance of equal relationships and what it would be like for a baby to grow up in a controlling environment. In particular, the Family Nurse worked with the client and her partner to explore ideas around brain development, and the effect that negative relationships and stress could have on their baby’s brain. The Family Nurse reported that the couple were responsive to this work, and worked well to try and support each other and recognise each other’s strengths. The client’s partner commented that: "I feel I have a better understanding of relationships and the impact of stress on my baby" as a result of this work with the Family Nurse.
Since birth, the baby has thrived. She is a settled baby who meets all her developmental milestones and benefits from the good routines that the client and her partner have put in place. It is clear to the Family Nurse that a strong attachment bond has developed between the baby and her mother. Most significantly, while she was on the FNP programme the baby was removed from the Child Protection Register, with their social worker noting that it is clear that the client now knows "what is right and what is not right" in relation to looking after her baby and keeping her safe." (Clients Mother)
Thus in the first months of the baby’s life, this client has been able to take important steps in breaking the cycle of poor parenting and abuse that negatively impacted on her own childhood. She was able to reflect on the poor parenting that led to her own abuse during childhood, and, along with her partner, to see how their behaviour might have a similar effect on their own child.
As well as helping young mothers to ensure that their children are not exposed to potentially harmful situations, Family Nurses are also seen to play an important role in helping clients to recognise a wide range of other potential risks to their children’s health and safety. For example, one client who, during the first few months after her baby was born lived with a relative in a house which was unsuitable for a baby, credited her Family Nurse with helping her realise that her child needed more appropriate accommodation:
"I realised one day when my nurse was talking about the baby crawling about on the floor, that the house I was living in was not good for him to be in and that spurred me on to get my own place." (Client).
While social workers had been concerned about the poor condition of the house that this client was initially living in with her baby, the client had been reluctant to engage with social work. However, as a result of the long-term, trusting relationship her Family Nurse had built up with her, she began to recognise the risks to her child, and subsequently sought a new tenancy.
Other clients highlighted important work that their Family Nurses had done to help them raise their children in more healthy environments. For example, one client noted that she had managed to make her home completely smoke-free as a result of the intervention of her Family Nurse:
"I have made my family home smoke-free – both my parents smoke and they used to do so in the house – they now only smoke outside and my mum is now thinking about stopping and has asked my nurse for advice." (FNP Client)
As this example demonstrates, the Family Nurse’s influence can extend beyond the client herself, to help the client’s family members also adjust their behaviour in order to ensure a safe, healthy environment for the child.
These examples give a sense of the wide-ranging nature of the interventions that Family Nurses provide – from protecting children from violence, to helping them out of inadequate housing, to reducing the risk of poor physical health – demonstrating the importance of FNP’s holistic, agenda-matched approach which ensure that each client receives the support that they and their children need, depending on their own unique circumstances.
4.4.3 Supporting Child Development
More than just helping parents to ensure that their children are not exposed to situations in which they might be at risk of harm, Family Nurses see the contribution that they make to actively promoting positive child development as equally valuable. Family Nurses encourage their clients to support their children’s development in all areas, including physical, cognitive, emotional and social development, and positive child health.
For Family Nurses, this can be particularly rewarding as they see close-hand how, with the right support and encouragement, parents who might otherwise have struggled to support their children, develop into sensitive mothers who can read their babies’ cues and encourage all aspects of their development. As one Family Nurse highlighted:
"Watching my clients develop happy secure attachments to their children is amazing to watch. The most impressive thing I have observed is how well these children develop both cognitively and physically. I believe the Family Nurse with the support of the programme materials contributes to this." (Family Nurse)
This Family Nurse suggests that the strength of FNP lies in the quality of the programme materials, such as PIPE, DANCE, and the specially-designed facilitators, and a structured programme of visits, that forms the foundation of the programme. These are seen as crucial in helping guide clients in their relationships with their babies, and to teach them how to recognise and support their children’s development. Similarly, another Family Nurse draws attention to the importance of the intensive nature of FNP visits that allow Family Nurses the time to explore ideas around child development in-depth:
"As a comparison I would imagine that if some of my clients didn’t have the intensive visiting programme [of FNP], I would see them as a Health Visitor at the 27-30 month child development stage and I would be referring the child to speech therapy. I have been amazed at the development and potential of my graduating 2 year olds." (Family Nurse)
For this Family Nurse, the value of FNP lies in the fact that it offers an intensive period of education for the client which helps them not only to prevent harm to their children, but to support their children to meet their developmental milestones, giving them best possible chance of positive outcomes over the course of the rest of their lives. Family Nurses see this as something that is less likely via other channels, suggesting that without FNP more children might fail to get the early support that they need, and their needs might only be picked up later in childhood.
Clients, too, see the value of the work that Family Nurses put into helping them learn how to support and encourage their childrens’ development. As two clients explained some of what they have learned:
"I’ve learned lots about baby brain development and baby cues. This helped me to look after [child] and think about what he needed or was trying to tell me’. (Client)
I have learned to trust my instincts. Nothing is ever as bad as it seems, and it is good to "talk it out". I have learned a lot about feeding my baby healthy foods. I have also learned that babies are resilient. They need their mum, but they are also smart and independent. I have also learned where my priorities lie. [My child] is my most important relationship." (Client)
Family Nurses and their clients, then, see great value in the job that Family Nurses do in terms of both preventing harm and supporting child development. Family Nurses see themselves, and are seen by others, as uniquely positioned to help young mothers ensure that their babies are not exposed to potentially harmful situations. And they also see themselves as having the time and resources to help client’s give their children the best possible start in life in terms of their physical, emotional and cognitive development. This is attributed to the intensive nature of the programme, which allows nurses the time and resources to set parents on the right path for encouraging their child’s wellbeing from pregnancy onwards.
4.5 Value for Other Professionals and Services
4.5.1 Inter-agency working
"Everything now requires partnership working. Take the ante-natal care pathway. Health Visitors and Family Nurses want the same thing. It is a partnership; it’s really important you work closely with others." (FNP Lead).
Family Nurses, FNP Supervisors, and FNP Leads stress the importance of working positively in partnership with a wide range of different statutory services and organisations to give each client the best support possible based on their individual needs and circumstances. Given the nature of many FNP clients’ situations, clients often require support from a number of professionals, including GPs, midwives, mental health professionals, social workers, housing support workers, and others.
The contributions from other agencies suggest that many professionals acknowledge that working closely with Family Nurses helps other services to support young mothers in a way that both identifies and meets their needs in a person-centred way. In particular, professionals outside of FNP drew attention to the ease with which they are able to work with Family Nurses, and the vital role that Family Nurses can play in providing early intervention which has the potential to reduce the need for more serious interventions later on. As one social worker, speaking about a particular case, describes:
"[The] FN was able to make plans at an earlier stage for the family and ask for social work intervention or other professional interventions at an early stage which is way more beneficial and reflects in better outcomes for the family. Having clear and defined roles within the multi-agency (GIRFEC) plan also made for a good working relationship and made it easier and clearer for the parent when looking for support and which people can support with which issue. Early intervention and consistent multi-agency work makes for better outcomes for the child. I have always found the role working with FNP positive, especially when they take the lead (as in this very case) as often this makes the situation and support for the family less stressful and often we can be involved for as little or as much as deemed necessary to reduce the risks for the child." (Social worker)
4.5.2 Helping ease workloads of other services
Interviews with other professionals also revealed a sense among staff in other agencies that the existence of a Family Nurse in a client’s life is beneficial for their whole organisation because interventions by the Family Nurse can help to ease their workloads. FNP is seen to both reduce the need for interventions from other services, and to relieve the workloads of other professionals as Family Nurses are able to do the groundwork that allows a client to engage constructively and effectively when they do need to seek support from services.
For example, the work that Family Nurses do with clients who are struggling with mental health issues, such as providing them with coping strategies, was credited by one manager of a community mental health service with decreasing the need for their services among FNP clients:
"[The] FNP Programme is invaluable. The work Family Nurses do with clients prior to accessing our service has noticeably reduced our workload as less [sic] interventions are required due to coping strategies already learned by clients as part of the FNP Programme." (Manager of a community mental health service)
Similarly, others expressed the view that Family Nurses’ work with clients enables other professionals to focus specifically on helping clients using their professional expertise. Furthermore, the Family Nurse is able to deal with wider issues faced by clients which may otherwise take up much of the time that could be dedicated to delivering specialist interventions. Consequently, agencies are able to spend the time that they have with each client focusing specifically on what their staff are most qualified to help the clients with. As one clinical psychologist explained:
"The role of the FNP allowed me to focus specifically on the young person’s mental health needs and the continued assessment of this. In addition to allowing me to focus on the mental health needs and treatment plan, contact with the FNP and information obtained from them helped to inform treatment planning and risk management." (Clinical Psychologist)
As this quote suggests, it is also seen as beneficial to other services that Family Nurses are able to give service providers important background information, helping these services to ensure that each client receives the right care, at the right time, from the right person.
4.5.3 Helping clients and professionals to engage with each other effectively
There were also suggestions both from other professionals and from clients that the Family Nurse’s involvement with the client reduces stress in relationships between clients and other professionals, enabling both parties to engage comfortably and constructively with one another. Because of the trusting relationship that a Family Nurse builds up with their clients, it appears that clients may be more likely to trust other professionals if they know that the Family Nurse is supportive and encouraging of their engagement with them. For instance, one client claimed that, thanks to the support of her Family Nurse:
"We now can feel more relaxed around social workers so that they see the best of us." (Client)
Complimentary to this, the manager of a third sector agency suggested that their staff also feel more at ease when dealing with a service-user who has an FNP nurse. They suggested that the presence of the FNP nurse in the client’s life gives the agency workers confidence that they will be working alongside a dedicated professional who will work and communicate well with them:
"[We have] excellent working relationships [with FNP], excellent communication, same ethos, no conflict of interest. We really work hand in hand. FNs are very professional. We know what we are going into and we have a named person to refer back to. It’s not phoning through call centres when time can be crucial such as in child protection concerns. Staff can breathe a bit easier when the clients have a Family Nurse." (Manager, Third Sector Organisation).
More than just easing relationships between clients and other agencies, in some cases Family Nurses have also been seen as having played a pivotal role in creating relationships between clients and other services where the client might otherwise not have been able or willing to engage. For example, encouraging clients to engage with services in circumstances in which relationships between a client and a particular service (or services) might have been challenging or have already broken down altogether, and in circumstances where a client is fearful of a particular service. In one case, for example, a Family Nurse reported being able to broker positive communication between a client, social work and criminal justice systems in a context in which the client had a history of criminal convictions and, by her own admission had been "oppositional" in her interactions with both of these services.
In another case, a client’s partner summed up how the trusting relationship that developed between him, the client and their Family Nurse allowed for this couple to engage positively with a social worker who had been assigned to them. Both the client and the partner had serious mental health issues, and they feared the child would be removed from their care if social work became involved in their lives. However, the Family Nurse helped him to understand why the social worker needed to be involved, and gave him the confidence to engage with social work:
"Working with the Family Nurse was really good. She talked us through everything. In pregnancy we felt really out of our depth, we were very worried when social work got involved. When the Family Nurse told me they were coming I thought why do we need them? We thought they might take our baby from us. I wanted to lock myself away in the bedroom when social work came to the house. [But] I clicked with the Family Nurse, I had a huge trust in her [and] she helped me understand why we needed the meetings and social work involvement." (Client’s partner)
The importance that Family Nurses place on partnership working is thus often seen by other professionals, clients, and their families as a valuable aspect of the client’s relationship with the Family Nurse. It is seen as enabling relationships between clients and other professionals and reducing stress in these relationships, as well as potentially reducing workloads for other professionals and allowing them to offer focused and effective assistance to FNP clients.
4.6 Value for Family Nurses
As part of this exercise, Family Nurses were asked to reflect on their own careers to discuss what they personally valued about being a Family Nurse. Two main themes emerged from these discussions. First, that Family Nurses feel a tension between the rewarding nature of the job and immensely challenging nature of their work. And second, that Family Nurses tend to see the education, supervision and support that they receive as extremely valuable.
4.6.1 Family Nursing Rewarding as yet Challenging
Family Nurses tend to describe the experience of working as a Family Nurse as both intensely rewarding yet extremely challenging. As one Family Nurse summed up:
"[Being a Family Nurse is] the best job I have ever had. [But it is also] the hardest job I have ever had, challenging me in so many ways, feels like a rollercoaster at times. So many happy, enjoyable times along with some very challenging situations which has tested my inner strength, resilience, organisational skills and time, and home-life/work balance." (Family Nurse)
When discussing the rewarding aspects of the job, Family Nurses focus predominantly on the changes that they saw in their clients over the course of the programme, as well as the sense of feeling valued at all levels of the programme, from clients right up to the top of the Scottish Government. As one FNP Supervisor explained:
"One thing that is important is that we as Family Nurses feel valued at all levels. We feel valued by our clients, Family Nurses feel valued by their supervisors, and we feel valued by the [Scottish] Government as well. That the FM [First Minister] is invested in FNP and supports it is important for Nurses’ morale. So Family Nurses feel valued from the clients right up to the FM." (FNP Supervisor)
However, Family Nurses also noted finding the job challenging for a number of reasons, particularly relating to time and workloads, and the emotionally draining nature of the work. With a full caseload, a Family Nurse will have 25 clients. For each client, they must prepare and deliver as much of the FNP programme as possible with each visit tailored to the needs of the individual client, as well as delivering the full Universal Heath Visitor Pathway, attending training, weekly supervision and team meetings, writing up each visit, and conducting a large amount of data collection on client and child outcomes. One FNP Supervisor described how, given this workload, it is frequently difficult to fulfil all the fidelity requirements demanded by the programme every time, leading Family Nurses to feel frustrated that they are unable to deliver every aspect of the programme to every client. As a result, this supervisor explained that Family Nurses can either begin to burn out because they push themselves too hard to reach all their targets, or they lose morale because they feel that they are failing to reach their targets.
For nurses working in both urban and rural settings, the challenges of this heavy workload can be compounded by the need to spend long periods of time driving either long distances in rural areas or through congested city traffic, between clients’ homes.
Family nurses also speak of finding their work emotionally draining. A full caseload comprises of 25 clients, most of whom have multiple, significant vulnerabilities, and many of whom are unwilling to engage with any other service. This means that the Family Nurse often feels a heavy weight of responsibility for her clients. Moreover, the need to develop the deep, trusting relationship between clients means that Family Nurses feel a strong obligation to be "fully switched on" for every visit.
As a result of the stressful, all-consuming nature of the job, some nurses highlighted the fact that while they do love working as Family Nurses, they believe that it is not sustainable long-term career for them, given the risk of burn-out and the toll it can take on their personal relationships outside of work. Others, however, spoke of trying to find ways to ensure that they were able to avoid burning out and to continue working as Family Nurses as long as possible.
4.7 Support for Family Nurses: The Education programme and Supervision
4.7.1 The Education Programme
All Family Nurses and FNP Supervisors receive 18 months of structured FNP training education and support provided by NHS Education for Scotland (NES), as well as additional training for FNP Supervisors. On top of this, NES provides Continuing Professional Development (CPD) for Family Nurses and FNP Supervisors, and within each heath board FNP teams carry out their own local training in conjunction with the training received from NES. Like FNP itself, the education programme provided to Family Nurses is adapted to suit the needs of new Family Nurses, depending on the backgrounds and experience they join the programme with. It seeks to foster the same nurturing, strengths-based, and affirmative values that FNP aims to foster among its clients. As one Family Nurse summarised:
"The training for FNP has been second-to-none: positive; evidence-based; and a safe, respectful environment." (Family Nurse)
Family Nurses tended to express their appreciation for the level of training they receive when they joined FNP, and the continuous training they undertake once they have become Family Nurses. One Family Nurse spoke of feeling, before joining FNP, that she would never be capable of carrying out such a role because she did not feel that she would be able to develop the skills demonstrated by Family Nurses:
"I never thought I’d get that FNP job, they’ve got so many skills. I thought I’d never get these skills – but the training I’ve had! And then continually developing your skills, you don’t get that as a health visitor!" [Family Nurse]
However, Family Nurses spoke of the in-depth, rigorous training that they receive when they become Family Nurses, and which they continue to receive throughout their time working for FNP. One Family Nurse described the increased level of understanding she gained in how to deal with clients as compared with her previous health visiting role:
"When I worked as a Health Visitor I would have said I tried to use a strengths-based approach with the families on my caseload. [But] I realised since becoming a Family Nurse I may have come across as the expert and provided lots of advice and information." (Family Nurse)
Family Nurses praised, not only the value of their content of their training in terms of learning the practicalities of how to deliver FNP, but also of the importance of learning the theoretical underpinnings of the programme, to understand why FNP is structured as it is, and how what they do works to change their clients’ lives.
4.7.2 Supervision model
On top of the rigorous training that Family Nurses receive, each Family Nurse also receives structured weekly one-hour individual supervision sessions from his or her FNP Supervisor, as well as regular observed visits to clients, and weekly team case discussion meetings led by the FNP Supervisor. This structure is seen as hugely valuable in helping Family Nurses to cope with complex, demanding caseloads and the emotionally draining nature of their work. Supervision is structured in such a way that the relationship between Supervisor and Family Nurse parallels that of Family Nurses and clients, with supervisors creating a nurturing, trusting and positive environment in which Family Nurses can feel valued and listened-to.
Supervisors and Family Nurses see supervision as hugely important as a means of ensuring that Family Nurses are coping with their caseload, and that they have a space in which they feel comfortable raising any concerns, express any challenges that they are facing, and seek advice and support from their supervisors. As one FNP supervisor summed up the need for supervisions:
"We all start out with a vision of FNP as a lovely soft service. But six months down the line, with a complex caseload, that view can sit uncomfortably. And that’s why we try to create an open, honest [and] transparent space to say ‘how does it feel?’ and ‘what would help?" (FNP Supervisor)
Again, this was spoken of by Family Nurses as a valuable asset. As one Family Nurse explained:
"‘It’s the first time I’ve ever had structured supervision and have found this beneficial as there’s so much vulnerability on the caseload." (Family Nurse)
4.8 Client Vulnerabilities
All clients within FNP Scotland (2,083)[4] were considered by Family Nurses in terms of the vulnerabilities that they presented with at the outset of the programme. They were provided with a checklist of 43 potential vulnerabilities for clients (Appendix 1). The list was not presented to the clients , vulnerabilities were rated by the Family Nurse based on their knowledge of the client and her partner. What follows is indicative of the vulnerabilities experienced by clients rather than a definitive figure.
4.8.1 Demographic Profile
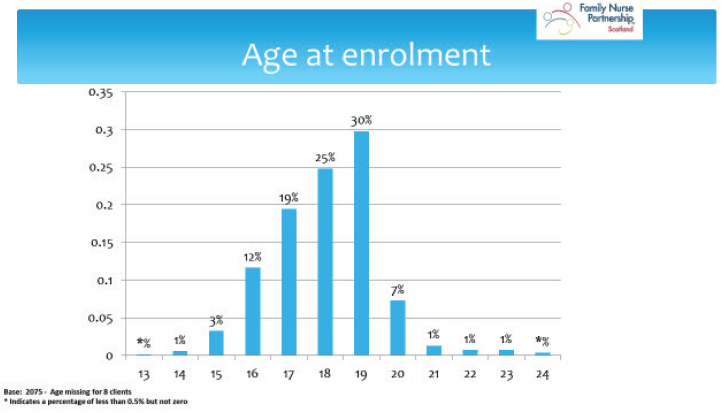
At commencement in the programme, the majority of clients (89%) were aged 16-19 years and 16% aged 16 or under. A small proportion of clients were aged 20-24 years (10% - 139 clients) reflecting the recent adaptation to include clients aged 20-24 years. In 2016/17, 3.6% of all births in Scotland (1,917) were to mothers aged under 20 years old. The proportion of births to younger mothers in Scotland has continued a significant downward trend over the last 20 years.
Overall, almost a quarter of clients were in the pregnancy phase of FNP (23%), two in five were in the infancy stage (41%) and over a third were in toddlerhood (36%).[5] This profile of programme stage is very similar to that detailed in the 2017/18 FNP Scotland Annual Report, with 24% of clients in pregnancy, 41% in infancy and 36% in toddlerhood.
Recording of deprivation using the Scottish Index of multiple deprivation quintiles (SIMD) was requested, however SIMD data was missing for almost half of the current case load (43%). Where SIMD was recorded, 73% of clients were shown to live in the most deprived areas (SIMD 1 and 2).
4.8.2 Vulnerability Profile
Overall, the average number of recorded vulnerability factors per client was nine, with Family Nurses rating very few clients as presenting with no vulnerabilities (36 clients - 2%). The most prevalent perceived vulnerabilities for FNP clients at entry to FNP were; anxiety or other mental health issues (63%), experience of parental separation (63%), low income (60%) and not being in work, education or training (57%).
The following table (Table 2) shows the percentages of nurse-rated vulnerabilities in the FNP caseload:
Table 2: Percentage of Nurse-rated vulnerabilities in FNP caseload
| Vulnerability | Percentage of Clients |
|---|---|
| Anxiety or other mental health issue | 63 |
| Experience of self-harm | 22 |
| CAMHS (ever) | 20 |
| Experience of attempted suicide | 10 |
| High or low BMI | 22 |
| Any previous pregnancy | 8 |
| Substance misuse | 8 |
| Carer for dependent other | 7 |
| Alcohol misuse | 7 |
| Long-term health issues | 7 |
| Learning disability | 5 |
| Registered disabled | 1 |
| Involvement with social services | 36 |
| Family known to social services | 31 |
| Ever been a looked-after child | 18 |
| Ever been on Child Protection Register | 16 |
| Involvement with criminal justice system | 6 |
| Parental separation | 63 |
| Experience of poor parenting | 33 |
| Parental mental health issue | 32 |
| Experience of emotional abuse | 25 |
| Experience of bullying | 22 |
| Experience of emotional neglect | 19 |
| Experience of intimate partner violence | 18 |
| Client’s mother treated violently | 17 |
| Parental alcohol misuse | 16 |
| Experience of physical abuse | 16 |
| Parental substance misuse | 14 |
| Experience of physical neglect | 14 |
| Death of client’s mother/father/main attachment figure | 10 |
| Experience of sexual assault | 9 |
| Family member incarcerated | 7 |
| Experience of sexual abuse | 6 |
| Experience of childhood sexual exploitation | 3 |
| Low income | 60 |
| Not in work, education or training | 57 |
| Living in an area of deprivation | 49 |
| Social isolation/limited networks | 36 |
| Irregular/limited/no school attendance | 31 |
| Poor/unsuitable housing | 28 |
| Experience of homelessness | 28 |
| Low job stability | 11 |
| Entered FNP under age of 16 | 4 |
4.8.3 Socio-economic disadvantage
Almost all clients (88%) were believed to have at least one socio-economic disadvantage upon entry to FNP. This disadvantage was evident across all age groups, including those over 20 years old on entry to the programme. Six in ten (60%) of all clients were rated as living on a low income and 11% were viewed as having low job stability such as zero hours or temporary contracts.
The majority of clients (57%) were not in work, education or training at the time of enrollment. 16 and 17 year olds were the most likely of all groups to be not in education, work or training. This is the case for 67% of 16 and 17 year old clients, whereas 19 and 20 year olds are less likely to be not in education work or training at 45%.
A third of all clients had irregular, limited or no school attendance (31%). This varies substantially by age with over three quarters of 13-15 year olds having irregular, limited or no school attendance (76%) compared to a quarter of those aged 18-24 years (22%).
Over a quarter of clients (28%) were rated as having experienced homelessness and 28% were viewed as living in poor or unsuitable housing at the start of the programme. Of those that were living in poor or unsuitable housing almost half (47%) were also recorded as having experienced homelessness.
A slight majority of clients were parenting on their own (58%), while two in five were recorded as having had a partner at the start of the programme (42%). Over a third of clients (36%) were viewed as having limited social networks or as being social isolated. This was spread across the age ranges. However, for those that had ever been looked after or on the child protection register this was 56% and 53% respectively.
4.8.4 Health Challenges
Family Nurses rated three quarters of clients as having health issues upon entry to the programme (75%) with 63% experiencing anxiety or other mental health issues. Physical health issues were reported at a much lower rate among this group compared to mental health issues.
A small proportion of FNP clients were recorded as having had a long-term health issue (7%) or were registered disabled (1%). 5% of clients are thought to have a learning disability.
Within the FNP cohort, less than one in ten (8%) were rated as having substance misuse issues or alcohol misuse issues (7%) when they entered the programme in pregnancy. Clients rated as having a parent with substance misuse problems were more likely to use substances themselves (21%).
A significant proportion of clients were judged by their nurses (based on subjective judgement rather than a BMI measurement) to have been at an unhealthy weight (either over-weight/obese or underweight) (22%).
Within FNP, 63% of clients were thought to have anxiety or other mental health issues upon entry to the programme. Meanwhile, 22% were thought to have self-harmed, 10% to have attempted suicide, and 20% had attended Child and Adolescent Mental Health Services (CAMHS).
Almost one in ten (8%) of all clients have experienced a previous pregnancy, and 7% of clients were judged to have had caring responsibilities for dependent others.
4.8.5 Social Services
The proportion of FNP clients recorded as ever been looked after or on the child protection register is 22%. Similarly, a significant minority of FNP clients were rated as being from families with previous involvement with social services (36%) or from families that are known to social services (31%).
4.8.6 Criminal Justice
Overall, 6% of clients were rated as having been involved with the criminal justice system, this increased to 17% among those that have ever been looked after or on the child protection register. In terms of intergenerational effects, Family Nurses recorded that almost a quarter (22%) of clients who had experience of a family member being incarcerated had also had involvement with the criminal justice system themselves.
4.8.7 Adverse Childhood Experiences
Adverse Childhood experiences have been defined as intra–familial events or conditions causing chronic stress responses in the child’s immediate environment. These include notions of maltreatment and deviation from societal norms. Evidence shows that adversity and trauma in childhood can impact on a wide range of education, health, justice and social outcomes.[6]
Of the top ten vulnerabilities identified by Family Nurses for clients at entry to FNP, only two are regarded as adverse childhood experiences. These are parental separation (63%) and parental mental health problems.
Overall, 7% of FNP clients had experience of incarceration of a family member and 10% were believed to have experienced the death of their mother, father or primary attachment figure.
At least a fifth of clients are recorded as having experienced bullying, with clients aged 15 and 16 years old more likely to experience bullying (30%).
A quarter of FNP clients (25%) were recorded by Nurses as having experienced emotional abuse on entry to FNP. Exposure to emotional abuse in childhood decreases in prevalence among FNP clients with age on entry. Those entering the programme at a younger age (13-17 years) appear more likely (31%) than the older age groups (16%) to have experienced emotional abuse. This pattern is similar among clients who have experienced emotional neglect, with younger clients (23%) more likely to have experienced this than older clients (12%). Exposure to sexual abuse also decreases with age of entry with clients who entered the programme at a younger age being more likely to have experienced some form of sexual abuse (20% of those aged 13-17 years) than their older counterparts (12%). Finally, experience of physical abuse was recorded for 16% of clients.
18% of clients were rated as having experienced intimate partner violence in their relationships. A similar figure was recorded (17%) for FNP clients experiencing their mother being treated violently. Family Nurses recorded higher levels of intimate partner violence in clients whose mothers were reported treated violently (33%).
Whilst we need to bear in mind that these recorded vulnerability ratings are based on perceived vulnerabilities, the findings highlight the complexity of the challenges and substantial burden of challenge that young women entering FNP face.
4.9 Deepened Client Story Examples
To illustrate the deepened client stories two have been selected for sharing in this report. Whilst the families have consented to sharing their stories, care has been taken to protect identities by anonymising and changing specific details.
4.9.1 Case study 1: Claire
Claire enrolled on FNP when she was aged 16 and still at school. She lived with her mum and her family had received intermittent social work input. Her mum had a long history of substance use and was on a harm reduction programme. Claire had experienced a number of Adverse Childhood Experiences.
Claire was keen to engage with FNP and from the start she presented as resilient and determined to do her best despite her circumstances. She was not in a relationship with the baby’s father throughout the bulk of the programme but his family were very supportive of Claire throughout. She was loyal to her mother despite of her mother’s limited support for her.
Throughout Claire’s childhood there had been concerns about her mother’s substance abuse and their poor housing conditions. Social work had highlighted the need for significant changes in Claire’s mother’s house for it to be fit for the her and her baby to live in. At social work meetings during the pregnancy phase of the programme her family expressed a very negative view of social work. Claire initially brought her child home to her mother’s house and some changes were made, but four months after her baby’s birth she sought and achieved her own tenancy to improve conditions for her child. Social work input ceased once Claire secured her own tenancy.
"She has flourished as an independent parent - is a "good mum" – with no ongoing requirement for social work support."
Claire remained in education throughout her pregnancy and engaged well with the FNP programme. Part of the programme was delivered in school in partnership with her school. Her guidance teacher at school described Claire as "very hard working" "very polite" and "resilient". Claire subsequently attended and completed college and by graduation from the FNP programme she was seeking work.
"I also liked how my nurse was always on the phone to the school or nursery or even social work in the early days getting things sorted out for me. My nurse helped me to see what kind of support I had within my family, I love my family and they are important to me and my nurse respected how I felt about them and also helped me to seek support from other people."
The value of FNP for Claire and her baby
In the context of both prior social work involvement with Claire and her family and range of pre-existing vulnerabilities, the FNP programme is considered to have disrupted a cycle of neglectful, unsupportive caregiving. There was no requirement for social work child protection at any stage, and social work closed the case early. FNP is thought to have added value by supporting this young mother to develop her self-efficacy. Over the course of the programme, Claire completed school and college, applied for and managed her own housing tenancy. FNP is described as resulting in effective multi-agency working between social work, her school, college and her child’s nursery. A very productive partnership between FNP and the school was highlighted, in particular the flexibility of school in enabling her to attend a part-time curriculum and her Family Nurse to deliver some of the programme in her school.
4.9.2 Case Study 2: Jodie
Jodie enrolled in the programme aged 15, when she was 12 weeks pregnant. She had previously experienced a range of adverse experiences including physical abuse, sexual abuse, unstable housing and a period of homelessness. Jodie was attending Child and Adolescent Mental Health Services (CAMHS) to deal with self-harm and emotional difficulties.
Jodie lived with her partner’s family and was thought to have made good preparations for her baby, helped by her partner’s mum. Her father provided financial support.
Jodie engaged well during her pregnancy with FNP, CAMHS and her midwife forming a good therapeutic and trusting relationship with her Family Nurse. At birth, Jodie’s baby was placed on the Child Protection Register but was removed after three months because of the positive nature of relationship between Jodie and her baby. Social Work planned to remain involved on a voluntary basis. Although painful, Jodie broke off her relationship with her own mother because of her concerns of risks of harm from her mother’s alcoholism to her baby.
Jodie is reported as having made good progress during her engagement with the programme. In particular by managing the stressors that affected her mood and by learning how to meet all of her baby’s physical and emotional needs. She often phoned or texted her Family Nurse with any worries or anxieties regarding her or her baby’s health and wellbeing. Jodie re-engaged with education and completed her 4th year at school, securing a place at college to study childcare.
The value of FNP for Jodie and her baby
In this case, the FNP programme can be seen as breaking intergenerational cycles of neglect and child maltreatment. Other family members, including Jodie’s mother, had experienced the removal of their children from their care. Social work had considered removing Jodie’s baby at birth due to concerns about her mental health. However, her baby was instead placed on the Child Protection Register and removed from this after a three month period. Jodie’s Social Worker spoke of the support from the Family Nurse as being crucial to the child protection plan:
"mother was very, very guarded when it comes to SW but works well with FN."
Jodie’s CAMHS Nurse believed that by working with the Family Nurse to support her, they had enabled Jodie to consider a different parenting approach than her own experience and to provide a nurturing attachment. The nurse spoke positively of the family approach taken by the Family Nurse to promote bonding, parenting and their expectations of being a parent for Jodie. She described it as ‘..being on the same page’ and investing in the mother.
Contact
Email: carolyn.wilson@gov.scot