Family Nurse Partnership in Scotland: revaluation report
Findings from family nurses, the families they work with and wider stakeholders on how the Family Nurse Partnership programme works in practice in Scotland.
2. Introduction
2.1 The Family Nurse Partnership Programme
The Family Nurse Partnership programme (FNP) is a licensed, intensive, preventative home-visiting programme, developed over 40 years ago in the United States of America (USA) by Professor David Olds and the University of Colorado (UCD). Known as the ‘Nurse Family Partnership’ (NFP) programme in the USA, the FNP programme aims to improve outcomes for young, first time, mothers and their children. It has been developed specifically for these mothers and their children due to their increased risk of disadvantage and associated poor outcomes across a range of domains.
FNP focuses on helping first-time mothers to engage in preventative health practices, supporting parents to provide responsive, sensitive, and positive parenting, and helping them to develop self-efficacy to both identify and achieve their future goals.
A structured programme of tailored visits is delivered by specially trained Family Nurses. This begins early in pregnancy and continues until the child’s second birthday. The three key goals of FNP are:
- to improve pregnancy and birth outcomes, through improved prenatal health behaviours;
- to improve child health and development, through positive, responsive caregiving; and
- to improve the economic self-sufficiency of the family, through developing a vision and plans for the future.
FNP currently has a Level 4+ evidence rating from the Early Intervention Foundation (EIF). This is the highest rating given to programmes with evidence of a long-term positive impact established through multiple rigorous evaluations.[1] Outcomes highlighted include; supporting children’s mental health and wellbeing, preventing child maltreatment, enhancing school achievement and employment, preventing crime, violence and antisocial behaviour, preventing substance abuse, preventing obesity and promoting healthy physical development.
Three theories underpin the FNP model (Olds 2006) and form a central element of Family Nurses’ training and their application of the programme. These theories are:
1. Ecological Theory
According to Bronfenbrenner (1979, 1995) the social context in which we live influences our health and development. Children’s development is influenced by how their parents care for them, and in turn, this is influenced by the ‘characteristics of their families, social networks, neighbourhoods, communities, and the interrelations among them’ (Olds, 2003). Family Nurses help young mothers to create environments that enhance their children’s development by linking families to additional services that they need in the local community and by involving other family members and partners in home visits, where appropriate.
2. Attachment Theory
Originally developed by John Bowlby (Bowlby, 1969), attachment describes the nature of the bond that a child forms with their parent(s) or primary care-giver(s). A secure attachment style is associated with positive outcomes including self-esteem, self-confidence, emotional regulation, resilience and more harmonious relationships in childhood and early adulthood (Sroufe 2006; Prior and Glaser, 2006). The development of a secure attachment style is thought to be connected to sensitive, responsive care-giving. The FNP programme promotes and models sensitive, responsive care-giving, with Family Nurses aiming to parallel the mother-infant relationship in the relationships that they build with their clients. They also provide opportunities for activities that maximise contact between mothers and babies and help mothers become more responsive to their newborn babies’ cues (Ormston, McConville and Gordon (2012).
3. Self-efficacy Theory
Self-efficacy theory (Bandura, 1977) provides a framework for Family Nurses to understand how women make decisions for themselves and their children. According to self-efficacy theory, we choose behaviours that we believe will result in a particular outcome and that we can successfully carry out (Bandura, 1977; Olds, 2003). By using techniques like motivational interviewing (Houston Miller, 2010; Miller and Rollnick, 2013) Family Nurses aim to improve participants’ sense of self-efficacy and their feelings of control over their lives and relationships. Resulting in increased confidence to make changes for the better for themselves and their children.
Family Nurses are experienced, qualified nurses and midwives who undergo extensive, additional training to take on the role of a Family Nurse. Understanding of the underpinning theories and their application within the program is a key element of their training. In addition to training on the theoretical underpinnings, Family Nurses and their supervisors are provided with education, training and on-going support to use a range of clinical methods including: solution-focused approaches; strength-based approaches; client-centred principles; behaviour change strategies; agenda matching; and motivational interviewing. They carry a maximum caseload of 25.
The FNP programme sets out a potential schedule of structured visits with guidance on content. Family Nurses are encouraged to match their schedule of visits and the content of these to individual clients’ specific needs and goals. Family Nurses are provided with an extensive suite of materials to support client engagement and the development of knowledge, skills and confidence. During each visit the Family Nurse considers six domains; Personal Health; Maternal Role; Life Course Development; Family/friends; Environmental health and Health and Human Services with an aim to build on previous learning.
The development of a trusting, therapeutic relationship between the Family Nurses and their clients is regarded as a key mechanism for achieving positive client engagement and improved client outcomes which ultimately results in better outcomes for children. Family Nurses role model positive and consistent behaviours that many clients may not have experienced previously.
2.2 FNP in Scotland
2.2.1 Policy
The Family Nurse Partnership (FNP) was introduced to Scotland in 2009. Focused on addressing the individual, social and economic challenges faced by young, first time mothers and providing a licensed, evaluated programme, and monitored for quality and fidelity, FNP was viewed as an ideal, long-term investment from Scottish Government. FNP aligned with the aims of three overarching strategic policy frameworks that had recently been published by The Scottish Government. These aimed to tackle poverty (Achieving our Potential, 2008), health inequalities (Equally Well, 2008) and to provide an optimal start in life for Scotland’s Children (Early Years Framework, 2009).
Alongside these three frameworks was a revised national approach to the culture, systems and practice for services provided to children and families. This is known as the ‘Getting it right for every child approach’ (GIRFEC) (The Scottish Government, 2008), which is inclusive of the United Nations Convention of the Rights of the Child (UNCRC) (United Nations, 1989). National ambitions for giving every child ‘the best start in life’ were also clearly set out in the previous and current National Performance Frameworks (NPF) (Scottish Government, 2018).
2.2.2 Implementation
During 2009 preparations were made for delivery of FNP in Scotland, significant effort was put into ‘site readiness’ for the first test site in Edinburgh city (NHS Lothian), which included recruitment and training of the nurses, local infrastructure requirements – FNP base, data forms and data system. In January 2010 the first clients were recruited to the FNP programme in Scotland.
Following successful early implementation (Ormston, McConville & Gordon, 2014) the programme was gradually rolled out across mainland Scotland and is currently being delivered in 11 NHS Board areas (see Table 1 below):
Table 1: Implementation of FNP across Scottish Health Boards
| Board | Date recruitment began | |
|---|---|---|
| 1 | NHS Lothian | Jan 2010 |
| 2 | NHS Tayside | July 2011 |
| 3 | NHS Fife | August 2012 |
| 4 | NHS GGC | October 2012 |
| 5 | NHS Ayrshire and Arran | Feb 2013 |
| 6 | Highland | Feb 2013 |
| 7 | NHS Lanarkshire | July 2013 |
| 8 | NHS Forth Valley | March 2014 |
| 9 | NHS Grampian | May 2015 |
| 10 | NHS Borders | August 2015 |
| 11 | NHS Dumfries and Galloway | Oct 2018 |
Implementation of FNP in Scotland focused on developing and testing a model that aligned with outcomes of the greatest importance to Scotland, including short, medium and long term child development. It focused particularly on the strengths and risks of individual clients and on integrating with local services. In the past nine years, over 6,000 young women have benefited from the programme with over 2,800 graduations to date.
To ensure faithful replication and fidelity to the FNP model, the programme has a strong governance element. Scottish Ministers’ hold the license for Scotland and are responsible for national implementation and governance. Sub-licenses are held by NHS Boards/Local Authorities to oversee local implementation. There are standardised programme materials, visiting schedules, staff qualifications, training and supervision and data collection. Scottish Government has overall responsibility for ensuring the overall quality of the programme, monitoring fidelity, commissioning research, programme funding, setting strategic direction and providing an annual report to the University of Colorado, Denver.
2.3 Evaluation of FNP in the UK
As part of the licensing conditions, each implementing country should consider commissioning a Randomised Controlled Trial (RCT). England commissioned an RCT, carried out by Cardiff University, known as Building Blocks, this was published in 2015 (Robling et al, 2015). The study findings for the selected short-term primary outcomes raised some questions about the ‘added value’ of delivering the FNP programme, over and above universal service provision, in England. However, the study also identified areas where the programme showed some positive effects, largely related to early child development. This aligned closely to the reasons that this programme was implemented in Scotland, where FNP is considered to provide an important contribution to the Scottish Government commitment to improve early years outcomes and reduce inequality.
2.4 Evaluation of FNP in Scotland
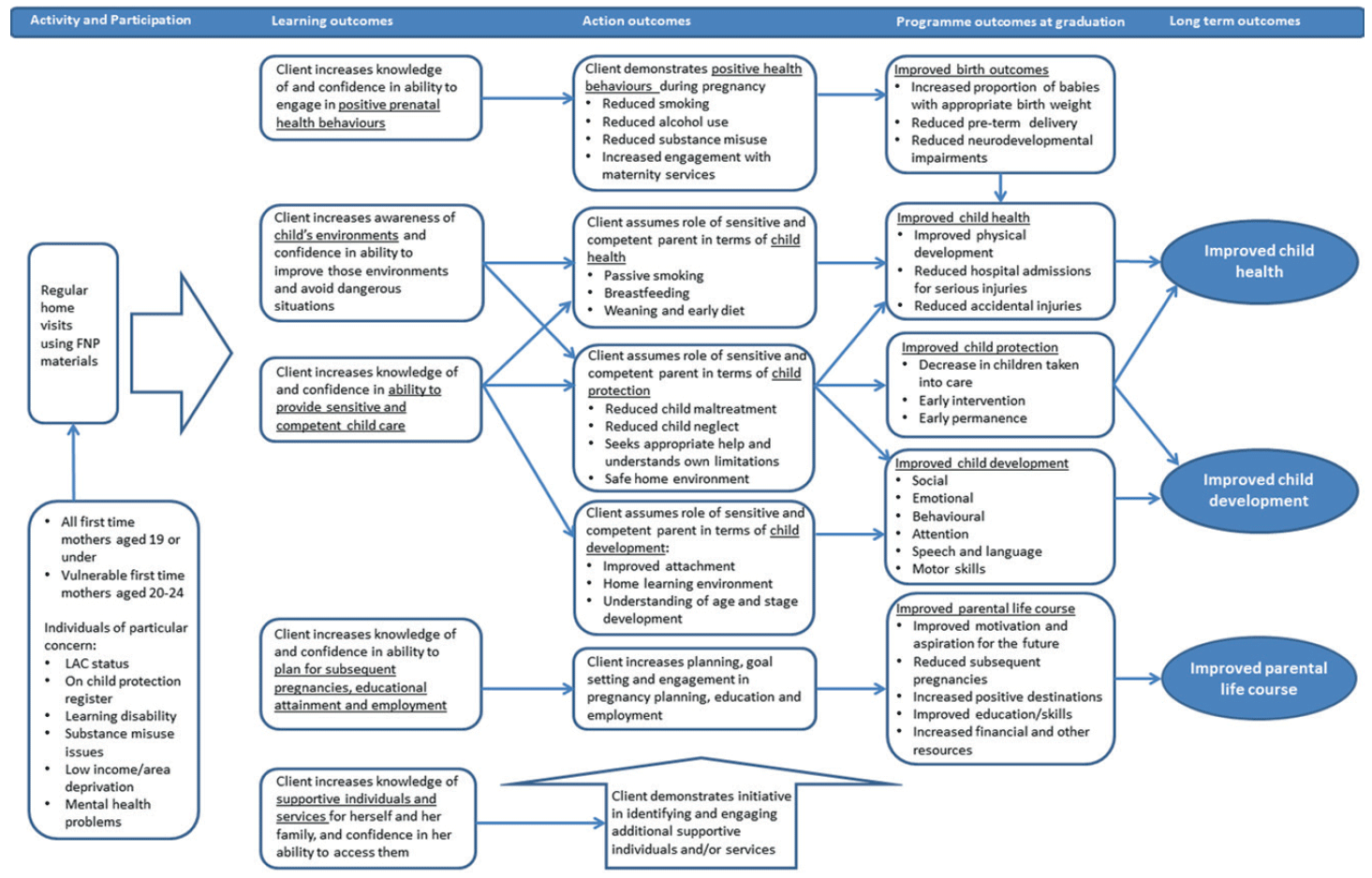
Early evaluation of FNP in Scotland focused on the process of implementation and understanding how the programme worked in the test site of NHS Lothian. This concluded that it was feasible to implement the FNP programme and meet the programme’s fidelity requirements in the Scottish context (Ormston, McConville & Gordon, 2014). This evaluation was not an impact evaluation, but provided evidence that the programme could plausibly achieve its intended long-term outcomes in alignment with its theory of Change (See Figure 1 for the FNP Logic Model).
2.4.1 Current FNP Evaluation
In 2015, an independent assessment of impact evaluation options for the FNP programme in Scotland was undertaken on behalf of the Scottish Government (Wimbush et al, 2015). This recommended options for evaluation including the use of a natural experiment method using routinely collected data on pregnancy, birth and child health to compare young mothers participating in FNP with a control group of young first-time mothers. This is currently being undertaken by Cardiff University (Cannings-John et al., 2018).
To complement this impact evaluation, and to qualitatively explore the perceived value of FNP from the perspective of clients, Family Nurses and other stakeholders in Scotland, the Scottish Government commissioned the Revaluation which is the focus of this report. This report does not provide a comprehensive analysis of primary data, but summarises the key findings of the Revaluation from materials provided by the Revaluation team.
Figure 1: FNP Logic Model
Contact
Email: carolyn.wilson@gov.scot