Residential rehabilitation - service mapping: report - 2019 to 2020
Mapping of residential rehabilitation provision in Scotland for alcohol and drug treatment.
2. Treatment and Care
2.1 Programmes Provided
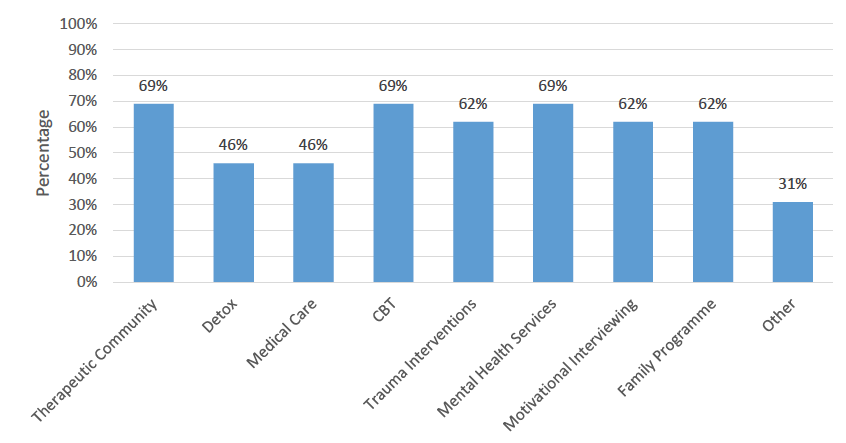
A range of programmes were available across these 13 facilities (Figure 2.1). Typically, the facilities which were classed as residential rehabilitation offered a range of medical and psychosocial programmes provided by in-house medical or mental health professionals, while those classed as specialised supported accommodation offered mostly psychosocial programmes. These figures should be treated with caution, however, as telephone conversations with a number of facilities suggested that there was a significant degree of variability in what individual providers classed as a specific intervention.
- Nine of the thirteen facilities reported offering Cognitive Behavioural Therapy (CBT); Mental Health Services, and Therapeutic Communities. Among those offering mental health services, a number of facilities offered programmes guided by mental health professionals, while others provided such services informally.
- Motivational interviewing, Trauma Interventions and a Family Programme were each offered by 8 facilities.
- In-house Detox and Medical Care were each offered by six of the facilities.
- Those who had selected 'other' reported providing a range of different services. Four provided programmes rooted in the 12-step recovery model. Five facilities reported offering a holistic rehabilitation programme. One offered education, training and employability programmes, as well as mindfulness, drama and complementary therapies. One facility offered a range of services, including recovery through nature, community engagement, mutual aid, peer mentoring, and the involvement of various partners offering interventions such as Move On Creative Writing, and women's/gender specific support. Another facility supported detox through community addiction team prescribing.
2.2 Aftercare Provision
Aftercare provision was available at 11 of the 13 facilities. This provision differed both in nature and duration. Two of the facilities stated that they offered aftercare for a specific period, ranging from 10 weeks to two years, depending on the nature aftercare provided. Four others stated that they provided indefinite support if possible. Two facilities offered formal support by weekly appointment for up to six months, while six facilities reported providing informal support to ex-residents with no time limit, if able to meet their needs.
- Aftercare Support Groups were offered by three facilities. Two of these facilities ran these support groups on a weekly basis. One offered eight different groups across two sites for two years post-treatment; four general groups, an intensive group for lapsers/relapses, a women's group, a managing anxiety group, and a mindfulness group. The weekly groups at one facility were provided in two different locations across two local authority areas and via Zoom for admissions from more remote areas. One facility offered support groups both in person (although currently online due to COVID-19) and through social media.
- Aftercare therapy packages were offered by two facilities. These involved individual and group therapy sessions undertaken post-treatment.
- Scatter flats were available to those attending one of the facilities which linked into their community-based teams and community-based social enterprises. Sixteen beds of recovery supported housing was available for those moving on after residence in another facility. One facility also provides a five-bed recovery house for homeless men who complete their treatment programme.
2.3 Peer Support and Peer Volunteering
All 13 of the facilities provide peer support and peer volunteering for those with lived experience of problematic drug or harmful alcohol use. These took varying forms. Figures relating to the take-up of such placements were not provided.
- Lived Experience in Employee Base - Ten of the facilities described having varying proportions of their employee base as having lived experience of problem drug or harmful alcohol use. At a number of these facilities, the majority of the staff and volunteers have lived experience of problematic drug or harmful alcohol use;
- Peer Support and Mentoring - Peer support programmes and mentor roles were available within two of the facilities;
- Educational and Training Programmes - Four facilities offer educational and training programmes. One offers placement opportunities for the Scottish Drugs Forum addiction worker training programme, as well as student placements for Nursing at a local college and Cognitive Behavioural Therapy (CBT) student therapist placements with the Centre of Therapy. One facility offers an accredited 12 week training, employability and education programme centring on a two-hour weekly session with Encompass. The course leads to a qualification at the end of treatment which can be added to the individual's CV. They state that more than 70% of our patients go on to complete the programme post-treatment. One facility also offers an SVQ in Health and Social Care, in conjunction with employment as a paid Trainee Recovery worker or trainee development worker, for some of those who access peer supporter and mentor roles;
- Employability Support - Five facilities described offering employability support. One of these offers employment opportunities through their social enterprises. Another facility stated that their peer supporter and mentor roles often lead to paid Trainee Recovery worker or trainee development worker roles (where work experience is combined with the SVQ in Health and Social Care). Trainees who complete this route usually employed in other positions within this organisation or other organisations in the sector.
2.4 Regulatory Frameworks
All 13 of the facilities operated within regulatory frameworks. Eleven were regulated by the Care Inspectorate (one in conjunction with the Service Level Agreement). Four of these also reported adhering to Scottish Social Services Council (SSSC) Guidelines. One facility was regulated by NHS Governance (with the residential component of their programme regulated by the Care Inspectorate), and another one by Healthcare Improvement Scotland (HIS).
2.5 Measurement of Recovery Outcomes
All 13 of the facilities monitored recovery outcomes. Five of these facilities reported monitoring recovery outcomes informally – describing maintaining informal contact with those who had left their service and monitoring relapse rates – while the other eight reported using a number of specific tools to measure recovery outcomes;
- Recovery Outcomes Web (ROW)[9] - Five of the facilities use the Recovery Outcome Web (ROW) Framework to measure outcomes. Two also assess externally corroborated outcomes for continuous total abstinence and non-offending.
- Outcome Star - Two facilities use the Outcome Star for recovery planning and measure of outcomes (with one also carrying quarterly reviews and gathering statistics when the client has finished aftercare).
- Mixed Measures – One facility reported using a number of measures. They have undertaken a longer term study to assess outcomes using the ASI-X (Addiction severity index, European version), with one-year outcomes published in a peer-reviewed journal. Successful completion of treatment is measured and reported to ADPs, Clinical Outcomes in Routine Evaluation (CORE-10) monitoring tool is used at admission and discharge, and the Treatment Perception Questionnaire is used at discharge. They also have active outreach for patients who do not attend aftercare or who are alerted to them by their peers or by themselves as needing extra attention. They also have an intensive aftercare group for those who are struggling or have lapsed or relapsed.
Five of the organisations stated that they measured medium-to long-term recovery outcomes or engaged in either formal or informal follow-up with individuals who had used their services. Two stated that they do not measure long-term outcomes. Four mentioned holding data on former residents for periods as long as 18 years but it was unclear if this referred to keeping data for an extended period of time, or if it related to long-term monitoring of recovery outcomes in individuals.
The five organisations who reported long-term measurement of outcomes described doing so for durations ranging from 18 months to 5 years. One facility reported undertaking informal follow-up with former residents for up to 14 years.
2.6 Links to Recovery Organisations and Mutual Aid
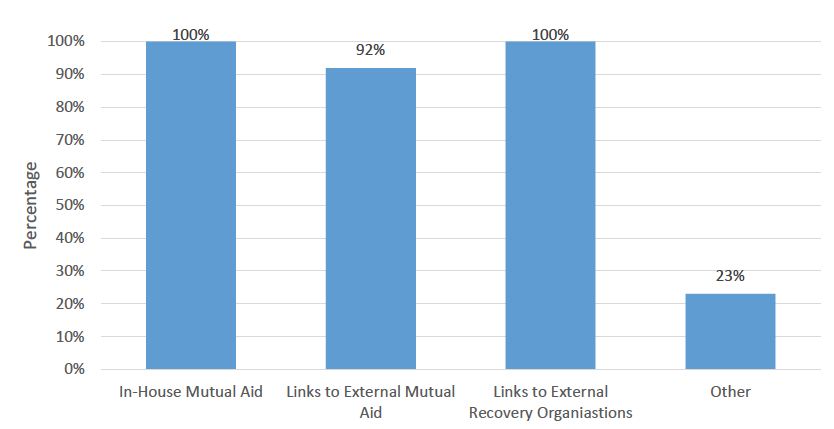
Facilities provided data regarding their links to recovery communities and mutual aid. All 13 of the facilities offered in-house mutual aid, and the vast majority (92%, n=12) linked residents to other recovery organisations upon completion of their programme. The majority (92%, n=12) also provided residents links to mutual aid organisations upon programme completion, while 23% maintained unspecified other links to recovery communities and mutual aid.
2.7 Outcomes
Five facilities provided their rehab completion rates (measured against a full program duration). One stated that they do not have a full programme duration, while another stated that their discharge and completion rates were not available.
Across these five facilities there was an average completion rate of 65.4%. In four out of these five facilities, more than two-thirds of those completed their full programme duration, while only 24% of those attending one facility completed their programmes[10]. The highest completion rate was 88%. In four of these five facilities, more than two thirds of individuals completed their full programme.
The data highlighted, however, the challenges in effectively measuring outcomes across residential rehabilitation facilities. Foremost, there is no standardised provision; the programmes and services offered across these thirteen facilities ranged substantially in nature. Linked to this, programme durations ranged from five weeks to over a year. Further, these facilities cater for different populations – focusing on a combination of drugs or alcohol, or both, and serving different demographics. Additionally, some have relatively exclusive entry criteria, while others have more relaxed entry requirements. The lack of comparability between outcomes across facilities is compounded by the lack of universal outcomes tools. Further work is therefore required in order to disentangle what length and type of programme works for particular groups.