Residential rehabilitation - service mapping: report - 2019 to 2020
Mapping of residential rehabilitation provision in Scotland for alcohol and drug treatment.
1. Mapping of Residential Rehabilitation Provision in Scotland
1.1 Background and Context
Harmful alcohol and drug use remain high in Scotland compared with similar countries. It is a challenge to reliably estimate the size and scale of problematic alcohol and drug use. However, the most recent prevalence study estimated that around 57,300 individuals aged between 15-64 were engaged in problematic use of opiates and/or benzodiazepines in Scotland[1], and it is estimated that between 4% and 6% of the adult population have possible alcohol dependency[2]. This means that it is likely that we all have someone in our life who has experienced these challenges.
Across Scotland, there were around 40,000 referrals to drug and alcohol treatment in 2019/20[3]. It is estimated that less than 5% of all referrals for drug and alcohol treatment are for residential rehab.
1.2 Number and definition of Residential Rehabilitation Services in Scotland
A scoping exercise identified a total of 18 residential rehabilitation and specialist supported accommodation services in Scotland for problem drug and harmful alcohol use. This scoping exercise involved discussion with key stakeholders and an online search. Residential rehabilitation was defined as facilities offering programmes which aim to support individuals to attain an alcohol or drug-free lifestyle and be re-integrated into society, and which provide intensive psychosocial support and a structured programme of daily activities which residents are required to attend over a fixed period of time.
It became clear during our investigations that the distinction between residential rehabilitation and many supported accommodation services is difficult to make[4]. The decision was made to adopt an inclusive approach, and therefore six specialised supported accommodation facilities were included in this scoping exercise (Benaiah; Hebrides Alpha Project; The Haven; Safe As Houses Project; Sunnybrae; Whitchester House). Throughout this document, the term 'residential rehabilitation' or 'rehab' is used throughout this document to refer to both of these service types. Residential crisis services or general supported accommodation services were not included in the list. A full list of organisations included is available in Appendix I.
A survey[5] was distributed to all 18 of these organisations. 13 (72%) of these facilities had completed the survey in the month prior to the 23/11/2020 closing date[6]. These 13 facilities contribute the majority of beds/referrals across Scotland.
Of the 18 residential rehab facilities identified by the mapping exercise, over three quarters (78%, n=14) provided rehabilitation from individuals experiencing issues with drugs and/or alcohol. Three – King's Court, and the two Jericho Houses in Greenock (Bank Street and Shankland Road) – placed sole focus on rehabilitation from problem drug use, while Jericho House Dundee was the only facility to focus solely on alcohol.
Just over half (56%, n=10) of the 18 facilities admitted those of any gender, while two of these suggested that they can provide gender specific support. Five facilities admitted only men, while two admitted only women. One (Benaiah) allowed women with children to stay with their children during the duration of the programme.
1.3 Provider Types
These 18 residential rehabilitation services are provided by a mix of public, private and third sector organisations. Voluntary or not-for-profit providers contributed the majority of residential rehab and specialised supported accommodation services in Scotland (78%, n=14), with the remaining provided by private (17, n=3) and statutory (6%, n=1) providers.
The 13 residential rehab facilities who completed the mapping survey were also spread across the public, private and third sectors. Of the 13 facilities who completed the survey;
- 10 (77%) are voluntary or not for profit - Benaiah; Hebrides Alpha Project; Jericho House, Dundee; Jericho House Greenock (Bank Street); Jericho House Greenock (Shankland Road); The Haven; Phoenix Futures Scottish Residential Service; Safe As Houses Project; Sunnybrae and Whitchester House;
- 2 (15%) are private sector - Abbeycare Scotland and Castle Craig Hospital;
- 1 (8%) is a statutory service (in the form of a partnership between the NHS, City of Edinburgh Council and the third sector) - Lothians and Edinburgh Abstinence Programme (LEAP).
1.4 Geographic Distribution
The 18 residential rehabilitation facilities mapped by the scoping exercise are distributed across 11 Local Authority areas. Glasgow City was home to the greatest concentration of facilities, with around one in five (22%) of these facilities located within this local authority area.
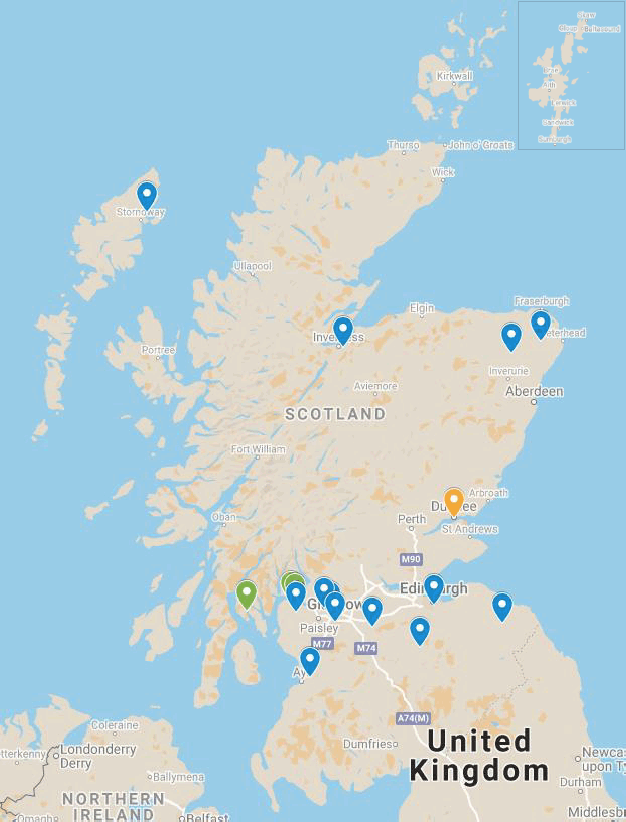
Blue pins: Drug & Alcohol, Orange pin: Alcohol only, Green Pins: Drugs only (Map generated through Google Maps)
- 4 – Glasgow City
- 3 – Inverclyde
- 2 – Aberdeenshire
- 2 – Borders
- 1 – Argyll & Bute
- 1 – City of Edinburgh
- 1 – Dundee City
- 1 – Highland
- 1 – South Ayrshire
- 1 – South Lanarkshire
- 1 – Western Isles
The 13 facilities who retuned completed surveys were spread across 8 Local Authority Areas, with three in Inverclyde, two in the Borders, Aberdeenshire and Glasgow City and one in each of the following; City of Edinburgh, Dundee City, South Lanarkshire and the Western Isles.
1.5 Number of Beds across Scotland
Data on the number of beds was available for all 18 facilities. The mapping exercise found a total of 365 beds across these 18 facilities, with an estimated 100 of these places having been taken up by those resident outwith Scotland in 2019/20.[7] Of this total of 365 beds, 173 were provided by third sector organisations, 122 by private organisations and 22 by statutory organisations.
The residential rehabilitation facilities ranged considerably in size. Castle Craig Hospital, a private provider, was by far the largest, making up over a quarter of the total provision with 101 beds (albeit having been reduced to half capacity (50 beds/places) for much of 2020 due to COVID-19 restrictions). However, less than one in six of these places were estimated to be filled by those resident in Scotland in 2019/20 (albeit with a greater proportion of Scottish residents from March 2020 due to the impact of COVID-19 on international admissions). The smallest (Maxie Richards Foundation's King's Court) has five places. Most facilities were relatively small with Castle Craig the exception; the next largest (Safe As Houses Project) was around a third of its size, with 36 beds, with two-thirds (67%, n=12) of facilities having fewer than 20 beds.
1.6 Staff Numbers at Each Facility
The 13 facilities who returned completed surveys each employed a considerably different make-up of staff (whole-time equivalent, WTE), depending on their size and on the nature of the services which they offered.
- Doctors - Four of the facilities employed doctors, with WTE ranging from 1 to 5 (average 2.1). Two facilities described holding contracts with their local medical practices for the support of detox and medical needs.
- Nursing Staff - Three of the facilities employed nursing staff, with WTE ranging from 2 to 25 (average 8.75). Two facilities again described having nursing needs supported as required by local medical practices.
- Ancillary Health Professionals - Seven facilities employed ancillary health Professionals, with substantial variation in WTE from 5 to 21 (average 10.8).
- Support Staff - Eleven of the facilities employed support staff. Again, these varied considerably from 2 to 34 WTE (average 11.8).
- Other Staff - Other staff were employed by five of the agencies. One stated that these included various trained sessional support staff to cover staff absences as required.
1.7 Duration of Programmes at Each Facility
The programmes offered by the facilities ranged considerably in length, typically depending on the nature of the programmes. The shortest minimum programme length – 5 weeks – was for the core programme at one facility (residents then have the option of moving to their extended care facility where they can stay for a number of months). Four facilities stated that they had a minimum stay of 44 weeks. It is worth noting that all of the surveyed facilities require a minimum length of stay. The programme offered by one facility was described as being open ended after an initial 3-4 month stay in their main residential unit.
1.8 Waiting Lists & Waiting Times
All but one of the facilities had a waiting list for their programmes (with one of these facilities only having a waiting list for some of their programmes). Those with waiting lists described waits ranging from a few days to a year, with waiting times within each organisation often depending on availability. Two stated that their average waiting times had been extended substantially due to capacity reduction caused by COVID-19.
These waiting lists operated in a number of ways.
- Motivation - Six facilities described admission as hinging on assessments of commitment or motivation to recovery. Three of these require individuals on the waiting list to phone the facility on a daily basis to indicate motivation.
- First-Come First Served - Six facilities described operating on a first-come-first-served basis as a space becomes available, one of whom assesses individuals within three-weeks of referral and engages them in preparation for rehab, including weekly group work. One of these reserved a bed space for emergency admissions, while another gives medical priority in certain cases.
- Greater Vulnerability & Need – Four facilities described prioritising individuals with greater vulnerability and need, including the prioritisation of those in life-threatening condition/circumstances.
1.9 Numbers Starting Residential Rehab Placements during 2019/20
A total of 1160 individuals started placements across the 13 facilities for which data was available during 2019/20, with those resident in Scotland making up an estimated 655 of this total[8]. Again there was substantial variation in the numbers accessing each facility, primarily due to the differing capacity and programme lengths across these facilities. The greatest number of individuals starting a placement at a particular facility was 407 (with 57 of these individuals estimated to be previously resident in Scotland) while the fewest was 11. Of the total of 1160 individuals starting placements across these 13 facilities, 56.6% (n=656) attended private facilities, 36% (n=420) attended rehabs provided by third sector organisations and 7.2% (n=84) attended the statutory facility.
It is estimated that a total of around 1340 individuals started a residential rehabilitation placement across all 18 facilities identified by the mapping survey in 2019/20, with an estimated 830 of these having been resident in Scotland prior to their placement. These estimates were calculated by extrapolating the ratio of beds to individuals starting residential rehab placements across the 13 facilities for which data was available to all 18 facilities. This estimate must be treated with caution, however, given the lack of data on programme lengths for a number of the facilities for which complete data was not available.
It is important to highlight that that the two rehab facilities with the greatest number of residents in 2019/20 were the two private providers. The not-for-profit provider with the greatest number of individuals starting residential rehab placement in 2019/20 had less than half the total starting placements (n=108) of the private provider with the least placements (n=249), albeit with only 40% of the private provider's total (n=100) having been resident in Scotland prior to placement.
1.10 Cost Per Case
The cost per case varied substantially across these 13 facilities, depending both on the nature of programmes offered and the funding model of the facility. The total cost for the minimum programme length across these facilities ranged from £4,615 for the 13 week core programme at one facility, to around £30,000 for the 44 week minimum stay at another. The average total cost for the minimum stay across these facilities was £17,774. The weekly cost ranged widely, from £335 per-person per-week (pppw) to £3,489 pppw, with an average of £902 pppw. These figures should be read with caution, as there is a chance that the survey question was misinterpreted as seeking a cost to the institution to provide rehabilitation programmes for each individual as opposed to a cost to the individual accessing their services. However, the margin between these two figures is likely to be small, particularly among the non-profit facilities. The list presented below displays the wide variation in both the total cost for the minimum stay and the across each facility.
- £17,445 for a 5 week programme (£3,489 pppw);
- £18,000 for a 12 week programme (£1,500 pppw);
- £18,744 for a 24 week programme (£781 pppw);
- £19,000 for a 26 week programme (£731 pppw);
- £30,000 for a 44 week programme (£681 pppw);
- £15,600 for a 26 week programme (£600 pppw);
- £25,000 for a 44 week programme (£568 pppw);
- £25,800 for a 44 week programme (£570 pppw);
- £24,900 for a 44 week programme (£565 pppw);
- £6,708 for a 12 week minimum programme, and £13416 for 24 weeks (£559 pppw), with additional detox costing £395 pppw;
- £6,500 for 12 weeks (£542 pppw);
- £4615 for 13 weeks (£355 pppw).
1.11 Admission/Exclusion Criteria
All 13 of the facilities stated, by means of an open-text question in the survey, that they maintained at least one criterion for admission or exclusion from their services. These criteria often hinged on assessments of risk to other residents or to the individual themselves, and on the likelihood of engagement in the rehabilitation programme;
- Mental Health – Five of the facilities included mental health conditions within their inclusion/exclusion criteria. Two of these stated that those with significant diagnosed or undiagnosed mental health conditions would not be admitted, while two undertake assessments on individual basis. One stated that they may not admit applicants who had recently attempted suicide or who have a history of self-harm. There is therefore a risk that those with ongoing mental health conditions who are excluded from rehabilitation facilities will also be excluded from mental health services due to continuing substance use.
- Prescription Medication – Five of the facilities included prescription medication for mental or physical conditions (primarily anti-psychotic medication and prescribed opioids). One of these did not admit those taking a high dose of these medications, while the others undertook an assessment. One stated that if individuals were on substance prescription, approval from community addiction services was required.
- Motivation – The majority of the facilities stated that they required participants to exhibit motivation prior to enrolment, often evidenced by requiring prospective residents to phone the facility on a daily basis.
- Physical Health – Two of the facilities stated that those with major physical health issues would be subject to assessment for their compatibility with participation in the recovery programme. One stated that those with significant mobility issues, complex needs requiring specialist or continual care, or incontinence problems would not be accepted.
- Detox Levels – Two facilities stated that they have exclusion criteria around detox levels from methadone (40mg), buprenorphine (16g) and diazepam.
- Homelessness status – One facility required that applicants are homeless, or at risk of homelessness.
- Previous community treatment – Community treatment which hadn't resulted in recovery from addiction was required by one of the services
- Previous offending – Previous offending formed part of the inclusion/exclusion criteria of four of the facilities. Three of these explicitly mentioned those with criminal convictions for arson, while another singled out sexual offences.
- Location – Two rehabs required that applicants are residents of the local authority area.