Reshaping Care For Older People - Update Paper
An update of the progress made in the first two years of the Reshaping Care for Older People Programme
APPENDICES

Progress and Impact
WHAT WE HAVE DONE SO FAR
The following examples represent only a tiny fraction of the work undertaken to date but they provide a flavour of the innovation in service delivery driven forward by different partners. The Joint Improvement Team (JIT) website13 and that of the SCVO14 provides further examples of good practice and opportunities to learn from other Partnerships. In addition, NHS Education for Scotland (NES)15 and the Scottish Social Service Council (SSSC) provide a range of educational resources to support health and social care workforce (nes.scot.nhs.uk and sssc.uk.com). Discover the Third Sector resource (www.discoverthethirdsector.org.uk) set up by the Quality Alliance Board or the resources available on the Scottish Coproduction Network (www.coproductionscotland.org.uk) also provide a number of resources that are highly relevant.
CO-PRODUCTION AND COMMUNITY CAPACITY BUILDING
We said…
We will:
- Use the Change Fund to drive service re-design and enable shifts in core budgets
- Put in place a community capacity building programme in collaboration with third sector providers.
- Provide support to local partnerships from the JIT in taking forward this challenging agenda.
The development of co-production and community capacity building is an essential part of developing sustainable care and support services that deliver the outcomes that matter most to people. These approaches are not new and there is clear evidence from across the globe of their efficacy but they are not necessarily widespread through Scottish health and care service provision.
What we have done since 2011
The work to support co-production and community capacity building approaches has focussed on developing the evidence base, ensuring that partners have the necessary skills and experience to undertake this work and the sharing of good practice between partnerships.
The Evidence Base
The Joint Improvement Team (JIT) have spent a good amount of time drawing together the evidence base for these approaches that demonstrate their ability to deliver better outcomes for people. In particular, the team have forged links with clinicians in Sweden who are using coproduction in clinical settings and who showcased their approach at the annual NHS Scotland event in 2013.
The development of this evidence base is supporting policy colleagues across the Scottish Government to consider how best to strengthen their own policy aims with these types of approaches. This is particularly evident in areas such as the Integration of Health and Social care where locality planning and joint strategic commissioning arrangements will have these approaches at their heart; and in SDS practice in co-producing support and care arrangements.
The Scottish Government has funded a three year 'A Stitch in Time' programme16 which will see Evaluation Support Scotland work with the four partnerships in the NHS Lothian area to establish a robust evidence base for the impact of third sector delivered services on the Reshaping Care outcomes
Increasing the skill base
Much of the emphasis over the last three years has been on ensuring that partners, especially those within the statutory sector, have the skills and experience to take forward these approaches successfully. To support this development, Governance International have provided further training on the Co-production Toolkit and a revised and extended edition of 'Coproduction in Health and Social Care: what it is and how to do it' has been published.
An outcomes planning tool called 'Contribution Analysis' was piloted with three partnerships; Ayrshire (North, East and South Ayrshire came together for this purpose), Edinburgh and the Western Isles, to test its usefulness in the Reshaping Care context. A learning report will be produced as a result in mid-2013.
The Scottish Government and the JIT have funded and support a three year project 'Change Fund: Enhancing the Role of the Third Sector' designed to build the capacity of the third sector to engage with Reshaping Care. This work will be delivered through a collaborative programme led by the Health and Social Care Alliance (The Alliance).
Sharing good practice
The key element of this has been the resourcing and support for The Scottish Coproduction Network (SCPN) to establish itself as the main forum for those interested in coproduction to connect, share learning and practice and promote the spread of the use of this approach. This has been augmented by a coproduction and capacity building conference, opened by the Cabinet Secretary for Health and Wellbeing, Alex Neill MSP, in February 2013.
To further support the sharing of good practice from across the Partnerships, case studies of good practice in the use of community capacity building and coproduction approaches in RCOP have been gathered from each of the 32 partnerships areas in Scotland. So far around three quarters of partnerships have been able to submit a case study and the can be found on the JIT website.17
What does this look like in practice?
Community Capacity Building in action - Day Care Services; Fife
In 2011, partners in Fife agreed to allocate £500,000 of the overall Change Fund (£4.89 million in total) to Community Capacity Building activity. Third Sector organisations were given the opportunity to apply for grants of between £15,000 and £50,000 (for one year in the first instance) to run initiatives which would meet at least one of the four Community Capacity Building outcomes. Nine initiatives made successful applications.
The Day Centre Service is a Voluntary Organisation which operates Day Centres for Older People in Kirkcaldy, Kinghorn and Burntisland. The centre originally opened in 1994 and provided services to frail older people who are mentally alert but are housebound or otherwise limited from accessing the community unaided. This part of the centre is known as the Rowans. The project enables 140 frail older people who have a diverse range of physical issues. The project provides specialised transport, with a trained escort, to and from the centre. This allows the individual to meet up with their peers in a safe environment and to enable them to continue to be part of the community. This is very much a preventative service, staving off loneliness and isolation and is proactive in enabling people to stay in their own homes for longer before having to go into Residential Care.
The organisation also operates specialised Dementia groups (The Haven) These groups offer social and mental stimulation, activities and companionship for older people who have Dementia and are limited in their ability to access the community unaided.
"Getting a place for my gran at the Day Centre has made such a difference in all my families' lives as we all see how happy she now is. She is always cheery, continually asking when she is going back, she says to me "the people she meets there are like her own family'.
This new found happiness in my gran's life makes such a difference in all our lives as a family. It certainly gives me reassurance that when she is in the Centre, I can get on with my life - looking after my children knowing how happy and cared for she is." Karen, main carer for grandmother Betty.
Community Capacity building in action: Signposting Project in Aberdeenshire
Under the theme of early intervention, Aberdeenshire Mental Health Signposting Service has been funded to expand service to over 65s presenting at GP practices with general health and well-being issues. Two new volunteer coordinators are recruiting and placing volunteers in GP practices and community hospitals receiving referrals from health practitioners to link older people with activities/facilities in local communities to address issues of social, psychological or physical isolation. 48 people over 55 years of age have received support from the service since it was set up in 2011/12. Qualitative feedback from users and health professionals has been extremely positive.
What will we do next
The next phase of this work will see us broaden the support that we offer to all the partners who deliver health and social care services, regardless of which sector they may be employed (or volunteer) within. There is an especially pressing need to promote these approaches more vigorously in the NHS context and, within that context, to clinicians in particular.
With these things in mind, the JIT intends to work with national partners to design and deliver a flexible, tailored, in-the-field programme of improvement support to those working in these services, with a non-exclusive focus on the NHS. This is intended to give a 'big push' to using these approaches - especially coproduction - in these many and varied settings.
This work will support the achievement of the national health and social care outcomes and other relevant outcomes connected to, for example, NHS HEAT targets, Single Outcome Agreements and supportive frameworks such the Community Care Outcomes Framework.
WORKFORCE DEVELOPMENT
In order to achieve our objective of providing high quality care and support for older people we need to be sure that our health and social services workforce has access to education and training to support new ways of working. NHS Education for Scotland (NES) and the Scottish Social Services Council (SSSC) are working in partnership to ensure the workforce is able to meet the needs of services that are personalised and delivered seamlessly for the end user A range of innovative workforce and educational developments have taken place as part of the RCOP agenda to build capacity for improvement and to drive new ways of working. In addition NES and SSSC commenced "The Equal Partners in Care (EPIC)", project in 2011 to support the education and training of the health and social care workforce which includes independent and third sector staff who work directly or indirectly with carers.
Scotland's National Dementia Strategy 2010 charged NES and SSSC with developing a dementia knowledge and skills frame work for all health and social services staff. 'Promoting Excellence: a framework for all health and social services staff working with people with dementia, their families and carers'18 and an associated workforce development plan were launched in June 2011.
One of the primary focuses of the JIT has been on developing partnership working, primarily between health and social care (and housing) but now - principally due to the Reshaping Care Change Fund - also involving the third sector and the independent sector. This has been progressed through, for example, direct facilitation in local partnerships, locally-run workshops, national learning & improvement networks and bespoke intensive support programmes. These have always been run at the request of local partnerships, and have been developed to suit local needs.
What we have done since 2011
Leadership: NES and SSSC have supported 20 CHP's to enhance collaboration and outcomes in health and social care partnerships through facilitated Action Learning sets.
Sliding Doors: Further creative methods, including the use of the Sliding Doors, have generated a connection between RCOP objectives and the people whose lives this policy is designed to improve:
Stage One - Three Scotland - wide events 'Sliding Doors to Personal Futures', presenting the policy direction and ethos of RCOP through conversations between a policy 'expert', service users and carers represented by actors.
Stage Two - 'Sliding Doors: The Next Five Years' is an online resource illustrating the change in attitudes and behaviours required over the next five years to deliver RCOP.
Stage Three - 'Sliding Doors: Making it Local': prepares cross-sector and cross-agency facilitators from Health and Social Care Partnerships to deliver the drama events locally.
Carers - Following engagement with a range of stakeholders, NES and SSSC identified the outline core values, knowledge and skills which will help staff to work with carers as partners and achieve better outcomes for carers and young carers. This informed the Equal Partners in Care (EPiC): "Core Principles for working with carers and young carers" which were launched on June 12th 2013. Good Practice Guidance and an online portal have also been developed. Central to the next phase will be the development of an EPiC Implementation Network across Scotland.
The role of the network will include disseminating the core principles and other resources in relation to working with and supporting carers and young carers; and sharing of practice, issues and challenges across the health and social care workforce in Scotland.
Dementia - Since its launch NES and SSSC have taken forward a range of activities, including a range of activities under the headings of learning programmes, educational resources and infrastructure development, including:
- the development of a range of educational and learning resources for staff across health and social care. A good example is the 'Informed About Dementia: Improving Practice DVD', which is available as a DVD or online resource. It offers a baseline of knowledge and skills for the whole of the health and social services workforce. Alongside this is the development of a resource for Pharmacists and technicians focussing on the safe use of medicines for people with dementia.
- the delivery of education and training programmes for staff at all levels of the Promoting Excellence knowledge and skills framework in range of areas including psychological therapies and interventions, support following a diagnosis of dementia and palliative care.
- the development of an infrastructure to support sustainability of learning across the sectors. For instance, 310 health and social services staff in acute hospitals have been trained as Dementia Champions.
Telehealth and Telecare - Building on the foundations of the highly successful Telecare Learning Network set up by the Telecare Development Programme, the Scottish Centre for Telehealth and Telecare (SCTT) now run an integrated Telehealth & Telecare Learning Network which provides a forum for interested stakeholders to discuss and learn about challenges, lessons and future plans and needs.
Regular monthly webcasts are now broadcast to highlight activities and advances in telecare and telehealth along with national conference events held at least twice a year (including the inaugural European Telemedicine Conference in Edinburgh on 29 October 2013). This is partly facilitated through a Knowledge Network19 platform, which is the national knowledge management platform for health and social care delivered by the Knowledge Services Group. It provides high quality knowledge support for delivery of health and social care
What we will do next
The next phase of 'Sliding Doors' will see further development of the resource at a more local level by supporting more change fund partnerships to engage in the programme and developing the resource to support a broader contemporary learning agenda. There will also be a robust evaluation of the impact of Sliding Doors to date.
Over the last year workforce intelligence has been collected and collated about the knowledge and skills required to support a future-focused integrated health and social care workforce particularly for those involved in the care and support of older people and this will further inform our future plans. In relation to self-directed support, SSSC are leading on the implementation of a workforce action plan which applies right across age groups, including older people - and seeks to further the values and principles of self-directed support amongst the social care workforce.
Carers - We will look to evidence the impact of the project on related workstreams, ensuring carers are integral to all work carried out by NES and SSSC. NES/SSSC will provide support for the Change Fund Partnerships to align and embed the EPiC Core Principles for Carers and Young Carers within the carer element of their change fund plans. NES/SSSC will also support Carers Information Strategy (CIS) training plans in 2013-14.
Strategic fora can ensure that all of the key stakeholders not only share intelligence, but also map out future collaborative initiatives for the development of the health and social services workforce. The Reshaping Care and Integration Improvement Network is one such forum. It is a multi-agency collaborative of improvement organisations working together to help Partnerships create the conditions to realise improved outcomes through Reshaping Care, the Change Fund and closer integration, and the Network will continue to share good practice and facilitate knowledge exchange.
Telecare and telehealth - Under the leadership of NES, early work has started to develop a Strategic Action Plan for Technology Enabled Learning. This Technology-Enabled Learning Action Plan will reinforce our shared key message that technology-enabled learning and workforce development is an effective catalyst for the transformation of health and care services.
The overarching aim is that the "health and social care workforce at all levels will have the learning opportunities, knowledge and skills to innovate and deliver technology-enabled care".
Dementia - Between 2013 - 2016, we will extend the reach of programmes, embed existing resources, support developing networks and infrastructures to ensure sustainability and evaluate impact: - Other activities include:
- continue to undertake a range of activities to support workforce development in mental health continuing care, care home, care at home and adult day care services.
- work with partners to develop of a future focussed and public facing digital platform, utilising technology to enhance information, education, self-help and management for people with dementia, families and carers and the health and social services workforce.
What does it look like in practice?
The Promoting Excellence Framework is a real credit in a time of limited resources. It ensures that your organisation is doing the best it possibly can to shape the values and practice of your staff whilst improving the quality of care received by people with dementia.
Dementia Champion, Fife
"We recognised that we are all older people in the making."
East Renfrewshire CHP participant on taking part in 'Sliding Doors'.
"There is a will-power to cooperate between NHS and Council enthusiasm. IT and paperwork create boundaries that have bad repercussions for patients. NHS and community services need to overcome formal barriers to cooperate in the patients best interests."
Moray CHP - Occupational Therapist comment on undertaking 'Sliding Doors'
It was GREAT! I'm really pleased that we were able to work with SSSC, NES and Forum interactive on this. I have a feeling Nursing and Social Work will find a way to do this again, and again, and again. It was really worthwhile and ticked boxes on so many different levels.
Professor Tim Kelly, Professor Of Social Work at Dundee University On Sliding Doors work with 3rd year Social Work and Nursing Students
COMPLEX CARE PATHWAYS
We said…
"We will…
- Create clear pathways into and through services, particularly for older people with complex needs"
The increase in the number of older people with complex and varying care and support needs challenges partnerships to develop new pathways to improve outcomes for older people and their carers. A wide range of work has been taken forward that considers different complex care pathways and how they might be best organised to deliver person centred quality care and support.
What we have done since 2011
Enabling Progress: We have taken forward national actions that will enable and accelerate local progress in implementing the Reshaping Care Pathway. These are represented in the following 'pathway':
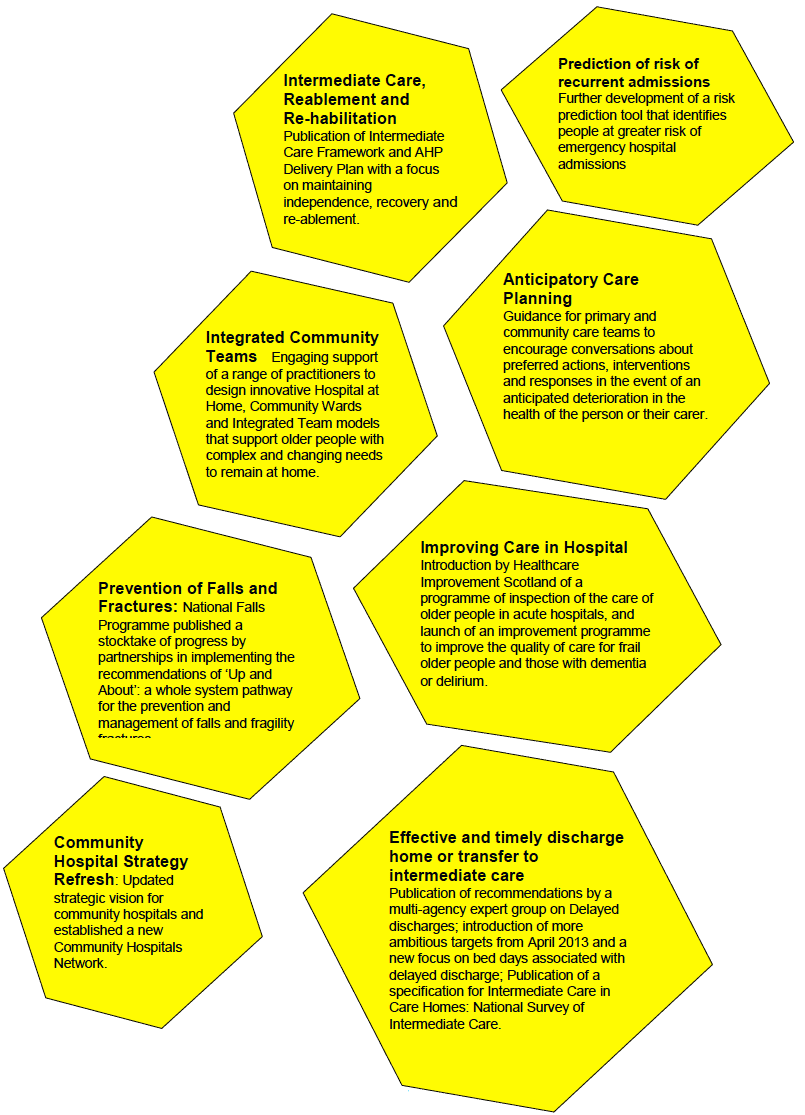
SmartCare: We have secured funding from the European Commission to deliver linked service provision across health, social care, family, informal carers and the voluntary sector.
The overarching mission of the SmartCare programme is to promote a more integrated and effective approach to the health and care of older people across Europe, by embedding an open, multifunctional ICT platform in support of joined up service processes and providers. The programme aims to unlock new services and value chains in active and healthy ageing including the involvement of relevant stakeholders in the design and operational deployment of new care pathways and organisational models for integrated care.
What does this look like in practice?
Anticipatory Care plans in action - Aberdeen City
Aberdeen City plan to put in place 1,500 Anticipatory Care Plans (ACPs) for over 75s for those people deemed to be at the highest risk of admission to hospital. The Aberdeen Partnership believes that this activity will have a major impact on reducing unnecessary hospital admissions and has contributed to the fall in multiple admissions in the last month. There are already anecdotal examples submitted by GPs of ACPs directly preventing a hospital admission. The project has also enabled a more holistic approach to be taken to supporting people to live at home, by considering issues such as home safety and wills. This focus has also been supported in another Change Fund project which seeks to identify, assess and support palliative patients (Living and Dying Well in Aberdeen) in residential settings.
Hospital at Home in North Lanarkshire
'Hospital at Home' is a key element of the North Lanarkshire Partnership's Reshaping Care for Older People Change Plan.
ASSET, an interdisciplinary, multi-agency team (AHPs, CPN, social work, Consultant Geriatricians, nursing staff, and support worker) with experience from both community and acute sectors, offers an urgent response to prevent avoidable emergency admission and deliver safe, effective and person centred care at home.
A GP responding to a patient in crisis, calls the emergency response centre (ERC), and is offered ASSET as an alternative to admission. The ASSET team will respond within 1 hour and provide the same level of care offered within hospital but in the persons own home. Assessment, diagnosis, and management of the acute episode is undertaken and communication/referral to community health and social care teams to continue support to maintain at home.
Outcomes data indicate that:
- around 80% of patients seen are able to be kept at home.
- mortality rate compares favourably with the rate for those hospitalised
- readmissions are low and are comparable with the rate following acute care.
- acceptability from patients and carers is high.
- average length of stay on Asset team is 4.4 days.
- reduced demand and improved flow has enabled closure of 18 specialty beds.
Hairmyres Hospital Discharge Hub
A Discharge Hub has been established in Hairmyres Hospital to reduce the delays experienced by people who required additional services waiting to be discharged home. Previously, people who required support from homecare services experienced delays in assessment of their needs and implementation of their package of support. Extensive joint work was carried out by health and social care staff at both managerial and operational level to identify the bottlenecks in the whole system. Following this analysis, a period of joint planning took place to ensure that the new process would address these delays and improve the journey for patients and their carers.
The Discharge Hub brings together discharge experts from nursing, social work, mental health, homecare, allied health professionals and a hospital carer coordinator. People who require support for discharge are referred from the hospital wards to the Discharge Hub and twice daily discussions of cases take place with all of the discharge experts having an input. Following this, the Hub will then allocate the case to either one of the following teams 1) CARS where the person requires rehabilitation 2) Home care 3) Social Work for complex cases. The next stage involves a mini - assessment being undertaken with the person in hospital and a support plan is put in place to facilitate the person's discharge home. The new processes are being evaluated positively and significant reductions in delays are being demonstrated consistently. In addition the roles, responsibilities and interventions of each professional are now better understood and integrated working is now evident in the team of staff working in the Discharge Hub.
The Integrated Discharge Hub is demonstrating an average reduction of circa 20 patients per day who would previously have been in Hairmyres Hospital pending access to home care, CCA processes etc.
What we will do next
The JIT will continue to support Partnerships to implement these complex and interdependent interventions at sufficient scale to demonstrate impact on outcomes and to sustain improvement through better use of their resources as they develop local Joint Commissioning Plans. Some further national actions that are underway are
- Publication of a national action plan for Active and Healthy Ageing as a platform for the 2014 Commonwealth Games and to build on the learning from Go for Gold and Making Every Moment Count programmes;
- Scaling up Intermediate Care and Hospital at Home across Scotland including maximising the contribution of community hospitals, Third sector, independent sector and housing partners.
- SmartCare will utilise technology to support the health, care and wellbeing for the over 50s with a specific focus on falls prevention. While initial work concentrates on 7 Partnerships across Ayrshire, Lanarkshire and the Renfrewshires until 2015, we will seek to scale up this approach across Scotland.
- Work with Primary Care and Pharmacy colleagues to provide guidance, share learning and maximise the impact from Anticipatory Care Planning and Polypharmacy reviews introduced in the GP contract from April 2013 - 80,000 people to benefit by 2015.

Source: NHS Scotland Photo Library
Intermediate Care
Intermediate Care is an umbrella term given to a collection of services delivered at 'transition points' in a person's life, particularly from hospital to home (and from home to hospital) and from illness or injury to recovery and independence; helping them achieve their personal outcomes.
Intermediate Care should be brought in at times of "crisis" to complement existing care services (where these are in place), providing a person centred, outcomes focused package of care. It can also form part of a range of planned interventions, this is particularly important for those with long term conditions. Wherever possible this will be provided in the person's own home, but a range of services are likely to be needed, including care homes and community hospitals. Good practice would suggest that part of the suite of services provided in local areas should be available on a 24/7 basis, with a fast, easy, single point of access to assessment.
What we have done since 2011
An Intermediate Care Framework for Scotland has been published. The document provides a Framework for local health and social care partnerships to review and further develop Intermediate Care within their area.
In line with the recommendations from a report by the Delayed Discharge Expert Group a new target has been introduced to further reduce the number of delayed hospital discharges:
- 28 day maximum wait for discharge to be achieved by April 2013;
- 14 day maximum wait by April 2015.
Health and social care partnerships are also now required to monitor the number of bed days lost through delayed discharge. Local trajectories could be set by local partnerships to reduce the number of bed days lost.
Making effective use of Intermediate Care services, will over time reduce the level of patients delayed, and the length of these delays.
What it looks like in practice
Enhanced Supported Discharge, Edinburgh Royal Infirmary
As part of the development of transformation plans under the Change Fund an Enhanced Supported Discharge team was established within Edinburgh Royal Infirmary. The team provided rehabilitation and re-ablement through AHPs, healthcare assistant and social care assistants to support discharge from acute medicine for the elderly, general medicine, stroke and respiratory wards in ERI. The servicer was set up as a 7 day services, delivering care for up to 7 days per person, with a flexible approach on an individual basis.
During the pilot 24 patients were supported resulting in:
- 109 bed days saved
- Reduction in average length of stay from 9.4 to 5.2 days
- Length of service provided in transition from hospital to community ranged from:
- 1-5 days 57%
- 6-10 days 33%
- 11-14 days 10%
CREATING THE RIGHT SERVICES AND SETTINGS
We said…
We will:
- Support a shift in focus to 'support' and away from 'services'
- Develop and extend low-level preventative services, including equipment and adaptations, handyperson services and housing support.
Joint Commissioning
Strategic commissioning is the term used for all the activities involved in assessing and forecasting needs, linking investment to agreed desired outcomes, considering options, planning the nature, range and quality of future services and working in partnership to put these in place. Joint commissioning is where these actions are undertaken by two or more agencies working together, typically health and local government, and often from a pooled or aligned budget.
Our proposals for the integration of adult health and social care explain that "each Health and Social Care Partnership will be expected to produce joint commissioning strategies and delivery plans over the medium and long-term". Further, the role of clinicians and care professionals, along with the full involvement of the third and independent sectors and service users and carers, should be embedded in the commissioning and planning process. This will strengthen the cross sector arrangements that have been established during the first two years of the Change Fund.
NHS Boards and local authorities, working with partners in the independent and third sectors, have published initial joint strategic commissioning plans in March this year. The Joint Improvement Team is leading a National Improvement and Support Programme to ensure that commissioning skills, and the quality of the plans themselves, are further developed before the statutory requirement to produce joint strategic commissioning plans comes in to effect in 2015. A national steering group has been established to set future direction and ensure all partnerships have the ability to develop local plans. Following the publication of a Learning Development Framework, we are also establishing training and education for those involved in strategic commissioning at a local level.
We envisage that good joint strategic commissioning plans should:
- Identify the total resources available across health and social care for each client group and relate this information to the needs of local populations.
- Agree desired outcomes and link investment to them.
- Use a coherent approach to selecting and prioritising investment and disinvestment decisions.
- Embed patients/clients and their carers in the decision making process.
- Treat the third and independent sectors as equal partners.
- Involve GPs, clinicians and social care professionals in all stages of the planning work.
Housing
What we have done since 2011
Shifting the balance of care, from care homes and hospitals, to more homely settings within the community, will require an increased focus on housing and housing related services. The Scottish Government, in partnership with COSLA, founded the Wider Planning for An Ageing Population Group and in 2011 published Age, Home and Community: 'A Strategy for Housing for Scotland's' Older People: 2012 - 202120.
The Strategy contains our vision for older people and housing in Scotland to be achieved through 34 commitments across 5 themes and underpinned by the principles of Older people as an asset; Choice; Planning Ahead and Preventative Support. Existing good practice is noted and gaps identified.
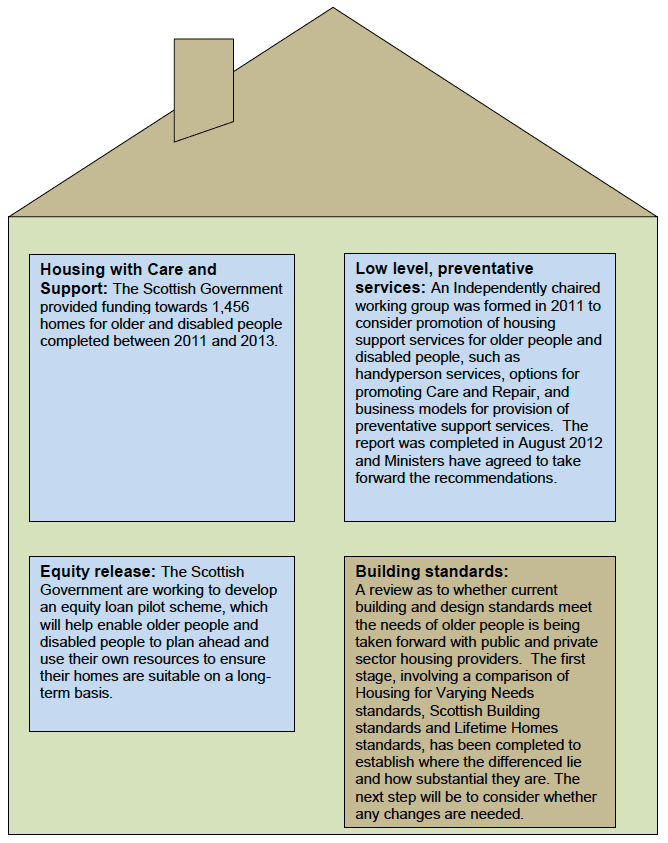
The following Figure illustrates the main elements of this work:
Housing Adaptations
The Scottish Government responded to Adaptations Working Group in March 2013, agreeing to take forward the recommendations, and work is now underway to do so.
In addition to this we have introduced a Housing Contribution Statement, as part of the Joint Strategic Commissioning Plans to improve alignment between Joint Strategic Commissioning Plans and Local Housing Strategies. We have also taken forward development work on the housing contribution to supporting people with dementia, including identifying the current levels of awareness amongst housing staff (Chartered Institute of Housing), and drawing up guidelines for design standards for adaptation of housing (Dementia Services Development Centre)
What does this look like in practice?
Very sheltered housing is a good example of how the housing sector has developed services to promote the independent living of residents. And the benefits are not confined to the positive social and psychological impact on tenants; there are clear financial savings too. A study published by Hanover, Bield and Trust Housing Associations found that there was a reduction of £19,000 care home costs per Very Sheltered Housing tenant. The Scottish Government would have been expected to pay over 60% of this.21 Whilst Mary, in the below example is a great example of how supported housing can provide the basis of an active, independent life, it's worth pointing out that nowadays, the average age of tenants upon moving into very sheltered housing is actually over 80.
Mrs Mary Stewart
Brae Court, Linlithgow
Mary moved to Brae Court 30 years ago with her husband, who had a heart condition (and has sadly since passed away). Mary was a nurse and enjoys interacting with people. Her great grandchildren call her "Supergran", and no wonder after reaching 100 years in stellar form.
"…I've lived here for 30 years, and I feel Very Sheltered Housing is an absolutely splendid idea. It allows me to keep my choice, my independence, liberty and dignity - this is what life is about! It enables you to keep thinking for yourself and do things for yourself - I've just been to the hairdressers for example - and choosing to do everything you are able to, when you want to - including helping others. Everyone here is treated as family and most people are delightful, the staff and managers are all so wonderful; This place lets me see the wider picture for people other than myself… the stimulus and physical exercise are here when you want it, which I do get involved in... and it gives my family great peace of mind to know I am happy, comfortable and safe. Independence and security are extremely important to them and to me, and I've never regretted coming here. I would recommend it to everybody."
What we will do next
- Work to take forward, as agreed by ministers, the recommendations of the Adaptations Working Group report
- Development of the aforementioned Equity loan pilot scheme.
Carers
We said…
We will:
- Support carers and communities to advance supported self care
What we have done since 2011
The Scottish Government's Carers Strategy, Caring Together, published jointly with COSLA in 2010, is being implemented across Scotland. Many local authorities have, with partners, developed their own local carers strategies with reference to the key messages and themes within Caring Together.
A key component of the Carers Strategy is identifying and supporting the carers of older people, many of whom are older themselves. Indeed, with the changing demographics an increasing number of older people will be in mutual caring situations, i.e. two older people caring for each other.
Scottish Government investment of over £97 million since 2008 to 2015 is being channelled through Health Boards and the voluntary sector to support carers, young carers and those they care for. Together with the Change Fund investment of nearly £50 million over three years, this is being used to improve outcomes for carers and those they care for. The key areas for support are through the identification of carers, the provision of carer's assessments and support through short breaks, information and advice, training, income maximisation, advocacy and so on.
There are ten Manifesto commitments to support carers, including supporting carers through the Change Fund.
What does this look like in practice?
The Change Fund working for carers
Ms G cared for her mum at home prior to her mum's admission to hospital and subsequent move into a nursing home. She had moved to the area to care for her mum and hadn't had the opportunity to properly settle into a new town and establish friendships and a support network. Ms G has both physical and mental health problems which she is addressing with input from appropriate services.
Personal Outcomes Identified with Ms G:
Ms G was referred to VOCAL's Hospital In-reach service by a social work hospital in-reach worker. At referral, Ms G felt that she had been well informed about the practical process of looking at long-term care for her mum but she was not aware of the support available for herself as a carer, at what was a very difficult and emotional time.
Ms G described herself as physically and emotionally fragile, she was tired and anxious. Arranging nursing home care for her mum, as well as hospital visiting, was taking its toll on her. She found it difficult to make time for herself. Although she felt the number of visits she made to the hospital and nursing home was too much for her, she felt that she couldn't reduce visits without feeling guilty.
Work with Ms G:
The emotional aspect of a move to long-term care was discussed at length. Reassurance was given around the consideration Ms G had given to choosing the right nursing home. Emotional support and further reassurance was offered when Ms G was in the position of deciding whether to move her mum to her 'first choice' nursing home or to have her remain in the 'interim placement' where she was settled.
Advice and some printed information was given on relaxation and improving sleep. Ms G was also encouraged to attend a Carers' Week coffee and pamper event run by VOCAL Midlothian. Ms G was given advice and reassurance around shortening visits to see her mum to ensure she had some time for herself. Ms G enjoyed a massage at the coffee/pamper event and was assisted to apply for a Carers Break Fund grant to enable her to purchase further massage sessions.
Ms G was encouraged to attend a carers singing group run by VOCAL Midlothian as a way to do something for her and also as an opportunity for peer support. At the group, Ms G was able to discuss the guilty feelings she was experiencing and she was informed of the 'Dealing with guilt' courses run by VOCAL.
Outcomes Identified at Review: Ms G decided that her Mum should remain in the current nursing home - having been able to talk this through she feels that this is the right decision and no longer has niggling doubts. Ms G attended the coffee/pamper event and "had a wonderful morning".
Ms G felt the benefit of the pamper treatments and of talking with other carers. "I simply loved the morning and left feeling people out there did care about carers"
"Just did not realise how isolated I had become"
Ms G now manages to combine visiting her mum with doing things for herself. She feels more comfortable with making shorter visits and with having 'days off' from visiting if she has other things planned.
The Carers Break fund application was successful and Ms G has begun a course of 6 massage treatments. Support was given to the Ms G on budgeting so she could continue with this once the funding had stopped.
What we will do next
The key challenge over the coming years is to ensure that carers are further supported so that they can continue caring in good health through a preventative approach. Given their significant contribution, making sure that carers are treated as equal partners and ensuring they have the right support and information is critical (it is also necessary to support existing and new carers as equal partners in care on human rights grounds and because providing preventative support helps to avoid more significant costs in the longer term).
Moreover, due to the changing demographics (increasing life expectancy, more children with complex needs surviving into adulthood and outliving their parents), family migration patterns, changing work patterns and other factors, there could be a deficit in unpaid care where the supply of unpaid carers does not keep pace with demand for unpaid care. We are undertaking further work on this important issue.
The priorities for the future are to continue the support to carers. The power in the Social Care (Self-directed Support) (Scotland) Act 2013 to support carers in their own right provides a good opportunity to do so. With partners, we will also be working on community capacity building to support carers. The integration of health and social care again provides a good opportunity to support carers on a consistent basis.
Self Directed Support and Personalisation
We said…
We will:
- Support a shift in focus to 'support' and away from 'services'
What we have done since 2011
We have begun the work to implement our 10 year strategy on self-directed support. This includes a range of activity aimed at reforming local practice in relation to assessment and support planning, reforming commissioning, instilling the values and principles associated with self-directed support, and providing the workforce with the skills that they need to deliver more flexible support with far greater choice and control for individuals.
We have delivered the Social Care (Self-directed Support) (Scotland) Act 2013, reforming the duties placed on local authorities with regard to assessment and the planning of support for individuals. The Act which applies to all age groups including older people enshrines a range of choices for individuals and helps to provide the framework of flexible alternatives for professionals and older people to work through the right solutions for them.
We have invested in transformation activity across local authorities, providers and support and information. This includes some innovative projects working with older people and their families - demonstrating how it can and how it should be done.
What does this look like in practice?
Kenny and Marlene - a new start with Self Directed Support
Kenny is in his mid 60's and lives at home with his wife Marlene. He was a well known publican in Ayrshire for many years where he and Marlene offered a warm hospitable welcome to their customers.
Kenny was then diagnosed with dementia and they moved to a sheltered housing complex specially built for people with dementia but they both felt they had no privacy and Marlene was only in her mid 40's and did not feel she had the opportunity to interact with people her own age. Kenny started to attend a local day care service but didn't really like going and only went sometimes to please his wife and give her a break.
Kenny became very isolated and rarely left the house other than to go to the day centre. Marlene was finding caring for Kenny difficult, their marriage was at breaking point and Kenny had stopped communicating with Marlene. Marlene felt that maybe their only option was to consider moving Kenny into a care home. Marlene was signposted to Alzheimer Scotland SDS project in Ayrshire and together with the family they developed a plan which would enable Kenny to remain living at home.
A crucial part of this was finding someone who Kenny would engage with and who could support Kenny to do the things he enjoys, whilst enabling Marlene to continue caring.
Kenny now employs a personal assistant (PA) using a self-directed support budget given by the local authority to meet his care and support needs. Marlene as Kenny's power of attorney deals with all the paperwork and finances for Kenny. Kenny and his PA spend time going on trips, playing dominoes at the local pub, attending social functions and have even been on short-breaks together around Scotland including to Knockhill Racing Circuit.
Having the right support has enabled Kenny to re-engage with old friends and he now returns home to tell Marlene the stories of what he has been up to and who he has met during his travels and adventures.
Kenny and Marlene have now moved into a new home and Kenny is enjoying spending time in their private garden, they are delighted with the support Kenny now receives which enables Kenny to do the things he enjoys which he can't do without support and Marlene benefits from having time to do the things she enjoys too!
Marlene said "With self-directed support I feel as if my life has come back to me…I have a life again. My husband is out and about he's meeting people, rekindling friendships - we have something to talk about….things are totally different and it's absolutely fantastic".
What we will do next
We will continue the work to implement the national strategy on self-directed support. We will ensure that older people are included in that strategy at both national and local level. We will complete our statutory guidance and regulations in support of the 2013 Act. We will share the success stories of when and how to implement self-directed support with older people - demonstrating the range of options available to current and future generations of older people.
Dementia
What we have done since 2011
Up to 86,000 people are estimated to have dementia in Scotland, a number that is expected to double over the next 25 years. Whilst the onset of dementia can occur from varying stages in adult life, the vast majority of people living with dementia are within the older population and two-thirds live at home.
A national commitment came into force on April 1 2013 to ensure that people diagnosed with dementia will see a significant improvement in the help and advice they receive. The commitment is based on Alzheimer Scotland's 5 Pillar model of post-diagnostic support and was made possible following significant research and practical work by the charity to address this major public health issue. Their work included a ground-breaking pilot in Renfrewshire and East Renfrewshire. The commitment is underpinned by a 3-year HEAT target that everyone diagnosed from 1 April 2013 will receive a minimum of a year's dedicated post-diagnostic support from a named Link Worker.
The Link Worker is responsible for creating tailored care plans to help those living with dementia and their families understand the illness, manage its symptoms and plan for future care. It will have a significant impact on the initial stages of a person's journey through dementia.
Scotland's second 'National Dementia Strategy' for 2013 - 16 was launched on 3rd June 2013 and will continue to focus on improving services for everyone with the illness, regardless of the stage of their illness or where they are being cared for. The Strategy highlights that 64% of those with dementia are now being diagnosed, a rate significantly higher than England and Wales, demonstrating effective joint working by clinicians, statutory bodies and third sector organisations.
The Report also looks forward to the impact to be made by the Life Changes Trust. The Trust was established in 2013 to manage a 10 year, £50 million investment by the BIG Lottery Fund focusing on two specific groups - young care leavers and people with dementia and their carers. The first phase of the £25 million dementia programme is expected to be delivered by the Health and Social Care Alliance Scotland (the ALLIANCE) on behalf of the Life Changes Trust.
The investment will focus on developing 'Dementia Enabled Communities', peer support and befriending, grants for individuals and third sector support organisations, and a programme of research, including establishing a 10 year longitudinal panel of people with dementia to record their lived experiences and changing needs following a dementia diagnosis.
The JIT and Scottish Centre for Telehealth and Telecare (SCTT) published a report into Telecare and Dementia, which showed that in one partnership 27% of clients with dementia would otherwise have required admission to a care home and that telecare avoided or delayed admission for an average of 606 days, saving over £29,100 per event.
What it will look like in practice
Case study - Henry Rankin, East Renfrewshire
Henry Rankin from East Renfrewshire received post-diagnostic support through the Alzheimer Scotland pilot and says it was a huge factor in helping him and his family come to terms with him being diagnosed with vascular dementia at the age of 58.
"It was dreadful. Absolutely dreadful. There's no other way to describe it. I didn't even know what vascular dementia was. I thought it was all over, that I had six months left to live."
Provided with no more information and feeling that he had no-one to speak to, he walked out to the street and burst into tears.
After months of trying to find out the cause of his memory problems and receiving little in the way of answers, it seemed like the final straw. He and his family were forced to look online for information about his illness, but could never discover what they really wanted to know: how to cope with dementia and what Henry's future was, if any.
Henry describes himself as fortunate that he was able to take part in the Alzheimer Scotland's pilot Facing Dementia Together project, which provides information and support to people recently diagnosed with early stage dementia, their families and friends.
"I can't praise Tracy [Gilmour, Manager of the project] highly enough," says Henry. "She put me at my ease straight away. She reassured me, gave me my confidence back. Getting my diagnosis had knocked the wind right out my sails, but she got me back on track. She spoke to my family too, gave them lots of information and advice. Best thing was; she was always there. We could speak to her at any time."
Tracy was able to put Henry and his family in touch with the various people, groups, public sector agencies and other organisations required to help the Rankins' plan for future legal, financial and care needs, as well as assisting them with the form-filling involved.
As Henry points out, "If someone is told they have cancer, they're pointed toward people that can help them. That didn't happen to me. They need to get diagnosis and post-diagnostic support right for people with dementia and their families. I'm glad the government's made a commitment to making that happen. It's brilliant news!"
What we will do next
We will continue to focus on improving services for everyone with the illness, regardless of the stage of their illness or where they are being cared for and work with NES and SSSC to ensure that the workforce is appropriately knowledgeable and skilled.
Over the course of the new dementia strategy we will also test and evaluate models of care for people with dementia whose symptoms have advanced to the extent that they need more intensive support to help them to continue to live well at home. This work will be informed by Alzheimer Scotland's 8 Pillar support model.
Nutrition
Access to nutritious, affordable food in the community has an important part to play in the reshaping care agenda, optimising the health and wellbeing of older people. Proper nutrition is key in preventing and reducing the nutrition related burden of disabilities, chronic disease and preventable mortality, reducing nutritional related risk factors and functional decline as individuals age, while increasing factors that protect health.
What we have done since 2011
The Scottish Government supported the production of Community Food and Health (Scotland) and Consumer Focus Scotland's report Meals and Messages published in 2011. It made a number of recommendations for local authorities to carry forward plans to provide a range of food services for people living at home in conjunction with third sector and community planning. The Scottish Government notes the findings of the WHO European Region Food and Nutrition Action Plan 2014- 2020 which cites research that in Europe 40 to 80% of care home residents of care homes and home care are at risk of being undernourished even when high quality food is available. (Forum on Nutrition in Care Homes and Home Care: how to put in place adequate strategies, 2010.) The Scottish Government also financially supports through grant funding initiatives including the Food Train which assists older people to access food deliveries and plays an important part in tackling social isolation in communities. Following a number of years of growth and success for the original Food Train in Dumfries, the last three years has seen the introduction of Food Trains in West Lothian, Stirling and Dundee, with the support of the Scottish Government and the local councils in those locations.
Equally important to nutrition is good hydration, which supports healthy nutrition but also prevents renal failure, falls, confusion and swallowing problems.

Source: LifeCare
What it looks like in practice
The Food Train initiative mentioned above started in Dumfries almost twenty years ago, and the model has been since replicated elsewhere, but there are many areas where local organisations are delivering this sort of support on the ground to meet the needs of the population. To explain the idea however, we focus on the Food Train below.
The Food Train services are available to anyone aged 65 and over who finds food shopping difficult. The Food Train operates with a great deal of flexibility: there are no minimum or maximum amounts for ordering; people are able to get the service weekly, fortnightly or less, and either short-term or long-term. Older people can join The Food Train through self-referral or they can be referred by someone else. The service is not linked to health assessments or means testing, which eliminates the bureaucracy of form filling and allows the service to start up immediately.
The Food Train provides each customer with a blank order form so they can write out their grocery order. Most customers have their order collected by the volunteers on a nominated day and a new blank form is left. Customers who have difficulty writing an order have their order taken over the telephone by staff and volunteers. Orders for the whole week are taken to the various shops, where teams of volunteers will start on them. In some shops the dried goods are packed the day before and fresh items added in the morning and in other stores the whole order is packed on the day of delivery. Delivery routes are arranged for geographical efficiency and worked around the capacity of each van. Customers receive their order complete with their own till receipt and their original shopping list, so it can all be checked off.
It is Food Train's vision that all older people throughout Scotland will be able to access innovative and affordable services which allow them to stay in their own homes, within their own communities, for as long as possible. In 2013, Food Train operates in six local authority areas, but there are many areas of Scotland where food access and home support remain an issue for older people and we want to help address this. Over the next few years, Food Train will continue to pursue our National Development Plan, expanding Food Train into at least one new geographic area per year, while continuing to grow our services in the areas we currently operate in.
What we will do next
We will continue to encourage access to food for older people to prevent admissions to hospitals caused by falls from dehydration or lack of sufficient nourishment.
Pharmaceutical care
What we have done since 2011
Pharmaceutical care is the responsible provision of drug therapy for the purpose of achieving definite outcomes that improve a patients' quality of life. It involves cooperation with the patient, and other professionals in designing, implementing and monitoring a therapeutic plan that will produce a specific therapeutic outcomes for the patient.
Medication is by far the most common form of medical intervention. Four out of five people aged over 75 years take a prescription medicine and 36 per cent are taking four or more. However, it is suggested that up to 50 per cent of drugs are not taken as prescribed, many drugs in common use can cause problems and that adverse reactions to medicines are implicated in 5 - 17 per cent of hospital admissions .
Research has demonstrated that patients on multiple medications are more likely to suffer drug side effects and that this is more related to the number of co-morbidities a patient has than age22. There is a clear and steady increase in the number of patients admitted to hospital with drug side effects. Patients admitted with one drug side effect are more than twice as likely to be admitted with another.
There may be the situation where the potential harm of the drug outweighs any possible benefit. Drug side effects can also be more common as a result of altered pharmacodynamics and pharmacokinetics in the elderly. This can lead to a situation where adults can suffer from side effects that can lead to hospital admission.
Non-adherence has been estimated to be responsible for 48% of asthma deaths, an 80% increased risk of death in diabetes and a 3.8-fold increased risk of death following a heart attack. Another manifestation of non-adherence is failure to collect prescriptions. Two small studies show that 2.9 - 5.2% of items prescribed were not dispensed, although they were conducted before prescriptions became free. Although one pound in every eight of NHS spending is on medicines, up to half of all the medicines prescribed are not used as the prescriber intended.
In October 2012, a Chief Executive's letter was issued to health boards to address appropriate prescribing and polypharmacy. This provided a guidance document which was produced by a national short life working group drawing on projects from across Scotland which had been delivered by local multi-displinary teams drawing on geriatrician, GP and Pharmacist input. Some of this work has been facilitated by health boards and others supported through the Change Fund. There have also been additional projects that have provided training and support for carers.
What does this look like in practice?
Personalised Pharmacy services - Aberdeen
Several of the Aberdeen City CHP pharmacists have started visiting Sheltered Housing Complexes in order to talk to residents about their medicines and how they manage them. The aim of each review is to check that all medicines being prescribed are still required and that they are being taken and managed safely. A summary of the review is then sent to the resident's GP so that they are aware of any issues. Stocketgrange was the first complex to be visited. We have had a very positive response from the residents and hope that they have benefited from the review! By the end of March 2012 8 sheltered housing complexes had been visited. Although it is the CHP pharmacists who are doing the reviews, the visits would not be possible without the help and support of the Senior Care Officers in the complex who spoke to the residents and organised suitable times for the visits.
What we will do next
The Scottish Government will shortly publish an action plan for NHS pharmaceutical care. The integration of health and social care services will also see closer working with GPs and other healthcare professionals and as a result, better continuity for patients.
Telecare and Telehealth
What we have done since 2011
Since the Programme for Change was published, we have secured £5 million from the Technology Strategy Board and, in partnership with our Enterprise Agencies, have matched that funding to deliver a £10 million programme for upwards of 55,000 people over 50 in five Health & Social Care Partnerships (Forth Valley, Grampian (Moray), Highland, Lothian and the Western Isles). 'Living it Up' is using co-production to shape the way that new and familiar technologies facilitate services, products, and information to support people to manage their Long Term Conditions and wellbeing over the next three years.23
In December 2012, jointly with CoSLA and NHS Scotland, we published A National Telehealth and Telecare Delivery Plan for Scotland to 201524 . With telehealthcare already recognised as having made an effective contribution to the early redesign of our health, social care, housing, third and independent sector services in Scotland, our challenge now is to continue to innovate and expand 'technology-enabled' service redesign at scale. This joint national delivery plan outlines our on-going commitment and investment in this area, and highlights areas of considerable achievement to date.
Through our engagement work with the European Commission - who recognise Scotland as being at the forefront in Europe when it comes to the use of tele-healthcare - we have secured €2.5 million to deliver the United4Health and SmartCare projects to seven Health & Social Care Partnerships in the West of Scotland (East Ayrshire, North Ayrshire & South Ayrshire, North Lanarkshire & South Lanarkshire and East Renfrewshire & Renfrewshire). These two projects will see home health monitoring for older people with long term conditions (diabetes, COPD and/or Heart Failure) and supported falls management delivered in an integrated care model approach over the next three years. These services are regarded as a phased implementation of the National Telehealth & Telecare Delivery Plan for Scotland and an important contribution to our Reshaping Care for Older People Programme.
The JIT and SCTT has collected case studies of successful implementation of telecare and telehealth in action. For example, telecare has proven particularly effective in reducing the level of emergency admission to hospital from Care Homes by utilising appropriate equipment to reduce the number of falls among residents.
Pilots exploring the value of telehealth in tackling chronic heart failure, asthma and rheumatoid arthritis at an early stage have had exciting results in cutting down the number of emergency hospital admissions and the number of bed days.
The JIT have also published the 'Alarm Monitoring and Response Services in Scotland' Report with SCTT in October 2012, which established a profile of telecare response services across Scotland, and identified a number of key recommendations for action.
What will it look like in practice?
Technological advances, coupled with the integration of health and social care mean that rather than the 'default' option of being admitted to hospital, people have a greater chance of receiving the treatment they need in the community and maintaining their independence while doing so. It also means that discharges from hospital can be facilitated quicker, and enables greater self-management and individual awareness.
Alice is in her mid-70s and has suffered from Chronic Obstructive Pulmonary Disease (COPD) for a number of years. She lives alone and is a regular visitor to her GP and in the past year she has been admitted (by ambulance) to hospital when she has become very breathless.25
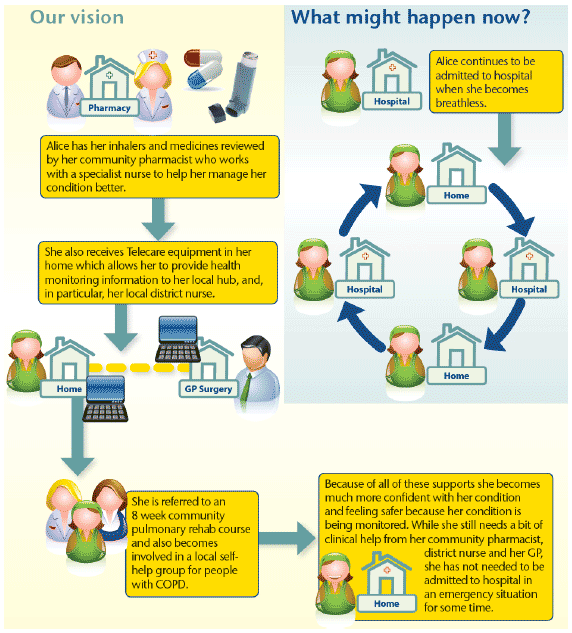
"When the practice first suggested one of the pods, I wasn't sure, but the longer I use the pod the more confidence I get. When I go out I know how far I can go before I need to use my inhaler. The pod monitors my oxygen level, pulse and sputum, so I know if I'm getting a chest infection and can start taking my antibiotics. It also gives me confidence to talk to my doctor about what I think is wrong."
Jesse, 74 year old great-grandmother on the impact of using a health monitor.
What we will do next
Clearly both telecare and telehealth have valuable roles to play in reshaping care for older people and it is important that we continue to fulfil our commitment to position Scotland is a world leader in the development and application of telecare and telehealth. The National Telehealth and Telecare Delivery Plan sets out to do just that, with one priority activity being to identify at least two further 'at scale' programmes of activity, with focus and funding opportunities to be identified by December this year (NB, the overarching commitment of the Delivery Plan is 'at scale'). JIT is working with SCTT and other stakeholders to support delivery and share learning and best practice as it emerges.
Community Equipment and Adaptations provision
Equipment and adaptations transcend condition and are an integral part of the 'service jigsaw' for people in many of the priority categories as defined by the RCOP agenda including carers, people with dementia, people receiving Reablement, those with complex care pathways, and those with palliative and end of life needs.
What we have done since 2011
Clarifying the scope of Community equipment service provision - The starting point for the work to support local Partnerships has been to help them understand the scope of the service (covering all care groups and a very wide and diverse range of equipment needs), and establishing a recognition that for the equipment service to achieve effective Outcomes for people, it must see itself as much more than a 'Store' service and an integral part of wider social care and health service provision.
Effective equipment provision starts from the point of 'assessment' and therefore the dimensions of the Community equipment service requires Protocols and policies which cover all service settings, and staff involved in identifying and assessing equipment needs.
Creating this understanding of a 'virtual service' which transcends traditional agency and professional boundaries, has assisted in improving Governance arrangements, and generating wider ownership and accountability for service provision, including appropriate financial support.
This approach also ensures that any service improvements will be developed in a collaborative way which provides a 'best fit' with the Integration agenda.
The Evidence Base - A number of reviews have been undertaken and reports produced which evidence the benefits of effective community equipment and adaptation service provision.26
This information can be used to inform services of the wider expected benefits (financial and Outcomes based) they can anticipate from improving and investing in all aspects of their services.
Increasing the skill base - A national training pack has been developed to develop standardised training material for use by any Local Authority and NHS members. The pack (which contains guidance on the provision of Trainers, presentation materials, and evaluation) was issued in Oct 2012 with the aim of improving the integrity and standard of training that is currently available, and creating on-going governance of training and quality assurance for those utilising the Pack.27
Sharing Good practice - A key element of the support to partnerships has been the sharing of good practice and evidence of 'what works' from other services. A toolkit of templates for all aspects of community equipment service provision has been utilised with partnerships to cover the key themes developed in each section of the Good Practice Guide for community Equipment provision. More recently work has been undertaken with Partnerships to improve similar aspects of service provision around Adaptations and case studies are in development to share the learning from this work.
Improving public information - To support people in our communities to be better informed about their choices in relation to equipment provision, we have produced guidance for Partnerships on the provision of public information and an example Service User leaflet, which provides information to people to allow them to make independent choices about purchasing equipment for themselves.28
What does it look like in practice?
Evidencing Outcomes- service user surveys
Gathering data on the impact equipment provision has made in achieving effective Outcomes for people, is essential to assist Partnerships to make decisions about the level of investment which should be applied to this aspect of service provision.
One Partnership conducts a regular survey of the people who have received its service. It includes questions to try to establish the difference the provision had made- the Outcomes. This has provided very useful data that confirmed that 30% of those surveyed needed less help from other as a result of the equipment provision. Nearly 90% felt that the equipment had helped them resume activities or do more for themselves and 70% felt it had made it easier for their carers to support them. This type of information is essential to prove the difference being made and in supporting future investment and shifting service provision. Work is on-going with a number of the Partnerships to implement Outcomes based service surveys which will evidence the difference the equipment provision is making.
Third Sector involvement
Building additional capacity in the 3rd sector is an essential component of the Reshaping strategy. To date much of the work around equipment has focused on services resolving fundamental issues with current inter-agency provision, and basic infrastructure issues, however all partnerships have been encouraged to consider opportunities related to involving 3rd sector providers in the provision of equipment.
- One island Partnership utilised Change fund monies to support a local community disability charity to provide a range of small items of household equipment to sell direct to the public. This has helped the Partnership to review its policy for the provision of equipment and agree the types of equipment that people in communities should be encouraged to pay for themselves.
What we will do next
Work will continue to drive forward the support work to Partnerships as detailed in the Equipment and Adaptations Workplan, and develop more case study evidence to illustrate the benefits of the service improvements. The next phase of this work will encourage Partnerships to provide and develop dedicated resources to support the extensive work required to address wholesale community equipment service improvements, and to ensure ongoing governance, service development and monitoring, in a cohesive Partnership basis.
There is also a need to widen the interface of the work around community equipment and adaptations with other key priorities within the RCOP programme.
Re-ablement
What we have done since 2011
The JIT has recently published a Report on a Survey of Re-ablement Activity in Scotland and Performance Measurement.29
The report indicates that there are a range of approaches to re-ablement being adopted across the country, from whole system activity, including joined up working with the health and independent sectors in some areas of the country, to discreet and focussed activity on discharge services. Some areas have developed step up, step down support which utilises care home and housing resources.
The report confirms that the re-ablement approach is shifting the focus of services from task and time approaches to person centred services through dedicated and goal focussed assessment which is well received by service users and carers.
The JIT will continue to lead work to understand the impact of re-ablement on personal outcomes, costs for care at home services and on the relationships to practices in rehabilitation and Intermediate Care
What will it look like in practice?
Re-ablement in action
Stirling Council have accelerated the implementation of re-ablement services across their partnership area. The impact has been a 30% reduction in home care needs and fewer long term care beds purchased as more people return home after a period of intermediate care delivered jointly by an integrated health and social care team.
2009
- 1285 Care at home service users
- 670 Older people in care homes
- Balance of Care - percentage of people with intensive support needs who live in housing, rather than a care home or a hospital setting 18%
- Cost of care £6.7m (Homecare)
- £9.6m (Care homes)
2013
- 1403 Care at home service users
- 472 Older people in care homes
- Balance of Care 35%
- Cost of care £6.7m (Homecare)
£7.3m (Care homes)
What we will do next
We will progress work to embed re-ablement in our approach to care and support for people with dementia, strengthen the links with Intermediate Care services, increase the adoption of re-ablement in the independent sector and in partnership with the Third sector. The re-ablement approach will increasingly be mainstreamed into all services.
Specifically, the JIT with partners including ADSW and the Independent sector will assist the development of practice in the coming year through
- Performance improvement and commissioning for reablement
- Dementia and reablement Training and development
- Supporting the contribution of Allied Health Professionals
- Promoting and sharing best practice
- Promoting the contribution of Self Directed Support
- Demonstrating Impact
- Medication
- Research
Palliative Care
The Scottish Government continues to support the implementation, governance and leadership of palliative and end of life care through the Living and Dying Well National Advisory Group and through collaborative working with NHS Boards, Healthcare Improvement Scotland, NHS Education for Scotland and the Scottish Partnership for Palliative Care (SPPC).
What we have done since 2011
Since 2011 there have been a number of outputs which support high quality palliative and end of life care. These include:
- Palliative Care Indicators
- Palliative Care Acute Hospitals: Development of Deteriorating Patient Stream and clearer links with the Scottish Patient Safety Programme
- Palliative Care Zone: Providing patient and carer information
- Children and Young People Palliative Care framework
- Palliative Care Guidelines
- Palliative and End of Life Direct Enhanced Service (DES)
SPPC have also worked with the JIT to deliver a series of webexes featuring case studies on palliative and end of life care and have published a special e-Bulletin, to raise awareness of the contribution of palliative and end of life care to the objectives of RCOP.30 31
The Scottish Government continues to support the SPPC in taking forward the Good Life, Good Grief, Good Death approach to death, dying and bereavement. Good Life, Good Death, Good Grief is a national alliance of organisations and individuals lead by SPPC and was launched in November 201132 . This initiative grew out of Living and Dying Well, and recognises that a major barrier to better death, dying and bereavement is the lack of knowledge and openness about these subjects in Scottish society. For example:- a lack of openness on the part of public and professionals makes it difficult to discuss plans for care towards the end of life, which leads to poorer outcomes. Bereaved people often experience isolation because people are afraid of saying the wrong thing. 60% of Scots die without having made a will, with the potential to leave behind financial and legal complications for loved ones.
What will it look like in practice?
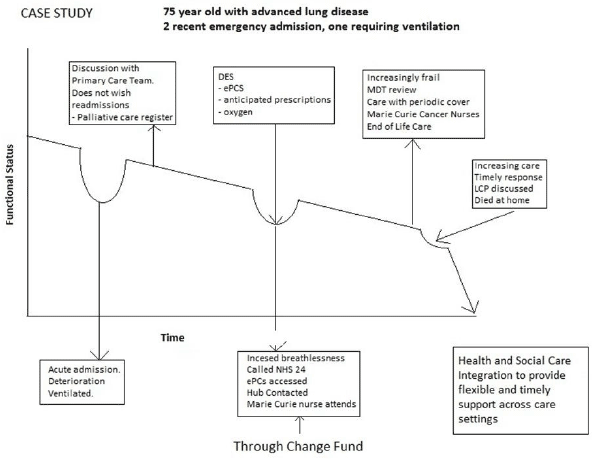
What we will do next?
The Scottish government and partners will continue to progress the key priorities for palliative care identified in Living and Dying Well. These include:
- Advance/Anticipatory Care Planning (ACP) (including DNACPR, ePCS (now KIS)
- Acute (now through SPSP Deteriorating Patient work stream).
- The Scottish Palliative Care Directed Enhanced Service (DES)
- Early identification of patients who may need palliative care
- Electronic Palliative Care Summary (ePCS)
- Children/Young People Acute Deterioration Management (CYPADM)
This work will need to be underpinned by continuing cultural and attitudinal change on the part of public and professionals, supported by the work of Good Life, Good Death, Good Grief.
In December 2012 the Scottish Government with the support of stakeholders issued a statement to provide clarity on the Liverpool Care Pathway. This included a FAQ's section which it is hoped will address the concerns faced by members of the public.
Adult Protection
Over the last 2 years, the Adult Protection Policy Forum has been created to allow Scottish Government and the bodies named in the Act to meet quarterly to consider key issues and to inform the strategic direction for adult protection policy in Scotland. Moreover the Scottish Government has been supporting the role of the National Adult Protection Coordinator - this role involves making connections to build stronger local networks and to improve the co-ordination, development and dissemination of best practice, as well as promoting joint working between Adult Protection Committees.
The Adult Protection Policy Forum and Scottish Government are currently working on 5 national projects with the aim to deliver outcomes to the benefit of the Adult Protection community and the people of Scotland.
Information and Advice
Access to care information for older people is vital. Our existing service, Care Information Scotland, is a telephone and website service which enables older people to access information about the range of services available, how to access care, care standards, charging information (which includes an explanation of free personal and nursing care and direct payments) and much more. We recognise the importance of the service and the other information channels available from other providers. We have undertaken a review of the service involving a wide range of stakeholders about broadening the reach of the service to all care groups and making interactivity with other users a much bigger feature. There are many considerations as we develop and implement the new redesigned service over the coming months. You can look out for developments of the service at http://www.careinfoscotland.co.uk/ or call the helpline on 08456 001 001. We would welcome feedback to ensure we provide a comprehensive and accurate picture for older people.

Contact
Email: Alan Martin