Reshaping Care For Older People - Update Paper
An update of the progress made in the first two years of the Reshaping Care for Older People Programme
3. WHAT WE ARE DOING
3.1 Our original commitments
Our initial paper, 'A Programme For Change 2011 - 2021' laid out the commitments that would be delivered through partnership working across central and local government; local communities; service providers, and more importantly, older people themselves.
- We will double the proportion of the total health and social care budget for older people that is spent on care at home over the life of this plan In 2010/11 care at home expenditure in Scotland was £404.5m which was 9% of the total health and social care expenditure on people aged 65+in that year, up from 6.7% at the start of the Programe.
- We will build the capacity of third sector partners to help them do more to support the experience, assets and capabilities of older people. Through the 'Change Fund: Enhancing the Role of the Third Sector' collaboration and development programme, and JIT's work on Community capacity building and Co-Production, there are many case studies of good practice now available.
- We will introduce a £70 million Change Fund for 2011/12 and in the region of £300 million over the period 2011/12 to 2014/15 to stimulate shifts in the totality of the budget from institutional care to home and community based care and enable subsequent de-commissioning of acute sector provision. With £80 million allocated in 2012/13, and a further £80 million for 2013/14, we have so far distributed £230 million to local Partnerships.1 When taking into account additional funds added by some partnerships, the total Change Fund resources to date is even higher.
- We will shift resources to unpaid carers, as part of a wider shift from institutional care to care at home. In addition to the £97 million allocated by the Scottish Government to support carers between 2008-15, a further £46 million of Change Fund monies for three years is providing direct and indirect support for carers, including the identification of carers, the provision of carer's assessments, opportunities for short breaks, information and advice, training, income maximisation, advocacy and so on.
- We will improve quality and productivity through reducing waste and unnecessary variation in practice and performance with regard to emergency admissions and bed days across Scotland.
A bill that will integrate our Health and Social care service was introduced to parliament in May 2013. After enactment, local authorities and health boards will commission care services through a joint framework, which will help drive out unexplained variation in referrals to care homes and hospitals. We have also released £50 million for Health Boards to develop Unscheduled Care Plans, and promoted the use of technology as having a key role in using information better in the management of patient flow in the unscheduled care environment.
- We will aim to reduce rates of emergency bed days used by those aged 75+ by a minimum of 20% by 2021 and at least 12% by 2014/15. Since 2009/10 the emergency admissions bed days rate for the over 75s has fallen markedly, as was intended: the most recent figures for 2011/12 are an estimated 5027 per 1000 bed days compared with 5393 per 1000 in 2009/10 - a 6.8% reduction.2 Although current performance varies by individual Health Board, overall performance is on trajectory to meet the target of at least 12% reduction in the rate for Scotland between 2009/10 and 2014/15.
- We will ensure older people are not admitted directly to long term institutional care from an acute hospital. Through our Reshaping Care Pathway and Change Fund initiatives to spread Intermediate Care, Reablement approaches and the availability of telehealth and telecare packages, an increasing number of people are being discharged back to their own homes and the number and proportion of older people resident in long-term care has fallen.
- All older people over 75 years will be offered a telecare package in accordance with their assessed needs. Although the number of people in Scotland in receipt of a telecare package is at an all-time high - more people now use telecare than receive home care - we know this is one area that can still be improved. We have published a National Telehealth and Telecare Delivery Plan to 2015 to help drive this forward.
Key Actions that were to take place to help deliver the vision of Reshaping Care for Older People were also introduced in our first paper. These are presented throughout this paper alongside evidence to demonstrate progress against them.

3.2 The Older People's Change Fund
As part of the Reshaping Care for Older People Programme, in 2011-12, Scottish Ministers allocated £70 million to the Change Fund where all 32 health and social care partnerships were required to agree a programme of change that satisfied the council, NHS Board, the third sector and independent sector. With a further allocation of £80 million in 2012/13 and 2013/14 and a final allocation of £70 million in 2014/15 across Scotland, this £300 million will continue to drive the development of services that optimise the independence and wellbeing of older people at home or in a homely setting. Two and a half years into the fund, we are already seeing an increasing proportion of funding allocated to preventative and anticipatory care and proactive care and support at home, and this is expected to grow. Future use of the Change Fund to 2015 is now explicitly linked to partnerships' delivery of joint commissioning strategies, as well as more radical, innovative redesign of older people's services. Progress will continue to be monitored over the whole Change Fund lifecycle.
The Change Fund approach has worked on a number of levels:
- as an enabler for the strategic vision on Reshaping Care;
- as a lever for closer joint working, via joint ownership of the Fund through shared signatures on change plans;
- as an accelerant in changing attitudes, cultures and behaviours;
- as a means of jointly testing and spreading innovative approaches to inform partnerships' longer term investment and disinvestment decisions;
- as an important element in helping partnerships develop and implement Strategic Joint Commissioning - with the expectation that this will become a permanent way of planning and providing services locally; and
- as a key catalyst for the changes envisaged in the integration Bill currently before Parliament particularly in relation to integrated budgets and the requirement to share partnership resources.
We already recognise though that the hard work and positive results that we have seen over the last two years have also highlighted challenges. Views were sought from local partnerships within their returns for the 2012/13 mid-year Change Fund progress report3 as to what they feel have been, and will be the greatest challenges facing them in transforming care and support for older people.
The most common challenge reported was the pace and scale of change, and how to make long term shifts towards prevention in the face of immediate and short term pressures from rising demand and significantly reduced funding. The complexity of the transformational change underway was also reflected in feedback about developing and sustaining new and changing relationships with multiple partners. Furthermore, there are the anticipated workforce challenges that will arise from integrating health and social care and having local authority and NHS staff come together.
It was particularly pleasing to have partnerships offer potential solutions to the challenges they had identified, many of which can be trialled and implemented at a local level, but also some useful suggestions that would be best implemented from 'the centre'. Examples of suggested solutions include:
- Surveying the key issues and support required and the available capacity knowledge and skills.
- Clarity on joint governance, individual roles and responsibilities
- On-going and regular communication with community groups, third and independent sector organisations and statutory services;
For many partnerships, the Change Fund has acted as a catalyst to accelerate progress in achieving sustainable improvements in outcomes for older people, enhancing collaboration and integrated working within and across sectors. It is true that some partnerships have experienced challenges in fully engaging all sectors and stakeholders, including those in acute and primary care sectors, as well as third and independent sector stakeholders. But many more have used the Change Fund to gear up for sustainable change by tackling more immediate problems (eg addressing inappropriate hospital admission by enabling earlier discharge to the community by providing both community and hospital-based interventions). The Fund has helped to redistribute resources away from hospitals and long-stay care homes and towards preventative, anticipatory and more proactive community based services.
There is good evidence that these approaches have helped deliver better outcomes for people. However it is clear that achieving longer term shifts will continue to present challenges to partnerships. Further insights into the effectiveness of the Change Fund will be provided by Audit Scotland, which will produce a report in autumn 2013; and by the Scottish Government's Analytical Services Division, which will publish an evaluation of the Change Fund in 2015.
Next steps for the Change Fund
The Reshaping Care Change Fund for Older People has been a powerful lever to engage NHS, local authority, third and independent sectors to work more effectively together and to share ownership of local change plans. It has helped bring about change in attitudes, cultures and behaviours and greater focus on preventative and anticipatory care. In the subsequent period, responses to emerging pressures are likely to focus on redesigning complex and high cost services that are currently not delivering the outcomes that people need, especially in less affluent areas. The Public Services (Joint Working) (Scotland) Bill has highlighted this in extending integrated care from older people to all adults, including those with multiple, long term conditions. Audit Scotland and other stakeholders are helping to determine where the Fund has made most impact during its lifetime, and this will inform future decisions on sustaining and developing the good progress already made.
3.3 Current Policy Framework
The last three years have seen a number of policies, strategic and legislative developments that will have an impact on the health of our older population. The Scottish Public Health Network has produced a 'Policy Landscape' that maps these back to 2005 providing a wealth of information across the range of activities that can support healthy living4 . Rather than re-iterate the detail of that work here, we try instead to give an overview of the themes that underpin much of the work undertaken to date and underpin the development of the revised outcomes framework for Reshaping Care for Older People. These themes can be seen to fall within two broad groups: individuals (and their carers) and communities; and partnership development.
For Individuals and Communities
Free Personal Care
Free Personal and Nursing Care was a proud achievement of the Scottish Government some years before the Christie Commission reported their findings. While the cost of it has often been scrutinized and challenged, the Scottish Government is committed to this policy which is a distinctively Scottish way of providing care without charge for our older people who have eligible care needs.
The Shift Towards Prevention
The Christie report found that as much as 40% of public spending was focussed on combating problems that could have been avoided had we invested more fully in a preventative approach. We have taken this on board, and progressed the agenda of prevention not solely for the financial benefits, but for the social benefit of improving people's quality of life. To this end, the Change Fund was set up to allow local partnerships across the country to distribute funding that would help maintain and develop preventative services.
It is also important to note that as part of the public service reform agenda, the Scottish Government and COSLA have committed to a renewal of community planning arrangements, to ensure that local partners have the tools to coordinate and plan all public services in pursuit of an agreed set of outcomes, as expressed in the SOA. In respect of older people, this will mean that there are new possibilities for the coordination of health and social care services with other important support arrangements like community transport, leisure, adult education and so on. It will also mean that resources can be used more flexibly at local level to invest in prevention.
Implementing Care Bundles for the Reduction of Recurrent Falls in the Community
The Scottish Government has worked with its partners in COSLA, the NHS, third and independent sectors to develop a phased multi-agency improvement programme to support a reduction in falls in a variety of care environments. Phase 1 will establish an improvement collaborative to drive this work with a range of care homes across Scotland. Phase 2 will seek to spread the improvement work at scale and extend into other care environments such as "care at home". The team supporting this activity will develop asset building approaches with leisure and planning services as well as housing associations and other third sector and older people's organisations.
The purpose of the programme is to introduce a systematic, effective and sustainable approach to reducing recurrent falls amongst older people in the community setting. The overarching aim is to contribute to a 20% reduction in the rate of emergency admissions in people 65 years and older across Scotland due to falls, by 2014/15
Active and Healthy Ageing Plan for Scotland (2013-16)
In 2012, building on the momentum gained during the European Year of Active Ageing, NHS Health Scotland, the Joint Improvement Team and the Scottish Government engaged partners from health, social care, housing, third sector, independent sector and the Scottish Older People's Alliance to develop a joint 3 year plan for Active and Healthy Ageing in Scotland.
The plan builds on the many existing strategies and good work already underway to improve the health, wellbeing, lives and life circumstances of older people in a range of settings across Scotland. It seeks to identify actions that can readily be spread or scaled up by Partnerships. All of the actions within the plan support the ethos of Christie and its focus on prevention. The plan is fully aligned with the current work to review the outcomes for Reshaping Care. It will also support local Partnerships to deliver their commitments for older people and prevention within their Single Outcomes Agreement.
National Telehealth and Telecare Delivery Plan
We know that, deployed thoughtfully and appropriately as part of service redesign, telehealth and telecare can support people to have greater choice, control and confidence in their care and wellbeing and enable safer, more effective and more personalised care whilst delivering better outcomes for the people who use our health, housing, care and support services. The National Delivery Plan recognises the synergies between telehealth and telecare, and brings them together into a strong Delivery Plan that sets out the contribution that telehealth and telecare can make to wider strategic policies for health, care, housing and wellbeing in Scotland; establishes some key priorities for action, and continues to support the development of good practice and shared learning of 'what works' (and what doesn't). Furthermore, it sets out an ambitious target of enabling choice and control in health, care and wellbeing services for an additional 300,000 people.
3.4 Self Directed Support
The Social Care (Self Directed Support) (Scotland) Act 2013 will ensure that people have greater power to choose how their support is provided to them by giving them as much control as they want over how they arrange their support.
The Act places the individual firmly at the centre of deciding what services they receive and helps to ensure that people receive the right support or services for them.
It will take time for Partnerships and communities to work through the opportunities presented by the new Act. However, steps are being taken locally to deliver the changes that are necessary to make self-directed support a reality for far greater numbers of older people. In particular, Partnerships are focussing on:
- Developing their approach to commissioning, ensuring that their strategies provide for a suitable variety of support options, recognise the role of individuals as commissioners of their own support and providing the appropriate range of information and support services for all age groups, including older people
- continuing their work to support the cultural shift required in social work and social care practice - raising awareness that self-directed support can and does work for older people and providing professionals with the guidance and training that they need, and;
- finding new and innovative ways to work in genuine partnership with both current and future generations of older people and their families
3.5 Partnership Development
Health and Social Care Integration
The Integration of health and social care agenda has developed significantly over the last few years culminating in the introduction of the Public Bodies (Joint Working) (Scotland) Bill to the Scottish Parliament in May 2013. Once enacted, this Bill will change the way that community health and social care services will be developed and delivered. Community provision will for the first time be delivered in a formally integrated fashion by the NHS and Local Authorities and will have real traction on the whole patient journey, including the time spent in hospitals.
The proposals are based on four key principles:
Nationally agreed outcomes will be introduced that apply across adult health and social care
Statutory partners will be jointly accountable for performance against outcomes
Integrated budgets will apply across adult health and social care
The role of clinicians and care professionals will be strengthened, along with engagement of the third and independent sectors, in the commissioning and planning of services.
This legislative change will fully support the aims of the Reshaping care Programme and will help support the drive to change how services are developed and delivered. It will cut through some of the existing organisational challenges and barriers, such as the separation of budgets, ensuring that partnerships can plan for the whole journey of care and have at their disposal all the relevant resources to better support people in their own homes.
Workforce
An understanding of the importance of an integrated workforce has been built up over the past decade, particularly - but not exclusively - from the experience of CHCPs. The development of a properly integrated and skilled workforce will continue to be a key factor in ensuring high quality outcomes for service users and carers.
Successfully integrated partnerships will need to span different organisational cultures to embed effectively-coordinated teams of professionals working within health and social care settings. Many partnerships have a pre-existing or developing culture of multi-disciplinary working which is based on effective communication, trusted referral processes and a shared professional ethos. However, more work needs to be done to ensure that we fully harness the potential of integrated teams, and to identify and overcome any technical obstacles. For example, despite the successes of the last decade, single assessment processes and the advantages of co-location have not yet been fully realised.
Workforce issues therefore continue to be central to partnerships' approach to change. They will also support delivery of the 20:20 Vision for Achieving Sustainable Quality in Scotland's Healthcare and the recommendations of the Christie Commission Report for all public services. A clear framework for improvement and education and training to support integration will be crucial, maximising the potential of workplace learning, and extending shared access to a broader range of learning opportunities embedded in the workplace.
Other areas of high importance include ensuring service users and their families have easy access to care information and advice, which Care Information Scotland aims to provide; effective regulation and adult protection, delivered through the Care Inspectorate and supported by key legislation.
The Reshaping Care for Older People Programme has a lifespan until 2021. Over that period, we expect the policy landscape to further develop in order to support the health and wellbeing of older people.
3.6 Third sector Interfaces
The contribution of the third sector to the delivery of Reshaping Care for older people cannot be understated, especially in regard to the preventative agenda and personal outcomes. A third sector interface is a representative body that provides a vital connection between a Community Planning Partnership and third sector within that partnership area. In general, third sector interfaces contribute to us taking the most holistic approach to reshaping care as possible, given that they see more than just the health and social care aspects of a person's life. Further information on thirds sector interfaces can be found on the Voluntary Action Scotland website.5
The third sector has an expert knowledge (although by no means an exclusive knowledge) of community planning, which given its integral role in the future of our health and social care, suggests that the role of the third sector is only going to be of increased importance.
3.7 Aligned Reshaping Care for Older People Outcomes
Three years on, we can now see the original commitments served a crucial role in driving the Reshaping Care Agenda. There is however, an opportunity to further improve this work through the development of an evidence based logic model to assist with the development of care and support options for older people. NHS Health Scotland leads a cross-sector group to build up a robust set of outcomes that will provide the foundations for the shift in the balance of care that our programme seeks to achieve. This work is about simplifying and aligning the outcomes for older people. It helps to align the national outcome for older people in the National Performance Framework with the outcomes for health and social care integration and provides a robust mechanism for ensuring that outcomes for individuals continue to be held at the core of the agenda as the policy and social landscape continues to evolve. Health Scotland will consider how best to develop the model further over the coming months with a range of partners.
Whilst there is still some detail to be worked through, there is a broad consensus on the intermediate and long-term outcomes. The draft of the logic model for Reshaping Care for Older People supports the Scottish Government and COSLA's vision for older people and sits within a wider suite of health and social care outcomes that support the National Outcomes of the Scottish Government.
Preceding the development of the Outcomes for Integrated Health and Care, work has been progressing on developing and embedding a personal outcomes approach to practice, involving most local authority areas in Scotland, and dozens of third sector and NHS organisations. The recent review of Talking Points personal outcomes approach identified benefits for people using services and practitioners6. However, while some organisations have changed cultures, systems and processes to focus on personal outcomes, others have taken more of a 'silo' approach to implementation, reflecting a more limited concern to demonstrate outcomes for performance purposes. A priority with the national outcomes is to ensure that support is available for partnerships to embed outcomes in practice so that the broader benefits can be realised.
Recent evidence, including the Francis inquiry into assuring patient safety and quality across the system of care, has highlighted that performance management which ignores the complexity of human lives can distort organizational priorities. This can result in staff collecting data about people rather than engaging with them.7 It is therefore recognised that - with particular reference to the integration agenda - an outcomes approach can help to provide a common language and shared purpose between services, and with people using services and support. Through engagement at assessment and review, the approach ensures that care and support are appropriate and effective, avoiding service use that does not make the difference required.
The RCOP outcomes framework is intended to support an outcome approach to planning, delivery and performance and the use of evidence. It has been created to support policy makers, delivery planners, evaluators and researchers make the process more systematic, explicit and targeted.
We recognise that there are a number of pre-existing frameworks in respect of the community care outcomes framework and health and social care integration. The new model that we have commissioned as part of this publication is not intended to replace these but to add to the evidence base and further support service planning.
We have developed the model in collaboration with a wide range of stakeholders so we now have agreed outcomes for reshaping care and there is clarity about where these sit alongside and within the proposed Health and Social Care Quality Measurement Framework. We hope that the diagrams and the tools that Health Scotland will provide within them, will provide professionals with new insights into the evidence base and help the public understand the goals we are trying to achieve as part of the reshaping care programme.
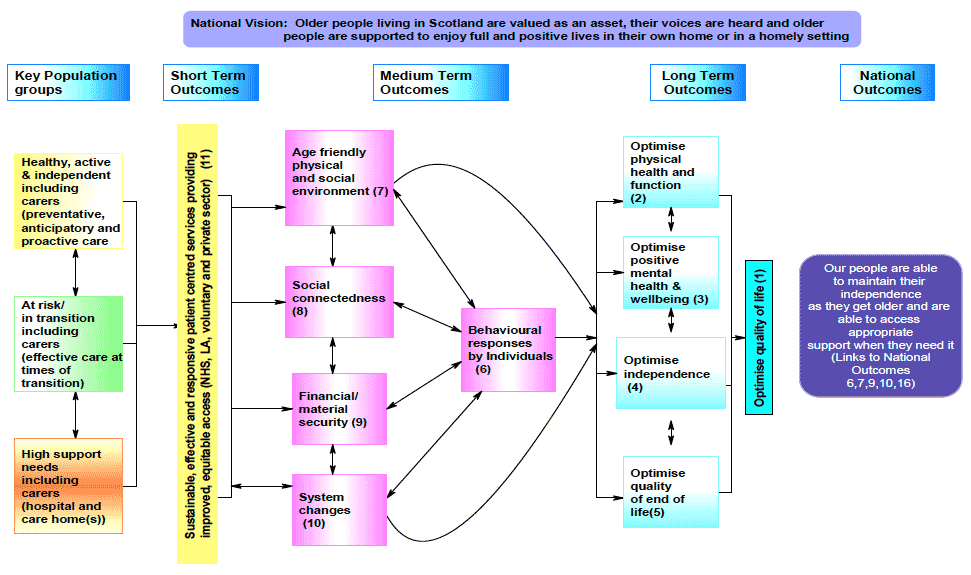
Notes on Models
The RCOP logic model is intended to support an outcome approach to planning, delivery and performance and the use of evidence. It has been created to support policy makers, delivery planners, evaluators and researchers make the process more systematic, explicit and targeted. The model identifies outcomes at four different levels:
1. National Outcomes: The vision for RCOP links to a number of National Performance Framework outcomes, which can only be achieved as the result of successful collaborative efforts across the public, private and third sector bodies.
2. Long Term outcomes (boxes 1-5) are desired population level outcomes which are the consequence of a wide range of interacting factors that many public sector organisations can only indirectly influence.
3. Medium Term outcomes (boxes 6-10) are improvements in the 'determinants' of these high level outcomes, for example:
- Behavioural responses by individuals (6) (enabled and supported to participate in healthier lifestyle e.g. physical activity, tackling sedentary behaviour, healthy eating, stop smoking safe drinking, drug use, sexual health).
- Age friendly physical and social environment (7) (housing that meets needs, feeling safe in physical environment, access to affordable transport, food and leisure opportunities, increased mobility, stigma and discrimination against older people reduced, people able to plan and discuss needs about ageing and dying).
- Social Connectedness (8) (Secure and supportive relationships, confidence and motivation to participate in community life, feeling valued and encouraged to make a positive contribution age friendly, resilient communities) .
- Financial/material security (9) (reduced poverty - adequate income, ability to pay for basic commodities e.g. fuel, food, rent, opportunities for paid and voluntary work, access to financial support available).
- System changes (10) (National policy and local practice reflect shared vision and outcomes of public service reform, culture embraces change and continual improvement).
4. Short Term outcomes (11) Local service providers have more control over short term outcomes and performance management within the service delivery partner organisations that contribute to SOAs can be monitored. Short term outcomes and related interventions will be expanded through the development of nested models relating to the medium term outcomes. For the purpose of the strategic model short term outcomes are currently described as sustainable, effective and responsive patient centred services providing improved, equitable access (NHS, LA, voluntary and private sectors).
5. Key population groups link to the Reshaping Care Pathway
More information about this framework is available at: http://www.healthscotland.com/scotlands-health/evaluation/planning/hi-performancemanagement-nhs.aspx
3.8 Reshaping Care Pathway
Using evidence from the Chronic Care Model and building on experience in Scotland developed through the Long Term Conditions Collaborative and the Reshaping Care Improvement Network, we have developed The Reshaping Care Pathway. This represents 4 'pillars' of interventions, approaches and enablers which span primary, community and acute sectors and make best use of the assets of the Third and independent sectors.
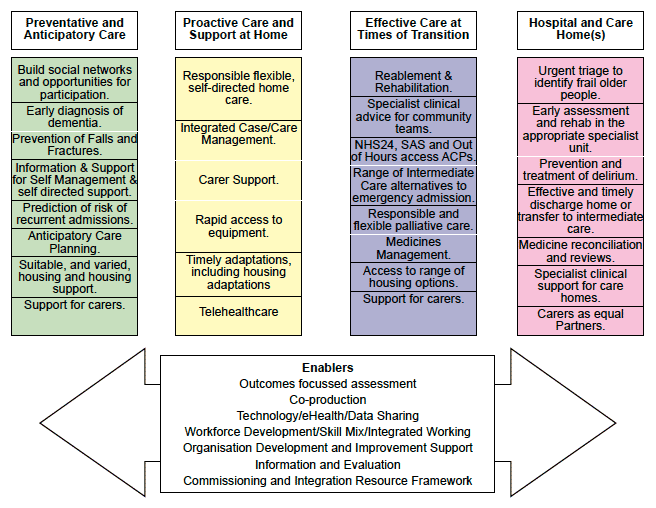
The 4 pillars of the Reshaping Care Pathway are:
- Preventative and Anticipatory Care
- Proactive Care and Support at Home
- Effective Care at Times of Transition
- Hospital and Care Home(s)
The following diagram shows the pathways and the elements within them.
3.9 Demographic Challenges to Overcome
In December 2012, the Scottish Public Health Network published an Epidemiological Assessment on the Health and Social Care needs of older people in Scotland8. It is a comprehensive body of information that can be used to inform planning over the next 20 years, in light of the twin challenges of demographics and tighter finances.
It is predicted that the total population of Scotland will increase by 8% during the 20 years period from 2012 to 2032. However, the population aged 65 years and over is expected to increase by 49% during the same period, and the population aged 90 and over will increase by 148%.
Whereas life expectancy (LE) is an estimate of how many years a person might be expected to live, healthy life expectancy (HLE) is an estimate of how many years they might live in a 'healthy' state. The most recent annual estimates for Scotland are for boys born in 2010 to live 76.3 years on average, 59.5 of these in a 'healthy' state. Girls born in 2010 would be expected to live 80.7 years on average, 61.9 of these years being 'healthy'.8
Additional healthy years for many gives the potential for additional years of work (paid or voluntary) and/or informal care for relatives; grandparents are already a key provider of childcare for 0 to 3s; the proportion of all over 60s working has increased from 11% to 16% over the last 10 years, though this rise is predominantly for those in their 60s where the rise is from 33% to 43%. However, more older people are also likely to require care.
It is suggested that if current models of care are to meet the consequential growth in service demand then Scotland's care budget for older people will need to grow from its current base of circa £5.0bn to £8.0bn by 2031.
These figures, along with the potential social benefits such as reducing isolation and promoting a sense of community give further impetus to the requirement for us to reshape care for older people.

Source: NHS Scotland Photo library
3.10 The Nature of the Public Economic Policy Challenge
The changing demographic brings a range of public policy and finance challenges related to:
- the reducing ratio of working age people to non-working age people (the dependency ratio moves from 60 per 100 to 68 per 100;)9; At a local partnership level there is a wide range of dependency ratio and
- the simple increase in people living to an age where they are more likely to access health and social care services due to frailty, cognitive disorders or other long term conditions. (the 50% increase in elderly people by 2033)
The key challenges can be summarised as follows:
Money In vs. Money Out. A reducing tax base (reserved power) relative to expenditure on pensions10 (reserved power) against increased expenditure on health and social care services vulnerable adults (devolved power). Changes to the state pension age are intended in part to address this issue. At UK level expenditure on services and pensions are expected to each increase by 2% of GDP over the period to 2057.
Workforce challenges.11 There is likely to be fewer people of working age relative to retirees; we also anticipate an increase in the proportion of the workforce engaged in providing publicly funded health and care services.
Social change.12 Social structural changes related to the family (more people living alone), geography (people living far away from relatives) and solidarity (people not actively engaged in mutual support) reduce the overall capacity for informal care. This is taking place at the same time as there are rising expectations about the quality and flexibility of care and support.
But there may be an upside, as additional healthy years for many gives the potential for additional years of work (paid or voluntary) and/or informal care for relatives; grandparents are already a key provider of childcare for 0 to 3s; the proportion of all over 60s working has increased from 11% to 16% over the last 10 years, though this rise is predominantly for those in their 60s where the rise is from 33% to 43%.
Future Demand for Health and Care Services
Assessing the impact on the demand for services is difficult to quantify with different approaches being taken to produce different estimates of change over time, though there is a consensus that everything else being equal, there will be a greater level of need. There is some consensus on drivers and elements of an approach to forecasting.
+ The simple increase in the number of older people, suggests an increase in need/demand for some services.
+ Similarly the increase in the very old living with complex long-term conditions (who have higher care costs) and in the number of people with dementia (forecast to double by 2031) is a further driver of additional demand.
- Against this we can set more years of healthy life for most people (currently only 10% of all over 65s receive formal continuing health and social care services, though about 40% of all over 85s receive such services).
- Service re-design with a shift to anticipatory and preventative approaches, alongside innovation through greater integration of health and social care has the potential to reduce the costs of care over time.
Resource Pressures
We currently spend approximately £5 billion of public funding each year on health and social care for those over 65 years across Scotland. Well over half (60%) of this is spent on providing institutional care in hospitals and care homes (and approximately one-third on emergency admissions to hospital - generally related to end of life). Less than 7% is spent on some 63,000 people who receive care at home.
The resource pressures over time are equally hard to assess, building as they do on our assessment of an increased demand for publicly funded services over time and on other factors.
We can presume some degree of inflation over time which is likely, based on recent experience, to be equal to or greater than growth in GDP. Over the next 20 years, increases in the real costs of these services have the potential to be a significant cost driver, both in respect of the availability of new treatments and in wage rises.
There is a focus on the efficiency of health and care delivery (rebalanced towards the home); constructed to maximise a person's ability to live independently; better integrated between health and social care; supported and/or delivered by technology where possible. It is difficult to assess the likely financial impact of this efficiency work and we are currently awaiting robust evaluation of these approaches.
However, even with strong presumptions about health gain and shifting the balance of care and other efficiency approaches we anticipate significant resource pressures on health and social care.
Work is currently underway to map out a number of scenarios setting out the best, worst and likely ranges in the demand for, and supply costs for health and social care for the next 20-30 years. Against these scenarios we need also need to project the possible fiscal positions for the Scottish economy over the same time period to better understand what demands will be placed on Scottish public bodies and individual to pay for health, care and support into the future.
We also recognise that we will need to develop a broader conversation about how care is funded and take steps to put that on a sustainable footing. That is one of the reasons that the Scottish Government, COSLA and other partners want Reshaping Care to be about more than service based reform: it also has to be about consulting with the public on the roles of the state and the citizen and what our citizens think about the funding of care into the future.
Contact
Email: Alan Martin