Video consultations - public and clinician views: consultation report
Consultation report of the national public engagement exercise held during June to August 2020, to understand the general public and health professionals’ views on using Near Me video consulting.
3 Analysis of feedback from other sources (public)
3.1 Introduction
Public feedback was received from a range of other sources. Individual participants completed hard copies of the survey and over the telephone and groups also responded in writing as described in Appendix 3.
3.2 Methodologies
3.2.1 Quantitative analysis
Through NHS Forth Valley's, Head of Communications they agreed to support some work to facilitate feedback by telephone. From the 22nd July 2020 until 6th August 2020 NHS Forth Valley Public Involvement Co-ordinator telephoned members of their public forum groups including:
- Carers Forums
- Gypsy Traveller Groups
- Muslim Women's Group
- Older peoples Forums
They also contacted individual members of the public who, from their networks, were known to be housebound and with deteriorating physical and mental health. During the phone call, as well as inquiring about general health and wellbeing, the facilitator asked the participants the survey questions and documented responses on hard copies of the form. Forty responses were completed in this way. A further seven responses were received via hard copies of the survey form facilitated through People First Scotland.
These responses were entered into a data base. This was to allow analysis to be carried out for cohorts who participated in the survey but who were not on-line (N=47). In part this was to test some methodologies for future use.
3.2.2 Qualitative analysis (written responses individuals and organisations)
Sentiment analysis was carried out to code comments submitted as 'benefits', 'neutral' and 'barriers' to align with the objective of the engagement exercise.
In addition, content of each response was themed, and these were ranked based on the number of mentions from different responders. Each theme was only documented once per response. Case studies were selected to reflect the balance of views.
3.3 Findings from survey responses completed over the phone or hard copy
A total of 47 responses to the full survey were received by phone or hard copy.
3.3.1 Demographics
Slightly more males (53%) than females (47%) responded. Age ranged from 27 to 88 with two thirds of working age. Of the respondents who provided their ethnicity, 89% identified themselves as white and 44% considered themselves to have a disability. Forty responses were from the Forth Valley area through the targeted telephone 'interviews'.
3.3.2 Awareness, experience, and confidence
Before participating in the survey 41% of respondents had heard about the Near Me service; 59% stating they had not and 13% had prior experience of a Near Me appointment.
Three out of four participants used a range of devices for social reasons or work with the most popular being Facetime (66%), WhatsApp (66%) and Facebook Messenger (57%) and they also had access to a video calling device, like a smartphone, tablet or computer (74%). Around two in three stated that they were confident using video calls (Figure 14).
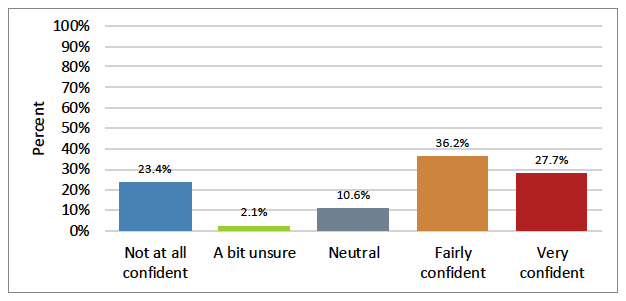
Figure description:
Not at all confident (23%), a bit unsure (2%), neutral (11%), confident, (36%) and very confident (28%).
Respondents had heard about the public engagement through a range of means (Table).
| Awareness of public engagement | Percent |
|---|---|
| Local media (newspaper, radio, TV) | 2% |
| National media (newspaper, radio, TV) | 4% |
| Social Media (Facebook/Twitter) | 13% |
| Website (e.g., Scottish Government, NHS board, third sector) | 26% |
| Community Council or local group | 0.0% |
| Elected representative | 0.0% |
| Word of mouth | 11% |
| I do not know | 0.0% |
| Other | 78% |
| Total number of responses | 47 |
3.3.3 Preferences
Reflecting on video consulting, 81% thought it should be offered for health and care appointments. During Covid-19, telephone (92%) was preferred over video (72%) with 19% selecting face to face. For all three appointments types, order of preference did not change once physical distancing is over but more people would prefer face to face (60%) with a corresponding reduction in telephone (79%) and video (62%) (Figure 15).
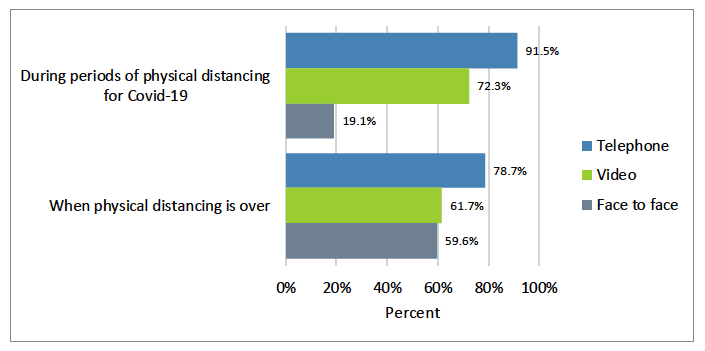
Figure description:
People who completed the survey over the phone or by hard copy were asked to consider their preferences around three types of appointments: face to face, telephone and video consultation.
During physical distancing, telephone (92%), video (72%) and face to face (19%). Once there are no restrictions due to physical distancing phone (78%), video (62%) and face to face (60%).
3.3.4 Benefits and barriers
Benefits of using Near Me that scored the highest were lower infection risk (4.7), better for the environment (4.5) and improved access to services (4.4). The potential benefit which scored lowest was 'easier to have a relative / carer to support their appointment' (2.9) (Figure 16).
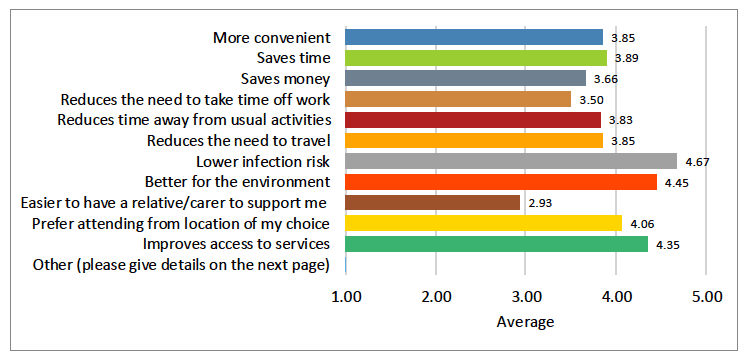
Figure description:
Responders were asked to rate the importance of several potential benefits to them on a scale of 1 to 5, where 5 is most beneficial. The top four benefits of using video were: it lowers infection risk (4.7), better for the environment (4.5) and improves access to services (4.4).
A range of free text comments were captured reflecting the self-reported benefits. Sentiment analysis has not yet been carried out, but the following are considered reflective of the tone and content of feedback.
"I would fully support being offered video consulting. I would be delighted to be able to use video consultations for all my appointments. Living in a small village in a rural setting can prove tricky in bad weather and appointments to hospital or GP has to be cancelled."
"I have not used it so far but think it would be a great advantage all round."
"I think video consultations is a fantastic way of working in the future. saves so much money in fuel, parking, stress levels will improve also."
When selecting disadvantages (barriers), the need for support (2.4) and internet connectivity (2.4) were the highest scoring barriers with the others more evenly spread (Figure 17).

Figure description:
Responders were asked to rate the barriers on a scale of 1 to 5 where 5 poses the biggest barrier: poor internet connectivity (2.4), cost of mobile data (2.4), and do not like video calls (2.4).
A notable difference from the online survey was 'private space for a call', which 70% (cf. 33%) considered to be 'not at all significant' (Figure 18).

Figure description:
70% thought having no private space for a call was not at all significant, 2% not that significant, 2% a little significant, 0% very significant and 24% not relevant.
This point reflects the wider feedback that the facilitator reported following the phone interviews (N = 40).
"I found when making calls I ended up signposting many people to other organisations such as "Silver Line", "Age Scotland", Mental Health organisations offering support by telephone. It was very apparent that loneliness and isolation was playing a big part in peoples' lives especially with the Covid-19 lockdown and "shielding" that was imposed." Evidently, for these individuals they had privacy to make a call should that be desirable but the more concerning issue for some was more of loneliness and isolation.
Quotes which typically illustrated the barriers included:
"No interest in social media or technology. Prefer face to face appointments at hospital or doctor's surgery."
"I do not have any inclination to start using internet at my age. I much prefer face to face contact with my doctor or nurse either at surgery or in my home."
"I have severe anxiety issues and a physical disability. I prefer to see my doctors and mental health workers in person. I do not own any smart phones or devices for internet, landline only."
Frequently participants described both benefits and barriers and highlighted the importance of having options such as:
"You cannot have a proper conversation over the internet about personal matters, specifically when it would require an examination. Its ok for certain circumstances, however these can change, and it would be good to have the option of a face to face consultation."
3.4 Findings from qualitative analysis (public, non-survey)
3.4.1 Individual written responses
Sixteen people who provided individual responses are documented (Table 6). The feedback was based on a combination of personal experience and / or general comments and perceptions.
All responses received were given personal reply in as close to real time as possible to address any specific queries raised and to thank the responders for their participation. The approach taken was to explain the process not 'sell' the Near Me service. Sometimes opinions and tone changed during the correspondence, however, for the purposes of this exercise the original feedback received is what has been documented.
Six of the responses highlighted both benefits and barriers; six noted only benefits and two only barriers. There were three 'neutral' responses relating to requests for further information.
Four case studies from the individual submissions were selected to reflect the range of views expressed.
Case Study No. 1 highlights a range of benefits alongside concerns and was submitted by a mum on behalf of her family including her daughter who has Chronic Kidney Disease (CKD), late stage 3b. It illustrates the complexity of care, balancing work with family life and how having choice and flexibility impacts positively on quality of life.
Case Study No. 2 is an example of the service being very person-centered and for a family living in a very remote part of highland offering many benefits including safe, convenient, cost-effective care with wider benefits linked to environmental and general wellbeing.
Case Study No. 3 was submitted by a daughter on behalf of her mum who does not have a computer and calling for a fair system.
Case Study No. 4 has been included as it sets out the wider range of issues reflecting health, wellbeing, and loneliness. It was submitted from a retired NHS chaplain who concluded:
"My final comment is that near me needs to develop alongside encouraging and enabling community/local care. Such as training people in Mental Health First Aid, encouraging basic listening skills, having 'pop us sessions' in community centres, church halls etc with information about health issues, how to look after yourself, importance of looking out for others.
Health is a community issue as well as about individuals. Video has so many benefits in helping individuals with specific health issues - but much less beneficial to community well-being."
While it is an individual view it offers a broader perspective seldom raised throughout the Near Me's development and therefore the authors feel worthy of inclusion to broaden the conversation. It illustrates, with examples, the deliberations around the merits or otherwise of having an appointment at home.
| Category | Board | Date | Sentiment analysis | Main themes | ||
|---|---|---|---|---|---|---|
| Benefits | Neutral | Barriers | ||||
| 1. Family | Unknown | 05/08/20 | √ | √ | Range of views reflecting benefits and concerns. Case study No. 1 | |
| 2. Member of Public | Tayside | 01/07/20 | √ | √ | "I think this is great, easy to use, instructions simple" "People in poverty, very elderly or people with sensory deficit might not be able to access." | |
| 3. Member of public | Ayrshire & Arran | 07/07/20 | √ | Requested further information; had not heard of Near Me | ||
| 4. Member of public | Tayside | 07/07/20 | √ | Requested hard copy of survey | ||
| 5. Member of public | Lothian | 09/07/20 | √ | "Excluding people who have no access to the internet (poverty, mental health, age, disability and lack of digital capacity etc)" | ||
| 6. Member of public | Unknown | 22/07/20 | √ | √ | √ | "I have no problem with this format of communication for those who are happy to use it. I just need to know that choice will be available." |
| 7. Member of Public | Forth Valley | 29/07/20 | √ | √ | "Useful in remote areas but not urban." | |
| 8. Member of public | Unknown | 02/08/20 | √ | √ | "A video doesn't give proper vision." OK for yearly check-ups. Not supportive for clinical scenarios and digital exclusion. | |
| 9. Member of public | Highland | August | √ | "Please continue expanding this service" Case study No. 2 | ||
| 10. Member of public | Lothian | August | √ | "I can see huge benefits in what is being proposed" | ||
| 11. Relative | Unknown | 27/07/20 | √ | "Need a system in place for people who do not have computers. We need a fair system for everybody." Case study No. 3 | ||
| 12. Retired NHS | Unknown | 23/07/20 | √ | √ | Range of views benefits and concerns. Case study No.4 | |
| 13. Service user | Forth V | 15/07/20 | √ | "Very successful and saved me an hour drive each way." | ||
| 14. Service User | Unknown | 05/08/20 | √ | "Great idea and much easier than attending in person." | ||
| 15. Service User | Lothian | 22/07/20 | √ | "I like this service." | ||
| 16. Service user | Tayside | 01/02/20 | √ | "I think this is a good alternative if the patient choses to - or if his/her symptoms could jeopardise the health of administrative or medical staff. | ||
| Total | 12 | 3 | 8 | |||
Case Study No. 1 Balancing complex health care with work and family life
"I am an NHS worker and mum to a daughter who has Chronic Kidney Disease (CKD), late stage 3b. I can see the positives and some negatives of Near Me from both aspects.
This service has no doubt been a positive addition for our family and a service that I hope can continue. Although it may be beneficial to have a combination of video and face to face appointments. There are times when patients and families still need to keep physical and face to face contact, especially when there are physical elements of an illness that need managed.
Face to face helps to maintain relationships with staff and familiarisation with the clinical environment which can often be an unfamiliar and frightening place for children. It is important for children with lifelong chronic conditions that can deteriorate over time and may require more frequent admissions, to be familiar with the hospital and its staff.
The Near Me service has provided many positives for our family and the main one being spending less time in the hospital. As parents to three school age children, a hospital appointment for my daughter has often meant arranging childcare for her siblings. Sometimes this is done on the day as appointments can run late. This can be stressful especially if we struggle to find someone and unsettling for my other children. When school returns, if Near Me is not available, we will have to juggle care again with covid restrictions in place for childcare.
My daughter through her illness and covid shielding has missed a lot of school. When appointments are in hospital this means a half to almost whole day out from school, usually due to travel there/back and waiting times in hospital. Now more than ever being able to stay in school is especially important to my daughter and us. VC appointments allow her to be in school for most of that day and with her peers.
Having Near Me has meant that my husband has been able to attend VC appointments without the stress of rearranging his working day and sometimes on the day. We have been able to feel more relaxed having these appointments at home."
Case Study No. 2 Remote and Rural
"We live in a remote rural area and have used Near me in our local surgery before the coronavirus lockdown. It saves us so much time and hassle as we do not need to travel to Inverness for every appointment (80 miles and 2 hours each way), but still have the 'face-to-face' experience. Many of our appointments are mainly talking and we can see the benefits for us and, also the hospital from removing the need to travel for every appointment. In addition, we would normally claim travel expenses for a hospital visit which is no longer needed, saving the NHS money.
If we have to wait for an appointment when the surgery is running late, this would be much nicer to do in our home rather than in a hospital waiting room with anxiety about our return journey and our dogs sitting outside in the carpark.
Of course, Lockdown has changed everything, and now it is also safer to have video and telephone consultations. The reduction in travel is also good for the environment and indirectly all our wellbeing
Where actual face to face appointments are not needed, this is such a great facility to be able to use. Please continue expanding the service with our blessing."
Case Study No. 3 We need a fair system for everybody
"I am emailing on behalf of my mum who does not have a computer.
My mum is 80 and is not interested in technology. My mum would not like video consultations even if she did have a computer.
So, what my mum wants to know is what happens to patients like her?
My mum has had cancer 3 times. She recently was diagnosed with bowel cancer in 2013 and stomach cancer in 2015. She is still under review at RIE but considering this seems to be the way forward "Near me" what happens to patients that do not have a computer?
My mum is a retired Nurse and worries patients like her and at her age are going to be forgotten about / missed out the system!
Going forward there clearly needs a system in place for people who do not have computers; people who are not comfortable having appointments via video.
We need a fair system for everybody."
Case study No 4 Health, wellbeing, and loneliness
1) The benefits of having a place to come to - as some form of 'health and social care hub' - where people could drop in to find information, whether by picking up leaflets, reading posters etc, or speaking informally with staff on the premises. Where this 'hub' is also where GP and nurse appointments, conversations with community nurse, community listener, counsellor etc take place. And possibly also meetings of various 'self-help' groups
If the focus of health care becomes video-linking, then the huge potential of such places will be lost
2) For the health professionals, appointments by video reduce the potential for them to be able to diagnose accurately through observing non-verbal communication - such as sitting position in waiting room, enthusiasm/reluctance when name called for appointment, restless movements of legs while talking etc For people who are used to communicating, and who are clear exactly what issue they want to discuss - video is fine.
3) I see as very helpful all the benefits of video such as no need to travel, takes less time, and so on. Which for people with a clear and specific issue are important and helpful. But I am so aware also that in my work with many people, it was really important that (even though I could do this within my job description and did so where appropriate) I did not normally make home visits. Because to make the effort to get up and dressed, and out, was such an important part of the health care of the people I was working with. Their visit out to help was a part of the helping process. And for those isolated at home/unemployed etc - their appointment was seen by some more as a 'special day out'. For these people, they would require only to get out of bed for the video time - not healthy for them.
4) For many people, especially those with learning disabilities for whom clear boundaries and patterns are so important, having doctor or nurse on screen in their home space can be confusing, disorientating and so on.
5) Sadly, for many people, meeting with a health professional is the only caring relationship that they have. While always working to encourage such people to develop other 'equal friend' type relationships and discouraging such dependence (good for neither patient nor health professional) it remains reality. So, to take that actual meeting in person experience away from them by meeting on video will not be good for their health
There are undoubtedly huge benefits in video/tele communication. And in rural areas where this enables consultations that could not happen at all without it - it is especially important to develop. But the personal contact that will be lost as a result; and the loss of easy access to information etc that will not happen if it is widely rolled out are a huge concern.
3.4.2 Written responses from organisations
From over 300 organisations contacted directly by the Near Me team, written responses (N=38) were received during the period from 1st July through until 18th August (Table 7). There was a diverse range of organisations who responded both from local (community councils) and national (Deaf Scotland, Mental Welfare Commission, RSPB Scotland) organisations; geographical spread, as well as organisations representing people with different health and care needs such as cancer, carers, inequalities, homeless, mental health, pensioners and end of life care.
As with the individual responses a range of benefits and barriers were highlighted and in a small number of responses varied quite markedly in strength of feeling from "We very much welcome the rapid scale up of the use of Near Me" to raising equality concerns and discrimination. Dundee Cancer Support Network response summed it up the balance of general views reflecting benefits and barriers.
"Benefits for all who can access. "Those in poverty, very elderly or people with sensory deficits might not be able to access."
The Lay Advisory Committee of Royal College of Physicians of Edinburgh comments included:
"Video consulting should continue to be offered after physical distancing is over, but it is not universally appropriate. It should therefore be an option rather than mandatory."
Taking an overview of these responses two further case studies were selected.
Case study No. 5 was submitted from Affa Sair a self-help group for chronic pain sufferers in North East of Scotland. Chronic pain has recently been in the headlines due to some services being paused near the start of the coronavirus pandemic. It has been reported that many patients turned to private treatment, travelling to England for help during lockdown. The response from Affa Sair does not refer to this at all but rather highlight the benefits in using Near Me including improving experience by reducing travel. Their insights would not be obvious to most people unless they had experience of living with chronic pain.
The submission from Dundee Pensioners' Forum (Case study No, 6) captures the challenges about carrying out public engagement during time of physically distancing and their concerns if choice is not offered for older people particularly for those who are not online.
| Name | National/Local | Date | Type | Sentiment analysis | Comments | ||
|---|---|---|---|---|---|---|---|
| Benefits | Neutral | Barriers | |||||
| 1. Affa Sair self-help for chronic pain sufferers | Local | 06/07/20 | e-letter | √ | "We very much welcome the rapid scale up of the use of Near Me." Case study No.5 | ||
| 2. Carers Trust Scotland | National | 07/07/20 | √ | "The Scottish Youth Parliament believes that optional video services …. for a GP appointment should be used for the future." | |||
| 3. Carers, Lothian | Local | 13/08/20 | virtual | √ | √ | "Systems need to be flexible and not 'one size fits all' to meet individual's needs. | |
| 4. Clackmannanshire Health and Social Care Partnership | Local | 15/07/20 | virtual | √ | Keen to explore how it might be used in social care. | ||
| 5. Community Council, in Ayrshire area | Local | 02/08/20 | √ | √ | "Would like to express support for vide consultations, not just during the current situation but as an ongoing change withing A&A." | ||
| 6. Community Council, in Falkirk area | Local | 27/07/20 | √ | "We can see a place for this type of technology" | |||
| 7. Community Council, in Stirling area | Local | 13/07/20 | √ | General enquiry noting poor internet connections. | |||
| 8. Deaf Scotland | National | 01/07/20 | Media Release | √ | "Near Me has provided a vital lifeline to health services and we would welcome its continued use when the current crisis ends." | ||
| 9. Dundee Cancer Support Network | Local | 01/07/20 | √ | √ | Benefits for all who can access. "Those in poverty, very elderly or people with sensory deficits might not be able to access." | ||
| 10. Dundee Pensioners Forum | Local | 04/07/20 | √ | Digital exclusion. Case Study No.6 | |||
| 11. Dundee Volunteer and Voluntary Action | Local | June/July | various | √ | General supportive comments. | ||
| 12. Education Scotland | National | 24/07 | √ | Collaborative working between education and health with Near Me. | |||
| 13. Equalities Organisation | National | July | emails | √ | Raising equality concerns and discrimination. | ||
| 14. Frontline Fife | Local | 03/07 | emails | √ | √ | Keen to promote clients living across rural populations and those that often lack the means to attend services. | |
| 15. Genetic Alliance | National | 23/07/20 | Report | √ | Covid-19 Impact Report stating 9 out of 10 people who received an online consultation rated the experience as positive. | ||
| 16. Greater Glasgow and Clyde | Local | 05/08/20 | Report | √ | √ | Report including telephone interviews to determine views of people whose first language is not English | |
| 17. Hospices in Scotland | National | 03/08/20 | Report | √ | √ | Feedback from hospices in Scotland around the use of virtual consultations, | |
| 18. Hub North Scotland | Regional | 07/07/20 | √ | "Looking forward to this type of technology playing a big part in future Hub North Projects." | |||
| 19. Lay Advisory Committee | National | 23/07/20 | √ | √ | "Video consulting should continue to be offered after physical distancing is over, but it is not universally appropriate. It should therefore be an option rather than mandatory." | ||
| 20. Marie Curie | National | 04/08/20 | Report | √ | √ | Eight focus groups with 37 participants, | |
| 21. Mental Health Advocacy | Local | 09/07/20 | emails | √ | √ | "The most distressing aspect for many people is that they have no safe, secure and private internet access at all." | |
| 22. Mental Welfare Commission for Scotland | National | 03/07/20 | √ | "Have not implemented Near Me yet but will be doing so." | |||
| 23. National Carer Organisations | National | 13/08/20 | letter | √ | √ | √ | Various examples and suggestions "ensure this continues to be a 'people' project rather than a technology project", |
| 24. NHS Grampian Interpreting Services | Local | 23/07/20 | Report | √ | √ | Incorporate as part of EQIA | |
| 25. NHS NSS | National | 07/07/20 | emails | √ | Discussion on net zero definition and measuring carbon reduction due to reduced travel | ||
| 26. North Ayrshire Health and Social Care Partnership | Local | 22/07/20 | Report | √ | √ | "Near Me is more than adequate for one to one consultation, with easy to use functions and secure conversations." | |
| 27. Outside the Box | National | 06/07/20 | √ | √ | "This could bring huge benefits, but people are also likely to face barriers (older people living in rural areas with poor broadband, people with no digital access or limited privacy etc" | ||
| 28. Parkinson's UK | National | August | √ | √ | Feedback mixed | ||
| 29. People First | National | August | Report | √ | √ | More barriers than benefits | |
| 30. Petal Support LTD | National | 02/08/20 | √ | "We will have a look at Near Me video consulting and get back to you if we feel we can use this system." | |||
| 31. Phillips UK | National | 13/07/20 | √ | Inquiry about how they could provide evidence as part of public engagement | |||
| 32. Realistic Medicine | National | August | Email and meeting | √ | Request to use Near Me platform to promote the principle of Realistic Medicine and Shared Decision Making amongst patients? | ||
| 33. Renfrewshire Health and Social Care Partnership | Local | August | Report | √ | √ | √ | Report based on feedback from 29 GP Practices local CQLs/PQLs, section xx of Report. |
| 34. RSPB Scotland | National | August | √ | "We can see huge benefits in what is being proposed. It is great to see the links between health and the environment are being recognised more widely." | |||
| 35. Stirling Council | Local | 15/07/20 | Phone | √ | Progressing work on connectivity in rural areas and how it might support roll out of Near Me | ||
| 36. University of the Highlands and Islands | Local | Emails | Various, including clinical use, connectivity, engagement and teaching. | ||||
| 37. Waverly Care | National | 23/07/20 | Report | √ | √ | "Services are most accessible when people have a range of different access options." | |
| 38. Yellow Card Centre Scotland | National | July | √ | Request to use the virtual 'waiting room' as a platform for promoting the Yellow Card Scheme. | |||
Case Study No. 5 Affa Sair Chronic Pain
"We were very interested to receive your email on the launch of the public engagement survey on the vision for Near Me.
Being able to easily obtain meaningful access to healthcare has long been a source of great difficulty for chronic pain sufferers in Scotland. Unlike most of the populace, chronic pain sufferers have great difficulty in attending appointments at Health Centres and Hospitals. For some, the simple act of having to sit on a hard seat in an overcrowded waiting area can be very painful and traumatic. Fibromyalgia and other similar conditions can be made worse by the usually acceptable noises in public waiting areas such as loud tannoy announcements, children playing crying or screaming, and adults engaged in loud conversations.
Getting to the buildings can be an insurmountable task when the patient is in constant intractable pain, unable to drive or travel by public transport and even to leave their house due to cold and stormy weather - a frequent occurrence in Scotland. In rural areas of the country, a visit to the hospital or care facility can involve return journeys of hundreds of miles which take days of recovery for some. Some chronic pain patients literally feel every bump in the road. Understandably, many non-clinical staff in the Health Service, find these reasons difficult to conceive and many frustrating interactions take place between staff and patients.
We very much welcome the rapid scale up of the use of "Near Me" video consultations and ask that Health Boards fully take up the Scottish Government's initiative and make "Near Me" consultations a normal method of patient care.
Affa Sair will be pleased to encourage our growing number of members to ask their Health Professionals, Doctors and Consultants to make Near Me the first option when arranging consultations with chronic pain sufferers."
Case Study No. 6 Dundee Pensioners' Forum
"It worries us greatly that once again, a consultation is put out that will directly affect the lives of many, many older people - and they do not really have access to it. Older people's voices must be heard in this discussion and it behoves those in authority to make sure they are.
Over 40% of older people are not on-line and, from what I've read so far, users will need a computer/laptop/iPad or smartphone with a webcam and Windows 7 or better, and the latest versions of Chrome or Safari - a reliable internet connection and, a private area in their home from which to take part in the discussion with the health care provider.
That is a big ask for many older people - and indeed disabled people and those on restricted budgets. It is a common misconception that all younger people are on-line. There is poverty in every community and £20 or more each month for a broadband connection is not possible for everyone. Many older people will need support to use the technology - what about confidentiality issues in this situation?
We appreciate how vital video consultations have been during this pandemic. There are, of course, situations where access to services because of distance (i.e. in the Highlands) makes video consultations very useful. But there is a difference between necessary and desirable. People prefer human contact - especially older people - for many a visit to the GP or a hospital appointment will be the only time they step outside the door. Health professionals can tell so much more about the general wellbeing of a person through direct face to face contact, and the opportunities this allows to observe body language, etc. It would be such a shame if we were to go too far down the virtual road.
In terms of social care, I just cannot imagine how this can be done virtually. A huge part of social care is the human interaction that takes place. If that disappears, social isolation with all its associated health and wellbeing detriments will spiral.
For Dundee Pensioners' Forum, this should be about choice. What worries us is that the perceived advantages of virtual consultations (efficiency and financial savings) will take precedence over what is really best for people and for the services that they need."
3.5 Service user feedback facilitated from organisations
Due to the differing way the feedback was collected or presented they do not all follow the same format. Benefits and barriers were coded and included as part of the wider analysis Appendix 4.
Any suggestions raised are highlighted (Appendix 5) alongside any comments specifically relating to technical issues/digital exclusion (Appendix 6). The full responses will be shared with the University of Oxford team.
3.5.1 Carers organisations and carers
Carers can and do play a key role in supporting medical appointments with a range of health professionals for the cared for person. The ability to join (as a third party) any remote appointment to: (i) potentially advocate or support the cared for, particularly in relation to individuals with a learning disability or who lack capacity; (ii) provide language or communication support for non-English speakers or individuals with additional communication needs; and, (iii) enhance information sharing which is necessary in the care and treatment of the cared for person, is of mutual benefit to all parties. Video consultation would also be extremely beneficial for working carers (where appointments take place for the cared for during working hours) and for carers who provide support from a geographic distance.
- Individual feedback
The following feedback was received from carers who had used 'Near Me' and was included as part of National Carers Organisations submission with the aim of providing examples of three individual experiences:
"I had a video consultation and had to show a lump on my chest. I was told it was a simple cyst and would have to live with it. When I called back the following week to say it was bleeding, I was not offered another appointment and surgery just reiterated what I had already been told. When services resumed and hospital/consultant saw it, it was not a cyst and I needed surgery. Definitely a shortcoming of the system when you have something that needs to be seen in person."
"I had a video consultation, but it was difficult with my daughter. She would just walk out the room and close the laptop because she didn't want to speak.' (parent of child with autism)."
"I found the video consultant really good. There was very little to no waiting time. The letter was very clear in its instructions and it was very easy to set up. The audio was very clear, and the picture was good quality. The only issue was the last 5 minutes the video froze. The doctor's internet was not as good as mine but the audio was still clear so he could still hear me and vice-versa. Overall, I found it to be a good experience although I don't know how I would have felt if I was having to show them something instead of just a conversation."
- Governance
"We strongly believe that the governance of the project should include both carer and patient representatives to ensure that the project 'is' and continues to be a 'people' project rather than a technology project."
West Lothian Carers
Four of the five carers were aware of the service. Two carers said the person they care for had used it for a GP appointment and found it a good experience and they would use it again. Everyone felt video link as an option is a good idea and shows the service is moving with the times. The five carers participating felt there was definitely scope to continue using this system going forward with video their first choice during and post Covid-19.
What might make accessing your care easier or better?
"Systems need to be flexible and not 'one size fits all' to meet individual's needs. A mix of video, face to face and telephone and so patients can choose what works for them."
3.5.2 Genetic Alliance UK
One of the recommendations from the Genetic Alliance UK 'Covid19 Impact Report' related to the provision of remote consultations should be continued.
"Care should be taken to integrate telemedicine into routine care practice with the necessary clinical assurance and data protection safeguards."
3.5.3 Hospices in Scotland
Hospices introduced a range of virtual services during the pandemic including supporting patients at home through Near Me.
The virtual hospice offers families nursing, medical and pharmacy advice by phone and video; bereavement support; money and benefits advice; practical advice around coronavirus; and activities for families.
Virtual outpatient and day service sessions are accessible by a much wider audience and are particularly useful to those who physically would not have been able to attend Outpatient groups previously.
General comments
- Positive feedback from patients and families
- Supports choice
- Successful model and looks likely to be an ongoing model of delivery
- Digital champions introduced with a lead role in ensuring all staff and clients have appropriate knowledge and access to allow them to engage in the services
3.5.4 Marie Curie Scotland
Marie Curie is in the early stages of research to understand the effect of digital consultations on health and social care teams, patients, and their families. Their initial data highlighted a significant shift from face-to-face consultations to telephone, but a slower uptake of video consultations. The types of consultations being supported through video:
- Outpatients
- Inpatient/family contact to discuss patient care facilitated by clinicians
- Day therapies
- Initial assessments
- Attempted to provide bereavement support but was unable to do so through poor digital connection
Their early findings indicate that telephone consultations were the preferred option throughout the pandemic. They believe this may be due to patients not having the appropriate technology to facilitate video consultations at home; nervousness about the ease of using video consultations or feeling uncomfortable on camera.
Future role of video consultations
- A patient being able to attend virtual day therapies if they were in hospital or not feeling well enough attend hospice
- Family living long distances away being able to be present for consultations or being able to speak to their relative
- A pilot loan tablet scheme is being developed at their hospice in Glasgow, which will loan tablets to people in some deprived local areas who may not have access to technology or be able to attend appointments in person.
- In their submission Marie Curie included several case studies, one of which is included below (Case study No. 7).
Case Study No. 7 Marie Curie Hospice Glasgow Case Study
An outpatient with a terminal lung condition who had been attending appointments at hospice with a member of their family had initially transitioned to video consultations when outpatient services were suspended. The family was able to help set-up the video consultation process at home and be present to help communicate the full extent of the patient's symptoms as the patient was reluctant to share these on occasion.
Once shielding regulations were enforced, however, the patient was not permitted any visitors at home and reverted to telephone appointments with hospice clinicians. The clinician advised to the best of their ability but did not have the complete picture of the patient's health which would normally be visible either on screen or in person.
3.5.5 NHS Grampian
A range of experiences and feedback was provided from NHS Grampian's interpreting services with ideas for improvements. These will feed into version 2.0 of EQIA. Overall, when there were no glitches with the technology the service was felt to be a benefit for clinician, patient, and interpreter.
"It was a very pleasant experience. I would love to use it again. It saves the travel time, can be accessed anywhere. Particularly at the lockdown period it reduces the infection risk. I would be happy for it to be continued even after the lockdown is released. Overall, it is a good idea to have the Near Me video consulting." - Foreign Language Interpreter.
Challenges raised were mostly related to technical issues, connectivity or user having problems to set up the video.
3.5.6 NHS Greater Glasgow and Clyde NHS GGC)
Various approaches to facilitating feedback was carried out by NHSGGC. Of the eight interviewees whose first language was not English none had heard of "Near Me" video service for health and care so none of the feedback was based on first-hand experience.
Whilst most of the interviewees could see benefits to video appointments (time and travel saving) most were also concerned that their circumstances were not really suited due to the complexity of their health conditions or communication issues.
Although willing to use phone or video appointments during the pandemic and its associated distancing etc., most said they would prefer to return to face to face appointments afterward. This sat alongside a feeling that all types of appointment should be available.
This was followed up with some further work with 22 respondents. The feedback given by all interviewees regarding "Near Me" is largely positive. Over-all it is a good system although some people experienced technical difficulties and/or required support of differing types to use it. This positivity does not represent the whole picture with some barriers described:
- Due to the nature of a person's disability or condition "Near Me" may never be a good appointment option
- Not everyone is digitally connected/aware or is able to be
- Some people are happy to use the system for now (during the Covid-19) restrictions but see it as purely temporary
In the conclusion of the report it was highlighted that that one size does not fit all and was well expressed by one interviewee:
"I think it is great that this service is available if someone wants to use it, as I said it can mean that you don't need to travel all the way to the hospital unnecessarily. However, I really feel that the issue of choice is an important one. If it is imposed, then you would not get the positive care result".
Further information on methodology and feedback is available in a full report submitted to the Near Me team and the methodology described in Appendix 3.
3.5.7 North Ayrshire Health and Social Care Partnership
Having conducted several tests with Near Me, all one to one consultation was carried out successfully, with only minor issues, such as internet connectivity. There was widespread agreement that Near Me was more than adequate for one to one consultation, with easy to use functions and secure conversations. However, significant further development would be required to bring it up to the standards of other platforms when holding group conversations.[12]
3.5.8 Parkinson's UK Scotland
Feedback was received via Parkinson's UK through various routes including the short survey. Generally, most were happy with Near Me or telephone appointments and would choose this as a first preference both during Covid-19 and afterwards. The main barriers identified were for those who do not have the equipment or skills to use Near Me. Comments included:
"For some people not having the right technology or not being able to use the technology. Also, if they don't have a private space at home to undertake the appointment."
Feedback received via Facebook included:
"I had a video call with my Parkinson's consultant, first time 'seeing' each other. I was diagnosed in December 2019, call was early July, she adjusted my medication. I think it went well all things considered. Although I will be happier to have a face to face in the future."
"I had a telephone consultation recently with my PD consultant - postponed from April - and it went very well; having said that, I had nothing of note to report on, however, and I've been quite stable for some time now."
"I have had both my appointments with my neurologist cancelled and no new appointment in place also no contact from my Parkinson's nurse to let me know of a new appointment
"Telephone consultation totally inappropriate for my Husband with Parkinson's."
"Are video calls available with every NHS hospital? My husband's Parkinson's nurse refused to do a video call instead of his six month appointment. Just cancelled his appointment. She claims the facility is not available at our large NHS hospital. Gave him an appointment for December which means no Parkinson's professional will have seen or spoken to him in over a year."
It needs to be borne in mind that this feedback is from people already using a computer / smart phone and the internet. For some the main problem seems to have been having their appointment cancelled and not getting any sort of replacement. [13]
3.5.9 People First (Scotland) and Scottish Commission for Learning Disability [SCLD]
Across all the feedback overall awareness of Near Me was low but in common with other groups there was a wide range of views. Feedback also appeared to vary based on how it was collected. Some of the generic feedback facilitated by People First (Scotland) across several areas had significantly more emphasis on the barriers.
"There is digital exclusion for any citizen with a learning disability or intellectual impairment in one shape or form" adding that "digital exclusion can be due to where and what type of setting people live in; what if any social care or other support they receive and their income, which is almost universally low and benefit based."
They went onto list the whole gamut of digital exclusion leaving People First (Scotland) worrying that use of technology, such as for Near Me, would widen inequalities.
Overall there was a preference for face to face from many members with a small number open to the idea such as psychology appointments, reducing travel and spread of infection was seen as positive for those that could access video consultations.
On the other hand, feedback from other participants, individuals and small groups highlighted a wide range of potential benefits. Several commented on the convenience and 'comfort' of their own home. Another theme was around not having the stress and worry of getting to and around hospital.
"It makes me less anxious because I amin the comfort of my own home - there's not the worry of finding where you are going in big maze like hospitals, and if I am having a bad day I can be in my room sitting comfy in bed."
Wider comments both in terms of benefits and barriers chimed with feedback described by through public survey with again privacy and lack of space being raised. Some described that they were worried that video would just 'cut out' after a certain length of time and another wondered would you get a longer appointment by video.
The feedback facilitated over the phone and on Zoom was also variable. The two groups on the Zoom had a completely different appetite for use of Near Me. While some could see benefits and thought it better than the phone whereas the second group were not supportive but also described general challenges of accessing services in whatever way. There were some concerns expressed around safety and whether people had capacity to use it.
3.5.10 Renfrewshire Health & Social Care Partnership (HSCP)
"As an HSCP we will continue to monitor progress on a regular basis and feedback any themes and issues."
Based on experience to date, from the patient's perspective, they quite like it when it works and saves them time coming into the surgery and waiting, and so easier for work/childcare. It is also safer at times of higher risk in the pandemic. On the other hand the level of technology patients typically have is another rate limiting factor.
3.5.11 Royal College of Physicians Edinburgh, Lay Advisory Committee
The group reported that they had very little prior awareness of Near Me until the consultation and none of their committee had experienced an appointment. All used Facetime, Zoom, Skype, Webex or MS Teams for other purposes and all had access to a smartphone, tablet, or computer with webcam.
There overarching conclusion was "Video consulting should continue to be offered after physical distancing is over, but it is not universally appropriate. It should therefore be an option rather than mandatory."
3.5.12 Waverly Care
In the experience of Waverley Care, sexual health and Blood Borne Viruses (BBV) services are most accessible when people have a range of different access options. For some people, face-to-face services are essential to ensure equitable access to care. For example, some services for people who inject rely almost exclusively on face-to-face outreach to consistently engage people with sexual health and BBV services.
"We would therefore strongly advise that Near Me consultations be offered alongside, rather than as a replacement for, face-to-face consultations." This is further explored below.
- Setting
Participants in recent research on trans people's access to sexual health services told Wavery Care that the environment in sexual health clinics could present a barrier to access. Participants described the environment as very clean, white, clinical, noting that there was often a lot of noise and activity. Some participants said that they would prefer to access services in a more relaxed and quieter environment. Video consulting would mean that people could access services within the comfort of their home, or another location where they felt comfortable. In doing so it could help to address privacy concerns. This is particularly relevant to sexual health and BBV services, because of the stigmatised and sensitive nature of these services.
- Choice
In recent consultation and research work, the people we work with have emphasised the importance of being able to access sexual health and BBV services in a range of different ways, so that they can choose the option that is right for them and their personal circumstances. If video consulting helped to increase capacity and flexibility within services, this would help to increase choice.
- Safety and privacy at home
There should be consideration given to whether people can safely and privately access video consultations at home. Home is not always a safe place for many people, particularly to discuss sexual health or another sensitive health issue. For example, some of the gay and bisexual men we work with are not open about their sexual orientation with their families or the people they live with. We support some men who are in heterosexual relationships or marriages, but also have sex with men.
Likewise, we support some women who would be at risk of gender-based violence if their partners were aware, they were accessing sexual health or BBV services. Many of the people we work with have not disclosed their HIV status to anyone other than healthcare providers.
It would therefore be important to ensure that there are local, safe spaces where people could access Near Me consultations if it were not an option to do this at home. To protect privacy, it may be helpful if this could take place in a generic health setting (e.g. GP or dental surgery), so that the person would have an 'excuse' to be attending an appointment.
- Equality of access
Levels of digital literacy and access to digital devices should be taken into consideration. Levels of poverty and deprivation influence this, as well.
Contact
Email: NSS.TEC@nhs.net