NHSScotland Chief Executive's Annual Report 2014/15
The NHSScotland Chief Executive's Annual Report 2014/15 presents an assessment of the performance of NHSScotland in 2013/14 and describes key achievements and outcomes.
Chapter 5: Securing Value and Financial Sustainability
Health policy is focused on the delivery of improved quality and safer patient care while ensuring that the service is sustainable and delivers value for the public purse.
Anne
To see Anne’s story see the online report at www.nhsscotannualreport.scot
FINANCIAL OVERVIEW
Health had an overall resource and capital budget of £12.0 billion in 2014/15 and spent in full the cash available for services and infrastructure. There was an underspend of less than 0.1 per cent of the budget relating entirely to non-cash budgets such as depreciation and asset impairments that therefore could not have been spent on services.[125] All of the money available was used to provide services and invest in health infrastructure across Scotland. This underlines the sound financial stewardship of NHS Boards and the Scottish Government Health and Social Care Directorates.
As in each year since 2010/11, the NHS frontline resource budget has been protected. The 14 Territorial NHS Boards received above-inflation baseline resource increases of 3.1 per cent in 2014/15.[126] Owing to the contributions of all those involved in the running of the NHS, all NHS Boards met their financial targets in 2014/15 and remained within budget for the seventh year in a row.
The health resource budget has increased by £409 million in 2015/16, taking spending to a record level. Resources allocated to Territorial NHS Boards have increased by 3.8 per cent,[127] an above-inflation increase that has ensured all Territorial NHS Boards have received above-inflation increases in each year since 2010/11.
How the Budget was Spent
The Scottish Government allocated £10.1 billion directly to the 14 Territorial NHS Boards. The seven Special NHS Boards and Healthcare Improvement Scotland received £1.3 billion, and the remaining £0.6 billion was used to provide funding for national public health programmes such as tackling health inequalities, improving access to services, eHealth initiatives and medical research.
Resource spending by NHS Boards can be categorised as shown in Chart Eight.
Chart Eight: NHS Expenditure 2014/15
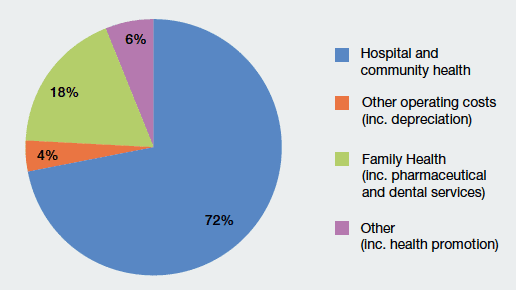
Investing in the Future
In terms of capital investment, and as part of the Scottish Government’s commitment to providing modern, state-of-the-art NHS facilities, the new £842 million Queen Elizabeth University Hospital campus in south Glasgow was delivered on time and on budget. This investment provides patients of all ages with access to services on a single site and ensures better continuity of care.
The contract was signed for the new NHS Dumfries and Galloway’s Royal Infirmary in March. The new Infirmary is due to open in the final quarter of 2017.
Other projects completed included NHS Grampian’s Forres Community Health and Care Centre (£6 million), NHS Fife’s Glenwood Health Centre (£5 million) and NHS Highland’s Tain Health Centre (£4 million).
In future, spending for community health will be the responsibility of Integrated Health and Social Care Partnerships and will focus on improving outcomes across traditional health and social care boundaries.
Efficiency Savings
Scottish Government health policy is focused on the delivery of improved quality and safer patient care while ensuring that the service is sustainable and delivers value for the public purse.
Complementing the record levels of investment in NHSScotland, all NHS Boards are required to deliver planned efficiency savings each year for reinvestment into patient care. These savings amounted to more than £285 million in 2014/15.[128]
Among the wide range of support that the Scottish Government provides to NHS Boards, the Quality and Efficiency Support Team (QuEST) has been at the heart of innovative good practice. QuEST has enabled the service to test, spread and embed innovation over a range of clinical and non-clinical areas through directly delivering specific programmes, supporting local initiatives and providing robust methodologies for knowledge capture and experience sharing.
NHS Boards achieve efficiency savings through a wide range of areas, such as procurement, facilities management and prescribing. In addition to cash savings, many initiatives lead to improvements in productivity, consequently avoiding additional cost.
Quality, Efficiency and Value
The Scottish Government approach to improvement was set out in its 2020 Framework for Quality, Efficiency and Value.[129] Launched in June 2014, the Framework included lots of examples of improvement, many of which were supported through the QuEST portfolio approach.
A primary objective of QuEST is to support NHS Boards to develop their own capacity and capability for continuous improvement. Staff at the sharp end of delivery are often best placed to identify ways to improve, as evidenced by more than 120 examples of improvement formally reported by v in the past three years.
Cash savings and cost avoidance are often at the forefront of decision making when individual NHS Boards review business cases for change. The return on investment and the payback period are critical measures when resources are under pressure. QuEST provides support to NHS Boards who may require additional help to identify and release efficiencies.
In addition to programmes related to support services such as procurement, human resources and facilities, v also supports major clinical improvement programmes. The Whole-system Patient Flow Programme includes the Safety Flow Huddle Project. Working collaboratively with the Scottish Patient Safety Programme, unscheduled care and person-centred health and care, the team supports the implementation, improvement and spread of effective hospital safety flow huddles across NHSScotland. The safety flow huddles provide an opportunity for multi-disciplinary teams to collectively discuss, prioritise and action issues of flow and safety. This provides a timely, proactive review and mitigation of clinical risks as part of a 24/7 system.
Chart Nine: Ward Length of Stay Cumulative Distribution
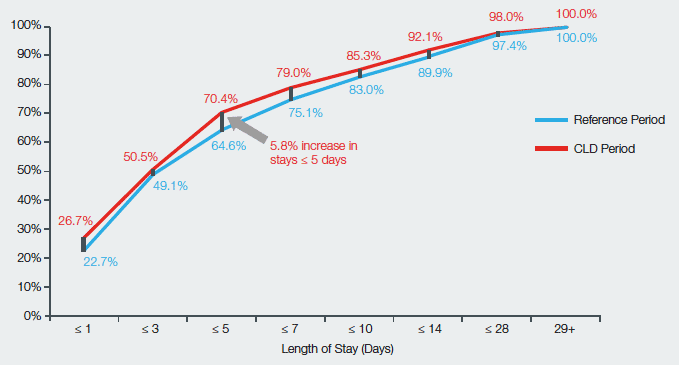
A whole-system patient flow project that exemplifies partnership working and utilising resources effectively across health and social care piloted a criteria-led discharge tool in specific wards in three NHS Boards in August 2014. Delays in discharge are a key blockage identified within the hospital system. They cause a reduction in performance against the Emergency Department Activity and Waiting Time standard, specifically producing ‘wait for bed’ breaches. This impacts on patient safety and quality of care, with patients’ length of stay in hospital extended due to delays in decision making, and the development of a ‘wait culture’ across the system. The purpose of this project is to create a tool to facilitate more effective and timely discharge planning. Criteria-led discharge enables delegated decision making by members of the multi-disciplinary team, ensuring discharge from an acute hospital at the optimum time and day for patients and the prevention of unnecessary delays.
All pilot wards realised benefits in the form of productive gain and quality improvement, including increased discharges before mid-day, increased discharges at weekends, improved patient flow, improved patient experience and reduction in length of stay.
The pilot NHS Boards are at different stages of implementation, but the ward in NHS Ayrshire and Arran that has gained the most momentum has achieved a shift to shorter lengths of stay with an increase of 5.8 per cent in stays of five days or less (see Chart Nine).
Away from the acute hospital setting, the Outpatients, Primary and Community Care Programme delivers projects to support the overall aim of moving care closer to home, enabling more people to receive the right care from the right person, at the right time, in the right place.
One change concept in the Transforming Outpatients Services Project was to implement patient reminder services to reduce appointment non-attendance and therefore release additional capacity for patient appointments. The result of pilots indicates a significant productive opportunity and an improvement in patient experience through reduced waiting times. Capacity release, reduction in non-attendance rates and cancellations resulted in a measured productive opportunity in pilot NHS Boards of up to 5,000 appointments per annum. Extrapolated across NHSScotland, this could be worth up to £5 million annually.
In addition to supporting quality and efficiency in specific areas, QuEST also supports the co‑ordination of emerging innovation and best practice across programmes. The portfolio office approach (QPO) provides benchmarking, data development and associated toolkits and shares these through national partnerships such as the Quality Improvement Hub. QPO also provides funding and monitors innovations that do not fit existing programmes.
The Future
The then Cabinet Secretary for Health and Wellbeing, Alex Neil MSP, announced in Parliament in 2014 that there would be an integrated improvement resource for NHSScotland to bring together the improvement aspects of QuEST with the Joint Improvement Team (JIT) and Healthcare Improvement Scotland. This new integrated improvement resource will harness and build on the unique and common capacities, capabilities and experience of the three teams and will be hosted within Healthcare Improvement Scotland.
QuEST support services programmes will transition to NHS National Services Scotland under the Shared Services Portfolio. The transition plan will ensure the new integrated improvement resource will be fully functional with governance in place by 1 April 2016.
Contact
Email: Andrew Wilkie