NHSScotland Chief Executive's Annual Report 2014/15
The NHSScotland Chief Executive's Annual Report 2014/15 presents an assessment of the performance of NHSScotland in 2013/14 and describes key achievements and outcomes.
Chapter 3: Improving Quality of Care
Empowering people to be at the centre of their care and listening to them, their families and carers is a strategic priority.
The Healthcare Quality Strategy for Scotland sets three clearly articulated and widely accepted ambitions based on what people say they want from their NHS: care that is person-centred, safe and effective.
The Quality Ambitions
Person-centred
Mutually beneficial partnerships between patients, their families and those delivering healthcare services that respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making.
Safe
There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate clean and safe environment will be provided for the delivery of healthcare services at all times.
Effective
The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit, and wasteful or harmful variation will be eradicated.
PERSON-CENTRED CARE
Empowering people to be at the centre of their care and listening to them, their families and carers is a strategic priority for public services, including NHSScotland, and the Scottish Government. NHSScotland is committed to developing a culture of openness and transparency that actively welcomes feedback and uses it to inform and drive continuous improvement.
Healthcare Improvement Scotland continued to work across NHSScotland and with third sector partners in 2014/15 to test and spread best practice in person-centred care. Building on the successes of the Person-Centred Health and Care Collaborative, national quality improvement support for person-centred care was refocused early in 2015 to help NHS Boards and Integrated Health and Social Care Partnerships gather and use feedback to improve experience of services, integrate person-centred care into other national quality improvement programmes and share evidence and best practice.
Improving Responses to Feedback, Comments, Concerns and Complaints
The Patient Rights (Scotland) Act 2011[35] introduced the right for people to give feedback, comments, concerns and complaints about the services they receive from NHSScotland. It places a duty on the NHS to actively encourage, monitor, take action and share learning from the views they receive.
In 2014/15, in line with one of the recommendations of the Scottish Health Council’s report Listening and Learning: How Feedback, Comments, Concerns and Complaints Can Improve NHS Services in Scotland,[36] the Scottish Government asked the Scottish Public Services Ombudsman’s Complaints Standards Authority to lead the development of a revised NHS complaints procedure. This will build on the requirements of the Patient Rights (Scotland) Act 2011 and the Can I Help You? good practice guidance for handling and learning from feedback, comments, concerns or complaints.[37]
The aim is to further improve outcomes for people by introducing a more standardised and person-centred complaints process, with a sharper focus on local ownership and early resolution. A working group that includes representation from NHS Boards, the independent Patient Advice and Support Service, the Scottish Health Council, Healthcare Improvement Scotland and NHS Education for Scotland has been convened to take this forward.
There were 22,417 complaints made about NHS services in Scotland in 2014/15[38] – the equivalent of 0.05 per cent of all NHS activity. This figure includes all hospital visits and GP, outpatient, dental and ophthalmic appointments, and represents a 9 per cent increase since 2013/14.
NHS Boards must listen to, and act, on every complaint made about the services they provide, using the information to identify changes or improvements that could be made to further improve quality of care and treatment. NHS Boards once again published annual reports this year showing where lessons have been learned and describing actions taken to improve services as a direct result of feedback, comments, concerns and complaints.
Satisfaction with NHSScotland – National Surveys
Satisfaction with NHSScotland remains high, with 89 per cent of hospital inpatients who participated in the Scottish Inpatient Patient Experience Survey 2014[39] reporting overall care and treatment to be good or excellent and 87 per cent who responded to the Health and Care Experience Survey 2013/14[40] rating the overall care provided by their GP Practice as good or excellent.
The Scottish Government published results from a new survey of NHSScotland radiotherapy patients in November 2014.[41] The survey found that the large majority had a positive experience: 97 per cent rated their overall care as excellent or very good, with patients particularly positive about staff.
Building on this work, the then Cabinet Secretary for Health and Wellbeing, Alex Neil, MSP, announced in August 2014 that a new national survey of cancer patients would be launched in autumn 2015. Scotland’s first national cancer patient experience survey will aim to provide high quality national and local data on patients’ experiences of cancer treatment and care to inform ways to enhance and improve services in Scotland. It will focus on elements such as diagnosis and treatment, information provision and the quality of care and support. Patients are expected to receive their questionnaires in October 2015, with results expected to be published in June 2016.
Development of Our Voice
In June 2014, the then Cabinet Secretary for Health and Wellbeing, Alex Neil, MSP, announced that: “We must do more to listen to, and promote, the voices of those we care for. We need the voices of our patients, those receiving care and their families, to be heard in a much clearer and stronger way.”
This is a key part of improving quality and integrating services to meet people’s needs. It will help to ensure services are person-centred and reflect the lived experience of patients and carers, and that services are designed and delivered with, rather than designed for and delivered to, patients.
The Scottish Government worked in partnership with the Scottish Health Council, the ALLIANCE, the Convention of Scottish Local Authorities, Healthcare Improvement Scotland and its public partners throughout the autumn of 2014 to develop high-level proposals for a new framework for hearing the voices of citizens in health and social care.
This aimed to find out what really mattered to people using services, families and carers, and the staff working with them. A wide range of methods, including national events, small focus group sessions, surveys, Twitter chats and virtual events, were used to gather views from individuals and groups across every Local Authority and NHS Board area in Scotland. The views were considered alongside key themes that emerged from desk research and fed into the Our Voice framework, which was launched at the NHSScotland Event in June 2015. Work is now underway to develop key elements of the framework, which is designed to support citizens’ involvement in local engagement, improvement and planning processes, and in national policy issues.[42]
Increased Use of Patient Opinion to Drive Change
The Scottish Government continued to support NHS Boards’ engagement with Patient Opinion,[43] an independent website that provides an online route for people to share their experiences of care – whether good or bad – directly with NHS Boards and engage in constructive dialogue with them about how services can be improved.
In 2014/15, 1,305 stories were shared on Patient Opinion, representing a 96 per cent increase on the same period in 2013/14. The vast majority (98 per cent) received a response, and 43 service changes to NHS services were made (or are being planned) as a direct result of the stories.
The Scottish Government has signed a contract with Patient Opinion that provides for each Territorial NHS Board and relevant Special NHS Boards, including NHS Education for Scotland, the Golden Jubilee Foundation, NHS 24, the Scottish Ambulance Service, NHS National Services Scotland and Healthcare Improvement Scotland, to be fully registered with Patient Opinion for up to three years from April 2015. A comprehensive package of support is available to NHS Boards to support them to engage effectively with the site.
Third Sector Partnerships
The NHSScotland strategic partnerships with third sector organisations continued in 2014/15 as part of the drive to improve care through active participation. The ALLIANCE brought together a number of workstreams involving third sector partners with expertise in delivering person-centred care to enable people with lived experience to contribute to the co-design of services and support local teams to make their services more person-centred. This reflects the partnership approach adopted to improving the whole system: it recognises the value of partnership and, indeed, patients and service users in the health and social care system.
The ALLIANCE has directed work with three early adopter sites (NHS Tayside, NHS Greater Glasgow and Clyde, and NHS Lothian) and two further sites (NHS Ayrshire and Arran and NHS Lanarkshire) to take forward the ‘House of Care’[44] approach to collaborative care and support-planning. This approach, which has an internationally recognised evidence base, puts people and their families in the driving seat of their care.
Funded by the Scottish Government and delivered in partnership with the ALLIANCE, ALISS (A Local Information System for Scotland) continued to map assets across the community to enable people to more effectively self-manage by connecting them with local sources of support. ALISS is now being rolled out across all Community Pharmacies in Scotland.
Work continued to support people to have the knowledge, understanding, skills and confidence they need to use health information, to be active partners in their care, and to navigate health and social care systems. A demonstrator programme as part of the Making it Easy: a Health Literacy Action Plan for Scotland[45] was initiated in NHS Tayside in March 2015. It is examining a range of tools and approaches to enable staff to recognise and cater for the health literacy needs of their patients.
Carers
Funding of nearly £34 million is being provided between 2008 and 2016 to NHS Boards and the Scottish Ambulance Service for direct support to carers, of which £5 million was allocated in 2014/15 to take forward a wide range of initiatives to support carers[46] and young carers. NHS Boards were asked to continue to support previous priorities for 2014/15, including funding carers’ centres that provide a range of services such as advocacy and advice, training for carers and the workforce, and short breaks.
The Carers (Scotland) Bill,[47] which was introduced in March 2015, will extend the rights of carers and young carers. It will make a meaningful difference to unpaid carers and will contribute towards the improvement of their health and wellbeing, ensuring they can continue to care but also have a fulfilling life. It will also reflect the importance of carers in improving care and quality. The Bill, which is currently in Stage 1 of Parliamentary consideration, is an important part of the wider programme of health and social care reform.
A new official statistics report was published in March 2015. Scotland’s Carers[48] gives one of the clearest and most detailed pictures of the caring population ever produced, covering issues such as gender, carers’ health, employment and deprivation.
Self-directed Support
The Social Care (Self-directed Support) (Scotland) Act 2013[49] has directly put eligible people from across Scotland at the centre of shaping their own care and support, enabling them to exercise greater choice and control and access more flexible support. The Act is helping more people to live more independent, fulfilling lives.
At the core of self-directed support is a support-planning conversation that identifies personal outcomes and ways in which they can be achieved. The Scottish Government has invested £7.5 million since 2012 in independent information and support to ensure everyone can participate in their support planning. Aggregated learning from 42 independent projects shows that people and carers now have clearer information about self-directed support, more opportunities for choice and control, and are better able to make informed choices. This evidence has led to a Scottish Government commitment to provide a further £2.4 million across 34 organisations in 2015/16 to build the capacity of independent support and information for people.
Innovative service design and delivery is essential to providing sufficient flexibility for people to achieve the personal outcomes they define during support-planning. Employment can feel like a distant goal for many people who require support. That is why the Scottish Government funded projects like Pilotlight in Moray,[50] in which a team of people who access social care services, commissioners and providers of social care and employment support services used co-design to deliver practical solutions and tools. These have enabled people who access self-directed support to set up their own small businesses.
The Scottish Government has invested £6.3 million since 2012 in over 30 third and private sector providers to support innovative service delivery. A further £1.1 million is being invested in 21 organisations during 2015/16 for building the capacity of providers and workforce development.
Self-directed support is most successful when independent information organisations, third and private sector providers of care services and support, community groups, Local Authorities, Integrated Health and Social Care Partnerships and people, families and carers work together in partnership.
Palliative and End-of-life Care
The Scottish Government established a new Palliative and End-of-life Care National Advisory Group in 2014 to strengthen governance and leadership in this area. Membership is drawn from across the health, independent hospice and care sectors, and is supported by a stakeholder group. This group is supporting the development of a strategic framework for action to provide a focus for, and support the delivery of, high quality palliative and end-of-life care.
The Scottish Government engaged widely throughout the early part of 2015, including with people working in health, social care and the third and private sector and members of the public, about What matters to them about the future of palliative and end-of-life care.[51] This inclusive approach to the development of the framework will help ensure that people can identify with the actions required to deliver change. The strategic framework will be published at the end of 2015.
Health Information Services
NHS 24[52] continued to develop and make available key health and care information for people during 2014/15, using a range of platforms and services that includes NHS Inform, the national health and care information service, along with Care Information Scotland, Smokeline,[53] Know Who To Turn To[54] and the NHS 24 website.[55] These platforms received 2.9 million contacts through internet, telephone and user-engagement sessions during the year. NHS 24 also provided five special helplines, including a UK helpline, as part of its service provision during 2014/15.
Other developments included the relaunch of Care Information Scotland as a new website and service for all carer groups, the redevelopment of NHS 24’s web-based self-help guide, the launch of the Fit for Work website and the start of an evaluation process to scope the future direction of the Smokeline service.
SAFE CARE
The Quality Ambitions articulate clearly the aim to ensure there is no avoidable injury or harm to people from the health care they receive, and that clean and safe environments will be provided for the delivery of healthcare services at all times.
The internationally acclaimed Scottish Patient Safety Programme[56] was launched in January 2008, focusing at that time on acute adult care. Its aim is to reduce avoidable harm to patients by improving the safety of care provided across NHSScotland. The Programme now has six strands – Acute Adult, Healthcare Associated Infection (HAI), Maternity and Children, Medicines, Mental Health, and Primary Care – and continues to drive improvements across a number of key areas of healthcare.
The Scottish Patient Safety Programme seeks to engage frontline staff in improvement work by promoting the application of a common set of tested, evidence-based interventions and a common improvement model based on the plan-do-study-act (PDSA) model. A key element is that the changes are led by staff who are directly involved in caring for patients. Staff can monitor improvements through the collection of real-time data at individual unit level.
Work to reduce Healthcare Associated Infections, implement electronic prescribing via the ePharmacy Programme and to support improved care for older people in hospital also continues. These developments demonstrate the breadth of effort in Scotland to provide safer outcomes for people accessing healthcare services.
Examples of key achievements of the quality improvement work across NHSScotland are set out here.
Reduction in Mortality from Sepsis
Sepsis is a life-threatening condition triggered by an infection. It is a whole-body inflammation that occurs when the body’s response to infection damages its own tissues and organs. Sepsis continues to be one of the world’s biggest killers, with incidence continuing to rise.
Sepsis is extremely dangerous because of its rapid onset. If it can be diagnosed and treatment with the appropriate antimicrobials and intravenous fluids offered within the first hour, survival rates can be higher than 80 per cent.
Someone dies of sepsis every 3-4 seconds[57] and is one of the harms being addressed by the Scottish Patient Safety Programme, which has developed the Sepsis Collaborative and supported NHS Boards to deliver its aims.
The Collaborative’s initial aim was to reduce mortality in acute care settings by 10 per cent through early identification of patients and completion of the Sepsis 6 Care Bundle within one hour. The Collaborative exceeded its aim of a reduction in mortality from sepsis with data showing a relative reduction in mortality of 21 per cent over the period from January 2011 to March 2015[58]. Eighty per cent of patients identified as having sepsis now receive antibiotics within one hour[59]
Safety in Inpatient Mental Health
The Scottish Patient Safety Programme for Mental Health[60] aims to reduce the harm experienced by people in receipt of mental health care so that both staff and patients within services feel, and are, safe. The work is delivered through a four-year programme running to September 2016, with the Scottish Government providing funding of over £245,000 in 2014/15.
The Programme enjoys a very high level of engagement from NHS Boards. Through collaboration and innovation from staff, service users and carers, and through the development and use of quality improvement interventions and processes, it has helped cultivate learning among those delivering and in receipt of care to improve the safety and quality of care delivered in mental health inpatient settings.
As a result, significant reductions in the number of patients who self-harm (up to 57 per cent), reductions in rates of violence and aggression (up to 54 per cent), and reductions in restraint (up to 63 per cent) are now beginning to be seen across a number of areas in Scotland. Nationally aggregated data gives a baseline and a route to comparison, but it is the individual ward data that is showing real improvement.
Recognition of the pivotal role of service users, carers and the third sector in the Programme has ensured that they have been involved in every step of the process. For example, the Patient Safety Climate Tool (PSCT),[61] developed by mental health service users and carers, has seen over 400 patients across Scotland given the opportunity to participate in a facilitated survey designed to enquire about environmental, relational, medical and personal safety. It is a Scottish innovation that is leading the way in person-centred and safe delivery of care.
Examples of themes from completed PSCTs have included the requirement for more information about medication and possible side-effects and positive comments about staff, particularly their ability to deconstruct and help to explain and interpret difficult situations such as being restrained or witnessing a restraint.
Reducing Harm in Primary Care
The Primary Care strand of the Scottish Patient Safety Programme aims to reduce the number of events which could cause avoidable harm from healthcare delivered across the wide range of Primary Care settings. Launched with an initial focus on General Practice, a range of tools and resources has been developed to support those working within Primary Care to improve the quality of care to patients, developing the patient safety culture within their teams and making higher-risk processes reliable. The work has now spread to Community Pharmacy, where a collaborative is currently testing approaches for national adoption in this setting, and recruitment to a similar dental collaborative has also commenced.
Within General Practice, the current GMS contract supports two principal pieces of work: reflective review of case notes by trigger tool; and a practice Safety Climate Survey.
The trigger tool review, using the NHS Education for Scotland Primary Care Trigger Tool, allows GP Practices to analyse a sample of case notes to determine whether any safety events, or near misses, have taken place. The resultant reflective report is discussed within the Practice before being shared with the NHS Board so that themes may be developed and further improvement activity undertaken taken if appropriate.
The Safety Climate Survey is a validated tool for all Practice staff, clinical and non-clinical, to express their views in six key areas of safety climate. This data can then be used by Practices to determine strengths and areas for development through the formation of a reflective report which is shared with the NHS Board where learning across the system may again be aggregated.
In addition to each of these areas, NHS Boards have commissioned a range of local enhanced services to improve areas of care that are recognised as being of higher risk to individuals; examples of these include warfarin therapy, disease modifying anti-rheumatic drugs, medicines reconciliation and laboratory results handling.
Improving the Care Experience for all Women, Babies and Families in Scotland
The maternity, neonatal and children’s strand of the Scottish Patient Safety Programme is continuing to improve care and reduce inequalities in healthcare outcomes by providing a safe, high quality care experience for all women, babies and families in Scotland.
The Scottish Government is committed to ensuring that every child has the best possible start in life. To support this endeavour, a Midwifery Champion has been funded for every Territorial NHS Board to facilitate capacity-building and implementation of the Maternity and Children Quality Improvement Collaborative. Champions work alongside national programme leads and local improvement colleagues to engage relevant multi-professional and multi-agency stakeholders from acute and Primary Care in the Collaborative’s work and build capability and capacity in improvement science in local communities. They also facilitate introduction of care bundles and other initiatives and support data collection and dissemination.
The Collaborative has achieved:[62]
- a 14.4 per cent reduction in the annual national stillbirth rate from 2012 to 2014;
- a 5.3 per cent reduction in the annual neonatal death rate from 2012 to 2014 (see Chart Six); and
- 93 per cent of women being offered carbon monoxide monitoring at booking.
Chart Six: Annual National Neonatal Death Rate (per 1,000 live births) – NRS (Run chart)
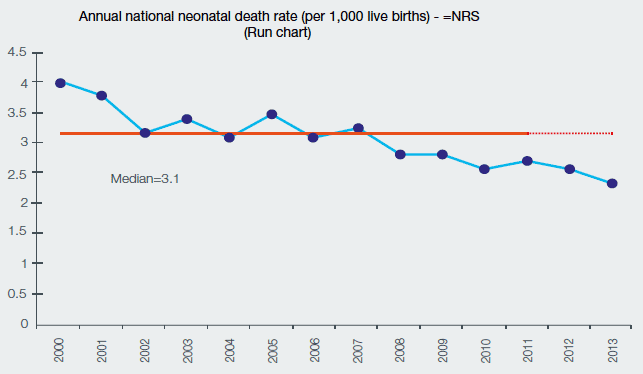
Source: Healthcare Improvement Scotland using NRS data
Reducing Healthcare Associated Infections
Reducing Healthcare Associated Infections (HAI) remains a priority for Scottish Government Ministers and NHSScotland. People should be able to have confidence in the quality of the care they receive and be assured that work continues to reduce HAI and improve outcomes.
The commitment to this priority is demonstrated by the reduction of cases of methicillin-resistant Staphylococcus aureas (MRSA) from 88 per cent from January to March 2007 to April to June 2015.[63] Cases of Clostridium difficile infection in patients aged 65 years and older reduced by 84 per cent in the same period.[64]
Tackling the rise of antibiotic resistance is another priority and the Scottish Antimicrobial Prescribing Group report on Antimicrobial Use and Resistance in Humans 2014[65] shows that the use of systemic antibacterials in Primary Care was 1.9 per cent lower in 2014 than in 2013 and the rate of prescribing in 2014 has reduced to the same level as 2005.
The Vale of Leven Hospital Inquiry concluded and published its report on the 2007/08 Clostridium difficile outbreak in November 2014.[66] The report identified system-wide failings and the occurrence of at least 34 deaths between 2007 and 2008 in which Clostridium difficile infection was a causal factor, but acknowledged the significant work taken forward in Scotland to prevent such a tragedy occurring again. Work progressed during the year (including with the families of those affected) to develop the Scottish Ministers’ response to the report,[67] learn lessons and continue to make improvements.
The Healthcare Environment Inspectorate’s annual report (published in February 2015)[68] highlighted 51 inspections in 34 hospitals in 14 Territorial and two Special NHS Boards in the period October 2013 to December 2014. The Inspectorate made 143 requirements and 61 recommendations. Requirements and recommendations have reduced significantly since the Chief Inspector’s first annual report, demonstrating the improvements and progress that continue to be made by staff across hospitals in NHSScotland.
The ePharmacy Programme and Electronic Prescribing
Over 100 million prescription items were dispensed in the community in 2014/15, with over 90 per cent prescribed by GPs.[69] The ePharmacy Programme is revolutionising the way GP prescriptions are issued, dispensed at Community Pharmacies and processed for payment by the NHS, using the Electronic Transmission of Prescriptions system. The system increases patient safety by avoiding transcription errors and increases the accuracy and efficiency of drug reimbursement payments to Community Pharmacies.
Over 98 per cent of GP prescriptions are now issued electronically. Approximately 88.3 per cent of those dispensed at Community Pharmacies are claimed electronically, with 87.8 per cent of claims automated for pricing purposes.[70] The automation of claim-processing delivers a more efficient payment process, enabling back-office costs to be saved and diverted to frontline NHS services.
The ePharmacy platform leads the way in electronic prescribing systems in other parts of the UK.
Care for Older People in Hospitals
Healthcare Improvement Scotland led the Chief Nursing Officer Directorate-funded Improving Care for Older People in Acute Care workstream, which focused on two key areas:
- care co-ordination – identification and immediate management of frailty; and
- cognitive impairment – identification and immediate management of delirium.
Patients identified as frail on admission to acute care settings receive comprehensive assessment and input from a specialist team on the day of admission. Evidence shows that appropriate and timely screening and assessment can reduce length of hospital stay and improve patient experience.
Healthcare Improvement Scotland published a case study report on innovations in identifying and managing frailty in four acute sites in NHSScotland in April 2011.[71] The case study’s overall conclusion, under the heading ‘Demonstrating Outcomes’, included the following: “This report highlights significant improvements and outcomes for frail elderly people coming into hospital. These outcomes include reduction in admissions and re‑admissions to hospital, reduction in length of stay, reduction in discharge to care home and reduction in mortality”.
Managing Falls for Older People in Care Homes
The Up and About in Care Homes Improvement Collaborative was established in January 2014 with the aim of reducing falls in participating care homes by 50 per cent by the end of 2015. It recognises and reflects the need to reduce ‘avoidable’ hospital admissions where it is known that outcomes will worsen and problems linked to frailty are likely to increase during a hospital stay.
The Collaborative has developed a number of resources and tools covering education, information and advice to support daily practice in the management of falls and fractures in care homes. Reductions in the total number of falls and the number of those resulting in injury has been reported in care homes that have taken a proactive approach to improvement, with one care home achieving a 74 per cent reduction.
EFFECTIVE CARE
Many of the areas for improvement prioritised over 2014/15 make a direct contribution to achieving the Quality Ambition of more effective healthcare services. A focus has been to identify improvements for which there is clear and agreed evidence of clinical and cost-effectiveness, then support the spread of these practices (where appropriate) to ensure reductions in unexplained and potentially wasteful or harmful variation.
Primary Care
Transforming Primary Care
Primary Care remains the place where people interact with NHSScotland on a day-to-day basis. Pharmacists, Dentists, Optometrists and GPs, along with their Community Nursing and Allied Health Professional colleagues, provide enormously valued services at the heart of local communities. They work with all parts of the community and play a significant role in ensuring excellent service delivery.
This is a key component of integrating health and social care. As the ‘front door’ to services, Primary Care will shape pathways of care, reflecting closer and joined-up working with other professionals, including those in social care.
Challenges continue to exist, including those related to health inequality and rurality. As the population grows and people are living longer, they need different Primary Care services to manage their long term conditions in the community. GP practices working in clusters and as part of multi-disciplinary teams are needed to support individuals in a holistic and person-centred way, delivering care at home or in a homely setting.
We are committed to transforming Primary Care services, and increasing training posts is one of many initiatives needed to achieve this. This has to be combined with making a career as a GP more appealing and work to do this is progressing through our reforms to Primary Care; such as abolishing the outdated Quality and Outcomes Framework rewards from GP contracts.
We need to be more innovative and flexible in our recruitment efforts and are working closely with stakeholders on this. This includes looking at the way in which GP trainees are recruited, and enhancing the potential roles for GPs including working in new models of care, such as one-year fellowships in a community hub.
The contract status of GPs was stabilised on a three-year basis in 2014 after years of annual fluctuation, and work began in earnest with the British Medical Association (BMA) on proposals for a new GP contract from 2017 that will be based on quality, leadership and person-centred care. The introduction of Integrated Health and Social Care Partnerships means GPs must play a key role in locality planning. GPs understand their communities and are often the key decision makers regarding care pathways, so they need to be actively engaged in shaping local services and have responsibility for how best to spend the money to deliver services that improve outcomes.
The crucial role of GP out of hours services was recognised when Professor Sir Lewis Ritchie was asked to chair a review of out of hours Primary Care in January 2015. Sir Lewis, whose approach has been inclusive and wide-ranging, will present his recommendations later in 2015.
Building Clinical Capacity
The Prescription for Excellence (PfE) Programme is working towards building clinical capacity in Primary Care as a key priority to improve access to high quality pharmaceutical care and ensure all patients get the best possible outcomes from their medicines, while avoiding waste and harm.
Delivery of Primary Care Fund activities complements key PfE workstreams and aims to develop Primary Care pathways. The Primary Care Fund has allocated £16.2 million over the next three years to recruit up to 140 additional Pharmacist Independent Prescribers with advanced clinical skills training to work as part of multi-disciplinary teams in GP Practices. These pharmacists will manage caseloads, carry out medicines reviews and support the care of patients with long term conditions, consequently freeing-up GP time to spend with other patients.
Independent Prescribing by Physiotherapists and Podiatrists
It is increasingly recognised that services need to care for the whole person, rather than expecting people to fit into historic structures and arrangements that have more to do with administrative convenience and professional boundaries. Non-medical prescribing is at the forefront of changing professionally defined boundaries and shifting the focus to what people need to promote their wellbeing.
Physiotherapists and Podiatrists have been able to train as independent prescribers since May 2014. Prescribing rights enable these professionals to fully treat and support patients by, for example, prescribing appropriate pain killers as part of a treatment plan.
Unscheduled Care
NHSScotland faced some very challenging times last winter with crowding in Accident and Emergency (A&E) Departments, mainly due to unprecedented levels of activity, bed days lost to delayed discharge and people awaiting care in their communities.
Substantial funding was invested during 2014/15 to alleviate these issues at central and local levels and to support sustained improvements. Over £9 million was allocated to building on local unscheduled care action plans, £10 million to supporting improvements in relation to delayed discharge, and £10 million for winter resilience, with a focus on delayed discharge.
As outlined to in Chapter 2, Scotland’s unscheduled care performance last winter deteriorated in line with other parts of the UK and, indeed, similar health systems across the world. Scotland’s core A&E performance was nevertheless almost 1 per cent better than England’s in winter 2014/15, having been almost 1 per cent worse in winter 2013/14. Although Scotland’s performance continues to be the best in the UK, more needs to be done, particularly in certain NHS Boards and sites.
Health and social care integration is key to this. While only in the implementation phase, integration presents great opportunities for preventative and anticipatory care planning, joined-up services that prevent unnecessary admission, and alternative care-based services. This will require a joint approach through Integrated Health and Social Care Partnerships in which all partners are involved and, importantly, Local Authorities and NHSScotland are jointly responsible.
The £50 million national unscheduled care action plans have delivered significant benefits since their launch in 2013, including the introduction of weekend discharge teams, widespread introduction of patient safety and planning huddles, enhanced use of discharge lounges and the introduction of models of care for frail older people. It was nevertheless recognised that something drastically different needed to be done to ensure patients arriving at A&E departments received the quality of care they deserve.
The Cabinet Secretary for Health, Wellbeing and Sport announced in January 2015 the move to an improvement-focused approach to unscheduled care based on six fundamental actions developed in partnership with the Academy of Royal Colleges. The ‘6 Essential Actions to Improving Unscheduled Care’ are:
- clinically-focused and empowered hospital management;
- realignment of hospital capacity and patient flow;
- operational performance management of patients presenting at A&E and progressing through the acute system;
- medical and surgical processes arranged to take patients from A&E through the acute system;
- seven-day services targeted to increase weekend and earlier-in-the-day discharges; and
- ensuring patients are cared for in their own homes or a homely setting.
This new approach, which was launched in May this year, is a two-year programme that aims to improve outcomes for people using services. It is multi-disciplinary in nature and requires commitment across every part of the health and social care system to ensure better care on a sustainable basis, joining up several work strands to ensure a much more strategic approach is adopted. National and local teams dedicated to progressing the 6 Essential Actions have been recruited.
While steady and significant improvements have been made in A&E over the spring (and beyond), ongoing challenges persist. NHSScotland and its partners are committed to addressing these to bring about sustained improvements for the people of Scotland.
Delayed Discharge
Tackling delayed discharge is one of the Scottish Government’s key priorities for NHSScotland and its partners. We invested an additional £18 million in 2014/15 to tackle delayed discharges by supporting the development of intermediate care and other services aimed at supporting people to remain healthy and independent at home or in a homely setting. Local partnerships increased the number of step-down Intermediate Care beds by 200 during 2014/15, with 700 such beds now in place across Scotland.
Alongside these additional resources, Scottish Government officials worked closely with those partnerships facing the most significant challenges to identify areas of improvement. These discussions took place under the new shadow integration arrangements, with local partnerships starting to think in terms of shared resources and shared solutions.
As a consequence of this targeted investment, delays of over three days reduced by over 30 per cent, from 947 in October 2014 to 633 in April 2015.[72] During the same period bed days occupied reduced by over 16 per cent (from 56,122 at October 2014 to 46,890 in May 2015)[73] (see Chart Seven).
Excellent progress has been made by a number of partnerships during 2014/15, in particular, by increasing the use of Intermediate Care, and their focus on a discharge to assess policy.
In January, a £100 million investment, over three years, was announced to help Integrated Health and Social Care Partnerships tackle delayed discharges.
Chart Seven: Delayed Discharge April 2014 - May 2015
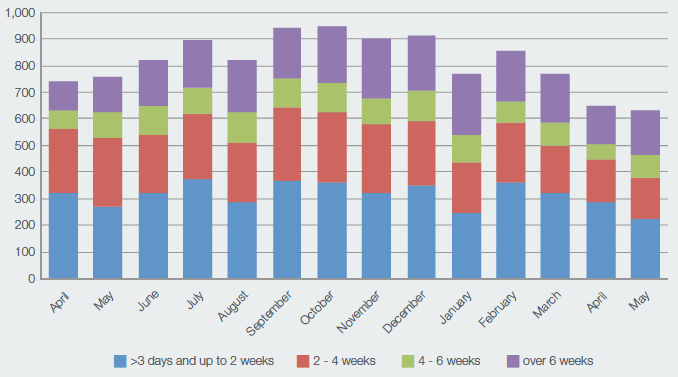
Move to New 111 Telephone Number
NHS 24 changed its telephone number to the new free-to-call 111 number in April 2014. The NHS 24 service remains unchanged, with people seeking help and advice during the out of hours period receiving the same high quality, safe and effective national unscheduled care service.
The switch to the free-to-call number was carefully planned to ensure a successful service transition. It was launched by the then Cabinet Secretary for Health and Wellbeing, Alex Neil MSP, and was supported by a public campaign using a mixture of public relations, social media and press, radio and outdoor advertising across the summer months.
Within eight weeks of introduction, 85 per cent of calls to NHS 24 were being made via the 111 telephone number. NHS 24 received 1,441,483 calls in total in 2014/15 (including 08454 and 111 numbers), a 16.7 per cent rise on 2013/14. The busiest day for the service since 111 was introduced was 2 January 2015, when it received 12,519 calls.[74]
Dementia
It is important that everyone in Scotland who has dementia has an early diagnosis and receives person-centred, safe and effective care at all stages of the illness and in all care settings – at home, in hospital and in residential care. Latest diagnosis information (from 2014) shows that between half and two-thirds of people with dementia are being diagnosed (depending on which prevalence model is applied).[75]
We are working with partners to support delivery of our world-leading service offer of a minimum of a year’s worth of dedicated post-diagnostic support by a named Link Worker. Delivery is underpinned by a Local Delivery Plan Standard, with performance data to be published in spring 2016. We are also testing Alzheimer Scotland’s proposed model of home-based support for people with
dementia whose symptoms have advanced to the extent that they need intensive care and support to stay at home. We are working with five test sites – North Lanarkshire, Midlothian, Highland, Moray and Glasgow City – and the usefulness and impact of the service model is being independently evaluated, with a report scheduled for 2016.
The national approach to up-skilling and developing the dementia workforce continues, backed by around £500,000 per annum. Over 500 healthcare and social care staff have been trained as Dementia Champions to support joint working with people with dementia (this is expected to increase to over 600 in the next two years) and around 800 Dementia Ambassadors in Social Care have been trained.
The Quality and Excellence in Specialist Dementia Care Programme was developed in 2014/15 to extend work in improving standards of dementia care in general hospitals to other hospitals and NHS settings (including specialist dementia mental health units providing care and treatment for people with progressed-stage dementia).
Driving Up Standards of Dementia Care in Hospitals
The three-year strategy to improve dementia care[76] includes a 10-point action plan to drive up standards of care in hospitals. The actions focus on improvements in leadership, person-centred care, the environment and discharge planning.
The Dementia in Acute Care Settings improvement programme, launched in July 2014, concentrates on leadership, workforce development, working as equal partners with families and minimising and responding to stress and distress. NHS Education for Scotland has produced resources to support staff working with people who have dementia, including in acute care.
An evaluation report looking at the impact of Alzheimer Scotland Dementia Nurse Consultants and Dementia Champions was published in June 2014.[77] The report states that: “Improving experiences and outcomes for people with dementia care in acute general hospitals is recognised in Scotland’s Dementia Strategies as requiring significant cultural change and service development. Despite the enormity of the task and the relative small scale and immaturity of the initiatives, a significant amount of change and improvement work has been initiated by the two roles, and would likely not have happened without them”.
Improving Mental Health Services
Psychological Therapies and Child and Adolescent Mental Health Services
Data published by Information Services Division (ISD) Scotland indicates that the total number of people starting treatment in the quarter ending 31 March 2015 increased 24 per cent for psychological therapies and 18.5 per cent for Child and Adolescent Mental Health Services over the same period last year (see Table 1).
Table 1: Starting treatment with psychological therapies and child and adolescent mental health services, 2014/15
| Psychological therapies | CAMHS | |
| March 2014 | 9,4061[78] | 3,6012[79] |
| March 2015 | 11,6593[80] | 4,2694[81] |
| Difference | +2,253 | +668 |
| As a percentage of March 2014 | +24% (23.9%) | +19% (18.55%) |
Suicide Prevention
The Scottish Government has continued to work with a range of cross-sectoral partners to improve mental health services and the diagnosis of depression and other mental health problems. More support is now available for those affected and much has been done to improve safety for patients experiencing mental health problems and tackle the stigma of mental ill-health.
Suicide rates in Scotland over the rolling periods 2000 to 2004 to 2010 to 2014 fell by 17.8 per cent, with the number of deaths by suicide in 2014 the lowest in a single year since 1977.[82] [83] The welcome continuing downward trend in the suicide rate suggests that suicide is preventable and that having the right support available can make a big difference.
Breathing Space
The NHS 24 national mental health support service, Breathing Space, reached its 10th anniversary in November 2014. The service has taken more than 525,000 calls since it was established. Key milestones include the development of a national website in 2005, the launch of an annual awareness-raising day (‘Breathing Space Day’) in 2007 and the introduction of an award-winning British Sign Language (BSL) service in 2010. A new website was also launched to mark the 10th anniversary year.[84]
Vocational Rehabilitation
Allied Health Professionals are leading on the implementation of the Individual Placement and Support (IPS) model of vocational rehabilitation, which can support up to 66 per cent of users to gain paid employment, producing 50 per cent cost savings for every individual in work.[85]
An increasing number of service users now have access to IPS, with more models in development. Evaluation using the Fidelity Review has resulted in improved client outcomes.
Cancer
Detect Cancer Early Programme 2014/15
As outlined in Chapter 2, the Scottish Government launched the Detect Cancer Early Programme in February 2012 to address the poor quality of life and poor survival rates resulting from late diagnosis. Early detection offers people the best chance of cure and possibly an opportunity to join clinical trials. Even in cases of advanced or incurable disease, early detection increases the chances of being able to offer treatment that prolongs life or allows more time to manage symptoms better and improve quality of life.
The Programme has successfully carried out five social marketing campaigns to help people spot the signs and symptoms of cancer earlier, encourage them to seek advice from their health professional and provide information to allow them to make an informed choice about participating in cancer screening programmes.
Fundamental to success is the need to address people’s deep-rooted attitudes about cancer and ensure they understand the disease is not what it used to be – it can be survived, and early detection is worthwhile.
The Programme reached its three-year milestone in February 2015, producing a short film highlighting achievements in 2014/15.[86]
A new regional campaign was launched in autumn 2014 to emphasise the benefits of breast screening in areas of low uptake. The campaign included a short film starring the actress Elaine C Smith that aimed to demystify the process of breast screening and the distribution of over 55,000 ‘thingymaboob’ keyrings. The bowel screening campaign helped contribute to an 80.6 per cent increase in the number of replacement bowel screening kits requested during campaign periods and over 4,300 extra test kits returned each month.
The lung cancer campaign was refreshed to include a ‘three-week cough message’. This resulted in a significant increase in the proportion of people aged 55 years and over who disagreed strongly with the idea that they would ‘feel silly’ going to the doctor with any small changes they
thought could indicate lung cancer – up from 24 per cent to 36 per cent. In addition, 93 per cent of the core Detect Cancer Early target audience (those most at risk of cancer and least likely to take part in screening) agreed that: “The earlier lung cancer is detected, there’s more that doctors can do to treat it”.
A two-year Primary Care initiative in which GPs are recognised for their role in supporting informed uptake of screening was supported by the large majority (83 per cent) of participating GP Practices across Scotland. The choice of whether to participate in screening programmes is a personal one, and those who are eligible are provided with information on the benefits and risks to enable them to make an informed choice.
Healthcare Improvement Scotland published refreshed Scottish Referral Guidelines for Suspected Cancer[87] in August 2014 and a mobile app is in development for late 2015 to ensure timely referral and diagnosis for all suspected cancer patients.
Building on this work, the ‘wee c’ strategy[88] was launched by the Cabinet Secretary for Health, Wellbeing and Sport, Shona Robison MSP, in August 2015. This strategy is a joint venture involving the Detect Cancer Early Programme in partnership with Cancer Research UK that aims to reduce the fear typically associated with cancer and push the message that: “Together, we can turn the Big C into the wee c”.
Development of National Cancer Quality Performance Indicators
National Cancer Quality Performance Indicators (QPIs)[89] have been developed to drive continuous quality improvement in cancer care and ensure consistency and quality in treatment across NHSScotland. The indicators are proxy measures of the quality of cancer care and have been developed for 18 tumour types including breast, lung and colorectal.
The QPI Programme aims to foster a culture of continuous quality improvement in which data is reviewed regularly at multi-disciplinary team/unit level and issues are quickly addressed. This ensures that activity is focused on the areas that are most important in relation to improving survival and enhancing patient experience while ensuring the most effective and efficient delivery of care.
NHS Boards are required to report against the QPIs as part of a mandatory publicly reported national programme.[90] Reports for breast, upper-gastrointestinal, lung and colorectal cancers have already been published and more will be released over the coming year.
Out-of-Hospital Cardiac Arrest Strategy
The Out-of-Hospital Cardiac Arrest (OHCA) Strategy for Scotland[91] was launched on 27 March 2015. This five-year plan aims to ensure that Scotland becomes a world leader in OHCA outcomes by 2020 by increasing survival rates by 10 per cent across the country. Increasing bystander cardiopulmonary resuscitation (CPR) is the cornerstone of improving outcomes: it can double or even triple the likelihood of survival.[92] The strategy aims to equip an additional 500,000 people with CPR skills by 2020.
The Strategy has been co-produced by a broad coalition of stakeholders, including emergency services, primary and secondary healthcare providers, third and private sector groups and academics. The commitment to improve OHCA outcomes is a collaborative effort, the success of which will depend on contributions and actions from many individuals and organisations. It will also require concerted clinical and political leadership and a change in culture around OHCA.
Increasing Access to Orphan, Ultra-orphan and End-of-life Medicines
More patients than ever are benefiting from access to new medicines for the treatment of orphan, ultra-orphan[93] and end-of-life conditions following the implementation of policy changes designed to increase patient access. Around 500 patients in Scotland were treated with medicines in these categories in 2014/15[94] ahead of the positive impact of decisions from a new approach being implemented by the Scottish Medicines Consortium. The changes were supported by the Scottish Government’s New Medicines Fund.
Increasing Access to Insulin Pumps
Following the Ministerial Commitment in 2012 to increase access to insulin pumps as an effective person-centred treatment for type 1 diabetes, more people than ever now have access to this potentially life-changing therapy.
A quarter of young Scots with type 1 diabetes had access to insulin pump therapy in 2014/15,[95] exceeding the overall commitment to increase the total number of insulin pumps available to people of all ages to more than 2,000. Having met this commitment for Scotland as a whole, work with NHS Boards continues to ensure that insulin pump therapy is fully embedded and delivered as a core part of diabetes services, and that improvements in access are sustained.
ScotSTAR Service
The Scottish Ambulance Service launched a world-class national specialist transport and retrieval service for critically ill patients on behalf of NHSScotland on 1 April 2014.
With an annual investment of £9.5 million, ScotSTAR provides a single integrated national service involving a sustainable multi-disciplinary team to make best use of road and air transport resources. It brings the three transport and retrieval services – the Scottish Neonatal Service, the Transport of Critically Ill and Injured Children Service, and the Emergency Medical Retrieval Service – together with the Scottish Ambulance Service, which co-ordinates the teams and road and air ambulances.
ScotSTAR delivers a centralised and co-ordinated approach that will create opportunities for greater shared working, training and education for staff. The new service transferred 2,654 of the most seriously ill patients to specialised treatment in 2014/15.[96]
Early Years
NHSScotland continues to be involved in the work of the Early Years Collaborative,[97] which is picking up pace across the 32 Community Planning Partnerships.
Eight Early Years Collaborative Key Change themes were agreed in 2014/15 and tests are helping to identify the high-impact interventions that are most likely to improve outcomes for children in their early years and achieve the stretch aims, which are ambitions aims that set out to challenge and stretch the service to achieve them. Highlights include tests that are supporting local improvements in: increasing the uptake of Healthy Start vouchers; joining up midwifery and addiction services for vulnerable families; increasing attendance at the 27- to 30-month child health review; and finding new person-centred ways to identify specific child health and wellbeing needs.
The number of tests across the Key Change themes continues to grow, with opportunities now being identified to spread interventions that have been proven to work across Community Planning Partnerships. This includes an income maximisation model that involves midwives identifying and referring vulnerable families to local welfare benefits advice services. The model has been spread to four Community Planning Partnership areas so far and is increasing the number of families receiving such advice and support.
Workforce
As Chapter 1 explains, the NHSScotland workforce is the key to delivering high quality healthcare. A healthy organisational culture is not about what we do, but how we do it. NHS Boards ensure everyone is clear about the values and behaviours expected of them. Local feedback from patients, staff and service users inform how well the values are embedded.
Recruitment
Recruitment of staff remains the responsibility of individual NHS Boards, but the Scottish Government has been able to help them with their recruitment challenges. For example, officials worked with NHS Boards to gather evidence of shortages across medical specialties and submitted evidence to the Migration Advisory Committee in December, resulting in the UK Government making additions to the UK-wide and Scotland-only Shortage Occupation lists. NHS Boards seeking to recruit specialists from this list should now find it quicker and less expensive to do so from abroad.
In January 2014, the Scottish Government announced a 6 per cent increase in pre-registration student nursing and midwifery intakes for the 2014/15 academic year. This follows a 4 per cent rise in 2013/14 (this equates to 2698 recommended training places for student nurses and midwives, up from 2530 in 2013/14). In February 2015, a further 3 per cent increase was announced for the 2015/16 academic year – a third successive rise.[98]
In February 2015, we also announced investment of £450,000 over three years to encourage former nurses and midwives back into the profession. This will enable around 75 former nurses and midwives to retrain each year and re-enter employment from April 2015.
The Scottish Government also worked with European Recruitment Services (EURES) and the Government of the Netherlands to promote NHSScotland as an employment option. EURES (UK) attended a medical careers fair in Amsterdam, returning with a number of expressions of interest in working within NHSScotland. The Scottish Government is building on this work as it continues to support NHS Boards’ efforts to recruit the staff they need.
Workforce Planning
Work to strengthen workforce planning began in 2014/15, with the Scottish Government working closely with NHS Boards through their Human Resource Directors to implement the recommendations of the Pan-Scotland Workforce Planning report.[99] Two data-quality improvement exercises were completed in 2014/15, resulting in more accurate data collection to better inform future workforce supply and demand forecasting. Midwifery and neonatal nursing sub-job family titles have been reviewed and staff have been re‑categorised, where appropriate, into the correct sub-job family; community nursing, particularly district nursing, health visiting and school nursing, has also been reviewed, with guidance prepared for users and staff being re-categorised where appropriate.
Further progress will be made in 2015/16 through the establishment of a Vacancy Short-life Working Group to look at workforce planning for Integrated Health and Social Care Partnerships and the establishment of a Workforce Observatory.
NHS Pay and Conditions
NHS Pay Review Bodies’ recommendations for 2015/16 have been implemented in full. This means that all NHSScotland staff on Agenda for Change pay points over £21,000 received a 1 per cent pay increase from 1 April 2015. Staff earning under £21,000 received a flat rate increase of £300. Executive and senior managers had a 1 per cent pay rise in line with other staff.
NHS Boards delivered an overall reduction in senior management posts of 437.0 WTE between 2010/11 and 2014/15: this reduction of 33.1 per cent exceeded the target by 8.1 percentage points.[100]
A new NHS pension scheme was introduced from 1 April 2015 following communication with all staff. The new scheme includes a later pension age and work on developing support for staff continues through the UK-wide Working Longer Review.
Together, these achievements improve efficiency and support staff in the continued delivery of quality services.
Sustainability and Seven-day Services
The aim of the Sustainability and Seven-day Services Programme is to ensure that people who require healthcare have timely access to high quality care whenever they need it, on a basis that is sustainable in the long term. The Sustainability and Seven-day Services Taskforce, which was established to drive this work, published an interim report in March 2015[101] that defined seven-day services, set out the Taskforce’s findings to date and clarified actions that would be undertaken in the next phase of work. The actions include a review of the 29 sites that undertake acute general surgery, considering new models for diagnostic imaging and interventional radiology, and looking at new models of care, such as community hubs.
The Scottish Government, NHS employers, staffside partners and healthcare professionals are working together in taking this forward, demonstrating commitment to a partnership approach in NHSScotland.
Workforce Integration
The workforce is vital to the successful delivery of integrated health and social care services and efforts to identify key workforce issues arising as a result of integration continue. As part of this, the second event in the successful Strengthening the Links series was held on 30 October 2014, with a focus on practical examples of workforce challenges.
This collaborative series of events forms a key part of continuous learning and networking processes around workforce issues. The events bring together those responsible for strategic human resources across health and social care, including representatives from the third and private sector, and staffside partners.
The Human Resources Working Group on Integration continued its work to address strategic-level workforce issues and advise on the practical human resource implications.
Youth Employment
NHS Boards continue to deliver against youth employment targets. Over the reporting year 2014/15, Boards created 96 new Modern Apprentice opportunities and delivered 3,050 new employment opportunities for young people (aged 16 to 24), making a positive contribution to building a sustainable workforce for NHSScotland.[102]
Over 8,000 opportunities have been offered to young people by NHS Boards over the past three years, with levels of activity measured through an annual survey. A new target of creating 500 Modern Apprenticeship opportunities between August 2014 and August 2017 was set for NHSScotland in the summer of 2014. Progress is being monitored and reported back to NHS Boards on a quarterly basis to manage delivery of the target.
eHealth
eHealth is the key to how information is accessed, used and shared within and across NHS Boards and with partner organisations to deliver integrated health and social care and, as such, is a prime enabler of the delivery of the 2020 Vision for Health and Social Care. eHealth supports patients and their carers to make informed decisions to manage their health and wellbeing and also enables health data to be used appropriately to improve the effectiveness of services and treatments and make significant advances in medical research.
The latest eHealth Strategy,[103] published in March 2015, was developed collectively with the support of NHSScotland Chief Executives. Current major strands of work include the use of portal technology to incrementally continue to build an Electronic Health Record (EHR) and make summary views from the EHR increasingly available to health and care professionals wherever and whenever they need them. These views will also be accessible across NHS Board boundaries. A Hospital Electronic Prescribing and Administration System was procured this year to enable NHS Boards to fill an important gap in the electronic information they hold (funded with an additional £1 million investment this year with further significant funding in following years as NHS Boards roll it out).
Another major strand of work that uses portal technology is progressively giving patients access to information held in the EHR so they can manage their health and wellbeing, order repeat prescriptions and book appointments online, and use secure two-way digital communication with their health and social care providers. Those with appropriate needs will also have access to a portfolio of proven technology enabled care solutions, such as Telehealth home-based health monitoring.
Significant initiatives this year include the Technology Enabled Care Programme, which aims to scale-up and embed Telehealth and Telecare solutions (funded with an additional £10 million annual investment over three years), and the Digital General Practice Programme that focuses on providing a broader and deeper set of digital services offered by GPs across Scotland (funded with an additional £2 million investment per year over three years).
Telehealth and Telecare
The NHS 24 Scottish Centre for Telehealth and Telecare continues to expand and embed digital health services across a number of NHS Boards. Innovations in mental health have been expanded to adults with mild to moderate depression and/or anxiety in a further four NHS Boards (NHS Shetland, NHS Grampian, NHS Lanarkshire and NHS Fife), transferring the learning from two early adopters in Scotland (NHS Forth Valley and NHS Tayside) and wider European experience.
MasterMind is a three-year European programme using clinically proven computerised Cognitive Behavioural Therapy (cCBT) to support a significant number of patient referrals from GPs and other mental health and care professionals. Provision of cCBT services aims to improve patient access to psychological therapies while providing additional treatment choice and early intervention. Commencing in January 2015, the trial has seen 1,117 patients start treatment up to the end of August 2015. MasterMind’s cCBT services are being delivered at home or in community locations such as libraries, supporting greater flexibility and accessibility for patients while enabling better targeting of specialist health resources.
Science and Research
Engagement with Leading Medical Research Charities to Co-fund Large-scale Research Projects and Fellowships
The Chief Scientist Office (CSO) co-funded six research projects and four clinical fellowships in 2014/15 with the following charities: Action Duchenne, Alzheimer’s Research UK, Breast Cancer Campaign, British Lung Foundation, MND Association, MND Scotland, Muscular Dystrophy UK, Pancreatic Cancer UK, Scottish Huntington’s Association and the Stroke Association.
The total amount of research funding made available through these collaborations was £3.2 million, with over 50 per cent being contributed by the third and private sector. A further four collaborations have been signed off and are awaiting announcement.
These collaborations are a vital component of CSO’s strategic aim of maximising research capacity in NHSScotland in areas of clinical importance and need. Increased effectiveness in health and social care depends on evidence gained from research, and this initiative helps build future research capacity within NHSScotland in a cost-effective manner.
NHS Research Scotland/Universities Scottish Senior Clinical Academic Fellowship Scheme
This new Clinical Academic Fellowship Scheme is funded jointly by the Scottish Government Health and Social Care Directorates, with universities playing a valuable role in providing medical training. The Scheme will recruit 15 senior fellows over a five-year period, with the first round advertised in January 2015.
Clinical academics are a valuable resource for Scotland and complement NHSScotland’s capacity-building activity. As university employees who spend at least half of their working week delivering and developing clinical services for the NHS, clinical academics undertake research that not only improves Scotland’s health and healthcare, but also drives economic growth. Without this scheme, there would be a significant risk that carefully nurtured early career clinical academics would be attracted to long-term career posts outside Scotland.
The Scottish Improvement Science Collaborating Centre
The Scottish Improvement Science Collaborating Centre (SISCC) is a Scotland-wide research initiative that aims to develop and promote evidence-based, integrated, sustainable ways of working in and across health and social care that consistently prioritise the needs of service users, carers and the public. It was established during 2014/15 and is being led by the University of Dundee and NHS Tayside through a collaboration involving eight universities and nine NHS Boards, national NHS and Social Care organisations, third and private sector and community groups, Local Authorities and the Scottish Government.
SISCC is supported by £3.75 million investment over five years from the Scottish Funding Council, Chief Scientist Office, NHS Education for Scotland and the Health Foundation, with matched investment from partner organisations.[104]
The Centre is building a large Scotland-wide collaboration that provides a firm foundation to support its mission to overcome the barriers that can exist between:
- research, practice and policy;
- acute and Primary Care;
- healthcare and public health;
- health and social care and the third sector;
- different professional groups; and
- those who provide services and those who use them.
Increasing Opportunities to Participate in Research for Patients in Scotland
The number of research study sites opened through NHS Research Scotland increased by 11.8 per cent over the preceding year, with the number of patients recruited to publicly funded research studies increasing by 4.6 per cent in the same period.[105]
Contact
Email: Andrew Wilkie