NHSScotland Chief Executive's Annual Report 2014/15
The NHSScotland Chief Executive's Annual Report 2014/15 presents an assessment of the performance of NHSScotland in 2013/14 and describes key achievements and outcomes.
Chapter 2: Delivering Outcomes for People – Our Story of Achievement
In future, the NHS will work with partners across the public sector to manage pressures and ensure the effective and efficient use of resources.
Gregor
To see Gregor’s story see the online report at: www.nhsscotannualreport.scot
This chapter sets out some of the achievements staff within NHSScotland and its partners have delivered during 2014/15. The achievements need to be seen in the context of the challenges faced over the winter,[6] including increased and prolonged pressures from influenza and respiratory illness (see Chart One).
Chart One: Weekly Emergency Inpatient Admissions with Respiratory Illness as a Primary Diagnosis, by Week 2010/11 to 2014/15
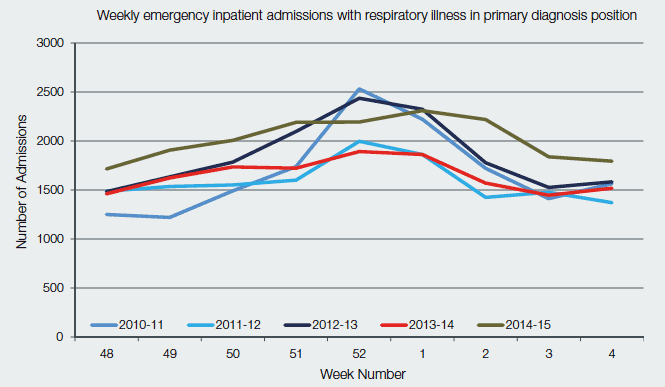
Source: ISD Scotland, provisional SMR01 data
The Scottish Government has taken steps to strengthen preparedness for winter 2015/16[7] which are based on integrating health and social care, the £100 million being invested to improve delayed discharge and the fresh approach to improving unscheduled care across Scotland – in winter and all year round – based on six essential actions.[8] Winter is defined here as the months of October to March, inclusive.
You can read more about our approach to improving unscheduled care across Scotland in Chapter 3 – Effective Care.
Capacity and Activity
Between March 2014 and March 2015, the NHSScotland workforce increased by 1,977.8 whole time equivalents (WTE) (or 1.5 per cent). This included an additional 224.8 WTE medical and dental consultants and 1,001.8 WTE nursing and midwifery staff (including interns).[9] In future, the NHS will work with partners across the public sector to manage pressures and ensure the effective and efficient use of resources.
NHS Boards plan and manage the number of acute medical beds required throughout the year to take account of seasonal pressures. The number of acute medical beds increased throughout this winter from 10,979 in quarter ending December 2014 to 11,275 in quarter ending March 2015 (excluding Highland, for which data is not available). This was on top of an increase of 149 between quarter ending September 2014 and December 2014.[10]
Chart Two: Premature Mortality, Under 75s Age-Standardised Death Rates per 100,000
Population for All Causes, 1994 to 2014
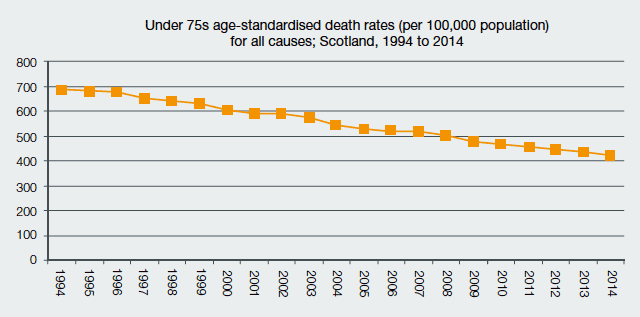
Source: National Records of Scotland
The number of calls answered by NHS 24 increased by 115,574, or 17 per cent, compared to last winter. This year’s increase may be partly attributable to the introduction of the free-to-call 111 number. Overall Scottish Ambulance Service emergency demand (by incidents) (Categories A, B and C)[11] increased by 17,499 (or 3.8 per cent) compared to last winter.[12]
Hospital activity was also at an increased level compared to winter 2013/14. Accident and Emergency (A&E) attendances were up 3,924, or 0.5 per cent; provisional emergency and transfer inpatient discharges up over 12,000, or 2.6 per cent this winter; and provisional elective inpatient and day case discharges up almost 1,500, or 0.5 per cent. Based on the most recently published information, the average annual increase in emergency admissions between 2009/10 and 2013/14 is 1.1 per cent.
Across Scotland, the rate of emergency bed days per 1,000 population aged 75 and over decreased significantly by a provisional 11.4 per cent, from 5,422 in 2009/10 to 4,805 in 2014/15, against the planned reduction of 12 per cent.[13]
Premature Mortality
Premature mortality (deaths among those aged under 75 years) has reduced substantially, down 23 per cent since 2004 to a death rate of 423 deaths per 100,000 population in 2014. Once again, some causes of premature mortality have seen a sharper fall during this time. Early deaths due to cancer – the leading cause of death – have reduced by 15 per cent over the last decade. Deaths due to heart disease and due to a stroke are each down by almost half, at 47 per cent and 46 per cent respectively, while deaths due to diseases of the respiratory system have reduced by 15 per cent (see Chart Two).
Cancer
Detect Cancer Early
There have been recent improvements in the early detection of cancer, the biggest cause of early death (under 75 years) in Scotland. The sooner that cancer is diagnosed and treated, the better the survival outcomes. In the combined calendar years of 2013 and 2014, 24.7 per cent of lung, breast and colorectal cancers were diagnosed at the earliest stage, an increase of 6.5 per cent on the baseline combined calendar years of 2010 and 2011.[14]
Cancer Waiting Times
Over 2014/15, NHSScotland also continued to deliver shorter waits for specific procedures.[15] While the 31 Day Decision to Treat to Treatment cancer waiting time Standard was met in each of the quarters in 2014/15, some challenges remain for the 62-day urgent referral with suspicion of cancer to treatment waiting time measure. In the period January to March 2015, 96.5 per cent of patients began cancer treatment within 31 days of a decision being taken to treat and 91.8 per cent of patients began cancer treatment within 62 days of urgent referral with suspicion of cancer. For each measure, the national standard is 95 per cent. You can read more about our approach to the early detection and treatment of cancer in Chapter 3.
For the financial year 2014/15 (using data from 2014 Quarters 2, 3 and 4, and 2015 Quarter 1), 93.8 per cent of patients began cancer treatment within 62 days of urgent referral with suspicion of cancer. The corresponding figure for 2013/14 for the 62-day standard was 93.1 per cent. The 31-day standard was met in both of the financial years.
The Scottish Government continues to work with NHS Boards to ensure prospective management information is used for the proactive scheduling of patient diagnosis and treatment.
Smoking
The proportion of adults who smoke cigarettes declined from 31 per cent in 1999 to 20 per cent in 2014.[16] The decline between 2013 and 2014, from 23 per cent to 20 per cent, is the sharpest year-on-year reduction over the series (see Chart Three).
Although the pattern is broadly similar to that of previous years, prevalence has reduced in all deprivation quintiles[17] in the last year, most notably from 39 per cent to 34 per cent in the 20 per cent most deprived areas.
Of 39,746 quit attempts made with the support of NHSScotland smoking cessation services, in the most deprived areas of Scotland in 2014/15, 7,017 were still not smoking at three months, a ‘quit rate’ of 18 per cent.[18] This represents 58 per cent of the NHSScotland HEAT target to achieve at least 12,005 three-month quits in the most deprived areas.
The number of quit attempts made with the support of NHSScotland smoking cessation services has dropped by 39 per cent since 2012. The reason for this decrease is not completely clear, but the rise in use of electronic cigarettes as an alternative to smoking is possibly part of the explanation.
The Scottish Health Survey 2014 report[19] shows that just under two-thirds (64 per cent) of recent ex‑smokers and current smokers who had attempted to quit said they used a nicotine replacement therapy (NRT) product or e-cigarettes in a recent quit attempt. The most common items used as part of a recent quit attempt were nicotine patches (36 per cent) and e-cigarettes (32 per cent).
Chart Three: Estimated Prevalence of Smoking; Scotland 1999 to 2014
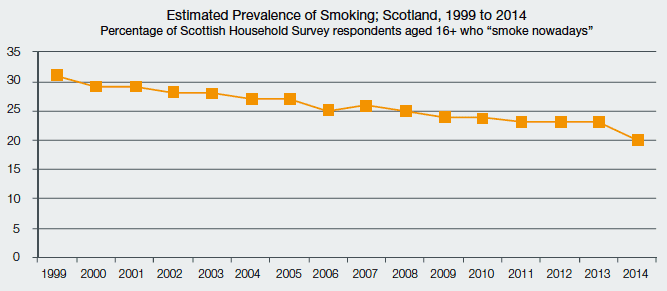
Source: Scottish Household Survey, 2014; [“Do you smoke cigarettes nowadays?”]
Alcohol
The Scottish Health Survey 2014 report shows that prevalence of drinking outwith the government guidelines for weekly and/or daily drinking declined significantly from 2003 to 2014, both for men (from 53 to 46 per cent) and women (from 42 to 36 per cent).[20]
Alcohol Brief Interventions (ABIs) contribute to the Scottish Government’s overall objective of reducing alcohol-related harm by helping individuals to cut down their drinking. In 2014/15, NHSScotland delivered almost 100,000 Alcohol Brief Interventions to help prevent the increased morbidity, mortality and social harm that result from excessive alcohol consumption.[21]
You can read more about our approaches to reducing smoking and alcohol consumption in Scotland in Chapter 4.
Eighteen Weeks Referral to Treatment
When NHS treatment is needed, shorter waiting times lead to earlier diagnosis and better outcomes, minimising unnecessary worry and uncertainty for patients.
The 18 Weeks Referral to Treatment (RTT) standard does not focus on a single stage of treatment, such as the time from referral to first outpatient appointment, or the time from being added to the waiting list until treatment starts: the 18 weeks standard applies to the whole pathway from referral up until the point where each patient is actually treated. This means that the RTT is dependent on stage of treatment and diagnostics performance.
For the financial year 2014/15, 88.9 per cent of almost 2.5 million patients (2,491,898) were seen within 18 weeks of referral to treatment (against a standard of 90 per cent). The corresponding figures for 2013/14 showed that 90.5 per cent of 2,479,708 patients were seen within 18 weeks of referral.[22]
Treatment Time Guarantee
The Scottish Government continues to support NHS Boards to deliver the 12 weeks legal treatment time guarantee for inpatient and day cases set out in the Patient Rights (Scotland) Act 2011. The legal guarantee is that patients requiring inpatient and day case treatment must be treated within 12 weeks from the patient and consultant agreeing to such treatment.
There were increased challenges over the winter, with NHS Boards reporting that they were experiencing increased levels of cancellations for routine treatment. Over 316,000 inpatients and day cases have benefited from the 12 weeks legal treatment time guarantee in 2014/15, meaning that 96.5 per cent of patients were seen within 12 weeks. The corresponding figures for 2013/14 showed that 97.8 per cent of patients were seen in 2013/14 with over 337,000 patients benefiting from the 12 weeks legal Treatment Time Guarantee.[23]
The Scottish Government has announced its intention to invest £200 million to build six new elective treatment centres at Aberdeen Royal Infirmary, Edinburgh Royal Infirmary, St John’s Livingston, Ninewells Hospital in Dundee, Raigmore Hospital in Inverness, and a new centre at the expanded Golden Jubilee National Hospital. This network of new centres will address changing demographics over the next 20 years, and the likely increased demand in hospital care from a growing elderly population. It is expected that the new facilities will be completed and delivered by 2021.
Outpatients
On 31 March 2015, 92.2 per cent (236,079) of new outpatients had been waiting 12 weeks or less for a first outpatient consultation. The corresponding figure on 31 March 2014 is 96.9 per cent, with 233,098 new outpatients waiting 12 weeks or less.
A number of NHS Boards have experienced capacity issues in relation to outpatient waits across a number of specialties. To help improve performance we have announced the Delivering Outpatient Integration Together (DO IT) programme to support delivery and identify sustainable solutions. The programme will be focusing firstly on redesigning dermatology and gastroenterology services, particularly for follow-up appointments, as well as optimising use of technology before moving on to all outpatient services. The Scottish Government has made available an additional £2.7 million in 2015/16 specifically to address outpatient waits, with the objective of achieving 95 per cent of outpatients seen within 12 weeks in 2016/17.
Drug and Alcohol Treatment – Referral to Treatment
Those needing treatment to help tackle problem drug and alcohol use benefited from NHSScotland support, with 95 per cent of the 11,881 people beginning treatment within three weeks of referral during January to March 2015.[24] For alcohol treatment, 95.7 per cent of 7,544 people waited three weeks or less between January to March 2015, and for drug treatment, 93.9 per cent of 4,337 people waited three weeks or less in the same quarter.
In Vitro Fertilisation Waiting Times
Improving access to In Vitro Fertilisation (IVF) by reducing waiting times for patients will potentially improve the chance of a successful outcome from the treatment and will increase equity so that all those eligible for NHS IVF will have a waiting time of 12 months or less. During the quarter ending March 2015, 397 eligible patients were screened at an IVF centre in Scotland.[25] Of these, around 96 per cent of eligible patients were screened for IVF treatment within 365 days (12 months). This compares to 80 per cent in the quarter ending December 2014. The Scottish Government target for IVF waiting times is that the target should be delivered for at least 90 per cent of patients, as for some patients, it may not be clinically appropriate for treatment to begin within the target’s time.
Child and Adolescent Mental Health Services and Psychological Therapies Waiting Times
Timely access to healthcare is a key measure of quality that applies equally in respect of access to mental health services. Early action is more likely to result in full recovery and, in the case of children and young people, will minimise the impact on other aspects of their development such as education, so improving their wider social development outcomes.
Demand for services has increased significantly. We have seen an increase in demand for mental health services through better identification of those requiring treatment, better diagnosis and more people being prepared to come forward. In addition, waiting times have decreased significantly despite a rise in the number of people seeking help.
During the quarter ending March 2014, 3,601 children and young people started treatment at Child and Adolescent Mental Health Services (CAMHS) in Scotland and 83.9 per cent were seen within 18 weeks. During the quarter ending March 2015, 4,269 children and young people started CAMHS treatment, an increase of 18.6 per cent on the same period last year. Of these, 78.9 per cent were seen within 18 weeks.[26]
During the quarter ending March 2015, around 11,659 patients started their treatment for psychological therapies in Scotland, an increase of 2,253 people or 24.0 per cent on the same period in 2014. Of these, 82.8 per cent were seen within 18 weeks.[27]
The Scottish Government will continue to work with NHS Boards to support Boards to improve waiting times for mental health services and deliver the HEAT standard of 90 per cent of patients being seen within 18 weeks. To that end, the Scottish Government committed to invest an extra £100 million in mental health over the next five years. This funding will be targeted at improving access to services, supporting responses to mental health in Primary Care, promoting wellbeing through physical activity, and improving patient rights, one of the elements of the Mental Health (Scotland) Bill.
Hospital Standardised Mortality Ratios
As well as providing timely access to services, it is also vital that NHSScotland delivers the highest standard of quality and safety when providing treatment. Hospital Standardised Mortality Ratios (HSMR) compare observed deaths to predicted deaths. The Hospital Standardised Mortality Ratio for Scotland has decreased by 15.7 per cent between October to December 2007 and January to March 2015.[28] Overall, hospital mortality at Scotland level had been falling prior to the baseline period.
The Scottish HSMR for January to March 2015 is currently 0.90. Compared to an index of 1.0, this means there were 10 per cent fewer deaths than predicted in the period. Hospital mortality has fallen for all types of admission; non-elective medical patients consistently account proportionately for the majority of deaths within 30 days of admission. Patients from the least deprived areas of Scotland consistently have lower levels of crude 30-day mortality than those from more deprived areas.
Clostridium difficile
For the year ending March 2015, the rate of identifications of Clostridium difficile (C.diff) across NHSScotland was 0.34 per 1,000 occupied bed days among patients aged 15 and over, maintaining the improvement seen in previous years. The standard NHSScotland was aiming for was a rate of 0.32 cases or less per 1,000 total occupied bed days among patients aged 15 and over (see Chart Four).
Chart Four: Clostridium difficile Rates Amongst Patients Aged 65+ per 1,000 Total
Occupied Bed Days, Year Ending March 2008 to Year Ending March 2015
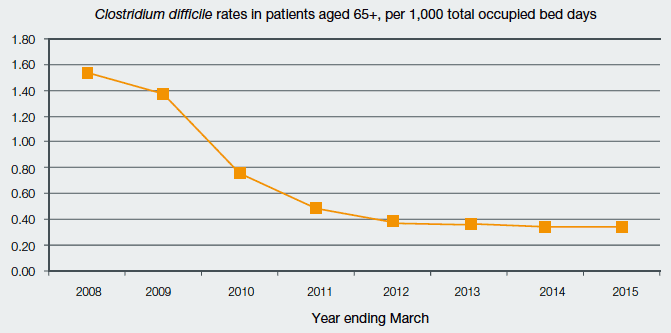
Source: Health Protection Scotland: Quarterly Epidemiological Commentaries – Clostridium difficile infection (CDI) and Staphylococcus aureus bacteraemias (SAB)
Staphylococcus aureus bacteraemia
Recent improvements in methicillin-resistant Staphylococcus aureas (MRSA), methicillin-sensitive Staphylococcus aureus (MSSA) and new Staphylococcus aureus bacteraemia (SAB) were sustained.
For the year ending March 2015, the rate of MRSA/MSSA cases across NHSScotland was 0.31 per 1,000 acute occupied bed days. The standard NHSScotland was aiming for was a rate of 0.24 cases or fewer per 1,000 acute occupied bed days (see Chart Five).
Accident & Emergency (A&E) Activity and Waiting Times
NHSScotland has again worked hard to tackle A&E waiting times over the past year. Increased and prolonged pressures over winter contributed to the reduced whole system four hour A&E waiting times performance in December, January and February. This winter, performance in Scotland[29] (88.8 per cent) was marginally above that in England[30] (88.2 per cent) and significantly above the performance in Northern Ireland[31] (72.4 per cent) and Wales[32] (79.3 per cent), based on ‘core’ (Scotland), ‘Type 1’ (England and Northern Ireland) and ‘Major’ (Wales) A&E. This is different from winter in the previous year, where England’s performance was marginally above that of Scotland.
Chart Five: Rates of Staphylococcus aureus bacteraemia (SAB) infections per 1,000
Acute Occupied Bed Days, Year Ending March 2006 to Year Ending March 2015
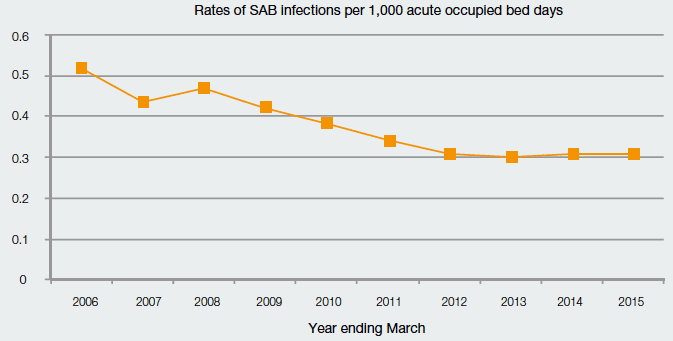
Source: Health Protection Scotland
The National Unscheduled Care Action Plan, which was previously launched in 2013, has now moved to an improvement-orientated approach to sustainability improving unscheduled care, focusing on six essential actions. This new approach was launched in May 2015 and is a two‑year programme aiming to improve outcomes for people who are using services. The programme recognises, however, that this is a multi-disciplinary issue requiring commitment across every part of the health and social care system to ensure better care on a sustainable basis, joining up several work strands to ensure a much more strategic approach. Integration of health and social care is therefore at the heart of the solution to the problems of unscheduled care. Strategic planning across the whole pathway of care – health and social care – is being taking forward under integration.
A new website, NHS Performs,[33] was developed to bring together information on how hospitals and NHS Boards are performing. It includes new statistics on weekly A&E waiting times, monthly delayed discharges and cancellations. NHS Performs will be developed further during 2015/16.
Delayed Discharge
Tackling delayed discharge is one of the Scottish Government’s key priorities for NHSScotland in improving the quality and experience of care and people’s outcomes. Joined up health and social care will allow people to be timeously discharged and receive care at home or in a homely setting.
In January 2015, a £100 million investment over three years was announced to help local partnerships to tackle the issue of delayed discharge. During the quarter January to March 2015, 151,098 bed days were occupied by delayed discharge patients.[34] This represents a reduction of 10 per cent compared to the previous quarter (168,526 during the quarter October to December 2014), but an increase of 2 per cent compared to the equivalent quarter in 2014 (148,079 during the quarter January to March 2014). At the April 2015 census, 357 patients were waiting over 14 days to be discharged from hospital. By comparison, at the January 2015 census, 517 patients were delayed and 418 were delayed at the April 2014 census.
Contact
Email: Andrew Wilkie