National health and social care workforce plan: part three
Part three of the plan sets out how primary care services are in a strong position to respond to the changing and growing needs of our population.
Chapter Five: Planning and Developing the Multidisciplinary Workforce – General Practitioners
- The new GP contract will deliver an enhanced role for the GP focused on complex care, undifferentiated illness and clinical leadership.
- There will be a reduction in GP workload pressures and responsibilities through service redesign.
- At least 800 (headcount) additional GPs will be added to the workforce over the next 10 years to meet increasing patient demand.
- A comprehensive package of retention measures will be put in place to support GPs, including during the first five years and towards the end of their careers.
- There will be enhanced support for GPs working in remote and rural areas.
- There will be enhanced support and encouragement for GPs working in the OoHs period
- On-going expansion of medical school and training places will help grow the GP workforce.
- The establishment of an Increasing Undergraduate Education in Primary Care Working Group to consider ways of increasing undergraduate education in primary care settings, which will help facilitate future careers in general practice.
- A marketing and recruitment campaign will promote Scotland as a great place to work as a GP.
Introduction
The GP has been at the heart of the health care system since the establishment of the NHS in 1948. Working within MDTs and wider community services, GPs manage the widest range of health problems, addressing multimorbidity, coordinating long-term care and addressing the physical, social and psychological aspects of patients' wellbeing.
The context under which GPs operate has changed significantly in recent years, with an ever more important role as clinical leaders in deciding how health services should be organised to deliver safe, effective and accessible care to patients in their communities within an increasingly integrated health and care system.
This evolving role formed the basis of the recent negotiation of the new GP contract between the Scottish Government and the BMA. The negotiations were guided by Barbara Starfield's "four Cs" of primary care [91] , namely that GPs are uniquely able to deliver:
- Contact – accessible care for individuals and communities;
- Comprehensiveness – holistic care of people – physical and mental health;
- Continuity – long term continuity of care enabling an effective therapeutic relationship;
- Co-ordination – overseeing care from a range of service providers.
These four pillars of primary care are also evident in the landmark Royal College of General Practitioners ( RCGP) report on Medical Generalism [92] . The ethos of generalism described in this report includes comprehensiveness, co-ordination and continuity. Generalism, by definition, is a form of care that is person - not disease - centred. It is precisely the type of medicine needed to meet the challenge of shifting the balance of care, realising Realistic Medicine [93] , and enabling people to remain at or near home wherever possible.
The new GMS Contract articulates a refocused role for GPs as Expert Medical Generalists ( EMGs). This recognises the GP as the senior clinical decision maker in the community, who will focus on:
- undifferentiated presentations;
- complex care in the community;
- whole system quality improvement and clinical leadership.
Expert Medical Generalists will ensure strong connections to, and coordination with, the enhanced primary care team, health and social care community based services and with acute services where required. Better coordination of patient care, including greater access to the right professional at the right time, will deliver improved patient outcomes and a more proportionate use of resources.
The role of the GP as an EMG can only be achieved if they have the capacity to develop this leadership role. We have set out in Chapters three and four how we will deliver enhanced MDTs to support comprehensive service reconfiguration in primary care. This chapter describes how we will support and retain our current GP workforce through a comprehensive package of support measures, while expanding the number of GPs working in Scotland by at least 800 (headcount) over the next decade.
Supporting and retaining the existing workforce
We recognise the pressures GPs are under due to changing demographics and the expectations of patients. The Cabinet Secretary for Health and Sport announced in December 2017 a comprehensive package of measures to retain and support the GP workforce:
- Mentoring – embarking on any career can be challenging and stressful and we know that young GPs want more portfolio type careers and a better work/life balance. GPs within their first five years will be offered mentoring support from experienced GPs as growing evidence suggests this may be an effective component to retaining GPs in workforce [94] .
- Continued Professional Development ( CPD) – heavy workloads can mean opportunities for CPD are limited. The new GMS Contract recognises this and will provide practices with resources to support 1 session per month for Professional Time Activities. Further support is being offered to GPs in first five years of their career.
-
Coaching – Research demonstrated that professional coaching can be successful in turning around intention to leave the profession.
Table 6: Pre- and post- coaching 'likelihood of leaving the profession' ratings [95]
Pre-coaching
(base 51)Post-coaching
(base 28)Average 'leave' rating 7.2 4.9 7 or above 74.5% 32% 4 to 6 23.5% 21% 3 or below 2% 46% Note: where 1 = highly unlikely to 10 = highly likely
The aim of the coaching programme is to help GPs develop their resilience and develop ways of self-management to combat burnout. Such a scheme is already operating successfully in NHS Lanarkshire. We intend to build on this success and offer a national coaching service across Scotland with an initial aim of providing four sessions of professional coaching to 100 self-identified GPs.
- Staying in practice scheme ( SIPS) – we are revising and extending the current retainer scheme (which is currently limited to those with caring responsibilities). The aim is to widen access to scheme to those who are considering leaving general practice early due to workload pressures.
- Support for GP appraisal – GPs undertake appraisal annually, and this is an important part of staying up to date, ensuring high quality patient care and is a route to GMC revalidation. However, some GPs report that they find the preparatory work for appraisal burdensome and bureaucratic. Working with NES, we will provide funding for tailored appraisal support to GPs who wish it through a series of workshops. The workshops will support the individual needs of the GP, for example, the challenges some GPs experience navigating the appraisal website or the articulating reflective component of CPD and Quality Improvement activities.
Support for rural GPs
We recognise that there are particular challenges in attracting and retaining GPs and other health professionals to Scotland's remote and rural communities. Along with the BMA we have committed to setting up a Rural Short Life Working Group which will support the implementation of the new GP Contract in rural areas. This will support the sustainability of remote and rural practices in particular for very small practices in remote areas.
An additional package of measures to support rural GPs includes:
- Scottish Rural Medical Collaborative – we will build on the current work of the collaborative to help target and tailor support to primary care services in remote and rural areas. It is anticipated that this may include a mentoring scheme for rural GPs, recruitment policies tailored for rural and remote areas, development of an overarching recruitment strategy, rural deprivation preference bursary to coach rural students prior to medical school application, including work experience.
- GP for GP – many very remote and rural GPs and their families have difficulty accessing routine general medical services, due to geography, remoteness or distance from registered GP. The NHS Highland GPs for GPs scheme, which has been running since 2003, provides a confidential service to rural GPs and their families at times of stress or illness, when they may have difficulty going to their own GP. In the past it has supported Highland GP's with problems such as stress, depression, inability to cope, and bereavement. We will extend this scheme to provide support for a greater number of remote and rural GPs across Scotland. This service is provided in addition to the GP Occupational Health Service which is available to all GPs and practice staff. The GP for GP scheme may refer or suggest self-referrals to the GP Occupational Health Service.
- Relocation package – we will encourage GPs to come and work in rural practices by offering an enhanced relocation package. The current scheme will be extended from a maximum of £2,000 to £5,000 to cover expenses such as removal costs, rent, etc. and we will widen the eligibility criteria from 44 Island practices to 160 remote and rural practices across Scotland.
- Golden Hello – to reflect the need to support sustainable rural services we will substantially expand the existing Golden Hello scheme from 44 to 160 practices in rural and remote areas, offering £10,000 for GPs taking up post in their first eligible rural practice.
Expanding the GP workforce
We know demand on primary care services will inevitably rise given increasing levels of multimorbidity from an ageing population and our strategic goal of shifting care from hospitals to community and home or homely settings. This requires a GP workforce that is both sufficient to meet demand but also flexible enough to address changing needs. As set out above, the new GMS contract is an important step in beginning to address workload issues by eliminating unnecessary bureaucracy, reducing and streamlining the number of services that GP practices provide, and expanding and reconfiguring the primary care MDT.
But we recognise the need to go much further. We are able to estimate the number of GPs likely to be in the workforce over the next 10 years by modelling the age and gender of the current workforce, the number that typically leave and join the profession on an annual basis (whether new GPs completing training, flows in and out of Scotland, retirement, etc.) and taking account of increased part-time working.
Using data from the past five years we estimate that the number of GPs will remain broadly stable up to 2027. There is currently limited evidence that the GP workforce will contract significantly in the next decade, although this is difficult to assess with any degree of certainty and is based on a number of assumptions ( e.g. that current rates of part-time working will remain uncharged). What does appear clear however is that the current workload issues are being driven by ever increasing demand of an ageing population rather than a significant reduction in GP capacity.
Figure 14: Forecast GP numbers to 2027 [96]
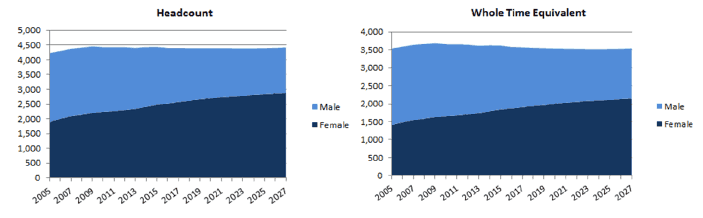
The anticipated stability in the size of the GP workforce is not sufficient to meet increasing demand, estimated to increase at around 1% annually. We are therefore committed to a package of measures to ease the pressure on GPs, both in terms of support to retain those that may be considering leaving the profession and in promoting general practice as an excellent career choice, both for those considering a career in medicine and those currently training to be a doctor.
In December 2017 the Cabinet Secretary for Health and Sport committed to expanding the GP workforce by at least 800 GPs (headcount) over the next 10 years. We recognise the need for both short and longer-term initiatives to address current GP shortages and that there are no simple solutions to expanding the workforce. We need to be realistic on what can be achieved, and by when, but our commitment to increase GP capacity within primary care is clear. This commitment will require constant monitoring and review, based on better quality data (see Chapter seven).
Medical education and training
The Scottish Government is implementing and developing a range of medical education and training initiatives to increase the sustainability of the current and future workforce in Scotland. A number of strands of work are being taken forward and will address each stage of the GP career pathway set out below.
Figure 15: Medical education and training pipeline
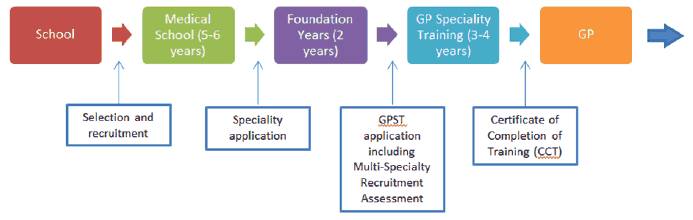
(i) The Medical Education Package
The medical education package is a £23 million investment in undergraduate medical education. As part of that investment the Scottish Government increased the number of medical undergraduate places by 50 in 2016, and this increase was sustained for 2017 and will be again for 2018.
In addition, Scotland's first Graduate Entry Medical programme ( ScotGEM) will commence in autumn 2018 adding a further 55 medical school places. The programme will be delivered by the medical schools in Dundee and St. Andrews in collaboration with the University of Highlands and Islands. This exciting new course focuses on primary care and remote and rural working offering immersive experience and aiming to attract students into these career paths.
The Scottish Government will pay the tuition fees of Scots domiciled and EU students who are accepted onto ScotGEM in order to offer as attractive a financial package as possible. Through ScotGEM we are also testing innovative retention methods. The Programme will also offer a 'return of service' bursary to all ScotGEM students. The scheme, to be administered by NHS Education for Scotland, will offer ScotGEM students a bursary of £4,000 per student per annum in return for a year of service up to a maximum of four bursaries and four equivalent years of service. We will evaluate ScotGEM over the short and long term, paying particular attention to the effectiveness of the return of service bursary and the numbers of ScotGEM graduates choosing a GP career.
(ii) Widening Access
As well as increasing capacity within medical schools, we are widening participation in medicine by promoting applications from talented young people from socially and geographically disadvantaged situations. The 50 places added in 2016, for instance, are targeted at students from the most deprived 20% of Scotland's, as measured by the Scottish Index of Multiple Deprivation ( SIMD).
The Scottish Government funded two new pre-medical entry courses at Glasgow and Aberdeen Universities, which commenced in autumn 2017. These courses support 40 places for pupils from less socially advantaged backgrounds to better prepare to undertake undergraduate medicine. This initiative supports key recommendations set out in the Report of The Commission for Widening Access, including a target that by 2030 students from the 20% most deprived backgrounds should represent 20% of entrants to higher education in Scotland. The programmes are also identifying school pupils from rural backgrounds who because of the size of their schools may experience disadvantage; this is an important part of the rural pipeline.
(iii) Proposed further action on medical school places
Part 1 of the National Workforce Plan committed to adding a further 50-100 undergraduate medical school places over the course of this Parliamentary term. These places will be awarded on a commissioning basis in line with strategic objectives which include significantly increasing the GP workforce. In order to attract as many young doctors into general practice as possible the Scottish Government has asked in particular for proposals which increase the percentage of clinical teaching that takes place in general practice to at least 25% of the clinical curriculum. It has also asked for proposals which ensure that all students are regularly selected, taught and/or assessed by GPs from the beginning of first year. The successful bids will be announced shortly.
Wider measures to increase exposure to primary care at undergraduate level
There is a clear need to address negative perceptions of careers in general practice. The RCGP's Destination GP report found a majority of students (91%) believe their peers hold negative views about general practice, and that they are most likely to associate the profession with being "boring", "lower status than other medical professions" and "less intellectually challenging" [97] . Research from the UK and abroad shows that exposure to general practice has a positive influence on students considering general practice as a career [98] . The RCGP has also found clinical placements in other specialities are particularly likely to expose students to negative views of general practice [99] . Equally, evidence demonstrates that medical students' perception of their GP teachers' job satisfaction positively affects their wish to become GPs [100] .
Currently some Scottish Universities teach as little as approximately a tenth of their clinical curriculum in primary care. Despite GPs comprising around 27% of the medical workforce, the UK's academic GPs account for only about 6% of all clinical academics [101] . We recognise that increasing clinical teaching in primary care and by primary care practitioners brings with it a number of complex challenges for medical schools and the Service and we do not underestimate these. As noted, these include the need to increase the number of GP educators and issues around competing demands on GP practice's time and around ACT funding and infrastructure. Under the joint auspices of the Scottish Government and the Board for Academic Medicine, we have establishment an Increasing Undergraduate Education in Primary Care Working Group, chaired by Professor John Gillies. It will consider ways of increasing undergraduate education in primary care settings, within a challenging but realistic timescale.
Post Graduate Medical Training
In 2016, as part of our programme to grow the numbers of graduates entering General Practice Specialist Training ( GPST), 100 additional posts were introduced in Scotland, coupled with a further round of recruitment to maximise the number of posts filled. In recognition of yearly recruitment data and trainee feedback indicating persistent problems in filling unpopular four-year GPST posts where the 4 th year of training is spent in hospital based posts, the Scottish Government asked NHS Education Scotland to reconfigure the balance of 3 and 4 year training programmes to prioritise 3 year rotations which maximised educational quality and ensured these posts met the curricular requirements. These measures will contribute towards making unpopular GPST posts more attractive options for potential trainees and help improve overall fill rates. Work to phase out educationally poor posts in favour of high quality 3 year rotations will continue in 2018 and 2019.
In tandem, to promote General Practice as an attractive career choice, a one-off bursary of £20,000 is available to trainees in posts that historically have found it more difficult to recruit including the Scottish National Rural Track Programme posts. The bursary payment is made to trainees as a lump sum on taking up the post and in return they agree to complete the three year placement in that location. If the trainees leave before completing three years they then have to repay the bursary.
Preliminary assessment of this initiative has shown there is a more even distribution of trainees, away from central areas and towards some harder to fill posts in rural areas.
To assist with increasing the number of doctors choosing a career in general practice we intend to offer additional support to foundation level doctors keen to undertake GPST. Where candidates have been unsuccessful in the GPST selection process, we would like to offer a 1 year development post with tailored support to equip individuals for re-application for subsequent GPST recruitment. A financial incentive would be offered to GP Trainers for supporting these candidates during their development post. We are in the process of gauging interest from previously unsuccessful GPST candidates in such a scheme.
Shape of Training
The Scottish Government is also committed to implementation of recommendations arising from Professor Sir David Greenaway's Shape of Training: Securing the future of Excellent Patient Care review [102] as outlined within the report of the UK-wide Shape of Training Review Steering Group published in August 2017. Many of these recommendations align with the transformational plans already set out by the Scottish Government. In relation to GP training, the commitment is to develop an enhanced training model in which qualified GPs are offered a further year of training to furnish them with additional skills. It is clear that the development of additional skills must be responsive to local provider and patient needs and complement the Expert Medical Generalist role, particularly the increasing delivery of complex care in the community. It is also evident that there is a clear desire by many GPs to enhance their skills and experience complementary to their Expert Medical Generalist role, which facilitates a portfolio career. Against that background there are a number of formats which a further optional year of post CCT training or development could take and in conjunction with key stakeholders, including the BMA and RCGP, we will continue to develop and test a variety of options.
Additional measures to increase GP numbers
(i) Marketing and recruitment campaign
Scotland has a lot to offer its GPs – no bureaucratic Quality Outcomes Framework ( QOF), no clinical commissioning and a new GMS Contract that refines and focuses the role of the GP as an Expert Medical Generalist and clinical leader of an expanded MDT. Patient satisfaction is consistently high with 87% rating the overall care provided by their GP practice as good or excellent in 2015-6 [103] . Scotland is also blessed with natural beauty and a vibrant and tolerant culture, and is an excellent place to bring up a family.
We must do more to make the best use of these assets and promote Scotland as a great destination for GPs to relocate. We will therefore launch a GP marketing and recruitment campaign during 2018 to increase the number of GPs who wish to work in Scotland from the rest of UK and overseas. The aim of the campaign will be to improve the way we market abroad the opportunities to work in NHS Scotland, improved the use of SHOW website, and to build better targeted and more effective advertisement of Scottish jobs in England and elsewhere.
We will look at opportunities to employ a recruitment agency to work run alongside the marketing campaign. Scottish recruitment agencies are already working with individual health boards to attract GPs to Scotland; working at scale will offer additional advantages and better value for money. This could include access to databases, recruitment events, headhunting, support and pastoral care during and after recruitment. We will ensure consistency and coordination with the planned marketing campaign to attract nurses to work in NHS Scotland.
(ii) Exploring ways to enable doctors to switch specialities
At present most registrars / consultants who wish to become GPs are required to undertake the full three year GP training. This is perceived as a barrier to moving into general practice. We propose working with NES and others to consider ways in which this route to general practice could be better supported. This can be achieved but needs a substantial amount of work to be put in place by 2019.
Conclusion
We recognise the workload challenges currently facing our GPs and the need to expand both GP numbers and the wider MDT that will help deliver the aspirations set out in the new GMS Contract. Our intention to increase GP numbers by at least 800 (headcount) over ten years is ambitious, but our assessment is that it is achievable through a range of measures targeted at every stage from medical school through to late career. It is an essential component of building a strong and sustainable primary care system which will continue to serve as the bedrock of the NHS in the years ahead.
Contact
Email: Naureen.Ahmad@gov.scot