National health and social care workforce plan: part three
Part three of the plan sets out how primary care services are in a strong position to respond to the changing and growing needs of our population.
Chapter One: Setting the Context
Introduction
Primary Care in Scotland: A definition from the professionals [8]
Most of the time, people use their own personal and community assets to manage their health and wellbeing and achieve the outcomes that matter to them. Primary care professionals enhance this by providing accessible health care and support to individuals and families in the community, when it is needed, at whatever stage of life.
Primary care is provided by generalist health professionals, working together in multidisciplinary and multiagency networks across sectors, with access to the expertise of specialist colleagues. All primary care professionals work flexibly using local knowledge, clinical expertise and a continuously supportive and enabling relationship with the person to make shared decisions about their care and help them to manage their own health and wellbeing. Primary care is delivered 24 hours a day, 7 days a week. When people need urgent care out of core service hours, generalist primary care professionals provide support and advice which connects people to the services they need, in a crisis, in a timely way.
Scotland's health is improving, driven by the skill and dedication of the NHS workforce and the bold measures taken on public health since the establishment of the Scottish Parliament in 1999. We are now living longer, healthier lives with a marked reduction (by over a third) in premature mortality between 1994 and 2015 (including significant falls in premature deaths caused by cancer, coronary heart disease, and cerebrovascular disease) [9] .
Despite pressure on services, patients are highly positive of their experience of the health service, with 83% of people rating the overall care provided by their GP practice as good or excellent in 2017-18 [10] . Of those who needed an urgent appointment, 93% were offered one within 48 hours, an increase from 91% in 2015-16. As figure 1 shows, people were also highly positive about their experiences of person-centred care at their GP practice, with positive ratings typically around or over 90%. Overall ratings for care from out of hours services were similar to those for the GP practice at 83%. These are achievements of which the primary care workforce should be rightly proud.
Figure 1: Patient experience, 2017-8
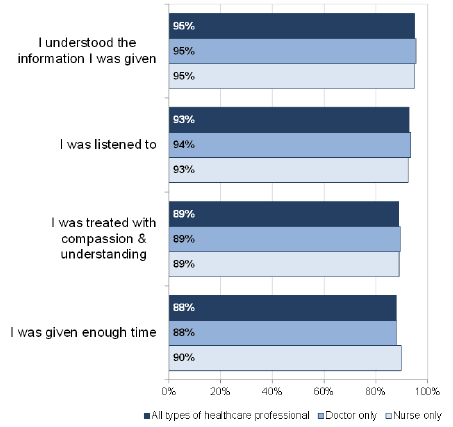
Challenges facing primary care
We are aware however, that as across the UK and internationally, demand on our primary care and social care services is steadily increasing due to a combination of an ageing population and rising levels of multi-morbidity [11] . The number of people aged 65 and over is estimated to increase by around 60% from 0.93 million to 1.48 million by 2039 [12] , leading to substantial rises in a range of long-term conditions [13] . Patients are also demanding more from their healthcare professionals: they rightly expect higher standards of care, more information about their treatment, more involvement in decisions about their care and improved access to the latest treatments [14] .
People with long-term conditions already account for about 50% of GP appointments [15] , placing significant and increasing strain on services. Evidence also demonstrates that people with co-existing physical and mental health problems often have longer hospitalisations, treatment failure, poor quality of life and premature mortality. As we said in the Mental Health Strategy for 2017-2027 [16] , our guiding ambition is that we must prevent and treat mental health problems with the same commitment, passion and drive as we do with physical health problems.
The benefits of a strong and integrated primary care system
Whilst our workforce has continually adapted and innovated to meet an increasing and more complex workload, maintaining consistently high standards of care and treatment has become more difficult to sustain. There is growing consensus that the NHS needs to focus more on the development of preventative models of care (including self-management), rather than reactive management of patients with long term conditions to be financially sustainable, tackle persistent health inequalities, improve long-term outcomes and to reduce pressure on the workforce. This calls for a modernised healthcare system as set out in the Chief Medical Officer's ground-breaking reports Realistic Medicine and Realising Realistic Medicine [17] . Realistic Medicine puts the person at the centre of decision-making and creates a personalised approach to their care.
Primary care is at the heart of this vision. The primary care workforce is uniquely placed to influence the level of demand for other care settings, acting as a 'navigator' or 'gatekeeper' to secondary care, developing anticipatory care plans, and co-ordinating care, screening and health promotion. It is best placed to support self-management by helping patients to fully understand and manage their own conditions, as well as promoting a focus on both primary and secondary prevention.
This is supported by greater integration of health and social care services to develop stronger care pathways between primary and social care focused on the need of the individual. The ambition set out in Part 2 of the National Workforce Plan [18] that social care supports people at all stages of their lives to live as independently as possible closely aligns with and supports the vision for a strengthened primary care system. The potential benefits in further strengthening primary care system, built on enhanced and expanded multi-disciplinary teams, are set out below.
Figure 2: Strengthening primary care: the benefits
The key benefits of a strong and integrated primary care system
- Half of cancers, three-quarters of cardiovascular disease and 80% of strokes are preventable. More systematic primary prevention in primary care therefore has the potential to improve population health outcomes and has been shown to be cost effective [19] .
- Lifestyle behaviours (such as smoking, diet, obesity and alcohol consumption) are driving non-communicable disease clusters, particularly in our most deprived communities, contributing to a legacy of health inequalities.
- Systematic and scaled-up secondary prevention – for example, prescribing statins to reduce cholesterol and taking measures to reduce high blood pressure – has been found to be cost-effective, clinically significant and an important way to tackle inequalities in health [20] .
- Improved access to primary and social care services could lead to a reduction in 'social admissions' – admissions based not on the severity of a patient's clinical condition but on their inability to cope without appropriate support unless admitted, or if discharged. Social admissions and delayed discharges pose significant issues for hospitals, with up to 40% of admissions of elderly patients who have attended A&E shown to be avoidable [21] .
- Improved access to in and out of hours primary care has the potential to reduce demand for A&E attendances and unnecessary ambulance call outs.
- In the medium term, an enhanced primary care workforce could support patients to take a more pro-active approach to managing their conditions, leading to an estimated 8% to 11% reduction in avoidable admissions (that is, admissions for ambulatory care sensitive conditions) [22] .
Citizen engagement
It is vital that we engage our citizens at every step of the journey to successfully reform primary care services. They must play a key role in helping to shape the services they need now and in the future. In 2015 the Scottish Government launched a National Conversation Creating a Healthier Scotland [23] and through this and the subsequent engagement via the Scottish Health Council's Our Voice Framework [24] , we heard that people want more flexible primary care services, with appointments that fit in with their lives, including work and caring commitments. Engagement via Our Voice has produced a range of innovative suggestions on how to develop services, including highlighting ways to take the pressure off primary care, reduce physical access issues and support self-management.
In addition, the Scottish Government has recently commissioned a series of workshops across Scotland inviting people to give their views on changes to primary care, to hear how general practice teams are changing, and how the development of these teams might impact on them and how they can work for them. The findings from this engagement exercise will help inform the implementation of the new GP contract and the reform of primary care more generally.
As set out in Chapter seven, we are developing a 10 year monitoring and evaluation strategy to capture learning from the reform of primary care. We will ensure that people's views help inform that work as it is taken forward.
Conclusion
We are aware of the significant challenges currently facing the primary care workforce as demand on services continues to increase. Our commitment to reform and invest in primary care services – continuing to shift the balance of care from hospital settings to community health and social care services – is founded on robust evidence that demonstrates that health systems based on strong primary care infrastructure have better outcomes in terms of population health, access, co-ordination experiences and a lower and more appropriate use of resources [25] .
Contact
Email: Naureen.Ahmad@gov.scot