National health and social care workforce plan: part three
Part three of the plan sets out how primary care services are in a strong position to respond to the changing and growing needs of our population.
Chapter Two: The Shape of the Primary Care Workforce
Introduction
The first step in good workforce planning is to have good quality, consistent data on the shape of the current workforce, including recent and predicted future trends in workforce numbers. For the primary care workforce, much has still to be done to improve existing data to provide a more comprehensive and robust evidence base to inform workforce planning. Our approaches to enhancing the data available to planners and clinicians are set out in Chapter seven.
While current workforce data requires further development, it provides useful context on the profile of the existing workforce and potential effects of future pressures. Our understanding of trends will improve as fuller and more integrated data becomes available, informing subsequent iterations of the health and social care workforce plan.
Community and primary care nursing
There are approximately 60,000 nursing and midwifery staff ( WTE) currently employed within NHS Scotland. Of those, around 12,000 ( WTE) work in community settings, almost 3,000 more than in 2007. The increase in nurses working in the community reflects our strategic goal of moving care out of hospital settings to home or a homely setting wherever possible.
Figure 3: Nursing and midwifery (qualified and support) in community settings, WTE, 2007-2017 [26]
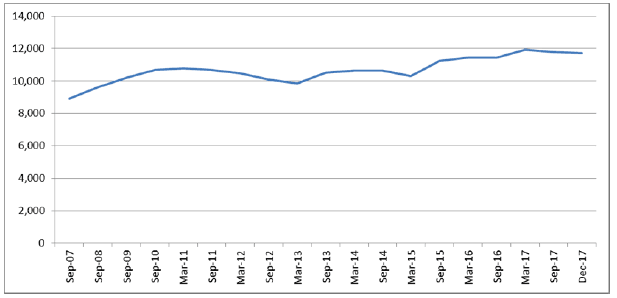
Note: Excludes nurses working in general practice.
General Practice Nursing
At present data on the number of nurses working in general practice (and not employed by NHS Boards) relies on biennial surveys of practices. As set out in Chapter seven our knowledge about the workforce will improve significantly as part of the workforce data that will be collected as part of the new GMS contract. The Primary Care Workforce Survey 2017 suggested that there were around 2,300 General Practice Nurses ( GPNs) working in general practice; approximately 1,540 WTE. These numbers have increased by approximately 160 (headcount) and 125 ( WTE) since 2009.
Figure 4: Estimated registered nurse headcount and WTE, Scotland; 2009 - 2017 [27]
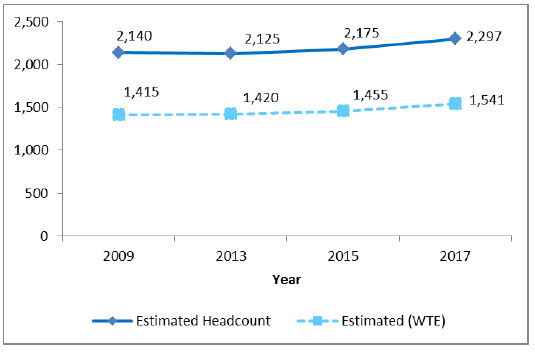
Of the 2,300 registered nurses (headcount) working in general practice, a quarter (544) are Nurse Practitioners or Advanced Nurse Practitioners ( i.e. have acquired the expert knowledge base, complex decision-making skills and clinical competencies for expanded practice). The estimated headcount for General Practice/Treatment Room nurses was 1,754. We have seen a rise of 5% (from 520 to 544) in the number of Nurse Practitioners/Advanced Nurse Practitioners between 2013 and 2017, a positive indication of the enhanced role nurses are playing in general practice across Scotland [28] .
The majority (98%) of registered nurses working in general practice are female. Over half (55%) of all nurses are aged 50 years and over, and this needs to be considered in planning for the workforce of the future.
Figure 5: Age profile of General Practice Nurses, 2017 [29]
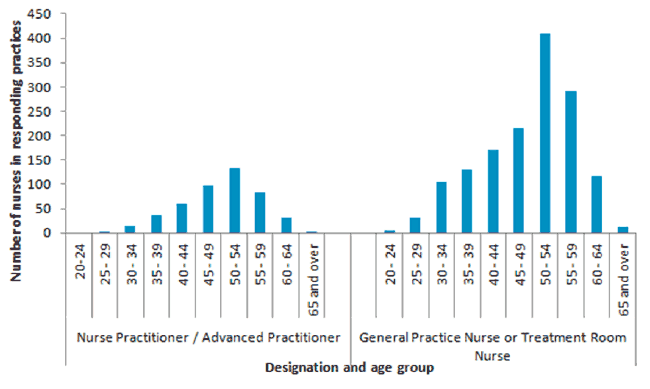
District Nursing and Health Visitors
Due to changes in classifications, longer term time series data on District Nursing and Health Visitors is unavailable. In December 2017 there were approximately 3,400 ( WTE) staff working in District Nursing in Scotland (a slight fall from December 2015), and almost 1,450 ( WTE) Health Visitors (an increase of approximately 270 since December 2015) [30] . Of the 3,400 working in District Nursing, around 1,000 are band 6 and 7 District Nurses ( WTE) [31] . The number of District Nurses has fallen by about 50 since December 2015.
Table 1: District Nursing and Health Visitors [32] ( WTE), Dec 2015 – Dec 2017
| Dec-15 | Dec-16 | Dec-17 | |
|---|---|---|---|
| District nursing | 3,504 | 3,514 | 3,443 |
| - of which District Nurses | 1,056 | 1,055 | 1,002 |
| Health visitors | 1,180 | 1,292 | 1,448 |
The age profile of District Nurses (band 6 and 7) are shown below. Approximately 60% are aged 50 years and over. This is likely to partly reflect career pathways, with District Nurses tending to be experienced practitioners. Planning for routine staff turnover in light of local workforce data is the responsibility of NHS boards, but clearly such a sizeable proportion of the workforce being aged over 50 also has important implications for workforce planning in ensuring a sustainable service.
Figure 6: Age profile of District Nurses (band 6 and 7), 2017 [33]
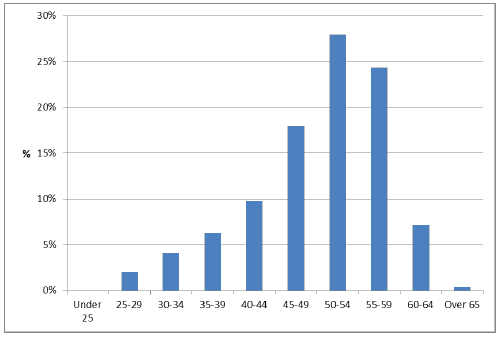
Care Home Nursing
There are approximately 4,600 nurses (headcount) working in care homes, the vast majority (around 4,250) in private care homes [34] . Further information on the numbers and trends in numbers of nurses in the social care sector is contained in Part 2 of the National Workforce Plan [35] .
Health Care Assistants [36] ( HCAs)
Health Care Assistants are a vital part of the community team, working across healthcare disciplines under the direction and professional accountability of registered practitioners, such as nurses, physiotherapists and pharmacists. For example, the Transforming Roles [37] review of district nursing roles in integrated nursing teams set out how support workers can work most effectively in a range of settings and activities.
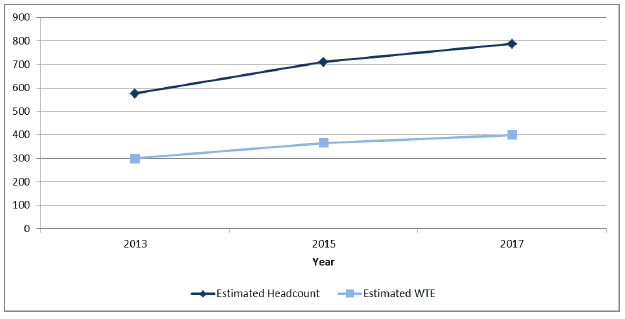
Data on the number of HCAs working in general practice is available from the biennial Primary Care Workforce Survey. In 2017 it was estimated that there were around 787 (399 WTE) HCAs, an increase of approximately 210 headcount and 100 WTE from 2013 [38] .
Figure 7: Health Care Assistants (estimated headcount and WTE), 2013-17 [39]
Allied Health Professions
Allied Health Professionals are a distinct group of health professionals [40] who apply their expertise to prevent illness, diagnose, treat and rehabilitate people of all ages. They deliver direct patient care, rehabilitation, treatment, diagnostics and health improvement interventions to restore and maintain optimal physical, sensory, psychological, cognitive and social functions. There are many developing AHP roles where practitioners are taking on extended generic skills and functions.
As shown in figure 8, the number of physiotherapists, occupational therapists, dieticians, and paramedics employed by NHS Scotland has increased since 2007, although there has been a slight fall in staff employed in podiatry. More comprehensive data on the AHP workforce is available at: http://www.isdscotland.org/Health-Topics/Workforce/Publications/data-tables2017.asp?id=2115#2115
We know the number of AHPs working in the community is substantial but data is currently not available at a national level on location of practice. We are aware of the significant gaps in AHP workforce data and outline approaches to improving these data in Chapter seven.
Figure 8: Selected Allied Health Professions groupings ( WTE), 2007-2017 [41]
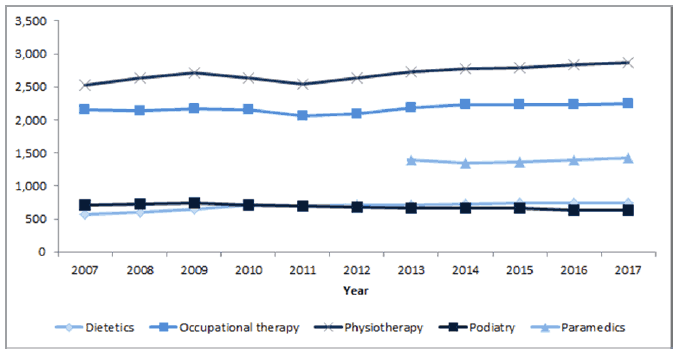
Note: Paramedics were reclassified as allied health professions from 1 st April 2013.
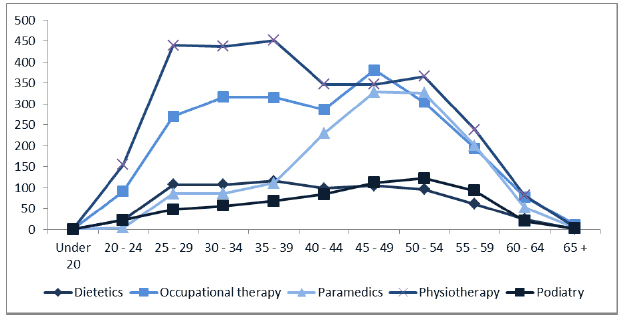
The age profile of the AHP workforce is provided below. The physiotherapist workforce is notable for having a relatively young age profile, with a significant proportion below the age of 40.
Figure 9: Selected AHP groupings, age profile, December 2017 [42]
General Practitioners
The number of patients registered with GP practices continues to rise slowly year on year and has increased by 5% since 2007, however the number of patients aged 65+ has increased by 20% since 2007. The number of practices in Scotland decreased by 7% since 2007, reflecting a trend towards larger practices [43] .
There were approximately 4,900 GPs working in around 960 practices in Scotland as of end of September 2017. The majority (3,500) of GPs are GP partners, with about 850 salaried GPs, 100 retainees [44] and 500 GP Registrars / specialist trainees. The number of salaried GPs (Board-employed and GP partner employed) has doubled over the last decade with falling numbers of GP partners and GP retainees. Around 60% of the GP workforce is female, up from half a decade ago.
Table 2: GP Designation by gender, Scotland, September 2017 (headcount) [45]
| Designation | Females | Males | All |
|---|---|---|---|
| GP Partners | 1,868 | 1,631 | 3,499 |
| Salaried GPs | 625 | 221 | 846 |
| GP Retainee | 91 | 0 | 91 |
| GP Registrar/ ST | 360 | 140 | 500 |
| All GPs | 2,935 | 1,985 | 4,920 |
The headcount number of qualified GPs working in NHS Scotland has increased by around 200 since 2005 to around 4,400. There has been a larger increase (of 400 to 4,900) in all GPs, including registrars and those in speciality training. However there has been a fall in the estimated whole time equivalent [46] in recent years (figure 10).
Figure 10: GP headcount and whole time equivalent, 2005-2017 [47]
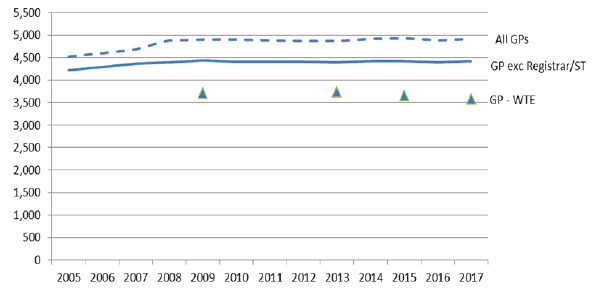
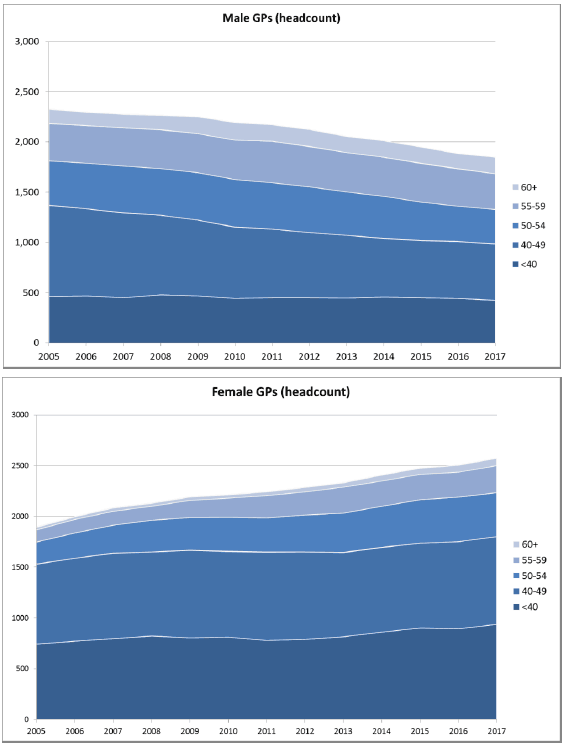
The fall in WTE shown in figure 10 is largely driven by falling numbers of male GPs (particularly those in middle-age), who have traditionally worked more sessions than their female colleagues. The number of female GPs (headcount) has increased by almost a third since 2005 (Figure 11) and this trend is expected to continue.
Figure 11: GPs (headcount) by gender and age, Scotland 2005-2017 [48]
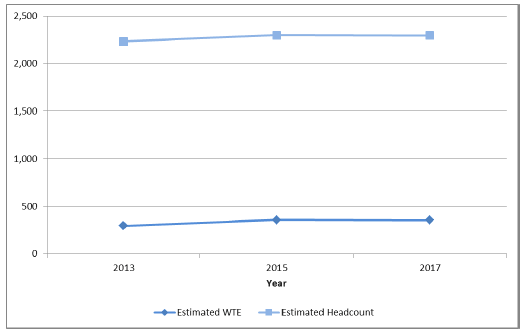
Out of hours services are vital in ensuring people with urgent care needs get the right advice at the right time. The number of GPs working out of hours has increased slightly since 2013 [49] . There approximately 2,300 GPs (including registrars/ ST) providing Out of Hours in the year ending 31 August 2017.
Figure 12: Number of GPs (headcount and WTE) working Out of Hours, 2013-2017
Locums constitute an important part of our workforce offering flexibility and temporary support. Over four fifths of practices (83%) reported requiring to recruit locums for planned events, and approximately half (47%) for unplanned absences. There has been a slight fall in the use of locum sessions (per 10,000 patients) between 2013 and 2017 [50] .
While general practice workforce data currently relies on a biennial survey, submission of workforce and other practice data will become a requirement under the new GP contract ( Chapter seven). This will improve the completeness and scope of the data available to planners.
Pharmacists
Pharmacists are located throughout our hospitals, GP practices and communities, from rural areas to deprived inner-city areas, providing pharmaceutical care on behalf of NHS Scotland. As well as dispensing around 100 million prescription items annually [51] , NHS pharmaceutical care services delivered in our community pharmacies include minor ailment, public health, and acute and chronic medication services. These services involve pharmacists in the community providing direct person-centred care as part of the wider primary care team.
Pharmacy workforce data is one of the areas that we are working to strengthen, particularly in community pharmacies where, as independent contractors, pharmacy owners and managers determine staffing levels needed to provide safe and effective services in line with the General Pharmaceutical Council standards and guidelines.
As a proxy measure of overall pharmacy workforce numbers, figure 13 below shows the number of registered pharmacists and technicians in Scotland by age as at January 2018. In total, there are currently approximately 4,800 registrant pharmacists and 2,100 pharmacy technicians in Scotland.
Figure 13: Age profile of Registrant Pharmacists and Pharmacist Technicians, Scotland, January 2018 [52]
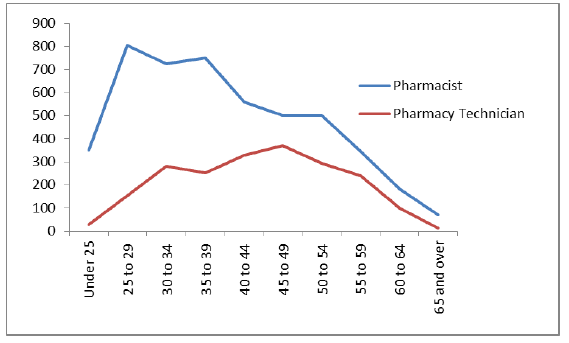
Table 3 represents the total number of pharmacy staff directly employed by NHS Scotland. As indicated above, it does not include those employed in community pharmacy as this is the responsibility of individual community pharmacy contractors.
Table 3: Age profile of Pharmacy Staff ( WTE) directly employed by NHS Scotland, December 2017 [53]
| WTE 31 st December 2017 | Age Group (years) | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Under 25 | 25 to 29 | 30 to 34 | 35 to 39 | 40 to 44 | 45 to 49 | 50 to 54 | 55 to 59 | 60 to 64 | ≥ 65 | TOTAL | |
| Pharmacy Staff | 198.9 | 375.2 | 372.8 | 385.7 | 349.9 | 347.0 | 341.9 | 260.5 | 86.7 | 4.1 | 2,722.6 |
NHS Boards across Scotland directly employ approximately 2,700 whole time equivalent pharmacy staff working in hospital and providing support to community health services working within or with GP practices.
These figures are made up of pharmacists, pharmacy technicians, trainee pharmacy technicians, pharmacy assistants and pharmacy administration and clerical staff. In broad terms over half (approximately 55%) are registered pharmacists, with the remainder employed in increasingly important roles such as pharmacy technicians and assistants.
While the current age profile at a national level suggests a steady supply of pharmacists and pharmacy technicians aged under 50, it is acknowledged that there are greater challenges in some areas around recruitment and retention for both hospital and community sectors.
Dentists
In relation to oral health the dental workforce consists of dentists working alongside dental care professionals, i.e. dental nurses, hygienists, therapists, dental technicians, clinical dental technicians and orthodontic therapists. As oral health improves particularly amongst the younger generation, the dental needs of patients will change, focussing more on prevention. This will take several generations to work through and the dental workforce will require to be sufficiently flexible to meet the differing requirements. At the other end of the age spectrum with an increase in the number of frail, elderly patients retaining their natural teeth other challenges are emerging for clinicians in providing care for frail people, often in the patient's place of residence.
The number of dentists in primary care continues to increase. The majority of Primary Care dental services are provided by independent General Dental Practitioners ( GDPs) with the remainder being provided by Public Dental Service dentists.
Table 4: Primary Care Dentists (headcount), Scotland, 2014-17 [54]
| 2014 | 2015 | 2016 | 2017 | % change |
|---|---|---|---|---|
| 3,332 | 3,348 | 3,397 | 3,407 | 2.3% |
The increase in the independent GDP workforce (from 2,261 in 2007 to 3,004 in 2017) means that there are 55.6 dentists per 100,000 of the population providing NHS dental care and treatment, compared to 44.0 in 2007 [55] .
Optometrists
Community eyecare is a contractor service provided by optometrists and ophthalmic medical practitioners ( OMPs). This has developed since the introduction of free eye examinations in 2006, to the service being the first port of call for people with eye problems, helping to detect eye diseases early.
Based on the most recent workforce data available, in 2016 there were approximately 1,453 optometrists and three OMPs (headcount) providing a community eyecare service in Scotland. In addition, there were approximately 410 dispensing opticians who advise and help with the supply of spectacles and contact lenses, as well as dispensing low vision aids and fitting spectacles for children [56] . Historically, the number of optometrists in Scotland has increased on average by approximately three per cent per annum. This is due to more optometrists qualifying than retiring, with only a small number entering Scotland from elsewhere.
Optometrists can become independent prescribers on completion of an additional professional qualification, which is part funded by NHS Education Scotland ( NES). Independent prescribing optometrists are able to prescribe licensed medicine for conditions affecting the eye, and the tissues surrounding the eye, within their recognised area of expertise and competence. To date, 214 community optometrists have qualified to become independent prescribers in Scotland – a third of the total UK figure.
Local variation
We have presented data at a national level to provide broad context on the shape of the current primary care workforce. We are aware that there is considerable variation across Scotland both in the size of the workforce and the pressures being experienced in retaining and recruiting staff. Data at Health Board level is available from Information Services Division: http://www.isdscotland.org/Health-Topics/Workforce/ and is used to informed local workforce planning. However, as noted, we fully recognise the need to improve the information available to both local and national planners.
Conclusion
This overview of the primary care workforce in Scotland is a starting point. We recognise that some gaps remain in the data currently available and Chapter seven outlines the improvements underway to data quality and completeness that will aid national, regional and local understanding and planning of the workforce.
We have already acknowledged in Parts 1 and 2 the need over the longer-term to develop more sophisticated workforce modelling, including the design of a 'pipeline' approach indicating how supply via training and recruitment numbers will meet estimated demand for services and take account of, for example, the changing demographic profile of the workforce. NHS Education for Scotland is currently developing a workforce data platform which will help drive more informed, comprehensive and integrated workforce planning. We recognise that it is important for this work to extend in order to encompass the primary care workforce, and good progress is already being taken to ensure this.
Contact
Email: Naureen.Ahmad@gov.scot