Health and social care: integrated workforce plan
Sets out our future workforce requirements in a national context and provides revised workforce planning guidance to health and social care employers.
Actions we will take to meet those needs & challenges
As we have set out earlier in this Plan, the demand and supply landscape for the health and social care workforce is a complex one. There is no one simple solution to address these issues and ensure that we have a sustainable workforce for the future. The solutions lie in a range of national and local actions to attract, retain and develop our whole workforce, which are based on the best available evidence and flexible enough to adapt to changing circumstances.
In this section we set out the actions which are underway or which we are committing to through this Plan. We are taking actions on:
- overall investment in health and social care;
- increasing the supply of staff into training or as qualified staff;
- supporting recruitment into health and social care careers;
- widening access to grow the workforce;
- supporting the development and retention of the current workforce;
- improving workforce planning across health and social care;
- improving fair work practices across the social care workforce.
In doing so we have a particular emphasis on building the workforce in our key priority areas to address the demand and supply issues identified in this Plan.
Overall Investment in Health and Social Care
Underpinning all of our commitments is investment in health and social care services. The investment Scottish Government has made to these services will continue, and over the remainder of this parliamentary term, the Scottish Government's main health and social care expenditure commitments will:
- Maintain baseline allocations to frontline Health Boards in real terms, with additional funding over and above inflation to support the shift in the balance of care and protect health expenditure from rising prices;
- Increase the share of the frontline NHS budget dedicated to mental health, and to primary, community, and social care in every year of the Parliament;
- More than 50% of frontline NHS expenditure will be community-based - so that a greater proportion of care is provided in settings close to a person's home rather than in a hospital;
- In 2019/20, we are increasing the package of investment in social care and integration to exceed £700 million. This includes support for the Living Wage, the continued implementation of the Carers (Scotland) Act 2016 and extending free personal care to under 65s;
- Funding for primary and community care will be increased to 11% of the frontline NHS budget by 2021/22, enabling increased spending of about £500 million - with around half of this growth invested directly into GP services, and the remainder invested in community primary care;
- Scottish Government have delivered the commitment to invest £1 billion in mental health, and over the life of this Parliament investment will exceed £5 billion. The Programme for Government 2018-19 announced an additional £250 million over the next five years to introduce a package of measures to improve services for children, young people and adults, and embed support for good mental health across public services.
Growing the Numbers in Training or Employment
Growth in Training Numbers
The health and social care workforce enter their roles in a variety of ways. There are also a number of points at which they are more likely to leave, and we need to focus actions on retaining and attracting staff at those key points of the pipeline. This is represented below.
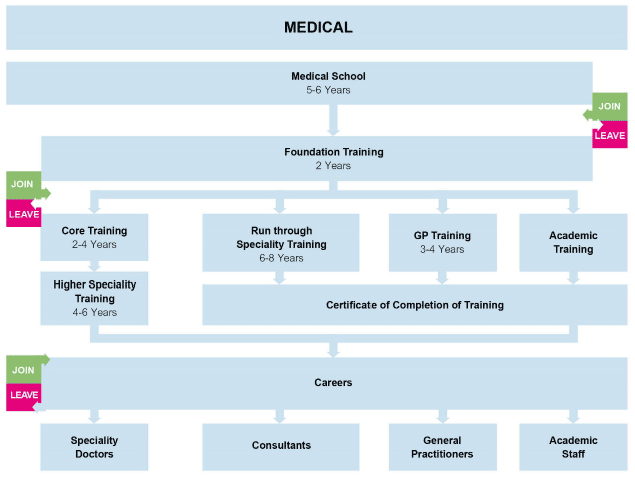
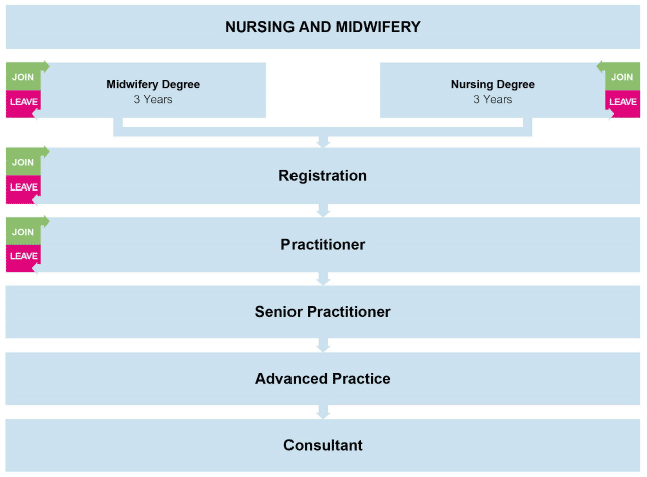
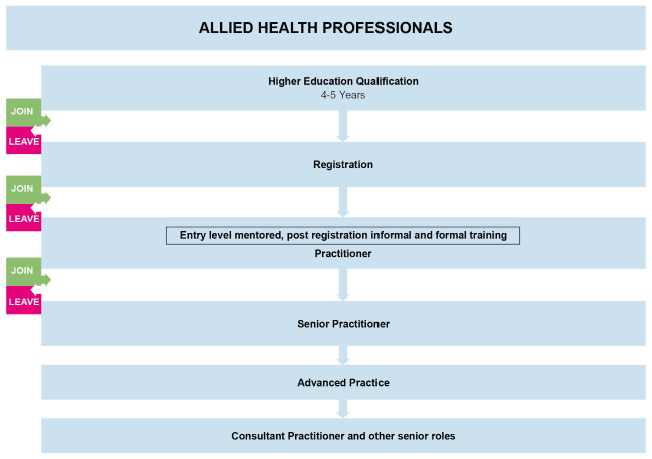
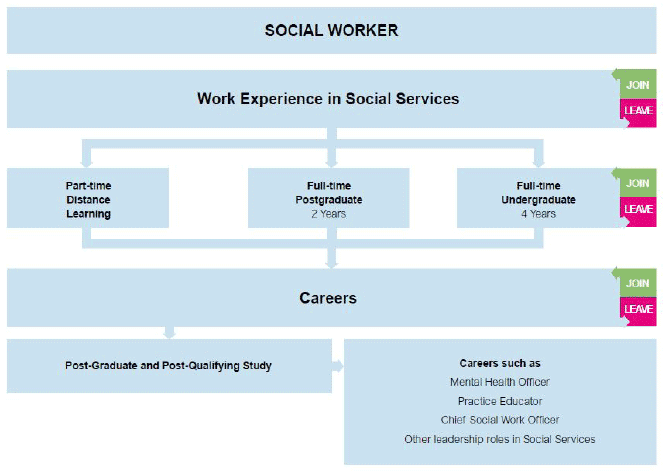
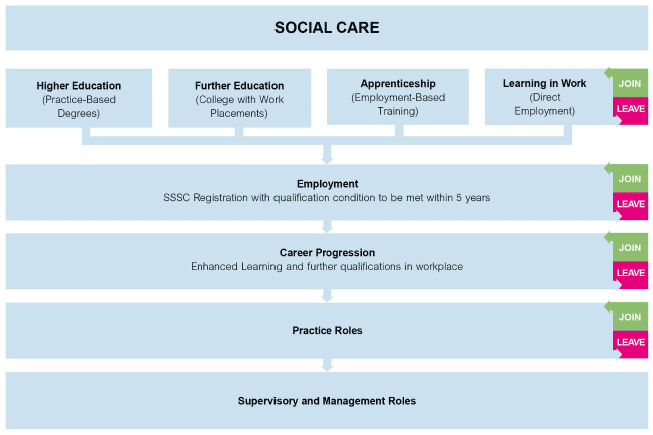
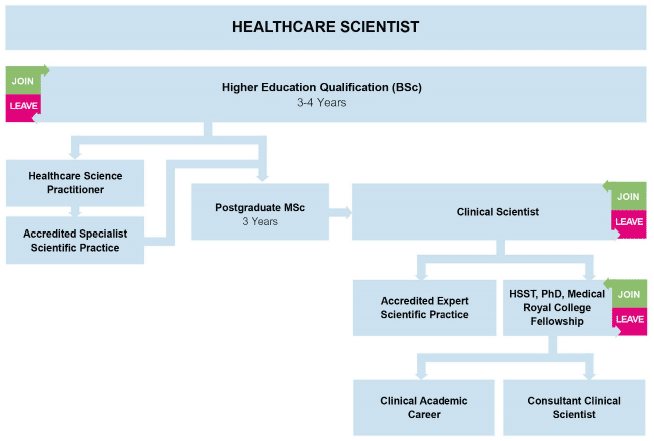
Most staff groups within NHS Scotland are required to achieve formal qualifications in advance of securing permanent roles. Social Workers achieve a graduate/post-graduate qualification in advance of entering the profession. However, within social care, the majority of staff typically achieve qualification once in employment.
The Scottish Government sets, and thereby controls, the numbers entering training for nurses and midwives, dentists and doctors (at undergraduate, foundation level and specialty training levels). Sufficient numbers of undergraduates need to both graduate and elect to remain in Scotland through post-graduate training to provide the necessary supply into the specialities that services require.
At national level the Scottish Government has very limited control over the supply pipeline for social care workers. The number of workers entering the social care sector is significantly influenced by the funding available for social care services, the commissioning of services and market forces affecting competition from other sectors and employment.
Decisions on those numbers are informed by workforce planning and provide a mechanism through which we can respond nationally to changes in demand and supply. Given that it takes a minimum of 10 years to train a GP (and in some medical specialties substantially longer) and to train a consultant doctor, this presents a particular workforce planning challenge.
Scottish Government have already increased or maintained training places in these controlled staffing groups.
- Scottish Government is on track to create 2,600 more nursing and midwifery training places by 2021, with a particular focus on increasing places in mental health, learning disability and midwifery;
- Scottish Government has committed to increasing the Student Nursing intake from 4,006 to 4,206 in 2020/2021;
- Scottish Government funds pre-registration nursing places through University of the Highlands and Islands (UHI) at its campuses in Inverness and Stornoway. Ensuring access to training and qualification to those from more remote, rural and island communities;
- To meet regional demand, particularly in remote, island and rural communities, for midwives in the Highlands and Islands, a pilot programme at UHI has been funded to allow nurses to retrain as midwives in a shortened time frame;
- Scottish Government will have created 190 additional Medical Undergraduate places by 2021 (a 22% increase over 2016 levels);
- To accommodate the additional undergraduate medical trainees Scottish Government will increase the number of Medical Foundation training posts by 51 in 2021 and by a further 54 in 2022. These will accommodate the first of the additional graduates and enable them to proceed to the next stage of their training in order to become qualified doctors. The new places will create a greater range of placements for trainee doctors, particularly in general practice and psychiatry and in remote or rural parts of Scotland;
- Scottish Government have increased Medical Specialty training posts by 190 since 2014, particularly specialties such as Paediatrics and Radiology and also increasing GP Specialty Training numbers by 100 to 400 per year;
- To grow the Pharmacy workforce in hospitals, GP practices and community settings, Scottish Government increased the number of funded pre-registration places from 170 to 200 in 2018-19;
- Scottish Government has committed to maintaining the Dental Student Intake numbers, funding 135 places in 2020/2021.
Training numbers for other staffing groups such as AHPs, healthcare scientists, pharmacists and social workers, who undertake formal qualifications in advance of employment, are not centrally controlled. Instead they reflect decisions on intake by the universities providing qualifying programmes and demand from potential students. However there are actions we can take to improve workforce planning for these groups.
Following the recent review of social work education, a Social Work Education Partnership between employers and academic providers of qualifying programmes is being established with support from the Scottish Government and COSLA. Part of the remit of the Partnership will be to work with SSSC to monitor supply and demand of qualified social workers and contribute to effective workforce planning for social workers at a national level, including through a shared approach to significant changes in student numbers.
In pharmacy, the one year pre-registration course is nationally funded by Scottish Government and managed by NHS Education for Scotland. In line with previous evidence there is an expectation that at least 80% of pharmacy students will remain in Scotland after qualification.
In Optometry, we continue to fund Optometrists to become independent prescribers, which helps reduce demand on GPs and hospitals. The number of independent prescribing (IP) Optometrists is growing every year, with more than a fifth of the workforce now having the qualification (representing approximately a third of all IP Optometrists in the UK).
In addition to growing the numbers entering the training pipelines in the staff groups where numbers are controlled, the Scottish Government is taking a number of actions to create the workforce to deliver in our three priority areas.
Building up our Community Based Workforce
If we are to embed and sustain health and social care integration and shift the balance of care, with a focus on early intervention and prevention, we need to build up the capacity in our community based workforce to treat people closer to home and prevent unnecessary admissions to hospitals.
In part we can achieve this by a growth in the overall numbers in some of the core community based staffing groups. Scottish Government are delivering on commitments to train 1,000 more paramedics by 2021 and we have increased health visitor numbers by 500. In addition to this we are making a further commitment, based on the scenarios developed, to train and introduce an additional 375 nurses into the district nursing service, based upon the current skills mix.
Supporting the shift in balance of care into community settings by delivering care in homes and reducing rates of admission to acute hospital service. Train and introduce into the workforce an additional 375 nurses within the district nursing service based upon the current skills mix, over the next 5 years.
Recognising that General Practice is at the core of community based healthcare services actions have also been taken to grow the numbers of both GPs and other practice based staff. A commitment has been made to expand the GP workforce by at least 800 by 2028 with, by 2021, all GP practices having access to pharmacists with advanced clinical skills and up to 250 community link workers working in GP surgeries.
We continue to look at further opportunities to grow our multi-disciplined community based healthcare teams. We have set out workforce scenarios for Advanced Musculo-Skeletal (MSK) Practitioners, Pharmacists and Pharmacy Technicians. These roles can reduce the workload on GPs by delivering care closer to people's homes and reducing unnecessary admissions to hospital - ensuring people see the right person at the right time. The scenarios set out the particular demand and supply situations for these staffing groups, and in light of these findings we will:
Create 225 more Advanced MSK Practitioners in Primary Care by increasing MSc training places for the Physiotherapy workforce.
Increase Pharmacy pre-registration training places by 40 each year over the next 3 years, creating the opportunity for more Pharmacists to enter primary care.
More broadly, we will ensure that we shape existing training programmes to increase the time spent in community settings. As well as gaining valuable experience in these settings, time spent in the community during training may have a positive influence on trainees choosing future community based careers. We are therefore taking the following actions:
- A five year integrated initial education programme for Pharmacists is being developed in Scotland, which will include more time spent in primary care and out-of-hours services during their undergraduate training;
- The Increasing Undergraduate Education in Primary Care Working Group established jointly by the Scottish Government and the Board for Academic Medicine is considering ways of increasing medical undergraduate education in primary care settings to encourage more medical students to choose General Practice. The report is due to be published shortly;
- Scotland's first graduate entry programme for medicine has an emphasis on experience in General Practice to produce doctors more likely to choose a career in General Practice;
- To meet regional demand, a new Optometry course is starting at the University of the Highlands and Islands from September 2020. It is aimed at improving recruitment and retention of Optometrists in remote and rural areas in the Highlands and Islands.
Building our Mental Health Workforce
To achieve our ambitious aims for mental health services in Scotland, we are supporting the creation of the multi-agency, multidisciplinary teams that will deliver them. Significant steps have already been taken to grow this workforce with a commitment to an additional 800 mental health workers in A&Es, GP practices, police custody suites and prisons by 2022.
The Children and Young People's Mental Health Taskforce has taken steps to build workforce capacity in early intervention and prevention, including:
- £4 million investment to recruit 80 additional mental health professionals to work with children;
- An additional 250 school nurses recruited by 2022 to help provide a response to mild and moderate emotional and mental health difficulties experienced by young people, helping to ensure that every secondary school has access to counselling services;
- An investment of over £60 million to provide around 350 counsellors in school education across Scotland;
- In further and higher education, an investment of around £20 million to provide an additional 80-90 counsellors over the next four years.
Through actions such as making mental health and suicide prevention training mandatory for all NHS staff who receive mandatory physical health training, we are also developing a better understanding of mental health issues across our health workforce.
Targeted action to further grow our mental health workforce is also being taken. In the annex published alongside this Plan we set out workforce scenarios for Clinical Psychologists and Mental Health Officers (MHOs).
Clinical Psychologists work across a number of different specialty work areas providing services across Child & Adolescent, Adult and Older Adult mental health. They support people to understand and make changes to their thinking, behaviour and relationships in order to relieve distress and to improve functioning. They are a particularly valuable resource because of their flexibility in working across these groups.
Mental Health Officers (MHOs) are social workers with a minimum of two years qualifying experience. They carry out statutory roles for local authorities in a range of areas including welfare guardianship orders, Emergency Detention Certificates and Compulsory Treatment Orders; they are required to complete the Mental Health Officer Award.
The scenarios set out the particular demand and supply situations for these two staffing groups and in light of those findings we will:
Support an 60 additional Clinical Psychologists in training by:
- Increasing the training programme intake by 10 students per year for the next three years
- Maintain the current intake level (30 per annum) for both Masters training programmes. This would continue the additional 10 places which have been available in recent years.
Support additional Mental Health Officer (MHO) capacity in local authorities by providing funding to help address the current shortfall in capacity of 55 WTE by 2022-23.
In the medium term, modelling work will take place to assess the impact of reforms to adults with incapacity requirements, particularly around guardianship applications on MHS workload and demand for MHOs.
Building the Workforce to Improve Waiting Times
In light of the potential impact the Elective Centres will have on workforce demand, a specific workforce plan for the centres is being developed, which focuses on the clinical teams required to provide increased capacity and the support these teams will need to function effectively. Using the new data platform developed by NES, indicative workforce figures for the centres have been collated. These will be refined as the models of care are developed to reflect modern work practices, which will be adopted in the centres.
To build the workforce capacity required we are building on existing academy models currently in place in several health boards and the new NHSScotland Training Academy that will be established at the Golden Jubilee Foundation. We are also linking with the Accelerating the Development of Advanced Practitioners programme which has been successfully tested and implemented in NHS Lanarkshire to increase the number of advanced practitioners required for the centres. Where there may be a shortfall, for example in medical specialties, we will develop a strategy to mitigate the risks and look at solutions including combined elective and acute roles and joint appointments.
In a general hospital, Cardiac Clinical Physiologist investigations include specialist echo cardiography, pacemaker checks and implantable cardioverter-defibrillator work. In terms of in-patient work, diagnostic testing is a critical part of a patients assessment, and delays in the system affect the patient flow. For every one additional trained Physiologist, capacity would rise by an additional 60 echos per week and 40 pacer ICD checks. The scenario developed shows the identified gap and that is why we will:
Increase the Cardiac Physiologist workforce, thereby increasing capacity to carry out diagnostic testing, by supporting an additional 30 training places on the 4 year BSc course in Clinical Physiology.
Over the next 3-5 years we will also focus on increasing the workforce by promoting recruitment into Scientist Training Programmes and Practitioner BSC Programmes.
Ophthalmology is the largest hospital outpatient specialty. Enabled by a new shared Electronic Patient Record, we are providing funding to enable 80 independent prescribing (IP) Optometrists to become accredited to safely manage 20,000 low risk glaucoma and treated ocular hypertension patients in the community. The first cohort of IP Optometrists will commence training in January 2020, with the first low risk glaucoma patients being discharged to their management in early 2021. Once fully rolled out in 2024, this shift in the balance of care will free up approximately 30,000 appointments per annum in the hospital eye service.
In addition we are taking targeted action in this Plan to increase diagnostic capacity which is key to further reductions in waiting times. In the workforce scenarios we set out a scenario for clinical Radiology and reporting Radiography, which draw on the workforce planning work undertaken by the Scottish Radiology Transformation Programme. We have already recognised the need for high growth in the clinical radiology medical specialty with increases in Radiologist training places since 2014 and continued growth going forward. By 2021 these training places will have grown from 103 to 175. Reporting Radiographers also have a key role in creating capacity in the Radiology multi-disciplinary team. The scenario developed sets out the particular demand and supply situation for this staffing group and in light of those findings we will:
Increase Reporting Radiographer trainee places by 30 (10 in each of the next 3 years).
Supporting Recruitment into Health and Social Care Careers
While NHS Boards, Local Authorities and Social Care employers have responsibility for recruiting and employing their staff, we are supporting them in that national and international recruitment role with a number of national actions.
We are investing £4m in recruitment campaigns for adult social care, nursing, and medical recruitment campaigns with targeted recruitment into professions such as GPs, Psychiatry, Anaesthetics, Paediatrics and Emergency Medicine. All of the campaigns are designed to reflect the particular demand and supply issues with those staffing groups:
- A national recruitment campaign for nursing, midwifery, allied health professionals (NMAHPs) and healthcare scientists was launched in November 2019, targeting students applying to universities. The campaign will promote the contribution NMAHPs and healthcare scientists make to positive outcomes in Scotland, and the range of positive career opportunities available in order to attract individuals into NMAHP and healthcare science careers and ensure a sustainable workforce is available to meet Scotland's future requirements;
- A national GP marketing campaign promoting Scotland as a positive place to work has been developed. The aim is to promote Scotland as a great place to work for GPs. This has been done through marketing stand representation at number of events and conferences throughout 2019/20. We are also developing a marketing strategy to design our approach to international recruitment of GPs;
- As part of the reform of adult social care programme, a national campaign to promote social care as a meaningful, valued and rewarding career choice is being developed. The campaign will support recruitment of frontline workers in care home services for adults, care at home services for adults and housing support workers. The campaign's primary focus will be on attracting people from early to mid-career stages, which form key entry points to the sector. The campaign is due to launch in early 2020;
- The medical campaigns in Psychiatry, Anaesthetics, Paediatrics and Emergency Medicine are targeting consultant level staff. The choice of those specialties are based on current vacancies, cross-referenced against the data we have on EU doctors living and working in Scotland. In the medium term, we will undertake further campaign activity across other medical specialties that support our Waiting Times priorities such as Dermatology and Urology.
These campaigns build on existing recruitment work. The SSSC delivers a range of support for recruitment and retention of the social services workforce including resources on career pathways and promotional materials for schools, colleges, employment services and employers; management and promotion of routes into careers (Foundation and Modern Apprenticeships); and a network of Ambassadors for Careers in Care. In addition, a Recruitment Working Group (RWG) established by the Coalition of Care and Support Providers in Scotland is stimulating change by providing information, analysis and support to improve recruitment outcomes in the Social Care Voluntary Sector. As a part of this process, three workshops were delivered to partners in the Voluntary Sector last year to explore key points in the recruitment process.
While recognising the diversity of the sector, future work will look at areas where there is benefit in collaborative and shared approaches to recruitment practice.
Improving fair work practices across the social care sector is a key element of the reform of adult social care programme. This is why the Scottish Government has also committed to taking forward the recommendations set out in the Fair Work in Scotland's Social Care Sector 2019 report to improve fair work practices across the health and social care workforce.
In medicine, we will learn from the recent experience of our national recruitment campaign on Radiology. Also over the last 5 years we have been working in partnership with NES and the medical Royal Colleges to recruit international doctors to non-Consultant posts by developing and supporting schemes such as the International Medical Training Fellowship and the Medical Training Initiative. Designed to provide high quality training and to support service delivery, the schemes typically offer 1 year posts, which can be extended. To date over 90 posts have been approved across medical specialties. We continue to assess and refine our approach to these schemes to ensure we are maximising benefit and attraction.
Alongside this, we are working with the General Medical Council (GMC) and the Royal College of General Practitioners to streamline and accelerate the Certificate of Eligibility for GP Registration process which support doctors trained outside the EU to come and work as substantive GPs in Scotland. We are already seeing a positive impact, with Australian GPs being able to get almost reciprocal registration with the GMC.
We have also established an International Recruitment Unit to improve Scotland's effectiveness in recruiting internationally and support the resilience of NHS Scotland as we approach potential EU Withdrawal. To this end, the unit is providing expert support on the immigration process and regulatory requirements to work in Scotland, as well as matching people to job opportunities. The unit is currently heavily involved in co-ordinating medical recruitment and will help successful candidates with relocation advice and on-boarding. Moving forward, a more systematic and collaborative approach to recruitment events will achieve economies of scale and capitalise on the strength of the NHS Scotland brand.
Widening Access to Grow the Workforce
In addition to attracting people from the rest of UK and internationally to work in health and social care in Scotland we also need to grow our own talent.
Around 360,000 people work in health and social care in Scotland. To maintain and grow that workforce, we must continue to attract significant numbers into these careers. We are committed to building on initiatives to help widen access to careers for young people and other under-represented groups in this sector.
A good illustration of the work we are doing to achieve this aim is the three year employability partnership between NHSScotland and Prince's Trust Scotland. "Get into Healthcare" will support around 400 young people from disadvantaged backgrounds to achieve their potential and develop their skills through a career in the health sector. We will also support similar schemes being delivered for social care in Scotland, in partnership with employers in the sector. This work will explore pilot approaches suitable for smaller employers that form a significant part of social care provision.
Modern Apprenticeships (MA) are available to young people aged 16-24 to widen access to health and social care careers. There are apprenticeship frameworks available with social services, clinical and non-clinical pathways, which give young people the opportunity to start a career in a range of job families in social care and the NHS and to work and earn whilst gaining a qualification. MA Frameworks that are available include Social Services and Healthcare, Healthcare Support (clinical and non-clinical), Business and Administration, Estates and Facilities, and IT. Foundation, technical and professional apprenticeships are also available in the social care sector. New routes and pathways are also being considered to provide a diverse range of career opportunities for young people in health and social care.
Within Nursing and Midwifery, work is being taken forward on recommendations from the Chief Nursing Officer's commission into widening participation to nursing and midwifery education careers. Recommendations include establishing a route from school into pre-registration nursing and midwifery through the apprentice route; adopting a positive approach to commissioning pathways into nursing careers for healthcare support workers; attracting people into the professions (particularly men); and extending existing routes such as the funded HNC and the Open University (OU) options to deliver a pre-registration nursing programme for health care support workers, with a particular focus on remote and rural areas.
The OU distance learning and part-time model means healthcare support workers can still work and earn during their studies. Funding has already been provided for 300 pre-registration nurses through the University of Highlands and Islands.
The NHS Professional Careers Programme is a two-year employment opportunity for disabled graduates to prepare for a long-term sustainable career. Since 2015 the programme has helped over 40 disabled graduates (90% of participants) go into a career of their choice.
In our medical education we have acted in recent years to support a greater number of students from areas of social deprivation into medical careers. 50 of the additional undergraduate medical places have been designated as 'Widening Access' places and we are also seeing some positive results from pre-medical courses at the Medical Schools in Glasgow and Aberdeen. These pre-medical courses provide students from more socially deprived backgrounds with the educational knowledge, skills and confidence to enter into medicine. 40 out of 42 from the first course intake progressed to medicine, a result that exceeded expectations. This will lead to an increase in the number of more "home grown" students from all sectors of Scottish society studying medicine. We know that Scottish domiciled students tend to be retained in NHS Scotland at a higher rate than students from elsewhere.
Developing and Retaining our Existing Workforce
Increasing workforce numbers alone will not ensure the sustainability of our health and social care services. We need to retain the workforce we already have by supporting them, investing in training and offering attractive and rewarding careers. We also need to ensure that they are well equipped to be able to adapt to new ways of working and different ways of providing services; and to ensure that we make best use of their skills.
Training and Career Development
Access to high quality learning and clear qualification pathways with opportunities to progress have the potential to raise the status and attractiveness of careers across health and social care. This area is one of particular focus in the social care sector.
In social work, we are working with the sector to provide an improved approach to social work professional development throughout careers through:
- delivering improvements to consistency and quality of social work education through a Social Work Education Partnership between employers and Universities providing qualifying programmes;
- piloting a supported year for Newly Qualified Social Workers;
- developing a Professional Framework for Practice for Social Work up to Advanced Practice level.
These initiatives seek to support career development and improve access to high quality training opportunities that reflect current and future developments in policy and practice.
In social care, we are seeking to improve career development opportunities and progression through:
- the development by the Scottish Social Services Council (SSSC) of a new careers resource that illustrates the qualification and career pathways open to staff working in the sector;
- taking forward the recommendations set out in the Fair Work in Scotland's Social Care Sector 2019 report[20] which specifies that key stakeholders in the social care sector should apply the Fair Work Framework and commit to improving opportunities for progression for social care workers;
- work by SSSC to understand barriers and enablers to progression and identifying options for improvement, including facilitating interchange and movement between health and social care;
- undertaking research into the local and national labour markets for social care, which will also identify factors that influence employees to join or leave social care.
Registration and qualifications in the social care workforce
The majority of the social services workforce must register with the SSSC within six months of starting work. With the exception of social work, registration does not require workers in front-line roles in social care to have formal qualifications before they enter employment. However they are required to attain the appropriate qualification for their role within five years of registration. The majority of qualifications required for registration are Scottish Vocational Qualifications (SVQs), and assess the individual's ability to carry out their role and function in a specific area of care. Modern and Foundation apprenticeships are one of the mechanisms through which this training is delivered.
A number of actions are under way to support this skills development:
- Scottish Care and the Coalition of Care and Support Providers in Scotland (CCPS) are working closely with the SSSC and Skills Development Scotland to ensure planning is in progress to support employers and the workforce to attain the qualifications they need for registration with the SSSC. As part of this work, the SSSC have analysed training provision and the qualifications of those on the register. The results will be used in considering how best to focus support.
- Scottish Government is also working with the Scottish Funding Council and Skills Development Scotland to ensure adequate training capacity is in place to support the expansion of the early learning and childcare workforce
- Scottish Care and CCPS are working with SSSC and Skills Development Scotland to support independent and third sector providers to access Modern Apprentices. This recognises that smaller employers in the third and independent sectors may find the level of support required for Modern Apprenticeships hard to resource. The demand for MAs from the registration of support workers in housing support and care at home is also likely to increase.
- Work on how best to support innovative approaches and encourage further uptake of Modern Apprentices in the sector will be explored over the next year.
- Scottish Government provides grants to the third sector to assist with training requirements for registration. Since 2008 funding of nearly £11.5 million has supported over 12,000 individuals to attain their qualifications. Grants are currently available for workers in Care at Home and Housing Support, nearly half of whom are employed in the third sector.
Attracting and retaining registered nurses in care homes
As part of the National Care Home Contract reform, COSLA and Scottish Care have established a Workforce Subgroup to consider the challenges facing care homes for older people. Attracting and retaining registered nurses in care homes is a key aspect of this work and actions being taken include on this include:
- Defining the role of nurses in care homes and introduce new roles such as more Advanced Nurse Practitioners;
- Developing a suite of education and training materials that care home staff can access including exploring access to NHS training, specialist training for care homes and a more streamlined mentorship programme;
- Working with the education sector and providers to ensure support for training and learning including pre-registration training support and mentoring;
- Promoting the image of care homes as a good place to work - in particular for students and registered nurses;
- Developing a skills and competency framework/passport for registered nurses and care support workers working in care homes to reduce the need to retrain staff who may move from one care home to another and to help support revalidation for nurses working in care homes.
- Additional support from the Scottish Government to Scottish Care in 2019-20 to enable engagement of the independent sector in these workstreams.
There is also work underway across the health and care workforce to improve training and career development:
- We are investing and supporting career development in our workforce through Project Lift, identifying and developing our leaders of the future at all levels. Recognising that leadership development is not a 'one size fits all' it provides a range of opportunities - informal and formal, including individual and collective approaches. More than 3,000 staff have registered with the App and around 1,600 have completed the self-assessment questionnaire, which identifies leadership strengths and areas for development. Our talent management database uses that to match individuals to opportunities. Over 100 Career Conversations have been offered to aspiring directors and we have developed a new bespoke Scottish leadership development opportunity for this cohort, named Leadership³. Moving forward, we are commencing a pilot with SSSC to extend these development opportunities beyond NHS staff and those working in Health and Social Care Partnerships into the social care workforce;
- As part of our Global Citizenship programme, an innovative project is being taken forward by our remote and rural NHS Boards and Edinburgh University. The project is testing whether designing medical consultant roles which enable work overseas alongside service delivery in our Rural General Hospitals can attract and retain staff in permanent roles by giving them the career development they are seeking, while also making services sustainable in locations where this has been a challenge such as our rural island communities;
- An additional £3.9 million over three years is being invested in training and education for district nurses;
- We are taking actions to ensure more flexible postgraduate medical training. The future needs of the population demands more generalist care, where our medical workforce can implement new technologies and innovations in patient care, and more easily change career paths;
- We are working with the General Medical Council (GMC) and others to ensure that medical credentialing is implemented. This affords national training bodies and employers more influence over the training content for doctors and the means to more rapidly upskill doctors to support national priorities;
- In the new GP contract, we have refocussed the role of GPs as Expert Medical Generalists in the community. This includes a renewed focus on improving quality, providing clinical leadership and focusing on undifferentiated and complex patient care, within a multi-disciplinary environment. We have also redesigned our GP Specialty Training posts, improving the quality of training and making them more attractive.
Upskilling Clinicians
In response to a recommendation by the Shape of Training Group (which advises Scottish Ministers on medical intake numbers) the Scottish Government is training and developing the medical workforce to meet the changing needs and priorities of patients and service providers, particularly in terms of new technologies. This involves developing credentials in medical skills that are approved by the General Medical Council (GMC).
A clear need identified is to upskill clinicians to deliver Mechanical Thrombectomy (MT) across Scotland.
MT is a new procedure used to treat stroke patients; the earlier the procedure is done (within 24 hours of the onset of the stroke) significantly contributes to improved patient outcomes, particularly in terms of reduced long-term disability.
Given the lack of trained doctors to perform MT, the Scottish Government in partnership with NHS Tayside has prioritised the upskilling of Interventional Radiologists to be able to provide MT.
Under the supervision of an experienced neurointerventional Radiologist skilled in MT, a bespoke training programme is now underway and includes:
- Investment in state of the art simulation facilities for the training of MT in Dundee with a view to developing a training centre;
- The combining of mechanical simulators with the unique Thiel cadaver model based in Dundee, which helps provide accelerated practical learning and will be the basis for initial external assessment of the participants, and is supported by the University of Dundee for the clinical training aspects and post-procedure care. The early outcomes are to have a cohort of upskilled IR consultants able to deliver a 24/7 service for the North region and for these MT skills to be recognised as GMC-approved credentials.
Digital Skills
As set out earlier, technology has the potential to have a positive impact on workforce demand, but we need our workforce to have the necessary digital skills to take advantage of these opportunities. Workforce development is an important part of the Digital Health and Care Strategy[21] and focusses on four key areas of skill development:
- Digital Leadership: The skills required by all staff at all levels to champion digital as an enabler in transforming health and care;
- Workforce Skills: The digital skills required by the general workforce to effectively deliver services to meet patients' and service users' expectations;
- Workforce Skills (specialist): The skills and development of those in specialist digital roles (ICT staff) to deliver digital solutions in health and care;
- Future Workforce: The skills that will be required and shaped by our ongoing transformation of services, in line with patient and service user demand.
NES and SSSC (working with COSLA and Health and Social Care Partnerships), are taking forward a programme of work to support implementation of this in the health and social care environment and providing the necessary leadership to drive changes. This approach includes:
- partnership with the Scottish Government's Digital Academy, to improve access to high quality digital skills training;
- developing digital leadership skills through partnership with bodies such as NHS Digital Academy and others;
- working with our universities and colleges to ensure that digital skills are an integral part of education and training for our future workforce;
- building capacity and capability across specialist digital, IT and data professions;
- promoting existing and new solutions that enable more mobile and flexible working;
- identifying solutions that bring the most modern of technologies to our business and administrative requirements, freeing up staff to focus on frontline services;
- providing productivity and collaboration services and tools, such as shared calendars, email, video and instant messaging, to support effective, efficient and secure ways for working across organisational boundaries.
Returners
Staff who have recently left or retired from health and social care services have a wealth of knowledge, skills and experience that we do not want to lose. We already have some schemes to encourage staff from the health workforce to return, and we are looking to develop these further and wider across the health and social care workforce. We are:
- Establishing a 'one point of contact' co-ordinated process to support AHPs who wish to return to practice;
- Enhancing our GP retainer scheme which enables qualified GPs who are currently unable to commit themselves to a full-time post, to continue working part-time in general practice and enter a permanent post when their circumstances permit;
- Creating a flexible resource of recently retired or part-time doctors, who are willing to take on short-term work to support our Rural General Hospitals. To date 30 Surgeons and Anaesthetists have expressed an interest in the Clinical Collaborative which was launched in March, and already, services in Fort William and Stornoway are being supported;
- Launching an innovative Professional Practice Adviser pilot offering recently retired nurses and midwives the opportunity to coach and advise newly qualified staff in midwifery, health visiting, district nursing and advanced nursing practice settings;
- Encouraging former nurses and midwives to return by providing the opportunity for them to undertake a Return to Practice programme. Since April 2015, almost 600 former nurses and midwives have taken up the opportunity to retrain.
Support to the Existing Workforce
While working in health and social care is extremely rewarding, we recognise the pressures that come with such roles and we need to do all we can to support staff and encourage them to stay in their roles.
Listening and acting upon staff concerns and issues is a key element of any successful organisation. One of the aims of the Health and Care (Staffing) (Scotland) Act is to improve working conditions for NHS clinical staff. Staffing levels are matched to workload and employers are required to take the views of staff and staff wellbeing into account when making staffing decisions. The legislation also puts in place real-time staffing assessment and escalation procedures that will ensure the professional voice is heard.
This is also being supported through the iMatter model, a continuous improvement tool designed to help individuals, teams and Health Boards understand and improve staff experience by taking actions at these different levels within the system. iMatter was initially used by NHS Boards, and is now being used in almost all of Scotland's Health and Social Care Partnerships and has recently been successfully tested in East Renfrewshire Council with their staff. Key to the system is that staff at all levels feel empowered and enabled to make improvements to support improved patient and client experience.
We also need to provide support for staff who are training and/or working in health and care to deal with the pressures of that career. Some examples of this to address issues doctors were facing include the new Lead Employer model introduced for all Doctors in Training. This new arrangement provides a continuous contract during training that avoids tax code complications and makes it easier for doctors in training to secure mortgages, as well as avoiding unnecessary administration related to changing employer.
For GPs, a package of support has been developed within their first five years of qualifying. This includes a mentoring scheme and training for a new group of 40+ mentors in 2018/19. We are also supporting Continuing Professional Development access and Quality Improvement project opportunities for up to 200 "First 5" GPs each year. Wider support for GPs also includes the rollout of the existing confidential wellbeing service GP across remote and rural areas of Scotland and a new coaching service launched last year and has now extended to 125 places in response to demand.
Recognising the particular issues faced by our workforce from other parts of the European Economic Area (EEA), we are ensuring that all such staff have access to advice and information and are supported through the process of applying for EU Settled Status. Through the Scottish Government's 'Stay in Scotland' campaign, this includes a support and advice service for EU citizens with more complex needs or particular challenges and a toolkit for employers.[22]
Pay and Reward
Pay and reward is an important factor in attracting and retaining our health and social care workforce and we continue to take action to ensure that these careers remain attractive employment options:
- While we recognise there have been some challenges in implementation, the introduction of the Real Living Wage for those working in adult social care has had a positive impact on pay in the sector;[23]
- In 2018, a three year pay deal for NHS Agenda for Change staff (which includes all nurses, paramedics, healthcare scientists and allied health professionals) was agreed from 1 April 2018 to 31 March 2021. This will restructure pay bands meaning higher starting pay and a shorter journey to the top of scales, as well at least a 9% pay rise over 3 years for all staff;
- On 27 August 2019, a pay uplift of 2.5% for medical and dental NHS Scotland staff from 1 April 2019 to 31 March 2020 was announced. The announcement means junior doctors working on typical rotas in Scotland can be up to £6,000 a year better off than their English equivalents, and specialty doctors, associate specialist doctors and consultants will remain the best paid in the UK. This will help ensure that NHS Scotland remains an attractive employment option for medical and dental staff;
- We are also targeting specific financial incentives where it will help to attract staff to train or work in rural area. Actions include:
- expansion of the GP Golden Hello scheme from 44 to 160 practices in rural and remote areas, offering £10,000 for GPs taking up post in their first eligible rural practice;
- a £20,000 bursary for GP trainees taking up placements in rural and other harder to fill areas. 101 GP trainees have taken this offer up in 2018, an increase from 60 in 2017;
- an enhanced relocation package is being offered to GPs moving to work in rural practice to cover expenses such as removal costs, rent etc. The maximum rate has been increased from £2,000 to £5,000.
Efficient Use of the Workforce
Alongside growth and retention, we need to make more efficient use of existing resources. This will involve a range of approaches, including improvements in rostering. We are procuring a NHS wide e-rostering system which will lead to implementation of a fully automated rostering system for all staff groups. This will create efficient rosters with full gap analysis and be responsive to real time situations, ensuring the most efficient and effective use of staffing resources clearly linked to demand. Alongside this a national rostering policy is being developed, which will provide roster rules and ensure more effective rosters, reducing the reliance on supplementary staffing where poor rostering is a cause.
Implementation of the Health and Care (Staffing) (Scotland) legislation will contribute to the efficient use of the workforce by providing consistent and robust analysis of the workload associated with patient need and real time assessment of staffing in those areas covered by the common staffing method to ensure safety and efficiency.
We are also looking at how new service models can maximise the efficiency of the existing workforce. An example is set out below.
Maximising workforce efficiency
The Reporting Radiographer pilot is testing how we might maximise efficiency of the current Radiology workforce and create greater capacity. It will assess the potential for a national Radiographer Reporting service by:
- Nationally coordinating Radiographer "plain film" reporting capacity and activity testing the new IT connectivity;
- Assessing the potential to utilise consultant Radiographer skills across boundaries;
- Assessing the potential to utilise a cross boundary consultant Radiologist support model;
- Establishing whether a Radiographer plain film reporting service could better utilise the existing workforce.
It will measure whether, in reality, there are sufficient numbers of reporting Radiographers to ensure adequate cover for the service. This will also allow us to quantify the workforce required to optimise this service and present an opportunity to manage this capacity differently. The pilot commenced in March 2019.
Improving Workforce Planning Across Health and Social Care
To most effectively plan for the future health and social care workforce, taking account of the changing demand and supply issues, we need to develop our workforce planning infrastructure. We will:
- further develop workforce planning capability;
- clarify roles and responsibilities on workforce policy and planning;
- encourage more consistent use of workforce planning tools across sectors;
- provide workforce planners across sectors with access to better data.
Further Develop Workforce Planning Capability and Examine Capacity
We need the health and social care sector to have the capability to develop more effective workforce plans and to understand, and use, scenario planning methodology that reflects their particular requirements.
Revised workforce planning guidance for NHSScotland, Integration Authorities and their commissioning partners in local authorities is being published alongside this Plan. The guidance introduces improvements to the existing workforce planning process and proposes a more collaborative approach in an integrated landscape. As workforce planning requirements and practices differ substantially across health and social care organisations, the guidance signposts a range of existing methodologies and encourages all health and social care employers to use these in planning for the workforce they require. It also references the need to consider the implications of planning activities for third and independent sector employers delivering commissioned services.
In addition to planned actions to improve the capability of existing workforce planners, the National Workforce Planning Board has also committed to examining the issue of capacity for workforce planning across social care employer sectors. Work will be designed by the Scottish Government, COSLA and partners, to improve understanding of workforce planning capacity and to make recommendations accordingly.
To further support development of the competencies and skills required to effectively undertake workforce planning roles across Social Care employers, NHS Boards, IJBs and Primary Care, we will:
Design and oversee work to obtain a national picture of workforce planning capacity, methodology and capability in Local Authorities/ Health and Social Care Partnerships for planning social care services. We will respond by considering how best to support effective collaborative and strategic workforce planning in light of the findings.
Over the next 12 months, Scottish Government and COSLA will work with the Scottish University and College sectors to examine, develop and build a workforce planning educational qualification as part of a strategic approach to developing workforce planning education and skills for the health and social care workforce.
Provide additional support in 2019/20 to the third and independent sectors to enable their contributions to the developments in workforce planning to be supported through this Workforce Plan.
Clarifying Roles and Responsibilities
As we improve workforce planning in an integrated way, it is important to be clear about respective roles in workforce policy and planning. The guidance being issued alongside this Plan sets out these roles for workforce planners nationally, regionally and locally across the sectors.
Greater Consistency of Workforce Planning Tools Across Sectors
Workforce planning requirements and practices differ substantially across health and social care organisations. A level of variation is entirely appropriate given that an independent company with a few employees will have very different workforce planning needs than an NHS Board with thousands of employees. Nonetheless if we are to workforce plan in an integrated way, there is benefit in a level of consistency in the methodological approach used. The guidance we are issuing along with this Plan signposts a range of existing methodologies and encourages all health and social care employers to use these in planning for the workforce they require. It also considers the implications of planning activities for third and social sector employers delivering commissioned services.
On workforce planning tools, the Nursing and Midwifery Planning tool has already been reviewed and improved and we are exploring workforce prediction tools for skill-mixed AHP services. A scoping exercise has reviewed and mapped the landscape of workforce planning tools within the Scottish Government, NES and ISD. Following this, work will start on ensuring consistency and transparency between tools, filling gaps where appropriate.
Improving Workforce Data
Better workforce data will support more informed decision making. Significant progress has been made on creating a single workforce data platform, and work is under way to better understand the labour market for social care.
As recommended in Part 1 and Part 2 of the National Workforce Plan, NES have brought together existing workforce data sources in a new supply side platform, which was launched in April 2019. Data from the platform is already being used to inform decisions on controlled group numbers, to identify workforce gaps, and develop enhanced roles and new staffing models to mitigate them. Work will continue to identify and add to the data available and to refine social care and primary care data, so that as the platform evolves, health and social care workforce data can increasingly be accessed in one place and analysed using an integrated approach. Extensive data on the social care workforce is already published as official statistics by the SSSC and is available for interrogation in an interactive data visualisation tool.[24]
The work being taken forward by NES is complemented by the legislative requirement being placed on Healthcare Improvement Scotland (HIS) in the Health and Care (Staffing) (Scotland) Act 2019. Under the Act, HIS is required to monitor Health Board compliance with staffing duties, monitor and review staffing tools and methodology and develop new staffing tools. In doing so, HIS, and NHS Boards, will generate robust data on the workload required to deliver high quality care which will, in turn, inform and improve workforce data. The procurement of an NHS wide e-rostering system, in addition to creating efficient rosters, will provide further data evidence clearly linking efficient and effective use of staffing resources to demand.
The Scottish Government has also commissioned NHS National Services Scotland to develop an online tool to collect workforce information as part of the National Primary Care Workforce Survey, which ISD regularly carries out on behalf of Scottish Government. This is an important source of information to support workforce planning for primary medical care services. This workforce data may also be used to develop workforce metrics to support sustainability work at a board, cluster and practice level.
Existing staffing tools and methodology for nursing and midwifery already contribute to improving workforce planning across health by providing access to better data. This will be further improved by effective implementation of the Health and Care (Staffing) (Scotland) Act and the oversight provided by HIS. HIS will continue to improve the existing tools and develop new tools with a focus on developing multidisciplinary tools and including staffing groups beyond nurses and midwives. The Act will also require Health Boards to report annually on how they carried out their staffing duties. This will create transparency in the staffing decisions being taken across all boards and better inform national workforce planning.
As we set out in this Plan, there are significant challenges in the supply of staff for social care. As indicated earlier in this Plan, a better understanding of national labour markets can help employers to understand issues and trends and plan ahead. The research we have commissioned on national and local labour markets and their interactions with the Social Care and Early Learning and Childcare workforce will incorporate ongoing analysis by the SSSC into movements within the registered social services workforce. The findings will aim to help workforce planners to anticipate and manage recruitment and retention issues.
Delivering the Plan
This first Integrated Plan will help achieve better integrated workforce planning across health and social care in Scotland. It initiates a programme of work for the future, covering many different employers and settings. And it sets a steady future direction for those who plan for the workforce in this complex landscape.
Getting this right is of national importance - everyone in Scotland will rely on this workforce at some point in their lives.
That is why this Plan highlights the need to build our workforce; to strengthen the workforce planning infrastructure; to build on our knowledge of the effects on our workforce of changing demand, services, technologies and population; to sharpen our analytical skills and competency, locally, regionally and nationally; and to co-ordinate these actions effectively to ensure the highest quality of health and social care services.
Building on earlier recommendations made in Parts 1-3 of the National Workforce Plan, this integrated Plan sets out a series of specific actions to meet demand and to grow the workforce. These actions focus on enhancing training numbers across a broad base of professions involved in delivering national priorities for health and social care. They augment and complement existing Programme for Government actions, and we have carried out scenario planning which for the first time takes account of estimates of demand in coming years, linking closely to Medium Term Financial Strategy projections.
The benefits of workforce modelling and scenario planning against a range of future demand factors are clear, and we will refine, improve and embed this approach as better intelligence develops. More effective links also need to be forged between workforce planning, service planning and financial planning, and the Plan's associated guidance sets out how we will do this.
Using and interrogating workforce data has been a continuing challenge for planners, due in part to a lack of a consistent approach to data collection. We continue to tackle this by bringing together existing data sources. In particular, the progress made with NHS Education for Scotland on its national TURAS data platform is beginning to yield better quality information, more consistently accessible and useable across both health and social care. The work being done with NHS Health Improvement Scotland on implementing the provisions of the Health and Care (Staffing) Act 2019 will benefit from this. The evidence needed to inform important decisions about the future shape of our services will depend on it.
All of us need to do more to observe, analyse, plan and prepare for future challenges. As the importance of effective workforce planning in this has become more widely recognised, so the demands made of planners have increased. To help address this, employers in health and social care need more people with the right skills and expertise, and an infrastructure which supports their development. The large numbers of providers, of many different sizes, across a complex landscape present particular challenges. This Plan therefore sets out what we will do to strengthen workforce planning capacity and capability across the health and social care sectors.
Along with this Plan we are publishing revised Workforce planning guidance, co-produced with members of the National Workforce Planning Group. The guidance has been developed for use by NHS Scotland, Integration Authorities and their commissioning partners in local authorities. It will be kept under review, and added to, as part of more regular and structured communications on workforce planning issues with employers.
The actions detailed in this Plan form a programme of work which will be overseen by the National Workforce Planning Group's Programme Board, in addition to its existing role in delivering earlier recommendations and commitments from Parts 1-3 of the National Workforce Plan. With representation from across health and social care, the Board will reflect contributions from all parts of the system.
The Board will also be responsible for publishing regular future iterations of the Plan. These will reflect further progress in our understanding of workforce demand and supply and add to the sum of our collective knowledge and intelligence around workforce planning issues. Importantly, future iterations of the Plan will link more closely to developing policies, such as work progressing on reform of adult social care.
Individually, the actions set out in this Plan will therefore enhance our capacity and capability, deliver tangible improvements, and provide a better evidence base in an integrated context.
But taken together, they elevate workforce planning to the strategic, whole-system position it needs to inhabit - right at the core of high quality health and social care services, now and into the future.
Contact
Email: nichola.hattie@gov.scot