The modern outpatient: a collaborative approach 2017-2020
Healthcare strategy providing opportunities for transformation which improves efficiency and puts individuals at the heart of their own care.
10. Engagement
10.1 The Programme will drive a major cultural and operational shift in the understanding of what an 'outpatient' actually is across the health and social care landscape in Scotland. Accordingly, the engagement and consultation process must ensure that all relevant stakeholders have an opportunity to contribute to and shape the approach.
10.2 The document was widely communicated to and discussed with stakeholders between December 2016 and February 2017. The first stage of engagement resulted in a 30,000 word strong written response from critical communities and stakeholders.
Simultaneously, a National Stakeholder Engagement Event was hosted an attended by over 200 delegates.
10.3 The engagement process will be used to:
- test the assumption that change is necessary, develop solutions that are collaborative and ensure that outcomes will be beneficial;
- ensure that the principles of patient safety and clinical decision-making fit with the model;
- understand implications and interfaces with other national programmes of work, with particular regard to sequencing and timeframes for delivery;
- identify any emerging concerns which need to be addressed in the short term; and
- identify any major risks or issues which may impact on the Programme in the mid to long term.
10.4 The Modern Outpatient consultation: Summary of responses
The Modern Outpatient Programme consultation document was published online in December 2016 as part of a three month consultation mechanism which sought to engage with key stakeholders, identify existing good practice and build collaboratively on innovation related to the delivery of the programme. Participants were invited to contact the programme director directly with responses. In February 2017, an open engagement event took place which provided a forum to offer views for over 200 attending delegates: an anonymous questionnaire was available during and after the event.
The total responses received from individuals, staff, patient organisations and professional bodies amounted to over 30,000 words: a summary of the collective response is detailed below.
We asked
The Cabinet Secretary for Health and Sport encouraged readers of the consultation document to consider whether the ambitions and proposals within the programme were the right ones and how best to redesign services for the future benefit of patients: the same question was asked of the delegates attending the open engagement event.
You said
A variety of opportunities and challenges were interpreted from the document. Across all submissions, commonly cited responses were that the overarching ambition and vision was broadly welcomed; respondents suggested placing the programme within wider public health strategy. Further description of underpinning evidence and implementation plans for elements of the programme was requested, and respondents placed particular emphasis upon the role of allied health professionals, digital infrastructure and systems, resource and workforce capacity, training for extended roles, and 'culture change' including professional and patient behaviour and expectations. Respondents anticipated concerns relating the approach to patients with multi-morbidities, and the effect on patient-clinician relationships. Description of the governance, monitoring and evaluation of the programme was recommended to support delivery of the stated aims within the timescale. It should be noted that these preliminary themes reflect the most commonly emerging categories across all of these data, rather than an exhaustive account of all responses received.
We did
All written consultation responses were categorised to enable a descriptive account to be produced using initial themes. Verbal responses from the engagement event and questionnaire data were also examined for any additional issues which had not emerged. The findings have been taken in to account by the programme director during the finalisation of The Modern Outpatient Programme document, which is due to be published in April 2017. As the programme develops, ongoing collaboration with citizens is anticipated and encouraged.
Initial categories
Figure 1: Cluster diagram showing most common initial categories emerging from responses as a whole.
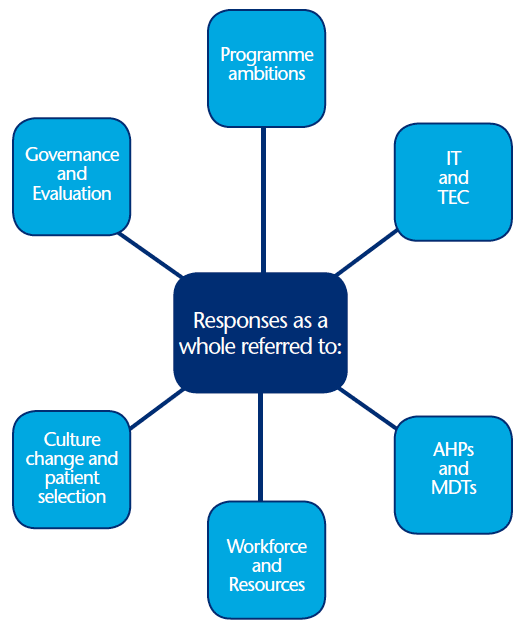
Key:
TEC
Technology-enabled care
AHP
Allied health professional
MDT
Multi-disciplinary team
Initial themes
Programme ambitions
Many respondents supported the guiding aspects of the programme as set out in the document; there were some requests for further description of the evidence underpinning some programme aspects, more detail of the synergy between the modernisation of outpatients and other divisions of healthcare alongside integration in to the wider health and social care system and public health strategy, and requests for a specific action plan.
Focus on information technology and technology-enabled care
A number of respondents supported the described potential of digital technology to facilitate decision support, as well as suggesting a need for linked-up IT infrastructure and data systems to support clinicians to work collaboratively. Some concerns were raised about standard access to broadband services and the timely co-ordination of information across information systems. Examples of comments include:
…traditional ways of doing things must be challenged. Technology enabled care and the use of Allied Health Professionals are pivotal to this change of mind-set...
Broadband and mobile connectivity is not available equitably across Scotland… and the multi-disciplinary team still cannot access all the patient data they require…
Focus on allied health professionals and multi-disciplinary teams
Further description of the role of allied health professionals and a model of the multi-disciplinary team across divisions of healthcare was encouraged by a number of respondents, and a suggestion to elaborate on the approach to multi-morbidities was also commonly cited. Examples of comments include:
…there needs to be a bigger focus in the paper on how we build the multi-disciplinary team model… maximising the roles of the wider team will be crucial…
The document tends to deal with single pathology data; some thought should be given to how we coordinate teams of specialists to see complex multi morbid patients at single visits?
Focus on workforce and resources
Respondents highlighted further opportunities to describe collaborative work with existing programmes and organisations, and many supported the ideas presented relating to increased engagement across boundaries and expansion of training for extended roles. Concerns relating to the description of the implementation of the programme with respect to workforce capacity were raised and clarity relating to training and resource planning was requested. Examples of comments include:
[Staff] will have a crucial contribution to emerging community collaborative work. It would be useful to further describe in the paper support that will be provided to develop new workforce model testing, training and decision support access…
The document does not address clearly enough how the different spheres of control in planning and resource allocation between NHS boards and Integration Authorities will cohere to support the transformation...
Focus on culture change and patient selection
The description in the document of the potential for patients to become more empowered in their own health care was welcomed, though respondents sought reassurance that individual suitability for increased self-management was considered. Many respondents suggested reference to the patient and professional engagement and leadership which would be required to successfully implement the collaborative approach described. Examples of comments include:
"Transforming patient experience and timely access to advice, treatment and support will also require a cultural journey in expectations."
"[Be] mindful that this is not suitable for all patients."
Focus on governance and evaluation
Respondents suggested clarity relating to evaluation and governance arrangements and frameworks within
the paper, including associated outcome measures relating to process, quality and consideration of unintended consequences. Some respondents suggested open sharing data relating to outcomes to drive development of the approach. Examples of comments include:
We would be keen to see the inclusion of an explicit measurement of any unintended consequences on other parts of the system.
[We suggest] governance and data frameworks [are] developed for quality assurance and quality control.
10.5 Engaging the wider network of stakeholders, as part of an iterative process, will be required to ensure a reflective, critical and collaborative approach to the design, implementation, and measurement of the Programme. On-going stakeholder engagement will include:
- Patients, carers and service users
- Primary Care clinicians
- Chief Executives
- Joint Integrated Boards
- Medical directors and lead clinicians
- Nurse directors
- British medical association ( BMA)
- Royal Colleges eHealth and other technological innovators
- Scottish Health Council (lead partner for patient engagement)
- The Alliance (to ensure Third Sector engagement).
10.6 There has been significant clinical engagement to date with regard to the improvement examples threaded through-out this document. Clinical colleagues have been and will continue to be key to driving change forward locally. This engagement and enthusiasm will continue to be built upon. The following comments are from clinicians actively involved in redesigning their services:
"With ever increasing demand and financial stress, traditional ways of doing things must be challenged. Technology enabled care and the use of Allied Health Professionals are pivotal to this change of mind-set. The historical referral patterns need to be challenged with care closer to home. Only those patients who need to be seen in the hospital setting should be seen there."
Mr Edward Dunstan, Director Of Surgery, NHS Fife and Chair: Scottish Committee for Orthopaedics and Trauma
"The National Ophthalmology Workstream has been a massive step forward for Scottish Ophthalmology. The focus on review (as well as new) patients marks a sea change in thinking that is directly benefiting ophthalmic patients.
"The national peer review visits have generated a new focus on eye departments and shone a light into the difficulties created by the necessary growth in new treatments. This has helped in moving forward with innovations and efficiencies in the current systems of care and highlighted the need for governmental support with the ongoing challenges."
Dr Graham Cormack - Consultant Ophthalmologist, NHS Tayside
"The National Ophthalmology Workstream has identified clinician based concerns and Scottish Government has worked with clinicians to identify solutions. The thrust has been on sharing good practice between peers across the country with the focus firmly on patient focussed models of care."
Professor Carrie MacEwen - President of the Royal College of Ophthalmologists
"I have had the fantastic opportunity to work alongside colleagues in Scottish Government as the National Lead for the Scottish Gastroenterology DOIT Collaboration. This has given me the opportunity to work closely with colleagues nationally across the clinical spectrum to design clinical models of care for gastroenterology patients that will be responsive to their needs, safe, sustainable and to the highest clinical standards. These models of care will only be deliverable however if we foster a culture of national, regional and local clinical leadership, engagement and cooperation between our clinical staff.
"Historically, there has been a perception within the NHS that changing anything is too difficult due to the complexities of the organisation, limitations of budget making service change difficult, clinical pressures preventing protected service development time and the development of an "us and them" culture i.e. clinical staff not seeing themselves as
being able to influence their clinical environment so it is therefore "not their problem". My hope is that through the Collaboration we can start to implement some of the required service changes identified in our supported working groups and this tangible outcome will encourage further engagement amongst colleagues who have not yet participated in our quality improvement programme. The implementation of such change will need strong leadership at all levels and all disciplines to drive this change forwards."
Dr Alan Clarke - Consultant Gastroenterologist, NHS GG&C, Clinical Lead National Gastroenterology Collaboration
10.7 As part of the commitment to secure and maintain on-going engagement the key themes which have emerged from the initial engagement stages will be considered, addressed and integrated within the Joint Governance and Accountability arrangements and forward planning considerations.
'Our Common Interests'
Greater patient, carer and service user participation and engagement in service redesign.
Promoting better and effective communication about care and coordination of care.
Addressing cultural and silo barriers by working collaboratively in a co-produced way which enables both national and local innovation.
A stronger focus on quality outcomes and monitoring of unintended consequence of new ways of working on patients, carers, clinicians or staff.
A focus and appreciation of the role of the wider multi-disciplinary team which is underpinned by timely training and availability of workforce in advance of any significant service redesign.
Access to data, both patient and clinically held, to support clinical decision making for all clinicians involved in managing patient care.
Contact
Email: Pauline Fyfe, pauline.fyfe@gov.scot
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG