Maternity and neonatal (perinatal) adverse event review process: guidance
Operational guidance to support health boards boards undertaking perinatal adverse event reviews incorporating the additional reporting required of maternity services.
4. National Framework – additional guidance for perinatal services for stages 4-6
Stages 1-3 of the National Framework are standard across all healthcare settings. However for stages 4-6, as a supplement to the National Framework maternity and neonatal services should follow the process outlined below.
A) Stage 4: Assessment and categorisation
At Stage 4 the adverse event is categorised and duty of candour requirements considered.
This is how the National Framework categories of adverse event equate to the type of review required:
Category 1 -
Type of Review: Significant Adverse Event Review (SAER)
Review Team: Full review team
Category 2 -
Type of Review: Comprehensive Care Review (CCR) or local management team review
Review Team: Service manager with multidisciplinary team input
Category 3 -
Type of Review: Local Review
Review Team: Managers / staff locally
MBRRACE-UK has established a national standardised Perinatal Mortality Review Tool (PMRT) which was launched in early 2018. The PMRT should be used and completed for all stillbirths or neonatal deaths. The process outlined in this guidance is consistent with the PMRT process, and the clinical report and report for parents generated through the PMRT process should be included as part of the Level 1 or 2 review when there is a stillbirth or neonatal death.
Definition of Category 1 Perinatal Significant Adverse Events
A number of national UK reports have defined a core set of perinatal adverse events that should be reported as Category 1 and have an SAER (e.g. MBRRACE, EBC).
1. Maternal death
2. Neonatal hypoxic-ischaemic encephalopathy (HIE) requiring therapeutic hypothermia
3. Unexpected stillbirth during inpatient stay (includes intrapartum stillbirth in any setting, using Each Baby Counts definition of intrapartum stillbirth – see Appendix C)
4. Unexpected neonatal death (>37 weeks) within 7 days of birth
5. Where triage process or a Comprehensive Care Review (CCR) (Local Management Review) identifies a need for further investigation
All other stillbirths and neonatal deaths are level 2 adverse events. Allocation of a level of review for stillbirths and neonatal deaths will be ascertained through the stage 4 assessment and categorisation process.
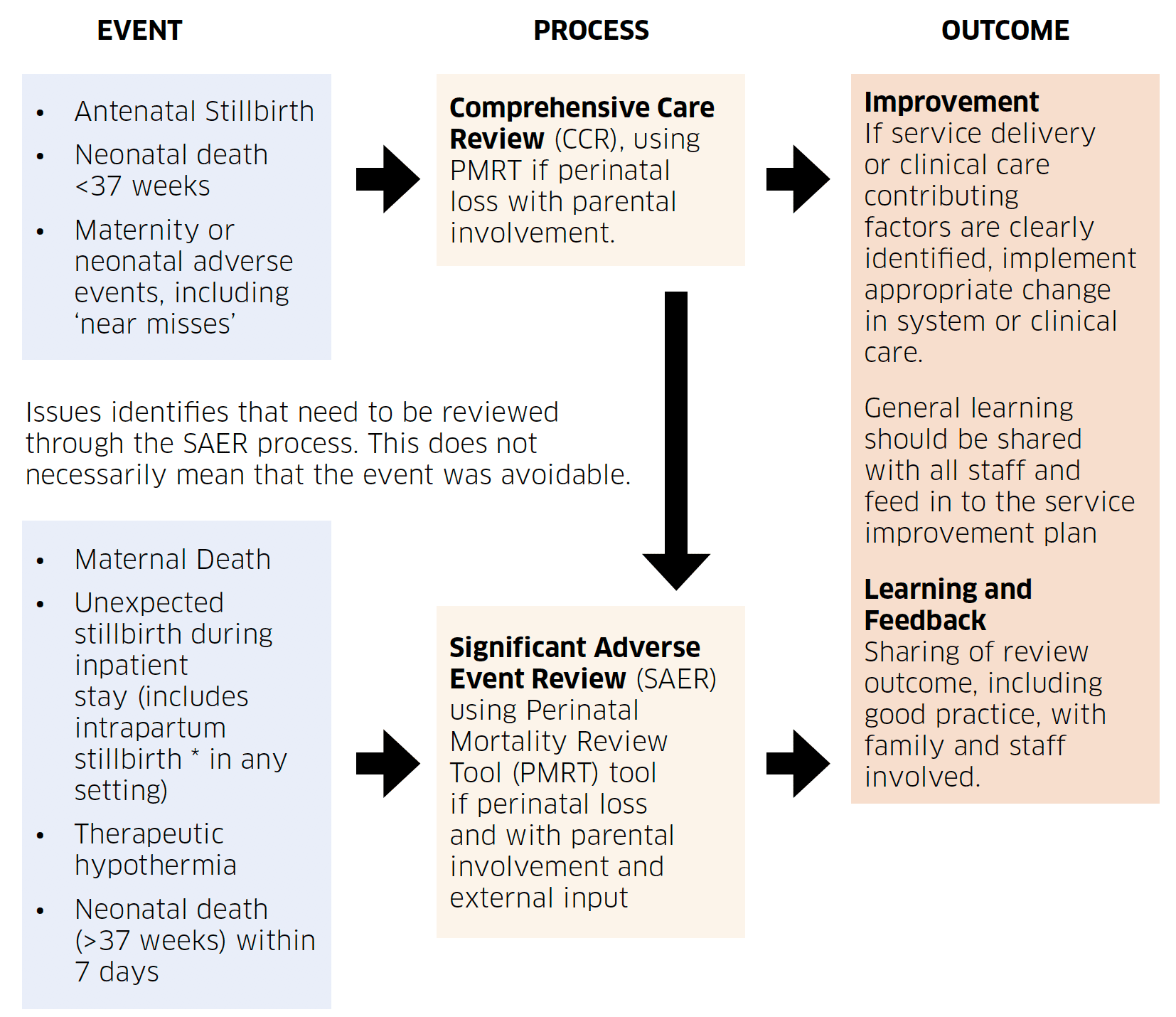
* Intrapartum Stillbirth: See Appendix C
Duty of Candour
The Duty of Candour Procedure (Scotland) Regulations 2018 came into force on 1 April 2018. The Regulations place a statutory duty on organisations that provide health, care and social care services to be open and honest when an unintended or unexpected incident occurs that results in death or harm, by following the Duty of Candour Procedure. Guidance has been produced for the organisations that provide health and social care services and other interested parties.
Organisations must now tell those affected, or acting on their behalf, when an unintended or unexpected incident resulting in death or harm has occurred during the provision of health or social care. Organisations must offer a written apology and carry out a review of what happened, fully involving the person who has been harmed, or their representative, at each stage of the process. In a SAER, the Lead Reviewer should consider whether the SAER process meets the requirements of the duty of candour procedure.
B) Stage 5: Review and analysis
At Stage 5, the review itself is established and undertaken, involving the patient/service user, their family and staff. The HIS National Framework provides guidance on methodology of review, reporting and communicating findings.
National Audit Reports (e.g. MBRRACE, PMRT) have made recommendations relating to reviews into maternity and neonatal adverse events. Taking account of these recommendations, maternity and neonatal adverse event reviews and comprehensive care reviews should incorporate the following additional features into their review process.
1. External panel input
1. SAER: PMRT and MBRRACE[8] recommend including an independent external member to support robust review.
For SAERs in maternity and neonatal care in Scotland that external input should be provided by a clinician from another Health Board. This input could be provided in person or by videoconference.
2. CCR (LMR) Recognising the value external input brings to reviews but being cognisant of the manpower required to achieve this with the number of CCRs, it is proposed that one or two professionals external to the Board will review all CCR reports from each Board on a yearly or twice-yearly basis (based on size of Board and number of CCRs).
2. Governance, and operational management of the review process
Health Boards should have a governance process for perinatal adverse events reviews. This process should provide oversight for commissioning, recording of information, closure, completion of action plans, feedback to families and staff and sharing learning. Defined standardised operational processes (SOPs) are needed to support the delivery of the perinatal adverse event review process.
In line with the National Framework, staff roles and responsibilities for the operational process should be clearly defined.
The roles should include coordination/administration of the process and a perinatal clinical leadership team.
The diagram below outlines an example of a process map for adverse event management in maternity and neonatal services.
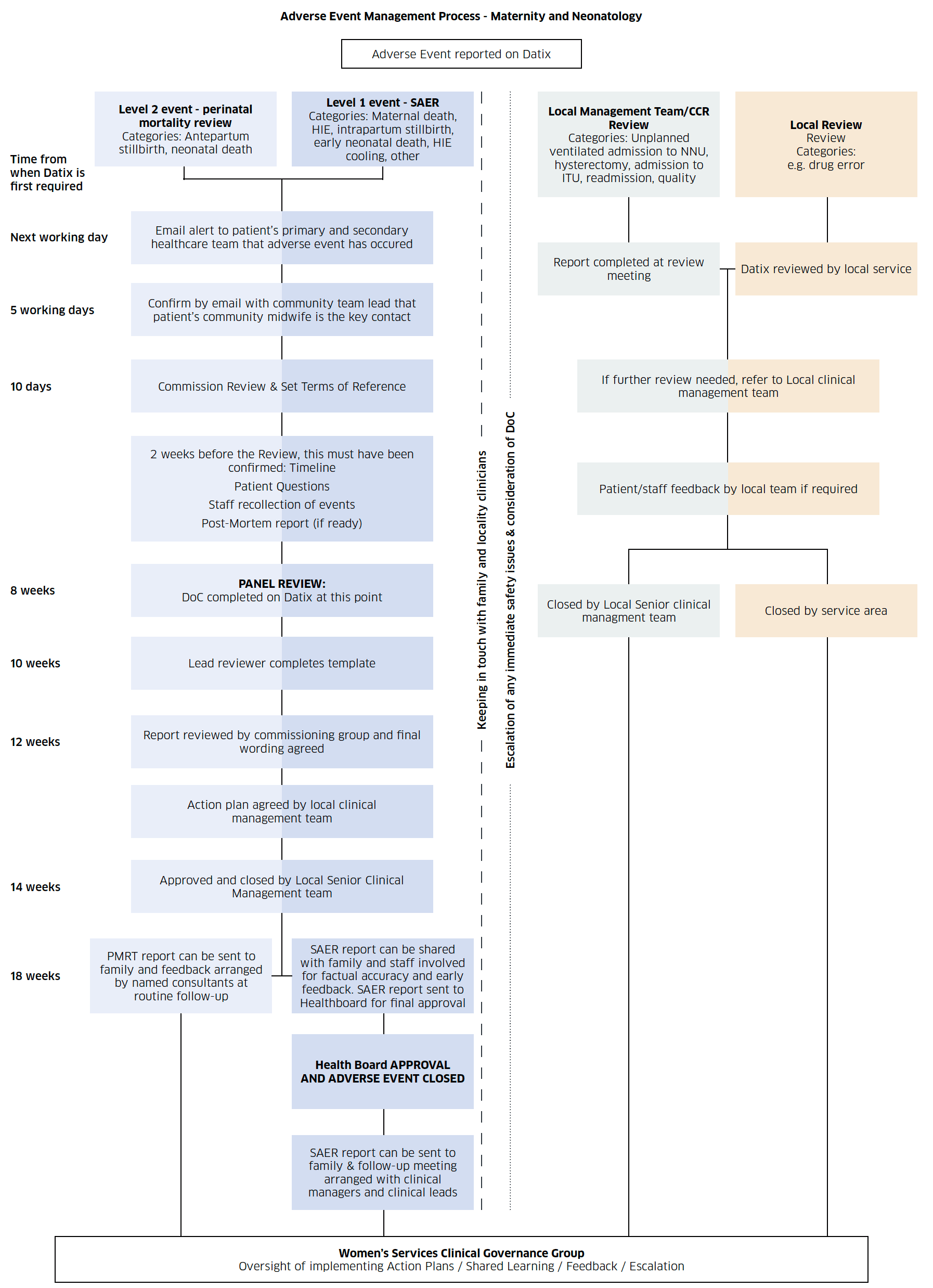
The table below summarises governance and panel composition for different types of review.
Figure 4: review team composition
Core Review Team
| Governance (including report sign off) | SAER | Perinatal Mortality Review (PMRT)* | Comprehensive Care Review (local management review) | Local Review |
|---|---|---|---|---|
Category 1 Health Board governance structure |
Category 1 or 2 | Category 2 Perinatal services management/clinical governance structures |
Category 3 Perinatal services management/clinical governance structures |
|
| Chair | 1 | 1 | 1 | 1 |
| Vice-Chair | 1 | 1 | X | X |
| Admin Support / Scribe | 1 | 1 | recommended | X |
| PMRT Champion | 1 | 1 | X | X |
| Obstetrician | 2 | 2 | *MDT panel where applicable | *MDT panel where applicable |
| Midwife | 2 | 2 | ||
| Neonatologist / Neo Nurse (for all NND or where resuscitation commenced) | 2 | 2 | ||
| Risk Manager / Governance Manager /Service Manager | 1 | 1 | 1 | X |
| Bereavement Team | 1 | 1 | X | X |
| External Panel Member | 1 | 1 | X | X |
| Service /Clinical Manager | x | x | 1 | X |
| Team / Ward Manager | x | x | 1 | 1 |
| Additional Named Members for invitation to PMRT and SAER reviews where applicable | ||||
| Pathologist | ||||
| Anaesthetist | ||||
| GP / Community Healthcare | ||||
| Radiographer / Sonographer | ||||
| Safeguarding Team Member | ||||
| Service Manager | ||||
| Any other relevant healthcare professional / team * consider transport team | ||||
* Review team members may fulfil multiple roles
* please note these are minimum expected standards
* PRMT guidance sets out who should be involved in PMRT reviews for stillbirths and neonatal deaths. In practice these reviews may be SAER’s or they may be CCRs (local reviews). In either case teams should consider the recommendations of the PMRT guidance when considering membership of the review team.
3. Review analysis and PMRT
As outlined in the HIS National Framework, the panel should use a human factors and systems analysis to review the care and service delivery issues, understanding the dynamic system interactions that contributed to the event, exploring contributory factors, agreeing key issues and organisational duty of candour, capturing lessons learned and making recommendations. A report of the review findings should be sent to local clinical management and an organisational governance group.
In addition to the review process, for stillbirths and neonatal deaths, clinical teams should also complete the Perinatal Mortality Review Tool (the PMRT). This tool has been designed with user and parent involvement to support high-quality standardised perinatal mortality reviews on the principle of ‘review once, review well’. The tool should be used as part of the review process for stillbirths and neonatal deaths.
4. Involving women and families in the SAER process
When families have been affected by an adverse event this can have lasting psychological consequences, and is often distressing for the professionals involved[9 10 ]. Improving communication when discussing adverse events supports families’ emotional adjustment, helps staff cope better with the after-effects of what has happened, and provides learning for improving performance and quality in the delivery of family-centred care11.
The principles underpinning learning from adverse events and involving families in reviews are described within the National Framework. In addition to this, HIS have published Being Open In NHS Scotland - Guidance on implementing the Being Open principles[12] and the Scottish Government have published Organisational Duty of Candour Guidance, both of which underpin the National Framework for Scotland. In addition a number of national reports into maternity and neonatal services have made recommendations about involving families in adverse event reviews[13 14].
Being Open provides a best practice framework for all healthcare organisations to create an environment where patients, their families, healthcare professionals and managers all feel supported when an adverse event occurs and have the confidence to act appropriately. Guidance on applying the Being Open principles and in communicating in a supportive and effective way with families and staff has been produced by HIS and can be accessed below the following link: ‘Effective Communication about Adverse Events in Maternity Units - A guide to talking with parents, families and staff’ [15].
MBRRACE-UK has developed parent engagement pathway materials through a multi-disciplinary group within the
MBRRACE-UK/PMRT collaboration including bereaved parents and are based on the findings from the PARENTS study and the ‘Being Open’ process: Parent Engagement Materials.[16]
These are the key learning points from testing a process to involve patients and families in the review (in line with the stages of adverse event management in HIS Framework) *fig 5
| Steps | Goal | Process | Staff | When | Form |
|---|---|---|---|---|---|
| Allocate a key contact for the family | Helps the family manage and deal with distress from the event by reducing uncertainty, providing continuity, being open and honest and providing an apology | A single key contact person should be identified for the family throughout the review process (ideally this would be the woman’s primary midwife) | Staff coordinating the review process | The key contact should be identified as soon as possible and no later than the 10-day timeline for commissioning | Email to community midwife team to confirm who will be the key contact |
| Discussing the review process with the family and how they can be involved | 1. Explain how the review of their care will be carried out 2. invite them to be involved 3. provide them with written information about the review process and how they will be kept informed during the review, when and by whom 4. outline the role of the key contact and introduce them if they are present 5. note any early questions that the family have 6. apologise for any harm caused |
Senior clinician and midwife or nurse | Ideally before discharge or within 7 days of adverse event | Face-to-face meeting | |
| Ongoing involvement of patient with review | The key contact should offer to help a woman and families describe and document their thoughts, concerns and questions about the adverse event - these should be submitted in time for the review | Key contact, or any other healthcare professional the family shares questions with | Up until the panel review | Patient meeting, email, phone | |
| Ongoing involvement of patient with review | The team responsible for the review should keep in touch with the family letting them about the progress of the review, when it has been completed and is ready to be shared with them | Risk team | Until review process is completed | Letter/ phone call | |
| Sharing review findings | The clinical management team should offer to send the report, considering timescales relevant to individual circumstance | Clinical management team, clinical leads | When report is closed | Patient meeting |
5. Supporting staff training and wellbeing
Staff leading adverse event reviews should have training and be competent in investigative methodologies, techniques and analysis, including human factors and report writing, and protected time to take part. Individuals who feed back to families should be trained in effective communication in the management of adverse events.
In addition to bespoke staff training provided by NHS Boards, NHS Education for Scotland provide a suite of three workshops designed to provide NHS staff involved in investigation work, and those in leadership/management positions, with the skills required. These include training on learning from safety incidents in complex care environments, building a safety culture and other associated areas. Further details are available on the NES website.[17] NES can provide the package of these workshops in a combined bespoke half-day session.[18]
NES also has an e-learning resource[19] for enhanced significant event analysis and entry-level Human Factors.
Staff involved in any adverse event process may need addition wellbeing support. It is therefore important that management ensure that appropriate measures are in place to support the wellbeing of the individuals throughout the adverse event review process.
6. Child Death Review Process
The Scottish Government are also developing a Child Death Review system, which ensure that a high quality consistent review is carried out into all child deaths (all live born children up to the age of 18 or 26 for care leavers or those in receipt of aftercare or continuing care at the time of their death). The Child Death Review system will include all neonatal deaths including those that require either a Significant Adverse Event Review or a Comprehensive Care Review. The Child Death Review process will complement the process described in this framework and there will be no requirement to undertake any additional investigation or review. The review process will include the information required to complete the Child Death Review core data set which will be collected for all deaths. Further information can be found online: National Hub for Reviewing and Learning from the Deaths of Children and Young People
C) Stage 6: Improvement planning
Capturing and sharing learning from adverse events and CCRs
The HIS National SAER Framework aims to ensure any staff involved are supported in a consistent manner, events are reviewed in a consistent way, and learning is captured and shared locally and nationally to improve the quality of services. Events subject to Perinatal Mortality Review should also follow national PMRT guidance.
Current position
Currently, following an SAER in any service, colleagues can access a generic Learning Summary Template and Guidance at an Online Community of Practice on Knowledge Network. Following a review process, Boards are responsible for uploading their own Learning Summaries directly to the site, in order that other services or Boards may review findings and potentially share in any learning. Whether or when to share learning in this manner is at the discretion of each Board and relies on positive engagement.
There is no forum available for post-SAER learning activities relating specifically to maternity, neonatal or perinatal communities.
Improvement Planning
The templates and Online Community of Practice are currently under review and will cease in March 2022. They will be replaced with an improved approach developed through a Joint Commission for Openness and Learning between HIS & NHS Education Scotland (NES).
There is ongoing discussion with the clinical community exploring the best ways to share learning at a local level and with HIS and the Scottish Perinatal Network (SPN) about sharing at a national level.
Supporting this Perinatal Adverse Event Review Guidance
The SPN will support the perinatal community to implement this guidance, in collaboration with strategic partners such as NES and HIS – including its Adverse Events Network and (the) Maternity and Children Quality Improvement Collaborative (MCQIC), which is part of the Scottish Patient Safety Programme (SPSP). The SPN will:
- Develop a ‘safe space’ learning forum on MS Teams and a corresponding ‘collaboration space’
- Facilitate regular case review events at which Boards can present, discuss and share learning (quarterly or six-monthly)
- Facilitate tailored learning opportunities, as requested, following particular incidents or events.
- Develop a process to ‘buddy-up’ smaller with larger Boards for peer support and to add structure to request for external reviewers.
- Establish a perinatal SAERs working group through which to support implementation of the framework, provide support, and share learning and best practice.
Reporting deaths to the Procurator Fiscal
Boards must continue to comply with statutory reporting of perinatal deaths. Any category 1 stillbirth or neonatal death should be reported to the Procurator Fiscal’s Scottish Fatalities Investigation Unit (SFIU) as soon as possible following a decision to carry out an SAER. It is accepted that events which go immediately to SAER will be reported sooner than events which undergo CCR first and are subsequently escalated to a level 1 review.
Where the Procurator Fiscal decides to investigate a death, if parents have not authorised a hospital post mortem, it is likely that SFIU will instruct one. Further details are available through the Crown Office and Procurator Fiscal Service (Reporting Deaths to the Procurator Fiscal, Information and Guidance for Medical Practitioners): Reporting Deaths to the Procurator Fiscal[20]
Contact
Email: thebeststart@gov.scot