Making it easier: a health literacy action plan 2017-2025
Making it Easier sets out an action plan for improving health literacy in Scotland.
Action area 2
Embed ways to improve health literacy in policy and practice
Headlines from this section
- We will embed health literacy improvements into policy and programme developments across sectors throughout the lifetime of the action plan.
- We will have a specific focus on building the common skills of connectors across all sectors.
- Library and information services have a key role to play.
We have made many useful links across the health and care system during the development of Making it Easy. Many of these links benefitted from being quick, simple and agile, but there’s an opportunity to better target our efforts in the next phase. This section sets out a range of policy and practice areas we’ll work with to embed our learning.
Primary care
Primary care is where many people first seek advice when they have a health issue. It’s a good place to get things right from the start. There is much work underway to ensure people are better informed, with access to the right person at the right time so they receive the best care in the most appropriate setting.
All members of the team have a role to play. Through primary care’s developing skills and roles of non-clinical staff improvement programme, we will include health literacy skills within training. In addition, we will work with the Royal College of General Practitioners ( RCGP) Scotland’s Patient Partnership in Practice (P3) network to promote and develop greater health literacy responsiveness in general practice.
Dentists have long made efforts to create positive environments in their surgeries, particularly to reduce anxiety for young children and parents. There is much to learn from this work.
Childsmile programme
The Childsmile toothbrushing programme aims to provide very young children with knowledge and skills which should stand them in good stead for looking after their teeth for life, saving them from unnecessary pain and suffering. It relies on bespoke resources which have been developed with, and for children and their carers and involves the children in the practical process of brushing their teeth in nursery school every day.
The combination of involving the children and their carers in the project and ensuring resources are accessible and appropriate has significantly improved child oral health over the last 10 years.
A recent Our Voice citizens’ panel report showed where we should target our efforts to support people in understanding more about pharmacy services. It also showed how we can help pharmacists meet people’s information needs. We will work with a variety of patient interest groups to progress this work.
We will work through the Modern Outpatient Programme [27] to give people at all levels of health literacy confidence to access the system whenever necessary, and ensure they have the skills and support to self manage their conditions when clinically appropriate. This will help to reduce health inequalities and minimise unnecessary demands on current services.
Urgent care services
In line with recommendation 25 of the National Review of Primary Care Out-of-Hours Services [28] , there is an opportunity to develop out-of-hours and urgent care services that respond better to people’s health literacy needs. Many of the challenges are the same in all care settings, but we will explore the best way to make changes in this particular area that meet the needs of people and their practitioners.
The role of NHS inform as ‘go-to’ source of online information
NHS inform is Scotland’s national health information service.
Its aim is to provide people with accurate information to help them make informed decisions about their own health and the health of the people they care for.
Inform has engaged with people on the development of information and resources to support self-care. A good example is the Musculoskeletal ( MSK) Help app – www.nhsinform.scot/care-support-and-rights/tools-and-apps
It has also produced self-help guides. These allow people to access information about common conditions and provide suggested outcomes based on the answers given, for example ‘contact a pharmacist’. The self-help guides can be accessed at www.nhsinform.scot/self-help-guides
Work is underway under action 14 of the Mental Health Strategy for Scotland 2017-2027 [29] to improve NHS inform’s online material for people with urgent mental health care needs.
Mental Health
The new Mental Health Strategy for Scotland 2017–2027 [30] (action 11) reaffirms the Scottish Government’s commitment to improve the response for people presenting in distress in Scotland, through the implementation of the Distress Brief Intervention [31] ( DBI) programme. This aims to build a framework for connected, compassionate support.
A DBI is a time limited and supportive problem-solving contact with someone in distress. It is a two-level approach:
- DBI level 1 is provided by front line staff and involves a compassionate response, signposting and offer of referral to a DBI level 2 service.
- DBI level 2 is provided by trained third sector staff who will contact the person within 24 hours of referral and provide compassionate community-based problem-solving support. This will include wellness and distress management planning, supported connections and signposting for a period of up to 14 days.
We will embed health literacy learning into practice through the DBI programme [32] by supporting the associated training programmes, building knowledge and skills, supporting the use and testing of the available tools, and influencing the evaluation framework.
Supported decision-making at times of impaired capacity
Supported decision-making is the term used to describe the process of assisting a person with cognitive disability to make decisions for themselves. Anyone may need support in decision-making but people with a learning disability, dementia, or mental ill health, face particular challenges while having the same rights as anyone else. Support is needed to ensure that they can make decisions about their lives, while recognising barriers in society such as stigma, paternalistic attitudes, and discriminatory systems.
There are many examples of good current practice across the health and social care sector in Scotland. We should build upon this to create the right environment for the types of good conversations that are the basis of supported decision-making. This will ensure that everyone in Scotland who needs support to make important decisions can access it, or be given the opportunity to have their wishes heard.
Information about medicines
Some of the most common interactions that people have with health and care services relate to medicines information. One of the key statistics from Making it Easy was the high proportion of people (43%) who lack the skills to calculate a dose of childhood paracetamol.
Not sure? Just ask!
To help people understand their medicines the Scottish Patient Safety Programme promotes Not Sure? Just Ask! cards. The cards were originally developed by NHS Tayside with input from patients, carers and members of the healthcare team.

There is an excellent opportunity to improve support for people who are taking complex medications by using clearer medicines information. At a Europe-wide level we can link to the SIMPATHY [33] programme to improve people’s knowledge and skills in managing their medicines.
At points where people are having their medicines reviewed, there’s a good opportunity to check understanding and be clear in communication. This video [34] offers an example of what good practice can look like.
Workshop with the Scottish Commission for Learning Disability’s ( SCLD) expert group
A key theme about the need for clearer information about medicines emerged during a workshop with SCLD’s expert group.
People like information in picture format, with easy words and clear explanations of “what it’s for”. What are the differences between capsules, tablets and caplets? What does that mean for how we take the medicine? Clearer packaging with no smallprint is vital. Reminders of when to take medicines would be helpful.
Pharmacists can help by giving more clear information about taking our medicines. Including a person with lived experience of learning disability in pharmacists’ training may be a good idea. This might also be helpful for GP receptionists’ training as there are some barriers to phoning for appointments.
Promoting Inclusive Communication
The Royal College of Speech and Language Therapists [35] promote improved inclusive communication. This approach recognises that people communicate in many different ways and that the environment must support this. There is a large body of work to draw upon and align with. Scotland’s Inclusive Communication Hub [36] is a key resource.
Significant work is underway to better support people with Augmentative and Alternative Communication [37] ( AAC) needs. Links need to be made between this work and improvements to health literacy to ensure that systems are more responsive to the needs of people with very complex communication needs. The same principle applies to the new framework for improvement on British Sign Language ( BSL).
Care and Support Planning conversations
New models of care, such as care and support planning [38] , place a strong focus on preparing people and their practitioners to make best use of precious face-to-face time. The theme of ‘good conversations’ [39] links policy and practice including Adults with Incapacity, Palliative and End of Life Care, Self-directed Support, Adult Carer Support Plans and Young Carer Statements, ‘thinking ahead’ in Anticipatory Care Planning, when discussing emergency care and treatment plans using processes like ReSPECT [40] , or any conversation about What Matters to You.
It is vital that these care and support planning conversations consider the range of health literacy needs that people are likely to have, including:
- creating more relaxed settings for conversations,
- how best to present test results in helpful formats,
- tools and techniques that can best support people to more actively participate, and
- supporting the skills and confidence of health and care staff at all levels to start these conversations, listen closely, and respond to people.
We need to avoid having prepared people but unprepared practitioners, though, by addressing and improving clinical consultation skills. In particular, we need to improve how we approach shared decision-making, setting priorities and action-planning. Examples of how we might do this include model examples of what good conversations, which promote people’s rights [41] , might look like, and building training on return consultations into training. We need to highlight the importance of practitioners having the time and space to allow the essential health literacy aspects of consultations to take place.
There is a need to promote the importance of good palliative and end of life care across all settings. The Strategic Framework for Action on Palliative and End of Life Care [42] sets out a vision that everyone in Scotland who needs palliative care will have access to it. We need to support people to have conversations that meet their needs and preferences. It should better explore people’s understanding about their condition, their preferences, as well as what is unacceptable to them, to achieve a clear picture of the extent they wish medical treatment. The focus is on listening firstly, and making sure that any information is in a form the person can engage with. These sorts of conversations should happen early, where people still have sufficient capacity, and must always involve those closest to the person where that capacity is limited.
In a number of locations in Scotland, public health approaches are being used to improve people’s experiences of death, dying and loss. These involve:
- creating supportive environments to promote open discussion,
- building individual skills and capacities such as how to listen to someone who is bereaved, and
- strengthening community action including developing informal networks of support [43] .
The integrated health and care workforce
Integration authorities across Scotland [44] are planning, innovating and working with health and social care staff, communities and the third and independent sectors to ensure person-centred approaches in the design of care and support locally.
The integrated workforce is supported by bodies such as NHS Education for Scotland ( NES) and the Scottish Social Services Council ( SSSC). They work together to support the education and training of health and social care workers. Their programmes of work are a good opportunity to develop and share what we have learned to date.
Three potential areas for mutual action across the Scottish Government, NES and SSSC have been identified:
- Systems work – to better understand how the healthcare system works and can be more easily navigated.
- Forum theatre – this is a way of co-produced working to bridge the interaction between people and their practitioners.
- Outcomes focused support planning – a co-design group is developing a resource to support outcomes focused support planning [45] at individual, organisational and local level in the context of implementing the Carers (Scotland) Act 2016.
There is also a chance to build on the examples, tools and conversation aids [46] that have been developed to help anyone who wishes to discuss funding support for their social care.
Creating common skills across the system
Strathclyde University, funded by the Economic and Social Research Council, has undertaken research [47] on the role that human information intermediaries, for example family nurses, support group leaders, and social workers, can have in improving information skills and understanding for the most disadvantaged people. They identify an important human intermediary role that can:
1. help to recognise where information needs exist and take measured, purposeful action that takes account of the context,
2. be a key source of information in themselves, and a key connection to other sources of information not otherwise accessed, and
3. tailor and personalise information for relevance, and communicate in ways that take into account individual digital and health literacy and learning levels.
Working through our networks of champions, these common skills of connectors competencies can be widely promoted across sectors, situations and contexts to build a more skilled workforce and health literate society. In particular, we will work with the Care Inspectorate to support social care services and staff to understand the role they can play in supporting health literacy.
Community Link Workers
Community link working [48] is a way to connect people to sources of support or resources in the community that are likely to help with their health problems and improve wellbeing. A link worker also maps local sources of support, and develops relationships with the third sector, keeping updated on the status of existing and new services. The link worker offers a key gateway to promote health literacy with people, their health and care workers, and the third sector. It is vital that health literacy is included in the range of skills and knowledge that link workers have.
Social welfare literacy
There’s an opportunity to spread learning from our health literacy work through the emerging welfare reform programme. In particular the agency established to deliver Scotland’s new social security system could incorporate many health literacy tools and techniques. This will ensure people are treated with fairness, dignity and respect by taking into account their communication needs and preferences. This will support people to navigate the new system from the outset and use the information they receive to make informed decisions, regardless of their situation or circumstances.
Common skills of connectors in the InS:PIRE programme
InS:PIRE (Intensive Care Syndrome: Promoting Independence and/or Return to Employment) is a Health Foundation funded project which aims to improve the health and wellbeing of Intensive Care Unit ( ICU) patients after discharge from hospital, measured through return to work levels, GP visits and quality of life.
It was a case study in Realising Realistic Medicine.
A key part of the project is linking people to sources of support in their communities, so we will work with InS:PIRE to embed the ‘common skills of connectors’ into their roles and responsibilities. This will provide a good chance to refine and develop how we describe the skills needed.

The role of librarians
The National Strategy for Public Libraries 2015-2020 [49] has a strand that relates to the promotion of social wellbeing:
‘Libraries can be key partners in tackling the problems of social isolation, inequality, disadvantage, fractured communities and ill health. Libraries provide an important space and resource for many disadvantaged people in a non-judgmental, public space, open to all.’
There is an appetite for librarians to play a more active role in linking people to useful sources of health and care information. There is work already underway. We will work with them to develop resources that better meet people’s needs by building upon the common skills identified by the Strathclyde University research. This will include drawing upon sources of support for improved digital literacy skills such as the SCVO’s digital participation programme [50] .
The role of public librarians
Reference: CILIP and University of Salford
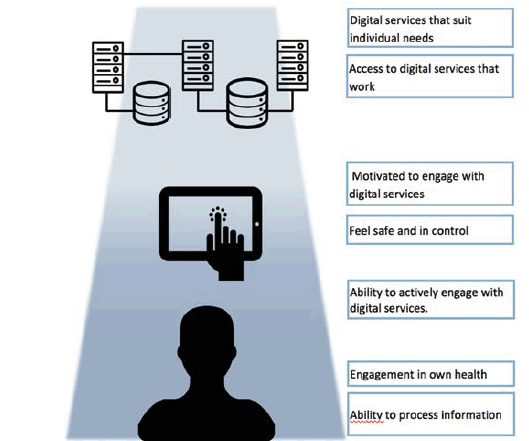
Digital transformation
Health literacy is an important consideration for organisations as they develop digital solutions to support more aspects of service delivery. As well as building capacity in the use of digital tools for self-management, there is a need to further explore how digital tools can effectively support the shared decision-making interaction between people and their practitioners. These digital health literacy challenges will be an area of focus for the new Digital Health and Care Strategy.
Macmillan information support services in Scotland’s public libraries
The Macmillan @ Glasgow Libraries service offers cancer information and emotional support in libraries across the city.
This ambitious and innovative service design allows people affected by cancer to improve their quality of life by ensuring they receive easy access to understandable information and support at the right time, regardless of where they are on their cancer journey or where they live. This includes those who have had a cancer diagnosis and also their carers, family, friends and those who are worried about cancer and would like to find out more.
People can drop in without referral or appointment. Within the centres they will find information zones stocked with free easy to read booklets, leaflets, audio-visual and electronic resources. Trained volunteers offer emotional support and tailored information on living with and beyond cancer, helping people understand complex information and think of questions they might wish to ask their doctors or nurses.
Access to practical support is also on offer, including benefits advice and counselling, which can all take place in libraries across the city. Volunteers also signpost to a wide range of local services from physical activity and leisure classes to carers support and befriending services.
The Right Decision – what NHS librarians do
The Right Decision campaign encourages people to make full use of the expert evidence services provided by NHS librarians.
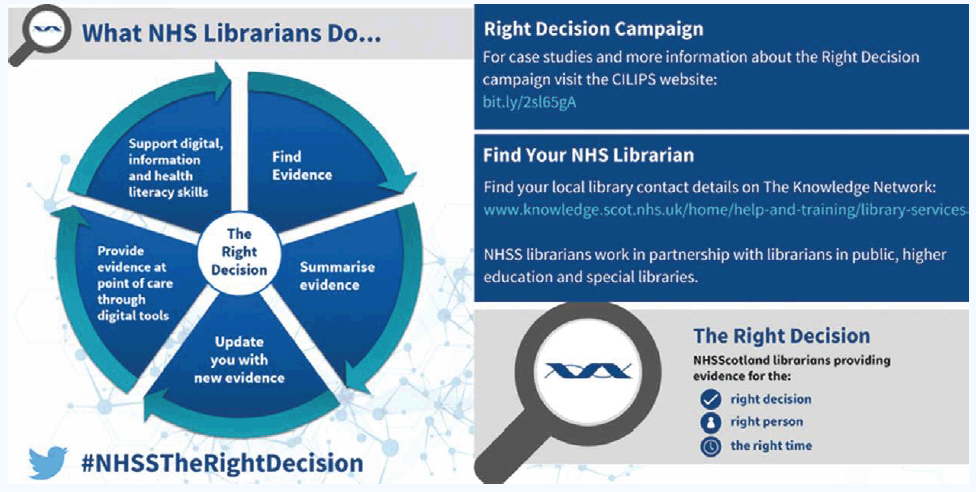
In addition, Going in the Right Direction – Health Information for Health and Wellbeing is a resource jointly produced by the NHS and the ALLIANCE to support library and information services across sectors.
Collaborative action with NHS England
We’ve made links with work across the UK through the UK Literacy Group [51] . Building on that, we will work with the NHS England National Health Literacy Collaborative to explore areas of common interest to derive clear actions for mutual benefit. An initial focus will be on medications information, but there will be opportunities to look at other topics throughout the lifetime of the action plan.
Harvey’s Gang – an example from NHS England
This story starts with Harvey Baldwin, a 7-year-old boy with leukaemia who was being treated at Worthing Hospital. Could Harvey visit the labs that processed his many blood samples? Chief biomedical scientist Malcolm Robinson agreed. Harvey sat there, transfixed, watching his own blood going through the machine. The lab coat he wore swamped him so overnight, the chief of service ran up a mini lab coat from discarded NHS sheets.
Then Malcolm got the idea of bringing these young patients who endure frequent blood tests into the labs on a more regular basis. Sadly Harvey – who would have made a great biomedical scientist – died, but Harvey’s Gang is his legacy.
Youngsters come into the labs, they get a special lab coat (not run up by the chief of service) and other goodies. Having been there, youngsters are less frightened about giving samples, and having explained how the lab works, parents are more reassured.
For the healthcare scientists involved, the experience of Harvey’s Gang has been transformative. ‘It reconnects us with our patients,’ says Malcolm, ‘and it’s also meant that we’ve made changes to our services which ensure better care for our patients’. Harvey’s Gang is now being rolled out not just in other UK units but across the world with places as diverse as the United Arab Emirates and Tennessee wanting to emulate it.