The keys to life - Improving Quality of Life for People with Learning Disabilities
The new learning disability strategy in Scotland, following on from, and building on the principles and successes of The same as you?, the original review of service for people with a learning disability, published in 2000.
Health
Setting the scene
The Scottish Government has set a key objective to make Scotland healthier. It will achieve this by tackling ill health and by focusing on health inequalities. To measure progress it has established two national outcomes of living longer, healthier lives and tackling the significant inequalities in Scottish society. To be able to make progress in respect of people with learning disabilities will require a much greater understanding of their specific needs in order to address them.
Wider socio-economic determinants of poor health outcomes for people with intellectual disabilities13
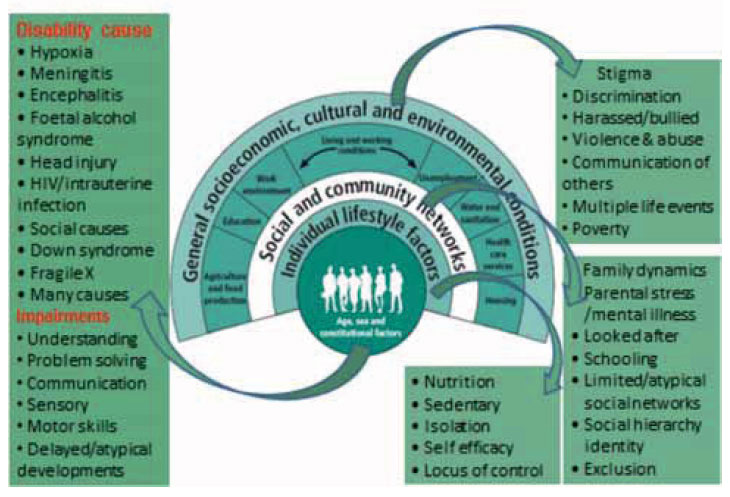
Research tells us that people with learning disabilities have some of the poorest health of any group in Scotland14. They are considerably more likely to die at an early age than the general population - on average 20 years before15. Some of the causes of death are potentially preventable, and the main causes of death differ from those of the general population. Whilst the most common causes of death for the Scottish population are cancer, heart disease and strokes, the most common causes of death for people with learning disabilities are respiratory disease, cardiovascular disease (related to congenital heart disease) and different forms of cancer, principally related to gullet, stomach and gall bladder rather than lung, prostate and urinary tract.
Many of the causes of learning disabilities may also lead to physical or mental ill health. This means that people with learning disabilities may be more likely to be prescribed multiple drugs due to complex and multiple health needs which, in turn, can sometimes adversely affect health through side effects and drug interactions.
In terms of prevention, people with learning disabilities are also less likely to exercise and eat healthily than the general public because they may not always have the knowledge or understanding to make healthy choices, and are reliant on others for support and communication. These issues are often added to by problems accessing the health services they need.
What is clear is that some conditions go unrecognised or are recognised at a later stage than would be the case for the general population.
Where there is a recognised condition, it may not be monitored as well unless individuals themselves, their carers and professionals pro-actively do this. Added to which, assumptions are sometimes made that a condition is part of the learning disability and it is not addressed because of this.
The way in which service responses are structured does not always help. One example of this is that there is no equivalent of the paediatric service for adults with learning disabilities in the NHS. Instead, responsibility within the community lies principally within primary care. There is no doubt that there is good practice in primary care, but routine exposure to the needs of people with learning disabilities because of the low numbers per average practice makes it harder to build up expertise. Overall these issues contribute to reduced life expectancy, reduced cognitive functioning, reduced quality of life, and disability and pain.
With the passage of the Health and Social Care Integration Bill there will be improved opportunities for health and social care practitioners to work more closely together in maximising their expertise to achieve best value in terms of quality outcomes for people. We know that since The same as you? there have been considerable investments to improve the social care and support of people with learning disabilities, and Scotland now has inclusive policies, and more appropriate housing and support provisions for people with learning disabilities. Integration should make it possible to learn from these interventions and to spread that learning across all disciplines and locations.
Scottish Learning Disability Observatory
In order to understand more about the health inequalities faced by people with learning disabilities and to make those needs more overtly visible, the Scottish Government is funding the University of Glasgow to create a Scottish Learning Disability Observatory which will be dedicated to robustly underpin health improvement and to address health inequalities.
As the health of people with learning disabilities cannot be measured in Scotland's routinely collected health statistics, it is not possible to measure the health care they receive. Considerable information is available in Scotland about a wide range of disease areas (such as heart disease and diabetes) that has resulted in these services being able to improve pathways to better manage these diseases. It has also provided policy-makers with the information they need to take better decisions and improve health policies, but the same is not the case for people with learning disabilities due to the lack of information available. So there has been a lack of awareness of the extent of need.
The Observatory will work with and for people with learning disabilities and their families, ensuring their views and priorities inform the programme of work packages. It will measure and watch health indicators and health service responses, and support the role of adult social care and education in health. Scotland has a strong tradition of using routinely collected data to measure, monitor and improve the health of the population, and can use this information to benchmark performance between services in Scotland, and to draw comparisons across countries.
The Scottish Learning Disability Observatory will be able to provide policy makers with the evidence and data required not only to take action on the basis of improved understanding but also to clearly demonstrate improvements from these actions.
Recommendation 9
That the Learning Disability Strategy Implementation Group will work with the Scottish Government to explore the development of a HEAT target for the NHS to establish a process whereby all adults with learning disabilities using health services are identified to Information Services Division and Scottish Learning Disabilities Observatory, so they can be visible in Scottish data systems by 2015.
Recommendation 10
That by 2015, the Primary Care Division of the Scottish Government and Scottish Learning Disability Observatory will work together to develop a process of annual reporting of trends in the management of the long term conditions of people with learning disabilities.
Recommendation 11
That the Scottish Learning Disability Observatory will work to develop a better understanding of the causes of unnecessary deaths of people with learning disabilities.
Recommendation 12
That by 2016 the Scottish Consortium for Learning Disability, local authorities and the Scottish Learning Disabilities Observatory will work in partnership to provide information to Information Services Division and Analytical Services Division of Scottish Government, to identify by unique NHS numbers the adults with learning disabilities using social work resources.
Health Inequalities
Poor health can result from social isolation and deprivation. Many people with learning disabilities have experienced lifelong exclusion resulting from lack of choice and opportunity as well as experiencing significant barriers to access. People with learning disabilities are more likely to be exposed to common causes of poor health such as poverty, poor housing, and lack of employment, social isolation and discrimination.
Many people with learning disabilities experience limited verbal communication skills which impacts on others' ability to understand health needs. Both paid and family carers play an important role in identifying health needs. Many people with more severe learning disabilities rely completely on others to communicate what their health needs are.
Communication difficulties are fundamental to explaining many of the barriers and poorer outcomes people with learning disabilities experience when using health services. Many healthcare workers have never had training in the kind of communication methods and techniques that facilitate appropriate access to services. In addition many healthcare professionals rely on individuals reporting symptoms and ill-health.
The National Needs Assessment outlined a range of barriers faced by people with learning disabilities in accessing services, including physical barriers, failure to make reasonable adjustments and negative attitudes and values from practitioners.
During 2008, as part of the on-going commitment to the quality improvement process the Scottish Government asked NHS Quality Improvement Scotland (Now Health Improvement Scotland) to undertake a national review of all general health services against Quality Indicators 2 and 3, Promoting inclusion and well-being and Meeting general healthcare needs. This work was completed in 2009 with the publication of a national overview report16. Despite varied practice across Scotland, progress was noted, with local examples of good practice and service developments that have improved access to general healthcare.
Many factors influence an individual's health and health choices. People with learning disabilities experience challenges maintaining good health because of a combination of factors, such as:
- Individual factors, for which services require to make reasonable adjustments, for example, communication needs; many co- occurring health needs; distinct health needs and low expectations of services.
- Health and social care service factors, such as: negative assumptions; inexperience and lack of knowledge; lack of experience and acknowledgement of the contribution of family and paid carers.
- Service structures, such as: inflexible and short appointments; over reliance on literacy skills; poor communication and information exchange.
Scottish Government Health Inequalities Funding
To tackle the on-going challenge of reducing the health inequality gap faced by people with learning disabilities, the Scottish Government has offered additional financial support to help NHS Boards build on the work that has been on-going since 2008 when Equally Well17, the report of the Ministerial Task Force on Health Inequalities, was launched.
This funding programme, from 2012-2015, will enable NHS boards and their partners to address the health inequalities recommendations arising from the evaluation of The same as you? and this new national strategy, as well as continuing to address the health inequality gap within the Equally Well report. The resources will be provided to create capacity in each area to scope and define service change, including improvements to information and partnership working between health boards which will ensure a better use of resources.
The Learning Disability Health Inequalities Network comprises of representatives from all NHS Boards and is facilitated by the Scottish Government. The Network meets on a quarterly basis to further enhance the sharing of ideas and services to avoid duplication of effort and ensure the best use of resources.
Recommendation 13
That Learning Disability Strategy Implementation Group will work with NHS National Services Scotland (National Information Systems Group) to ensure that both the Emergency Care Summary (ECS) and the Key Information Summary (KIS) meet the information needs of people with learning disabilities accessing health care.
Recommendation 14
That the Learning Disability Strategy Implementation Group will work with Healthcare Improvement Scotland to undertake a review of the Learning Disability Quality Indicators and Best Practice statement to ensure that they reflect the changing needs of people with learning disabilities. A review of general health services and specialist learning disability health services will be undertaken across NHS Scotland to ensure that there is full compliance with Learning Disability Quality Indicators and Best Practice statement on Promoting access to healthcare for people with learning disabilities.
Healthy Lifestyles - Prevention and Self Help
There is an increasing focus on health improvement activity for the general public around nutrition, physical activity, smoking, alcohol and drugs, cancer screening programmes and immunisation programmes18 which benefit the health of the citizens of Scotland, including people with learning disabilities. This section identifies a number of ways in which people can either avoid compromises to their health or slow up any potential deterioration. But we also know that many people with learning disabilities have fewer opportunities to make choices and decisions that impact on their health and wellbeing. Access to health improvement activity involves a range of service providers, with family and paid carers having an important role to play. Effective health improvement education must consider the wider context of individuals' lives.
Diet
Many people with learning disabilities are aware of healthy eating messages. However, it has been reported that less than 10% of adults with learning disabilities in supported accommodation eat a balanced diet19. Carers can sometimes be unaware of the public health recommendations on healthy diets20. It has also been reported that many people with learning disabilities face challenges with weight. Many more people with learning disabilities are likely to be either underweight or overweight than the general population21. In particular women with learning disabilities and individuals with Down's syndrome are at more risk of obesity.
Obesity
Obesity is a major public health concern, and the prevention and management of obesity is a priority for health care in Scotland. This is because obesity is associated with a reduced life expectancy, and strongly linked to chronic health problems, such as diabetes and cardiovascular disease.
The Scottish Government has funded Edinburgh Napier University to provide information on people with learning disabilities who have diabetes. The project will set out proposals relating to the prevention and management of diabetes in people with learning disabilities in Scotland.
Children, young people and adults with learning disabilities experience very high rates of obesity. The increased rates of obesity in children with learning disabilities, compared to children who do not have learning disabilities, are already present by the age of three years old. Adults with learning disabilities aged 16-24 experience higher rates of obesity than adults over 50 who do not have learning disabilities.
This increased prevalence and early onset of weight problems highlight the importance of reducing obesity to the health of individuals with learning disabilities clinical guidelines are clear about the types of weight management interventions and services that should be offered to people with obesity. However, there is a lack of evidence about what works for children, young people and adults with learning disabilities and obesity.
This means that in many areas people with learning disabilities and obesity find it difficult to access weight management services. To address this inequality, the Scottish Government has funded several pilot studies to develop evidence about the best ways to help individuals with learning disabilities manage their weight problems, and make healthier lifestyle choices.
Weight management for adults with learning disabilities and obesity
TAKE 5 is a multi-component weight management programme based on best practice recommendations in the SIGN clinical guidelines. Development of the TAKE 5 programme came about through partnership working between the University of Glasgow, the Glasgow and Clyde Weight Management Service, and NHS Greater Glasgow and Clyde learning disabilities services. This work has been funded by the Scottish Government. The evidence is that the TAKE 5 programme is an acceptable and effective way for adults with learning disabilities and obesity to lose weight and improve their health and wellbeing.
Case study
When Frances took part in the TAKE 5 pilot project she was 54 years old. Her weight problems were causing pain in her knees and she had to take medication to control her diabetes. The TAKE 5 worker helped Frances, and the paid carers supporting her, to find ways to change her diet and gradually increase how much exercise she was taking. To lose weight, Frances set her own goals and regularly monitored her weight. She followed a personalised diet that aimed for an energy deficit of 600 kilocalories a day. Frances also used a pedometer to help her slowly increase how much walking she was doing. The TAKE 5 worker provided training to the paid carers to help them support Frances lose weight. By the end of the three month weight loss phase, Frances had lost over 5% of her initial body weight. Her knees were no longer painful when she walked and Frances's GP decided she no longer needed medication to control her diabetes. The TAKE 5 worker continued to see Frances once a month to provide support and advice about long term weight loss maintenance. One year after taking part in the TAKE 5 pilot project, Frances has kept the weight off, feels good and is confident about managing her weight.
Exercise
Physical inactivity is one of Scotland's major health challenges, contributing to nearly 2,500 deaths in Scotland each year.22
There are well recognised barriers to exercise ranging from physical barriers and attitudinal barriers to support barriers. There is a strong message that people with learning disabilities view opportunities to exercise in the context of wider social factors such as the opportunity to develop friendships. Enabling people to make positive choices about their lives may prove a successful strategy in improving physical activity levels, as seen in the development of the 'You Can Do It!' DVD produced by SCLD23.
Doing more physical activity and reducing the amount of time we spend sitting down can have a big effect on health and wellbeing. The Scottish Government has set physical activity targets for children and adults in Scotland, and there are lots of initiatives to help people to get more active.
Many children and adults with learning disabilities do not have much opportunity to participate in physical activity. Instead, people with learning disabilities often have sedentary lifestyles. For example, children with learning disabilities spend 85% of each day sitting or lying down and a study in Glasgow found that, on average, adults with learning disabilities walk for around 15 minutes a week. These levels of inactivity cause health problems, such as heart problems or diabetes. Therefore, it is important that children and adults with learning disabilities are supported to become more active.
There are many projects in Scotland aimed at getting children and adults with learning disabilities to become more active. Everyone likes doing different types of activity so it is important that a range of opportunities is on offer. There are school-based projects to help children with learning disabilities become more active, leisure centres are finding ways to make their services more inclusive and community groups are supporting people to do more walking. Walking is a great way to become more active. Even walking for an extra 10-20 minutes a day has positive effects on health and wellbeing.
Dancing is also a fun way to be active and, with Scottish Government funding, a group of adults with learning disabilities made a dance DVD with Glasgow City Community Health Partnership24.
Case study
In March 2012, the Scottish Government funded NHS Ayrshire and Arran to work in partnership with Trust Rugby International to develop an integrated rugby 7's team.
Having attended a taster session in June 2012, player C showed the appearance and physicality of an athlete, he attended the gym and other activities and had a strong desire to compete. Emotionally he was very excitable; he would let his emotions build uncontrollably to the extent of screaming when a simple request of 'give me the ball' would have been sufficient.
In the initial stages, a direct coaching approach had to be adopted to educate him that his behaviour was inappropriate at times. The challenge for the coaches came with meeting his needs and balancing that with the diverse needs of the rest of the group.
Six months later, player C is now one of the cornerstones of the group; his fitness level is rising each week by being challenged in rugby conditioning activities. The biggest shift is with him taking personal responsibility for his emotional outbursts. He is also taking some personal responsibility asking for support to address his own nutritional needs - in his own words 'I want to change the food I want to eat'.
His skill level has improved continuously over the 6 months, including his hand eye co-ordination, his speed and agility and game awareness. He has learned that it is a team game and he is now a team player in every sense.
Smoking and Drinking
People with learning disabilities are less likely to smoke or drink than the general population. However some do smoke and drink at levels which can be harmful to health25. This highlights the need for accessible health improvement initiatives across health services that enable people with learning disabilities to make healthy lifestyle choices in their own home.
Good practice
During 2012 the Scottish Government funded the Inverclyde Learning Disability and Alcohol Project. The project aims to develop an evidence-based pathway in order to prevent harm from alcohol use in people with learning disabilities in Inverclyde. The project will work with people with learning disabilities to understand the issues associated with alcohol use. The project will develop an appropriate screening tool to detect hazardous and harmful use of alcohol in people with learning disabilities, develop health improvement packages to raise alcohol awareness and develop a pathway for those with harmful and dependent drinking.
Good quality general health support in the community
There will come a point where people with learning disabilities, like all citizens, will need health support beyond self-care. The literature on the health needs of people with learning disabilities in Scotland was outlined in the National Needs Assessment in 2004. We know that the majority of people with learning disabilities live in the community and have the right to access general health services provided by a wide range of specialists, including GP's, practice nurses, district nurses, community pharmacists and many others.
Strengthening the commitment26, which is a report of the UK Modernising Learning Disabilities Nursing review, recommended learning disability nurses should be supporting access to allow people with learning disabilities to receive care and treatment from general healthcare practitioners.
However, despite community health services being the most appropriate services to meet the general health needs of people with learning disabilities, many health specialists, including GPs, receive little training, if any, on the needs of people with learning disabilities.
To tackle the complex issues of multi-disciplinary and multi-agency training and effective joint working the Scottish Government funded NHS Western Isles to establish a Learning Disabilities Collaborative. Its purpose was to improve services so as to recognise and meet the needs of people with learning disabilities more effectively. This was achieved, in part, through training and education. eHealth and care systems to support patient pathways were also improved. Most importantly, the work of the project has been designed to ensure that all the changes and developments achieved over the duration of the project are sustainable and integrated into standard practice.
Recommendation 15
That the learning from the NHS Western Isles Collaborative is formally evaluated and its findings disseminated throughout Scotland through a Best Practice Conference to be led by NHS Western Isles and the Scottish Government in 2013. Application of the model to other areas of Scotland will be considered by 2014.
Information and advice
To get the most benefit from what is available they will need good information. Which is why NHS 24 Helpline staff 27 have been trained to be aware of the need to communicate effectively with callers with learning disabilities. In addition, NHS Inform28 provide details of all pharmacies, GP practices and dental practices in Scotland. They can also provide information about illnesses and conditions, treatments, NHS services and other support services. Within this public information system there is now an Easy Info Zone29 that provides online information on health conditions, tests and treatments and wellbeing in easily accessible language to enable people with learning disabilities to be better informed.
Recommendation 16
That by 2014 the Easy Info Zone of NHS Inform is publicised to ensure that people with learning disabilities and their families and carers can benefit from its use.
Health checks
Health screening programmes for the whole population across Scotland have consistently been shown to be poorly accessed by people with learning disabilities, including: Cervical Smear Tests; Breast Screening; Dental check-up, epilepsy checks and Sensory Impairment assessments.
This low uptake of health screening services may be due to the many access barriers which people with learning disabilities experience. The much higher level of health need experienced by adults with learning disabilities compared with the general population, and the very high level of unrecognised and unmet health need, provides overwhelming evidence to support health screening programmes (health checks) specifically for people with learning disabilities.
Health checks have been widely endorsed as the way forward to reduce the current high level of unmet health need and health inequalities experienced by people with learning disabilities, in Scotland, and more widely in the UK and internationally. Studies of health checks have shown benefits in disease detection and health promotion. The NHS Greater Glasgow & Clyde health check programme was evaluated after its first year of implementation. A high level of health need was detected and met. Health economic evaluation demonstrated that it was a cost effective intervention to deliver, with lower overall costs of health care and supports for those who received a health check compared to those who did not.
Recommendation 17
That the Learning Disability Strategy Implementation Group will work with the Scottish Learning Disability Observatory to establish and implement a targeted health screening programme for people with learning disabilities across NHS Scotland.
Good practice
NHS Lanarkshire has developed a range of resources that can equip people with learning disabilities and /or their carers (paid or unpaid) and health professionals with skills and knowledge necessary to facilitate positive health outcomes by making accessible to them national screening programmes and where necessary appropriate follow up treatment or investigations.
NHS Lanarkshire's Learning Disability Service worked with members of Lanarkshire Ace, Speak Out Advocacy and many others to develop a range of resources: Total Communication Aide (distributed across GP Practices, Acute hospitals, care providers, school nurses, relatives and carers); and five DVD's (How to check your Boobs, How to check your Balls, Going for a cervical smear, Going for a prostate exam and Bowel screening). These are available in Public Libraries and GP Practices. Twenty one easy read leaflets/booklets were also developed. All these resources are available on website www.healthelanarkshire.co.uk
Dentistry
One in three people with learning disabilities has unhealthy teeth and gums. This increases to four out of five for adults with Down's syndrome30. This may be due to poor diet, poor dental hygiene, co-occurring health conditions and because oral health promotion may not always be accessible to people with learning disabilities. They may also fear dental treatment and, in some cases, will require general anesthetic in a hospital setting to resolve matters.
Dental health improvement strategies for people with learning disabilities, family carers and paid carers are of key importance to address dental health. This is why the National Oral Health Improvement Strategy31 for priority groups is critical. This makes clear that an oral care plan should be developed according to the assessed needs of the individual. This should incorporate oral hygiene, care and treatment needs. It will be important for people with learning disabilities that the use of general anesthetic is given particular and careful consideration.
For those who are carers, the effects of a lack of attention to oral health may not always be obvious without training. The National Oral Health Improvement Strategy for priority groups recommends that:
- the Salaried Dental Service and oral health promotion teams should play a lead role in the delivery of training to staff with responsibility for caring for dependent people and those with special needs.
- training for care home staff should be undertaken as part of an ongoing programme and should be based on an appropriate training tool such as "Caring for Smiles" which was developed for this purpose.
- all care home staff, including managers, should attend training on the delivery of day to day oral healthcare to residents.
- oral health champions should be identified to promote ongoing awareness of oral health issues within the care home setting. Such individuals should attend ongoing training to support their role.
Recommendation 18
That by June 2014 all professionals working with those with learning disabilities take responsibility for assisting with implementation of the National Oral Health Improvement Strategy by promoting it at local level with individuals, carers and relevant others.
Epilepsy
People with learning disabilities who have epilepsy should, where appropriate, access the same epilepsy services as the general population. However, it is widely recognised that there are features of epilepsy presentation and management in learning disabilities which negatively affect access to, and treatment by, these largely hospital based outpatient services. Current services for the management of epilepsy in people with learning disabilities involve multiple agencies including hospital neurology services, epilepsy nurse specialists, community learning disability teams, general practitioners and practice nurses. As well as leading to confusion about who should take the lead in managing an individual's epilepsy, there is also a lack of specialism and expertise amongst the professionals involved. SIGN 7032 states that subspecialty clinics should be available to meet the needs of specific groups such as people with learning disabilities and that a multidisciplinary approach to treatment is delivered by professionals with an expertise in epilepsy.
Recommendation 19
That by June 2015 all NHS Boards should ensure that people with learning disabilities that have complex epilepsy have access to specialist neurological services, including access to learning disabilities epilepsy specialist nurses and learning disabilities psychiatrists (where applicable).
Sensory Impairment
The term sensory impairment describes the varying degrees of hearing loss and sight loss as well as loss of both senses. Both hearing and sight loss can be present from birth, but for many people a sensory loss will occur later in life, and the longer a person lives the more likely they are to develop either or both losses.
Action on Hearing Loss estimate that there are 850,000 people with a hearing loss in Scotland and expect that this figure will double in the next 20 years. RNIB Scotland estimate that there are over 180,000 people in Scotland with significant sight loss. It is estimated by DeafBlind Scotland that there are 5,000 people in Scotland with dual sensory loss.
The Scottish Government is committed to addressing these needs for all people with a sensory impairment through the publication of See Hear which lays out a strategic framework that will be adopted at local level by health and social care agencies. A critical component is the development of local care pathways based on self-evaluation which will include recognition of the needs of people with learning disabilities.
The report recognises that people with learning disabilities are more likely to have a hearing loss and are 10 times more likely to have a sight loss. This can have a profound impact on how they are understood and are able to interact with others. Someone with communication difficulties, as someone with learning disabilities may have, might demonstrate challenging behaviours if they are unable to communicate a hidden and undiagnosed sensory loss.
Good practice
The Scottish Government provided funding to RNIB Scotland to produce the Bridge to Vision training DVD for optometrists and dispensing opticians who work with people who have learning disabilities.
The Audiology Services Advisory Group, which informs and monitors audiology services across Scotland, produced guidance that enables audiology service providers to respond appropriately to the audiological needs of people with learning disabilities33.
Recommendation 20
That health and social care professionals apply the local See Hear policy to people with learning disabilities and their families and carers.
Recommendation 21
That work is commissioned in 2013 to understand and analyse the factors that promote person-centred care and individualised health outcomes for people with learning disabilities to ensure that they receive the same investigations and treatments as the general population and that reasonable adjustments are made by 2015 to achieve the same health outcomes.
The role of the GP
The same as you? evaluation34 established that access to good primary care, especially having a doctor who understood their needs, was essential in improving the general health of people with learning disabilities.
NHS Health Scotland has also published tip cards35 which are a quick, easy-to-use resource to help NHS staff know what to do to support disabled people.
The GP contract in Scotland should reflect the differing health needs of people with learning disabilities as well as seeking to ensure inclusion in all areas of the Quality Outcomes Framework relevant to the general population. For example, Practices are required to maintain a register of adults with learning disabilities.
In addition, the Scottish Government introduced a Directed Enhanced Service (DES) for services to adults with learning disabilities for 2006/7 and, in the Scottish Enhanced Services Programme (SESP) from autumn 2007. This meant that GPs flagged case notes so that people with learning disabilities were provided with longer appointments and were therefore better able to communicate their needs. Some areas took great care to communicate when an appointment was to take place in a medium that people with learning disabilities understood and this had the added bonus of reducing the number of defaulted appointments. As a consequence of devolved local autonomy to NHS Boards to allow for flexibility of delivery of SESP funding, this valuable support has only been sustained in three Health Board areas. There would be merit in re-introducing and extending this approach.
The role of primary care liaison support
NHS Greater Glasgow & Clyde have a dedicated liaison team of nurses who work with General practice to support the delivery of primary health care to all adults with learning disabilities. The learning disabilities liaison team was established to increase the capacity of primary care to develop inclusive, equitable, and responsive health services for adults with learning disabilities.
The team works with General practice and specialist learning disabilities services to deliver a multi-faceted programme of work, including offering proactive health checks; training for primary health care professionals, accessible information, responding to service access issues, advice on support infrastructures to primary care, and facilitation to health improvement and anticipatory care initiatives.
All GP practices are now required to complete a template about the health needs of their adult patients with learning disabilities and to arrange a meeting with their patients to do so. There is a very high uptake of this service by general practices (well over 90%). This dedicated team, working in partnership with General practice and specialist learning disabilities teams, ensures that there is a continued focus on anticipatory care and targeted responses to meet the needs of people with learning disabilities.
As well as this, a robustly designed randomised controlled trial (RCT) of health checks for adults with learning disabilities has recently been completed in Scotland. People with learning disabilities who received a health check from their practice nurse were found to have received much better health care in the long term conditions that practice nurses are familiar with. However areas of ill-health that are more common for people with learning disabilities were found to be overlooked.
Some inflexibility within the practices was identified as a barrier to health check delivery. The health checks took less than an hour to complete. Initially, the nurses had been apprehensive about undertaking the health checks and some thought them unnecessary. However their opinions changed after the health checks, and they perceived them to be beneficial.
The adults with learning disabilities and their carers described enjoying having the health checks. The study is the first RCT of health checks conducted in primary care in the UK health care system. It provides the scientific evidence to support the view that health checks for adults with learning disabilities should be included within the GP contract, and also identifies areas where the health checks could be improved upon.
Recommendation 22
That by the end of 2015 all NHS Boards across Scotland should ensure there is a dedicated primary care liaison resource to support General practice and primary care teams to ensure their services are equitable and, where required, targeted for people with learning disabilities.
Recommendation 23
That the Learning Disability Strategy Implementation Group will work with the Primary Care Division of the Scottish Government to explore how the GP contract in Scotland can best meet the needs of people with learning disabilities, including the possibility of the reintroduction of an enhanced service for people with learning disabilities and including additional learning disability indicators in the Scottish Quality Outcomes Framework by June 2014.
Health in Hospital
Scotland has legislation in place to ensure that people with learning disabilities have equal access to the care and support they require. However too often practitioners are unaware of the need to comply and implement fully the legislation that is in place. The Disability Equality Duty requires that all services, including health services, make reasonable adjustments to ensure that the needs of individuals are identified and addressed, thereby avoiding disadvantage which in some cases may result in significant harm and avoidable premature death. Therefore all healthcare practitioners require to have a full understanding of legislation to ensure that they respond appropriately to the needs of people with learning disabilities, thereby removing discrimination.
People with learning disabilities require access to the full range of services provided by general hospitals. However several Fatal Accident inquiries (FAI) in Scotland have highlighted the significant barriers and risks many people with learning disabilities face when using general hospital services36. Several studies have reported the difficulties experienced by people with learning disabilities during admissions to hospitals37.
The main themes from these studies are problems with communication, lack of staff training and the negative attitudes of staff. In an attempt to address the risk to individuals and in response to the FAI findings, many health boards across Scotland have developed general hospital liaison services, staffed by specialist nurses trained in the needs of people with learning disabilities.
Good practice
NHS Greater Glasgow and Clyde have developed a hospital information booklet. This is completed in advance of the person with learning disabilities being admitted to hospital and is presented to ward staff at the point of admission. It contains personal information to help staff understand the patient's needs better, such as what they prefer to be called, their likes and dislikes, and how they can be comforted when they are distressed.
Avoidable hospital admissions
People with learning disabilities are more likely to be admitted to hospital as an emergency than people who do not have learning disabilities, and many admissions may be preventable. The commonest causes for admission are convulsions, constipation, diabetes, influenza and epilepsy. Some of these admissions could have been prevented by care provided by community nurses and family doctors.
Use of Accident and Emergency Departments
High rates of accidents and injuries occur amongst people with learning disabilities. In particular, injuries due to falls are common. This may be attributable to increased rates of epilepsy, psychopathology, medication, sensory and neurological impairments and balance problems. Some injuries are attributable to problem behaviours such as pica, self-injury and destructive behaviours38. Appropriate risk assessment and management could significantly reduce the morbidity from accidents and injuries.
Good practice
Work in NHS Lothian is well established to identify and support frequent attenders to receive the healthcare and support appropriate to their needs. Definition applied as a frequent attender: more than 5 visits in 3 months or more than 10 visits in any 12 month period.
Staff are automatically alerted through NHS Lothian IT alert system which will flag that someone has reached the trigger point. The individual's circumstances are analysed by Primary Care physician within A&E to determine any reasons for frequency. This results in a letter to the individual's GP alerting them. Where appropriate, through collaboration between the individual, the GP and the Primary Care
Physician, a care plan is developed. This has demonstrated:
- More appropriate attendance
- Appropriate admissions
- Appropriate investigations
- More appropriate management and support of vulnerable people.
Where this involves people with learning disabilities the Learning Disability Nurse Liaison Service works in partnership with the A&E Primary Care physician to ensure that the holistic needs of the people with learning disabilities are considered, and that, where appropriate along with the GP, the local authority, care agency and Community Learning Disability Team are engaged in reviewing the individual's needs, and informing the care plan. Quarterly meetings to specifically consider frequent attenders at A&E are attended by the Learning Disability Nurse Liaison service to provide learning disability expertise, and to ensure that all adult support and protection issues are fully considered with and for people with learning disabilities.
The same as you? said that the general healthcare needs of people with learning disabilities should be met in the same setting as the rest of the population. This is an appropriate but challenging aspiration given the co-occurring nature of need.
Co-occurring health needs have the potential to add risk to the lives of people with learning disabilities. The quality and effectiveness of health care given to people with learning disabilities has been shown to be deficient in a number of ways. Dependence on others for mobility and feeding in hospital is more prevalent among those with learning disabilities. Family carers of people with learning disabilities sometimes feel that health professionals do not listen to them.
Case study
In 2011 Edward was an inpatient in an acute care hospital. Edward was unhappy with some areas of the care and treatment he received during his admission. He decided to share his feedback with NHS staff to highlight and reinforce the importance of delivering person- centered care. Edward was invited to work with NHS staff to improve services. Edward worked with senior staff to develop a film interview of his experience. He also worked with the Scottish Consortium for Learning Disability to produce a learning and education resource39. Edwards's hard work and dedication was recognised in 2012 when he was awarded NHS Greater Glasgow and Clyde Chairman's Award in the category of Patient Ambassador.
Recommendation 24
That NHS Boards and local authorities across Scotland should work in partnership to ensure that people with learning disabilities receive the appropriate levels of support in general hospitals. This should include appropriately funded support from familiar carers as well as support from specialist learning disability acute care liaison nurses.
Recommendation 25
That by the end of 2016 NHS Boards should ensure that people with learning disabilities who attend acute care hospitals, including all medical and surgical specialties and accident and emergency departments, are identified and monitored to improve outcomes of hospital care and treatment, ensuring that health care is provided in the most appropriate setting.
Dementia
The population as a whole is experiencing increased longevity and this applies as much to people with learning disabilities as it does to the general population. Studies predict a 36% increase in the numbers of older people living with learning disabilities between 2001 and 2021 as a consequence of improving health and social care40. This signifies that this group will encounter many of the conditions associated with ageing and this will include dementia.
Although studies vary, it is recognised that people with learning disabilities experience higher rates of dementia than the general population. Figures suggest that prevalence rates are 4 times higher regardless of the cause of learning disability and that onset of the condition is about 10 years earlier than in the general population41.
By contrast, people with Down's syndrome experience significantly higher prevalence rates and earlier onset of the condition is also reported at between 30-40 years younger than the general population42. It is also estimated that prognosis rates are poorer with an average of 5 years between diagnosis and death43.
Diagnosis itself can be difficult with typical tests not being suitable for people with learning disabilities, baseline assessments not implemented universally and problems with detection of the early signs of the condition leading to delay in referral for diagnosis and therefore treatment. Differential diagnosis must be considered and is essential in establishing correct diagnosis and appropriate interventions44.
Pain recognition and pain management is often over looked amongst people with learning disabilities and many with dementia will experience similar levels of pain as those with cancer45. The Scottish Government Dementia Strategy46 specifically highlights the increasing need of people who have learning disabilities and dementia and highlights that dementia care is a national priority for the government. As part of the second National Dementia Strategy we intend to undertake a specific piece of work looking at the need for national action around linkages between dementia and other disabilities and chronic conditions; and the need for national action around early onset dementia.
Everyone with dementia - including those with learning disabilities - are entitled to receive care, treatment and support in line with the Standards of Care for Dementia in Scotland47. People with dementia and learning disabilities should receive a multi-disciplinary assessment of their care needs, including attention to removing any barriers to effective communication between the person with dementia and service providers. The Promoting Excellence dementia skills framework48 - which is designed to help services meet the dementia standards - requires staff working at enhanced level and above to understand the potential impact of a diagnosis of dementia on people with learning disabilities.
There is a need to recognise that dementia is a life limiting condition and that it should be approached with a focus on palliative care with partnership and coordination between both learning disability and palliative care services.
Palliative Care
Life limiting illness is more prevalent in the learning disability population with an estimated 61% of people with learning disabilities living with a specific long term illness or additional disability49.
People with learning disabilities are less likely to access specialist palliative care than the rest of the population50. In addition, people with learning disabilities are less likely to be informed of a diagnosis of a life- limiting or threatening illness or condition or given indications of prognosis, compared to the general population, and they are rarely encouraged to explore sensitive issues such as loss, death and dying51 52. Furthermore, evidence suggests that many people with learning disabilities will not have their pain recognised or sufficiently managed as a consequence of the same factors that affect equity in accessing healthcare. Many now experience periods of increasing frailty, organ failure, cancer and dementia as well as other life-limiting conditions.
It has been reported that people with learning disabilities encounter all of the major life- threatening diseases at least 5-10 years earlier than the rest of the population and that the time frame for survival is poorer53. Consideration also needs to be given to the increasing numbers of infants surviving the neonatal period due to advances in medical care. Many are surviving not just infancy but into childhood and adulthood with multiple disabilities and complex health needs requiring palliative care54.
With increasing numbers of people with learning disabilities requiring continuing care and support it is vital that we recognise that the skills and knowledge of health and social care staff will influence the overall experience of the individual, carers and family.
It is therefore becoming increasingly important to grasp the significance of palliative care across the age range of people with learning disabilities who have life- limiting or life- threatening illness or conditions.
It is only through inclusion, education, by making reasonable adjustments and developing robust partnerships that lead to collaborative working that people with learning disabilities will experience equity in accessing palliative care services.
In order to move forward improvements in care for people with learning disabilities who have palliative care needs it is crucial that there is a commitment to partnership working between Palliative Care and Learning Disability services55. The array of unmet learning needs experienced by both specialist services can be addressed through joint working and learning.
Case study
An example of such partnership working is the ongoing project Learning Disabilities and Palliative Care-Building Bridges: Supporting Care which is hosted by The Prince and Princess of Wales Hospice in Glasgow and jointly led by two senior practitioners from learning disabilities and palliative care services. Key practitioners have been identified from both learning disability and palliative care services and meet regularly to develop skills, knowledge and confidence within a framework of partnership and collaborative working. The development of a care pathway, underpinned by evidence based practice, to promote the delivery of appropriate and high quality palliative care for people with learning disabilities is fundamental. A care pathway (currently being developed) aims to support practitioners across all settings including learning disability services, social care, primary care, secondary care and specialist palliative care services as well as other contributors.
Recommendation 26
That the Glasgow palliative care pathway is evaluated and rolled out nationally by 2015 to improve the care outcomes for patients with learning disabilities.
Bereavement and Loss
It is important that a strategy on learning disabilities takes into account the experience of grief following the death of someone close. Loss can be a very painful, complex and confusing mix of experiences for someone with learning disabilities56. Some believe, however, that people with learning disabilities lack the capacity to understand complex concepts such as death and loss, which results in a lack of social recognition of the pain they are experiencing.57 It is important that paid carers and professionals are educated in recognising and supporting people with learning disabilities who have been bereaved.
Each person with learning disabilities is an individual and will grieve as an individual. It is important not to make assumptions about grief, rather to think about what will be helpful for each individual. The person with learning disability may experience two or more major life changes in a very short time. If these changes occur in addition to loss, this may make the grieving process very difficult for the bereaved person. In addition, a number of factors can affect how someone responds to bereavement: the nature of the relationship, the circumstances around the death and the person's ability to understand and communicate.
Cultural aspects, religious and spiritual beliefs, will also impact the grieving process. Finally, existing mental health issues may further complicate grief.
Without sufficient support, people with learning disabilities do not cope well with grief. In supporting a person who is grieving, it is important to remember that grief is normal - when someone has been special to us, their death leads to a range of feelings all of which are normal.
It is also important to remember that grief can also produce physical symptoms. An understanding of the person's use of communication can help to identify how best to explain the death. This part of the process is important because people with learning disabilities do experience change and an explanation is necessary. People with learning disabilities may already find change very difficult. A loss will inevitably cause major changes in the person's relationships and surroundings. A process of planning for a change may be helped by considering the transitions that might take place following a loss, these also include anticipating difficult times (e.g. anniversary of loss, Christmas). In supporting people with learning disabilities who are experiencing grief it is important that they are listened to and have their experience acknowledged and validated.
Giving the person opportunities to talk about the loss can reassure them that their experiences are normal. In addition, there needs to be a wider recognition of the importance of attending rituals of remembrance for people with learning disabilities, - for example, attending the funeral.
Support from others is crucial to the person's ability to accept the reality of the loss, experience the emotions that come with loss, adjust to life without the person and find an enduring connection with them.
Contact
Email: Julie Crawford