Medical students at Scottish universities: EQIA
Equalities impact assessment (EIA) relating to plans to increase the number of Scots dom/EU medical students by 100 and decrease the number from the rest UK by the same, to retain an estimated 36 extra doctors per year within specialty training.
3. Background
The Scottish Government is committed to creating a sustainable medical workforce.
Scotland, in common with other UK nations is facing a number of supply side challenges most notably in particular specialities and locations. The Scottish Government is taking a number of actions to ensure that we have a sufficient number of trainee doctors coming through the system to supply us with the qualified doctors we need in the specialities that we need.
As part of this effort we are growing the medical workforce. The Scottish Government has invested significantly in medical undergraduates. By 2021, the Scottish Government will have increased medical school places by 190 in total, an increase of 22% from 2016 levels.
In addition to growing the workforce, however, it’s clear that we need to retain more of those whom we train. A number of initiatives have been introduced to improve the retention of medical graduates – for example a trial of a ‘return of service’ bursary, available to students of the new ScotGEM graduate entry medicine programme.
Evidence shows that Scotland domiciled graduates from Scottish medical schools are retained at almost twice the rate of graduates from the rest of the UK (rUK) into speciality training. The retention rate is lower again for fee paying international students (see Table 1 below).
Table 1 Retention rate into year 1 of speciality training of domicile groups studying at Scottish Medical Schools[1]
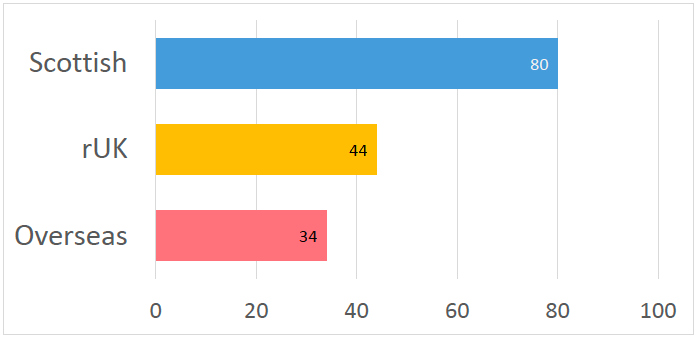
A profile of our medical student population also reveals that Scotland has far fewer “home” i.e. Scotland-domiciled medical students in comparison to England and Northern Ireland. Data shows that just over 50% of the intake to undergraduate medicine at Scottish universities is Scotland domiciled and this has been the case for a number of years.[2] We do not have reliable decoupled data from which we can reliably ascertain a retention rate in NHSScotland for EU students.
In November 2017, the General Medical Council (GMC) published a report[3] which provided an analysis of the transition from the foundation programme to the next stage of training. It found that-
“Scotland and Wales have a smaller proportion of their own high-school students entering their foundation programmes, and this matters. A number of factors feed into the differences between the four countries.
The first is that Scotland and Wales have far fewer home-domiciled medical students, and consequently, fewer home-domiciled foundation doctors than England and Northern Ireland.”
In 2016 around 78.2% of England’s Foundation doctors were home-domiciled (the figure is higher for Norther Ireland 89.0%) but for Scotland this drops to 52.4%.
The report confirms that this matters for two reasons.
1. Home-domiciled doctors are less likely to take a break from training.
2. Home-domiciled doctors are less likely to move to another UK country.
Consequently, despite recent significant investment, evidence confirms that if we do not take action to improve the retention of medical undergraduates then this investment will not translate into the medical workforce that we need.
Ministers therefore wish to see further action taken to increase the number of Scots domiciled students in medical intakes and have been working closely with the SFC on this matter. Ministers consider that replacing 100 RUK medical students with 100 Scots dom/EU students on a phased basis over the next three years would help to retain medical school graduates in Scotland in the long term. Ministers have given guidance to the SFC which the SFC can take into account when allocating funding to universities.
The benefit of adopting this policy is that it improves the sustainability of the medical workforce in Scotland. Once we have increased Scotland/EU domiciles by 100 and decreased rUK domiciles by a corresponding amount we estimate that we will retain approximately 36 extra doctors per annum within current headcount (including the planned increases.)
Contact
Email: rachael.fairbairn@gov.scot