Improving Together: A National Framework for Quality and GP Clusters in Scotland
Complements the development of the Scottish national GP contract.
The GP Cluster
As senior clinicians, in their role as expert medical generalists where continuity of care and the longitudinal therapeutic relationship with patients remains important, GPs are ideally placed to be able to contribute effectively within a quality framework that is contextualised locally. The Scottish GMS contract will therefore facilitate and encourage some GPs to take on a greater role in the assessment and monitoring of quality within the systems in which they work as Practice Quality Leads and Cluster Quality Leads as part of the internal quality assurance of local services.
GP clusters were introduced in Scotland in the 2016/17 GMS agreement between the Scottish GP Committee of BMA Scotland and the Scottish Government [4] in the context of health and social care integration and formation of localities within HSCPs. The agreement specifies that each GP practice will have a Practice Quality Lead [5] that will engage in a local GP cluster. Each GP cluster will have a GP designated as a Cluster Quality Lead who will have a coordinating role within the cluster [6] .
Definition
A GP cluster is a professional grouping of general practices, represented at periodic meetings by Practice Quality Leads ( PQL), which may take place either face to face or by video conference depending on individual circumstance or need. Each GP cluster will have a Cluster Quality Lead ( CQL) whose role is to facilitate and guide the members and liaise with locality and professional structures.
To do so fully and effectively, there must be adequate infrastructure that supports the cluster and those assuming roles as PQLs and CQLs. This includes resource for protected time within their contract, and an infrastructure that supports leadership, assists data provision and analysis, facilitation and improvement activity, with appropriate and robust local governance structures in which they can operate.
Clusters may be of different sizes, influenced by the local circumstance and geography. As a principle, they should be viable for small group work, with typically a membership of between 5 and 8 practices. The purpose of these clusters is to provide a mechanism whereby GPs may engage in peer-led quality improvement activity within and across practices and also contribute to the oversight and development of care within the wider healthcare system. These purposes may further be described as intrinsic and extrinsic quality roles:
| Intrinsic | Extrinsic |
| Learning network, local solutions, peer support | Collaboration and practice systems working with Community MDT and third sector partners |
| Consider clinical priorities for collective population | Participate in and influence priorities and strategic plans of Integrated Authorities |
| Transparent use of data, techniques and tools to drive quality improvement - will, ideas, execution | Provide critical opinion to aid transparency and oversight of managed services |
| Improve wellbeing, health and reduce health inequalities | Ensure relentless focus on improving clinical outcomes and addressing health inequalities |
Fig 2 Roles of the GP Cluster
Each Health and Social Care Partnership is divided into localities, and it is perhaps within these that the majority of GPs will make their most valuable contribution.Given this intention, the geographical alignment of practices within these localities is important. Though it is recognised that at the outset some practice boundaries may extend across localities, practices should be members of a cluster within the locality that their main premises and / or majority of patients are based.
This arrangement will build upon existing clinical governance and quality structures within health boards and Health and Social Care Partnerships, but more fully involves GPs in the discussion, using the data that they hold alongside data and intelligence from other sources.
The purpose of these locality quality structures is to use data and health intelligence at a local level, cognisant of local priorities, to facilitate assurance and to drive improvement in the quality of care provided by different parts of the health and social care system.
Where this assurance is not evident, further information may be requested or specific actions mandated to the practices, clinical or management teams, in line with the established purpose and principles of the framework. A route of escalation within the local governance arrangements is necessary and may best be provided via the clinical and care governance structure of the integrated authority, or its local equivalent.
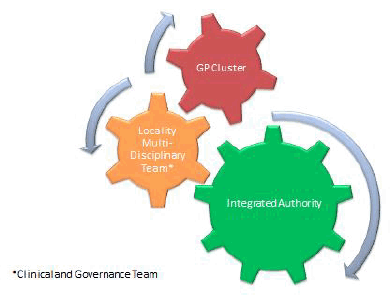
Fig 3 System of Influence
Figure 3 demonstrates schematically the potential system of influence between these different groups within a Health and Social Care Partnership structure; each has influence on each other, regardless of "size". The cluster quality leads have an important role in the GP cluster, in particular by demonstrating leadership in how discussions and activity here link to the wider clinical priorities, quality structures and to the locality management team. This allows optimal communication, analysis and discussion about all aspects of care within the locality and its linked community services and hospital(s). Experience in the transition arrangements already demonstrates the value of integration of public health practitioners with their expertise proving valuable to aid understanding and discussion on local population health within clusters.
Utilised in this way, each Health and Social Care Partnership may receive internal assurance about the care in each locality, be made aware of any action plan necessary to address identified gaps, or influence resource necessary to address this. Links between the locality quality group and the locality management team will allow clinical risk associated with any perceived issues or problems to be managed, with a clear structure of escalation where this cannot be addressed at the locality level.
In order that this is fully effective, there needs to be appropriate, open and transparent sharing of agreed datasets within these networks for public and patient benefit. Alongside this, agreed mechanisms of escalation and response should be identified in the event that progress to address acknowledged actions or gaps be incomplete.