Improving Together: A National Framework for Quality and GP Clusters in Scotland
Complements the development of the Scottish national GP contract.
Background
Since 2012, the GP contract in Scotland has increasingly developed its own characteristics, showing divergence from the GMS contract in the rest of the UK. The Scottish Government and BMA Scotland have agreed to develop a Scottish GP contract aligned with the Scottish Government's 2020 Vision of Health and Social Care that will deliver positive outcomes for our citizens, helping GPs to fulfil their potential in addressing the health and wellbeing of their patients and communities in a sustainable model of care.
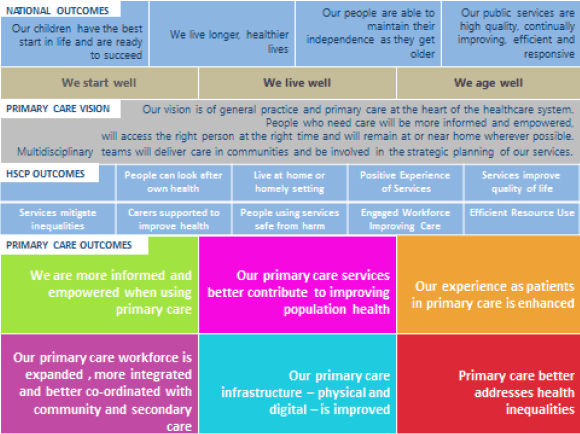
Fig 1 Outcomes
This will support GPs to care for their patients and address the health needs of their local communities better, and to help exploit the opportunities that are created by health and social care integration and closer working with colleagues across the whole system of services from whom our communities receive care.
Caring for an increasing population, which is living longer, and more often with multiple conditions; together with addressing the underlying determinants of ill health and the health inequalities that are experienced by some communities has been a challenge. However, by supporting practices through a suitable contract and approach to quality that better recognises and addresses the needs of its local population and workforce, there will be a greater opportunity to respond to these issues at an individual and community level.
It is, therefore, critical to preserve and nurture the generalist approach to providing longitudinal care across the ages, so that our citizens are supported to Start Well, Live Well, Age Well, and, indeed, Die Well.
Improving Together offers an alternative route; facilitating collaborative relationships; learning, developing and improving together for the benefit of local communities
GPs cannot address all of these issues by themselves. It is by strengthening the role and professional relationships of the entire multidisciplinary team in Primary Care; by enabling better informed and empowered patients; by improving the interfaces of care between professionals and between sectors; and making best use of the therapeutic and supportive assets within communities, that this becomes possible.
There is over a decade of experience from the current GMS contract, and much innovation within the general practice profession from which to learn. The Quality and Outcomes Framework, from 2004 - 2016, defined for many Quality in General Practice, but in reality touched only upon a little of what GPs' everyday experience of delivering high quality care actually was. Indeed, much of this care is difficult to measure in any quantitative way, but we must learn from experience in other countries and industries how best to do so in order that we can improve.
As professionals, clinically ambitious to provide high quality care for our communities, it is well recognised and understood that the approach taken in the Quality and Outcomes Framework did not universally support GPs in using their experience and expertise across this diverse population of people and complex workload.
GP Clusters require: Data; Health Intelligence Analysis; Facilitation; Improvement Advice; Leadership.
Improving Together offers an alternative route to continuously improve the quality of care that citizens receive by facilitating strong, collaborative relationships across GP Clusters and localities with, at its heart; the intention of learning, developing and improving together for the benefit of local communities.
To realise this potential fully requires support; relevant and timely data; analytical expertise to assist in its interpretation; facilitation of constructive conversations; and implementation of appropriate improvement strategies. Without these components, there is a credible risk that they will fail in their intention.
Common Purpose
In describing this common purpose and to ensure a transparent and unrelenting approach that improves the health and wellbeing of the population, a series of principles and values will underpin this framework:
- Respect the professionalism and clinical ambition of GPs and practice staff in their pursuit of continuously improving the quality care that they provide.
- Recognise this by a proportionate and an appropriate use of data and/or indicators with greater focus on system-wide care and outcomes where this is possible.
- Utilise GP Clusters as the means of establishing peer-led, values driven quality improvement activity with both a focus on practice based (intrinsic) quality and contribution to system based (extrinsic) quality.
- Establishes a sound and proportionate approach to internal quality assurance and shapes the necessary external quality assurance approach in Scotland
- Provide for local flexibility; enabling use of evidence to identify local clinical priorities and also proper engagement with local communities about what matters to them in the interactions that they have and services that they receive from their GP practice.
- Promote a more equal partnership with patients in decisions relating to their care, encouraging shared decision making and a stronger emphasis on conversations that establish what is important to individuals, their families and their carers.
- Be complementary to the new ways of working within Health and Social Care Partnerships and facilitate the key leadership role of GPs in shaping and monitoring the quality of services provided by those partnerships, in both primary and secondary care settings.
- Recognise that continuing and developing the generalist approach, which encompasses both biotechnical and psychosocial aspects of care, is essential for the future of high quality care in GP clusters.
Common Values that underpin this framework
- To provide open, consistent, high quality and accountable public services.
- To encourage mutual respect between all stakeholders, encompassing health care and staff governance.
- To ensure openness in appropriate and proportionate transparency of necessary information.
- To encourage partnership in local needs assessment, and strategic planning with the shared ambition of improving population health.
- The application of joint approaches across primary, secondary and social care to common problems.
- The provision of best value and best use of available finite resources, recognising the need for choices to be made in how resources are used in primary healthcare.
- To promote continuous improvement in citizens' experience of care and transparency and candour in our interactions with other professionals and the public.
- To ensure that the GP cluster supports the sustainable delivery of high quality healthcare in a community setting, based upon identified local community needs, and contributes towards addressing the NHS Board and Health & Social Care Partnership priorities.
- To recognise that evaluation and research are essential to support an evidence-based approach to quality improvement.
In articulating this common purpose and values, those organisations involved in the development of this framework demonstrate their commitment to Realistic Medicine and to achieving the triple aim of improving citizens' experience of care, the health and wellbeing of the population and the pursuit of high value care whilst also creating a professional working environment that is more attractive in which to practise.