Human Tissue (Authorisation) (Scotland) Bill: BRIA
Business and Regulatory Impact Assessment (BRIA) exploring the costs and benefits associated with the move to a soft opt out system of organ and tissue donation.
2.0 Purpose and Intended Effect
This Business Regulatory Impact Assessment presents a range of economic costs and benefits utilising 3 scenarios (low estimate, best estimate and upper estimate). The low estimate (do nothing) is used as a baseline against estimates of potential impact if an increase in the authorisation rate were to result from the move to a soft opt out system of organ and tissue donation.
2.1 Objective
Organ and tissue donation and transplantation is an incredible development in modern healthcare which continues to save and significantly improve lives. Conditions that severely limit lives, or which are ultimately fatal, can be cured or significantly improved by the transplantation of replacement organs and tissue from donors. Yet despite the very real benefits of transplantation there is still a shortage of organs, and over 500 people in Scotland are waiting for a transplant at any one point [1] . It is important therefore that as much as possible is done to maximise the number of donors, particularly as only around 1% of people die in circumstances where they can become a deceased organ donor [2] .
Organ and tissue donation and transplantation is dependent on the generosity, commitment and skill of a number of different people. Deceased donations occur immediately following tragic events and at a time of great sorrow. The willingness of donor families to think of other people and the gift of donation at such times makes their generosity all the more special. Donation is also reliant on the commitment, dedication and skill of those in the NHS who work collaboratively across many disciplines to facilitate donation and transplantation. This work is supported by a commitment from the Scottish Government, working in partnership with others to continue to promote donation.
Authorisation is an important factor which often affects whether donation, and ultimately transplantation, can proceed. Although Scotland has the highest proportion of people registered on the NHS Organ Donor Register ( ODR) in the UK (46% [1] compared to a UK average of 38% [3] ), surveys show that the majority of Scots support donation [4] .We know, therefore, that many people who support donation simply do not get around to registering their wishes. Additionally, each year a significant proportion of families refuse authorisation for their loved one's organs to be donated. In 2017-18 in 44% of cases in Scotland where family members were approached about donation, authorisation was not given or (in a few cases) the family overrode the authorisation the person had previously given [5] . It is important, therefore, to look at ways in which we can ensure individuals who would want to donate, are able to do so. A move to a soft opt out system is a way to do this.
The primary purpose of the Bill is to introduce a soft opt out system of organ and tissue donation for the purposes of transplantation. The Human Tissue (Scotland) Act 2006 ("the 2006 Act") currently provides the legal basis for authorisation of donation for transplantation and other purposes. The 2006 Act provides that organs and tissue can only be donated by someone if either they have authorised donation before they died, or if their nearest relative authorises the donation on their behalf – this is known as an 'opt in' system. The Bill will provide a new, additional category of 'deemed authorisation' which will apply to most adults who have not otherwise explicitly opted in or out of donation via the ODR, or who have not otherwise recorded an explicit decision about donation. This would mean that where the person was not known to have expressed any objections to donation, the assumption would be that the donation could proceed. As well as retaining the legal basis for individuals to explicitly opt in to donation, the Bill will also provide a legal basis for an explicit declaration of non-authorisation (or 'opting out').
Deemed authorisation will not apply to people in excepted categories - children under the age of 16, adults who do not have the capacity to understand the nature and consequences of deemed authorisation, or adults resident in Scotland for less than 12 months. These groups would require explicit authorisation – either self-authorisation during their lifetime or, upon their death, authorisation by a nearest relative (for adults) or a person with parental rights and responsibilities ( PRRs) (for children).
Organ and tissue donation and transplantation is a complex and multi-faceted process, often operating to time pressures. No single measure will radically increase donation rates; instead action needs to be taken on every single part of the donation pathway in order to drive continuous improvement. The Scottish Government has already committed to a package of measures to increase donation and transplantation. These are set out in A Donation and Transplantation Plan for Scotland 2013-2020 [6] (the Plan). The introduction of a soft opt out system of donation will add to these existing efforts.
At the same time, it is important to guard against any harm to the progress made so far as international experience shows that if legislative change is not implemented carefully donation rates can be negatively impacted. The Government's policy in supporting organ and tissue donation and transplantation, and in developing the Bill, continues to have these important potential consequences in mind.
2.2 Background
To support and encourage donation a range of non-legislative measures are already being taken forward. In 2013, the Scottish Government published A Donation and Transplantation Plan for Scotland 2013-2020 which sets out the ways in which the Scottish Goverment hopes to improve donation and transplantation in Scotland. It builds on the progress made by implementing the recommendations of the UK Organ Donation Taskforce. The monitoring of implementation of the Plan is overseen by the Scottish Donation and Transplant Group.
The Plan identifies five priorities the Government wishes to deliver: increasing the number of people who have made their wishes about organ donation known; increasing the availability of organs; making every donation count; ensuring NHSScotland supports donation and transplantation; and ensuring the public in Scotland is informed and engaged about donation and transplantation. Significant progress has been made in increasing numbers and delivering meaningful improvements through recommendations in the Donation and Transplant Plan, for example:
- high profile publicity campaigns to encourage people to join the Organ Donor Register;
- internationally recognised schools educational resource pack to increase awareness of pupils about organ and tissue donation;
- work with Kidney Research UK which trains volunteers from South Asian communities to become peer educators to increase awareness of kidney disease and organ donation;
- dedicated regional manager for Scotland to manage the Specialist Nurses for Organ Donation and to take forward key initiatives to help increase donation.
Since the start of the plan of improvement in 2008 there has been:
- an 89% increase in deceased donor numbers in Scotland (up from 54 [5] to 102 [1] )
- a 78% increase in the number of lifesaving transplant operations from deceased donors undertaken for patients living in Scotland (from 211 [5] to 375 [1] )
- a 22% decrease in the number of people resident in Scotland on the active transplant waiting list (689 [5] to 534 [1] ).
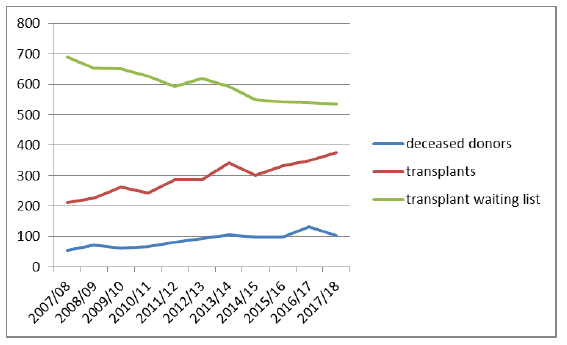
While figure 1 shows that numbers of deceased organ donors have been gradually increasing over recent years, donation rates do fluctuate, particularly given the relatively small numbers involved. Given the complexity of the donation process and pathway, there are a number of different unrelated factors which can affect organ or tissue donor numbers, including: the number of individuals dying in circumstances suitable for donation; co-morbidities of potential donors; and the timing of death – either in advance of a donation discussion taking place, or after the permitted timeframe for donation to proceed. Despite significant improvements to the process and pathway in recent years 2017-18 has seen a decrease in the numbers of deceased organ donors [1] compared with the exceptionally high number of donors in 2016-17. This reflects that many of the factors which impact on donor numbers are not within the control of NHS staff. It is important therefore that we continue to do all we can to increase donation and transplantation.
Figure 1: changes in number of deceased organ donors in Scotland, transplants and those on the waiting list over time [5]
2.3 Rationale for Government intervention
The Purpose of the Scottish Government is to focus Government and public services on creating a more successful country, with opportunities for all of Scotland to flourish, through increasing sustainable economic growth. Encouraging people to support organ and tissue donation and increasing the number of donors will contribute to realising our Purpose by contributing to two of our Strategic Objectives:
- HEALTHIER - The introduction of a soft opt out system of organ and tissue donation aims to support a Healthier Scotland and in particular support the Purpose target of increasing healthy life expectancy in Scotland.
- WEALTHIER & FAIRER - It will also to some extent, over the longer term, help support the Purpose target of maintaining our position on labour market participation as the top performing country in the UK. This is because increasing the number of transplants undertaken will allow more people to get back into work.
2.4 Evidence Base to Establish Impact of Proposed Legislation
The evidence presented in this section is based on a rapid evidence review undertaken by Scottish Government Opt Out - Organ Donation: A rapid evidence review
2.4.1 International evidence on the impact of opt-out
The international evidence suggests that as part of a range of measures opt out systems can increase both deceased donation and transplant [7] . However, there is little robust evidence that demonstrates that opt out legislation alone will increase deceased organ donation and transplant. The evidence highlights the importance of non-legislative factors [8][9] , which can work effectively in both, opt out and opt in systems.
This section outlines research which suggests opt-out is effective and outlines its limitations.
A wide range of international evidence highlights that there is an association between countries with opt out legislation and higher rates of deceased organ donation and greater willingness to donate [10][11] . Illustrating that opt out systems can be successful. There is however a degree of uncertainty as to the size of these associated increases, with studies reporting opt-out legislation is associated with increases in deceased organ donation rates of 13 – 18 % [12] and 25 – 30% [13] . In contrast , several countries with the lowest numbers of deceased donors in Europe (Bulgaria, Turkey, Cyprus and Greece), also have opt out [14] which might indicate that that opt-out alone does not always lead to a high level of donations and that the relationship is more complex and dependent on other factors. Evidence as to why opt out has not been as successful in some nations as others is limited, but Bilgel (2012) study suggests that the impact of the opt out legislation in Greece was limited by a lack of medical staff and transplant units. The impact of infrastructure changes is discussed further below.
Whilst a few before and after studies provide some indication of success, these are limited and it is not possible to rule out the influence of other known or unknown factors [15] . Often changes to opt-out system occur with other changes, such as increased infrastructure changes, making it impossible to establish the impact of the legalistation alone. Rithalia et al (2009) [16] identified five before and after studies, which represented the experience of three different countries: Austria, Belgium and Singapore. Following the introduction of opt out organ donation legislation the studies found an increase in organ donation rates. The evidence of increase in organ donation in Austria was from 4.6 to 10.1 donors per million population per year in the four years after the introduction of presumed consent. However the largest increase was to 27.2 per million in the five years after introduction of infrastructure changes, such as full time transplant coordinators. The study therefore indicates that whilst presumed consent legislation change can influence an increase in organ donation registration, it cannot be viewed as a panacea; infrastructure changes seem to have a greater impact on organ donation.
Experimental research conducted in artificial setting provides some indications of how opt-out potentially increases donations [17] [18] . Potentially, individuals in opt out systems attribute less personal cost to donating their organs than in opt in systems, and simply framing organ donation as the default may increase individuals' willingness to donate. Caution should be applied when applying this evidence to real world settings.
There is encouraging evidence to support the use of opt out, however it is currently impossible to infer that an increase is due to the opt out legislation alone and the evidence highlights the importance of other factors in driving increases.
Other important factors
Evidence suggests that in order for opt out to be effective in contributing to an increase in donation rates it has to work as part of a package of measures [19][20] . Family consent, use of a register, media coverage, public/staff support and staff training have all been suggested as important factors in ensuring the success of opt-out. Further, it is important to guard against any harm to the progress made so far as international experience shows that if it is not implemented carefully donation rates can be negatively impacted. Chile experienced an increase in family refusals and a decrease in donation rates following the implementation of opt-out legislation [21] . 70% of the population were unaware of the legislation change and this was highlighted as a key factor in the lack of success of the legislation [22] . Moreover, Brazil had to withdraw the implementation of its opt-out legislation largely due to an increase in medical mistrust and public anxiety [23] .
Currently, Spain has the highest rate of organ donors in the world and utilises an opt-out system which was introduced in 1979. However, the rate of organ donation only increased, from 14.3 to over 43.4 donors per million population in 2016, with the creation of Organizacion Nacional de Trasplantes in 1989. In particular, the introduction of well-trained transplant coordinators and public health campaigns helped influence this dramatic increase in deceased donors; suggesting infrastructure could be a primary factor in the increase.
It is clear from the evidence that both context and non-legslative measures are important in the success of organ donation systems, but there are positive indications to suggest that opt-out legislation can contribute to increasing deceased donation as part of package of wider measures. Further detail on the evidence can be found in a rapid evidence review undertaken by Scottish Government in 2018 'Opt out organ donation: A rapid evidence review'.
2.4.2 Evidence from Wales
The Evaluation of the Human Transplantation (Wales) Act: Impact Evaluation Report [24] which was published on 30 November 2017 suggests that a longer period of time is needed to draw firmer conclusions around the impact of the change in the law. The evaluation found that there had largely been limited impact on deceased donation, although it recognised that the timeframe since implementation was insufficient to firmly establish this.
Evidence from Wales shows that prior to the introduction of the opt out system in Wales in December 2015, there had been an increase in the number of people who have opted in to the NHS organ donor register. In 2014/2015 the share was 34% of the Welsh population. The increased continued post opt out and in 2015/2016 the share was 36% of the population; further increase was experienced in 2016/2017 with a share of 38% of the population. However, it is too soon following the introduction of the system in Wales to determine whether the increase can be attributed to introduction of the legislation. Overall public awareness of the legislation also increased.
Associated with the change in legislation there has also been an increase in the percentage of people who have opted out on the organ donor register. 2014/2015 the percetage was 0% of the population; (as there was no option to opt out ); in 2015/2016 the percentage increased to 5% of the population and in 2016/2017 the percentage further increased to 6% of the population opted out. Although this number is increasing, slightly, this suggests that people are able to make an informed decision about whether or not toopt out.
The overall consent rate for deceased donation in Wales has increased from 54% in 2013/14 to 64% in 2016/17. It is still too early to judge the impact on deceased donor rates; it is also difficult to estimate how much of this change is due to the introduction of the legislation and the communication campaign that was introduced with it. Overall the Welsh study concludes that it is too soon to draw firm conclusions.
2.4.3 Public opinion
The most recent Scottish survey shows that the majorit of the public are supportive of an opt out system. The TNS survey 2016 found that 59% agreed that "everyone should be presumed to be willing to be a donor unless they register a wish otherwise".
Prior to Wales moving to an opt out system; the Welsh Government conducted a review of three public opinion surveys. The public opinion survey of a representative sample of adults living in Wales in 2012, found that 49% of respondents were in favour of changing to an opt out system, while 22% were against. A further 21% said they 'needed more information to decide'. Another Wales-based survey indicated a greater proportion of respondents supported the move to an opt out system than were against it. The Welsh Government also conducted public surveys where they found that the public support in Wales for opt out increased after implementation of the legislation, from 49% in 2012 to 67% in 2015. Therefore this suggested that the Welsh public were supportive of opt out prior to legislation change.
However some groups within the population were not so supportive of the legislation change. In 2010 interviews with UK leaders of the main faith and belief organisations found that the majority supported an opt in system and wanted to retain this over an opt-out system [25] . There is insufficient data on the representative views of the religious populations themselves due to the small numbers involved and caution should be applied in drawing inferences. Although a survey of Western Muslims (British, European, North American and Oceanic geography) on attitudes to organ donation found that only 26% of respondents agreed with the concept of presumed consent (or 'opt out'). This compared with 55% who did not, and 20% who did not know [26] .