Guidance on Health Assessments for Looked After Children in Scotland
This guidance has been produced to assist those involved in carrying out health assessments of our looked after children and young people. It sets out the minimum standardised elements of a health care pathway which we would expect Boards to implement in collaboration with local authorities and other organisations.
Section 4: How to Deliver a Health Assessment
The following charts show the systems and processes required to deliver comprehensive health assessments for children and young people who become looked after.
There may not be a requirement to have repeated comprehensive health assessments every time the child moves into and out of care.
Looked After Children and Young People Health Assessment Pathway
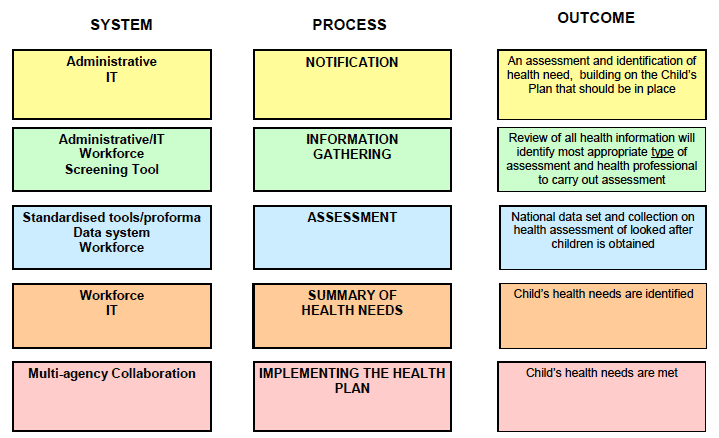
| Task | Requirement | |
|---|---|---|
| Notification | Local Authority to inform Health Board re status of child | Every Health Board to have a central administration co-ordinator for looked after children |
| Health Board to ensure consent to carry out assessment from person with parental rights and responsibilities is confirmed via Lead Professional | IT system | |
| Central admin to identify the key health partner to the plan | Local Authorities should have a standard list of essential information to be provided at time of notification | |
| Information Gathering | Generate a profile which includes:
|
Identify appropriate admin system and support to complete profile An IT system which connects primary care/universal services to secondary care and includes dental services, eg NHS SIRS, CHI and ISOFT/Education and Social Work systems |
| Review of profile by clinical staff | ||
| Identify most appropriate health professional to undertake a health assessment | A clinician with appropriate knowledge and skills should make this decision | |
| Inform appropriate person of their role/task | Health visitors, school nurses and paediatricians should know they have specific roles and tasks in this assessment and should be provided with adequate training and resources | |
| Has an assessment of emotional wellbeing /mental health been made? | A suitable screening tool has been used, eg WEMWS, SDQ, BAAF emotional and behavioural wellbeing profile | |
| Assessment | Carry out age appropriate health assessment as per agreed national guidance | Provide supporting documentation:
|
| Complete appropriate pro-forma | Health Board to provide a standard proforma based on national minimum data set | |
| A national system should be developed to collate the agreed dataset | ||
| Summary of Health Needs | Summarise identified health needs | Electronic communication |
| Complete child's health plan | ||
| Communicate with key health partner to Plan | ||
| Integrate health needs within inter-agency Child's Plan | Child's Plan | |
| Implementing Health Plan | Identify who will address health needs | Meeting required with Lead Professional to discuss how health needs will be addressed |
Part 1 - Notification
Referral Process To Health
The local authority must inform the health board nominated administrator for looked after children within 5 working days of any child or young person who becomes looked after. A health assessment should be carried out within 4 weeks of this notification to the Health Board. The Health Board should ensure there is a clear process to carry out a health assessment.
Consent
Local authorities should have guidance in relation to consent to the medical examination and treatment of children/young people who are looked after. They should make this known to the child/young person, health services, the parents, carers and staff. The arrangements for medical consent should be set out in each care plan where a child/young person is looked after. These will vary according to the legal status of the child/young person (Section 17(6) of The Children (Scotland) Act 1995), the age and understanding of the child/young person and whether a local authority does or does not have parental responsibilities for the child.
In Scotland, the starting point for who is entitled to consent to medical treatment for an individual child/young person is section 2(4) of The Age of Legal Capacity (Scotland) Act 1991. This states that:
A person under the age of 16 years shall have legal capacity to consent on his own behalf to any surgical, medical or dental procedure or treatment where, in the opinion of a qualified medical practitioner attending him, he is capacity of understanding the nature and possible consequences of the procedure or treatment.
Part 2 - Information Gathering
Before the health assessment, it is essential to gather as much relevant health and social information as possible.
This will include information from the following sources:
- local authority's information on the child, including child's plan incorporating social work report, child protection report and any available parental health information;
- child health surveillance information, including child health screening and immunisations;
- GP-held information;
- community health services;
- Health Visitors/School Nurses/AHPs;
- NHS system (eg TRAKCARE), access to note, attendance at Accident and Emergency and other paediatric departments, or out of hours GP services;
- referrals or contact with hospital services;
- referrals or contact with child and adolescent mental health services;
- referrals or attendance at primary care dental services (Public Dental Service or General Dental Practice).
Local authorities and NHS Boards should have in place protocols, which establish the framework for information sharing. The issues to consider would include:
- who has access to what information and how data security is ensured;
- arrangements for seeking consent to information sharing;
- how children, parents and other third parties are informed of, and allowed to challenge, information that is kept on them;
- how carers contribute to and receive information;
- mechanisms for sharing information between local authorities and health boards.
Guidance from the Information Commissioner's Office on information sharing between services in respect of children and young people is attached at Annex C.
Part 3 - Comprehensive Health Assessment
Objectives of health assessment
The objectives of the health assessment are to:
- Provide an opportunity to collate and to analyse the child/young person's health history including antenatal, birth, neonatal, past medical and family history.
- To identify unrecognised/unmet health needs, ascertain if the child/young person has missed or has any outstanding appointments, and to plan appropriate action.
- To comprehensively assess the child/young person's current physical, developmental and emotional health needs.
All assessments and planning by each Agency involved in a child's plan should be constructed around the 8 wellbeing indicators; safe, healthy, achieving, nurtured, active, respected, responsible and included. The Child's Plan should contain a holistic overview of all information gathered and assessments carried out and structured around the wellbeing indicators; a summary of how this information was considered in terms of the child's circumstances identifying strengths and pressures; how specific actions/ priorities were identified; and detail of a clear action plan. This must include the health assessment and action plan.
The comprehensive health assessment will lead to a single agency health plan that can be shared and integrated to develop the multiagency Child's Plan. The initial health assessment should be submitted to the multi-agency plan in My World Assessment format - ie strengths and pressures around SHANARRI.
This comprehensive assessment is best achieved using a proforma to prompt clinicians to seek relevant details and the recommended content for the different stages of childhood are outlined on pages 24-25. Local arrangements may vary, but standardised assessment tools have been developed which may assist NHS Boards (eg BAAF health assessment tool).
Information relating to the child's attendance, behaviour and achievement at school should also be taken into account as these factors can be related to unmet health needs and low self-esteem.
The clinician carrying out the assessment has a duty of clinical care to the child which includes making any necessary referrals for investigation and possible treatment of any health needs identified at the assessment. The clinician should follow up any concerns sharing appropriate, and proportionate information with the Named Person.
It should be ascertained at the time of this assessment whether the child/young person is already receiving or awaiting health treatment. Every effort should be made to ensure that being looked after does not disrupt existing arrangements or cause them to lose a place on a waiting list. Health professionals must be informed of placement changes in a timely manner.
The content of the assessment should be age sensitive and developmentally appropriate. The recommended content for the different stages of childhood are outlined on the following pages.
Age-appropriate recommended content of the comprehensive health assessment for looked after children and young people
Under 5s
For children under five years or pre-school, the focus will be on:
- Assessing child development, in particular the development of speech and language, gross and fine motor function, vision and hearing, play and pre-literacy skills, social and self-help skills and progress in nursery. Standardised assessment tools such as Schedule of Growing Skills may be useful.
- Assessing physical health and identification of health conditions.
- Assessing and interpreting growth.
- Ensuring childhood immunisations are complete for age.
- Dental health and registration with a dentist.
- Consideration of antenatal exposure to drugs and alcohol and exposure to blood borne viruses, either from birth or exposure in the home.
- Emotional wellbeing including consideration of attachment issues.
Ages 5-10
For primary school age children the focus will be on:
- Assessing child development, in particular the development of speech and language, gross and find motor function, vision and hearing, play, social and self-help skills, and progress at school.
- Assessing physical health and identification of possible health conditions.
- Assessing and interpreting growth.
- Level of physical activity, dietary intake and understanding of a healthy lifestyle.
- Dental health and registration with a dentist.
- Emotional wellbeing including consideration of attachment issues
- Assessing level of self-care skills; eg personal hygiene, tying shoe laces, telling the time.
- Awareness of basic safety issues, including road safety and social media.
- Where appropriate, to recognise and cope with the physical and emotional changes associated with puberty.
- Ensuring childhood immunisations are complete for age.
Adolescence and Leaving Care 11-18
For secondary school age children and young people and care leavers the focus will be on:
- Assessing physical health and identification of health conditions.
- Ability to take age appropriate responsibility for their own health, including responsibility for specific health conditions eg asthma, diabetes.
- Assessing and interpreting growth.
- Level of physical activity, dietary intake and understanding of a healthy lifestyle.
- Dental health and registration with a dentist.
- Vision and hearing - last eyesight test.
- Progress/attendance at school and whether any additional supports required.
- Ensuring childhood immunisations are complete for age.
- Communication and interpersonal skills, including ability to make and sustain friendships.
- Emotional health and wellbeing including consideration of mental health issues.
- Where appropriate, to recognise and cope with the physical and emotional changes associated with puberty.
- Assessing young person's understanding of relationships, sexual health and the particular risks of early sexual activity.
- Assessing young person's understanding of involvement with health risk taking behaviour eg smoking, misusing alcohol and drugs, inappropriate access to social media.
- Assisting the young person to access appropriate sources of information and advice about a range of health issues.
- Ensuring care leavers have an understanding of their own health history and knowledge on how they can access their health records so they are able to make informed choices relating to their health.
Specialist assessments
If the Comprehensive Health Assessment identifies the need for any further specialist assessment that the child or young person may require, the assessing clinician should discuss this need and make the appropriate referrals. Such specialist assessment may include:
- Specialist LAC assessment
- Child and Adolescent Mental Health Assessment
- Education Psychology Assessment
- Speech and Language/Physiotherapy/Occupational Therapy assessment
- Specialist Paediatric/Surgical Paediatric assessment
- Ophthalmology/Audiology
Part 4 - Summary of Health Needs
After the assessment the clinician should compile a health care plan specifying any timescales for actions to be completed and when the health care plan will be reviewed. As outlined in CEL 16 (2009), the clinician undertaking the health assessment takes responsibilities for ensuring the care plan is delivered/co-ordinated as appropriate.
Part 5 - Implementing The Health Plan
Where two or more agencies need to work together to help a child or young person, there will be a lead professional to co-ordinate that help. It is the responsibility of the Lead Professional to ensure that relevant assessment information, outcomes and actions are integrated into the Child's Plan and that what is recorded is agreed by the contributing parties.
Clear explanations should be given to the child/young person about any further consultations, treatment or care. Referral to local services should be made where appropriate.
If the child/young person ceases to be looked after the social worker needs to inform the LAC Administration team. On-going implementation of the child's health care plan will then be the responsibility of primary care.
Implementing Health Services for Looked After Children
Nursing Workforce
The Children's (Scotland) Act (1995) emphasises that looked after children are entitled to the same health services as any other child. In response most Health Boards have established LAC Health Teams based on local needs and requirements. Currently therefore, roles, titles, responsibilities, delivery models and managerial arrangements differ across Scotland. Initially aims of LAC Teams were to improve outcomes through assuring appropriate health assessment and intervention. In support NHS Education Scotland and the RCN developed A Capability Framework for Nurses who Care for Children and Young People who are Looked After Away from Home (2009).
Universal services
Universal services, Midwives, Health Visitors and School Nurses play a vital role in reviewing and improving the health of looked after children. For all pre-school children Hall 4 sets out a number of child health reviews from 0-5 years of age. For the majority of school age children, currently universal school health reviews are provided only once at Primary One although many school age looked after children are more likely to have poor attendance at school, be excluded, have more complex needs, and in addition many experience a number of placements making continuity of care and intervention difficult. For children of school leaving age to 18 years, no universal health services are identified to undertake the child's health assessment.
Specialist Looked After Children (LAC) Health Services
Over the past 12 years, the introduction of LAC Health Services, Lead Nurses and LAC Health Teams; paediatricians and LAC nurses, have made significant improvements in improving the health needs of looked after children. The principle aim is to improve outcomes through assuring delivery on statutory and CEL16 (2009) requirements and by providing continuity of health assessments from age 0-19. LAC Teams have evolved to include a variety of roles and complexities ranging from staff nurse to those at advanced practitioner level. These encompass engaging with vulnerable children, assessing and analysing health information and providing comprehensive reports detailing implications of the information for the child's current, future health and wellbeing. Prior to the development of specialist services for looked after children identified challenges included: inconsistent, delayed or repeated health assessments of variable quality, use of a variety of assessment tools, lack of consistent health care together with the need for additional consideration to be given to such issues as blood borne virus testing, sexual exploitation, abuse in care which universal services may not have previously considered.
CEL16 (2009) is currently the only performance measure against which all NHS Boards report in respect of looked after children.
Current Nursing Workforce
In June 2013 a review of current nursing provision for looked after children was undertaken by the Scottish Government's Directorate for Chief Nursing Officer, Patients, Public and Health Professions (CNOPPP) to identify existing nursing roles and resources. Findings indicate that the majority of current service provision is directed to looked after and accommodated children and young people. Some Board areas have expanded this to include all looked after children, as per CEL 16 (2009) requirements. Two models of service provision were identified.
Model 1 - Designated Specialist LAC Health Teams
Specialist designated nurses and LAC Health Teams offer health assessments for looked after and accommodated children. Usually these specialists are Band 6 or 7 nurses who may be led by a Band 8 nurse. These teams are responsible for undertaking statutory health assessments for looked after children, developing health care plans, coordinating health care and supporting staff and carers. They ensure information is gathered on admission to care, is regularly reviewed and provide reports for children undergoing permanency and adoption processes. Some teams are multi-disciplinary including paediatricians ensuring appropriate health action plans are in place based on health needs. Standardised comprehensive health assessment tools such as the BAAF are used. All approaches to medical consent and information sharing, complies with The Children (Scotland) Act 1995, Age of Legal Capacity Act and conditions of orders from children's hearings. The LAC nurse co-ordinates children's health care irrespective of the number of care placement moves, ensuring coordinated continuity of health care and avoiding repeated assessments.
These designated nursing services are in addition to universal services such as health visiting and school nursing and encompass leadership and management responsibilities. Teams serve as a HUB and central point of contact for health information, the local authority and care placements irrespective of where a child is placed. Roles are highly developed, understanding the impact of neglect and abuse on children and child development, attachment difficulties and high level health risk taking behavior. Children have a named LAC nurse who follows the child irrespective of placement and children who are excluded from education or have left school are offered a consistent service up to 18 years.
Model 2 - Lead Nurse for Looked After Children
NHS Boards have a Lead Nurse for looked after children (Band 7 or 8) who provides professional leadership within the NHS Board structure for staff caring for looked after children. The role of the Lead Nurse centres on ensuring improvement of outcomes and delivery of legal and CEL 16 (2009) requirements within universal services. The role manages a system wide process which ensures health professionals (across all disciplines associated with the child), are active, accountable and responsible for delivery of care as the child moves across placement. The role also includes up skilling, training and support of staff in universal services, clinical supervision and governance of staff with looked after children on their case load, Quality Assurance of health assessments, input to the multi-agency plan, working at a leadership level within the NHS Board, with systems in place to support staff in universal services support looked after children. In terms of competencies of the workforce, the Lead Nurse needs specialist skills, however the role is principally professional lead with the driver to improve the skills in the universal workforce in respect of looked after children.
Future Models
There are advantages and disadvantages associated with both current models described but currently both lack a robust evaluation or research base. Although future team compositions are likely to continue to vary across Health Boards due to differing levels of need, it is essential nursing staff are able to evidence competency and job descriptions should state the range of duties related to the role. Examples of current role descriptions are attached at Annex B.
Implications for Nursing Resource
As set out in CEL 16 (2009) the health needs of all looked after children should be assessed within 4 weeks of notification by the local authority or evidence exists that a health assessment has taken place within the previous three months.
The review by CNOPPP recommended that, despite the need for locality responsive models, it is essential that a consistent approach is taken nationally to roles, support and supervision of nursing resource, and expected levels of service provision. The following good practice is required:
- Universal services should be provided to all looked after children 0-19 years as set out in Hall 4 and according to additional HV/SN guidance (currently under development).
- Assessments should be undertaken regularly by HV/SN in line with GIRFEC and HPIs allocated accordingly, based on individual needs.
- Each Health Board should have a named designated lead nurse for LAC and or ANP with appropriate knowledge and skills to ensure appropriate leadership and governance and to assist nominated Board Directors fulfil responsibilities in accordance with CEL 16 (2009).
- Looked after children aged 5-19 should be frequently assessed by SNs and or LAC Health Care Teams according to local needs, models and requirements.
- Looked after children may require additional specialist assessments. These may be carried out by LAC Specialist Nurses, LAC Teams and or universal services (supervised by LAC specialist nurses) depending on local delivery models.
- LAC Teams and Specialist Nurses should provide specialist and additional support, assessment and intervention as required. They should provide a key leadership role for universal services which includes training, education, supervision and quality monitoring.
- National nursing guidance for looked after children should be re‑assessed and/or developed which standardises roles, appropriate knowledge, skills and competencies required.
- LAC Nurses job titles should be standardised and job descriptions should be precise and transparent.
- In areas where numbers of looked after children are high, Boards may benefit from specialist LAC nursing teams.
- LAC Teams and Specialist Nurses should ensure practice, professional and/or managerial links with universal services, nursing and child protection services and structures and/or LAC nursing services should be supported and line managed through a nursing structure within children/community services
- On-going professional clinical supervision, support and professional development are essential for the LAC Nurse, when providing a service to this highly vulnerable child population.
- Consideration at Board level needs to be given to expected levels of input from universal services for looked after children if this is in addition to the core programmes. It is well recognised that Health Visitors due to more structured contact with families often have a more established relationship with parents, children and or foster carers. For school age children, this is more challenging due to children from the same placement attending different schools, SN caseload size and a possible lack of relationship with the child or placement. It may be that for children of school age, health needs are co-ordinated by a specialist nursing team, due to care placement complexity and levels of vulnerability of the child.
Medical Workforce
The Medical Workforce delivering clinical assessments of looked after children has historically been based in Community Child Health (CCH) services, with little uniformity across Scotland in sizes of medical teams, and no matching of medical resource against population need. In addition, demands for statutory provisions of medical advisers to adoption and fostering panels has far outweighed supply of a new generation of doctors. There is a national shortage of paediatricians training in CCH, and even fewer applying for consultant posts, leaving Consultant Paediatricians being appointed with competing demands between acute paediatric services and community based services including looked after children.
In 2013 there were 45 doctors working within looked after children's services across 14 Health Boards and liaising with 32 Local Authorities. The extent of each doctor's involvement with looked after children, those moving towards permanence, adults wishing to care for all these children varies on an individual basis. The Adoption Act (2007) states a legal requirement to have a Medical Adviser appointed to each adoption, permanence or fostering panel. Although it is not a requirement for them to attend fostering panels there is a considerable workload in evaluating the health assessment of looked after children so that all the relevant medical information is available for the other panel members in a timeous fashion.
Medical Workforce resource
Whilst developing this guidance, an informal audit of the present medical workforce roles and responsibilities was carried out. It is apparent that the vast majority of medical staff, if not all, were unable to fit their current workload into agreed job plans. Nearly all require to read the detailed, extensive paperwork for panels at home, in their own time in order to complete this before panels take place. As local authorities have increased the number of LAC permanence panels, the workforce is struggling to meet the demand for medical reports.
| LAC stats | Consultant | Assoc. Spec. | Specialty Dr | GP/GPS |
|---|---|---|---|---|
| Total number | 9 | 21 | 10 | 5 |
| Total PAs (WTE) | 11 (1.1) | 24 (2.4 ) | 9 ( 0.9) | 4.5 (0.45) |
Total PA's for clinical assessments = 48.5 ( WTE 4.85)
Total PA's for Panel work = 46.5 ( WTE 4.65 )
Several of these paediatricians are due to retire leaving significant gaps in service. The specialist nature of these jobs necessitates specific training and experience to fulfil these positions. Although some roles could be filled by GPs with a special interest, they require training and supervision to deliver their responsibilities adequately.
The fourth edition of Health for All Children estimated that a Health Board covering a population of 100,000 would provide about 50 comprehensive assessments and 100 health reviews per year. It suggests that a comprehensive assessment report takes on average 6 hours. For workforce calcuations, they suggest:
- 2 notional half-days per week of medical time for comprehensive assessments
- One FTE designated nurse (H Grade) to undertake and coordinate health reviews
- One session per week for the designated doctor
- Administrative and data management support
However, medical skill mix has been used creatively with specialty doctors, consultants and GPs with special interests participating on provision of services.
In addition most Health Boards have appointed a Lead Paediatrician for LAC, mainly Associate Specialists with a few Consultants but in some areas, the strategic lead is providing direct clinical care to looked after children.
Implication For Medical Resource
- New Consultant job descriptions need to be explicit about the tasks that require specific competencies, to deliver medical assessments of looked after children. BAAF and RCPCH (should) have detailed job descriptions of these roles.
- LAC health teams should consider skill mix across specialist medical and nursing CCH teams, to deliver the tasks that require specialist competencies.
- LAC Executive Director at Board level should engage with local authorities at the earliest opportunity, through the Integrated Service's Plans, and Single Outcome Agreement, to detail the investments in medical and nursing resource needed to increase capacity to deliver timeous reports for the Permanence and Adoption Panels.
- Board Workforce Planners should participate in a workforce exercise across health and social care, to deliver robust medical and nursing resource to meet the CEL16 requirements.
Contact
Email: Carolyn Younie