Guidance on Health Assessments for Looked After Children in Scotland
This guidance has been produced to assist those involved in carrying out health assessments of our looked after children and young people. It sets out the minimum standardised elements of a health care pathway which we would expect Boards to implement in collaboration with local authorities and other organisations.
Section 2: Health Outcomes in Looked After Children
Evidence from research and practice[1] shows that looked after children and care leavers are more likely to experience health problems than young people in the general population.
A number of studies have identified that the mental health problems for looked after children and young people are markedly greater than that of their peers in the community. The prevalence of speech and language problems is above average, as are issues with co-ordination, eyes and sight. Oral and foot health can be poor, and across all age groups the number of looked after children identifying themselves as regular smokers and consumers of alcohol is significantly higher than the average.
It is estimated that a quarter of young women leaving care are pregnant or have a child and that the numbers of young women who give birth increases within 18-24 months of leaving care.
Looked after children experience a greater number of moves than children in the general population. Moving between different homes or units can mean that health problems get overlooked. Moves may involve changing health board areas, resulting in appointments being changed, missed, delayed or cancelled. Changes in placements can also result in changes in schools and this, together with higher truancy rates, can mean looked after children miss out on universal school health services and health promotion initiatives within school.
The disruption of children's attachments caused by multiple placements can have a negative impact on long-term outcomes.
Research informs us that a child's first attachments are vitally important. Children whose needs have been met in a sensitive, loving and timely way by their primary carer have a sense of trust and confidence in themselves. Securely attached children do better at school and these early attachments help them to form close relationships later in life. They grow up knowing that when they need something, someone will help them. Children whose early experiences of attachment have been less optimal can have insecure or disorganised attachments. These children will potentially be more vulnerable with respect to coping with future relationships and life events.
Secure, organised attachments are associated with the development of effective physiological regulatory systems and better physical and mental health outcomes across the life cycle. Children with disorganised attachments are more likely to have a developmental trajectory associated with anti-social behaviour and violence. They are more likely to require disproportionate levels of health care themselves and in some cases their behaviour to others may result in physical or emotional injury.
Fetal Alcohol Spectrum Disorder
Because many looked after children will have come into care because of parental drug and alcohol use, it is important that family history is well documented, and a clear understanding of the effects of alcohol on the developing foetus and the child is appreciated by all health and care workers.
Fetal Alcohol Spectrum Disorder (FASD) is the leading known preventable cause of permanent learning disability worldwide and is caused by maternal use of alcohol during pregnancy. Affected children can have a wide range of physical, growth and neurobehavioural problems which impact on their everyday lives and limit their independence.
Fetal alcohol spectrum disorders are permanent lifelong developmental disabilities caused by maternal use of alcohol during pregnancy. Alcohol consumption in Scotland is high, but recognition of children affected by fetal alcohol harm in the UK is poor, much lower than in other parts of the world.
Young women in care should also be made aware of the dangers of drinking in pregnancy. Pre-conception and pregnancy are arguably the earliest stages at which services can work effectively together to offer guidance and support to families at risk from substance misuse issues. Women do not need to be alcohol dependent to have a child with FASD, although it is much more common in children of dependent women, and alcohol use is often a co‑occurrent substance use with drug problems. Since the brain of the foetus develops throughout the duration of pregnancy, it can be damaged at any time during pregnancy.
Health for All Children 4 (Hall 4)
Where a child is Looked After, they should receive the full core/universal programme of screening, surveillance and health promotion as set out by Hall 4 in addition to any specialist health assessment required.
Hall 4 is the programme of screening, surveillance and health promotion contacts which every child in Scotland should receive.
The Hall 4 guidance introduced a tiered programme of support and intervention for those children who are vulnerable or are considered to be at risk, empowering health visitors and school nurses to assess the level of support and intervention required according to assessed need. The guidance expects health professionals to work closely with other agencies and services, in particular childcare and early education to build on existing contacts with children and families. Looked after children should have access to the full range of health services, including General Practitioner (GP), health visiting/school nurse, child and adolescent mental health, speech and language therapy, audiology, vision, health promotion, oral health, specialist, and sexual health services. All Hall 4 contacts will result in data being recorded about a child's looked after status on the National Child Health Surveillance Programme.
A New Look at Hall 4, launched by the Scottish Government in January 2011, set out the way forward for the successful delivery of Hall 4 in the Early Years. It supplements the 2005 guidance and addresses key issues identified as requiring further clarification. In line with GIRFEC, it recommends the Health Visitor should be the Named Person for the 0-5 age group or until the child enters school, to act as the first point of contact for children and families.
From April 2013, a new review at age 27-30 months has been introduced to the universal core programme of contacts. This review covers issues such as child development (including social, emotional and behavioural, speech and language, and gross and fine motor skills), nutrition and growth, physical health, home learning environment, early learning and childcare as well as parental health (all those in a parenting role, including foster parents and other carers).
Dental Health
Childsmile is a national programme designed to improve the oral health of children in Scotland and reduce inequalities both in dental health and access to dental services. The programme combines targeted and universal approaches to tackling children's oral health improvement. This combination provides a comprehensive pathway of care that is tailored to the needs of individual children.
At a population level, every child will have access to:
- A tailored programme of care within Primary Care Dental Services.
- Free daily supervised toothbrushing in nursery.
- Free dental packs to support toothbrushing at home.
Directed support targeting children and families in greatest need through:
- Additional home support and community interventions.
- An enhanced programme of care within Primary Care Dental Services.
- Clinical preventive programmes in priority nursery and primary schools and facilitation into dental services as appropriate.
- Daily supervised toothbrushing in P1 to P2 of priority schools.
Health Promotion
Health promotion is the process of enabling people to increase control over and improve their health through evidence-informed action within health education, protection and prevention. Health professionals play a lead role in health promotion through a range of action such as screening, immunisation, health education, signposting, behaviour change, and promoting healthy lifestyles. Health promotion acknowledges the wide range of factors which influence health and wellbeing. It extends beyond the individual to include the wider social and physical environments which influence health and wellbeing.
Adopting a multi-agency approach encourages health professionals to liaise with a wide range of partners such as education, social care and the Third Sector. These partners are in a strong position to support behaviour change, reinforce health promotion messages and influence the social, emotional, physical and organisational environments within which people live their life. As such, they have a supporting role to play in responding to health promotion activity identified as part of a comprehensive health needs assessment for looked after children.
Mental & Emotional Health
There are a number of factors which may impact on a looked after child's mental health including: the child's experience in terms of poor parenting, trauma, bereavement or serious illness, mental health difficulties in one or both parents, and the impact on the child of the environment such as poor neighbourhoods, deprivation, social exclusion and poverty.
Additional factors can include stability and quality of care, and the child's links to family, friends and peers.
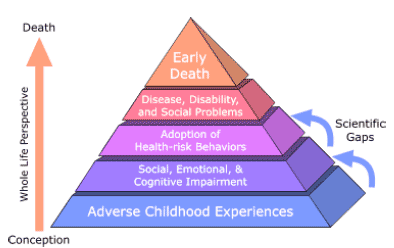
Source: Centers for Disease Control and Prevention
The Mental Health of Young People Looked After by Local Authorities in Scotland (2004) found that among young people (n=242), aged 5-17 years, looked after by local authorities, following assessment:
- 45% were diagnosed with a mental disorder
- 38% had clinically significant conduct disorders
- 16% were assessed as having emotional disorders - anxiety and depression
- 10% were rates as hyperactive
It is recommended that looked after children are screened for emotional and mental health difficulties using Goodman's Strengths and Difficulties Questionnaire (SDQ). This can be easily used by the professional carrying out the health assessment and can be scored using online programmes. The form can be discussed as part of the assessment or completed by the young person as they wait for their appointment.
While it is important to pick up any formal 'mental disorder' amongst these children, arguably a more important task is to respond appropriately to the emotional distress that they experience. Understanding that distress in the contents of attachment processes is quite a challenge, but one that health professionals should try to respond to.
The SDQ is weighted towards externalising difficulties like ADHD and behavioural problems and tends to be less useful for picking up internalising problems such as anxiety, depression or attachment difficulties. To address this, additional questions should be added to capture more information about internalising difficulties.
Where the tools is being used for younger children, questions about attachment should be included.
If further specialist services are required, consultation should be provided by CAMHS for any concerns raised during the health assessment and mental health screening, or if there is uncertainty around results. Where children are thought to have significant emotional and/or mental health difficulties, they should always be referred to a specialist service for full assessment.
It is worth remembering that CAMHS services are specialist children's services and that access to clinical psychology, educational psychology, primary care mental health workers and voluntary agencies may be more useful to support looked after children.
Contact
Email: Carolyn Younie