Growing Up in Scotland: Birth Cohort 2. Results from the First Year
This Growing up in Scotland report provides a detailed insight into the first set of data collected from the study’s second birth cohort – representative of all children born in Scotland between 1st March 2010 and 28th February 2011 – around the time they were all aged 10 months old.
Chapter 4 Infant feeding
Pamela Warner and Katherine Smith, Centre for Research on Families and Relationships
4.1 Background
Almost all of the children in birth cohort 2 (BC2) had been born by January 2011 when the Scottish Government published Improving Maternal and Infant Nutrition: A Framework for Action (Scottish Government, 2011). However, this framework was based on evidence that was already in the public domain and aimed to support and promote strategies to improve infant feeding in the population. Many of these strategies would have been developed or piloted in the preceding 12 months, when the babies were being born. The framework was influenced by the UNICEF UK Baby Friendly Initiative which, in 2009, when publishing a strategy for improving breastfeeding outcomes, noted that "although the World Health Organization (WHO) and the Department of Health recommend that all babies are exclusively breastfed for the first six months, the rate of exclusive breastfeeding at six months in the UK is less than 2 per cent" (UNICEF UK, 2009).
The rationale for the infant feeding part of the framework is that "the feeding received by the infant in the first few months of life, the process of weaning onto solid foods and the diet and nutrition status of the growing infant all contribute significantly to the long term health of the population" (Scottish Government, 2011). The framework recognises the detrimental effect of health inequalities on infant nutrition and recommends targeted support to those most in need, with the aim of optimising health outcomes for children and reducing the gap between the most and least healthy.
Infant feeding guidance focuses on two main areas: breastfeeding and weaning (or the introduction of solid foods). With respect to breastfeeding, the first aim is to maximise rates of breastfeeding initiation, and the second is to optimise duration of exclusive breastfeeding, if possible until at least six months of age, as per the recommendations of the WHO systematic review (Kramer et al. 2002). In this context, 'exclusive' breastfeeding is defined
as breast milk only, with no other liquid or solid foods[10]. With respect to introduction of solid foods, whether exclusively breastfed, formula fed or mixed, the aim is to delay solids until six months of age (Kramer et al. 2002; NHS Health Scotland, 2011), but also to ensure children receive a variety of foods and textures at an age appropriate to their developmental stage (NHS Health Scotland, 2011).
4.1.1 Breastfeeding: initiation, duration, and information provision
2004-2005 policy context - relevant to the first birth cohort (BC1)
Infant nutrition policy in Scotland developed considerably following the Scottish Joint Breastfeeding Initiative in 1990 (Scottish Office, 1993) culminating with the Breastfeeding etc. (Scotland) Act (2005), while more recent public policy has continued to promote breastfeeding in Scotland (Scottish Government, 2008, 2011). In the decade preceding the birth of the first birth cohort (BC1), the Scottish Government worked on national targets to raise breastfeeding rates among mothers in Scotland. While no specific target was set with regard to breastfeeding take-up (ie. mothers who breastfeed at least once), in 1994 a national target was set to increase the proportion of mothers who were still breastfeeding at six weeks from 30% to 50% by 2005 (Scottish Executive, 2000).
A National Breastfeeding Adviser was appointed in 1995 to provide training resources and advice and assist NHS Boards in meeting targets. The Scottish Breastfeeding Group was also launched in 1995 which provided a national resource of information and advice about breastfeeding and set up a website providing information for mothers (NHS Health Development Agency, 2003). In subsequent years, NHSScotland also worked to implement the joint WHO/UNICEF initiative on breastfeeding and raise awareness of breastfeeding benefits by promoting support groups set up by professionals and peers (Scottish Executive, 2000). Subsequently, the Integrated Strategy for Early Years focused on improving service provision, particularly for vulnerable children aged 0-5 and their families, and increasing the proportion of women breastfeeding (Scottish Executive, 2004). By 2004, Scotland had the highest level of participation in the UNICEF UK Baby Friendly Initiative of any UK country (more than 85%), and there were nine breastfeeding peer support programmes across Scotland and 150 breastfeeding support groups. The Ready Steady Baby booklet was also launched in 1998 as an all-inclusive booklet with breastfeeding information for parents.
2010-2011 policy context
In the years preceding the birth of children in the second birth cohort (BC2), there was some policy change related to breastfeeding. In 2007 and 2008, new HEAT targets were aimed at increasing the proportion of infants being exclusively breastfed at 6-8 weeks from 26.2% in 2006-2007 to 32.7% in 2010-11 (Scottish Government, 2007; 2008). This represented a move from the previous mixed (breast and formula) feeding targets, towards exclusive breastfeeding and reflected the WHO recommendations on exclusive breastfeeding, albeit for six months. Whilst the Scottish Government endorsed the WHO guidelines (Scottish Intercollegiate Guidelines Network and NHS Quality Improvement Scotland, 2010), the working target itself focused on exclusive breastfeeding at 6-8 weeks (NHS Health Scotland, 2011).
In support of the revised breastfeeding targets, an Infant Nutrition Co-ordinator was appointed in 2008 to lead the development and the implementation of the Maternal and Infant Nutrition Strategy. This strategy was aimed at improving the nutrition of pregnant mothers and their infants (Scottish Government, 2008). In 2010, the Maternal and Early Years website was launched to provide accessible and updated information to early years professionals, on topics including breastfeeding (http://www.maternal-and-early-years.org.uk/topic/background).
Significant funding allocations by the Scottish Government to encourage breastfeeding (and other measures to improve maternal and infant nutrition) between 2008-2011 were made following the publication of CEL 36 (Nutrition of Women of Childbearing Age, Pregnant Women and Children under 5 in Disadvantaged Areas). Breastfeeding was a key priority for implementation, and Health Boards were encouraged to use a proportion of their allocation to assist with progress towards achieving the breastfeeding HEAT target. Emphasis was also placed upon the connected Equally Well recommendation that NHS Boards should improve breastfeeding rates in deprived areas and among disadvantaged groups.
Change between the two cohorts
The box below highlights changes in breastfeeding targets between BC1 and BC2. Duration of exclusive breastfeeding was not assessed for BC1, so the two cohorts can not be compared in this respect. However, if the extensive promotion of breastfeeding prior to, and at the time of, the births of children in BC2 has resulted in behaviour change then we would expect to see an increase in rates of breastfeeding initiation and of continuation to six weeks and six months.
Relevant breastfeeding policy targets for BC1 and BC2
| BC1 | BC2 | |
|---|---|---|
| Percentage breastfeeding at all at six weeks | 50 | |
| Percentage breastfeeding exclusively at six weeks | 33 | |
| Percentage breastfeeding exclusively to six months | No target |
Breastfeeding promotion initiatives gained momentum between 1995 and 2005, but since then (and hence the context for BC2), breastfeeding promotion has largely built on existing initiatives. It is expected that the breastfeeding support networks that have evolved may mean the mothers of BC2 will feel they had access to and used more breastfeeding resources than mothers of BC1.
4.1.2 Timing of weaning and drinks
2004-2005 policy context: BC1
In the years running up to the birth of BC1, the guidelines on weaning recommended that parents introduce solids at four to six months (Scottish Intercollegiate Guidelines Network (SIGN), 2003; Scottish Executive, 2005). Since 1996, sugar has been discouraged for infants (Scottish Office Dept. of Health, 1996), and in 2002 it was recommended that parents should avoid sugary juice in babies' bottles (Scottish Executive - Dept. of Health and NHS Scotland, 2002). While in 2003, the only drink recommended for children aged under 2 years was full-fat milk (SIGN, 2003).
2010-2011 policy context: BC2
Recommendations for the introduction of solid foods changed in the years preceding the birth of children in BC2. From 2006 to 2010, revised guidelines recommended that the introduction of solids should be avoided until six months, for both breastfed and formula fed children (NHS Health Scotland, 2006; SIGN and NHS Quality Improvement Scotland, 2010). More recent advice for mothers allows for a little more flexibility, with weaning recommended at 'around six months', but still with a clear recommendation that babies need nothing more than milk until six months of age, and advising mothers wishing to wean earlier to avoid certain foods (NHS Health Scotland, 2011). However, as children in BC2 were born between March 2010 and February 2011 and this version of weaning advice was first disseminated in July 2011, most of the cohort would have already been six months of age or older by the point of its release.
With regards to drinks other than breast or formula milk, advice from 2006 suggested that children aged under 2 years should not be offered sweetened drinks and that fresh unsweetened fruit juice should be offered only at meal times (Scottish Executive, 2006). More recent guidance, from 2011, recommends that, in order to protect teeth, fruit juice should be offered only at meal times and should also be diluted with water (NHS Health Scotland, 2011). Milk and plain water were recommended as suitable drinks throughout the day and between meals, although cows' milk, as a main drink, is not suitable for babies under one year old.
Change across the time between the two cohorts
The box below shows changes in weaning guidance between BC1 and BC2. If these changes in guidance have changed behaviours, then we may expect to see, in BC2, a reduction in weaning prior to six months and a fall in consumption of natural, undiluted fruit juice, compared with BC1.
Changes in weaning guidance between BC1 and BC2
| BC1 | BC2 | |
|---|---|---|
| Age for weaning | 4 to 6 months | 6+ months |
| Giving child natural fruit juice | None | Restricted to mealtimes and should be diluted |
4.1.3 Receipt of Healthy Start Vouchers
The Healthy Start scheme was launched in November 2006, replacing the longstanding Welfare Food Scheme. Healthy Start is a UK-wide Government scheme to improve the health of low-income, pregnant women and families. The scheme targets women and children aged under 4 in families who receive certain benefits and tax credits and all mothers under 18 years of age. At introduction, Healthy Start vouchers could be exchanged in participating shops for fresh milk, fresh fruit and vegetables, vitamins and infant formula milk (but only formula labelled 'suitable from birth'). In 2008, the government expanded the range of foods which could be purchased with vouchers to include plain frozen fruit and vegetables (Scottish Government, 2008).
If the Healthy Start scheme has improved nutrition then we would expect children in families who are entitled to the scheme to have an improved diet in terms of more milk, fruits and vegetables. However, this outcome can not be assessed by means of BC2 sweep 1 data, not least because of the very young age of the children and their limited diet, consisting of significant quantities of milk, over the reference period. As the children age, and with future data collection, it may be possible to consider whether receipt of Healthy Start vouchers has had such an influence.
4.2 Aims and methods
This chapter provides a detailed description of the infant feeding experiences of children born in 2010/11 (BC2) and, where possible, compares this to experiences of children born
in 2004/05 (BC1).
For BC2, these experiences are described in relation to:
- breastfeeding initiation
- breastfeeding at all for six or more weeks
- exclusive breastfeeding for six or more weeks
- exclusive breastfeeding for at least six months and
- age at introduction of solids
Some examination of take up and use of Healthy Start vouchers is also included. However, this analysis does not permit an assessment of impact of these vouchers on nutrition. Unless otherwise stated, the data refer to BC2.
For BC1, there was no assessment of exclusive breastfeeding, so the two cohorts will be compared on their rates of: breastfeeding initiation, breastfeeding at all for six or more weeks, breastfeeding at all for six or more months, and age at introduction of solids.
There are a number of methodological issues that should be borne in mind when reflecting on the results reported here. The most crucial is the need for the respondent to have recalled details of events that occurred three to 11 months in the past. This is because the data collection interview with the child's main carer took place when the child was approximately 10 months old. While the fact of breastfeeding at all, or not, is likely to be well recalled, the features of infant feeding that are of particular interest (age at stopping breastfeeding, age at introducing solids) are likely to be considerably more prone to recall error.
There are other methodological issues which have been summarised in Appendix B. One
of these is related to differences in how age at starting solid food was recorded for BC1 (months) and BC2 (weeks). This raised two methodological concerns: whether mothers recall the timing of events in mid-first-year of their baby's life as precisely as in weeks as they do in months; and if they remember in months, how well they manage the conversion into weeks. BC2 'weeks' had to be converted into 'months' to assess results against recommendations, and also to compare ages at introduction of solids between cohorts.
As explained in the appendix (section 2), and shown in Table 1.1, two different methods
of converting weeks to months were applied to the BC2 data to allow these comparisons.
Table 4.1 Age group at starting solids - two versions of converting 'weeks' to 'months' for BC2 data
| Coding version | Before 4 months |
4 months |
5 months |
6 months |
7 months or older | |
|---|---|---|---|---|---|---|
| Months (as in BC1) |
<= 3 | 4 | 5 | 6 | >= 7 | |
| 'At least' | BC2 - weeks | <= 16 | 17 to 20 | 21 to 25 | 26 to 29 | >= 30 |
| 'Mid' | BC2 - weeks | <=14 | 15 to 18 | 19 to 23 | 24 to 27 | >= 28 |
4.3 Key findings
- 36% of children were exclusively breastfed for six or more weeks and 11% until six months or more.
- Breastfeeding outcomes are strongly associated with multiple socio-demographic factors.
- The proportion of children who were breastfed at all (but not necessarily exclusively) for six weeks or more was unchanged between BC1 and BC2 (42%). However, after controlling for socio-demographic factors, the rate was actually found to be lower in BC2.
- 42% of parents delayed introduction of solids until 21 weeks (five months) and 14% delayed until 26 weeks (six months).
- Introduction of solids at six months was more likely amongst parents who had breastfed for at least six weeks, and even more amongst those who continued breastfeeding to six months.
- 75% of mothers recalled having received breastfeeding advice 'at the time of birth' from any source. It is possible mothers also received such advice outside of the period they defined as 'at the time of birth'.
- Initiation of breastfeeding was higher amongst those mothers who recalled receiving breastfeeding advice, from any source, 'at the time of birth', but particularly amongst those who recalled receiving advice from a midwife.
- Among those who had initiated breastfeeding, recall of breastfeeding advice from a health visitor or other health professional was associated with continuation of breastfeeding to six weeks or more.
4.4 Breastfeeding
4.4.1 Description of infant feeding of birth cohort 2
Breastfeeding outcomes
Table 4.2 shows the breastfeeding outcomes for birth cohort 2. The percentage of mothers initiating breastfeeding is 63%, but only about two-thirds of those initiating are still breastfeeding at six weeks (42% of all mothers), and even fewer are breastfeeding exclusively at that point (36%). However, this rate does exceed the target figure of 32.7%. Figure 4.1 shows, by milestones in cohort children's ages, the percentages of mothers continuing with breastfeeding at all (indicated by the symbol 'x'), and who were still breastfeeding exclusively (indicated by the symbol ' ').
').
Table 4.2 Breastfeeding outcomes for BC2
| % | Base: all families | |
|---|---|---|
| Child was breastfed at all | 63 | 6108 |
| Child was breastfed for >= 6 weeks | 42 | 6026 |
| Child was breastfed exclusively for >= 6 weeks | 36 | 5994 |
| Child was breastfed for >= 6 months | 25 | 6026 |
| Child was breastfed exclusively for >= 6 months | 11 | 5994 |
This graph shows that the early decrease in breastfeeding happens mainly in the first
two weeks postnatally. It also shows that the exclusive breastfeeding rate begins to fall more sharply after 17 weeks of age (four months). By six months of age only 25% of babies are breastfed at all, and fewer than half of these are exclusively breastfed (11%).
Figure 4.1 Percentage of BC2 still breastfeeding (BF) - 'any' or 'exclusively' - at selected milestones in terms of child's age (in weeks since birth)
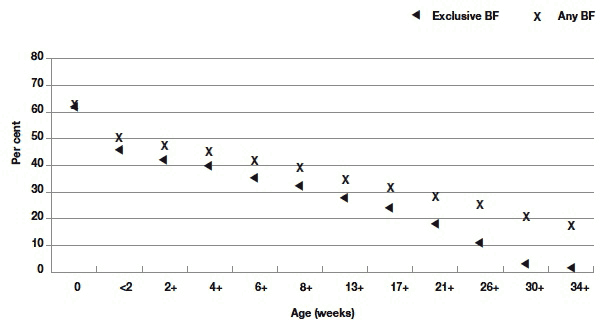
Base - all families where mother was in household: exclusive BF = 5882, any BF = 5983
Reasons given for choosing not to breastfeed, or for stopping
Table 4.3 lists reasons given by mothers for choosing not to breastfeed. Personal preference or past bad experience are the most commonly cited reasons, but the largest group of all is 'other' which represents complex mixture of additional personal and specific reasons (33%).
Table 4.3 Reasons for not breastfeeding
| Reason | % of those who gave one or more reasons |
|---|---|
| I didn't want to | 29 |
| Previous bad experience | 12 |
| Embarrassed/not comfortable | 7 |
| Thought bottle feed better | 6 |
| Baby didn't want to/couldn't | 6 |
| I was ill | 5 |
| Not enough milk | 4 |
| Inconvenience/fatigue | 3 |
| Problem with technique | 3 |
| Sore nipples etc | 1 |
| Lack of information/support | 1 |
| Wanted to drink/smoke/had poor diet | 1 |
| Health professional advised not to | 1 |
| Partner/father did not want me to | <0 |
| Other | 33 |
| Base: all who did not breastfeed | 2351 |
Table 4.4 below gives reasons cited for stopping breastfeeding for those in BC2 who had initiated breastfeeding but had stopped prior to the interview (83% of those who initiated breastfeeding). Reasons are given at an overall level and subdivided according to whether at least six weeks breastfeeding was achieved (rightmost two columns).
The most common reason given overall was 'other', followed by 'not enough milk' (31% each). The table is ordered so the reasons more often given if stopping after six weeks are in the first set, with the rest given in the second set.
Table 4.4 Reasons for stopping breastfeeding overall and by whether or not six weeks of breastfeeding was completed, with reasons grouped into three sets
| Reason given | % of all who gave one or more reasons | Breastfed for 6 or more weeks | |
|---|---|---|---|
| No % |
Yes % |
||
| More often given if stopped after 6 weeks | |||
| Other reason | 31 | 13 | 18 |
| Not enough milk | 31 | 13 | 18 |
| Baby not interested | 12 | 3 | 9 |
| Returned to work | 9 | >0 | 8 |
| It was long enough | 6 | 1 | 5 |
| Inconvenience/fatigue | 5 | 2 | 3 |
| Given more or less equally often whether or not stopped before 6 weeks | |||
| Problem with technique | 8 | 6 | 2 |
| Sore nipples | 6 | 4 | 2 |
| Painful | 8 | 4 | 5 |
| I was ill/on medication | 6 | 4 | 3 |
| Health professional advised not to | 1 | 1 | 1 |
| Embarrassment | <1 | <1 | <1 |
| Planned to stop then | <1 | <1 | <1 |
| Wanted to drink alcohol | <1 | 0 | <1 |
| Partner/father wanted me to stop | <1 | 0 | <1 |
| Base: all who had stopped breastfeeding | 3147 | 1241 | 1906 |
Information and advice
Table 4.5 and Table 4.6 summarise the sources mothers recalled receiving breastfeeding advice from, for all mothers, and only those who breastfed, respectively. The question asked was: "Did you receive any help or advice about breastfeeding at the time of (childname's) birth?".
We have assumed that the 'time of childname's birth' has been interpreted broadly by parents. Information about breastfeeding and decision-making is needed both before birth - to inform feeding intentions and, whatever the decision, to make practical preparations - and following the birth. In addition, given the way pregnancy and birth services are organised, relatively few new mothers will see a health visitor until about 10 days after birth. Yet a 'health visitor advice' option was included and the percentage of women recalling advice from a health visitor was fairly high for 'at time of birth' (25%). Since there are no other questions about receipt of advice, we assume that the period in question covers both antenatal advice immediately prior to the birth and advice given in the early weeks, once breastfeeding is attempted.
Table 4.5 Advice received about breastfeeding - all mothers
| Source of BF advice 'at time of birth' | % recalling advice from this source | ||
|---|---|---|---|
| All | Separately by whether breastfed at all | ||
| % of Yes | % of No | ||
| Any | 75 | 85 | 60 |
| Midwife | 65 | 71 | 53 |
| Health visitor | 25 | 32 | 14 |
| Other health professional | 14 | 18 | 8 |
| Getting Off to a good start leaflet | 7 | 8 | 5 |
| Bases: All cases where mother was in household | 5987 | 3759 | 2217 |
Among all women, 75% recalled receiving advice about breastfeeding from any source 'at the time of birth' and 65% recalled having received advice from a midwife.
In general, midwives would have earlier, individual opportunities (that is, earlier than the time of birth) to raise the issue of breastfeeding with a pregnant woman, but it is unclear whether respondents considered such provision of advice as falling under the remit of the 'at the time of birth' question asked. Often the main way breastfeeding information is given is during antenatal classes (as a group) and it is uncertain whether women know the class leader is a midwife (if she is), or whether they see information gleaned in antenatal classes as 'receiving help or advice from a midwife', in the sense that the question asks.
However, there was a positive association for recall of advice from a midwife and attending antenatal classes, with 77%, 68% and 58% recalling such a source of advice if attending all, some or no antenatal classes. For those having a second or later baby, a midwife might not proffer advice if it was documented the mother had breastfed successfully before. Certainly, for all mothers, recall of advice was greater amongst those having first babies, particularly for 'any' advice (83% compared with 68%) and advice from a midwife (71% compared with 59%), but also for advice from a health visitor (28% compared with 24%) or other health professional (19% compared with 10%). For those who answered specifically for 'at the time of birth', it might have been documented already in a woman's notes that she has rejected the idea of breastfeeding at a prior discussion, which could account for some omissions to raise the issue of breastfeeding at the time of birth. Alternatively, it might seem tactless if the birth has been exhausting or difficult.
Significantly more women who initiated breastfeeding than those who did not, recall receiving any breastfeeding advice (85% compared with 60%). Differences are also evident in relation to advice from a midwife or health visitor, or other health professional. Very few? mothers recall receiving advice via the Getting Off to a good start leaflet (7%), and only marginally more of those who started breastfeeding, compared with those who did not, recall the leaflet as a source of advice about breastfeeding (8%).
As discussed above, it does not seem that responses to this question were restricted to
'at time of birth', so temporally it is not possible to establish which source(s) cited were associated with the decision to breastfeed, and which supported successful continuation.
It should be borne in mind that there is the possibility of some recall bias, in that receipt of advice has little chance of being recalled at later interview, unless it has some salience to a woman. That is, the advice might be readily forgotten if breastfeeding is unappealing and out of the question (women falling into the 'did not initiate breastfeeding' sub-group), or if the woman is not a first time mother and does not need to recall advice because she has succeeded before in breastfeeding. Certainly the association between recall of advice and initiating breastfeeding was significantly stronger among first time mothers than women having a later pregnancy (results not shown). So some of the apparent difference between those initiating or not could be recall bias. With regard to the association with antenatal classes, there is some possibility of confounding, in that first-time mothers, and perhaps particularly those who (already) have aspirations to breastfeed, are more likely to attend antenatal classes than mothers who already have children.
Table 4.6 presents, for all BC2 women who breastfed, the sources of advice they recalled having received about breastfeeding, overall (which repeats some data from Table 4.5) and subdivided according to whether they ultimately went on to breastfeed for at least six weeks.
Here, there was little relationship between having received 'any' advice and succeeding in breastfeeding to six weeks, with the difference being - if anything - in the reverse direction to that which may be expected. That is, six weeks breastfeeding was lower for those receiving 'any' advice than for those not recalling receipt of advice (83% compared with 88%). There was a similar trend for advice from midwives specifically. However, there was
a difference in the expected direction for recall of advice received from a health visitor, and other health professional.
Again, the possibility of recall bias needs to be considered, and 'reverse causation', such that if one is determined to succeed in breastfeeding past six weeks, then one might be both more likely to attend more carefully to advice given (and make a point of recalling it
so that it can be implemented) and be more likely to achieve this goal.
Table 4.6 Advice received about breastfeeding - mothers who initiated breastfeeding
| Overall % of BC2 who ever breastfed | Separately by whether BF for 6 weeks or more |
||
|---|---|---|---|
| Yes % |
No % |
||
| Any | 85 | 83 | 88 |
| Midwife | 71 | 70 | 74 |
| Health visitor | 32 | 29 | 8 |
| Other health professional | 18 | 15 | 7 |
| Getting Off to a good start leaflet | 8 | 8 | 2 |
| NCT or other voluntary group/organisation | 7 | 5 | 1 |
| Bases | 3769 | 2443 | 1278 |
Association of 'exclusive breastfeeding' to six weeks with socio-demographic factors
Table 4.7 summarises findings from a multivariate logistic regression analysis of the association of 'breastfeeding exclusively for six weeks or more' with socio-demographic factors[11]. This shows that exclusive breastfeeding for past six weeks is strongly jointly associated to a number of factors: higher educational qualifications, couple parenthood, minority ethnic group, lower deprivation and maternal age of 20 years or older. After adjustment for these factors there was no association with income or the infant being first born.
Table 4.7 Multivariate associations of breastfeeding exclusively for six weeks or more, with socio-demographic factors*
| Factor | Odds of exclusive BF for >=6 wks: |
|---|---|
| Resp. education | Highest amongst mothers with 'other' or 'higher education' qualifications, lowest if no qualifications |
| Single parent | Higher if living with partner (versus single parent) |
| Ethnic group | Higher amongst mothers from 'other' ethnic group (versus white) |
| SIMD quintile | Higher amongst mothers living in less deprived areas (the least deprived the highest) |
| Maternal age | Higher amongst mothers aged 20 years or older (versus under 20 years) |
| Income** | No association |
| First born | No association |
* Multivariate logistic regression model: p values for 'income' and 'first born' non-significant, for 'maternal age group' = 0.004, and for all other factors <0.001; table arranged in order of strength of association with factor. ('Working now' and urban-rural were excluded after checking they were not statistically significant.)
** Equivalised household income (quintiles)
The analysis reported in Table 4.7 was based on all mothers. However, 'not breastfeeding exclusively for 6 weeks or more' can arise either because there is no breastfeeding ever, or because breastfeeding is started but is not continued exclusively to six weeks, and so the associations estimated will reflect influences at one or both stages. It is therefore of interest to rerun this analysis, selecting only those who breastfed at all, so as to be able to explore associations with respect to proceeding to six weeks, at least, of exclusive breastfeeding, given that breastfeeding has been initiated. For this subset model (not shown), factors no longer associated with continuing exclusive breastfeeding to six weeks given that breastfeeding has been initiated, were age, ethnic group and deprivation. Factors which remained associated, were education and living with a partner. The child not being the mother's first born was also now associated (with continuing to six weeks). This suggests that deprivation, ethnic group and maternal age are primarily associated with the decision to start breastfeeding, in contrast to non-first born status which is associated with succeeding once a breastfeeding decision is made. In contrast, education and having a partner are associated both with the initiation decision and succeeding to six weeks.
4.5 Weaning (starting solid foods) and drinks
When starting solid foods
The median age for starting solids was 20 weeks. 25% of the cohort had started solid foods by one week short of four months of age (16 weeks), 50% by one week short of five months of age (20 weeks) and 75% by two weeks short of six months (24 weeks). In terms of policy guidance, only 14% had waited until six months of age before weaning, but 42% have waited until at least five months of age.
However, there is evidence of 'value preference' - that is, higher proportions of parents selecting 16 weeks, 20 weeks and 24 weeks and much smaller proportions selecting the ages one week either side of these, which is not what one would expect in random 'nature'. As it happens, these values (16, 20 and 24) are the (erroneous) 'age in weeks' one would calculate if converting age at starting solids from months to weeks by multiplying age in months by four, a common error, as discussed in the annex. If we act on this strong impression (that what many of the women who gave these specific responses were recalling was ages of four, five and six months respectively, but then converting inaccurately to weeks), we should for the six months threshold consider responses of 24 weeks (and, logically, 25 weeks too) as also denoting 'at least six months of age'. By that method, 31% of children did not start solids before six months of age.
The box-plots shown in Figure 4.2 demonstrate the wide range of weaning ages (in weeks) reported. Variations are shown by deprivation quintiles and by extent of breastfeeding (three sub-groups: none or very brief, >= six weeks, >= six months). The line and circles represent the full range of ages whilst the box represents the middle 50% of responses, from the lowest 25% to the highest 25%. The middle value (median) is shown by the dark cross bar. The dashed horizontal reference lines show thresholds of six months (bold) and four months (thin).
This graph shows the wide range of reported ages at starting solids, within each sub-group, with a number of babies in all deprivation quintiles starting at 10 weeks or younger, and also a number not starting until seven months (30 weeks) or older. In addition, the position of the boxes shows a relationship between 'extent of breastfeeding' (different coloured 'boxes') and age at starting solids. Within each SIMD quintile, this is seen as a generally lowest median age (thick line across 'box') for 'brief/none', and highest for '>= 6 months'.
Figure 4.2 Box-plots for BC2 of child's age at starting solids (in weeks since birth), by SIMD deprivation quintile and extent of breastfeeding (not weighted)
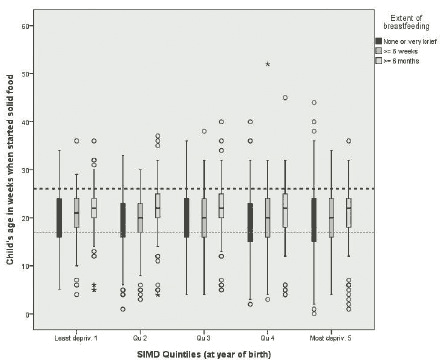
Base - all cases where mother was in household: Most deprived = 1153, Qu4 = 1171, Qu3 = 1267, Qu2 = 1233, Least deprived = 1283
Multivariate logistic regression analysis was undertaken to test for independent relationships between the various factors already considered, and starting solids before five months[12]. After controlling for socio-demographic variables - parental level of education, family type, maternal age, area deprivation and area urban-rural classification - the factors firstborn, household income and ethnicity were not significantly associated with delaying solids until at least five months of age. All the other variables had statistically significant associations despite mutual adjustment for each other (p<=0.001), with higher odds of waiting until five months or older in the case of:
- degree or 'other' education qualifications
- living with a partner
- older maternal age
- less deprived area
- large urban or remote rural area
If the three-group 'extent of breastfeeding variable' (as used in Figure 4.2) was added to the model, this showed by far the strongest association with delaying until five months, with the odds of doing so being increased by 25% (relative to no breastfeeding or very brief) if the baby had been breastfed to at least six weeks, and increased by 150% if breastfed for at least six months. Nevertheless, the socio-demographic variables listed above retained their significant associations, except for living with a partner (probably because its effect had been subsumed into 'extent of breastfeeding', which had been added to the model).
Other drinks apart from milk and formula
At 10 months of age, the vast majority of children drink water or baby/sugar-free fruit juice during the day, as shown in Table 4.8. Once in bed, just under half drink nothing other than water (41%), and a similar proportion do not drink at all in bed (42%), leaving 17% who do have non-water drinks in bed. This proportion is associated with deprivation, ranging from 9% in the least deprived to 23% in the most deprived group.
Table 4.8 What do children have for drinks?
| Drink | % |
|---|---|
| Water | 83 |
| Baby juice | 31 |
| Fruit juice etc (diet/sugar free) | 24 |
| Fruit juice etc (NOT diet/sugar free) | 7 |
| Tea | 5 |
| Only milk or formula | 3 |
| Herbal drinks | 1 |
| Something else | 1 |
| Fizzy/soft drinks | <1 |
| Coffee | <1 |
| Base: all families | 6217 |
It is not possible to assess compliance with the diluted juice recommendation since the necessary questions were not asked at this stage (eg. whether or not drinks taken only at mealtimes, whether natural juice is diluted).
Healthy Start vouchers
Overall 24% of main carers received Healthy Start vouchers. Of those who received vouchers (n=1327), 62% used them to buy fresh fruit and vegetables, 54% bought formula milk and 48% bought ordinary milk. Any other purchases using HSV are not allowed under the scheme, and would constitute fraud. Nevertheless, 7% of respondents reported using the vouchers for ordinary food shopping, 6% for non-food items and 4% other foods. This suggests some misunderstanding of the question, and/or erroneous responses. For example, some mothers may have confused HSV with the Health in Pregnancy grant.
As expected - given that only families on low incomes and in receipt of certain benefits or tax credits are eligible to receive the vouchers - there is a very strong association of receipt of Healthy Start vouchers with area deprivation, ranging from 44% in the most deprived quintile, to 9% in the least deprived quintile.
4.5.1 Comparing breastfeeding and weaning outcomes between cohorts
Breastfeeding outcomes and advice
Table 4.9 shows the breastfeeding outcomes for birth cohorts 1 and 2. Ignoring any socio-demographic changes, the overall percentage of mothers who breastfed has increased marginally from 60% to 63%. The percentages breastfeeding for six weeks or more, and
for six months or more, have remained virtually unchanged.
Table 4.9 Breastfeeding outcomes by cohort
| BC1 % |
BC2 % |
|
|---|---|---|
| Child was breastfed | 60 | 63 |
| Child was breastfed for >= 6 weeks | 42 | 42 |
| Child was breastfed for >= 6 months | 24 | 25 |
| Base: all families where mother was in household | 5135 | 5983 |
*The base for each measure is slightly different. The bases shown represent the lowest of the three
Overall, there was little change between BC1 and BC2 in recall of 'any' advice about breastfeeding received at the time of birth (74% compared with 75%), or advice from a health visitor (24% compared with 25%). However, there was a significant reduction in recalling advice from a midwife (69% compared with 65%) and an increase in recalling advice from an 'other health professional' (9% compared with 14%).
Assessing change between cohorts in the context of associations of breastfeeding outcomes with socio-demographic variables
Logistic regression modelling was undertaken to explore the association of breastfeeding for six weeks or more, with the available socio-demographic variables, and taking account of cohort.
Table 4.10 lists the independent associations found (that is, after adjusting for all other variables included in the model). The first thing to note is that there is a statistically significant, albeit modest, difference between cohorts. Breastfeeding for six weeks or more was greater in BC1, after multivariate adjustment for the other factors in the model (odds of breastfeeding for at least six weeks are 13% higher in BC1 relative to BC2).
With respect to socio-demographic factors, the model shows that the circumstances most strongly associated with breastfeeding for six weeks or more, versus shorter duration or no breastfeeding at all, are:
- extent of education
- living with a partner
- non-white ethnicity
- not living in deprived areas
- older age of mother at birth
- living in more remote/rural areas of Scotland
Whether or not the child was first born was not associated.
Table 4.10 Associations of breastfeeding (at all) for six weeks or more, with socio-demographic factors and cohort*
| Factor | Odds of BF at all for >=6 wks: |
|---|---|
| Education | Higher amongst mothers with degree or 'other' education qualifications |
| Single parent | Higher amongst mothers living with a partner |
| Ethnic group | Higher amongst mothers from non-white ethnic group |
| SIMD quintile | Highest amongst mothers living in less deprived areas, greatest in least deprived |
| Maternal age | Higher amongst older mothers, greatest in oldest age group |
| Urban-rural | Higher amongst mothers living in remote rural areas or remote small towns |
| Cohort | Higher amongst mothers in BC1 |
| Income** | Higher amongst mothers in highest two income quintiles |
| First born child | Not significant |
* Multivariate logistic regression model, p values for 'first born' non-significant, for cohort and for income = 0.02, and for all other factors <0.001; table arranged in order of strength of association with factor ['Working now' omitted for the sake of stability of the model.]
** Equivalised household income (quintiles)
Whereas Table 4.9 showed that, considered on its own, the percentage breastfeeding for six weeks was unchanged between cohorts 1 and 2 (42%), this multivariate analysis shows that, after adjustment for all the socio-demographic factors in the model (and how their distributions might have changed over the six years between cohorts), there was a small statistically significant effect for cohort, with cohort 2 having reduced odds of breastfeeding for at least six weeks, counter to policy aims.
Figure 4.3, Figure 4.4 and Figure 4.5 each show the proportion of mothers who breastfed at all for six weeks or more in both cohorts 1 and 2 (first two bars), and who breastfeed exclusively for six or more weeks in cohort 2 (third bars). They report percentages for these outcomes across the key socio-economic variables: maternal age, education, and area deprivation. Examining first, the change across time between BC1 and BC2 for the 'any BF' outcome (first two bars in each set), it can be seen that:
- there has been very little change across time with respect to maternal age, except that the achievement of the target has fallen in mothers aged 40 or older
- there is minimal change across time with respect to deprivation quintile
- with respect to education, there has been an increase from BC1 to BC2 among those with no educational qualifications, albeit also deteriorations among those with standard grade or equivalent, higher or equivalent, or vocational level education short of degree
Exclusive BF for six weeks or more (third bar) is a more stringent condition, so percentages achieving this are generally lower, particularly in the groups who tend to have been most successful in achieving the previous less stringent threshold (the oldest age group, the least deprived and those with highest education).
Figure 4.3 Percentage breastfeeding outcomes by maternal age at birth
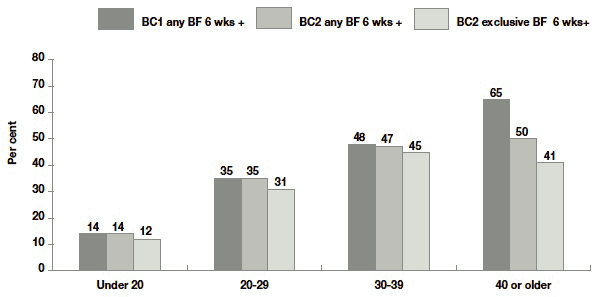
Base - all cases where mother was in household: BC1 - under 20 = 353, 20-29 = 2098, 30-39 = 2569, 40 or older = 183; BC2 - under 20 = 343, 20-29 = 2550, 30-39 = 2948, 40 or older = 267
Figure 4.4 Percentage breastfeeding outcomes by SIMD deprivation quintile
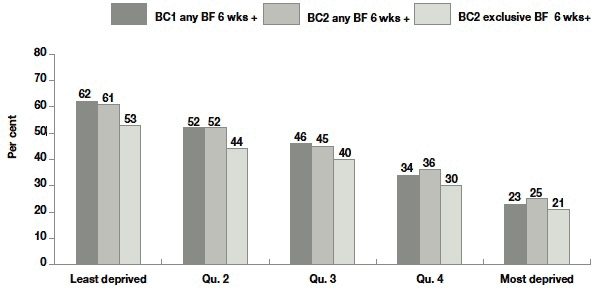
Base - all cases where mother was in household: BC1 - Least deprived = 1170, Qu2 = 1057, Qu3 = 1043, Qu4 = 931, Most deprived = 1015; BC2 - Least deprived = 1283, Qu2 = 1233, Qu3 = 1267, Qu4 = 1171, Most deprived = 1153
Figure 4.5 Percentage breastfeeding outcomes by education
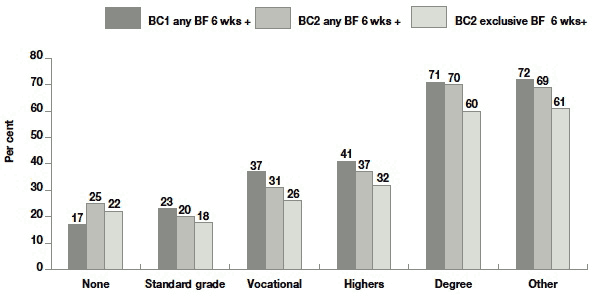
Base - all cases where mother was respondent: BC1 - None = 471, Standard grade = 938, Vocational = 1915, Highers = 382, Degree = 1456; BC2 - None = 388, Standard grade = 1002, Vocational = 1935, Highers = 489, Degree = 2135
The modelling analysis reported in Table 4.10 was based on both (entire) cohorts, insofar as there is not missing data for one or other variable. It is of interest to rerun the analysis selecting only those who breastfed at all, so as to be able to explore the associations for continuing to six weeks at least, given that breastfeeding has been initiated. For this subset analysis, the model (not shown) reveals that associations remain with all factors except household income. One notable change is that cohort becomes more pertinent (p<0.001), with odds of continuing to six weeks at least, among those where breastfeeding has been initiated, being 27% higher in BC1 relative to BC2. Another change in the model is that the factor 'non-first-born child', which was non-significant in the full analysis, is strongly associated with achieving six weeks, while ethnic group and maternal age have become less strongly associated. The strongest associations are with education, living with a partner, non-first born, cohort, not living in a deprived area, and remote rural living. This suggests that social factors are differentially associated with the decision to initiate breastfeeding, and once this decision is made, with succeeding to six weeks at least.
4.5.2 Solid foods
When started solid foods
As explained above, the switch in measurement units (from months to weeks) for this item makes it difficult to undertake a reliable comparison between BC1 and BC2. Figure 4.6 shows a comparison for BC1 (recorded in months) against two versions of BC2 data (where age was recorded in days, weeks or months as preferred, and was subsequently recoded into age in 'months').
For both of these two versions of age at starting solids (BC2), the distribution was statistically significantly different from BC1. But the 'at least' version (middle bars) shows deterioration against BC1 (left-hand bars), with more babies starting solids as early as three months of age. On the other hand the 'mid' version (right-hand bars) shows an improvement over BC1, with fewer babies starting solids as early as four months (41% in BC2 compared with 60% in BC1) and as early as five months (69% in BC2 compared with 82% in BC1). This means more have waited until six months, in line with the refreshed recommendations.
Figure 4.6 Cumulative percentage of children starting solids foods, by age at introduction - BC1 and BC2 (using two formats of 'age')
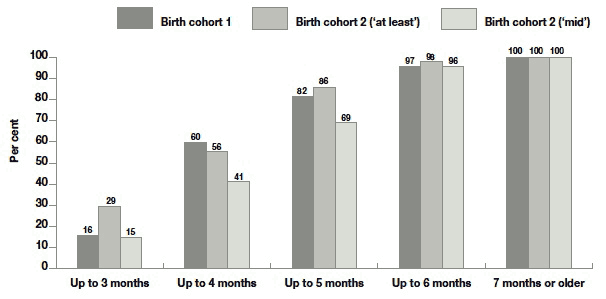
Please see Methods section for explanation of 'age'
Bases - all families: BC1 = 5133, BC2 = 6109
4.6 Summary
With regard to breastfeeding rates, the target of 32.7% mothers breastfeeding exclusively to six weeks was exceeded (36%). However, the prior target of 50% breastfeeding (not necessarily exclusively) to six weeks has not been met (42%), and was unchanged from BC1, six years previously. In terms of exclusive breastfeeding, only 11% of BC2 continued this to six months of age, but this rate is substantially higher than the rate reported by the 2005 infant feeding survey (<1%). The percentages of mothers in BC1 and BC2 continuing breastfeeding to six months or more were also very similar - 24% and 25%.
Breastfeeding rates (initiation and continuation to six weeks/six months) are strongly associated with socio-demographic factors. Multivariate analysis showed that breastfeeding is more likely to occur, and continue to six weeks, if: either parent has a degree or 'other' educational qualification; the mother has a resident partner, is of a minority ethnicity, or is older; if the family live in a rural area, or a less deprived area; and, to a lesser extent, if the household has a high income. These are not easy circumstances to remedy.
Despite the simple comparison showing no change in rates of breastfeeding at all to at least six weeks between BC1 and BC2 (42%), the multivariate analyses suggested this was misleading. After adjusting for these relevant socio-economic factors, there was a statistically significant decrease between BC1 and BC2 in the rates breastfeeding to six weeks at least.
It is striking that one of the strongest factors for achievement of exclusive breastfeeding up to six weeks is 'other ethnic' group (ie. not white). Many of these mothers may have considerable difficulties of language and access to information, advice and support, but they succeed with breastfeeding. Perhaps the key is mind set and cultural experience and expectation as to how a mother should nourish her new infant. It is noticeable in the entire cohorts (mainly the majority white ethnic population) that there are big disparities in breastfeeding rates across the rural-urban classification, over and above the well-known effects of education, deprivation and young age. It might be fruitful to reflect why/how a pregnant woman with all the risk factors for not breastfeeding, but who lives in a remote/rural location, succeeds with breastfeeding when a similar mother living in an urban environment does not, and what lessons can be learned.
Age at starting solids was measured in weeks for BC2. However, the guidance is measured in months making comparison difficult. The adjusted data suggests that only 14% of parents waited until six months (26 weeks), the threshold as per guidance. However, 42% had waited until at least five months (21 weeks). It was found that the age at starting solids was older if more extensive breastfeeding had happened, and even older if breastfeeding had continued to six months at least.
Given that age at introduction to solids was assessed in months for BC1, and the methodological concerns, it is difficult to be sure how to compare BC1 and BC2 with respect to starting solids, but it appears that fewer BC2 babies have been introduced to solids as early as four months of age (a reduction of between 4 and 18 percentage points depending on method applied to weeks-months calculation).
Efforts to improve infant feeding outcomes focus on information, advice and support, since this is what health services can deliver. The latest Getting Off to a good start booklet (a written resource providing breastfeeding information to new mothers), provided parents with information as well as contact details for a vast array of networks and resources, many of which are web-based, to which mothers can turn to for additional advice on breastfeeding (NHS Health Scotland, 2012). There is some evidence in the GUS data that this is helpful. Of those who recall receiving breastfeeding advice at the time of birth, 85% did try breastfeeding, versus 60% among the rest. In terms of continuing to six weeks, at least once initiated, there is evidence of the advantage of advice from a health visitor or other health professional.
The two most common reasons for stopping breastfeeding (31% each) were 'not enough milk' and 'other' (stated reasons that could not be categorised into any of the main themes). These might be fruitful areas for further research and development of initiatives.
It is important to bear in mind that the data on advice received regarding breastfeeding has to be recalled at interview, some 11 months to a year after the birth of the child, and the accuracy of recall is likely to be related to interest in breastfeeding. The same applies to reasons for not breastfeeding, or for stopping breastfeeding. There is potential for recall error, and recall bias. That said, temporal ordering is important, with information and advice most needed before delivery, to be prepared to breastfeed, and only 65% of mothers recalled having received advice from a midwife (and indeed, there has been a significant decline in advice from this source between birth cohorts 1 and 2). If midwives do not have the time to advise breastfeeding before or at the time of the birth, this would seem a missed opportunity.
4.7 References
Kramer, M.S., Kakuma, R., World Health Organization (2002). Nutrition for Health and Development., Geneva: Dept. of Child and Adolescent Health and Development, World Health Organization.
Kramer, M.S., Kakuma, R., (2002) The optimal duration of exclusive breastfeeding: a systematic review. Geneva: Dept. of Nutrition for Health and Development, Dept. of Child and Adolescent Health and Development, World Health Organization.
National Statistics (2007) Infant Feeding Survey 2005, London: National Statistics.
NHS Health Development Agency (2003) Effectiveness of public health interventions to promote the initiation of breastfeeding, London: NHS Health Development Agency.
NHS Health Scotland (2006) Getting Off to a good start: all you need to know about breastfeeding your baby, Edinburgh: NHS Health Scotland.
NHS Health Scotland (2011) First fun food: an easy guide to introducing solid foods. Edinburgh: NHS Health Scotland.
NHS Health Scotland (2012) Off to a good start: all you need to know about breastfeeding your baby. Edinburgh: NHS Health Scotland.
Scottish Executive (2000) Our national health a plan for action, a plan for change. Edinburgh: Scottish Executive.
Scottish Executive (2004) Eating for health - Meeting the Challenge: Co-ordinated action, improved communication and leadership for Scottish food and health policy, Edinburgh: Scottish Executive.
Scottish Executive (2005) Health for all children 4: guidance on implementation in Scotland Edinburgh: Scottish Executive.
Scottish Executive - Dept. of Health, NHS Scotland (2002) Towards better oral health in children : a consultation document on children's oral health in Scotland. Edinburgh: Scottish Executive.
Scottish Executive, S. (2006) Nutritional guidance for early years: food choices for children aged 1-5 years in early education and childcare settings. Edinburgh: Scottish Executive.
Scottish Government (2007) Better health, better care: action plan. Edinburgh: Scottish Government.
Scottish Government (2008) Healthy eating, active living: an action plan to improve diet, increase physical activity and tackle obesity (2008-2011). Edinburgh: Scottish Government.
Scottish Government (2011) Improving maternal and infant nutrition a framework for action. Edinburgh: Scottish Government.
Scottish Intercollegiate Guidelines Network (2003) Management of obesity in children and young people: a national clinical guideline. Edinburgh: SIGN.
Scottish Intercollegiate Guidelines Network, NHS Quality Improvement Scotland, (2010) Management of obesity: a national clinical guideline. Edinburgh: SIGN.
Scottish Office (1993) The Scottish Diet (the James report), Edinburgh: Scottish Office.
Scottish Office - Dept. of Health (1996) Eating for health: a diet action plan for Scotland. Edinburgh: Scottish Office Department of Health.
UNICEF UK (2009) Developing a breastfeeding strategy. The UNICEF UK Baby Friendly initiative, London: UNICEF.
Contact
Email: Sharon Glen