Growing Up in Scotland: Birth Cohort 2. Results from the First Year
This Growing up in Scotland report provides a detailed insight into the first set of data collected from the study’s second birth cohort – representative of all children born in Scotland between 1st March 2010 and 28th February 2011 – around the time they were all aged 10 months old.
Chapter 10 Parental Health
Tessa Hill, ScotCen Social Research
10.1 Introduction
Parental health and wellbeing is important to parenting and in shaping the early experiences of young children, including their health and development (Anderson et al. 2007). Previous GUS reports have shown that maternal health problems are a significant factor associated with child outcomes (Barnes et al. 2010). Maternal psychological wellbeing has been found to be a key association between maternal health and behaviour difficulties in children (Kelly and Bartley, 2010 cited in Chanfreau et al. 2011).
Factors such as problematic parental drug and alcohol misuse can impact on family life and pose harm to children (Hill, 2012). In a study of children's telephone calls to ChildLine Scotland about parental and significant carer health and wellbeing, parental alcohol misuse was the most frequently reported concern (Ogilvie-Whyte, 2005).
Given the importance of parental health to family wellbeing and children's development, a range of policy initiatives have been introduced in Scotland with the aim of improving health and promoting healthy living. Equally Well[50] aims to tackle the underlying causes of health inequalities and is also supported by a range of frameworks to improve maternal health and reduce health inequalities[51]. Other initiatives include: the Healthy Eating Active Living action plan[52] which aims to improve diet, increase physical activity and tackle obesity; an obesity prevention strategy;[53] the Health Works strategy which recognises the links between health and wellbeing, work and other meaningful activity;[54] the Good Places, Better Health strategy on health and the environment;[55] and Framework for Action on alcohol[56].
A key factor influencing quality of life, and parental health and health behaviour, is socio-economic status (SES). For example, SES has been found to be a key association between parental health and children's cognitive ability (Kelly and Bartley, 2010 cited in Chanfreau et al. 2011). The factors associated with living on a low income (eg. food poverty, fuel poverty, restrictions in social participation, living with debt) can undermine present and future physical and mental health and wellbeing (Ridge, 2009; Ghate and Hazel, 2002; Turner, 2006), lead to stigma, exclusion and isolation for the whole family (Green 2007; Ridge 2009; McKendrick et al. 2003b), and undermine a parent's capacity to maintain a satisfactory family life. The stress arising from financial difficulty can have a detrimental effect on parenting (Ghate et al. 2002; McKendrick et al. 2003a; Ridge, 2009), and affect outcomes for children (Katz et al. 2007). The combination of working long hours and low pay can make it difficult for parents to provide nutritious meals for children (Green, 2007), yet some parents do not apply for free school meals for fear of stigmatisation (Seaman et al. 2005).
Aside from socio-economic factors, life-events such as physical or mental ill-health, bereavement, and parental conflict or separation can influence parents' emotional wellbeing, put pressure on family relationships, and undermine parents' capacity to parent in the way they would wish (Parentline Plus, 2008; Walker et al. 2010).
The factors outlined above can combine to undermine parents' involvement in services. Preventive services (for example, services that aim to promote quality of life and wellbeing,
or prevent or delay the need for costly and intensive services) usually rely on parents actively seeking help or voluntarily accepting help offered to them. However, families such as those living on low-incomes or in rural areas, can face practical barriers (eg. lack of transport) to accessing healthcare and advice and support services (McSorley 2008; Palmer et al. 2006; Bradshaw et al. 2009; Green, 2007; Ridge, 2009). Without transport, mothers are particularly likely to not attend preventative (but non-urgent) healthcare services (Bostock, 2001 cited in Ridge, 2009).
Barriers to using mental health services relate to perceptions, feelings and beliefs, rather than availability, affordability and access (Brownlie, 2011; Anderson and Brownlie, 2011; Broadhurst, 2003). This suggests that expanding provision alone may not be sufficient to increase service use (Anderson et al. 2009).
While a range of initiatives have been developed in recent years to promote wellbeing and positive health behaviour, and address the underlying causes of health inequalities, the factors outlined may undermine the extent to which some families' can benefit from such developments. In addition, the current economic climate and proposed welfare changes (including changes to disability related benefits), combined with the ongoing cut-backs in existing welfare advice and other local services, are likely to increase anxiety and uncertainty amongst families and deepen health inequalities.
This chapter provides an overview of the health of the parents. It includes information on a number of indicators covering physical and mental health, and health behaviours such as smoking, drinking alcohol and use of illicit drugs.
10.2 Key findings
- 88% of main carers said that their general health was good, very good or excellent. Socio-economic status, whether measured by income, NS-SEC or area deprivation, had the greatest effect on general health. For example, 93% of parents living in the least deprived area reported their health as good or better compared with the proportion dropped from 93% in the least deprived quintile to 83% in the most deprived.
- 14% of main carers had a long standing illness, including 5% who said this was limiting. Variations were again evident by area deprivation, particularly in relation to limiting illness.
- Socio-economic status was also associated with physical and mental wellbeing as measured by the SF-12. Parents in more disadvantaged circumstances were more likely to report lower levels of both.
- 24% of main carers smoked. This represents a decrease - from 28% - compared with 2005.
- 12% of main carers were classified as hazardous drinkers according to the AUDIT-PC scale.
- Hazardous and binge drinking varied according to demographic and socio-economic characteristics. Differences were particularly stark in relation to maternal age with younger mothers significantly more likely to be classed as hazardous drinkers and to report binge drinking monthly or more often.
- 24% of main carers had taken drugs at some point in their lives though only 3% had reported drug use in the last year.
- Similarly, 4% of those in the top income quintile had used drugs in the last year, compared with 22% in the bottom income quintile. Younger mothers and parents living in more deprived areas also reported higher drug use in the last year.
10.3 General health
All respondents were asked to assess their general health as either 'excellent', 'very good', 'good', 'fair' or 'poor'. The vast majority of parents (88%) said that their general health was good or better (Table 10.1). In fact almost a quarter of parents (24%) said that their health was excellent. Only 12% regarded their health as fair or poor, with only 2% reporting the lowest rating. Fair or poor health was reported for both parents in just 1% of families.
Table 10.1 Parental self-reported general health
| % | |
|---|---|
| Excellent | 24 |
| Very good | 40 |
| Good | 25 |
| Fair | 10 |
| Poor | 2 |
| Can't say | <1 |
| Base: all families | 6024 |
Family composition was associated with how the respondent rated their general health.
Eight out of 10 respondents in lone parent families reported their health to be good or better compared with nine out of 10 in couple families. The proportion of respondents reporting good or better health decreased as the number of children in the household increased. 90% of respondents with one child reported good or better health compared with 87% of those with two or three children and 82% of those with four or more children.
General health also varied with ethnicity; 11% of white respondents reported fair or poor health compared with 19% of those from other ethnic backgrounds.
Socio-economic status, whether measured by income, NS-SEC or area deprivation, had the greatest effect on general health. The proportion reporting good or better health ranged from 93% in managerial and professional occupations to 77% amongst those who had never worked. Similarly for area deprivation, the proportion of parents with good or better health dropped from 93% in the least deprived quintile to 83% in the most deprived. Figure 10.1 shows how the proportions varied according to income quintile. Those in the lowest income quintile were almost 4 times more likely to report fair or poor health than those in the top income quintile (5% compared with 19%).
Figure 10.1 Self-assessed general health by income quintiles
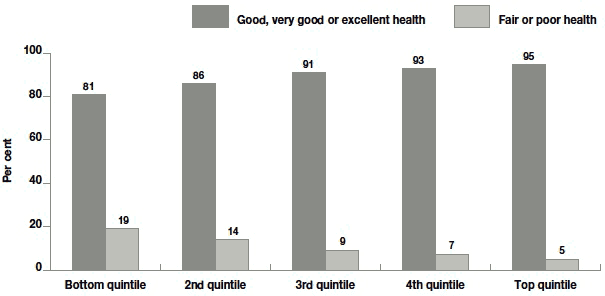
Base - all families: bottom quintile = 1101, 2nd quintile = 1019, 3rd quintile = 823, 4th quintile = 1354, top quintile = 1046
10.4 Long-standing illness
All respondents were asked whether they had any health problems or disabilities that had lasted or were expected to last for more than a year. They were then asked to say whether their illness limited their ability to carry out normal day-to-day activities in any way. Around one in seven parents (14%) reported a long-standing illness, of which just over a third (35%), or 5% of the whole sample, said it was limiting.
Lone parents were more likely to report a long-standing illness than parents in couple families (17% compared with 13%). Nearly a quarter of parents (24%) with four or more children had a long-standing illness, twice the proportion of those with only one child (12%). In both cases, the long-standing illnesses were also more likely to be limiting.
All measures of socio-economic status affected the prevalence of a long-standing illness. 10% of those in the top income quintile had a long-standing illness compared with 18% of those in the bottom income quintile. The proportion ranged between 11% and 16% for the most and least deprived area deprivation quintiles respectively, but the most striking differences were seen in the proportion of those illness that were limiting. Those in the most deprived quintile were over three times more likely to have a limiting long-standing illness than those in the least deprived quintile (7% of the total sample compared with 2%; Figure 10.2).
Figure 10.2 Long-standing illness by area deprivation quintile
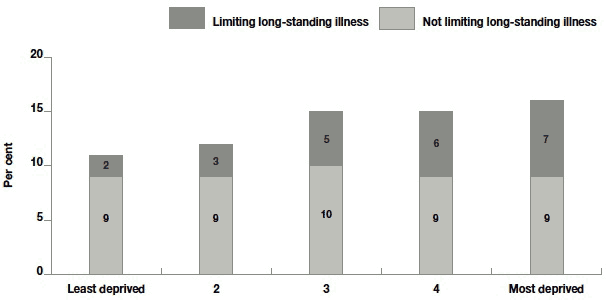
Base - all families: least deprived = 1147, 2nd quintile = 1166, 3rd quintile = 1243, 4th quintile = 1212, most deprived = 1252
10.5 Physical and mental wellbeing (SF-12)
Health-related quality of life was measured by the Medical Outcomes Study 12-Item Short Form (SF-12). This measure has been used on previous sweeps of GUS and is also widely used on other large population surveys such as the Scottish Health Survey. The SF-12 gives two summary scale scores: a physical component score (PCS) and a mental component score (MCS). Higher summary scale scores are indicative of better health-related quality of life. However, as the results are based on the respondents' self-reports of their own physical and mental functioning they are subjective and may lead to differential reporting between respondents with an equivalent health status.
Table 10.2 presents the results for the items that make up the SF-12 scale split by those in the lowest 15% of area deprivation scores compared with the highest 85%, and for the sample as whole.
Those in the lowest 15% scored consistently lower on both mental and physical health items. For example, around one in six (16%) of those in the lowest 15% said that their health limited them at least a little in moderate daily activities. This was compared with around one in eleven (9%) of those in the rest of the country. The difference was also apparent on the emotional measures. 27% of those in the most deprived group reported that they had felt down some of the time or more often compared with 20% of the rest of the country.
Table 10.2 Health-related quality of life (SF-12) by area deprivation
| SIMD deprivation score % | |||
|---|---|---|---|
| Health-related quality of life measures | Top 85% |
Lowest 15% | All % |
| Health assessed as fair or poor | 10 | 18 | 12 |
| Extent to which ill-health limits ability to perform moderate activities | |||
| A lot | 2 | 4 | 2 |
| A little | 8 | 11 | 8 |
| Not at all | 91 | 85 | 90 |
| Extent to which ill-health limits ability to climb several flights of stairs | |||
| A lot | 2 | 5 | 2 |
| A little | 9 | 15 | 10 |
| Not at all | 90 | 80 | 88 |
| Accomplished less as a result of poor physical health | 11 | 16 | 12 |
| Limited in work or other daily activities as a result of poor physical health | 8 | 13 | 9 |
| Accomplished less as a rest of emotional problems | 12 | 16 | 12 |
| Performed work or any other activities less carefully as a result of emotional problems | 8 | 12 | 9 |
| Pain interfered with normal work at least slightly | 18 | 27 | 20 |
| Extent to which felt calm and peaceful in last 4 weeks | |||
| All/most of the time | 50 | 53 | 51 |
| Good bit/some of the time | 42 | 39 | 41 |
| A little/none of the time | 9 | 8 | 9 |
| Amount of time had a lot of energy in last 4 weeks | |||
| All/most of the time | 41 | 42 | 41 |
| Good bit/some of the time | 48 | 46 | 47 |
| A little/none of the time | 11 | 12 | 11 |
| Amount of time felt down in last 4 weeks | |||
| All/most of the time | 3 | 5 | 3 |
| Good bit/some of the time | 17 | 22 | 18 |
| A little/none of the time | 80 | 73 | 79 |
| Amount of time felt that physical or emotional problems interfered with social activities in last 4 weeks | |||
| All/most of the time | 2 | 6 | 3 |
| Good bit/some of the time | 10 | 14 | 10 |
| A little/none of the time | 88 | 80 | 87 |
| Mean physical component score (PCS) | 53.4 | 51.5 | 53.1 |
| Standard error of mean | 0.09 | 0.24 | 0.86 |
| Mean mental component score (MCS) | 52.0 | 51.3 | 51.9 |
| Standard error of mean | 0.11 | 0.27 | 0.11 |
| Base: all families | 911 | 5046 | 6024 |
The summary scores were compared across a range of other groups within the sample. They were also associated to other measures of deprivation such as income and NS-SEC, with those in more disadvantaged circumstances scoring lower on both the PCS and MCS. For example, those in the top income quintile scored an average of 54.5 on the PCS, compared with 51.5 for those in the bottom income quintile. The respective scores for the MCS were 52.7 and 50.7.
Family type and composition were also associated with SF-12 scores. Lone parents averaged significantly lower on both component scores compared with those in couple families (PCS: 52.2 and MCS: 50.3 compared with 53.3 and 52.3 respectively). Those with four or more children were also more likely to score lower on the summary scores (PCS: 51.9, MCS: 49.7) compared with those in smaller families (PCS: 53.1, MCS: 52.0 respectively).
Non-white respondents scored lower than white respondents (50.3 compared with 53.2) on the physical component. However, there was no difference by ethnicity on the MCS (51.7 and 51.9 for non-white and white respondents respectively). It may be explained by the self-report nature of the measure. Those from non-white backgrounds typically report lower physical wellbeing. However, they may perceive their mental wellbeing to better than those from white ethnic backgrounds who are in a similar state of physical wellbeing. In other words, lower scores on both the PCS and MCS would be expected amongst non-white respondents but due to a more favourable perception of their mental health, the difference is only apparent on the PCS score. There is some tentative evidence to support this from the latest Scottish Health Survey equalities report (Whybrow et al. 2012). This shows that adults classed as white British have the lowest mental wellbeing scores of all ethnic groups in Scotland.
10.6 Smoking, alcohol and drugs
Respondents were asked a number of questions on smoking, drinking and drug use. Because of the sensitive nature of these topics, the questions were asked in the self-complete section of the interview where the responses were not seen by the interviewer.
The data relating to current smoking, drinking and drug use are presented in this chapter. For questions relating specifically to the pregnancy see chapter 3.
10.6.1 Smoking
Overall, 24% of parents were current smokers at the time of interview, similar to the percentage of Scottish women smoking in the equivalent Scottish Health Survey data (22%; Dowling, 2012). 22% of households had at least one adult who smoked in the house. Any current smokers were also asked how many cigarettes they smoked on a typical day, the average
of which was 10.
The responses to all of the questions on smoking varied significantly according to socio-economic status. Those in the bottom quintile for area deprivation, the lowest income quintile and the lower NS-SEC categories were all more likely to be current smokers, to smoke more cigarettes per day and to have at least one smoker in the house than their respective top categories.
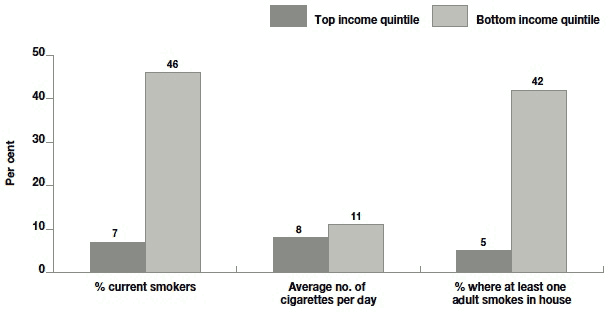
Base: For current smokers and adult smoking in house, all families - top income quintile = 1046, bottom income quintile = 1101;
For average no. of cigarettes per day, all where respondent smoked - top income quintile = 68 , bottom income quintile = 493
For example, 46% of those in the bottom income quintile smoked compared with 7% of those in the top income quintile. Smokers in the bottom quintile smoked an average of 11 cigarettes per day compared with eight by those in the top quintile. 42% of households in the bottom quintile had at least one adult who smoked in the house compared with 5% in the top quintile (Figure 10.3).
Lone parents were far more likely to smoke compared with those in couple families (49% compared with 18%), as were those with four or more children compared with those in smaller families (36% compared with 24%). They were also more likely to smoke more cigarettes per day and more likely to have at least one adult who smoked in the house.
Those from a white ethnic background were nearly three times more likely to smoke than those from non-white backgrounds (25% compared with 9%). They were also more likely
to have at least one adult who smoked in the house but the average number of cigarettes smoked per day by smokers did not differ.
Mother's age at birth also influenced the likelihood of the respondent being a smoker, with those under 20 being three times more likely to smoke than those over the age of 40 (46% compared with 15%). There was also more likely to be one adult who smoked in the house amongst younger families, but the number of cigarettes smoked per day was the same across all age groups.
Comparison with BC1
Across all measures, smoking had decreased between the two birth cohorts. Smoking prevalence decreased from 28% amongst BC1 respondents to 24% amongst BC2 respondents. The average number of cigarettes smoked per day decreased from 11 to 10. In addition, the proportion of households with at least one adult who smoked in the house decreased from 30% to 22%. This is in line with population trends documented by the Scottish Health Survey in recent years.
10.6.2 Alcohol
Six questions were asked on the topic of alcohol; two covered frequency and quantity of regular drinking and four related to more serious drinking. Together, five of these questions formed a version of the Alcohol Users Disorders Identification Test (AUDIT-PC) which is used to identify hazardous drinkers. The sixth item contributes to a shorter 3-item screening tool (AUDIT-C).
This section focuses on the responses to the questions on regular drinking and, although the questions differ slightly from those used with BC1, it makes some comparisons with the data from the previous cohort. The results of the AUDIT-PC are also presented[57].
Regular alcohol consumption
One in five parents said they never drank alcohol (21%). This is slightly higher than the proportion reported in the 2011 Scottish Health Survey for all adults (17% of women, 11% of men; Sharp, 2012) Given that all GUS respondents have young children, this is not surprising. The proportion of non-drinkers was highest amongst those in more disadvantaged groups (low income, higher deprivation quintiles, lower NS-SEC category). For example, those in the lowest income quintile were three times more likely to never drink alcohol compared with the top income quintile (29% compared with 10%).
Four out of five parents said they drank some alcohol (79%), with two in five (39%) drinking two times per month or more frequently (see Table 10.3). Those in more advantaged circumstances were more likely to drink more regularly. The proportion of those drinking twice per month or more frequently ranged from 59% in the least deprived areas to 27% in the most deprived areas. While there was no difference in the proportion that never drank alcohol between lone parents and couple families, lone parents were significantly less likely to drink alcohol on a regular basis (two times per month or more frequently) than those in couple families (27% compared with 42%).
Those sub-groups that tended to drink alcohol less frequently were, however, more likely to drink higher quantities on a typical drinking day. For example, parents in the bottom income quintile were over twice as likely to drink 5[58] or more units on a typical drinking day compared with those in the top quintile (45% compared with 20% respectively). There
was a difference of a similar magnitude when comparing between family types. 49% of lone parents reported drinking 5 or more units on a typical drinking day compared with 26% of those in couple families.
These trends are also reported in the latest Scottish Health Survey report (Sharp, 2012). For example, adults who lived in the most deprived quintile were more likely to be non-drinkers. However, amongst those that did drink, levels of alcohol consumption were higher than those in the less deprived quintiles.
The most striking differences were seen when comparing the sample by maternal age at birth (Figure 10.4). Over half (52%) of mothers aged under 20 drank 5 or more units on a typical drinking day compared with 38% of mothers in their twenties, 23% of mothers in their thirties and 13% of mothers who were over 40. Nearly one in five mothers under 20 (19%) reported drinking 10 or more units on a typical drinking day, over three times as much as any other age group.
Figure 10.4 Alcohol units consumed on a typical drinking day by maternal age
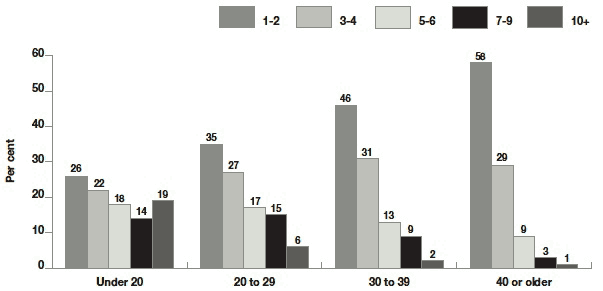
Base: all families where main respondent drank alcohol - under 20 = 267, 20 to 29 = 1927, 30 to 39 = 2376 , 40 or older = 215
Comparison with BC1
Similar questions were about the frequency and quantity of alcohol consumption were asked at BC1 sweep 1. However, the responses were changed for BC2 to allow for the calculation of the AUDIT-PC. Table 10.3 shows the original responses at sweep 1 for BC1 and BC2, and the responses for BC1 when some answer categories are combined to match those of BC2. Although this allows for easier comparison, caution should be applied when interpreting these results as the number of possible responses and their position on the list can influence the response given.
Table 10.3 Frequency of alcohol consumption by cohort
| BC1 % | BC1 % | BC2 % | ||
|---|---|---|---|---|
| Do not drink at all | 14 | Never | 14 | 21 |
| Not in the last year | 5 | Monthly or less |
33 | 40 |
| Once a month or less | 28 | |||
| 2-3 times per month | 15 | 2-4 times per month |
35 | 27 |
| Once a week | 20 | |||
| 2-3 times per week | 13 | 2-3 times per week |
13 | 11 |
| 4-6 times per week | 4 | 4+ times per week |
5 | 2 |
| Every day | 1 | |||
| Can't say | 1 | |||
| Base: all families | 5188 | 5157 | 6023 |
Note: Bases differ between the two BC1 columns because the 31 respondents who answered "Can't say" were recoded to missing for the comparison with BC2.
Nevertheless, the data appears to show that the majority of BC1 respondents were drinking on an almost weekly basis while the majority of BC2 respondents drink less frequently. This may be indicative of the general trend identified by the Scottish Health Survey, as the proportion exceeding the recommended guidelines for alcohol consumption has decreased in recent years. However, as the GUS respondents are predominantly female and all carers of young babies, they are not nationally representative of the entire Scottish adult population and so may demonstrate different trends over time.
AUDIT-PC
The Alcohol Use Disorders Identification Test 5-item version (AUDIT-PC) has been shown to be a reliable tool for screening for hazardous alcohol intake (Piccinelli et al. 1997). Responses are allocated points between 0-4 which are then summed to give an overall score out of 20. Those scoring 5 and above are classed as hazardous drinkers[59].
The scores from the GUS respondents ranged between 0 and 20 with 12% being classed as hazardous drinkers. The vast majority of these hazardous drinkers were on the borderline, scoring 5 points. Only 4% of respondents scored 6 or more points.
This is considerably lower than the proportion of Scottish adults classed as hazardous or harmful drinkers in the 2011 Scottish Health Survey (Sharp, 2012) although the definition is different (being based on units consumed per week[60]). SHeS data found that one quarter of men (25%) and just under a fifth (18%) of women were classed as hazardous or harmful drinkers (Sharp, 2012).
Interestingly, the prevalence of hazardous drinking was associated with household income but not with area deprivation. Those in the lowest income quintile were more likely to be hazardous drinkers than those in the top quintile (15% compared with 10%).
The most striking difference was again related to maternal age at birth; 23% of mothers under 20 were classed as hazardous drinkers compared with 11% in the older groups. This is partly explained by the responses to the item on units consumed on a typical drinking day as noted above. 19% of mothers under 20 drank 10+ or more units compared with 4% of the older age groups.
Binge drinking
The further single item included that did not form part of the AUDIT-PC asked how often the respondent had 6 or more units of alcohol on one occasion. This is the current definition of binge drinking[61]. 34% of respondents said they had never drunk 6 or more units of alcohol on one occasion. Nearly half of all respondents (48%) said that they had done this, but that it occurred less than monthly. 16% said that it occurred monthly, 3% weekly and less than 1% said that it occurred on a daily or almost daily basis.
The percentage of parents who reported binge drinking monthly or more often varied by many of the same characteristics that influenced the results of the AUDIT-PC. For example, those in more socio-economically deprived circumstances were more likely to report more frequent binge drinking. This was particularly highlighted by 26% of those in the bottom income quintile reporting monthly or more frequent 'binge' drinking compared with 16%-18% of parents in all other income quintiles.
Again, maternal age at birth was a strong differentiating factor. 34% of mothers under 20 reported binge drinking monthly or more often compared with 18% of mothers over 20. Also, lone parents were almost twice as likely to report 'binge' drinking on a monthly or more frequent basis compared with those in couple families (29% compared with 16%). This reflects, to a large extent, the younger average age of lone parents compared with parents in couple families as described in chapter 2.
10.6.3 Drugs
Parents were asked a series of questions about their use of certain illicit drugs - whether they had ever used drugs, whether they had used drugs in the last 12 months (since the birth of the cohort child) and what types they had used. Although the questions were included in the self-completion section of the interview - to provide a more confidential setting for the collection of this more sensitive information - there are a number of limitations associated with the data.
Firstly, it is likely that more 'serious' or 'chaotic' drug users are under-represented in the sample as they are more likely to be homeless, in prison or never available for interview. Secondly, as the drugs included are mostly illegal (though methadone could be prescribed), it is likely that drug use is under-reported within the survey, particularly amongst the 'heavier' substances. Finally, it is possible that people have forgotten occasional use of drugs, particularly if it was a long time ago.
Table 10.4 Percentage of parents ever using drugs and use in the previous 12 months by type of drug used
| Ever taken drugs | Taken drugs since birth of child |
|||
|---|---|---|---|---|
| % of all parents | % of those who ever taken drugs | % of all parents | % of those who have taken drugs since birth of child | |
| Cannabis | 22 | 92 | 2 | 79 |
| Amphetamines | 5 | 20 | <1 | 8 |
| Cocaine | 5 | 19 | <1 | 9 |
| Crack | <1 | 1 | <1 | 1 |
| Ecstasy | 5 | 21 | <1 | 6 |
| Heroin | 1 | 2 | <1 | 2 |
| Methadone | 1 | 2 | <1 | 13 |
| Acid or LSD | 2 | 8 | <1 | 1 |
| Another illegal drug | <1 | 2 | <1 | 1 |
| None of these | 76 | 3 | ||
| Base: as detailed in top row | 6021 | 1442 | 6008 | 172 |
24% of respondents said that they had taken drugs at some point in their lives. The majority of this was accounted for by cannabis use (92% of those who had taken drugs, and 22% of all parents). The next most common drugs to have been used were amphetamines, cocaine and ecstasy. However, these were all in very small proportions in comparison (reported by 19-21% of those who had taken drugs and 5% of all parents). The proportion of respondents who had ever taken drugs did not vary by any socio-economic characteristics.
Just 3% of all respondents had taken drugs in the last year (that is since their child was born). The majority of this was again accounted for by cannabis use (2% of all parents, 79% of those who reported drug use in the last year). However, in this instance, the next most common substances used were harder drugs such as methadone (used in the last year by <1% of all parents and 13% of those who used drugs in the last year) and cocaine (0.3% of all parents, 9% of those using in last year).
Drug use in the last year was influenced by various deprivation characteristics. For example, 8% of those in the least deprived quintile had used drugs in the last year compared with 23% in the most deprived quintile. Similarly, 4% of those in the top income quintile had used drugs in the last year, compared with 22% in the bottom income quintile. Mothers aged under 30 were also more likely to have used drugs in the last year than those aged 30 or over (17% had done so compared with 9%).
Comparison with BC1
Between 2005 and 2011, there was a small but significant decrease both in the proportion of parents reporting having ever taken drugs and having taken drugs in the last year (Figure 10.5).
Although this may reflect recent campaigns and interventions to reduce drug use amongst parents, it may also be due to sampling variation with fewer drugs users being included in the BC2 sample. It is also possible parents in BC2 were more likely to under-report drug use than those in BC1 given a greater perceived stigmatism about drug use generally and specifically amongst parents.
Figure 10.5 Drug use in both birth cohorts
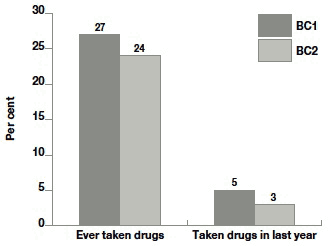
Base - all families: BC1 = 5182, BC2 = 6021
10.7 Summary
The data in this chapter presents a broad overview of the health of parents in Scotland with young children. The majority (88%) report to be in good health or better and 95% are without a limiting longstanding illness.
Smoking prevalence amongst main carers of children was similar to that of the overall Scottish population (around one in four). This proportion is considerably less than that reported at amongst parents in BC1 at the equivalent time point. This reduction can be attributed, at least in part, to the ban on smoking in enclosed public places introduced in 2006 and mirrors a decrease in smoking prevalence across the broader adult population during that time. Encouragingly, the percentage of households with at least one adult smoking inside the house dropped by a greater degree. This may be a by-product of the smoking ban increasing awareness of passive smoking and encouraging more parents to keep their homes smoke-free too.
The vast majority of parents drank some alcohol and most drank within the recommended guidelines. Indeed, alcohol consumption amongst parents is lower than amongst the general adult population. Only a small proportion reported drinking habits which categorised them as 'hazardous'. Alcohol consumption varied, in particular, by maternal age. Compared with older mothers, younger mothers, particularly those aged under 20 at the child's birth, reported more frequent drinking, a higher level of units on a typical drinking day, more binge drinking and were more likely to be classed as hazardous drinkers. Along with smoking, alcohol consumption had also reduced between cohorts.
Many parents had also tried drugs at some point in their lives, though very few had done so in the last year. Almost all drug use was accounted for by cannabis. Drug use had also decreased between the two cohorts.
With less smoking, lower alcohol consumption and less drug use, parents in 2011 appear to have adopted a healthier lifestyle when compared with parents in 2005. Nevertheless, the well reported links between deprivation status and health outcomes are still evident. On measures of general health and long-standing illness, physical and mental wellbeing, and smoking, drinking and drug use, parents in more disadvantaged circumstances continue to report poorer outcomes and health behaviours than their more advantaged peers.
10.8 References
Anderson, S., Bradshaw, P., Cunningham-Burley, S., Hayes, F., Jamieson, L., MacGregor, A., Marryat, L. and Wasoff, F. (2007) Growing Up In Scotland: Sweep 1 Overview Report. Edinburgh: Scottish Executive.
Anderson, S. and Brownlie, J. (2011) 'Build it and they will come? Understanding public views of 'emotions talk' and the talking therapies'. British Journal of Guidance and Counselling 39 (1):53-66.
Anderson, S., Brownlie, J., Given, G. (2009) Therapy Culture? Attitudes towards emotional support in Britain in Park, A., Curtice, J., Thomson, K., Philips, M., Clery, E British Social Attitudes: 25th report. London: National Centre for Social Research.
Barnes, M., Chanfreau, J. and Tomaszewski, W. (2010). Growing Up in Scotland: The circumstances of persistently poor children. Edinburgh: Scottish Government.
Bostock, L. (2001). Pathways of disadvantage? Walking as a mode of transport among low-income mothers. Health & Social Care in the Community, 9(1): 11-18.
Bradshaw, P., Sharp, C., Webster, C. and Jamieson, L. (2009) Growing Up in Scotland: parenting and the neighbourhood context report. Edinburgh: The Scottish Government.
Broadhurst, K. (2003) Engaging parents and carers with family support services: what can be learned from research on help-seeking. Child and Family Social Work 8:341-350.
Brownlie, J. (2011) '"Not 'going there": limits to the professionalisation of our emotional lives'. Sociology of Health and Illness 33(1): 130-144.
Chanfreau, J., Barnes, M., Tomaszewski, W., Philo, D., Hall, J. and Tipping, S. (2011) Growing Up in Scotland: Change in early childhood and the impact of significant events, Edinburgh: Scottish Government.
Dowling, S. (2012) "Chapter 4: Smoking" in Rutherford, L., Sharp, C. and Bromley, C. (Eds.)The Scottish Health Survey 2011: Volume 1 - Adults, Edinburgh: Scottish Government.
Ghate, D. and Hazel, N. (2002) Parenting in Poor Environments: stress, support and coping. London: Jessica Kingsley.
Green, M. (2007) Voices of people experiencing poverty in Scotland. Everyone matters? York: Joseph Rowntree Foundation.
Hill, L. (2012) Listening to and learning from children and young people affected by parental alcohol problems: CRFR briefing 58. Edinburgh: Centre for Research on Families and Relationships.
Katz, I., Corlyon, J., La Paca, V. and Hunter, S. (2007) The relationship between poverty and parenting. York: Joseph Rowntree Foundation.
Kelly, Y. and Bartley, M. (2010) "Parental and child health". In Hansen, K., Joshi, H. and Dex, S. (Eds.) Children of the 21st Century: The first five years. Bristol: The Policy Press.
McKendrick, J., Cunningham-Burley, S., Backett-Milburn, K. and Scott, G. (2003a) Life in low income families: a review of the literature. Edinburgh: Scottish Executive.
McKendrick, J., Cunningham-Burley, S. and Backett-Milburn, K. (2003b) Life in low income families: research report. Edinburgh: Scottish Executive.
McSorley, L. (2008) Special Study on Living in Poverty in Rural Areas Report to The Scottish Government Rural and Analysis Research and Analysis Directorate (RERAD). Edinburgh: SAC.
Ogilvie-Whyte, S. (2005) Children's concerns about health and wellbeing of parents and significant others, Research Briefing 22, Edinburgh: Centre for Research on Families and Relationships.
Palmer, G., MacInnes, T. and Kenway, P. (2006) Monitoring poverty and social exclusion in Scotland 2006. York: New Policy Institute.
Parentline Plus (2008) '"Love your children more than you hate each other." The impact of divorce and separation on families: Views of parentline plus service users'. London: Parentline Plus.
Picinelli, M., Tessari, E., Bortolomasi, M., Piasere, O., Semenzin, M., Garzotto, N. and Tansella, M. (1997) "Efficacy of the alcohol use disorders identification test as a screening tool for hazardous alcohol itake and related disorders in primary care: a validity study", BMJ, 314:420-424.
Ridge, T. (2009) Living with poverty: a review of the literature on children's and families' experiences of poverty. Department for Work and Pensions Research Report No. 594. London: Department for Work and Pensions.
Seaman, P., Turner, K., Hill, M., Stafford, A. and Walker, M. (2005) Parenting and Children's Resilience in Disadvantaged Communities. London: National Children's Bureau.
Sharp, C. (2012) "Chapter 3: Alcohol Consumption" in Rutherford, L., Sharp, C. and Bromley, C. (Eds.) The Scottish Health Survey 2011: Volume 1 - Adults, Edinburgh: Scottish Government.
Turner, H. (2006) Stress, Social Resources, and Depression among Never-Married and Divorced Rural Mothers. Rural Sociology 71(3): 479-504.
Walker, J., Barrett, H., Wilson, G., Chang, Y-S. (2010) Understanding the Needs of Adults (Particularly Parents) Regarding Relationship Support. London, Department for Children, Schools and Families.
Whybrow, P., Ramsay, J., MacNee, K. (2012) Scottish Health Survey Topic Report: Equality Groups, Edinburgh: Scottish Government.
Contact
Email: Sharon Glen