Growing Up in Scotland: Birth Cohort 2. Results from the First Year
This Growing up in Scotland report provides a detailed insight into the first set of data collected from the study’s second birth cohort – representative of all children born in Scotland between 1st March 2010 and 28th February 2011 – around the time they were all aged 10 months old.
Chapter 3 Pregnancy and Birth
Pamela Warner, Centre for Research on Families and Relationships
3.1 Background
In the six years between the births of GUS birth cohorts 1 (in 2004/5) and 2 (in 2010/11), Scotland has seen the publication of a range of policies having potential to impact on outcomes in pregnancy and birth. A few years prior to the birth of children in birth cohort 1 (BC1), the Scottish Government published its first ever Framework for Maternity Services in Scotland (Scottish Executive Health Department, 2001). The overarching aim was that all Scottish women should receive high quality maternity care before, during and after the birth of their child. The framework was developed from the General Health Action Plan published the year before, a programme of work designed to improve the quality, but also access and responsiveness, of healthcare in Scotland (Scottish Executive Health Department, 2000). Therefore, the maternity services framework also placed an emphasis on the importance of access, to routine services, to accurate information to inform decisions, and to specialist services (if needed).
One of the key principles underpinning the first maternity services framework was that "good health before and during early pregnancy benefits the woman, her unborn baby and the wider family" (Scottish Executive Health Department, 2001). One aim of the framework was that all women of reproductive age should be empowered and encouraged to be as healthy as possible. While it was noted that "social influences before, during and after pregnancy have a significant and far-reaching impact on child and maternal health", it was also judged that "pregnancy is an ideal opportunity to involve women, their partners and their families in a far greater understanding of their personal health, the benefits of health promotion and changes that can affect future health".
This was forward-thinking, because in the subsequent years attention focused more and more strongly on the stark inequalities in health found in Scotland. This culminated in the Equally Well ministerial report (Scottish Government, 2008), and then two frameworks - Achieving our Potential, to tackle poverty (Scottish Government, 2008), and the Early Years Framework (Scottish Government, 2009). Both the Early Years Framework and Equally Well place emphasis on the key role antenatal care has in reducing inequalities in health and improving health in the early years (Scottish Government, 2009, Scottish Government, 2008). They also address concerns regarding usage of alcohol, drugs and tobacco during pregnancy, but contend that women will do what is best for their babies, and will be willing to change their lifestyles, if their social and emotional circumstances are acknowledged and their hopes and aspirations for themselves and their babies are addressed. All of these policies addressing inequalities were published in the time period between the two GUS cohorts. While there was no inequalities policy specifically addressing maternity care, it is reasonable to assume that increasing attention was being given to find ways in which health care efforts could be focused to help reduce inequalities in health.
Subsequently, in January 2011, a 'refreshed' maternity services framework for maternity care in Scotland, was introduced - developed by the Maternity Services Action Group (MSAG) (Scottish Government, 2011). The revised framework acknowledged that the many determinants of poor outcomes are interlinked in a complex way, and that they cannot be addressed by health policy or healthcare alone. Nevertheless, the main aim of the new framework was to strengthen the contribution NHS maternity care makes to improving maternal and infant health and to reducing the observed inequalities in maternal and infant health outcomes. However, as hinted above, by the time this 'refreshed' framework was published, most of birth cohort 2 (BC2) had been born, and the remaining ongoing pregnancies were in their last trimester. Therefore data from GUS BC2 is slightly too early to evaluate any impact of this 2011 framework.
This chapter provides a detailed description of the pregnancies resulting in, and the births of, the BC2 children. In addition, selected characteristics and outcomes of BC2 are compared with the pregnancies and births of the BC1 children who were born six years earlier. For selected outcomes there was examination in a multivariate model of associations with key socio-demographic variables - maternal age group at birth, education, ethnicity, first child and, as at applying at time of interview, deprivation, equivalised household income, single parent or not, urban-rural living. This enables estimation of the association of the maternity outcome of interest (for example, attendance at antenatal classes) with each socio-demographic variable when there is simultaneous adjustment for all the other socio-demographic variables in the model. This is necessary because of the many-interlinked factors associated with behaviours and outcomes[8].
Multivariate modelling was also utiltised to adjust for socio-economic variables when undertaking other analyses such as comparing some outcome or behaviour between cohorts, or examining certain associations (eg. with receipt of Healthy Start Vouchers).
The main policy changes between BC1 and BC2 were associated with the growing concern to address inequalities in health in Scotland, although this was not enshrined in specific maternity care policy until after most of BC2 had been born (Scottish Government, 2011).
3.2 Key findings
It is important to bear in mind that each GUS cohort is representative, not of all pregnancies in the relevant timespan, but of the subset of pregnancies resulting in a live birth in Scotland, following on from which that infant is still resident in Scotland at 10 to 12 months of age.
- Median timing for first antenatal appointment (booking) was 9 weeks gestation, with 75% of women booking by 12 weeks.
- 19% of BC2 women reported they had been 'not very' or 'not at all well' during pregnancy, an increase from 13% in BC1 six years before. The proportion of women reporting an 'illness or problem' during pregnancy increased from 38% to 41% between BC1 and BC2.
- 90% of women took folic acid during pregnancy but only 38% took vitamin D. Women in receipt of Healthy Start Vouchers (HSV) were less likely to have taken these supplements. After adjustment for socio-demographic factors it was found that there was no difference in vitamin D intake between those receiving HSV or not, but the difference for folic acid persisted (fewer receiving HSV took folic acid).
- 84% of BC2 mothers believed it is better to avoid alcohol altogether during pregnancy, while 80% reported that they had drunk no alcohol during the pregnancy with the BC2 child. This latter percentage is higher than for BC1 (74%).
- 73% of BC2 women never smoked during pregnancy, compared with 75% in BC1, but a further 9% of BC2 stated that they gave up once they discovered they were pregnant (a response option not offered in BC1).
- 40% of all BC2 mothers attended antenatal classes, a decrease from BC1 (from 46%), however there was no significant difference between cohorts in the number of first-time mothers who attended antenatal classes (71% of BC1 compared with 69% of BC2)
- Sources of information when pregnant that were most commonly cited were health professionals (90%), family/friends (71%), internet (55%), and Ready Steady Baby booklet (48%), with mention of the internet having more than doubled since BC1. The three sources felt by parents in BC2 to be most helpful were health professionals, family/friends and then internet, which was similar to BC1 except that internet had replaced books/magazines in third place.
- 60% of BC2 births were described as 'normal', a small, but statistically significant reduction from BC1 (62%).
- Mean birthweight of children in BC2 was 3391g, very similar to BC1, and the prevalence of low birthweight (<2500g) was 7% in both cohorts. As would be expected, low birthweight was associated with whether the baby arrived early, on time or late and with socio-demographic factors (lower education, low household income and older maternal age).
3.3 Planning and recognition of pregnancy
Overall, responses regarding planning of the pregnancy did not change statistically significantly between the two cohorts. However, the proportion of pregnancies planned jointly by the couple increased marginally from 58% in BC1 to 60% in BC2. There was also a change in the proportion of completely unplanned pregnancies, reducing from 24% in BC1 to 21% in BC2. Percentages for one-sided planning (by the woman) and for not-planned-but-not-prevented were unchanged across the cohorts (1% and 17% respectively).
In BC2, the weeks of gestation when the mother became aware of the pregnancy had a median of five weeks, with half of all responses lying between four to six weeks gestation, and the range running from zero weeks (four respondents) to 39 weeks (one respondent).
Commencing antenatal care
The median timing for the mother's first antenatal appointment for BC2 was 9 weeks (with three quarters booking by 12 weeks). The proportion having their first booking at 23 weeks or later was 1%. The range in gestation at booking ran from 0 weeks (10 respondents) to
38 weeks (1 respondent).
The first antenatal appointment was with a midwife for 59%, GP for 22% and hospital clinic for 19%.
3.4 Health during pregnancy
Self-reported health during pregnancy
The comparison of self-reports of general health in pregnancy by cohort is shown in Figure 3.1. Self-reported health during pregnancy deteriorated between the two cohorts, with fewer mothers in BC2 reporting having been very well (46% compared with 51% in BC1) and more reporting 'not well' to some degree (19% compared with 14%).
Figure 3.1 Self-report of health during pregnancy by cohort (BC1 vs BC2)
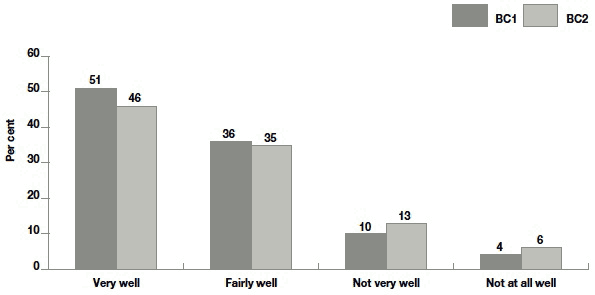
Base - all families: BC1 = 5210, BC2 = 6106
Specific medical problems
To the specific question about 'any illness or problem in pregnancy' the number of respondents answering 'yes' increased between BC1 and BC2 from 38% to 41%. Table 3.1 lists the most frequently reported illnesses/problems out of the 30 items coded. 'Multiple pregnancy' is one of the list of possible 'problems' enquired about, but in these GUS cohorts, the number is very low - just 6 in BC1 and 4 in BC2, well less than 1%.
Table 3.1 Illness or problems occurring during pregnancy (BC1 and BC2)
| Problem/illness | BC1 % |
BC2 % |
|---|---|---|
| (Pre-)eclampsia or raised BP* | 7 | 4 |
| Persistent vomiting* | 4 | 5 |
| Anaemia during pregnancy | 4 | 4 |
| Threatened miscarriage* | 4 | 3 |
| Symphysis pubis | 3 | 3 |
| Backache* | 2 | 3 |
| Urinary infection | 2 | 2 |
| Non-trivial infection | 2 | 2 |
| Blood group incompatibilities or other disorders* | 2 | 1 |
| Other pelvic joint problems* | 1 | 3 |
| Diabetes in pregnancy/ Gestational diabetes* | 1 | 2 |
| Depression/mental illness | 1 | 1 |
| Liver/gall bladder problems | 1 | 1 |
| 'Other'* | 9 | 14 |
| Base: all families where mother was respondent | 5139 | 5996 |
* Statistically significant difference between cohorts, p<0.05
Between the two cohorts there was a reduction in the proportion of women reporting 'raised blood pressure (BP), pre-eclampsia or eclampsia during pregnancy', threatened miscarriage and blood group disorders. However there was an increase in the proportions reporting persistent vomiting, backache, pelvic joint problems, diabetes in pregnancy and 'other' problems. The table reports combined percentages for 'diabetes in pregnancy' and 'gestational diabetes', but in each cohort there was a very similar mix of the two problems reported - roughly half and half.
Taking supplements (BC2 only)
Parents in BC2 were asked whether they had taken certain supplements during their pregnancy with the cohort child. Overall, 62% of BC2 women took no vitamin D supplement at all. The percentages taking some vitamin D were:
- 15% prior to pregnancy
- 32% during the first three months of pregnancy
- 26% during the second three months
- 1% during the last three months
The percentages of BC2 women reporting having taken folic acid were:
- 48% prior to pregnancy
- 90% during the first three months of pregnancy
One possible impact of the Healthy Start voucher (HSV) scheme (see also 3.3.2) is that it might improve intake of supplements around pregnancy. Women who were receiving HSVs at interview were compared with those who were not, in respect of supplement intake in pregnancy. It was found that there was a statistically significant difference in rates between the two subgroups for all six forms/timing of supplementation listed above, in that women receiving HSVs were less likely to have taken vitamin D supplements (26% of those receiving HSVs took any vitamin D at all compared with 42% who were not receiving HSV. For specific timings of vitamin D in order of the list above: 6% of HSV recipients compared with 18% of non-recipients; 20% compared with 36%; 18% compared with 28%; and 16% compared with 25%). For folic acid there was a similar picture (27% amongst HSV recipients compared with 54% for non-recipients for prior and 80% compared with 92% during pregnancy).
However, this might be partly to do with the fact that those eligible for receipt of HSVs have multiple characteristics that have been found to be associated with less 'healthy' behaviours and actions in pregnancy. Hence it is possible that the HSVs have nevertheless ameliorated what would have been a worse situation. The association of supplement intake around pregnancy was therefore examined in a multivariate model[9], to determine factors associated with 'folic acid in first three months of pregnancy' and 'any vitamin D intake around pregnancy'. This enabled examination of the association of HSVs with supplement intake adjusted for important socio-demographic variables.
On multivariate analysis, 'any' intake of vitamin D was statistically significantly and strongly associated with education (the more extended the education the more prevalent was intake) and household income (the more affluent the more prevalent folic acid intake). There was also a modest association with age (vitamin D use more likely if younger), but no association with ethnicity nor deprivation. The lack of association with ethnicity is disappointing, since people with dark or black skins living in high latitudes have greater requirement for vitamin D (regardless of pregnancy). When receipt of HSVs was added to the model, it was not found to be statistically significantly associated with folic acid intake, after adjustment for the socio-demographic factors. So this means that the significantly worse intake for any vitamin D, found above (via 'univariate' analysis), would appear to have been an artefact of confounding by socio-demographic variables that differ between recipients and non-recipients of HSVs. Therefore, after multivariate adjustment for socio-demographic variables, HSVs are not associated with differential vitamin D intake, better or worse.
On multivariate analysis of folic acid intake in the first three months of pregnancy, this was found to be significantly associated with education (the more extended the education the more prevalent folic acid intake), household income (the richer the more prevalent folic acid intake), and ethnicity, but not with maternal age nor deprivation. The association with ethnicity was that white mothers had odds of folic acid intake that were higher - by 170% - relative to other ethnic mothers. When receipt of HSVs was added to the model, this was found to be statistically significantly associated with folic acid intake (p<0.002), but again in the reverse direction from what might have been hoped, in that those not in receipt of HSVs had higher odds of folic intake, by 54% relative to those who did receive HSVs. This means that, contrary to the situation with vitamin D, even after adjustment for socio-demographic factors, there remained a statistically significant association of HSVs with worse folic acid supplement intake. However, the association was less strong after adjustment (odds ratio reducing from 2.94 to 1.54), so this suggests that in the initial univariate analysis above, there had been a degree of confounding by socio-demographic factors, which had inflated the apparent association.
In addition, Healthy Start vitamins are not normally available to mothers before their tenth week of pregnancy. Along with the time required to process applications, this may have resulted in few women taking HS vitamins before 12 weeks of pregnancy.
3.5 Alcohol, smoking and drugs in pregnancy
Knowledge of alcohol guidelines
Almost all BC2 respondents said they knew the alcohol guidelines for pregnancy (93%). Their 'own words' statement, at interview, of the gist of the guidelines, was categorised as shown in the left section of Table 3.2. Respondents were also asked their personal views about drinking in pregnancy. Their distribution of responses (chosen from a show card) is as shown in the right section of Table 3.2. Considerably more women state that they believe there should be no drinking in pregnancy, than there are who believe the guidelines recommend abstinence (84% compared with 69%).
Table 3.2 Respondents' understanding of the alcohol guidelines and views about drinking alcohol in pregnancy (BC2)
| Respondents' understanding of the guidelines about drinking alcohol in pregnancy (said in own words and subsequently categorised) | % | Respondents' own view about drinking alcohol in pregnancy (wording as on showcard) | % |
|---|---|---|---|
| Regular alcohol OK during pregnancy | 17 | Women do not need to worry how much alcohol they drink when pregnant | >1 |
| Occasional alcohol OK in pregnancy | 6 | Drinking a moderate amount of alcohol can usually be considered safe | 1 |
| A little is OK but best not to drink | 6 | Drinking a small amount of alcohol can usually be considered safe | 16 |
| No alcohol | 69 | It is better not to drink at all during pregnancy | 84 |
| Not sure | 3 | ||
| Other specific views? | 4 | ||
| Base: all families where mother was respondent | 5984 | 5990 |
Amount of alcohol consumed while pregnant - self complete
In both cohorts respondents were asked how often they drank alcohol in pregnancy. The distributions of responses are given in Table 3.3. These percentages show a statistically significant reduction between the two cohorts in frequency of alcohol consumption in pregnancy. However, it should be noted that in BC2 there were 15 respondents (weighted) who drank alcohol more than three times a week while pregnant and eight who drank it every day. In BC2, views about drinking alcohol (views as reported in the right hand section of Table 3.2) were very strongly related to alcohol consumption during pregnancy.
Table 3.3 Alcohol consumed in pregnancy (BC1 & BC2)
| BC1 % | BC2 % | |
|---|---|---|
| 1-2 times a week or more often | 4 | 2 |
| 2-3 times a month | 5 | 3 |
| Less than once a month | 17 | 15 |
| Never | 74 | 80 |
| Base: all families where mother was respondent | 5107 | 5885 |
In BC2, respondents who drank alcohol during pregnancy were asked how many units they usually drank on a day they were drinking. The vast majority stated 1-2 units per day (96%), while 3-4 units were usual for 3%, and 5-10 plus for the remaining 1%.
Smoking during pregnancy
The smoking questions (asked in the self-complete section) differed across the two cohorts. Item response options are presented in Table 3.4, roughly in order from unchanged smoking, or smoking most days during pregnancy, down to stopping once found out pregnant, and finally to never smoked at all while pregnant (75% and 73% in the two cohorts). No formal comparison is possible, but in terms of never smoking there has been a slight reduction, with the percentage falling from 75% to 73% between BC1 and BC2.
Table 3.4 Smoking while pregnant (BC1 & BC2)
| BC1 % | BC2 % | |
|---|---|---|
| Yes, most days | 13 | - |
| I continued smoking as before I was pregnant | - | 4 |
| I tried to stop but did not manage to | - | 5 |
| Yes, occasionally | 12 | - |
| I reduced amount | - | 9 |
| I stopped when I found out I was pregnant | - | 9 |
| Never | 75 | 73 |
| Base: all families where mother was respondent | 5107 | 5883 |
Drugs during pregnancy
Of 1390 BC2 women who were past drug users, 32% had stopped well before becoming pregnant, 3% while trying to get pregnant or as soon as they found out, 62% did not use any drugs while pregnant, 2% reduced the amount used, while 1% continued (some of these having tried to stop and failed).
In all 6% of BC2 women had used drugs during some or all of their pregnancy. There were no specific questions as to which drugs were used during pregnancy, only 'ever' (life-time) use, and use in past 12 months (the latter would have included the last month or two of pregnancy for those 3% continuing throughout, but would not have included the 3% who stopped in the early stages). For the 59 BC2 women who took drugs at all during pregnancy, the drugs they had cited for use 'ever' were: cannabis (87%), methadone (36%), amphetamines (36%), heroin (32%), ecstasy (31%), cocaine (28%), LSD (16%), crack (14%) and 'other' (9%). In all, 19 women (weighted 21) who had been using drugs during pregnancy received treatment/ help/advice from a range of sources.
3.6 Antenatal classes
Attendance by mother
Attendance by the pregnant women at antenatal classes became less common between the two cohorts, and fewer classes attended are NHS, as shown in Table 3.5. However, when attendance at classes was examined separately for those who were first-time mothers, versus those who had an older child, it was found that the proportion of firs-time mothers attending classes was essentially unchanged between cohorts (71% of BC1 compared with 69% of BC2). However, there was a statistically significant decline in the percentage of mothers with other children attending classes (20% compared with 13%).
Table 3.5 Attendance at antenatal classes by mother (BC1 & BC2)
| Frequency | BC1 % | BC2 % |
|---|---|---|
| Yes, went to all or most classes | 34 | 29 |
| Yes, but only went to some classes | 11 | 11 |
| No, did not attend any | 54 | 60 |
| Base: all families where mother was respondent | 5139 | 5996 |
| Type of class | ||
| NHS | 97 | 93 |
| Other | 2 | 4 |
| Both | 2 | 4 |
| Base: all who attended antenatal classes | 2366 | 2423 |
Over half of all mothers did not attend antenatal classes, and the reasons given are shown in Table 3.6. An asterisk against a reason indicates that the difference in percentage between the cohorts is statistically significant. For BC2, there has been an increase in non attendance 'because classes are not available' (from 2% to 4%), and 'for other reasons' (from 31% to 44%).
Table 3.6 Reasons for mother not attending antenatal classes (BC1 & BC2)
| BC1 % | BC2 % | |
|---|---|---|
| Done for previous pregnancy | 47 | 50 |
| Not needed | 29 | 28 |
| Do not like classes/groups* | 12 | 9 |
| Did not know of any | 5 | 5 |
| No childcare | 4 | 3 |
| None available* | 2 | 4 |
| Travel problems | 3 | 2 |
| Cost problems | >0 | >0 |
| Other reasons* | 31 | 44 |
| Base: all who did not attend antenatal classes | 2768 | 3568 |
Multivariate logistic regression showed that attendance at antenatal classes is strongly associated with all the socio-demographic variables (even after mutual adjustment for each other), other than for the urban-rural classification. The odds of attendance are most increased (19-fold) if there are no older children, but also significantly increased if there is more extended education, greater household income, less deprivation and older age, and if white ethnicity. Finally, after adjustment for all these socio-demographic variables, the effect of cohort is highly statistically significant, and indicates a reduction in antenatal class attendance across the time-span between the two cohorts as first suggested in Table 3.5.
Attendance by father
This analysis was restricted to children whose mothers attended antenatal classes (at least to some extent), because the question pertaining to fathers was asked only if the mother reported attending. There has been a marginal increase in attendance at antenatal classes by the father, increasing from 66% in BC1, to 68% in BC2. Among fathers who did attend, Table 3.7 shows the frequency of attendance across the 'course', ie. the planned set of classes offered. There has been minimal change in the shape of this distribution of responses between cohorts.
Table 3.7 Attendance at antenatal classes by father (BC1 & BC2)
| BC1 % | BC2 % | |
|---|---|---|
| Yes all classes | 41 | 40 |
| Yes most classes | 23 | 25 |
| Yes some | 37 | 35 |
| Bases (all where partner attended antenatal class) | 1554 | 1673 |
3.7 Sources of information
Table 3.8 displays the sources of information mothers used when pregnant and indicates with asterisks the sources for which the percentages have changed significantly across the two cohorts. Almost all women use health professionals as a source of information, but this percentage has decreased from BC1 to BC2 (from 92% to 90%). The most dramatic increase has been for internet-based sources, which has more than doubled (increase from 27% to 55%), while use of books and magazines has fallen (from 48% to 35%).
Table 3.8 Sources of information when pregnant for questions/concerns
| BC1 % | BC2 % | |
|---|---|---|
| Health professionals* | 92 | 90 |
| Family or friends | 70 | 71 |
| Books/magazines etc* | 48 | 35 |
| Ready Steady Baby book | 46 | 48 |
| Other mothers | 29 | 31 |
| Internet* | 27 | 55 |
| TV radio | 13 | 7 |
| Not applicable - no concerns | 2 | 1 |
| Base: all families where mother was respondent | 5139 | 5996 |
Women were also asked to select what they felt was the most useful source for them, and the distribution of responses for this is given in Table 3.9. There has been a marked change between the two cohorts, with health professionals less often being identified as most useful source (down from 53% to 47%), and similarly for books/magazines (decreased from 10% to 4%), while believing the internet the most useful has increased from 5% to 14%.
Table 3.9 Most useful source of information when pregnant
| BC1 % | BC2 % | |
|---|---|---|
| Health professionals | 53 | 47 |
| Family and friends | 19 | 20 |
| Books/magazines | 10 | 4 |
| Ready Steady Baby leaflet | 9 | 11 |
| Internet | 5 | 14 |
| Other mothers | 3 | 4 |
| TV radio | 1 | >0 |
| Base: those who used more than one source | 4430 | 5133 |
Use of the internet as a source of information is strongly associated with all the socio-demographic variables other than ethnic group. The odds of using the internet for information increases with household income, level of education, and with more urban dwelling, but reduces with increasing deprivation. With respect to age, the odds are lowest in the youngest age group and highest in 30 to 39 years olds. Finally, with all other variables adjusted for, the odds of using the internet for pregnancy information are higher in cohort 2, by 260%.
3.8 The birth
Type of delivery
The mode of delivery can be associated with various birth outcomes for both the mother and child. A range of work associated with the Keeping Childbirth Natural and Dynamic Campaign and the Maternity Services Action Group has sought to reduce the number of caesarean sections performed by improving antenatal and perinatal care to be more anticipatory of those at higher risk.
There was a statistically significant change in type of delivery between BC1 and BC2 (Table 3.10), with 'normal' deliveries decreasing from 62% to 60%, and elective caesarean increasing from 12% to 14%.
| BC1 % | BC2 % | |
|---|---|---|
| Normal | 62 | 60 |
| Forceps | 7 | 9 |
| Ventouse | 4 | 2 |
| Forceps & ventouse | 2 | 1 |
| Caesarean section prior to onset of labour | 12 | 14 |
| Caesarean section after onset of labour | 13 | 13 |
| Base: all families where mother was respondent | 5138 | 5995 |
Delivery at due date
The woman's account of the timing of her delivery in relation to due date was very similar across the two cohorts, as shown in Table 3.11.
Table 3.11 Gestation at delivery
| BC1 % | BC2 % | |
|---|---|---|
| Weeks early | 23 | 24 |
| Days early | 18 | 18 |
| On time | 14 | 14 |
| Late | 45 | 45 |
| Base: all families where mother was respondent | 5141 | 5997 |
Birthweight
The mean birthweight has very slightly increased across the two cohorts, from 3376g to 3391g, giving a mean increase 14.5g (95% CI -11.4g to 40.4g). The distribution of birthweights for the two cohorts is shown in the box plot of Figure 3.2. The 'boxes' plot the middle 50% of each distribution (vertically encompassing the lower to upper quartiles), while the thick line across the box indicates the median. The additional circles and asterisks plotted show the upper and lower tails of the distributions, that is, the upper and lower 25% of infant weights. Visual comparison of these box-plots shows very little change in birthweight distribution across the time-interval between the two cohorts, but suggests some stretching of the upper tail of the distribution for BC2 to include a number of heavier birthweights.
Figure 3.2 Box-plot of the distributions of birth weight (g) in the two cohorts
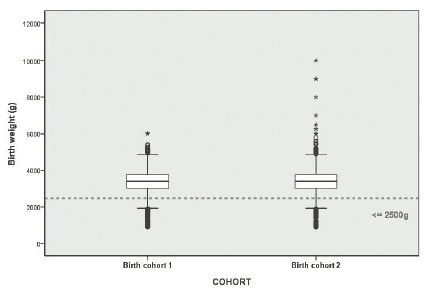
Base - all children: BC1 = 5199, BC2 = 6109
Clinical judgement of gestation at birth is not available for analysis, but maternal recollection of the timing of birth relative to due date was ascertained at interview - as presented in Table 3.11. There was a strong association of birthweight with this timing variable such that the mean weight for babies born early, compared to those 'on time', was 510g lower if 'weeks' early, and 83g lighter if 'days' early, while for babies born late the mean weight was 192g heavier.
The prevalence of 'low birthweight' (<2500g) babies was almost identical across the two cohorts (7%), and as would be expected was strongly associated with recalled timing of birth (overall, 25% LBW if 'weeks early', 3% if 'days early' or 'on time', and <1% if 'late'). The distributions were almost identical in the two cohorts. Low birthweight is strongly associated with older maternal age, no educational qualifications, lower household income, and 'other' ethnic group. Low birthweight is also strongly associated with type of delivery, being most common in elective caesarean deliveries.
3.9 Summary
The main reason for collecting the pregnancy and birth data within GUS is as a context for later development of and outcomes for the child. The fact that only live births can progress to be BC2 participants, means that the GUS data is not representative of all births in Scotland in 2010/11. Furthermore, the fact that first interviews took place when BC2 babies were 10 to 11 months old, means that details of the pregnancy, antenatal care and information sources are subject to a considerable recall interval. For this reason only fairly imprecise information can be gained about, for example, gestation at birth, and so there is no possibility of examining a standard outcome such as birthweight adjusted for gestation. However there are plans to link GUS data to the NHS maternity health record, in the near future, which will provide an opportunity to obtain prospectively-collected and more accurate clinical information about the pregnancy and birth.
In absolute terms there have been, generally, very small changes in outcomes for BC2 compared with BC1. Improvement was observed in that more BC2 mothers reported not drinking alcohol during pregnancy, but on the other hand fewer BC2 births were described by the mothers interviewed as 'normal' and fewer BC2 mothers overall attended antenatal classes (although there was no change for first time mothers).
The first Framework for maternity care in Scotland (Scottish Government, 2001) noted that social factors have a far-reaching impact on maternal health and the recently published 'refreshed' framework (Scottish Government, 2011) commented on the many complex and interlinked determinants of health. Multivariate modelling with respect to use of supplements in pregnancy, attendance at antenatal classes, and use of the internet as a source of information, gave results that are in line with these statements - showing strong evidence
of inequalities in health behaviours and access to information.
3.10 References
Scottish Executive (2001) A Framework for maternity services in Scotland, Edinburgh: Scottish Executive - Health Department
Scottish Executive (2000) Our national health a plan for action, a plan for change, Edinburgh: Scottish Executive - Health Department
Scottish Government (2008) Equally Well report of the Minsterial task force on inequalities in health, Edinburgh: Scottish Government
Scottish Government (2008) Achieving our potential, Edinburgh: Scottish Government
Scottish Government (2009) Early Years Framework, Edinburgh: Scottish Government
Scottish Government (2011) A refreshed framework for maternity care in Scotland, Edinburgh: Scottish Government.
Contact
Email: Sharon Glen