GMS contract: 2018
This document is intended primarily to provide an accessible explanation to Scotland’s GPs of the changes we propose to effect in regulations.
4 Manageable Workload
Key Points
- GP and GP Practice workload will reduce.
- New staff will be employed by NHS Boards and attached to practices and clusters.
- Priorities include pharmacy support and vaccinations transfer.
- Changes will happen in a planned transition over three years when it is safe, appropriate and improves patient care.
- There will be national and local oversight of service redesign and contract implementation involving SGPC and Local Medical Committees.
Introduction
We know that workload is currently one of the most challenging aspects of being a GP. We are introducing measures to address this by:
- continuing to reduce contractual complexity
- improving primary/secondary care interface working
- building a wider primary care multi-disciplinary team
Reducing contractual complexity
The process of reducing the contractual complexity of the Scottish GMS contract has already begun.In 2015 the Scottish Government and the SGPC announced that Scotland would become the first country in the UK to remove the Quality and Outcomes Framework ( QOF). QOF no longer incentivised the direction of travel needed with respect to demographic change (an ageing population and increasing multi-morbidity), because the disease specific, procedural basis of QOF encouraged diseases to be viewed separately. This was counter to the holistic, person-centred care required for the increasing numbers of people with multiple long term conditions.
In April 2016, the remaining 659 QOF points were retired and transferred to the general practice core standard payments, signalling one of the first steps towards the development of the new contract, and a significant shift towards placing greater trust in the clinical judgment and professionalism of GPs.
Transitional arrangements for quality assurance were introduced in the Statement of Financial Entitlements 2016/17 alongside the removal of QOF. These included early instructions for the creation of GP clusters in Scotland, setting the direction for the new contract.
Other arrangements have also been improved while the new contract was being developed. These include removing the discretionary element for parental leave and sickness leave locum cover payments so all eligible GP practices will receive these payments. We have also created an occupational health service that all GPs and GP practice staff can access, and improved the re-imbursement rate for appraisals.
The new contract will build on these improvements to further reduce contractual complexity. Some of the proposed simplification of the contractual landscape was set out in chapter two. Our proposed changes to the GMS regulations will include updates on dispute resolution, closing practice lists and defining the practice boundary. These changes are described more fully in chapter eight.
Improving interface working
- To ensure effective working between primary and secondary care, we will continue to implement the recommendations of the Improving General Practice Sustainability Advisory Group as set out in its report on November 2016.
Within the recommendations there are a number of broad themes including effective primary and secondary care interface working. Interface working will be better achieved through well-functioning primary and secondary care interface groups. These groups will support NHS Boards and HSCPs to reduce GP workload and provide a better patient experience by removing the need for GP involvement when it is not clinically necessary. The recommendations include:
- Improved processes for routine follow-up of hospital procedures and results of tests
- Allow the issuing of fit note certificates by secondary care providers at the time of discharge, where the condition being treated is the sole cause of a temporary disability
- More efficient use of the primary care multi-disciplinary team by ensuring secondary care staff request patient visits by the most appropriate professional for their condition e.g. social care or district nurse
- Changes to the referral pathway for patients who do not attend ( DNA) hosptial appointments to remove the need for GP referrals
Building the primary care multi-disciplinary team
In line with commitments to be made in the MOU referred to in chapter one, HSCPs and NHS Boards will place additional primary care staff in GP practices and the community who will work alongside GPs and practice staff to reduce GP practice workload.
Practices will be encouraged to use the additional capacity created by reducing GP provided services to focus on activities that directly support GPs as expert medical generalists. We will increase protected time to allow GPs to maintain and develop their training and skills, and those of their practice teams.
Service Redesign – 2018-2021
To enable and empower GPs to function as expert medical generalists, non-expert medical generalist workload needs to be redistributed to the wider primary care multi-disciplinary team, ensuring that patients have the benefit of the range of expert advice needed for high quality care.
Local areas are already beginning to reconfigure primary care by redistributing workload to the multi-disciplinary team as capacity becomes available.
An MOU between these local commissioning and delivery partners, the SGPC and Scottish Government is in development. It sets out agreed principles of service redesign, identified ring-fenced resources to enable the change to happen, national and local oversight arrangements, and the priorities for the transfer of responsibility for service delivery.
These agreed principles include patient safety and person-centred care. Patient engagement in the planning and delivery of new services will be critical to their success.
It is intended that GPs will become better embedded in HSCPs as senior clinical leaders working in collaboratively with managers to achieve better outcomes for patients. [14]
To help ensure sufficient, visible change in the context of a new contract, we have agreed to focus on a number of specific services to be reconfigured at scale across the country. These include:
- vaccinations services;
- pharmacotherapy services;
- community treatment and care services;
- urgent care services; and
- additional professional clinical and non clinical services including acute musculoskeletal physiotherapy services, community mental health services and community link worker services.
To ensure the continued delivery of high quality, safe, person-centred care, the transition will happen over an agreed period of time.
Primary Care Improvement Plan
Each of the 31 HSCPs in Scotland will develop a Primary Care Improvement Plan which will outline how these services will be introduced before the end of the transition period in 2021. These Plans will be overseen by a GMS Oversight Group with representation from the Scottish Government, the SGPC, HSCPs and NHS Boards. This group will be formed to oversee implementation by NHS Boards of the Scottish GMS contract and implementation by the HSCPs of the Primary Care Improvement Plans. Plans will include clear milestones for the redistribution of GP workload and the development of effective primary care multi-disciplinary team working.
As well as the requirements on the HSCPs to develop Primary Care Improvement Plans, NHS Boards with HSCPs will develop clear arrangements to deliver the commitments in respect of the new Scottish GMS contract. These arrangements include the priority areas of service redesign set out below and must be agreed with the local GP Subcommittee of the Area Medical Committee and the Local Medical Committee ( LMC).
Leadership and management
Under the new contract GPs will be concentrating on their role as expert medical generalists with a focus on improving outcomes for patients. There is an explicit understanding that part of this role will be senior clinical leadership of the multi-disciplinary teams.
Line management of much of the primary care multi-disciplinary team staff will be provided through the employing authority (usually NHS Boards). This will include the provision of employee support, training, cross cover and cover for holidays and other absences. The purpose of the line management is to support staff in their role as a member of the primary care multi-disciplinary team attached to one or more practices and their patient lists.
While all professionals involved in patient care have a leadership role to play, the senior clinical leadership role of doctors will be outlined in the GP role in Primary Care Improvement Plans. Not all GPs will feel that they have all the skills to undertake this role, but training will be available and be part of core curricula in the future. Leadership which is intended to improve outcomes for patients will clearly require collaborative working with a wide variety of professionals who will be involved in primary care multi-disciplinary teams. Various members of these teams will also undertake leadership roles to achieve changes and improvements.
There are many examples of effective teams whose membership have different employers. Many GPs will have had experience of this with district nurses and other professionals not directly employed by their practice. The MOU is a clear statement of intent to deliver this form of team working. We have agreed shared principles to ensure these teams operate in optimum ways to the benefit of patient care.
Some of these primary care multi-disciplinary team members will be attached to individual practices but inevitably, in some cases, resources may have to be shared between different practices. GP clusters will have an important role in facilitating cross practice working including developing common working practices and pathways.
We believe that the best way to deliver relationship-based care to patients is through the effective relationships between the members of these primary care multi-disciplinary teams.
Vaccination Services
In 2017, as part of the commitment to reduce GP workload, the Scottish Government and SGPC agreed vaccinations would progressively move away from a model based on GP delivery to one based on NHS Board delivery through dedicated teams. The Vaccinations Transformation Programme is reviewing and transforming how we deliver vaccinations in Scotland. Delivery will move away from the current position of GP practices being the preferred provider of vaccinations on the basis of national agreements.
The vaccination services delivered by the programme will form part of the Primary Care Improvement Plan in each area. It is expected that each area will make meaningful progress over the first two years of transformation to demonstrate commitment to the change.
The aim of the programme is to reduce workload for GPs and their staff. This will mean that other parts of the system, with primary care multi-disciplinary teams, will begin to deliver vaccination services instead of GPs. This will be a step towards enabling GPs to focus their time on expert medical generalism, whilst ensuring that patients’ needs are met through the reconfiguration of services which will make the best use of the mix of skills in primary care. How this programme is delivered will vary regionally, depending on local circumstances and factors.
The funding that was historically associated with the delivery of vaccinations will remain within general practice. An additional £5 million is being invested in 2017 to start the Vaccination Transformation Programme ahead of the delivery of the proposed new contract.
The Vaccination Transformation Programme will draw in expertise from across the NHS and will take three years to complete. Transition to the new model will be planned to ensure that it can operate safely and sustainably, and changes will be made only in line with an agreed process (detailed in the Primary Care Improvement Plans).
The Vaccination Transformation Programme can be divided into different work streams:
1. pre-school programme
2. school based programme
3. travel vaccinations and travel health advice
4. influenza programme
5. at risk and age group programmes (shingles, pneumococcal, hepatitis B)
We expect HSCPs and NHS Boards to have all of these programmes up and running by the end of the 3-year transition period - in April 2021. The order and rate at which HSCPs and NHS Boards make the transition may vary but progress is expected to be delivered against milestones in each of the 3 years.
1) Pre-school programmes in NHS Board areas such as Lanarkshire and Tayside are already established. This is a complex, time-critical programme and HSCPs and NHS Boards that do not currently provide this service will, early on in the transition period, prioritise the adoption of lessons learned from service delivery and workforce development in those areas that have already introduced the service.
2) The school based programme is already established across all areas delivering influenza vaccine and HPV vaccine to girls.
3) Travel vaccinations and travel health advice are currently a significant time burden on GP practices and the Vaccination Transformation Programme will prioritise optimal alternative options for re-provision in the first year.
4) The influenza programme will tackle the seasonal challenge of delivering to those in certain age categories and those at particular high risk. HSCPs will plan how they deliver vaccinations to the high volume over 65 category. Pre-school and school age children could have this vaccination delivered by their respective programmes. Consideration needs to be given to particular risk groups such as pregnant women and adult at-risk groups, and how vaccines can be provided in a way that is safe efficient and acceptable to patients.
5) For at risk and age group programmes , consideration needs to be given to providing relevant vaccines to eligible patients in a way that is safe, acceptable, and which maintains, or increases uptake.
Pharmacotherapy Services
Multi-disciplinary team working is crucial to reducing GP workload. The proposed contract includes an agreement that every GP practice will receive pharmacy and prescribing support.
The GP Pharmacy Fund has already enabled 160 pharmacists and 34 pharmacy technicians to be appointed to posts in over one third of GP practices across Scotland.
We are investing £12m in the GP Pharmacy Fund in 2017/18. We intend that investment in this service will continue under the new contract to allow more pharmacists and pharmacy technicians to work in general practice, reducing GP workload and improving patient care.
As part of the proposed contract, we would also introduce a new pharmacotherapy service to allow GPs to focus on their role as expert medical generalists, improve clinical outcomes, more appropriately distribute workload, address practice sustainability and support prescribing improvement work.
Case Study – Pharmacy support in Caithness
Pharmacists and pharmacy technicians are already developing an increased, specialised role within primary care multi-disciplinary teams. They are well placed to support GPs to focus on their role as expert medical generalists by ensuring workload is distributed more appropriately, undertaking prescribing improvement work, and providing medication reviews and specialised clinics.
In Caithness in NHS Highland, pharmacist prescribers are embedded in the primary care MDT. One pharmacist, who works in a GP practice with 5,447 patients, has taken over all the medication reviews that were previously provided by the practice GPs, and completed a total of 2,811 reviews in an 18-month period. This includes re-authorising repeat prescriptions and transferring suitable patients to serial prescribing. They also triage all daily acute requests, carry out all medicines reconciliation for hospital discharges and clinic letters and manage individual patients requiring more intensive medicines input, such as dose titration of a pain medicine. Caithness pharmacists also provide domiciliary medication reviews for patients in care homes and patients receiving care at home, reducing the number of visits required by GPs.
The pharmacist input has resulted in a marked reduction in GP time spent on medicines-related activities, enabling them to focus on other activities. Patient response has also been overwhelmingly positive.
“Having an in-house pharmacist has shown many benefits for patients including reducing polypharmacy, being able to monitor more closely patients on high risk medications, and supporting patients though medication changes after hospital discharge.” GP, Caithness
From April 2018, there will be a three year trajectory to establish a sustainable pharmacotherapy service which includes pharmacist and pharmacy technician support to the patients of every practice. This timeline will provide an opportunity to test and refine the best way to do this, and to allow for new pharmacists and pharmacy technicians to be recruited and trained.
In order to increase the pool of qualified pharmacists to provide the pharmacotherapy service, additional funding has been secured to increase the number of pharmacist training posts from 170 to 200 per year from 2018/19. This will ensure that there is sufficient capacity to deliver the pharmacotherapy service within the proposed timescales.
By April 2021, every practice will benefit from the pharmacotherapy service delivering the core elements as described below. Some areas will also benefit from a service which delivers some or all of the additional elements described below. The level of additional services available in different areas will be dependent on workforce availability which will build throughout the three years leading up to 2021 and beyond.
Figure 2: Core and additional pharmacotherapy services
| Core And Additional Pharmacotherapy Services |
||
|---|---|---|
| Pharmacists |
Pharmacy Technicians |
|
| Level one |
Acute and repeat prescribing requests includes/authorising/actioning:
|
|
| Level two |
|
|
| Level three |
|
|
As outlined in the MOU, the pharmacotherapy service will evolve over the three year transition, with pharmacists and pharmacy technicians becoming embedded members of the core practice clinical teams. While not employed directly by practices, the day-to-day work of pharmacists and pharmacy technicians will be co-ordinated by practices. Pharmacists and pharmacy technicians will take on responsibility for:
a) Core elements of the service, including: acute and repeat prescribing, medicines reconciliation, monitoring high risk medicines
b) Additional elements of the service, including: medication and polypharmacy reviews and specialist clinics (e.g. chronic pain)
Figure 3: Integrated pharmacotherapy service
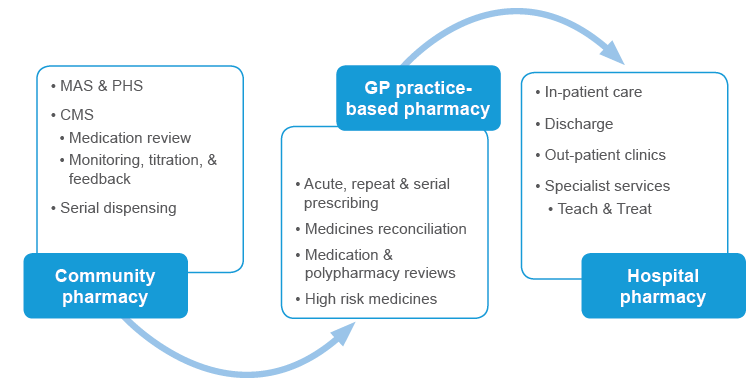
Community Treatment And Care Services
Community treatment and care services include many non- GP services that patients may need, including (but not limited to):
- management of minor injuries and dressings
- phlebotomy
- ear syringing
- suture removal
- chronic disease monitoring and related data collection.
There will be a three year transition period to allow the responsibility for providing these services to pass from GP practices to HSCPs. By April 2021, these services will be commissioned by HSCPs, and delivered in collaboration with NHS Boards that will employ and manage appropriate nursing and healthcare assistant staff. Phlebotomy will be delivered as a priority in the first stage of the Primary Care Improvement Plans.
Local circumstances and demand will determine where it is most appropriate to safely situate these services. It is expected that many of these functions will be provided in the GP practice premises for patient convenience and the benefits of having these services carried out with the close support of the wider practice team. This would also enable easier sharing of necessary data and the patient records.
In some areas, (for reasons of premises, practicality or geography) the NHS Board may operate these services from separate facilities. The principles agreed by the parties to the MOU will ensure that patient safety, person-centred care and sustainability remain at the heart of these services as they develop, wherever they are delivered.
Patients should be able to conveniently and confidently access community treatment and care services. In some circumstances it may be appropriate for certain GP practices, such as small remote and rural GP practices, to locally agree to deliver these services. If GP practices locally agree to deliver community treatment and care services, then support will be provided in the form of either expenses for the required practice employed staff capacity, or the deployment of NHS Board employed staff.
It is expected that community treatment and care services will be available for use by primary and secondary care. For example, pre-hospital clinic bloods could be carried out for a requesting consultant without having to involve the GP practice staff. The consultant’s name would be on the test result to avoid unnecessary GP involvement.
It will be clear in the agreement represented by the MOU that local arrangements will determine how services will be provided. This will help to remove the responsibility for service provision away from GPs to the HSCPs, allowing GPs to focus upon their expert medical generalist role. NHS Boards and HSCPs will work with practices to plan and manage service transfers in a way that ensures patient safety and maximises benefits to patient care.
Delivery of the Vaccination Transformation Programme, pharmacotherapy service and community treatment and care service are priorities, and responsibility for these services will be transferred to HSCP by the end of the transition period in April 2021. Within that timeframe, delivery at a local level will vary based on local factors such as the extent to which comparable services are already in place, upon local geography, and prioritisation based on local demographics and demand.
Urgent Care Services
In addition to these priorities, the MOU will support the redesign of other services to reduce GP workload and free up GPs capacity to focus on their expert medical generalist role. These redesigned services will focus on urgent and unscheduled care, and developing the roles of other clinical and non-clinical professions, working in the practice, to support physical and mental health.
The Scottish Government and SGPC have agreed that another area of GP workload that needs to be addressed is urgent unscheduled care including the provision of advanced practitioner resource as first response for home visits.
A number of tests of change in Scotland over the last two years have focused on the role of Scottish Ambulance Service ( SAS) paramedics in primary care. Evidence from pilots in Inverclyde, Hawick and Kelso shows that support (such as responding to urgent call out to patients) allows GPs to provide more appropriate patient care. Relevant support includes advanced practitioner resource, such as a nurse or a paramedic, for GP clusters and GP practices, serving as first response for home visits.
The MOU will support the implementation of sustainable advance practitioner provision in all HSCP areas, based on local service design. These practitioners will assess and treat urgent or unscheduled care presentations. This will allow GPs to focus on scheduled appointments with patients most in need of their skills as expert medical generalists. Where service models are sufficiently developed, advanced practitioners will also directly support GPs expert medical generalist work by carrying out routine assessments and monitoring of chronic conditions for vulnerable patients at home, or living in care homes.
It is expected that the workload for paramedics would mean that most GP practices would not have sole access to a paramedic. It is likely that paramedics would work across a number of GP practices to meet patient needs. GP clusters will play an important role in enabling this service to ensure effective working and good patient outcomes.
Paramedics and specialist paramedics can practice in all aspects of urgent, unscheduled, and emergency presentations as needed, underpinned by GP review and consultation with the GP and wider multi-disciplinary team where required. A specialist paramedic in urgent and emergency care is a paramedic who has undertaken, or is working towards a post-graduate certificate in Specialist Paramedic Practice. They will have acquired, and continue to demonstrate an enhanced knowledge base, complex decision making skills, and competent judgement in urgent and emergency care. Paramedics (as non-specialists) can also provide care and support to patients in primary care, both in and out of hours as part of a wider primary health and care team.
Case Study – Paramedic Support in Inverclyde
Part of the Inverclyde tests of change included SAS supported transformational change in GP clusters. Regent GP practice in Greenock piloted paramedic support in general practice using a Trainee Specialist and a Paramedic; and Gourock Health Centre retained a Specialist and a Paramedic.
Baseline data was collected for the month of June 2017. In that month, GPs carried out 102 home visits from Regent practice and 106 from Gourock. The average time taken for visits was 34 minutes. This includes travel time and updating patient records. In the first three months following paramedic support to practices being put in place, the percentages of home visits carried out by GPs reduced by over 60%. In addition to home visits, paramedics are also able to assess urgent presentations within the surgery. Referral rates to secondary care are very similar between GPs and paramedics. The most common conditions seen are acute respiratory illness, abdominal and back pain, UTIs and falls. Feedback from staff and patients so far has been positive. The GPs report they are happy with how the model is working and relationships between the professional groups continue to develop.
Additional Professional Services
Additional professional roles will provide services for groups of patients with specific needs that can be delivered by clinicians other than GPs, serving as first point of contact in the practice setting as part of the wider multi-disciplinary team. These include (but are not limited to) physiotherapy services, community mental health services and community links worker services.
Physiotherapy services focused on musculoskeletal conditions
Musculoskeletal problems frequently cause repeat appointments and are a significant cause of sickness absence in Scotland. The majority of a GP’s musculoskeletal caseload can be seen safely and effectively by a physiotherapist without a GP referral. However the existing patient pathway often includes an unnecessary delay while initial non-physiotherapeutic solutions are attempted prior to access to a musculoskeletal physiotherapy service. There are variable waiting times across the country for access to face-to-face physiotherapy.
Physiotherapists are already well situated to work collaboratively with primary care multi-disciplinary teams and support the GP role as a senior clinical leader. Physiotherapists are an expert professional group. They have a high safety record and are trained to spot serious pathologies and act on them. Physiotherapists utilise their wider knowledge and skills as part of their assessment. A first point of contact service could also be seen in the context of the wider muscoloskeletal pathway.
Under the new contract, HSCPs will develop models to embed a musculoskeletal service within practice teams to support practice workload. In order to provide a realistic alternative for patients, access times must be comparable to those of general practice. Priority for the service, such as focusing on elderly care, will be determined by local needs as part of the Primary Care Improvement Plan.
Case Study – Physiotherapy services in Inverclyde
Inverclyde piloted the use of an Advanced Practice Physiotherapist ( APP) as an alternative first point of patient contact within the GP practice. Since August 2016, an APP has worked in three GP practices with a total patient list of 14,000. Reception staff at each practice were trained to offer patients APP appointments where appropriate. To date the APP has provided over 1000 consultations, most of which would otherwise have been GP appointments. 94% of patients were seen once and did not need a further appointment with the physiotherapist.
GPs at one participating practice, Lochview practice in Greenock, noted a number of benefits. By seeing the majority of patients with musculoskeletal conditions the APP has freed up GP appointments. GPs are able to use their time more effectively by focusing on patients more in need of their expertise, and are spending more of their patient facing time on complex care needs. In qualitative evaluation, the pilot was rated highly by GPs, practice staff and patients, with patient feedback in particular being extremely positive.
‘Of all the work that’s ever been done in GP practices, this has been the one that feels like it has truly taken work away. Patients are safer – there is quicker access to the most appropriate intervention because triage assessment conducted by the physiotherapist gets people to the right place sooner’.
( GP, Greenock)
Community mental health services
Community clinical mental health professionals (eg nurses, occupational therapists), based in general practice, will work with individuals and families assessing their mental health needs, providing support for conditions such as low mood, anxiety and depression. The outcome sought is improved patient care through rapidly accessible, appropriate and timely mental health input.
Community Links Worker Services
A Community Links Worker ( CLW) is a non-clinical practitioner based in or aligned to a GP practice or cluster who works directly with patients to help them navigate and engage with wider services. They often serve a socio-economically deprived community or assist patients who need support because of for example, the complexity of their conditions. As part of the Primary Care Improvement Plan, HSCPs will develop CLW roles in line with the Scottish Goverment’s manifesto commitment to deliver 250 CLWs over the life of the Parliament. The roles of the CLWs will be consistent with assessed local need and priorities and function as part of the local models of care and support.
Rural support
The rural and remote GP shares much of the same generalist workload as their colleagues in urban areas. In many areas, being a rural GP means being the expert medical generalist providing the broadest range of skills because of their remoteness, because they usually have smaller primary care teams and because the locality services that may be available in areas with larger populations may not be available.
Many remote and rural GPs have chosen to work where they do in part because it fits with their desire to provide a more complete primary care service to their patients and see delivery of some services as welcome opportunities to engage with their patients. In some rural areas where there are larger list sizes, there will be the opportunity to move the responsibility for some services like immunisations to reduce workload pressures.
The service redesign described above requires practices to be involved via their GP clusters, so they have a say in how services will work locally.
Workforce
The introduction of the services described above relies on the establishment of a new workforce which will be part of practice teams but not employed by practices. These practice-attached staff will be largely employed by NHS Boards, embedded in practice teams with their day-to-day work co-ordinated by the practice.
Patient safety will be fundamental in delivering this workforce at scale. Taking the paramedic support service as an example, at all stages of the roll-out, we will ensure the capacity and capability of the workforce is sufficient. This means that the safety of patients requiring urgent unscheduled care is assured and core Scottish Ambulance Service performance is protected. This will require consistent and reliable provision of paramedic staff working in primary care teams, with appropriate training and education, supervision and support arrangements. Positive relationships between colleagues in the primary care multi-disciplinary teams will be crucial. This approach to attached staffing will be taken in the development and roll-out of all services – the principles for which are outlined in the MOU.
Further detail on delivering this new workforce will be set out in the Scottish Government National Health and Social Care Workforce Plan: Part 3 Primary Care.
As this chapter sets out, an expanded primary care multi-disciplinary team will bring substantial workload benefits to GPs and deliver better services and outcomes to patients. As well as improvements to workforce we will introduce measures to reduce risk and improve infrastructure in general practice. These are explained in chapter five.