Attend Anywhere / Near Me video consulting service evaluation 2019-2020: report
This report presents the findings of an external evaluation of the Attend Anywhere / Near Me video consultations service used across health and care services in Scotland
Executive Summary
Introduction
Attend Anywhere is a video consultations service used across health and care services in Scotland. In July 2019 the Scottish Government commissioned the University of Oxford (Department of Primary Care Health Sciences) to undertake an independent evaluation of the service. The aim of the evaluation was to review progress and achievements in relation to the use and outcomes of Attend Anywhere, and to develop an understanding of the implementation experience to date. We also sought to make recommendations relevant to any future scaling-up, spread and sustainability of Attend Anywhere and similar digital services. The field work was done between August 2019 and early March 2020, before the COVID-19 outbreak.
Attend Anywhere is the name of the video consultations platform, purpose-built to meet the needs of the health and care sectors, for which a national licence has been procured for Scotland.
Near Me is now the public-facing name used to describe video consulting services provided via the Attend Anywhere platform in Scotland. This name was developed by patients in NHS Highland, and was not in universal use across Scotland at the time of the fieldwork for this evaluation.
For the purposes of this evaluation report, the term 'Attend Anywhere' is generally used, unless research participants referred specifically to 'Near Me'.
Background
Attend Anywhere was launched in Scotland in December 2016 as part of a wider national Technology-Enabled Care (TEC) programme, which aimed to drive the widespread adoption of technology to help plan and improve health and care services and outcomes for citizens. The TEC programme was set up to respond to the need for service transformation in the context of rising demand for health and social care; and to re-engineer services and care pathways in a more person-centric way. A key objective is to improve citizen access to health and care services from remote parts of Scotland. Attend Anywhere is intended for use by both health and social care organisations, and by both primary care (community-based health services including GPs) and secondary care (mainly hospital services). However at the time of this evaluation most activity was hospital-based, on which this report therefore has a strong focus.
The Attend Anywhere video consultations platform works via the internet. People can access a video clinic through a device, such as a laptop computer, mobile smartphone or tablet, provided that they use specified internet browsers. People use an internet link to access a 'virtual' online waiting area, where service providers meet them and provide the video consultation. This process has been designed to align with the ways in which people usually attend face to face appointments, and with established health and care processes and workflows. This is illustrated in the diagram below.[1]
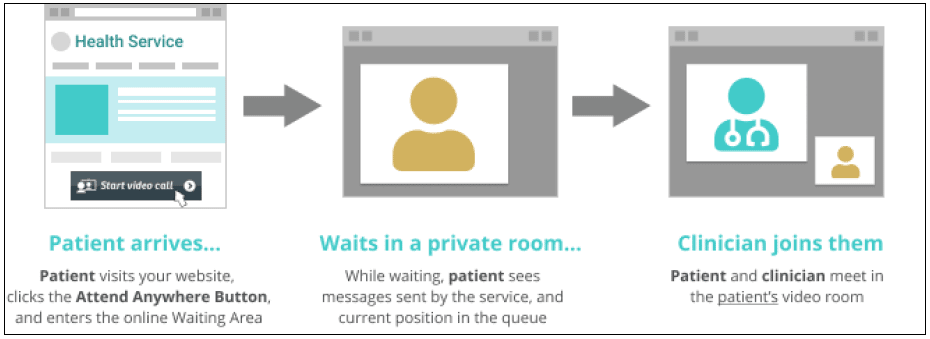
Research Methods
The evaluation used mixed-method (mainly qualitative) methodology, structured and guided by a multi-level theoretical model (NASSS: non-adoption, abandonment and challenges to spread, scale-up and sustainability [1]), developed to explain individual and organisational challenges to adoption and sustained use of technology-supported programmes in health and care.
Between August 2019 and early March 2020, we undertook research with seven of the 14 local territorial Health Boards in Scotland, six of which we visited in person. These boards were selected to explore variation of experience in different geographical areas (urban, rural, islands) and in boards with higher and lower use of Attend Anywhere. We visited 11 sites across Scotland (10 hospitals, one GP surgery), conducted remote interviews with staff from a further 17 sites (7 hospitals, 7 GP practices, 2 community settings and one third-sector organisation), and observed some video consultations. We also met and interviewed senior-level stakeholders. In total, we conducted 140 interviews with doctors, nurses, allied health professional, healthcare and third sector support workers, clinician and non-clinical managers, administrators, IT support staff, patients and their relatives, and national-level stakeholders (government, policy implementation, professional leaders, industry). The report also incorporates routinely-collected data on uptake of the service in different localities, extracted from the Attend Anywhere system.
We analysed data thematically, combining descriptive quantitative data with synthesized qualitative themes. Draft findings were presented to study participants in face-to-face and virtual meetings in February 2020 and a draft report was shared with the Scottish Government in March 2020. This report incorporates feedback from those consultations.
Use of Attend Anywhere
At the time of our evaluation, Attend Anywhere was being used for a wide range of conditions and clinical services (see summary table Appendix A). Three different service models were in use:
- Hub-home: Clinician connects from clinic to patient at home.
- Dyadic hub-spoke: Clinician in specialist 'hub' centre connects to patient in remote 'spoke' health or care site without additional staff member present (e.g. in an unstaffed kiosk).
- Triadic hub-spoke: Clinician in specialist 'hub' centre connects to patient in remote 'spoke' health or care site with an additional staff member (nurse, GP, healthcare support worker [HSW]) present.
In all the above models, the specialist clinician occasionally consulted from home.
Video consultations via Attend Anywhere were occurring in all 14 local Health Boards and at the Golden Jubilee National Hospital (NHS Scotland's National Waiting Times Centre). Two boards, Highland and Grampian, had both been 'early adopters' and accounted for 62% of all activity in 2019, but use of Attend Anywhere was still at an early stage in most Boards. The Attend Anywhere service in Highland was strongly branded as 'NHS Near Me' from the outset; the 'Near Me' branding was subsequently applied across the whole country.
In 2019, almost 7000 consultations were conducted via Attend Anywhere across approximately 35 different clinical specialties involving 180 clinical departments and 64 GP services; 91% of this activity was in secondary (i.e. hospital care). Attend Anywhere has also been used by a number of third sector organisations to provide advice, support, counselling and palliative care to service users. This includes two services in particular: Rape Crisis Grampian (159 consultations during 2019) and MS Revive (which supports people affected by multiple sclerosis: 120 consultations).
We observed many examples of up-and-running video consultation services using Attend Anywhere, and heard predominantly positive comments from staff and patients, who described various advantages of video consultations over conventional face to face appointments, although some clinicians had concerns about video consulting in general. However at the time of our study (up to Mar 2020), the proportion of Attend Anywhere activity in relation to other outpatient appointment activity (i.e. face to face and telephone appointments) still appeared to be relatively low. In the highest-using health board, video consultations were estimated to be 1-2% of overall board activity. Across all health boards, many services were still at early stages of implementation, and there was great variation in terms of levels of activity. Approximately 130 clinical departments (70%) had conducted five or more video appointments during the 12-month collection period.
Key Findings
Using the domains of the NASSS framework, our assessment of the reasons for both the adoption and use of Attend Anywhere, and its relatively limited uptake to March 2020, are listed below.
Clinical appropriateness
a. Attend Anywhere consultations appeared to be most readily implemented for routine follow-up of chronic, stable conditions, especially when the main purpose of the consultation was to convey test results and affirm that the patient remained asymptomatic. Clinicians generally considered it clinically inappropriate and unsafe to use remote consultations for poorly-defined and less predictable conditions, rare conditions, and those where specialist tests or treatments were unavailable locally. In relatively high-volume specialties such as diabetes and heart failure with well-established clinical networks (e.g. where specialist nurses and GPs with special interest worked from a community hospital with a specialist available for phone advice), local staff considered that video consultations were rarely clinically needed.
b. For some conditions, such as care of the elderly with complex needs, there were both advantages (e.g. less travel) and disadvantages (e.g. deafness, low digital literacy) with remote consulting by video.
c. The triadic hub-spoke model could also support care of more complex conditions such as chronic pain or cancer. Such models relied on a high degree of trust between the specialist and the local staff member; they seemed to depend on a positive and longstanding personal relationship between them, and (often) individualised training. Such models tended to work well until a particular individual left but then folded, raising questions about their sustainability.
The Technology
a. The Attend Anywhere technology was, in general, dependable and produced high-quality video and audio, partly due to the software and partly because many services (especially in Highland) had invested in high-quality peripherals such as screens and noise-cancelling microphones. Patients reported that staff with strong accents were harder to understand via a remote connection.
b. The kit available in most clinics (both hub and spoke) was experienced by staff as easy to set up and use, and more or less standardised instructions and protocols were found across the country. The strong 'Near Me' branding in Highland was popular with most but not all staff.
c. Many clinicians expressed reluctance to move from a hub-and-spoke model to a hub-home model because they would be unable to control the technical quality of the patient's connection and also because some clinicians considered the home setting inappropriate for clinical or confidentiality reasons. In some settings, patients were assessed for their suitability to use the hub-home model and offered a trial technical connection before their appointment.
d. Attend Anywhere is modelled on the workflow of a medical clinic (rather than a conference call), with a 'single point of entry' (typically a button to click on the hospital website) and a virtual waiting room for each patient, where the clinician can join them when ready. We observed many clinicians and reception staff who were adept at managing the 'arrival' of patients and the virtual waiting room; we also met staff who had not yet gone up the learning curve for this task and who were uneasy about this step.
e. We identified some technical problems with integration of Attend Anywhere software with appointment-booking software in hospitals (usually TrakCare), and also compatibility issues with internet browser and local network firewall arrangements that were in place in some hospitals (notably, the Golden Jubilee Hospital National Waiting Times Centre).
Summary of benefits as perceived by staff and patients
Staff and patients described various advantages of the Attend Anywhere service over conventional clinic appointments.
a. Less need for travel meant financial savings (including patient travel, staff travel and the costs of staff accompanying patients transported between sites), environmental benefits (reduced carbon footprint) and less stress and hassle. Some patients were too unwell to make long journeys.
b. Access to specialists was sometimes quicker and more direct, and with advanced technology, specialist opinions could be provided (e.g. ophthalmology examinations using a virtual slit lamp).
c. Staff and patients perceived the virtual consultations to be shorter and more to-the-point (for example, time was not spent bringing the patient into the room).
d. The triadic model allowed a support nurse or GP to directly observe a difficult conversation (e.g. breaking bad news or explaining options).
e. In some cases, the hub-home model allowed holistic care of a complex or dying patient by involving family carers in the consultation.
f. Occasionally, patients who were reluctant to attend hospital (e.g. because of past trauma) were able to engage with the service.
g. Because Attend Anywhere created the possibility to radically redesign a service, some staff members gained development opportunities. They received bespoke training from a specialist clinician, which, along with self-study, allowed them to undertake aspects of an extended role under supervision.
Other staff views about Attend Anywhere
With few exceptions, the concerns we heard were not about the technology but about the concept of video consulting in general or the logistics of the service.
a. A minority of staff interviewed (most of whom had had little or no experience of Attend Anywhere) were opposed to video consulting on principle, mainly because they felt it threatened the quality and safety of the clinical consultation, especially the ability to connect emotionally and develop a strong therapeutic relationship with the patient.
b. Other staff were supportive in principle but saw no immediate clinical need to set up video consultations. GPs in remote sites, for example, were happy to do home visits to the few patients who could not get to the surgery, and staff in remote community hospitals said that patients had to attend for their blood tests anyway so might as well see the clinician at the same time. For those in less remote sites, the introduction of video was rarely a priority.
c. Some staff who had not yet set up Attend Anywhere locally (or been involved in a video consulting service) described a high logistical barrier to establishing and running a video consultation service (e.g. developing a new system of transmitting a prescription to the patient's local pharmacy when the patient was not there to take it).
d. Some staff in remote community hospitals expressed concern that the introduction of video clinics would mean "losing" a consultant-led local service (in the sense that a monthly in-person visit would cease), though other staff in the same settings depicted the change in terms of "gaining" a service (in the sense of access to certain specialists who had previously been unavailable).
e. Our dataset included two examples of consultants who were depicted as providing poor value for money because they provided clinics from a distant location without committing to training and developing local staff or helping to improve the service.
Organisational conditions associated with implementation and scale-up
a. Organisations which adopted Attend Anywhere most readily had the following features: a receptive context for change (history of successful innovation; strong, visionary leaders; a clear, positive narrative about the technology; and good data systems that can monitor the effects of the change in a timely way), slack resources (people or money that could be channelled into the change effort), a predominance of supporters over opponents, and senior clinical and management buy-in.
b. Variation in preconditions and the presence or absence of innovators (people keen on new products and new ways of working), champions (people who believe in an innovation and seek to persuade others of its benefits) and change agents (people with the skills, time and personal qualities to drive through the change and recruit others to help) helped explain why different specialties and remote sites came on board with Attend Anywhere at different rates.
c. Sites where Attend Anywhere was working well (notably Highland and Grampian, which had a longer history of using virtual consultations to improve access from remote areas), had taken a system approach to supporting spread and scale-up, informed by the principles of participatory co-design, workflow redesign and quality improvement. In some sites, the introduction of Attend Anywhere clinics was strongly data-driven and strategic (for example, to address the problem of a service that was underperforming or the retirement of a key specialist).
d. Such examples appeared to be more embedded and enduring than when a local Attend Anywhere service had been set up by a single enthusiast, or where the project was framed in terms of installing a technology, making sure it works and responding to problems.
e. Both dyadic and (even more so) triadic hub-spoke models raised logistical challenges and required various kinds of double-handling (e.g. appointments needed to be made, rooms booked, and staff members made available, at two sites). In some remote sites, there was much redundancy (e.g. staff were allocated to a hub clinic for a whole morning but only one or two patients were seen); in others, a lone staff member had to juggle multiple roles.
f. Hub-spoke appointments also depended on a strong sense of mutual awareness. To ensure smooth running of the clinic at the remote site, for example, staff in the 'hub' site needed to gain a sense of the realities and pressures there and accommodate to those. Where this did not happen, the clinic was perceived by staff and patients as problematic and stressful.
Wider contextual issues
a. The strategic drivers for introducing Attend Anywhere in Scotland include a strong national policy push for technology-enabled care; a system-wide quality improvement ethos (a major goal of which was to reduce the human, financial and environmental burden of travel); the emergence of a new generation of high-quality, affordable technology; and positive feedback from patients. But as noted above, these drivers did not play out evenly, since some organisations were inherently more innovative and had a more conducive set of preconditions.
b. Staff and patients in all the sites we visited were proud of their NHS, which they saw as reflecting deeply-held and widely-shared core values including high-quality universal healthcare provision and equity of access. In this context, the Attend Anywhere video service was generally (but not universally) seen as enhancing the existing service rather than replacing or threatening it.
c. The introduction of video consultations, especially to rural and remote areas, should be seen in the context of a wider move to improve connectivity and reduce isolation for Scottish citizens (e.g. the 'Reaching 100%' infrastructure to deliver superfast broadband to 100% of homes and businesses by end 2023 and the 'Infil' programme to improve mobile coverage in Scotland). The expansion of these broadband and 3G/4G networks provide multiple routes for Attend Anywhere to be used across the country. Whilst 92% of Scottish homes now have access to broadband, for many this has happened relatively recently.
d. The TEC Attend Anywhere scale-up programme has played a key role in providing local programme leads with the technical and human resource needed to introduce and support the new service model. But it has also facilitated the inter-organisation learning, leveraging national level resources for support (e.g. the national video consulting (VC) support team) and informing national level policies (e.g. ICT infrastructure standards) that have a bearing on local implementation of Attend Anywhere in clinical settings.
Outcomes
In 2018 the Scottish Government commissioned a TEC Data Review and Evaluation Options Study [2], which presented potential outcomes of a generic VC workstream. We have used our analysis to reflect on likely contributions to the potential short-term outcomes shown in that model, summarised briefly below.
a. Increased number of patients using VC instead of face to face. Clear increase in Attend Anywhere appointments. However, context of use is important, such as an understanding of what video is actually replacing (e.g. home visits or out-patient clinic appointments; phone or face to face appointments).
b. Improved access to specialist services. Greatly improved access for patients living in remote areas, and to rapid specialist opinion.
c. Less need to travel. Reduced travel and other time savings for patients living in remote areas and travelling from the islands.
d. Improved management of certain conditions. VC can support person-centred and holistic care; multi-disciplinary and multi-site working with the patient; and infection control.
e. Improved access for hard to reach groups. Improved access for patients with frailty, multi-morbidity or anxiety; but risks excluding people with low digital literacy, confidence, access to technology.
f. Reduced professional travel and improved efficiency. Reduced need for travel among clinicians, allied health professionals and specialists on-call for emergency care; improved service efficiency and quality.
g. Improved collaboration between professionals and new ways of working. Opportunities to redesign services, develop less specialist staff and create new local service capabilities.
Recommendations
Based on the findings, we suggest the following actions to support continued scale-up, spread and sustainability.
Recommendation 1: Produce for each clinical specialty 'rules of thumb' for what kind of clinical conditions and encounters are generally safe for video consultations.
Recommendation 2: Basic training and multiple try-out opportunities for staff and patients.
Recommendation 3: Develop and disseminate analysis of system-level evidence about potential financial savings from Attend Anywhere.
Recommendation 4: Identify and address clinical and care governance and safeguarding issues.
Recommendation 5: Working with professional networks, disseminate stories of up-and-running services.
Recommendation 6: Communicate the "gaining a service" narrative.
Recommendation 7: Assign and support local champions.
Recommendation 8: Provide set-up support for ready-to-roll sites, paying careful attention to routines between participating sites.
Recommendation 9: A Quality Improvement Collaborative to maximise inter-site learning.
Recommendation 10: Implement a consistent national branding for the video consultation service across the country.
Postscript
A further phase of the evaluation has been commissioned to explore the rapid scale-up of Attend Anywhere in response to the COVID-19 pandemic.
Contact
Email: socialresearch@gov.scot
There is a problem
Thanks for your feedback