Demand optimisation in diagnostics: standardising diagnostic testing in NHS Boards
Report highlighting current good practice, guidance on strategy and support for implementing demand optimisation.
Section 3: NDOG Output
This section details the overall activity and output of the NDOG in relation to the aims stated above.
3.1 Information Gathering
On establishment, the national Demand Optimisation Group ( DOG) sought to identify relevant work taking place at a local level to address demand optimisation / demand management issues.
Demand Optimisation Survey - Summary Findings
The Demand Optimisation survey was circulated to all NHS boards delivering diagnostic services (Laboratory and Radiology). The main aim was to understand how demand optimisation governance and work streams were managed and delivered across Scotland.
The survey highlights an appetite across the NHS Boards to delivery around the overall ambitions of demand optimisation, in providing the 'right test, at the right time, for the right patient' in order to provide appropriate clinical testing and treatment. There is significant variation across Scotland in terms of the existence of a co-ordinated delivery and associated governance, along with limitations in IT systems and a lack of tools to measure baseline activity and overall clinical impact.
The key points highlight:
- The majority of boards do not have a formal demand optimisation group or committee operating at NHS board level; there are different governance models in operation across the boards
- There is variation across the boards with adoption of national guidelines and minimum retesting intervals.
- There is variation across the boards in the provision of activity feedback to clinical users.
- The survey highlighted some good areas of demand optimisation practice.
- The survey highlighted that currently demand optimisation initiatives in general have not been linked to patient care quality or outcomes.
- There is no national IT platform, with limited local ability to control the ordering of tests
Overall Findings
Evidence from the survey and case studies highlighted that Demand Optimisation was high on the agenda for Scottish NHS Boards given the current financial climate; however, there was a lack of consistency and coordination with much variation apparent. The known limitations of the "silo budget" effect and IT systems that were not fit for purpose/interoperable across boards also came to light.
Demand Optimisation Test Case Library
Where the diagnostic exercise identified innovation, greater detail was sought to allow the development of a library of Demand Optimisation test cases.
The aim of such work was to allow cross-fertilisation of knowledge in this area and to act as a catalyst for change for a variety of clinical and management teams working within Health and Social Care.
Examples of work include:
- Collaborative working between laboratory services, Sexual Health and Primary Care to optimise the diagnosis of female genital infection.
- Optimisation of the use of urinary culture in asymptomatic patients to ensure that it was not used where results were unlikely to alter clinical management.
- Evidence based alteration to the protocol for serological testing for rheumatoid arthritis.
- The use of a dashboard tool within Primary Care to provide feedback on the use of diagnostic tests and optimise their appropriate use within this setting.
- A review of the clinical appropriateness of the need to refer samples for the assessment of markers CA19-9 and CA153 to laboratories.
- Reviewing the constituents of the Liver Function Test Panel.
Examples of work from the library can be found at appendix B.
3.2 Demand Optimisation Data
The ability to identify and measure diagnostic test use activity is fundamental to any Demand Optimisation programme. The existence of such data brings with it many opportunities:
a) Benchmarking of diagnostic test use - allowing comparisons between GP practices, hospital wards or even NHS Boards.
b) Identification of variation in practice enabling interventions to be formulated and targeted towards known problems.
c) Specific identification of under and over requesting areas allowing targeted outreach interventions to be made with minimal resource implications.
d) Pulling of "Big Data" to allow clinical observations to be made and linkage with other benchmarking data to assess public health issues, impact and uptake of guidelines and clinical strategy effect assessment.
e) Longitudinal data allowing assessment of Demand Optimisation strategies and trends in specific test requesting.
f) Financial planning and identification of resource intense practice areas.
Keele benchmarking - it was acknowledged that all laboratories participate in Keele benchmarking which includes data collection on diagnostic test utilisation. This data is not however suitable for the kind of interrogation required to allow specific identification of sub-optimal requesting behaviour - such as GP practice level data.
Information Services Division ( ISD) Role - Discussion also took place between members of the NDOG and ISD regarding any utility of data that they currently collect. It was once again acknowledged that the source, availability and level of data collection was not suitable currently for full demand optimisation purposes. Furthermore, the lack of standardisation of diagnostic test coding and the lack of interoperability between the Health Board systems meant that such data could not feasibly be collected on an automatic basis and would require manual download/extraction at Health Board level followed by compilation in order to allow pan-Scotland comparisons to be made.
3.3 Atlas of Variation Pilot
It was decided early on that the NDOG, given their remit and time limitations, would not be in a position to deliver a comprehensive Atlas of Variation for Scotland. It was instead proposed that a proof of concept pilot would be developed to assess the ease and feasibility of data collection and the potential opportunities that such data would bring.
Background
The NHS England Diagnostic Atlas of Variation was published in November 2013. The focus in this publication was on diagnostic tests and incorporated data from not just Laboratory Medicine, but also some limited data on radiology, endoscopy and other physiological diagnostic services. In summary, the Atlas showed the variation in the requesting of diagnostic tests across the then 151 Primary Care Trusts ( PCTs) adjusted per 1,000 population. The large variations exhibited require further discussion as to their validity, significance and potential for corrective action.
Across the range of diagnostic testing examined, there are of course valid reasons to explain some of the variation observed: different PCT populations/case-mix, deprivation, disease incidence/prevalence, local policy decisions on specific services and availability of relatively new diagnostic services. Despite that, some of the variations in test requesting seen remain so significant that the only conclusion is that they represent the individual requesting patterns by doctors collectively within each PCT. As examples, even when outliers are trimmed off, the variation in the requesting of ALT, rheumatoid factor, CA125, vitamin D and urine protein-creatinine tests showed 56, 170, 9, 392 and 334-fold differences respectively across the PCTs. The significance of such variation in requesting, whatever the reason, needs further consideration.
Such variation in the use of diagnostic tests can be said to have significant impact not only on the utilisation of scarce resources within the NHS but also can have real impact on patient care and subsequent morbidity and mortality. It should also be emphasised that while these differences between PCTs are large enough in themselves, when the data is drilled down further to individual practices or indeed individual GPs, then the variations are multiplied even further.
These differences do of course matter and do reflect different approaches being used to manage patients by individual practitioners, between practices and even across different PCTs. Much of this variation may reflect inappropriate use of resources but more importantly may signal sub-optimal and even damaging patient care as a result of inappropriate diagnostic choice.
While this data originates from English PCTs, it is likely that very similar variations in requesting would be observed across other regions of the United Kingdom including Scotland. Benchmarking of requesting rates is not a new concept, nor is the observation of large variations in such requesting patterns. Explanations for the potential variation in diagnostic testing observed are many. The variation in diagnostic test use demonstrated within the NHS England Atlas could not be explained by differences in patient numbers or health demographics. It is likely that similar unwarranted variations in diagnostic test use exist across NHS Scotland.
Methodology
Laboratory Services within NHS Grampian and Tayside volunteered to formulate and collect data relating to GP practice utilisation of laboratory tests in order to test proof of concept that the relevant data could be easily collected, combined and made use of to highlight variation and inform demand optimisation strategies.
Data on individual GP practice requesting rates for laboratory tests were collected for an entire year (Sept 1 st 2015 to August 31 st 2016) from the Laboratory Information Management Systems ( LIMS) of NHS Grampian and NHS Tayside. This data was combined with information including GP practice list size so that requesting patterns could be adjusted for this confounder and allow more appropriate analysis and comparisons to be made.
The following tests were targeted for data collection:
- General - Sodium, Creatinine, Bilirubin
- Bone - Calcium, Vitamin D, PTH
- Endocrine - TSH, fT4, fT3, Glucose, HbA1c
- Cancer - CA125, CEA, PSA
- Cardiac - Cholesterol, TGS, HDL
- Therapeutic Drugs - Lithium, Phenytoin, Carbamazepine
- Immunology - Thyroid Peroxisomal Abs, Rh Factor, IgE ( RAST)
- Haematology - FBC, B12, Folate (serum + red cell), Ferritin
- Urine - Protein/Creat ratio, albumin/creat ratio
A data download was extracted from the Laboratory Information Management System ( LIMS) operating within Laboratory Services of NHS Grampian and Tayside using a standard query based extraction tool - this enabled the relevant fields to be populated on an Excel spreadsheet for further analysis. While LIMS will differ across the NHS Boards, the process of data extraction relating to requesting rates attributed to specific geographical locations is straightforward and usually carried out on a regular basis - such as for data collection for Keele Benchmarking returns and for turnaround time evaluations. Despite the lack of interoperability, there should therefore be no barriers to the NHS Boards contributing a common format excel based data extraction with the requesting rate data required for this process.
Results
Firstly, the data was relatively easily extracted from the LIMS systems of both NHS Boards. Secondly, it became clear that the data would be able to provide a snapshot of laboratory requesting activity and allow comparisons between the two NHS Boards and the GP practices contained within.
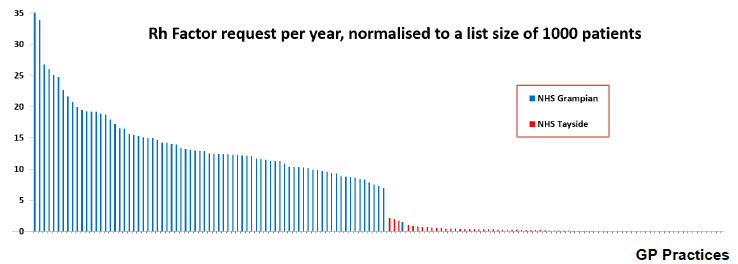
As expected, significant variation in requesting was demonstrated across the GP practices. Figure 2 shows the variation between both NHS Grampian and Tayside for requesting rates for Rheumatoid Factor, a blood test. Clearly, this test is rarely used across NHS Tayside, whereas across NHS Grampian Practices there is a 70-fold variation in requesting rates for this test, which remains around 7-fold when outliers are stripped off.
Figure 2. Rheumatoid Factor requesting rates across GP Practices within NHS Grampian and Tayside
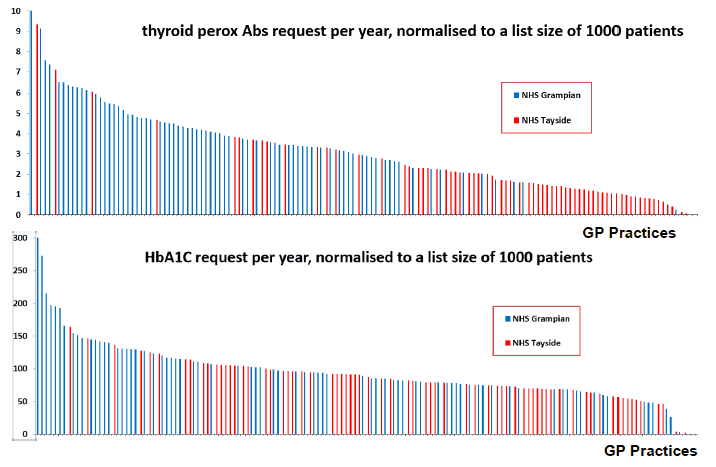
Similarly, tests for Thyroid Peroxidase Antibodies (figure 3) show a 10-fold variation in adjusted requesting rates across practices, whereas that variation is 5-fold for HbA1c - a test for diabetes diagnosis and monitoring (figure 4).
Figures 3 and 4. Thyroid Peroxidase Antibodies and HbA1c requesting rates across GP Practices within NHS Grampian and Tayside
Conclusions
This pilot demonstrated proof of concept that laboratory services within NHS Grampian and Tayside were able to extract the relevant data that could be used to populate a Scottish Atlas of Variation. It is likely that other NHS Boards would also be able to provide this data on a rolling basis.
The pilot also demonstrated that there exists across the GP practices assessed, significant variation in requesting that pointed towards sub-optimal utilisation or availability of diagnostic tests. This observation is likely to be replicated across the rest of Scotland.
Clearly existence of this data on a Scotland wide basis would allow the focus and targeting of specific demand optimisation strategy to be implemented.
3.4 General Demand Optimisation Guidance.
A guidance document highlighting the main, "Top Ten", implementation strategies for demand optimisation that could be introduced across all NHS Boards was formulated by the group - this is available as Appendix C. A particular focus within the guidance on Minimum Retesting Intervals has also given rise to more specific guidance on this with priority MRIs documented as Appendix D.
The aim of this document was to illustrate clearly the main strategies that all NHS Boards should be implementing and to drive consistency across Scotland. The actual uptake and implementation of the strategies contained within the guidance relies heavily on sufficient governance structures and mechanisms within the NHS Boards to allow this to happen.
3.5 Educational Feedback in Primary Care
This workstream stemmed from activity already happening across NHS Grampian in 2016. It was agreed that its development was relevant and would serve as a proof of concept/pilot for potential roll out across other NHS Boards.
As well as the planned ongoing pilot within NHS Grampian, there was also discussion within the NDOG around the potential for such requesting rate activity to be made available on a rolling basis for GPs - an example system made available to GPs across NHS Grampian is in development that provides such data via a Sharepoint Web access login. It is worth noting that the data collection for this is the same data set/source as is used for the enhanced educational feedback service and indeed for a proposed Atlas of Variation. In addition, it would also be feasible to enhance this dataset further by adding in the relevant costs of specific laboratory tests and providing clinical areas with a comparative measure of their diagnostic financial burden to the NHS.
Enhanced Educational Feedback in Primary Care Pilot
Background: The feedback of laboratory test requesting rates to GP practices along with educational guidance on appropriate test use is not a new concept, having been trialled elsewhere - notably within NHS Grampian as part of a randomised controlled trial reported in the Lancet in 2006 (Thomas et al. The Lancet 2006; 367: 1990-1996). This labour intensive paper-based intervention carried out ten years ago has now been replaced by an automated electronic system that involves the generation of PDF feedback tailored to specific GP practices.
Methods: Tailored feedback documents detailing requesting rates (adjusted for practice list size and in comparison to NHS Grampian averages) for general and specific laboratory tests were generated for all 78 practices (578 GPs) across NHS Grampian and reported electronically to the practice managers/ GPs. Educational messages were also appended for the focused tests. This process was repeated on a two monthly basis commencing August 2016.
The targeted tests were selected on the basis of tests that a perceived variation in requesting was suspected or were thought to be of particular clinical importance. An example of the enhanced educational feedback report can be seen in Appendix E.
Results: The first observation being that the extraction of the data was straightforward and the incorporation into a spreadsheet with automated report generation macros built in was feasible and achievable. Secondly, it was clear that significant variation in requesting existed across the tests being assessed - similar to that observed from the Atlas of Variation pilot work given the common origin of the data.
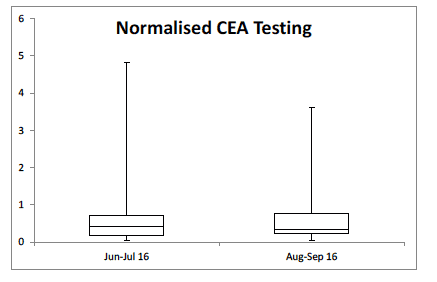
At time of writing, the project has just delivered its second of two monthly individualised feedback reports to GP practices. As educational interventions are likely to take some time to demonstrate effect, it is probably still too early to see the expected changes in requesting rates - these changes may not necessarily equate to overall reduction in requesting but may simple be reflected as a reduction in variation (reflecting a reduction in both under and over-requesting). For example, two month changes in overall requesting rates for the Tumour Marker CarcinoEmbryonic Antigen ( CEA) has shown a reduction in requests from 1.49 to 1.11 (average requests per 1,000 population), with a contraction in overall variation (p = 0.05). While small at this stage, these changes would signal a potential reduction in inappropriate use of this test which would not only save laboratory resource but also other unnecessary healthcare knock-on effects.
Figure 5. Initial change in Requesting rates for CEA across NHS Grampian
Conclusions: This piece of work demonstrated proof of concept that the relevant data could be easily extracted and incorporated into electronic, automated feedback reports for Primary Care that provided them with comparative requesting rate activity and educational support to promote appropriate test use. It is likely that this tool could be populated with data by other NHS Boards and rolled out in a similar fashion. Similar applications for Secondary Care could also be developed.
3.6 Information Technology ( IT) Guidance
The importance of fit for purpose IT systems to allow interrogation of diagnostic test use and to ease the implementation of specific strategies cannot be under-estimated. The NDOG has formulated a set of guidance aimed at directing NHS Boards along a consistent path that takes into consideration the issues and challenges that provide both opportunities and barriers to demand optimisation strategy implementation. The guidance can be found in Appendix F.
Ideally, the whole approach to demand optimisation and the move to promote more rational use of diagnostic tests would be enhanced if common IT systems could be adopted across NHS Scotland. Within laboratory services, the concept of a common LIMS and a national laboratory medicine catalogue with standardised test name, units of measurement, reference intervals and IT coding remains a huge challenge but one which should remain as a high priority in the longer term.
3.7 Effective Diagnostic Pathways ( EDPs).
It is clear that variation exists between NHS Boards regarding the availability or the way in which specific tests are used within patient pathways. This exploratory piece of work looked to scope out ways in which standardised diagnostic pathways (patient pathways that are particularly heavy on diagnostic test incorporation) can be defined from a national level under a "Once for Scotland" approach. This may then make it easier for local Health Board funding and implementation to be realised. This approach could be potentially used not just for new or emerging diagnostic tests but also for established ones where there is noticeable variation in the way the test is being offered, used or interpreted across the NHS Boards.
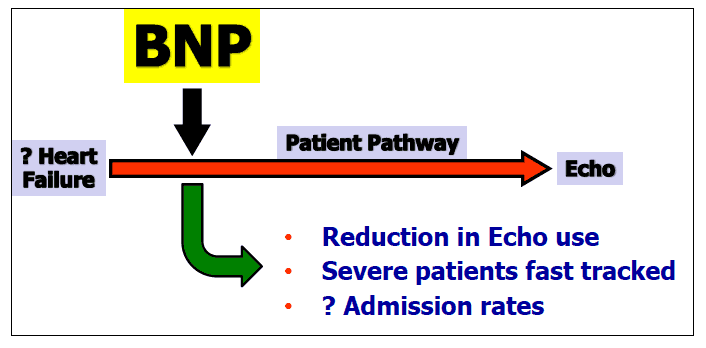
Examples of potential EDPs can be focused around specific diagnostic tests, disease pathways or be symptom based. The use of B-Type Natriuretic peptide ( BNP) for example, could be focused at all three levels - use of the test within a primary BNP test pathway, a cardiac failure pathway or a breathlessness pathway. A possible schematic for the use of BNP is illustrated below (figure 6), with the main reasoning being that its use can triage breathless patients for echocardiography thereby saving resource and allowing more critical/severe cases to be dealt with quicker. Following recommendation of best practice there would be the need locally to determine the operational requirements and relevant contribution of Primary Care, relevant specialties and clinical professionals in delivery of the pathway
Figure 6. EDP for B-Type Natriuretic Peptide use in patients with suspected heart failure
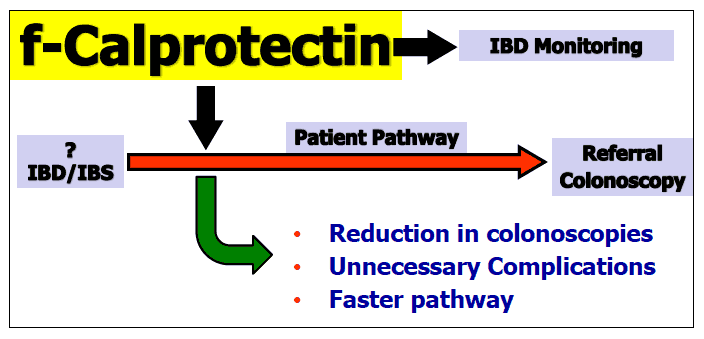
Another example would be the use of the Faecal Calprotectin test, whereby similar triage of patients to colonoscopy could be rationalised by the use of this test. The pathway is outlined below (figure 7) but with commentary required again to define where in the healthcare system this should be carried out.
Figure 7. EDP for Calprotectin use in patients with symptoms of possible inflammatory bowel disease ( IBD) or irritable bowel syndrome ( IBS)
Governance and Implementation
A major barrier to the implementation of new diagnostic tests is the typical silo budget arrangement that generally applies to services across the NHS Boards. Therefore even when there are potential savings for the NHS, and more importantly, improvements in patient care, from the introduction of new tests it is difficult to get that investment into laboratories to enable such provision. Flexibility within laboratory budgets to enable delivery of new tests is further constrained by the need to balance laboratory budgets subject to cost improvement programmes. Conflicting priorities placed on Boards for resource combined with a siloed rather than a whole system focus on return on investment delivers barriers to improvement. This is why we see significant variability across NHS Scotland in terms of availability of newer test such as BNP and Calprotectin - effectively, post code diagnostics.
It is essential therefore that NHS Boards formulate mechanisms and governance arrangements to help ensure that EDP recommendations can be explored from an entire patient pathway perspective and to create enough fluidity with budgets to allow savings made in one part of the NHS to flow back to other parts that are taking a financial hit to stimulate the pathway.
Contact
Email: Karen Stewart