Demand optimisation in diagnostics: standardising diagnostic testing in NHS Boards
Report highlighting current good practice, guidance on strategy and support for implementing demand optimisation.
Appendix C - General Demand Optimisation Guidance
THE SCOTTISH NATIONAL DEMAND OPTIMISATION GROUP
Demand Optimisation in Diagnostic Services - Guidance for Implementation
Background
Demand optimisation is defined as the process by which diagnostic test use is optimised by maximising appropriate test requesting which, in turn, optimises clinical care and drives more efficient and effective use of scarce resource. Interventions need to be focussed on not just minimising over-requesting, but also under-requesting and reducing unnecessary repeat requesting. The concepts defined and the aims formulated within the National Clinical Strategy 1, Realistic Medicine 2 and the Shared Services 3 agenda align directly with the objectives of demand optimisation given its focus on reducing waste, minimising variation and the promotion of appropriate testing within a patient centred healthcare system. This guidance outlines strategy that should be considered for implementation across all diagnostic interfaces within NHS Scotland.
There are many areas across the diagnostic test end to end pathway whereby demand optimisation interventions can be implemented:
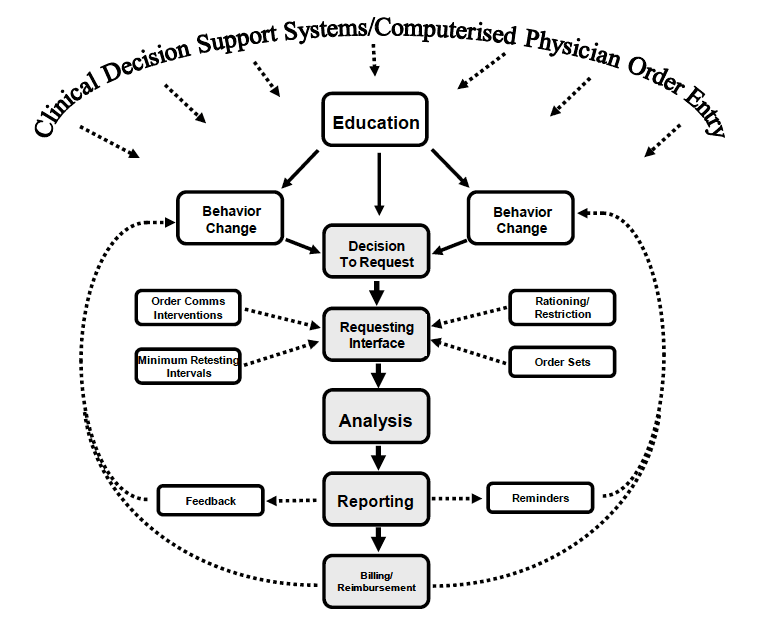
* adapted from Croal BL4 - Opportunities for Demand Optimisation strategy implementation across the diagnostic test end to end pathway.
It will be in the best interests of NHS Scotland and patient care if an organised and consistent approach towards the implementation of demand optimisation strategy can be realised. The NHS Scotland National Demand Optimisation Group for Diagnostic Services would therefore outline the following key interventions and processes as being essential for implementation across all Scottish NHS Boards.
1 Diagnostic Workload Data Collection
The fundamental key component for any demand optimisation programme has to be the ability to measure and compare diagnostic test demand and use. This is vital to not only highlight unwarranted variation (over and under requesting) but also to allow gaps in test availability to be identified (both new and existing tests). In addition, such measures of workload can serve as a baseline from which to assess the effectiveness of particular demand optimisation strategies.
The NHS England Diagnostic Atlas of Variation 5 published in 2013 used test requesting data from 151 Primary Care Trusts to demonstrate large variation in test use across many key diagnostic services. Such variation could not be explained by differences in patient numbers or health demographics. It is likely that similar unwarranted variations in diagnostic test use exist across NHS Scotland.
For many years, laboratory services have submitted workload data to the Keele Benchmarking Service. It will be important that a refreshed look at the value of this exercise is made with a focus on collecting data that will be more aligned with the demand optimisation objectives. The potential for a Scottish Atlas of Variation for Diagnostic Services needs to be considered.
Principle 1: All NHS Boards to collect local data relating to diagnostic test utilisation and actively engage with national programmes of diagnostic workload data collection including a potential future Atlas of Variation.
2 Workload Feedback to Users
The value of feedback of diagnostic requesting data to clinical services has been well documented within the Scottish NHS 6,7. Such requesting data can help diagnostic services identify areas of potential over and under requesting and allows the user groups to ascertain their own requesting behaviour patterns in comparison with their peers. The addition of other data such as financial costs or educational commentary on best practice can further enhance the positive effect on driving more appropriate test use.
A pilot of an enhanced educational diagnostic test use feedback in Primary Care is currently being assessed within some of the Scottish NHS Boards. The possibility of a live SharePoint database that will allow users to see their own live requesting patterns in comparison to local, regional and national data is also being explored. Similar but different strategies for secondary care requesting feedback will also need to be developed.
Principle 2: All NHS Boards to consider actively implement strategies to allow feedback of diagnostic test use requesting data to clinical services. Early adoption of national roll out of common mechanisms should be prioritised.
3 Minimum Retesting Intervals Implementation
Unnecessary repeat testing represents wastage within scarce healthcare budgets. The concept of defining, where possible, time intervals whereby repeat testing would be unjustified, is one that could be useful for demand optimisation purposes. The Royal College of Pathologists have recently published guidance on Minimum Retesting Intervals in Pathology 8 (2015). This guidance serves as a baseline for laboratory services to define, in conjunction with their users, a strategy for limiting unnecessary repeat testing within their domain.
While some requesting interval blocking can be made at the laboratory/radiology department level, focus should be paid to the point of request, usually at the available requesting interface - such as the order communications module, in order that unnecessary test requests can be avoided at this stage before an order is made or a specimen taken. The early adoption of automated IT systems, as they are developed, should be encouraged.
The National Demand Optimisation Group will issue separate guidance on Minimum Retesting Intervals that focus on key priority areas to implement.
Principle 3: All NHS Boards to actively implement minimum retesting intervals strategy. Adoption of automated IT systems should be encouraged in order to implement such strategy.
4 Diagnostic Request Vetting
Diagnostic test request vetting is of much value - especially for high cost or potentially harmful procedures such as is found in Radiology. Vetting strategies vary but may only be practical when the necessary clinical information is provided or when the volume of requests is low enough to practically enable this process to be efficiently performed. Low volume/high cost diagnostic tests should be prioritised.
Vetting can also be carried out using IT functionality if available - currently such requesting interface functionality is early in development. Vetting at this level can of course be carried out more simply on the basis of location of request, via an additional added question at the order comms level or via a minimum retesting intervals strategy.
Principle 4: All NHS Boards to implement diagnostic request vetting where practical, focusing on high risk, high cost but inevitably low volume type tests. Early adoption of electronic vetting processes should be encouraged.
5 Terminology Standardisation
Significant variation exists across Scottish diagnostic services with regard to how diagnostic tests are named, requested and reported. Additional variation exists within laboratory medicine at the level of units of measurement, reference intervals and the components of composite test panels - such as U&Es, LFTs, etc. There would be significant advantages to the Scottish NHS, clinical research, patient safety and the economy, if standardisation could be developed that would allow true interoperability between NHS Boards to exist. Such standardisation within radiology largely exists, however this is not the case within laboratory medicine. This will limit the big data approach, composite research databases, direct to patient results and many of the demand optimisation strategies identified in this document.
Developments such as the National Laboratory Medicine Catalogue ( NLMC) should be supported along with piecemeal harmonisation exercises emanating from Colleges, Societies and the Scottish Managed Diagnostic Network system. In the interim, adoption of diagnostic test request translation services such as the National Pathology Exchange ( NPEX) should be encouraged for all send away testing from Scottish laboratories to facilitate safe and efficient data transfer across Health Board boundaries.
It is also vital that any send away tests and point of care testing activity is also incorporated within the electronic diagnostic test domain and ultimately is recorded within the electronic patient record.
Principle 5: All NHS Boards should seek to adopt national consensus harmonisation/standardisation recommendations and make plans to implement NPEX and NLMC coding when available.
6 Information Technology Solutions
It has become clear that many of the recommended interventions to promote rational and appropriate diagnostic test use are dependent on IT solutions with the necessary functionality to align with such strategy. Such functionality to support test vetting, minimum retesting intervals, decision support and indeed test requesting data collection/feedback is very much in its infancy. It is therefore vital that diagnostic services play close attention to the availability/early adoption opportunities of such functionality and ensure any procurement processes across Order Comms, Laboratory Information Management Systems ( LIMS) and linked clinical databases contain the demands of such functionality within the relevant service specifications.
The National Demand Optimisation Group will issue separate guidance on this topic.
Principle 6: All NHS Boards to actively implement IT solutions that support and facilitate demand optimisation strategies and ensure future IT procurement for diagnostic services incorporates the likely functionality required.
7 Local Health Board Governance Structures
Implementation of a national, consistent approach to demand optimisation across all Health Board areas requires considerable buy-in and collaboration. It is vital that any recommendations on national demand optimisation strategy are supported by local health board governance that allows implementation and control of such activity. It is vital that such governance structures incorporate not just diagnostic service involvement but also embrace representation and collaboration from clinical services, primary care, management and financial sectors within the boards - a whole systems approach.
Principle 7: All NHS Boards to develop multi-disciplinary governance structures to assist the implementation and management of demand optimisation strategies that enables whole system approaches to implementation and funding.
8 Effective Diagnostic Pathways Implementation
Health Improvement Scotland ( HIS) have recently developed plans for a programme of work focussing on Effective Care Pathways ( ECPs) 9. This work is likely to focus on pathways of care that encourage best practice and a consistent value driven delivery of healthcare. Given that diagnostic tests are involved in the vast majority of all clinical decisions made across healthcare, it has been recognised that many of these ECPs will incorporate or be heavily influenced by diagnostic test use. The National Demand Optimisation Group has been developing a parallel strategy of Effective Diagnostic Pathways ( EDPs) as standalone recommendations on diagnostic test use. These will initially be focussed on areas where variation in test use is perceived but will also be useful in promoting the adoption of new tests across all NHS Boards, thereby minimising the diagnostic postcode lottery that currently exists.
Initial EDPs will focus on breathlessness (natriuretic peptides), Bowel disease (calprotectin/ NFIT) and tests for DVT (D-Dimer) as examples.
Principle 8: All NHS Boards to engage with the ECP/ EDPs strategy and implement any recommended pathway locally. The developing "whole systems approach" demand optimisation governance structures within the boards could be used to facilitate such pathway adoption.
9 Specialist Services Consolidation
The shared services agenda for diagnostic services promotes the concept of 'Once for Scotland'. While this approach is not suitable for the vast majority of diagnostic test services, there will be some areas identified whereby duplication of high cost or highly specialised services could be deemed as sub-optimal use of healthcare resource. This may include specific radiology examinations, some specialised histopathology services and some metabolic/genomic based testing within blood sciences. The shared services programme is likely to address some of these options in the near future.
Principle 9: All NHS Boards to engage with the shared services programme and implement any recommendations on specialist services rationalisation or consolidation.
10 Educational Support
Education relating to appropriate diagnostic test use has been challenging in recent years as formal diagnostic teaching has decreased within medical schools in favour of a 'systems' approach. As a result, many feel that the general knowledge around appropriate diagnostic test use has significantly diminished.
All NHS Boards should be encouraged to re-engage with their medical, nursing and AHP staff to facilitate learning around rational diagnostic test use. The advent of e-learning, on-line CPD, eKSF and personal proficiency testing provide the potential opportunity to incorporate such educational input. Additional educational guidance should also be implemented via any diagnostic test requesting feedback strategy and as a component of any developing diagnostic electronic decision support modules within IT systems.
The adoption of the Medical Undergraduate Curriculum 11 by RCPath should also be promoted through all NHS Boards incorporating Medical School involvement. In addition, there should be a national approach from the National Demand Optimisation Group and the Managed Diagnostic Networks to develop common learning material on appropriate diagnostic test use for widespread dissemination.
Principle 10: All NHS Boards should actively provide educational support to facilitate better understanding of appropriate diagnostic test use amongst all staff. Use of nationally produced material should be encouraged.
Conclusions
The implementation of activity to support demand optimisation is vital for modern, efficient diagnostic services. Diagnostic services must be equipped to work with and enable users to optimise requests for examinations within a patient centred context and be able to deliver effective knowledge rich reports to the point of care that deliver the maximum positive impact to a patient pathway.
This document provides basic guidance to all NHS Boards to assist the facilitation and implementation of interventions to promote appropriate diagnostic test use. It remains vital that such strategy is supported by not only national guidance and inter-board collaboration via the diagnostic networks, but also by the development of specific and explicit governance arrangements within NHS Boards that incorporate diagnostic services, clinical users, management and financial elements. In this way a true culture of demand optimisation can be realised at all levels of healthcare interface across NHS Scotland.
References
1. The Scottish Government, 2016. A National Clinical Strategy for Scotland. http://www.gov.scot/Resource/0049/00494144.pdf
2. The Scottish Government, 2015. The Chief Medical Officer's Annual Report 2014-15. Realistic Medicine. http://www.gov.scot/Resource/0049/00492520.pdf
3. Shared Services. http://www.sharedservices.scot.nhs.uk/health-portfolio/
4. Croal BL. Demand Management: Controlling Laboratory Workload. In Evidence Based Laboratory Medicine, 2nd Ed. Chapter 18. AACC Press, Washington DC, 2007.
5. Right Care 2013. The NHS Atlas of Variation in Diagnostic Services: Reducing unwarranted variation to increase value and improve quality. http://ukgtn.nhs.uk/fileadmin/uploads/ukgtn/Documents/Resources/Library/Reports_Guidelines/Right_Care_Diagnostics_Atlas_2013.pdf
6. Eccles M, Steen N, Grimshaw J, Thomas L, McNamee P, Soutter J, Wilsdon J, Matowe L, Needham G, Gilbert F, Bond S: Effect of audit and feedback, and reminder messages on primary-care radiology referrals: a randomised trial. Lancet 2001, 357:1406-9.
7. Thomas RE, Croal BL, Ramsay C, Eccles M, Grimshaw J. The effect of enhanced feedback and brief educational reminder messages on laboratory test requesting in primary care: A cluster randomised trial. The Lancet 2006; 367: 1990-1996.
8. The Royal College of Pathologists 2015. Minimum Re-testing Intervals in Pathology. A Final Report Detailing Consensus Recommendations for Minimum Re-testing Intervals for Use in Pathology. https://www.rcpath.org/resourceLibrary/g147-minretestingintervalsinpathology-dec15-pdf.html
9. Effective Care Pathways Programme. http://ihub.scot/a-z-programmes/effective-care-pathways-programme/
10. The Royal College of Pathologists 2014. The Pathology Undergraduate Curriculum. https://www.rcpath.org/resourceLibrary/pathology-undergraduate-curriculum-.html
Contact
Email: Karen Stewart