Demand optimisation in diagnostics: standardising diagnostic testing in NHS Boards
Report highlighting current good practice, guidance on strategy and support for implementing demand optimisation.
Appendix B - Demand Optimisation Test Case Library
The library will continue to build as the DOG work progresses its implementation phase. It can be found at http://www.mcns.scot.nhs.uk/dog/resoures/test-cases/
NHS Forth Valley
Collaborative working between laboratory services, Sexual Health and Primary Care to optimise the diagnosis of female genital infection
Collaborative working between the laboratory, Sexual Health services and Primary Care was undertaken in NHS Forth Valley with the aim of optimising the diagnosis of female genital infection. Traditionally clinicians had taken two swabs when undertaking vaginal examinations to look for bacterial infection in the vagina and cervix as well as a third swab of the cervix to screen for infection with Chlamydia. These swabs were then sent for formal processing within the laboratory. By testing the acidity of the vagina within Primary Care it was possible to reduce the requirement for testing by laboratory services for a number of these patients. The basis of such change being guidance provided by Sandyford Sexual Health Services in Glasgow and the local Sexual Health Services within the Board.
The benefit of such a change in diagnostic practice allows more timely prescription of treatment to those whom will benefit while ensuring that where specific diagnostics are required that these targeted to maximise diagnostic yield while minimising waste. In turn this reduces workload at all stages of patient journey and has potential to result in cost savings.
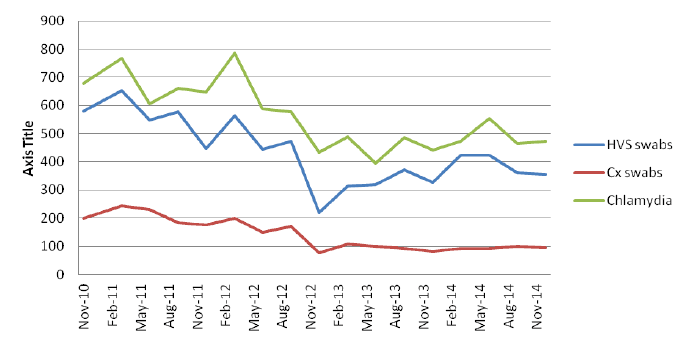
As illustrated in the chart below there was clear evidence that the number of samples received in the lab before and after the alteration of the diagnostic pathway fell. More recently it has become common place to undertake urinary testing for Chlamydia in those defined at risk and although the numbers of endocervical tests has fallen this has been offset by the less invasive and more patient centred modality of testing.
Monthly Primary Care HVS & Servical swab (for culture),
and Chlamydia PCR test Nov 2010 - Dec 2014
NHS Tayside
Optimisation of the use of urinary culture in asymptomatic patients to ensure that it was not used where results were unlikely to alter clinical management.
The introduction of a laboratory testing algorithm by NHS Tayside was undertaken to deliver demand optimisation in the diagnosis of urinary tract infection. Using their unique laboratory requesting interface, clinicians were required to confirm that the patient was symptomatic for infection (eg abdominal pain, fever, burning on urination, need to pass urine frequently, offensive smell or colour to urine or acute confusion) at the time of the test request. Where patient was asymptomatic they were required to confirm whether there was an another appropriate indication for the test to take place. Examples being pregnancy, acute confusion, sepsis, post renal transplantation or the need to screen for organisms showing antibiotic resistance.
The system was also configured to provide evidence of best practice in the diagnosis of urinary tract infection. The basis for this process of demand optimisation was evidence that many asymptomatic patients were having samples submitted for culture at the time of routine urinalysis ( e.g. diabetic review or hypertension check). Clinicians had assumed that where there was evidence of protein, leucocytes, blood or nitrites that the sample should be submitted for culture and that in many cases patients were prescribed antibiotics that were not indicated and had potential to cause side effects or result in bacterial resistance.
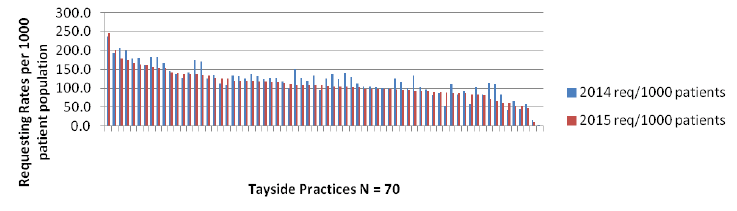
The effectiveness of this intervention was measured and the graph below shows evidence of a change in clinical practice in the requesting of urine cultures and a reduction in variability by individual practice. The algorithm is in place across NHS Tayside and where outliers are identified it is planned that support will be provided to discuss reasons for this variation with the practice. It will only work if the algorithm can be implemented on the Board's laboratory test requesting system (Tayside use ICE).
MSU Requesting Rates in Tayside Primary Care
Headlines
51 (73%) practices showed an overall fall in the rate of
requesting, though 2 surgeries showed no discernible change
28 (40%) of 70 practices showed a greater than 10% reduction
in requesting rates
17 (24%) of 70 practices showed an increase in rate of
testing
Biggest fall in requesting was 39.3% in one surgery
Biggest rise in requesting was 46.1% in one surgery
2014 median fell from 124 to 107 per 1000 practice patients
overall
The efficiency gains through the implementation of guided decision making for the clinical service user: 16865 MSU investigations avoided, £3,373 costs avoided.
The limitations of such change is the requirement that IT system in place locally has to be configured in a manner to allow decision aided requesting and at the present time this is not universally available across Scotland with variation by Boards in the systems used to support laboratory services.
NHS Tayside
Evidence-based alteration to the protocol for serological testing for rheumatoid arthritis
Partnership working between the Immunology Laboratory and Clinical Rheumatology Service in NHS Tayside identified that patient referrals for rheumatoid arthritis were disproportionately high in comparison to the expected epidemiology.
To address such a discrepancy the clinical decision was taken to alter the primary serological screening pathway for rheumatoid arthritis. The change from IgM rheumatoid factor ( RF) to IgG anti-cyclic citrullinated peptide ( CCP) antibodies was undertaken in 2005.
CCP is a more clinically specific test (Clinical specificity CCP >96% versus 86% for RF) and provides a more useful serological tool to triage patients with high likelihood of RA to secondary services, thus reducing inappropriate referrals.
Full demand management protocols were introduced in the laboratory resulting in increased scrutiny of CCP and RF requests. Processing of samples was undertaken being cognisant of clinical presentation for Rheumatoid Arthritis and relevant prognostic criteria. This protocol has continued for the last 10 years.
To this end it rationalised the requesting of rheumatoid serology by:
1. Removing the large scale (7500 per annum; 1.6% of total population of Tayside each year) inappropriate requesting of rheumatoid factor by users for general joint pain.
2. Use the funding saved by removing 95% of requesting for RF, to introduce CCP as the front line test for RA. NHS Tayside also undertook management of that change by clinical evidence based demand management, with a target to maintain testing of CCP to 1000 test per year (0.2% of total population of Tayside). Readers of this paper should note that Rheumatoid Arthritis is a rare disease, epidemiological evidence shows that the frequency of new presentations in the UK is 1:5000-10000 patient years (This would result in an estimate of 90-180 new patients each year in NHS Tayside.)
3. The process also allowed the diagnostic and clinical service to work together to minimise the inappropriate referral for patients with positive RF and no clinical evidence of RA, to secondary care rheumatology services.
This work has been shared with other diagnostic immunology providers in Scotland and as a result is being considered by other Boards with a view to introduction within a number of other laboratories. The process has also resulted in the consideration of whether similar work could be undertaken in the diagnosis of Connective Tissue Disease.
NHS Forth Valley
Primary Care Whole System Working
Laboratory managers participated in a Primary Care Whole System Working project in 2011/12 within NHS Forth Valley. The aim of such work being to use a dashboard to provide targeted feedback and identify variation by clinicians requesting diagnostic investigations.
One of four priority areas for this project was laboratory and radiology services. This included a review of biochemistry requesting of cholesterol tests.
The aim was to encourage adherence to the NHS Forth Valley Lipid Lowering Guideline which recommends that for primary prevention of cardiovascular disease there is no need to recheck cholesterol levels. The project ran between May 2011 and March 2012 with the GPs providing feedback on the workstreams in September 2011.
The laboratory worked with Forth Valley Information Services department to provide data to GPs on their requesting of laboratory tests and allow comparison with other practices in Forth Valley.
The project encouraged best practice and resulted in a sustained reduction in primary care cholesterol requests, with the clear benefit to patients and laboratories of reduced unnecessary testing.
The project also provided an opportunity for GPs to reflect on clinical behaviour through the use of comparative data which demonstrated variation. The project subsequently promoted and provided best practice guidelines and an evidence base.
The inclusion of laboratory tests was encouraged through the Community Diagnostic Users Group - a group established in 2009 to improve communications between diagnostic and primary care and to help inform primary care of new developments and best practice. Laboratories, radiology, cardiology and endoscopy are represented along with service managers and GPs. This highlights the need for appropriate governance to support service change and improvement.
Areas chosen to prioritise were those where guidance exists or was being developed:
- The use of Lumbar Spine X rays in Lower Back Pain
- The use of Abdominal Ultrasound
- The use of B12/Folate assays
- The use of MSSU in non-pregnant women with simple UTI
- The 'Treat and Forget' strategy in Primary Prevention of Cardiovascular Disease
The NHS Forth Valley Lipid Lowering Guideline v4 (2010) was used to inform the Treat and Forget part of the workstream and cholesterol requesting was reviewed.
GPs were asked to reflect upon their own activity levels compared to that of other practices in NHS Forth Valley. Practices were also asked to undertake sample audits of their own clinical practice to inform their reflective learning. Information on requesting rates for cholesterol were provided. The Treat and Forget strategy augmented significant levels of work already undertaken by the Forth Valley prescribing team.
The majority of GPs were happy to now adopt the Treat and Forget strategy although some remained concerned as the change is hard to explain to patients who have undergone many changes in their lipid management.
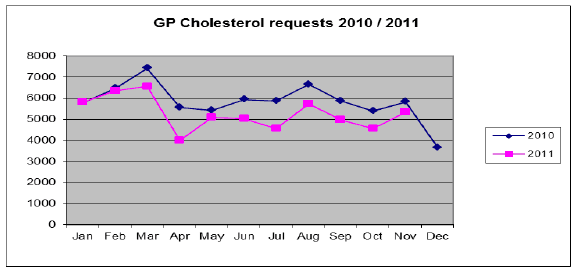
Data collected by the laboratory show a reduction in the use of cholesterol following the project. The Whole System Working project 2011/12 report contained chart 1 below:
Chart 1. Cholesterol activity 2010/2011 taken from the
Whole System Working 2011/12 Output Report
Updated data on GP cholesterol requests is shown in chart 2 below:
Chart 2.
GP cholesterol
activity 2009 - 2014
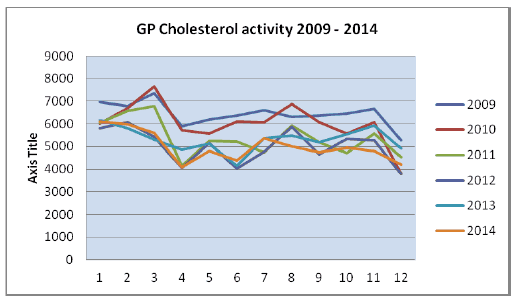
The percentage reduction in annual GP cholesterol activity in 2014 compared to 2010 is 16.8%, just over 12,000 tests a year. The project has been completed and the change to requesting cholesterol has been sustained.
Laboratory testing was included again in the 2012/13 Whole Systems Working project but not since then.
The Community Diagnostic Users Group continues to meet regularly and provides an invaluable communication link to primary care including discussion about requesting in relation to patient pathways. The introduction of a direct ordering system in Forth Valley over the past 12 months has involved this group in agreeing test groups for primary care and approving any changes.
Unfortunately no such group currently exists for secondary care diagnostics users due in part to the variety of specialities and the difficulty of providing an agenda that would be of interest to all.
Access to up to date laboratory test data is very important when reviewing the effect of changes on demand e.g. when new guidelines are issued. A dashboard is being developed by the Forth Valley Information Services department which currently holds primary care requesting information. A similar dashboard for secondary care will be the next development, which will be a key enabler in the identification of waste and variation.
NHS Highland
A review of the clinical appropriateness of the need to refer samples for the assessment of markers CA19-9 and CA153 to laboratories outside local lab.
NHS Highland carried out a review of CA19-9 and CA153 referrals to outside laboratories.
The aim was to reduce the numbers of samples sent away for testing, also to ensure that the tests were being performed on appropriate patients e.g. patients with KNOWN pancreas cancer and KNOWN metastatic breast cancer.
This review was undertaken because a previous review of samples revealed that a number of CA19-9 tests were being done as part of 'tumour marker screen' which was not an appropriate indication for testing
Despite reporting no reduction in the number of tests; there has been benefit to patients as tests are now being done on the correct patients e.g. for appropriate indication.
This work is now being carried out in the board and there is currently a vetting of tumour markers as part of the duties of the Duty Biochemist.
NHS Fife
Transforming Liver Function Testing
Colleagues in NHS Fife improved services by transforming the liver function test ( LFT) profile by withdrawing gamma-glutamyltransferase ( GGT) and total protein. Both tests are still available should they be required through requesting on a case-by-case basis; however they are no longer automatically done as part of the LFT.
GGT is considered the least specific of the LFTs and continually causes GP colleagues problems when they receive a result that is slightly abnormal and "do not know what to do with it". A few years ago it was removed from the LFT profile in the Acute Hospital. That resulted in a dramatic fall in GGT workload at that time, which has continued. It was therefore hoped that this finding would be repeated with GGT requesting in Primary Care. At the same time it was decided to review the LFT profile further and explore the impact of removing total protein.
Following the introduction of the change in May 2016,
GGT requests
have fallen by 90% and total protein by 98%. Both tests are still
available and workload will be continually monitored.
Projected savings are about £8000 per year
Following on from the success of this exercise this is now standard practice in NHS Fife. It was highlighted that getting the full support of the Medical Directors, together with dialogue with service users was an essential part of the process. The NHS has made cost savings with no change in the availability of tests.
Contact
Email: Karen Stewart